Abstract
Introduction
One in 14 people older than 65 years, and 1 in 6 of those older than 85 years has a form of dementia. Estimates indicate that in 2013 there were 815 827 people living with dementia in the United Kingdom, a figure expected to increase to more than 1 million by 2025. 1 However, approximately only one-third of people living with dementia receive an accurate diagnosis 2 ; leaving a significant number of people with dementia without access to appropriate care and support. Considerable emphasis is now being placed on addressing low diagnosis rates, and in England, the government has expressed its commitment to these with the National Dementia Strategy (NDS) for England. 3 The NDS aims to enhance awareness about dementia, increase diagnosis rates and increase earlier diagnosis, and develop a higher quality of care. Diagnosis is a crucial part of the dementia journey; the manner in which this is handled is of considerable importance to people living with dementia, their families and carers. A “good” diagnosis in terms of accuracy, timeliness, and delivery leads to better patient outcomes. 4 Earlier diagnosis results in longer periods of higher quality of life and of living at home, as well as major savings in hospital and residential care costs. 5 Obtaining a diagnosis enables people to plan for the future, as well as providing treatment options; pharmaceutical and nonpharmaceutical. Historically, dementia diagnosis was considered the remit of old age psychiatry, remaining the case until the early 1980s with the introduction of memory clinics, a model of care adopted from the United States. Memory clinics intended to provide a less stigmatized approach to the assessment and diagnosis of memory problems and dementia than old age psychiatry. 6
National Institute for Clinical Excellence (NICE) guidelines recommend that memory assessment services (MAS) should be a single point of referral for people with dementia, provided either by a memory clinic or community mental health teams (CMHT). Memory clinics have been seen as the way to meet this guidance. The 2013 English National Memory Clinics Audit 7 estimated that there are 214 memory clinics in England. The Memory Services National Accreditation Programme (MSNAP) 8 outlines a set of standards and criteria that memory services should aim to attain. The overarching principles around these standards are that everyone with memory problems has fair access to assessment and that they receive person-centered care. Memory assessment services (clinics) are considered to be cost-effective on the basis that they facilitate early diagnosis and have the potential to prevent 10% care home admissions per year. 9 While there is evidence that memory services can be clinical and cost-effective, the implementation of these services has been stifled by capacity limitations. For example, after their inception specialist memory clinics quickly became overwhelmed with referrals, had long waiting lists, and were unable to provide follow-up. 10 Furthermore, an audit of memory services by the NHS Information Centre found that, while 94% of primary care trusts and health boards said they commission memory services, less than 32% of them were nationally accredited, and over a quarter lacked some of the recommended features of a memory service. 11
Primary care–involved services offer one route to easing the burden on secondary care–based memory services. The All Party Parliamentary Group (APPG) on Dementia (2012) 12 report suggests that Primary Care could be an ideal route for addressing low diagnosis rates in the United Kingdom. More recently, there have been amendments to the NICE clinical guidelines for supporting people with dementia (GC42) which recognize the role of “other healthcare professionals such as GPs, nurse consultants and advanced nurse practitioners with specialist expertise in diagnosing and treating Alzheimer’s disease” in relation specifically to the initiation of pharmacological interventions—in the past, this was limited to secondary care medical specialists. 13
The APPG suggests that general practitioner (GP) services are well placed to initiate the assessment of people with dementia, this might be particularly useful for hard to reach communities reluctant to access secondary care. One reason for this might be a greater prevalence of stigmatizing views about dementia, which makes accessing mental health services more problematic. 14 For this reason, locating services in primary care is a route to promoting access to services for these communities, for example engaging people with nurse practitioners at a local practice has been shown to increase referrals to specialist secondary care–based assessment services. 15 This evidence suggests that primary care is well placed to play a role in diagnostic care pathway, even if unable to act as a single point of referral, that is, for initial assessment and/or less complex cases—with more complex presentations the reserve of specialist services. 16 Recent initiatives such as the Directed Enhanced Service demonstrate a government led impetus to enhance the involvement of primary care in screening and diagnosing people with memory problems. 17 The Royal College of General Practitioners has also pioneered developed a set of criteria for GPs with a special interest in dementia suggesting that specialist GPs have a significant role to play in the assessment, postdiagnostic support, and end-of-life care for people living with dementia. 18
In response to policy initiatives and evidence suggesting primary care has a role in assessment a range of different models of service within primary care have been developed.19-21 This review provides a summary of the types of service design currently being employed across England and the extent to which they involving primary care, with examples of innovative practice being highlighted. Issues for the future, including the need for more integrated postdiagnostic support, are also discussed.
Method
The rapid review literature search was conducted in July 2016. Rapid reviews use aspects of the systematic review process in order to produce the key information of interest in a relatively short time frame. 22 Rapid review methodology was chosen as it is well suited to synthesizing evidence in a timely manner and is perceived as useful in health care settings to inform decisions and practices. 23 We sought to elicit evidence to enable us to understand the nature of the involvement of primary care in diagnostic pathways for people with dementia. On the basis of established rapid review methodology, the review was directed at the following databases felt to be most likely to elicit synthesized and good-quality evidence (Cochrane, PubMed, Google Scholar). The search terms were agreed by authors to relate to and meet the needs of the study question. The search terms that were used were: “dementia diagnosis pathway,” “dementia care pathway,” “primary care pathway dementia,” and “assessment pathway dementia.” Three databases were searched in the following order: Cochrane, PubMed, Google Scholar, for potential to include reviews and elicit significant health related primary research. Searches were restricted to articles published since 2000, and in the case of Google Scholar, where >2000 records were returned for each search term, the search was conducted on the first 40 pages of items. More than 70 000 results were initially returned. The first author performed a manual search of the titles and abstract according to the eligibility criteria to establish inclusion. For inclusion, articles must have considered patients with dementia, present dementia assessment pathways in England. Articles included could present primary evidence such as an evaluation of a service or a review of relevant services. Articles were excluded if they described pathways that were not based in England, focused on secondary care–led services, focused on pharmacological interventions, were neurobiological in focus, described randomized control trials, palliative care, or were primarily concerned with more general mental health care in older adults or adults with learning disabilities. After the initial title and abstract search, 6 articles were included. A further full text screening of each document was then conducted by both authors to ensure eligibility.
Figure 1 outlines the search process. When articles duplicate discussions of pathways, this is indicated in Table 1.
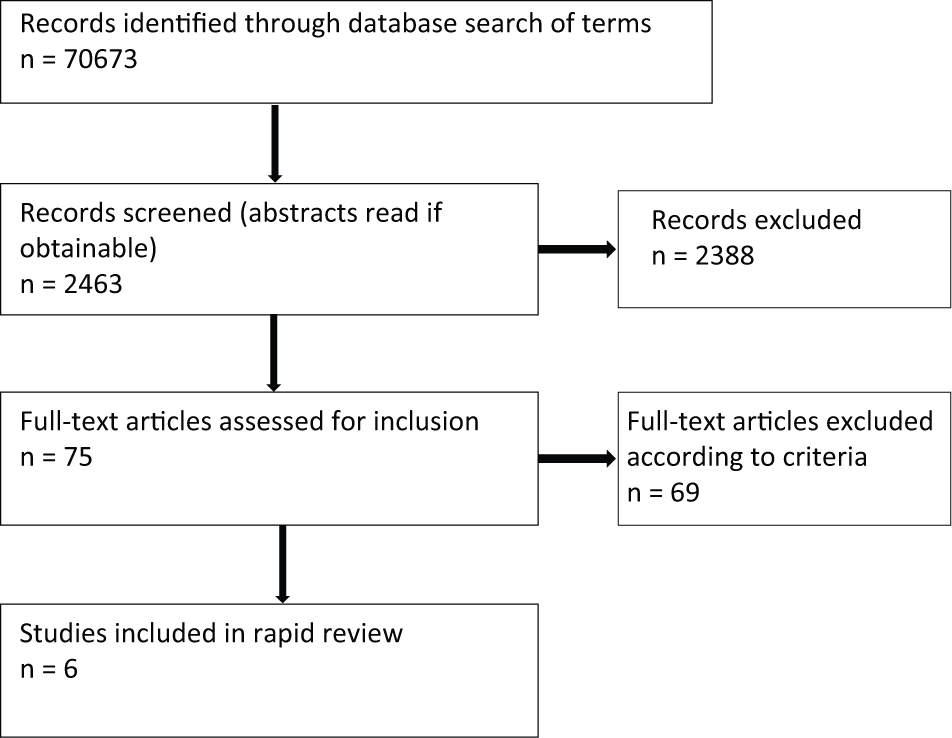
Flow chart of studies included in the rapid review.
Data extraction table.

Abbreviations: CMHT, community mental health team; GP, general practitioner; MAS, memory assessment services; MCI, mild cognitive impairment; MDT, multidisciplinary team; OT, occupational therapist.
The authors constructed a data extraction plan on the basis of information that would help us to understand the question of the review, namely the nature of the involvement of primary care in assessment and diagnosis pathways. The related to the extent and quality of the involvement—therefore data were extracted according to the following parameters:
Type of primary care involvement—where service is led, practitioner involvement, location of service, activities of service
Quality of primary care involvement—the outcomes of evaluations of these interventions (when such evaluations were included); useful statistics indicative of the success of services, eg, reductions in waiting times for appointments after referral; evidence of innovative practice and feedback from service providers and service users (when this information was provided).
Results
Six articles and reports were identified which discussed current pathways or evaluated pilot services, with some articles including more than one service. The articles discuss services that are situated in a wide range of geographical locations across England. The section below outlines these pathways and highlights examples of innovative practice being implemented across a range of regions in England.
Evaluative Review of Current Pathways and Services
Minghella 24 audited 5 diagnostic pathways in the southwest of England, a region with comparatively low diagnostic rates. The 5 services (referred to by color to maintain anonymity) reflected existing variation of service design. The primary aim of the Green service is that GPs are primarily responsible for diagnosis and treatment, with only more complex cases or individuals younger than 65 years referred to the MAS. Subsequently, diagnosis rates increased from 37% to 53% of expected prevalence in 1 year. Alterations were also made further along the pathway. The caseload of ongoing reviews was reduced and therefore freed up MAS staff to spend more time on assessment. The Yellow service offers assessment and diagnosis in 1 appointment. Referrals are managed by a primary care referral management system which reviews referrals, liaises with the MAS and CMHT and then allocates referrals to the appropriate services. Patients undergo one 2- to 3-hour appointment at the clinic for full assessment and diagnosis by a nurse, psychologist, and psychiatrist. While the “one-stop shop” was perceived to have benefits, both service providers and users noted that the process may be too quick and overwhelming for some. 13
Three well-established services were also included in the evaluation. The Blue service is a secondary care–based service and largely nurse-led. It reported the longest waiting time for referral, which was attributed to the fact that primary care services had much less input into the process. The Red service is also secondary care based and nurse-led. The team has close links with the older people’s mental health team, with input from a multidisciplinary team (MDT), including a consultant psychiatrist. The service provides central and community-based clinics with most patients seen by the lead nurse in a clinic. The Purple service is clinic-based and comprised an MDT of physicians, psychologists, nurses, and occupational therapists. It is an independently run organization with charitable status and has a considerable research component. The services outlined in this audit highlight the variation in current pathways, with some services moving toward situating assessment and diagnosis within primary care. 13 Efforts are being made to both reduce referral times for diagnosis and improve the timeliness of the diagnostic process itself. Interestingly the author notes that the services with the shortest waiting times are also those that had more primary care involvement in diagnosis and treatment (see Table 1). This had the additional benefit of allowing MAS staff to focus more time and effort on more complicated presentations.
The positive role of primary care–led services in reducing referral times and improving diagnostic rates is also supported by a recent qualitative study reporting on the experiences of health care professionals and service users of primary care–led dementia diagnosis services in South Gloucestershire. 25 The findings support the assertion that practitioners perceive a primary care–led service to enable a faster and more efficient process, where GPs feel confident to make a diagnosis. However, it was also noted that there is a need to balance speed and efficiency with the need to enable people with dementia and their families sufficient time to process the news of a diagnosis, an issue also raised through feedback about the Yellow “one-stop shop” service. 24
Another relevant article evaluated primary care–led services in Bristol, 26 conducting interviews with service users and providers. The service model was piloted in 11 of 53 GP practices between August 2012 and December 2013. The aim was to provide accurate and timely diagnosis within primary care whenever possible. Three memory nurses were seconded to work with the 11 practices, and GPs in the pilot took part in a training session on assessment and diagnosis. The remaining 42 practices continued to use the preexisting model whereby patients with suspected dementia symptoms were referred on to secondary care. Evaluation of the pilot found that GPs felt cautious about making a diagnosis, with some GPs referring cases onto the nurses for assessment rather than just consulting them for advice. Interestingly, patients and carers gave positive feedback for both primary and secondary care based services, their experiences with the memory nurses being the most valued aspect irrespective of where the care was based. The new model was deemed a success and implemented across Bristol as of January 2014.
Further evidence that primary care–led service evaluations can lead to equivalent levels of satisfaction has been demonstrated by the the Gnosall Memory Clinic, established in Stafford in 2006, 27 which delivers a primary care–based pathway. Monthly memory clinics are held at the GP practice, and are run by a psychiatrist. Patients who are believed to be at risk or who report memory problems are seen by their GP and may be referred on for further assessment. They are referred to the practice eldercare facilitator, 28 who arranges a home visit to make a more thorough assessment of the patients’ needs and then, if appropriate, arranges an appointment at the next memory clinic. Appointments include assessment, provisional diagnosis and plans for further investigation if necessary. Follow-up is usually conducted through progress reviews in the practice. The eldercare facilitator remains in close contact with the patient and their family postdiagnosis, with one aim being to help identify and access appropriate support. Patients and carers have been positive in their feedback about the memory clinic, and there is interest in replicating this model more widely. 28 Other examples in equity of efficiency of service were seen in the South Gloucestershire services, 14 which found that similar numbers of people seen in primary care services are diagnosed, referred onto specialist services or declined assessment.
Koch and Iliffe 29 outline a primary care–based pathway developed through partnership with a GP surgery, the Alzheimer’s Society, and the older peoples’ CMHT in Berkshire. 19 Patients are seen for assessment, diagnosis, and initiation of treatment in a “one-stop” clinic. The clinic is staffed by a MDT, including psychologists and memory nurses. This service reduced waiting times from 15 to 4 weeks and throughput of patients doubled. The development of this service has featured an inbuilt process of research, evaluation and stakeholder involvement from early on to help refine and redevelop the pathway. 29 This demonstrates models initiated in CMHT can be replicated in primary care without impact on the quality of service.
Innovative Practice
Many of the pathways feature elements of innovative practice. The Green service 24 ensures that all GP practices are dementia-friendly, with dementia leads in each. They run events aimed to educate and increase awareness (eg, holding “local roadshows”). Receptionists receive training, which has produced positive results (eg, identification of behavior, such as forgotten appointments, which may indicate the presence of memory problems). Some services incorporate home visits whenever possible, including the Green service. 24 Others, such as the Berkshire clinic, follow a clinic-based “one-stop shop” model, the primary aim being to provide diagnosis and support within as short a time frame as possible. 29
The use of standardized memory assessment has been seen as a barrier to good-quality assessment and diagnosis in primary care, and many GPs report being under confident in the use of standardized tests. 30 This is an aspect of the process that is being addressed by some GPs. One example of innovation and changing practice has been highlighted by Koch and Iliffe. 29 A GP in Warwickshire reported a significant increase in diagnostic rates when they began using the Mini-Cog, a test designed to be administered by nonspecialists. They also reported that, due to its ease of administration it could also be used by district nurses. After implementation, rates of diagnosis increased to more than twice the national practice average. In another example, a West Country GP used the 6-item Cognitive Impairment Test (6-CIT) instead of the MMSE, and similarly found this helped to increase diagnosis rates. Consequentially, other local GPs adopted this test and reported similar increases.
In summary, the adoption of quicker screening tests that can be used by nonspecialists can elicit increased diagnosis rates but also improves the confidence of GPs in diagnoses. Many people that are undiagnosed with dementia are living in care homes. The identification of dementia in people living in care homes is important to facilitate access to important care and support. Anecdotally, practitioners report the use of standardized assessment tools with this population can be problematic. For example, people may be too severely impaired to complete assessments using standardized tools. Koch and Iliffe 29 identified that the use of nonstandard assessments and intuition can prove beneficial in these circumstances. For example, a London GP providing care for a residential/nursing home conducted assessments as routine on admission to the home. He did not use validated screening tools in the first instance, instead gathering a detailed history of deteriorating memory and functional capability of the patients from their relatives. He reported finding the screening tools as useful when there was uncertainty about differential diagnosis.
Recognizing the Value of Multidisciplinary Team Members
In addition to enhancing the abilities and role of GPs in assessment and diagnosis, efforts are being made to expand the contribution of other health professionals, as evidenced by the use of a health visitor as the intermediary in Gnosall and receptionists at the Green service.24,27 Services such as Gnossall and GP practices in Bristol 26 have designed services that make use of preexisting expertise based in secondary care and relocating it within primary care. The development of distributed responsibility is in line with Department of Health recommendations.
In summary, the articles reviewed provide an overview of the current state of provision of assessment and diagnosis of dementia in primary care. Key aspects are discussed below, as are some additional issues that arose and are of broader relevance.
Discussion
The articles discussed in this rapid review demonstrate that considerable effort is being made to improve the assessment and diagnosis of dementia through the integrated use of primary care. This is being achieved both service redesign and the implementation of innovative approaches. Some of the services discussed are being (re)designed through the incorporation of primary care–led memory clinics which potentially provide a less stigmatized method for people with suspected memory problems to access support (eg, for minority ethnic communities 15 ).
Involvement of primary care in service delivery appears to be beneficial on the whole. This was highlighted in the report by Minghella. 24 It was noted that GPs tend to be involved in the diagnosis of older and more frail people, for whom progression through a more lengthy and complex assessment pathway may be inappropriate. This suggests that a “one fits all” approach to service design would not fit the needs of all patients and contravene principles of person-centered care central to the NDS, 3 ensuring that services meet the needs different patient groups.
Evaluative data suggested that patients are generally happy with services provided in primary care.24,26,27,28 Partial involvement of primary care is also beneficial, such as the referral management service incorporated into the Yellow service presented in the report by Minghella. 24 Indeed systems such as this may reduce waiting times for secondary care–based services. If diagnosis and ongoing support is provided within primary care this will enable MAS staff to see the more complex cases much more quickly, which will be of huge benefit to patients.
Innovations often involve use of preexisting resources, such as drawing on staff from a wider team to facilitate assessment and diagnosis services.24,27,28 While the findings from the review encourage innovative practice, one of the emergent issues is the importance of thoroughly evaluating new developments to highlight possible negative outcomes. For example, Dodd et al 26 found that GPs in the Bristol pilot were very positive, reporting that it was very useful to be able to discuss patients with the memory nurse. Conversely, the nurses reported that liaising with the GPs was time consuming, and sometimes led them to take on assessment-related duties rather than maintaining an advisory role. This may indicate that greater provision is needed in terms of training to ensure that GPs with this responsibility feel more confident in their ability to provide diagnoses independently of the memory nurses.
The issue of training underpinning the successful implementation of primary care–led services is one that has been identified in the past. This ties into the notion that the reluctance to embrace support for people with dementia in primary care may be associated with therapeutic nihilism, risk avoidance, concerns about competency, and resources. 31 A large-scale complex randomized control educational intervention that took place in the Netherlands (EASYcare) for dyads of GPs and primary care nurses indicated that training elicits positive benefits for adherence diagnostic procedures as well as enhancing diagnostic accuracy. 30 The Dementia Training Programme increased the number of cognitive assessments, improved adherence, and also improved recipient’s attitudes toward people with dementia. Ensuring that primary care practitioners appropriate access to training and support should be a key consideration in the development of new services. The competencies associated with these roles have been outlined by the Royal College of General Practitioners in their overview of competencies for the role of GP with a special interest in dementia. 18
Commissioners should also be cognizant of barriers to engagement with diagnostic and postdiagnostic services. Koch and Iliffe 29 broadly summarize the categories barriers can fall into: patient/societal factors (eg, stigma, consciously or unconsciously delayed presentation), GP factors (eg, diagnostic uncertainty, insufficient knowledge or experience), system factors (eg, time constraints and lack of support for practitioners). These issues are reflected on in several of the papers discussed, including evaluations by Dodd et al 26 and Minghella, 24 suggesting that these should be of central focus when developing or altering current service provision. Researchers should engage to further understand the factors presenting in these categories and how we can alter service provision to address these.
Gold standard evaluative criteria such as the MSNAP criteria were rarely referred to in the papers discussed, particularly regarding how they should be implemented in primary care. Dodd et al 26 discuss the importance of gaining informed consent during the process of assessment and diagnosis, and note that this is one of the good practice measures that is absent in primary care due to the more informal working practices in these settings. This is therefore an issue that requires closer consideration if assessment and diagnosis increasingly fall within the remit of primary care. Commissioners should clearly consider quality assurance for new primary care–based MAS and the standards most applicable to benchmarking the performance of these services.
Issues relating to the provision of postdiagnostic support emerged in several of the articles included in this review. Postdiagnostic support is now receiving an increasing amount of attention, as illustrated by the recent Department of Health policy paper (Joint declaration on postdiagnostic dementia care and support). 1 NICE guidelines 13 indicate that everyone diagnosed with dementia should have access to postdiagnostic support. Awareness and willingness to link more effectively with postdiagnostic support services was expressed in several of the papers discussed, with clear expressions of interest from both service providers and service users to improve access to support.24,26 Signposting to support and advice could be more clearly communicated. Dodd and colleagues 26 reported that while support services such as Memory Cafes were available in the Bristol area, service users tended to lack awareness of those, and those who were aware cited stigma as a barrier to making use of them, which links to issues mentioned earlier in the discussion.
Services with strong research links are more likely to have links to or provide support. 24 Many people referred to some of the services mentioned were part of ongoing research projects and so had contact with the service beyond their diagnosis, for example related to support for Advance Care Planning. Minghella 24 reported that patients using these services were keen to be involved in research and found participation valuable. This suggests opportunities for research organizations to develop mutually beneficial links with assessment and diagnosis services, which is also a mechanism through which ongoing support can be provided to people diagnosed with dementia. Patient involvement in research is important and links back neatly to the person-centered principles that should be underpinning our approach to dementia care.
A related issue raised was that improving early identification will increase numbers of people with a diagnosis before they reach crises point (with associated requirements for more complex support) and people with mild cognitive impairment. Minghella 24 reported that people with an early diagnosis really valued information and ongoing support, but that there was a lack of provision and resulted in rereferrals of people who had been given an early diagnosis and whose needs had changed as their condition progressed. This pattern was also noted among people who had originally been diagnosed with mild cognitive impairment and had subsequently converted to dementia. Ideally, postdiagnostic support, should be part of an integrated and clearly signposted system of pre- and postdiagnostic processes. Dodd et al 26 note that a well-structured postdiagnostic pathway is crucial in aiding people to adjust to a diagnosis of dementia, not least for those individuals given an early diagnosis. Therefore, the issues highlighted by Minghella 24 suggest that it may be useful to incorporate mechanism(s) to prevent people with early stage dementia and MCI from feeling unsure as to how to access support as/if their symptoms progress.
Conclusion
This review demonstrates that there is considerable effort being put into addressing the need to improve dementia assessment, diagnosis, and subsequent support. Innovative approaches are being implemented and evaluated to address this, and this should be encouraged, as should the improved access and signposting to postdiagnostic support.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This rapid review was funded by the Department of Health as part of wider evaluation project concerning dementia assessment in primary care.
