Abstract
The purpose of this study is to examine how organizational culture and job satisfaction affect clinician turnover in primary care pediatric practices. One hundred thirty clinicians from 36 primary care pediatric practices completed the Primary Care Organizational Questionnaire (PCOQ), which evaluates interactions among members of the practice and job-related attributes measuring 8 organizational factors, along with a separate 3-item instrument measuring job satisfaction. Random effects logistic models were used to assess the associations between job satisfaction, the organizational factors from the PCOQ, and clinician turnover over the subsequent year. All 8 measured organizational factors from the PCOQ, particularly perceived effectiveness, were associated with job satisfaction. Five of the 8 organizational factors were also associated with clinician turnover. The effects of the organizational factors on turnover were substantially reduced in a model that included job satisfaction; only 1 organizational factor, communication between clinicians and nonclinicians, remained significant (P = .05). This suggests that organizational culture affects subsequent clinician turnover primarily through its effect on job satisfaction. Organizational culture, in particular perceived effectiveness and communication, affects job satisfaction, which in turn affects clinician turnover in primary care pediatric practices. Strategies to improve job satisfaction through changes in organizational culture could potentially reduce clinician turnover.
Turnover, or separation from employment, is a major concern for providers of medical care. 1 Clinician turnover jeopardizes continuity of patient care, compromises quality of care and patient satisfaction,2-6 and has major fiscal implications. 7 Job dissatisfaction is a major reason why clinicians and other medical personnel leave a practice.1,8
Job satisfaction and turnover among primary care clinicians, and their interaction, cannot be fully understood without examining organizational culture 9 defined as “a set of basic tacit assumptions about how the world is and ought to be that is shared by a set of people and determines their perceptions, thoughts and feeling and to some degree their behavior.” 10 Organizational culture is thought to be responsible for 40%-50% of a clinician’s performance. 11 Elements of organizational culture include such attributes as openness, collaboration, teamwork, learning from mistakes, leadership, communication, coordination and problem solving/conflict resolution; and they are measurable. These characteristics could affect clinician job satisfaction and turnover. Organizational characteristics could also affect turnover independent of job satisfaction rather than directly through their effect on job satisfaction. Understanding important organizational factors associated with clinician turnover could lead to effective interventions to reduce clinician turnover.
In this study, we examined the relationships among clinician turnover, job satisfaction, and organizational culture as measured by perceived effectiveness, teamwork, leadership, communication, and conflict resolution. We hypothesized that job satisfaction directly affects clinician turnover and that organizational culture contributes to job satisfaction and clinician turnover both directly and indirectly, i.e., that job satisfaction mediates the association between organizational culture and turnover. The study was approved by the Institutional Review Boards of the University of Connecticut Health Center and Connecticut Children’s Medical Center.
Methods
Study Population
Clinicians from 36 primary care pediatric practices in Connecticut who were being recruited to participate in a randomized, controlled study of interventions designed to improve adherence to an asthma disease management program completed the Primary Care Organizational Questionnaire (PCOQ) 12 at study entry. Clinicians included physicians, Advanced Practice Registered Nurses (APRNs), Pediatric Nurse Practitioners (PNPs), and Physician Assistants (PAs).
Instruments
The PCOQ is a 56-item 5-point Likert scale survey that evaluates organizational culture by examining the interactions among members of a practice and job-related attributes. Many of the items were taken from a longer survey developed by Shortell et al that has been used to study the organizational attributes of intensive care units, 13 or from another instrument from Karasek et al.12,14 Eight organizational factors among the 56 items were empirically identified: Conflict Resolution (how disagreements were managed between clinicians), Perceived Effectiveness (of the practice in meeting patient and family needs), Communication between Clinicians and Staff, Communication among Clinicians, Physician Leadership, Decision Authority, Communication Timeliness, and Psychological Job Demands. 12 In addition, respondents completed a separate 3-question instrument to determine their satisfaction in their current job. Previous analysis 12 showed substantially more across-practice variability for the factors than variability across clinicians within practices, showing that they effectively measure practice-specific characteristics rather than simply individual perceptions. Questions for both instruments are included in the Appendix. One year after participants completed these questionnaires we documented those who left the practice.
Analytic Approach
Based upon previous studies,7,8,12,15-17 we hypothesized that job satisfaction would directly predict turnover and that organizational factors from the PCOQ, as measured by individual clinicians’ responses, would directly predict job satisfaction. We further hypothesized that organizational factors affected turnover at least partially through their effect on job satisfaction. Although the distribution of the organizational factor scores might make it possible for the factors to mediate each other, we had a strong a priori reason to examine job satisfaction as the mediator because it has already been shown to affect nursing turnover 8 and because we believe that organizational factors are more likely to be the targets of successful intervention.
Linear mixed models with a random intercept were used to examine the association of job satisfaction with each of the 8 PCOQ organizational factors. 12 Logit-normal generalized linear mixed models with a random intercept were used to examine whether job satisfaction or any of the 8 organizational factors predicted turnover, defined by whether the clinician was still working in the same practice after 12 months. Finally, job satisfaction was added as a predictor to each model for the 8 organizational factors to evaluate it as a possible mediator. Clinician demographics, the practice staff (defined as nurses, office managers, receptionists, and billing personnel) to clinician ratio in each practice, and whether the practice was located in an urban area (defined as an area where at least 20% of households had incomes below the federal poverty level with a population density of greater than 1000 per square mile, and serving primarily low income Medicaid children) or a privately owned practice located in a nonurban community, were included as potential confounders in all models. The STATA procedures xtreg and xtlogit were used for the primary statistical analyses. (Stata Corporation, College Station, TX, USA, http://www.stata.com.)
Results
Thirty-six practices agreed to participate (of 46 invited). Thirteen of the 36 practices were located in urban areas, serving largely a low-income, Medicaid population, and were either hospital based or a federally qualified health center (urban clinic). Remaining practices were located in nonurban areas, served largely a commercially insured population (71% versus 22% for urban clinics, P < .0001) and had fewer nonphysician clinicians (20% versus 63%; P = .01). There were no differences in practice size or patient demographics in the nonparticipating practices compared with the participating practices. All physicians, nurse practitioners, and physician assistants working in the practices at the time of the study’s commencement were eligible; 139 of 149 (93%) agreed to participate, and 130 of 139 (94%) who completed the PCOQ and responded to the job satisfaction instrument were included in the analysis. The 19 clinicians not included in the analyses did not differ from those included in terms of level of training, full-time status, years since completion of training, or gender. The 3-question job satisfaction instrument proved highly reliable in this cohort of clinicians (Cronbach alpha 0.94). Table 1 shows demographics of the participating clinicians by level of training. Physicians had more experience than the nonphysician clinicians (21 versus 12 years, Mann-Whitney P < .0001).
Study Demographics


data expressed as frequency (% of nonmissing responses) or mean ± standard deviation (range)
For continuous measures, P values are from Mann-Whitney nonparametric tests and for categorical measures from Pearson chi-squared tests.
Of the 130 clinicians, 12.3% (9 physicians and 7 nonphysicians) left their practice during the 12-month follow-up period. Urban clinics had more turnover than private practices (12/62 = 19% versus 4/68 = 6%; P = .030, Fisher’s exact test). There was no difference in turnover rates between physicians (18%) and nonphysician clinicians (21%) in urban clinics. However, in private practices, more nonphysician clinicians (3/17 = 18%) left than physicians (1/51 = 2%; P = .046, Fisher’s exact test), which most likely reflects the fact that some of the physicians held equity interest in the private practices.
Physicians reported greater job satisfaction than nonphysician clinicians (4.33 versus 3.88, Mann-Whitney P = .008). Nonphysician clinicians described their practices as having less timely communication (3.66 versus 3.89; P = .027) and providing less authority to make decisions (Decision Authority 3.96 versus 4.22; P = .044) compared with physicians. For all factors, private practices had greater job satisfaction, better communication and decision authority as evidenced by higher mean values than the urban clinics (all P < .01), indicating that the clinicians in the private practices on average had a more favorable perception of their organization’s culture. The organizational factors were all positively correlated with each other, with Pearson correlations ranging from 0.20 to 0.68, indicating that a clinician who has a more favorable perception of 1 aspect of organizational culture is likely to have more favorable perceptions of other aspects. All 8 organizational factors showed considerable stability (intraclass correlation ≥0.86) over 18 months of follow-up in the clinicians who completed the survey at both time points.
All 8 factors of the PCOQ were associated with job satisfaction (P < .001 for each) (Table 2) in the univariate models controlling for clinician type, staff to clinician ratio, and practice type. Of the 8 organizational factors, Perceived Effectiveness (at meeting patient and family needs) was most strongly associated with job satisfaction; using the same scale, each 1 unit difference in Perceived Effectiveness was associated with an 0.91 unit difference in job satisfaction.
Descriptive Statistics for the PCOQ Factors, and the Results of the Linear Mixed Models for the Association Between Each PCOQ Factor and Job Satisfaction


The T1 → T2 ICC is the intraclass correlation from the baseline and 18 month follow-up administrations of the organizational culture survey. The Estimate gives the expected difference in job satisfaction for a unit difference in the value of the PCOQ factor. For example, a 1 unit difference in leadership is associated in a difference in job satisfaction of 0.723 units. The mean job satisfaction was 4.169, with as standard deviation of 0.960, in scores for job satisfaction that ranged between 1 and 5.
Five of the 8 organizational factors—Leadership, Perceived Effectiveness, Communication between Clinicians and Non-Clinicians, Communication Timeliness, and Conflict Resolution—predicted turnover over the 12-month follow-up period in the univariate models (Table 3, left) that controlled for clinician type, staff to clinician ratio, and practice type. Higher values for each factor, eg, more effective leadership, more timely communication, etc., were associated with lower rates of clinician turnover during the follow-up period as indicated by the odds ratios of less than 1. Perceived effectiveness was the strongest predictor of turnover, just as it was for job satisfaction; there was a 79% reduction in the odds of a physician leaving his/her practice for each 1-unit increase in perceived effectiveness. As expected, job satisfaction also was a strong predictor of turnover.
Results of Logit-Normal Models Examining the Association Between the PCOQ Factors and Job Satisfaction, With Clinician Turnover Measured Over the 1-Year Follow-up Period
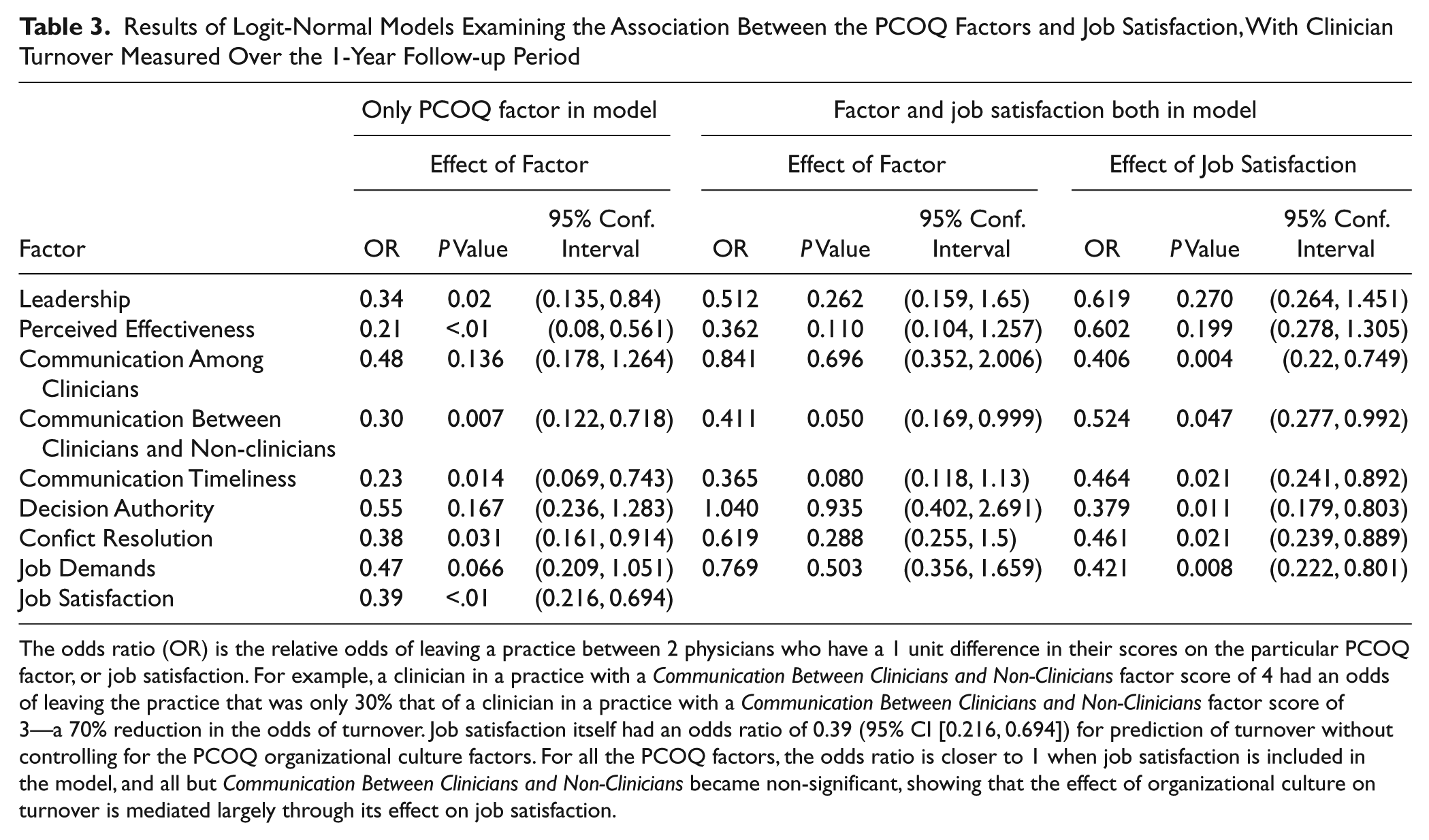

The odds ratio (OR) is the relative odds of leaving a practice between 2 physicians who have a 1 unit difference in their scores on the particular PCOQ factor, or job satisfaction. For example, a clinician in a practice with a Communication Between Clinicians and Non-Clinicians factor score of 4 had an odds of leaving the practice that was only 30% that of a clinician in a practice with a Communication Between Clinicians and Non-Clinicians factor score of 3—a 70% reduction in the odds of turnover. Job satisfaction itself had an odds ratio of 0.39 (95% CI [0.216, 0.694]) for prediction of turnover without controlling for the PCOQ organizational culture factors. For all the PCOQ factors, the odds ratio is closer to 1 when job satisfaction is included in the model, and all but Communication Between Clinicians and Non-Clinicians became non-significant, showing that the effect of organizational culture on turnover is mediated largely through its effect on job satisfaction.
We then fit 8 multivariate models that each included both job satisfaction and 1 organizational factor from the PCOQ, along with the same confounders as before to determine whether organizational characteristics were associated with clinician turnover over and above the mediating action of job satisfaction (Table 3, right). In these models, communication between clinicians and staff was the only organizational factor that remained significant (P = .050) and all odds ratios for the organizational culture factors were closer to 1, indicating that the 8 organizational factors measured by the PCOQ affect turnover primarily through their effect on job satisfaction. In the model that included perceived effectiveness and job satisfaction, and also leadership and job satisfaction, neither remained a significant predictor, probably because each these 2 organizational factors were the most strongly associated with job satisfaction.
Discussion
Turnover is a significant problem for many organizations, including medical practices. Turnover is associated with lost productivity, lost wages, organizational disruption, and additional costs associated with recruiting and training new clinicians. This study confirms previous reports that high turnover is associated with lower levels of job satisfaction, and shows that job satisfaction in turn is associated with 8 factors associated with organizational culture. Five organizational factors (Leadership, Perceived Effectiveness, Communication Between Clinicians and Staff, Decision Authority, and Job Demands) predicted clinician turnover when measured prospectively over a 1-year follow-up period; only Communication Between Clinicians and Staff was a significant predictor of turnover over and above the effect of job satisfaction. Although the literature on job satisfaction and turnover is substantial, typically it has not examined organizational factors, and this report of a 1-year follow-up provides unique insights into job satisfaction and turnover in primary care pediatric practices. We observed higher turnover rates in urban clinics; possible reasons might include the greater clinical and administrative burdens faced by clinicians serving urban patients, patient issues complicated by language, culture, low health literacy and low socioeconomic status, 15 and the challenge of maintaining stable funding.16,18 These conditions might influence a clinician’s perception of his or her clinical effectiveness, and that in turn, is a salient factor associated with satisfaction and ultimately turnover.
A limitation of this study is that we were not able to distinguish between voluntary and involuntary turnover, which might reflect different practice characteristics. However, many of the organizational consequences of turnover would be present regardless of the reasons that clinicians leave practices. Another limitation is that the practices were all drawn from 1 geographic region (central Connecticut) and it is possible that participating practices do not represent urban and suburban primary care pediatric practices elsewhere in the United States. While this would affect generalizability, we are unaware of any reason why there would be such differences.
Because different methods have been used to assess turnover rates in the literature, it is difficult to directly compare our rates with those reported elsewhere. 19 Further research is needed to examine whether interventions designed to change organizational culture improve job satisfaction prospectively; an intervention study in which attempts are made to modify organizational culture and clinician job satisfaction could confirm the conclusions observed here, and we are continuing follow-up of clinician turnover in these practices as part of a randomized intervention study to improve adherence to an asthma disease management program. There are many other factors such as practice location, practice size, salary, call schedule, and added benefits that could contribute to job satisfaction and turnover but were beyond the scope of this study, which was limited to aspects of organizational culture that we believed to be possible intervention targets.
Most individuals in the United States today receive their medical care in primary care practices, which offer great benefit to the health care system.19-21 Yet, primary care practices are facing challenging times; changes in the health care system and in reimbursement have resulted in primary care physicians expressing dissatisfaction on long work hours, high stress, and erosion of scope of practice. 19 Strategies implemented at the organizational level to decrease primary provider turnover potentially offer the opportunity to improve overall quality of patient care. This research identifies several factors that should be considered as potential targets of such interventions.
Footnotes
Appendix
Factors from the Primary Care Organizational Questionnaire (PCOQ)

| COMMUNICATION AMONG CLINICIANS |
| Likert Scale from 1 (Strongly Disagree) – 5 (Strongly Agree) |
|
It is easy for me to talk openly with the clinicians in this clinic/practice. Communication between the clinicians in this clinic/practice is very open. I find it enjoyable to talk with other clinicians in this clinic/practice. When clinicians talk with each other in this clinic/practice, there is a good deal of understanding It is easy to ask advice from other clinicians in this clinic/practice. |
| COMMUNICATION BETWEEN CLINICIANS AND STAFF |
| Likert Scale from 1 (Strongly Disagree) – 5 (Strongly Agree) |
|
It is easy for me to talk openly with the staff in this clinic/practice. Communication between clinicians and staff in this clinic/practice is very open. I find it enjoyable to talk with the staff in this clinic/practice. When the staff talk with the clinicians in this clinic/practice, there is a good deal of understanding It is easy to ask advice from the staff in this clinic/practice. |
| COMMUNICATION TIMELINESS |
| Likert Scale from 1 (Strongly Disagree) – 5 (Strongly Agree) |
|
I get information on the status of patients when I need it. When a patient’s status changes, I get relevant information quickly. There are needless delays in relaying information regarding patient care. In matters pertaining to patient care, staff notify clinicians in a timely manner. |
| PERCEIVED EFFECTIVENESS |
| Likert Scale from 1 (Strongly Disagree) – 5 (Strongly Agree) |
|
Our clinic/practice almost always meets its patient care treatment goals. Our clinic/practice does a good job of meeting family member needs. Our clinic/practice does a good job of applying the most recently available technology to patient care needs. We are able to recruit the best clinic/practice staff. We do a good job of retaining clinic/practice staff in the clinic/practice Overall, our clinic/practice functions very well together as a team. Our clinic/practice is very good at responding to emergency situations. |
| LEADERSHIP |
| Likert Scale from 1 (Strongly Disagree) – 5 (Strongly Agree) |
|
Physician leadership in this clinic/practice emphasizes standards of excellence to the clinic/practice members. Physician leadership is sufficiently sensitive to the different needs of clinic/practice members. Physician leadership fails to make clear what they expect from clinic/practice members. Physician leadership discourages other clinicians from taking initiative Physician leadership often makes decisions without input from the other clinicians in the clinic/practice. Physician leadership effectively adapts its problem-solving style to changing circumstances. |
| CONFLICT RESOLUTION |
| Likert Scale from 1 (Not At All Likely) – 5 (Almost Certain) |
|
All points of view will be carefully considered in arriving at the best solution of the problem. All the clinicians will work hard to arrive at the best possible solution. The clinicians involved will not settle the dispute until all are satisfied with the decision. Everyone contributes from their experience and expertise to produce a high quality solution All points of view will be carefully considered in arriving at the best solution of the problem. The staff and clinicians will work hard to arrive at the best possible solution. Both parties involved will not settle the dispute until all are satisfied with the decision. Everyone contributes from their experience and expertise to produce a high quality solution. |
| DECISION AUTHORITY |
| Likert Scale from 1 (Never) – 5 (Always) |
| In general, how often… |
|
Do you have a lot of say about what happens on your job? Do you have freedom to decide how you do your work? Does your job allow you to make a lot of decisions on your own? |
| PSYCHOLOGICAL JOB DEMANDS |
| Likert Scale from 1 (Never) – 5 (Always) |
| In general, how often… |
|
Are you asked to do an excessive amount of work? Are you given enough time to get the job done? |
| Job Satisfaction Instrument |
| Likert Scale from 1 (No, Definitely Not) – 5 (Yes, Definitely) |
| Please circle the number, which best represents your opinion. |
|
Would you recommend this organization to someone who is seeking a job? Do you consider your organization a desired place for employment? Likert Scale from 1 (Very Dissatisfied) – 5 (Very Satisfied) Overall, how satisfied are you with your job? |
Acknowledgements
We thank Dr Michelle M. Cloutier, principal investigator for the study, for her many intellectual contributions to this work and for her enthusiastic support. We also thank the providers and office staff of the 36 primary care practices and clinics in Connecticut for their willingness to participate in this project: Burgdorf Health Center; Central Pediatrics and Adolescent Medicine; Charter Oak Health Center at Connecticut Children’s Medical Center; Charter Oak Family Health Center; Child and Adolescent Health Care, Waterbury; Community Health Clinic, New Britain; Community Health Services, Hartford; John J. Fote, MD, John H. Lavalette, MD, Jennifer L. Schwab, MD, and Jennifer L. Nichols, APRN; Kids Station Pediatrics; Sobhy Ghabrial, MD; Grove Hill Medical Center; Healthwise Medical Associates, LLP: Naseem Deen, MD, Vernon Pediatrics; Pedicorp, PC; New Britain General Hospital Department of Pediatrics; Pediatric Associates of Marlborough; Pediatric and Medical Associates, Cheshire and New Haven; Personal Care Pediatrics; Prohealth Physicians Mso Inc; Children’s Medical Group; Sherry Banack, MD and Candra Smith-Slatas, MD, PhD; Vandana Sacheti, MD; Mark Peterson, MD; Michael Rokosky, MD; St. Francis Hospital; St. Mary’s Hospital; Hospital of St. Raphael; Kweku Sam, MD; Shoreline Pediatrics and Adolescent Medicine, PC; Teresa Szajda, MD; Robert R. Toscano, MD, Leslie S. Dick, MD, Eric Cohen, MD and Janna Zempsky, APRN; UCONN Health Partners; and Yale University Health Services. None of the participating practices had a role in the analyses of the data or in the preparation of the manuscript.
The author(s) declared no potential conflicts of interests with respect to the authorship and/or publication of this article.
This research supported by National Heart, Lung, and Blood Institute (NHLBI) Grant # RO1 HL70785-01 (The Provider and Organization in Asthma Guidelines, PI: Michelle M. Cloutier, MD). The sponsor had no role in the design of the study, the analyses of the data, or the preparation of the manuscript.
The authors have no financial conflicts of interests to report.
