Abstract
Transient global amnesia (TGA) is a condition characterized by a sudden, temporary lapse in memory without focal neurological deficits, usually in middle aged adults, sometimes precipitated by an inciting event. We describe a case of a young patient, who presented with a constellation of symptoms consistent with TGA post-concussion with a right temporal lobe hypodensity on CT head. This patient’s memory returned to baseline within 24 hours, with only a mild residual headache which resolved within the next day and no MRI findings 48 hours after, illustrating that his clinical trajectory favours TGA rather than post-concussive amnesia. While the pathophysiology of TGA is still a mystery, clinicians and researchers continue to hypothesize the anatomical basis of this condition.
Transient global amnesia (TGA) is characterized by sudden temporary loss of memory accompanied by repetitive questioning without focal neurologic deficits, often in middle aged adults. While risk factors, including age above 50 and migraines, are known, TGA’s pathogenesis remains to be understood. We examine a case of TGA in temporal relationship to concussion.
A healthy 38-year-old male with a past medical history of only hypothyroidism and no known history of migraines or prior concussions was admitted to our hospital after falling and hitting the back of his head on cement. He presented with retrograde amnesia for events one hour prior to his injury with subsequent anterograde amnesia, which resolved within 16 hours. He had repetitive questioning with intact language and no focal neurological deficits. Initial non-contrast head CT in the acute setting while symptomatic is shown in Figure 1, demonstrating a right anterior temporal lobe hypodensity suspicious for an area of contusion or edema. An MRI brain was completed 48 hours later and did not show any T2/FLAIR hyperintensity in the region, nor any change on diffusion-weighted or susceptibility weighted imaging, as shown in Figure 2. Approximately 24 hours after his injury, eight hours after his episode of TGA resolved, he developed a unilateral pulsatile headache that was associated with light/sound sensitivity, nausea, and tinnitus, which also resolved within a day. He was asymptomatic thereafter, including at six-month follow up. Despite his young age, this patient’s constellation of symptoms, lack of focal neurological deficits, and overall clinical trajectory meet criteria for TGA.
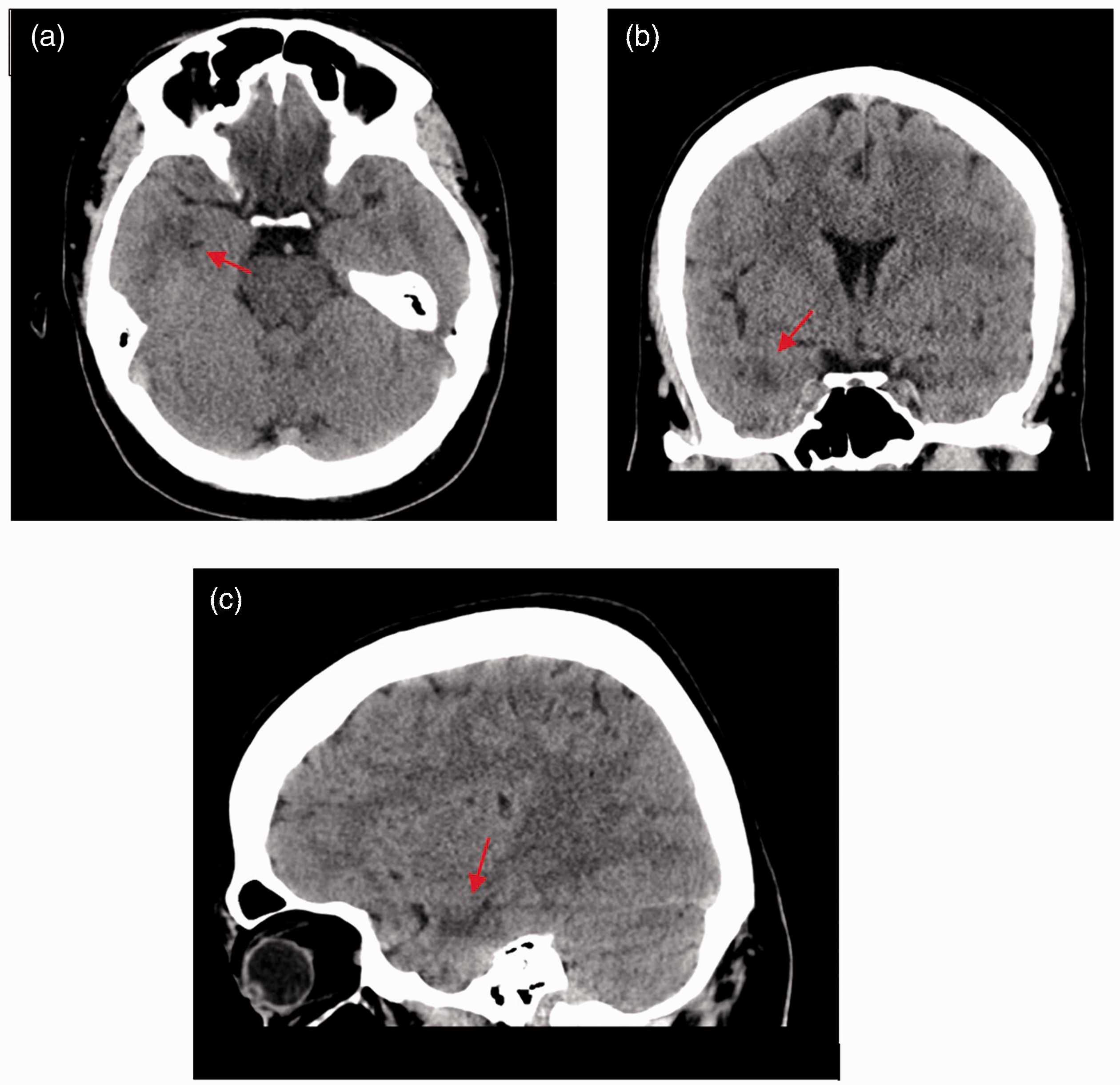
Non contrast CT head (a) axial cut, (b) coronal cut, and (c) sagittal cut, illustrating right temporal lobe hypodensity possibly in keeping with edema or contusion. This could be a result of the patient’s fall or a transient TGA-related phenomenon.
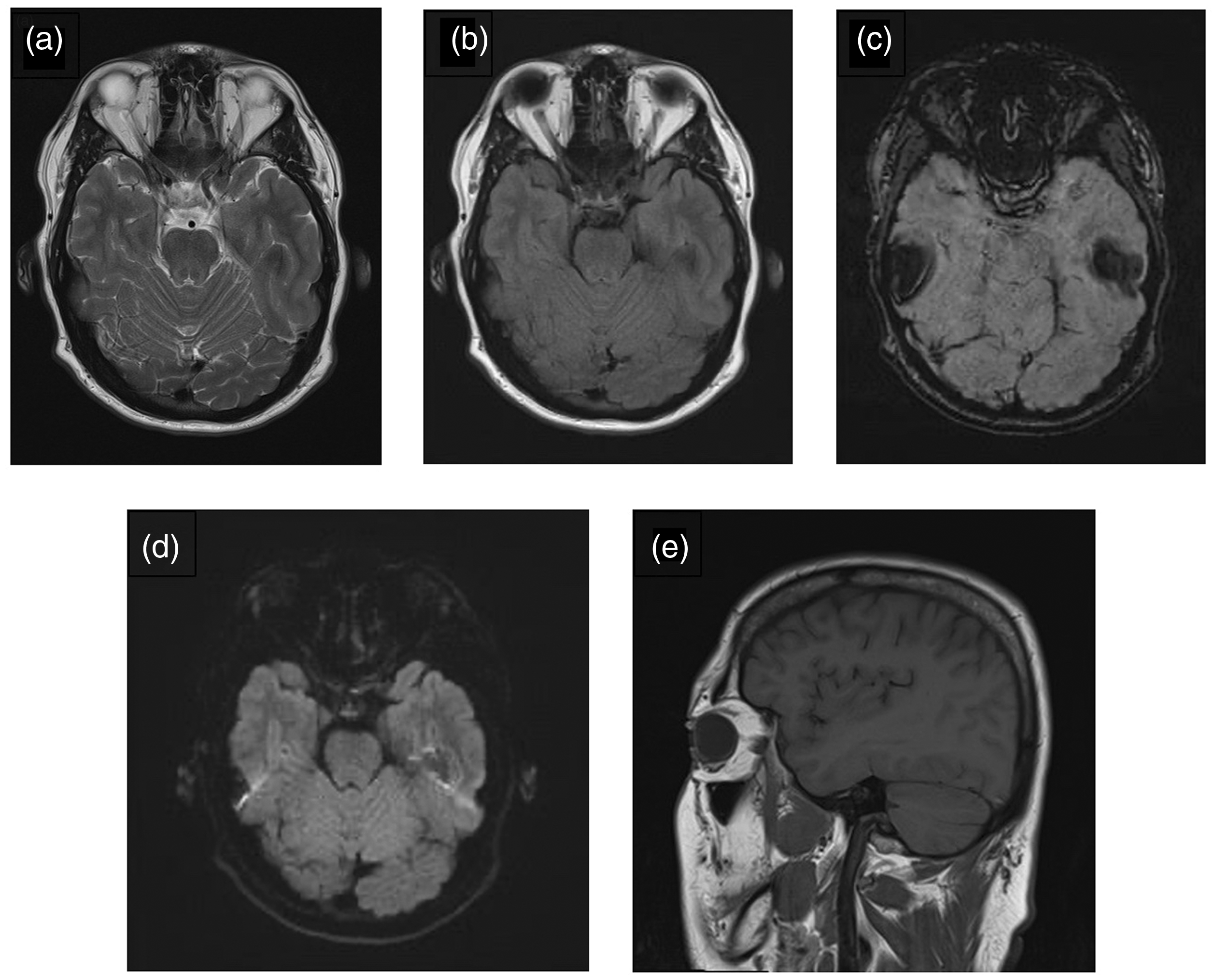
Normal non-enhanced MRI brain (a) axial T2, (b) axial FLAIR, (c) SWI, (d) DWI, and (e) sagittal T1 performed 48 hours after symptom onset.
TGA has been a neurological enigma since its original description in 1956. Over the years, diagnostic criteria have been refined but no specific discernable pathophysiology has been confirmed, although multiple hypotheses exist. TGA’s resemblance to migraine, transient ischemic attack, and seizures has been explored, with the most recent etiological hypothesis involving venous congestion and possible hypoperfusion of the hippocampus and associated structures – key elements of the Papez circuit, which provides a neuroanatomical correlate to amnesia, the hallmark of TGA.1,2 There have also been literature reports of associated neuroradiological findings with transient hippocampal diffusion restriction seen on MRI. A similar clinical-radiological correlate was seen in this case of a young patient who experienced classic TGA symptoms post-concussion.
In our case, the patient experienced abrupt onset repetitive questioning and amnesia (both anterograde and retrograde) resolving within 24 hours, which is typical for TGA. Thereafter, he experienced a headache, which can also be seen in TGA. One atypical feature of this case is the patient’s young age, with TGA usually affecting individuals greater than 50 years old. TGA has been reported in younger patients in the literature, although with much lower incidence.3,4 In addition, there was a precipitating event, with our patient having struck his head. While post-traumatic amnesia is also on the differential, it is important to emphasize that TGA can have a precipitating event such as a physical/emotional trigger. Nonetheless, mild trauma with significant transient amnesia disproportionate to other post concussive symptoms with complete resolution within 24 hours is more in keeping with the clinical trajectory of TGA rather than post-concussive amnesia.
There have been multiple hypotheses regarding TGA triggers with one consideration being that a precipitating event associated with Valsalva maneuver transiently increases intrathoracic pressure and prevents venous return from the superior vena cava. This results in retrograde jugular venous flow secondary to an incompetent jugular valve with subsequent temporal lobe hypertension. 1 Another theory is that the stressful precipitating event is associated with hyperventilation and subsequent hypoxic cerebral vasoconstriction leading to cerebral hypoperfusion, which disproportionately affects CA1 neurons in the hippocampus. These neurons are particularly susceptible to ischemic insult and play an important role in polysynaptic intrahippocampal circuits and memory consolidation in the Papez circuit.1,3 Nonetheless, there remain many questions about these theories, including why TGA is not always associated with a precipitating event and why many patients with an incompetent jugular valve never develop TGA, suggesting that these are not straightforward causal relationships.
Either of the theories described above could be compatible with the imaging findings that were seen in this case. While the right temporal lobe hypodensity could represent contusion or edema secondary to a minor concussion, it might also represent transient findings in the context of TGA. Some reports in the literature document no imaging changes on CT and MRI of the brain, even when performed early.1,4 Unilateral and bilateral temporal lobe abnormalities have also been documented in TGA, primarily by way of unilateral or bilateral transient parahippocampal diffusion restriction. In addition to this being an unusual area for isolated infarction, the transient nature of these changes reinforces that they do not represent a complete infarct but may support the hypothesis that there is a transient ischemic insult in TGA. 1 MRI brain in our patient done 48 hours after the event was unremarkable. While CT head hypodensity can be seen in the setting of non-hemorrhagic brain contusion, particularly in the inferior temporal region given it abuts the petrous ridge, it often represents edema and takes time to develop and resolve. 5 Hence, the timeline of our patient’s rapidly reversible temporal hypodensity, which was visualized immediately after his injury on CT head and resolved on his 48-hour MRI scan, would be atypical for contusion.
Although often anxiety provoking, TGA is a self-limiting condition characterized by an acute, short lived episode of amnesia and repetitive questioning with return to baseline within 24 hours with no focal neurologic deficits. Recurrence has been reported to be quite variable, with some sources quoting 8–18% over approximately six years. 1 Our patient did well after his isolated event with complete symptom resolution. His precipitating fall and reversible unilateral temporal lobe hypodensity seen on CT head reinforce the anatomical basis of this mysterious neurological condition and add to the body of literature speculating on its possible pathogenesis.
Footnotes
Authors’ contribution
B Shah and MW Hussain contributed to article concept, writing, and review. S Poonja contributed to article writing, review, and submission.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
