Abstract
Objectives
To retrospectively review data of concussed and non-concussed elite cricket athletes following head impact to describe which clinical features on the day of injury are associated with concussion diagnosis. A secondary aim was to describe the recovery time of concussed athletes.
Design
Retrospective cohort study.
Methods
This study reviewed five seasons of Sport Concussion Assessment Tool (SCAT) data and clinical records for elite male and female cricket athletes who sustained a head impact during a cricket match or training.
Results
Data from 30 concussed and 37 non-concussed athletes were compared. Symptoms of ‘don’t feel right’ and ‘feeling slowed down’ had the strongest clinical utility for a concussion diagnosis post head impact. Concussed athletes reported a significantly lower ‘percent of normal’ (median 60%, IQR 60–90%) compared to athletes who sustained a non-concussive head impact (median 99%, IQR 95–100%, p = 0.003). No other component of the SCAT distinguished concussed from non-concussed athletes on day of injury. Concussed athletes typically experienced symptom resolution within 2–8 days and completed a graded return to play protocol within 4–14 days. No differences in SCAT findings or recovery times were observed between genders.
Conclusion
The SCAT may be used as a clinical tool to assist in diagnosis of concussionin elite cricket athletes. The components of the SCAT with the greatest clinical utility on day of injury were athlete-reported symptoms and ‘percent of normal’. Concussed cricket athletes typically complete their graded return to play protocol within 14 days however individualised management is paramount.
Practical implications
Athlete reported symptoms particularly ‘don’t feel right’ and ‘feeling slowed down’ and lower ‘percent of normal’ may be indicative of concussion in cricket athletes.
Performance on the objective SCAT domains of orientation, concentration, balance and neurological screening was not necessarily impaired in concussed cricket athletes.
Concussed cricket athletes typically experience symptom resolution in eight days and complete a graded return to play protocol within 4–14 days.
Introduction
Sports-related concussion has emerged as an important area of injury research and is a significant cause of athlete morbidity. Concussion is defined as a mild traumatic brain injury evoked by biomechanical forces resulting in complex pathophysiological process affecting the brain. 1 Concussion impairs function in many domains including vestibular-ocular function, sleep and emotional regulation as well as impacting the athletes ability to complete cognitive and motor tasks. 2 Timely and accurate diagnosis is important to guide management including to establish whether an athlete requires removal from play or is safe to continue. This is imperative for athlete wellbeing and to ensure appropriate clinical management is undertaken.
Concussion diagnosis remains a clinical challenge. It is a spectrum of injury rather than an isolated diagnosis. The diagnosis of concussion requires assessment of multiple domains including symptomatology, cognition, concentration, neurological disturbance and balance. 2 Further challenging diagnosis is variation in clinical presentation and diagnostic guidelines across different sports, 3 hence sport-specific research is needed. The diagnosis of concussion generally relies on the clinical judgement of the diagnosing practitioner however objective tools have been developed to assist practitioners.
The Sport Concussion Assessment Tool (SCAT) is an evidenced-based standardised tool to assist medical practitioners assess a player with possible concussion. 4 The tool is designed to assess multiple domains including symptoms, orientation, memory, concentration and balance. The most recent addition, the SCAT5, was revised following a systematic review and collaboration between concussion experts at the 2017 Concussion in Sport Group meeting in Berlin.4,5 Modifications included increase from a 5 word recall to 10 word and a Rapid Neurological Screen to increase the utility of the assessment tool. 6 The SCAT5 can be used at the point of diagnosis as well as part of serial monitoring within the first 3–5 days. 5
Once a diagnosis of concussion is made, informed decision-making regarding athlete recovery and return to play (RTP) timeframes is vital knowledge for practitioners managing athletes, as well as the athlete themselves and coaching staff. This includes typical recovery time and potential indicators that an athlete may experience prolonged symptom resolution outside of the expected timeframe of 10–14 days. 5 A RTP prior to complete athlete recovery from concussion has the potential to result in persistent symptoms and can increase the risk of a second concussion injury. 7
In Australian elite level cricket, concussion is reported with an annual incidence of 0.9 concussions per 100 athletes, or 2.3 males and 2.0 females per 1000 player days.8,9 At present, there are limited studies on symptom resolution and recovery time, but a recent study suggested that elite cricketers generally RTP in a timely manner with 83% of players missing no more than one game. 9 There is currently limited research evaluating whether symptoms or other domains assessed by the SCAT are associated with concussion diagnosis or recovery time. Current literature is predominantly focused on male collision sports with less research performed on female athletes and non-contact sports.10–13
The aim of this study is to retrospectively review SCAT data from concussed and non-concussed elite cricket athletes following a head impact to describe which clinical features on the day of injury are associated with concussion diagnosis. A secondary aim is to describe the typical recovery time of concussed athletes including symptom resolution and RTP.
Methods
This research was approved by La Trobe University Human Ethics Committee (S17-195). Participants included Australian male and female cricket athletes playing at a national or international level who sustained a head impact during a cricket-specific activity (training or match) between July 2014 and February 2019.
Data was extracted from Cricket Australia’s Athlete Management System (Fair Play AMS Pty Ltd). Data included diagnosis, SCAT data follow up clinical records and training data. For comparison, data was also extracted for athletes who sustained a head impact in the 2018–2019 season and completed a SCAT as part of their routine clinical assessment yet were not subsequently diagnosed with concussion. The protocol for assessment of concussion are in accordance with the Berlin Consensus Statement on Concussion in Sport 5 and diagnosis was based upon practitioner review, review of video of head impact if available, neurocognitive testing using the Computerised Cognitive Assessment Tool for Sport (CogSport; Cogstate Ltd.), and SCAT. Assessments were administrated on the day of injury by the highest qualified medical practitioner (medical officer or physiotherapist familiar with the concussion assessment protocol). If a physiotherapist administered the test, it was discussed with a medical officer and diagnosis was later confirmed by a medical officer. As per internal concussion protocol, definite concussion diagnosed from signs and symptoms at the time of head impact did not require neurocognitive testing or SCAT on the day of injury. Neurocognitive testing is compared to an individual athlete’s baseline, however baseline SCAT is not routinely completed in this setting as the tests have an element of subjectivity to them, and players may be assessed by different medical practitioners in different training and match settings.
Recovery times were established from a combination of follow up neurocognitive and SCAT assessments, clinical records, and training data. The protocol for graded RTP is in accordance with the Berlin Consensus Statement on Concussion in Sport and tailored to incorporate sport-specific adjustments. 5 Prolonged recovery was defined as symptoms resolution greater than 10 days in accordance with the Berlin Consensus Statement. 5
Data was excluded from analysis if the athlete experienced a concomitant illness or injury at the time of injury which may have influenced clinical findings and RTP timeframes. Athletes who were playing for a non-Australian cricket team (e.g. playing domestic cricket overseas) at the time of injury were also excluded as they were not clinically managed using the same protocol.
SCAT and recovery time data were not normally distributed, hence descriptive statistics are reported as median and interquartile range (IQR). Median tests were used to compare results between concussed and non-concussed athletes, and male and female concussed athletes. Proportions were calculated with a Wilson 95% confidence interval (CI). The diagnostic value of symptoms were evaluated using 2 × 2 contingency tables to calculate sensitivity, specificity, positive predictive values (PPV), and negative predictive values (NPV) with Fisher’s exact p-values. Analysis was completed using Excel (Microsoft, 2016 MSO) and SPSS (version 25, IBM, Armonk, NY, USA) and significance set a-priori at p < 0.05.
Results
Sixty athletes were diagnosed with concussion over five seasons of national and international level cricket (male n = 43, mean age 24.1 ± 5.1 years; female n = 17, mean age 23.5 ± 4.0 years). Concussions were sustained during a match (n = 36), match warm-up (n = 2), or training (n = 22). All concussions were diagnosed on the day of injury, with the exception of three athletes diagnosed on one, two or five days after injury. Three athletes were excluded due to concomitant significant injury or illness that resulted in missed training and/or game time and impacted on their symptom resolution timeframe.
SCAT data on the day of injury was available for 30 of the 60 concussions (males n = 22, female n = 8). Findings are detailed in Table 1, with findings of non-concussed athletes presented for comparison (n = 37: male n = 31, female n = 6). Between the groups there was no difference in age (p = 0.260).
Comparison of SCAT domains between concussed and non-concussed athletes; male and female concussed athletes.
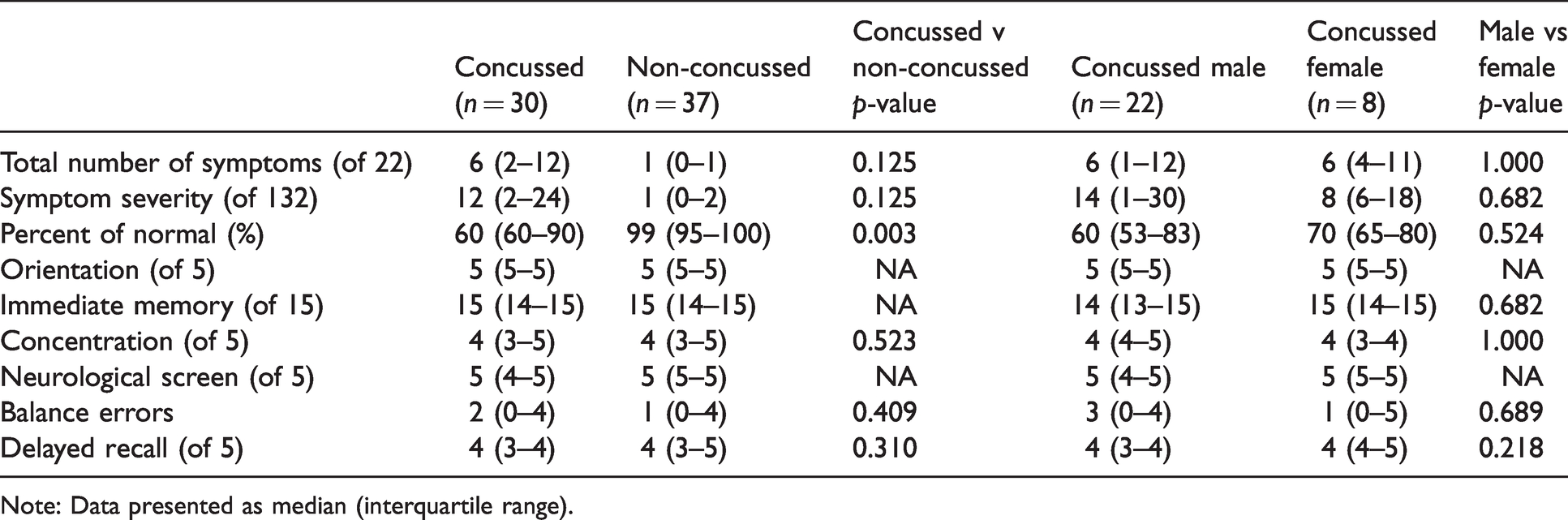
Note: Data presented as median (interquartile range).
The most commonly reported symptoms for concussed athletes were: headache (73%, 95% CI: 56–86%), ‘don’t feel right’ (67%, 49–81%), pressure in head (67%, 49–81%), ‘feeling slowed down’ (53%, 36–70%), fatigue or low energy (43%, 27–61%), neck pain (40%, 25–58%), difficulty concentrating (37%, 22–54%), drowsiness (37%, 22–54%), dizziness (33%, 19–51%), feeling like in a fog (33%, 19–51%), and nausea or vomiting (30%, 17–48%). Median rating for headache severity was 2 out of 6 (IQR 0–4), ‘don’t feel right’ 2 (0–3), pressure in head 1 (0–3) and ‘feeling slowed down’ 1 (0–2). The most commonly reported symptoms for non-concussed athletes were: headache (22%, 95% CI: 11–37%), pressure in head (22%, 95% CI: 11–37%) and fatigue or low energy (16%, 95% CI: 8–31%). The diagnostic value of each symptom is detailed in Table 2. All symptoms except for sadness, nervous or anxious, and trouble falling asleep were significantly related to concussion diagnosis.
Diagnostic value of symptoms reported on SCAT to distinguish between concussive and non-concussive head impacts.
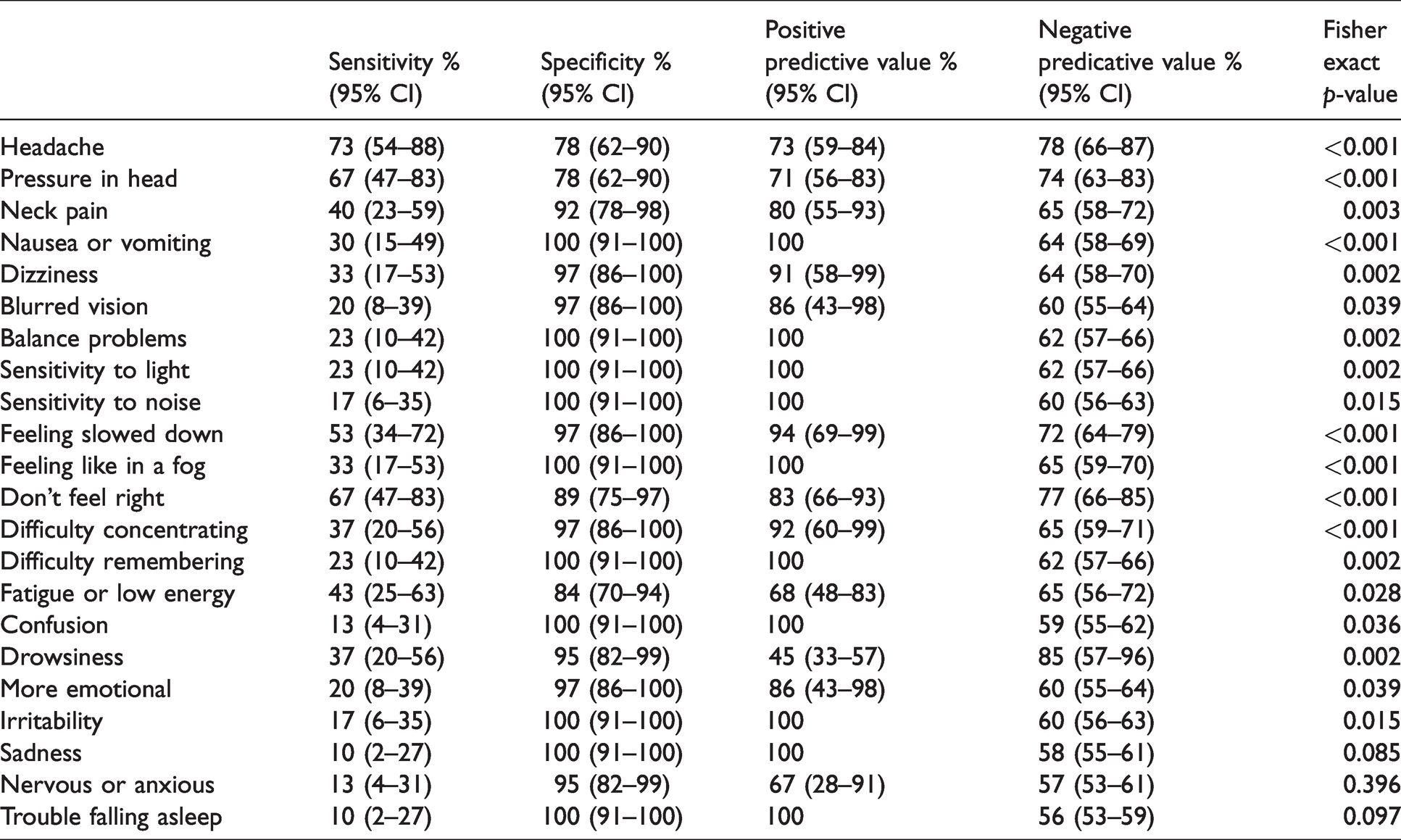
Recovery times are detailed in Table 3. Of the 51 athletes with known symptom resolution time, 42 (82%, 95% CI: 70–90%) had symptom resolution in less than or equal to 10 days. Nine athletes (male n = 7, female n = 2) had persistent symptoms more than 10 days. For these athletes, the median days to symptom resolution was 16 days (IQR 13–32) and the median time to complete a graded RTP protocol was 27 days (IQR: 16–46). There was no difference in recovery time between males and females. There was insufficient data to describe SCAT findings for athletes with prolonged recovery.
Days to recovery.
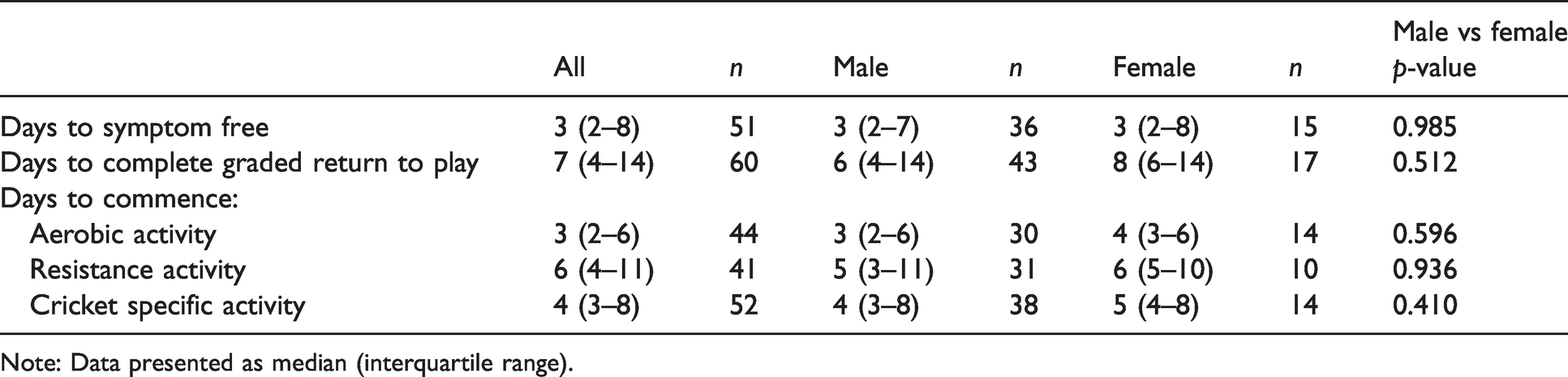
Note: Data presented as median (interquartile range).
Discussion
This retrospective analysis of SCAT findings in elite cricket athletes over five seasons aimed to describe key clinical features which may assist with concussion diagnosis. Reported symptoms were the clinical feature most strongly associated with the diagnosis of concussion. Concussed athletes tended to report more symptoms and more severe symptoms than non-concussed athletes (6 (2–12) vs 1 (0–1) total symptoms and 12 (2–24) vs 1 (0–2) symptom severity) although neither was significant (both p = 0.125). A significantly higher number of symptoms and symptom severity has been reported in concussed professional hockey players compared to non-concussed players following a possible concussive incident, yet with median scores of 0 for both groups. 12
Commonly reported symptoms of headache, pressure in head, neck pain, and fatigue or low energy in concussed athletes were reported by both concussed and non-concussed athletes and therefore had lower diagnostic value. This finding is supported by other studies which have also found symptoms such as headache to be sensitive for concussion, however not specific if used in isolation without the assistance of other concussion assessment tools. 6 By contrast, the symptoms ‘don’t feel right’ and ‘feeling slowed down’ were commonly reported by concussed athletes only and had higher diagnostic value. Therefore, these symptoms may have greater clinical utility for diagnosis of concussion in cricket athletes by raising the suspicion of the practitioner to possible concussion and dictating more cautious management. It should be noted by practitioners that concussed athletes also presented without these symptoms, hence the lower negative predictive values. Similarly, symptoms may also be present in non-concussed athletes, hence the importance of clinical judgement rather than sole reliance upon a clinical tool such as the SCAT. Symptoms of drowsiness, nervous or anxious and sadness had the lowest clinical utility for concussion diagnosis. Further analysis to consider patterns of present and absent symptoms was not conducted and may be a direction for future research.
Athlete reported ‘percent of normal’ was considerably lower for concussed athletes (60% (IQR: 60–90) compared to 99% (IQR: 95–100) for non-concussed athletes). This question was an important addition to the SCAT5 guided by a systematic review, expert panel and current research. 6 Answering this question requires athletes to interpret how they are feeling in the context of how they felt prior to the head impact, and how they normally feel with match fatigue and environmental stressors. The merit of similar contextual self-evaluation has been demonstrated previously in other athletic contexts for example rating of perceived exertion and subjective wellbeing.14,15 Therefore, ‘percent of normal’ may be more valuable than previously thought for concussion diagnosis and warrants further research.
Performance in the objective SCAT domains of orientation, concentration, balance and neurological screening were comparable between both concussed and non-concussed athletes. Another study of sports-related concussion also found poor utility of cognitive domains for concussion diagnosis. 16 It is possible that performance in these domains experiences a ceiling effect and therefore scaling and multimodal testing is vital.5,17 These domains of the SCAT may have lower clinical utility for concussion diagnosis in cricket, particularly if considered independently, however further research is needed.
Elite cricket athletes typically experience resolution of symptoms within 8 days, with 82% (95% CI: 70–90%) recovering in less than 10 days. This is consistent with the expected recovery timeframe of 10–14 days.5,18,19 Previous research has found longer recovery time in female athletes, however this was not observed within this study. 10 The median time to complete the graded RTP protocol was approximately one to two weeks which is also within the expected time for sports-related concussion.5,18,19 Prolonged recovery may be associated with a higher number of total symptoms at diagnosis,16,19,20–22 more severe symptoms,5,10,13,19,21,22 and impaired balance13,23–24 as has been shown in other sports. The data for this study does not adequately permit such analysis of an association between SCAT findings and recovery timeframes, hence further research is needed to determine if these clinical features are also seen in elite cricketers who have prolonged recovery. Even with an understanding of presentation on the day of injury and recovery timeframes, it is important to stress that the management of concussion remains a clinical decision which allows for consideration of individual and environmental factors not accounted for in studies.
A strength of this study is the consistent methods and data entry over five seasons which allowed for a relatively large number of concussed athletes to be included. A key limitation, however, is that the components of SCAT data analysed are not independent of diagnosis, as SCAT findings were used alongside neurocognitive testing, video review and clinical assessment to inform diagnosis. These assessments were performed on the day of injury and over subsequent days to ensure athletes with delayed concussion presentation were not mis-diagnosed as non-concussed based on their presentation on the day of injury. Delayed presentations, which have been reported previously,9 were not considered separately in this study as the objective was to describe findings on the day of injury, and as such highlighting the individual variability which should be considered by the clinician.25
A further limitation is the incomplete data available for SCAT completed on the day of injury. This may be attributable to a small number of cases where concussion diagnosis was clear and a SCAT not completed, and an inability to retrieve historical paper records from all practitioners. The SCAT has since been digitised for direct entry in the Athlete Management System to address this limitation. Another limitation was the revision of the SCAT3 to a SCAT5 in April 2017 with one of the major additions in the latter being the question on ‘percent of normal’. As such, only 47% of the SCAT included in this study included this information, therefore reducing the statistical power of this seemingly critical component. The lower proportion of females in the non-concussed comparison group may have also biased results. A large, multination prospective trial investigating SCAT findings in cricketers would be of value for future research. Lastly, clinical judgement remains the accepted standard for diagnosis of concussion and there is currently no objective test that can be used in isolation to diagnose concussion. Therefore, findings in this retrospective study cannot be held in higher regard than a practitioner’s judgement at the time of the concussion.
Conclusion
Head impacts in cricket require timely and accurate assessment to establish whether an athlete requires removal from play or training. This study retrospectively reviewed SCAT data from concussed and non-concussed elite cricket athletes following a head impact to determine which clinical features are associated with concussion diagnosis. The components of the SCAT with the greatest clinical utility were athlete-reported symptoms, particularly ‘don’t feel right’ and ‘feeling slowed down’, and how athletes rated their ‘percent of normal’. Concussed athletes typically did not perform worse on objective components of the SCAT. Symptoms typically resolved within 2–8 days and athletes completed a graded RTP protocol within 4–14 days. The range of recovery time illustrates the need for individualised management of the concussed athlete. The findings of this study may help to inform clinical management of head impacts in elite cricket.
Footnotes
Acknowledgements
The authors would like to acknowledge the medical professionals who collected the data over the five-year study period.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and publication of this article: This research was supported in-kind by Cricket Australia.
