Abstract
Objective
A retrospective audit of minor traumatic brain injury presentations to three Brisbane emergency departments aiming to assess rates of CT scans and compliance with the Canadian CT Head Rule (CCTHR), as well as reviewing the demographics of patients and their management.
Method
Minor traumatic brain injury presentations to the Emergency departments of the Royal Brisbane and Women’s Hospital, Redcliffe Hospital and Queen Elizabeth II Hospital between July 1st and August 30th, 2019 were identified via diagnosis searches in patient tracking systems. Data collected included patient demographics, use of CT scans and Abbreviated Westmead Post Traumatic Amnesia Scale assessment, length of stay and discharge advice regarding return to sport.
Results
200 minor traumatic brain injury presentations were included. 75% of patients received a CT head with only 9% of these found to be non-compliant with the CCTHR. The most common indications for CTs were age >65, GCS <15 at 2 hours post injury and anticoagulation. Only 40% of patients that qualified for A-WTPAS received the assessment. 18% of presentations were due to sporting injuries and 69% were not given return to play advice. The average length of stay was 250 minutes with 41.5% of presentations longer than 4 hours. 99% of the patients were discharged home from the ED with 1% admitted.
Conclusion
The study characterised minor traumatic brain injury management across three emergency departments and showed that most patients received CT head scans that were indicated. However, other areas of management such as A-WPTAs and return to play advice must be improved.
Introduction
Minor traumatic brain injuries (mTBIs) represent a significant patient burden for the emergency department (ED). Recent Australian research similarly reports a significant patient load, with confirmed mTBI cases making up approximately 1.2% of all ED attendances. 1, 2 However, the true number of mTBI cases is likely to be even higher, with the incidence of hospital-treated mTBI likely underestimated because of challenges in recognition and documentation of diagnoses. 3
mTBI can lead to potentially significant long-term consequences if not appropriately identified and managed.4,5 Patients commonly suffer from both cognitive and behavioural symptoms in the initial days to weeks post injury, which may include headache, dizziness, difficulty with concentration and memory, insomnia, and mood swings. This constellation of symptoms can persist for weeks to months and is often referred to as post-concussion syndrome (PCS). 6
One commonly accepted definition of mTBI is a blunt trauma to the head with a Glasgow Coma Scale (GCS) score of 13–15 after 30 minutes post injury, with one or more of confusion/disorientation, amnesia, or witnessed loss of consciousness for 30 minutes or less. 7 There remains a lack of uniformity in terminology in the literature, with the terms ‘minor/mild head injury’, ‘minor/mild traumatic brain injury’ and ‘concussion’ all often used interchangeably to describe a similar clinical syndrome. 8 Distinction has also been made between minor and trivial/minimal traumatic brain injuries, which is defined as head injury without loss of consciousness, amnesia or confusion/disorientation with a GCS score of 15. 9
An important subgroup of mTBI presentations is sport-related concussion(SRC). This is a growing health concern in Australia and can affect athletes at all levels of sport. 10 While quality data on sSRC in Australia is lacking, one Victorian study found that SRCs made up as much as 16.5% of hospital admissions for concussion. 11 This population is important to identify in ED as they require specific advice on physical and cognitive rest, as well as graded return to play (GRTP). 10
The diagnosis of mTBI can be challenging and is often missed due to differences in diagnostic criteria as well as transient and subtle symptoms. 3 In the acute phase, GCS score remains the mainstay of clinical assessment however recent evidence suggests that GCS alone is a limited tool in the assessment of mTBI. 12 This is because GCS alone does not allow for assessment of a patient’s ability to form new memories, which has been shown to be one of the best predictors of outcome following TBI. 13 The inability to lay down new memories following a TBI is now widely known as post-traumatic amnesia (PTA). PTA testing has been shown to be superior to GCS alone in demonstrating cognitive impairment in patients following mTBI, which is useful indicator of head injury severity and is a good predictor for functional neurological outcome.12,14–16 One of the most widely used forms of PTA testing in Australia is the Westmead Post-Traumatic Amnesia Scale (WPTAS). While the original test measures patient responses over three days, an Abbreviated Westmead PTA Scale (A-WPTAS) was developed in 2003 by Ponsford et al. 17 and validated by Meares et al. in 2011. 16 It allows for rapid, standardised testing for PTA in an ED environment with hourly measures of orientation and memory and provides a useful tool to assess patient recovery from PTA to aid in determining their disposition, i.e discharging home or admitting to hospital. A-WTPAS do have limitations in that they cannot be used to assess patients under the influence of drugs or alcohol or in patients with a history of cognitive impairment.Another key area in the ED management of TBI is the decision for neuroimaging. Computed tomography (CT) scan remains the mainstay of imaging in neurotrauma, with good sensitivity and specificity for significant intracranial haemorrhage 18 ) There is only a small subgroup of mTBI patients who have significant intracranial pathology which may be fatal if missed, and this presents a challenge in differentiating patients who require imaging and those who can be safely discharged without further intervention. There are several clinical decision-making tools available to aid in the CT referral process. One of the most widely used and validated such tools is the Canadian CT Head Rule (CCTHR), which forms the basis of many mTBI imaging clinical guidelines, including that of the Australasian College for Emergency Medicine (ACEM). 19 It was developed in 2001 to help predict mTBI patients who may have had a intracranial injury and thus required neuro-imaging. 9 Both the initial paper and multiple subsequent validation studies have found that the CCTHR has a high sensitivity for identifying injuries requiring neurosurgical intervention, balanced with reasonable specificity to still allow for judicious use of CT.9,20–22 One systematic review of 22 different studies found that the CCTHR parameters allowed for CT scanning to be avoided in a reasonable proportion of patients without an excessive risk of missed significant intracranial injury, describing a sensitivity of 99–100% and specificity of 48–77% for the rule. 23
However, while there is a wide base of evidence supporting use of the CCTHR, it is often inappropriately applied or ignored in clinical practice. This paper aims to analyse the management of mTBI in three urban emergency departments in South East Queensland. The primary objective is to assess the rates of CT head and compliance with the CCTHR, with secondary measures of:
A-WPTAS testing patient disposition following ED treatment adequacy of discharge advice (especially with regards to sport-related concussions) length of patient stay in the ED.
Method
This was a retrospective cross sectional study, with data collected from three urban EDs in South-East Queensland; the Royal Brisbane & Women’s Hospital (RBWH), a tertiary metropolitan adult department and major trauma referral centre for the Metro North region of Brisbane, Redcliffe Hospital (RDH), a mixed adult and paediatric urban district department in Metro North and Queen Elizabeth II Hospital (QEH), a mixed adult and paediatric urban district department in Metro South Brisbane. All 3 sites regularly see minor head trauma patients for which they implement the CCTHR and have access to a CT scanner on site. The institutional review board reviewed the study and provided an exemption from full ethical review (LNR/2020/QRBW/67,477).
Data collection
Data was collected from the emergency patient tracking systems for each ED: Emergency Department Information System (EDIS) for RBWH and RDH, and Integrated Electronic Medical Record (ieMR) for QEH, with subsequent chart review of each case. Each database was searched for patient presentations with a recorded diagnosis of “minor head injury” or “concussion” (including “concussion - loss of consciousness” and “concussion - no loss of consciousness”) between July 1st and August 31st, 2019. Medical records were then reviewed by one of three investigators (JT, RS, GJ). Only encounters involving patients age 16 or over, that sustained trauma to the head with a loss of consciousness, amnesia of events or witnessed confusion post trauma were included for subsequent analysis (see Figure 1). Any presentations where the patient received a CT head and it showed an intracranial injury were excluded (n = 1). The data was de-identified, and the informationcollected included patient demographics (age, gender), sporting nature of the injury and anticoagulation status. Data on management of each patient included the decision for CT head, patient disposition, length of stay (from triage to discharge) and whether GRTP advice was given. Presentations were also analysed to determine if A-WTPAS were indicated and if they were completed, it should be noted that at the time of the study Redcliffe hospital ED did not conduct A-WPTAS as part of head injury assessments and so this data was excluded. The presentations involving a CT head were then analysed to assess if the CTs were indicated based on the CCTHR and what the indication was.
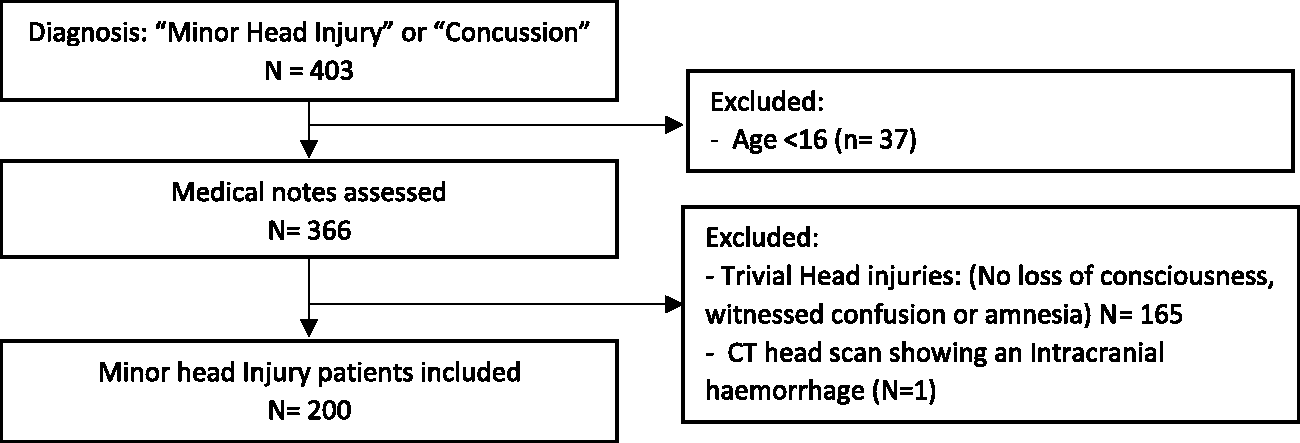
Patient selection flow diagram.
Statistical analysis
The mean and standard deviations of patients age and length of stay were calculated. Descriptive statistics have been included in the results. To examine the effects of CT scans and A-WPTAS assessments on length of stay, a T-test was completed from the means to calculate a p value. To examine the effect of CT scan on A-WPTAS assessment odds ratios (ORs) were calculated with CT head scan against the incidence of A-WPTAS assessment. Statistical significance was set at p < 0.05.
Results
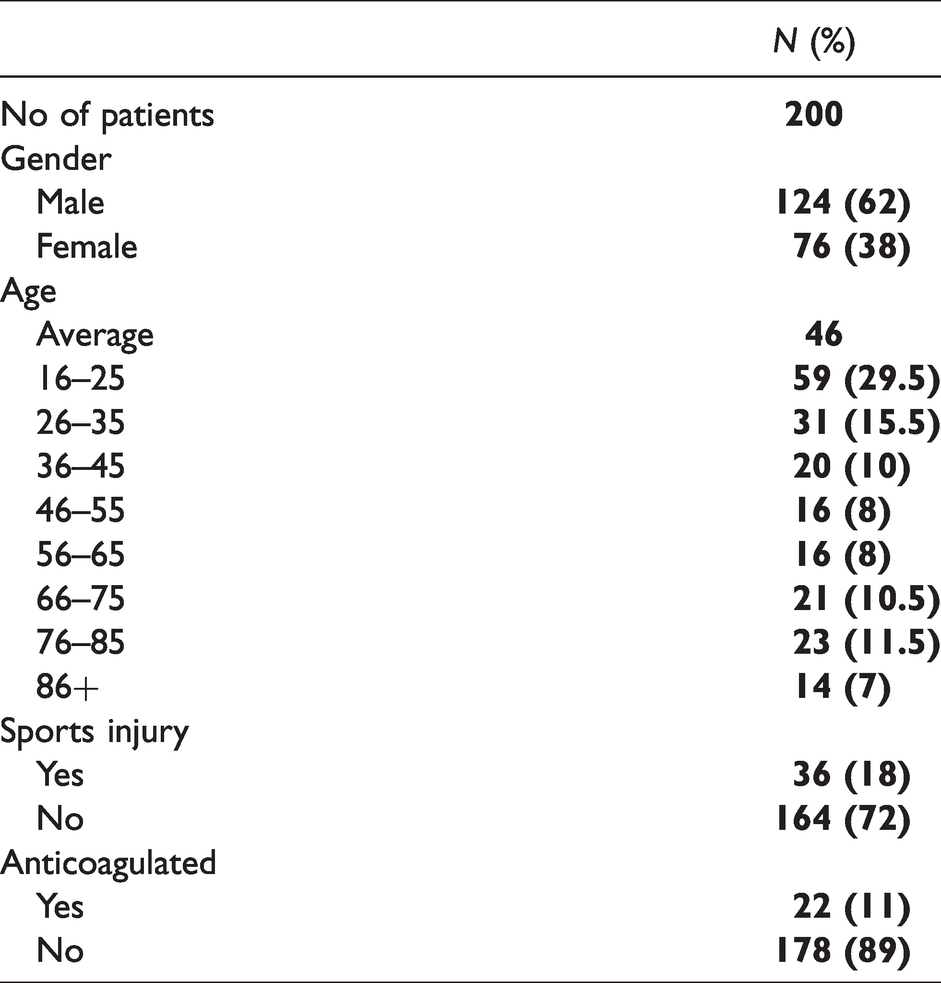
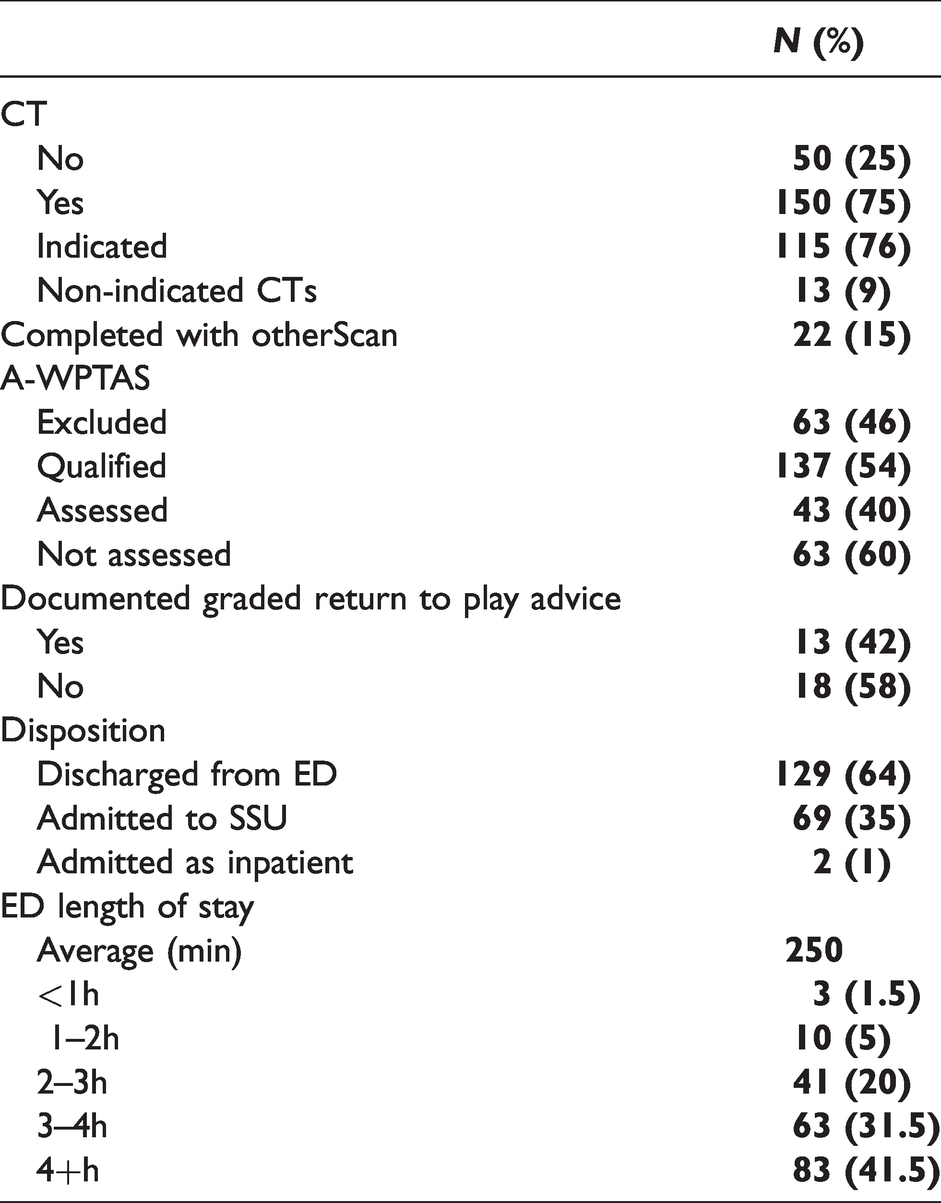
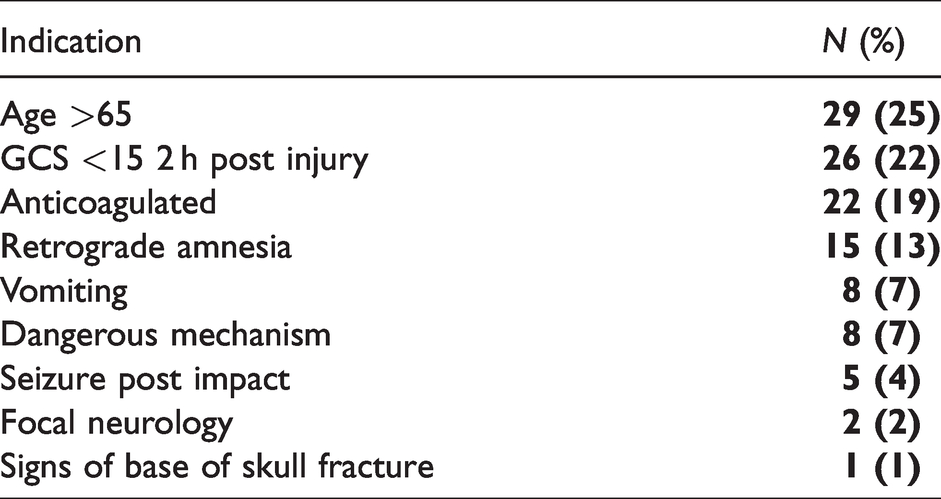
200 presentations were identified in the time period matching the required criteria (RBWH n = 106, RDH n = 53, QEII n = 41) and pooled for analysis. Table 1 shows the key demographic data of the 200 patients included in the study. It shows a predominance of male gender (n = 12,462%) and younger age with 55% being under 45 (n = 110). 18% (n = 36) were due to sports injuries, and 22 cases (11%) had been prescribed anticoagulant medication. Table 2 shows the key data in relation to the management of the mTBI presentations. 75% of the patients received a CT head, with 9% of these not indicated according to the CCTHR and 15% were scans completed with scans of other areas (e.g. C-spine or face) which most sites deem as acceptable practise. There were 5 patients who met the CCTHR but did not receive CT scans. 54% patients qualified to receive A-WPTAs, however only 40% had evidence of this being completed during their admission. As seen in Table 1, there were 36 sport related injuries and only 13 (31%) of whom received documented GRTP advice. Only two patients from the study were admitted to hospital, with the 198 others being discharged either from ED (n = 12,964%) or from the short stay unit (n = 69, 35%). The average length of stay was 250 mins with 41.5% (n = 83) of patient ED stays over 4 hours. For the patients for whom A-WPTAs were indicated, their assessment status had no statistically significant difference on length of stay (assessed µ= 239, sd= 82, not assessed µ= 245 sd= 108, T = 0.25, p = 0.08). Unsurprisingly, it was found that patients who received CT head scans had an average longer length of stay of 74 mins (T=−4.1, p = 0.0006) compared to those who did not. Receiving a CT scan had no statistically significant effect on administration of the A-WPTAS assessment (OR 0.6, 95% CI 0.24– 1.48, Z = 1.18, p = 0.26). Table 3 shows the Canadian CT Head Rule indications for completed CT scans. Age over 65 was the most common indication (n = 29, 25%), with GCS <15 2 hours post injury (n = 26, 22%) and anticoagulation (n = 22, 19%) being the next most common. Figure 2 displays the number of presenting patients in age groups and divided into those receiving CT head scans or not. It shows a higher number of young patients presenting but with a lower proportion of these patients receiving a CT scan.
Patient demographic data.
Key data characteristics in the management of mTBI presentations.
Indications for CT scans.
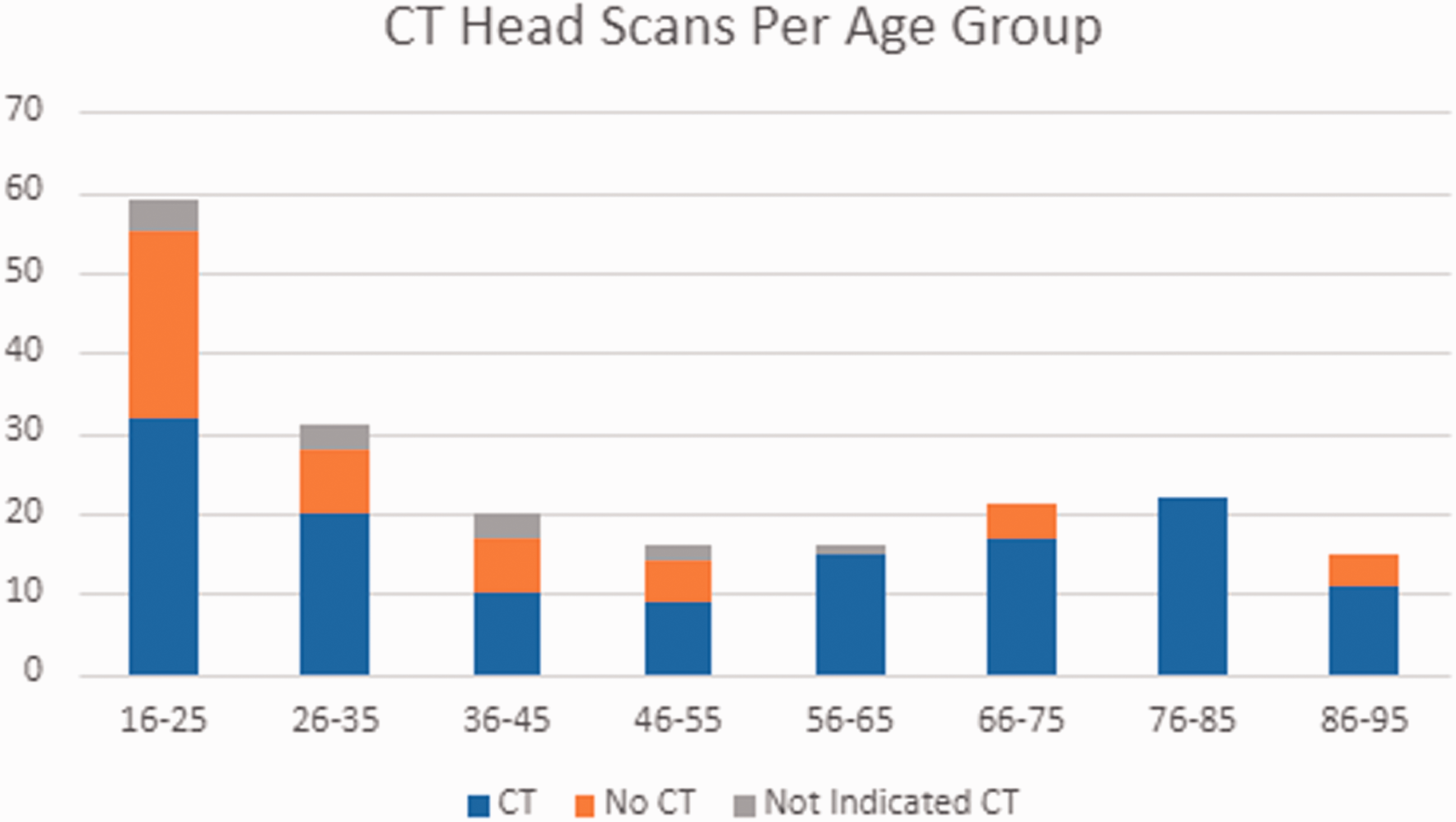
The number of mTBI presentations based on age group and whether they received a CT or not, and if they were indicated.
Discussion
Overall, there appeared to be good adherence to the Canadian CT Head Rule, with only 9% of CT heads performed across the 3 centres found to be non-compliant to these rules. However, it should be noted that data only included patients that met mTBI injury criteria (one of the inclusion criteria for the CCTHR). Data from individuals with a trivial/minimal traumatic brain injury (head injury without loss of consciousness, amnesia, disorientation or GCS <15) were not included. CT scanning in this subgroup may also occur, with inappropriate application of the Canadian CT Head Rule. Therefore, clear conclusions around overall prevalence of CT scanning in head trauma cannot be drawn from this study.
When used appropriately, the CCTHR allows for a scanning protocol that can clearly be linked to a reduced length of stay (LOS) in ED, with this study finding that when a CT scan was perfomre dit lead to an increased average LOSof 74 min. In contrast, appropriate use of the A-WPTAS assessment did not lead to any significant impact on LOS. With EDs in Australia following the National Emergency Access Target (NEAT) of 4 hours, reducing LOS in ED continues to remain a key performance indicator. Improving adherence to the CCTHR could achieved by clearly endorsing and displaying the CCTHR/CT imaging guidelines in visible areas of the department similarly to other clinical decision rules and pathways.
One of the major findings and areas for improvement is the rate of A-WPTAS assessments, with only 40% of qualifying patients having the A-WPTA completed. It may have been hypothesised that the low rate of A-WPTAS may be due to the high CT rate and clinicians incorrectly substituting CT scanning for A-WPTAS Creation of clinical pathways or flow charts for investigation and management of minor head trauma that involve A-WPTAS should improve not only rate of A-WPTAs but the overall management of head injuries, similar to what has been seen with investigation of suspected pulmonary embolism pathways in EDs in Melbourne, Australia. 24
From the audit data, 18% of presentations were sports-related minor traumatic brain injuries within this sub-set, 69% were not given documented GRTP advice, despite this being a key element of treatment and recovery. Clear GRTP is a cornerstone of concussion management and should be considered standard care when discharging patients from ED. Improvement in discharge advice as well as documentation of this would be an achievable and measurable post-study quality improvement initiative. Production of and distribution of written patient information handouts with clearly documented return to play/work plans would likely improve this. It is well known that verbal advice on discharge from EDs is often quickly forgotten and providing written information alongside verbal counselling improves patient knowledge and recollection.20,25
Limitations
There were some limitations to this study. Most of the data recorded is reliant upon the medical notes. The initial data collection was via a diagnosis-coded search in patient tracking systems. Often in patients with multiple isnjuries, minor traumatic brain injuries are not recorded as a diagnosis, and there was likely a cohort of patients missed as a result of this. Specific details around the head trauma are key to the diagnosis of a mTBI, such as a loss of consciousness, amnesia and witnessed confusion post the injury. Often one or multiple of these features are omitted in the clinical notes. Future studies would benefit from clearer documentation and ensuring all diagnoses are recorded. The second limitation is that this study was limited to three EDs within a single city conducted over two months. Future studies held over many departments in multiple cities over a longer time frame may help further characterise patient demographics and assess CT head and A-WPTAS assessment rates.
Conclusion
This study characterised mTBI injury presentations and audited management for the three participating emergency departments. The findings showed that most (75%) of patients presenting with a mTBI received a CT head scan and that the large majority (91%) of these were indicated. However other important areas of management such as A-WPTAS assessments and GRTP advice can be improved on. Given that mTBI’s are an increasingly common presentation to EDs and their potential long-term health effects are becoming more well identified, further education and training around the management of mTBI is needed.
Key findings
75% received CT heads, of these 9% were not indicated based on Canadian CT Head Rule
Most common indications for CT head scans were age, GCS <15 at 2hrs post injury and anticoagulation
99% of patients were discharged home (65% from ED unit, 34% from the Short stay unit)
Average length of stay was 250 mins with 41.5% of presentations staying longer than 4 hours
60% of patients that qualified for A-WPTAS did not receive them
18% of presentations were due to sport injuries and 69% of these patients did not receive return to play advice
Footnotes
Authors’ contributions
Gary Mitchell: study coordination, manuscript preparation, study design.
Jack Taylor, Rahul Snelling, Gilbert Jin: data collection, data analysis, manuscript preparation.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
