Abstract
Objective
To determine if there are differences in post-concussion symptom levels depending on 1) when physical therapy treatment is begun after the concussion and 2) the length of treatment.
Method
Retrospective chart review yielded 202 patients who sustained concussions and were referred for physical therapy. Participants/patients were assigned to independent groups based on time elapsed between concussion and physical therapy (0–14, 15–30, 31–60, 61–120, 121–365 days), and on months spent in treatment (1–4). Pre- and post- treatment scores were documented for the following measures: Sport Concussion Assessment Tool (SCAT), Convergence Insufficiency Symptom Survey (CISS), Dizziness Handicap Inventory (DHI), and Modified Clinical Test of Sensory Interaction on Balance (mCTSIB) using ANOVAs, with a Bonferroni-corrected
Results
All patients demonstrated improvements with treatment, with no significant differences in outcomes for time elapsed since injury (SCAT Symptom Score (
Conclusions
Improvements were similar for all patients receiving post-concussive physical therapy, regardless of time between injury and treatment onset, and regardless of time spent in treatment. These results may have implications for clinical decision-making and for third party payors’ coverage of post-concussion treatment. Longer periods of treatment may not necessarily be of greater benefit and application of treatment if delayed may also be beneficial. Limitations to the study, such as its retrospective nature, lack of randomization, and convenience sample size are discussed.
Keywords
The increasing recognition of concussion in sports has resulted in state concussion management legislation, sports rules changes, and increased public awareness.1,2 Concussion, also known as a mild traumatic brain injury, continues to be well-studied, however treatments for this medical condition have been elusive. 3 The Berlin Guidelines of the 5th International Consensus Conference in Concussion in Sport affirm the importance of rest during the acute period, approximately 24–48 h following the injury, followed by a gradual, carefully paced introduction of physical exercise so as not to exacerbate symptoms. 3 Studies of the acute post-concussion period have asserted both the detrimental effects of too much activity 4 as well as of too much rest 5 on recovery. Other studies have documented the benefits of introducing physical exercise as soon as tolerated.6,7
Active rehabilitation through exercise at one-month post injury was found to improve outcomes in a sample of 16 children and adolescents who had sustained mild traumatic brain injuries. 6 These findings were extended to slow-to-recover adolescents (i.e. after four weeks), who showed symptom improvement with activity. 8 A 2017 systematic review of therapy and rehabilitation for concussion identified 14 randomized controlled trials (RCTs), with only one employing physical therapy as treatment, and that study indicated improvement on the Post-Concussion Symptom Inventory by patient report. 9 Individualized “subthreshold exercise programs” have been recommended for patients in the acute recovery phase of concussion, using sub-symptom aerobic exercise as treatment for concussion, 10 and researchers have supported the efficacy of supervised exercise within 16 days of sport-related concussion. 11 In recent research, Leddy et al. have suggested, in their randomized clinical trial of adolescents, that individualized subthreshold exercise treatment in the early post-concussion period speeds recovery. 7 In this context, the Berlin Guidelines assert: “…closely monitored active rehabilitation programmes involving controlled sub-symptom-threshold, submaximal exercise have been shown to be safe and may be of benefit in facilitating recovery” and advise that “further research evaluating rest and active treatments should be performed…” 3 (p.15). The use of an individualized program of exercise, often in the form of physical therapy, has grown as the treatment of choice following concussion. 12
Physical therapy employs sub-symptom aerobic exercise as well as vestibular and oculomotor screening and therapy as treatment for concussion. 13 Exercise that is carefully titrated in the post-acute period may be beneficial in reducing incidence of persistent post-concussive symptoms, and the proposed reason for this improvement is that exercise may normalize cerebrovascular physiological dysfunctions. 14 However, the available research in this area of physical exercise titration and cerebrovascular physiological dysfunction has its limitations. Furthermore, it appears that some symptoms of concussion are oculomotor and vestibular in nature, occurring in up to 60% of concussed athletes, and these clinical subtypes of concussion may benefit from targeted vestibular therapy rehabilitation strategies, 15 not just physical exercise.
Currently, the practicing clinician is advised to rely on rest followed by active rehabilitation in the acute period as symptoms resolve. Time elapsed since the concussive event is a moderating variable that may affect treatment efficacy. 14 However, in typical clinical outpatient practice there are many times when active rehabilitation is not made available during the acute or early post-concussion phases of recovery, due to a variety of reasons that may include, but are not limited to, lack of physician awareness, patient avoidance of treatment, and insurance denials. Furthermore, the ongoing concerns of third-party payors/insurers about improper utilization of health care treatments and of access to treatment can impact early access to treatment in the acute period. 16
The predominance of research literature focuses on early intervention in the acute period, which shortens recovery time. Yet, are there benefits to delayed interventions? In a prospective quasi-experimental control group study of 49 “slow-to-recover” youth aged 8 to 17 years, active rehabilitation did not seem to affect post-concussion symptoms but did seem to improve quality of life and “energy”. 17 In contrast, an earlier randomized controlled trial that investigated cervicovestibular rehabilitation in 31 adolescents and young adults with persistent symptoms of sport-related concussion found that a combination of cervical and vestibular physiotherapy decreased time to medical clearance for sports. 18 A more recent retrospective study that employed physical therapy as an early, middle or late intervention in 120 adolescents indicated no significant differences in symptom reporting across the three groups, 19 and concluded that applying intervention early in the three weeks after a concussion is feasible and tolerable. Although research on the effectiveness of delayed physical therapy that includes sub-symptom aerobic training is still lacking, the research that is available suggests that such interventions may be of benefit. 20
Thus, the above research reveals mixed findings on the efficacy and value of delayed physical therapy treatment. Since many individuals often do not receive physical therapy treatment early in their concussion recovery, and since physical therapy is growing as the treatment of choice in the early recovery period, the aim of the present study was to determine whether there may also be value in initiating such treatment later in recovery. An additional aim was to help further determine whether the length of treatment should be a consideration for the clinician who is prescribing physical therapy treatment, especially when cost and time often prohibit lengthy treatments. In the current health care climate that positions health care providers as gatekeepers to treatment, appropriate referrals that are evidence-based increases the likelihood of effective outcomes. Although the efficacy of delayed physical/active interventions for concussion is limited, the findings in the more recent study by Lennon and authors described above suggest that physical therapy may also be of benefit if applied after a delay. 19 Thus, we predicted that in the present study patients in the post-concussion symptom period would benefit equally from physical therapy treatment even if the treatment was delayed. In addition, we sought to determine whether or not a longer treatment duration was of additional benefit.
Methods
Study design
Institutional Review Board approval was obtained for retrospective analysis of de-identified data. This was a retrospective study of a multi-office physical therapy private practice database/convenience sample. Patient (participant) consent was not required and the study size was pre-determined by the available database at the time of the study.
Participants
Participants consisted of patients who had been referred to a New Jersey multi-office out-patient physical therapy private practice by other health care providers and who were entered into the practice database between March 2014 and August 2018. These were patients who for the most part received services through health insurance coverage. Out of an initial pool of the eligible 212 patients, for whom an electronic record was available, retrospective data were obtained for a total of 202 patients, for a 4.7% attrition rate (which is lower than the 10% overall rate reported in a review of the literature
9
). All participants were assigned to groups based on the following two criteria: 1) time elapsed between concussion and initiation of physical therapy (0–14 days vs. 15–30 days vs. 31–60 days vs. 61–120 days vs. 121–365 days, and 2) number of months spent in physical therapy (1–4 months). The mean age of the sample was 25.0 (S.D. = 13.7) (Table 1), and 27.2% (
Patient demographics: Months spent in treatment.
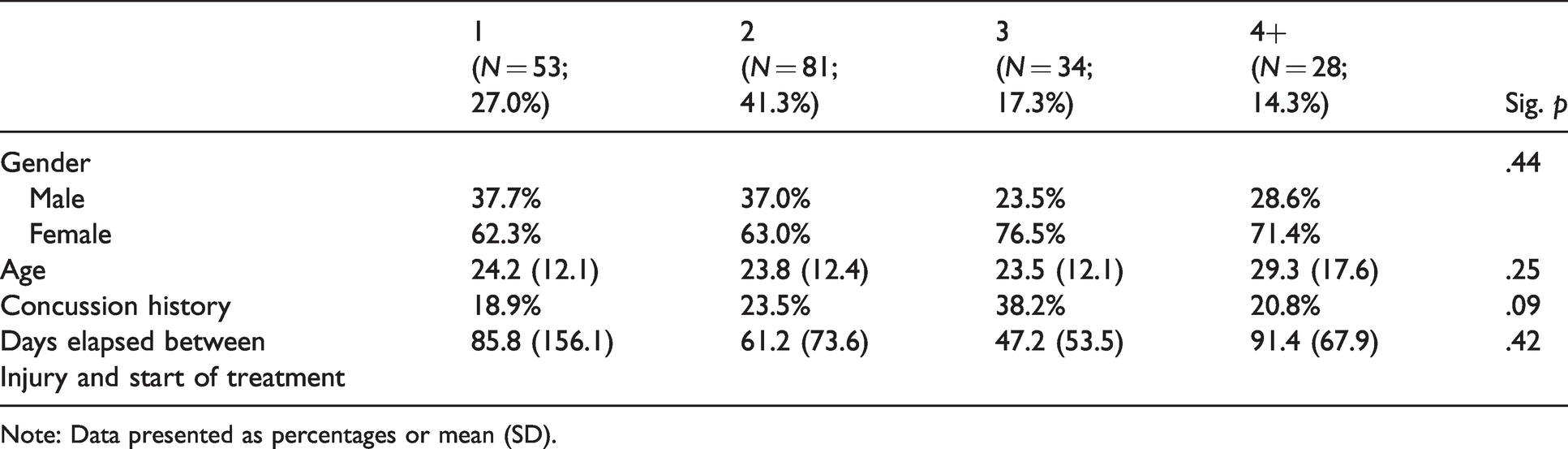
Note: Data presented as percentages or mean (SD).
Symptom endorsement/primary complaints.

Medication usage in the sample.
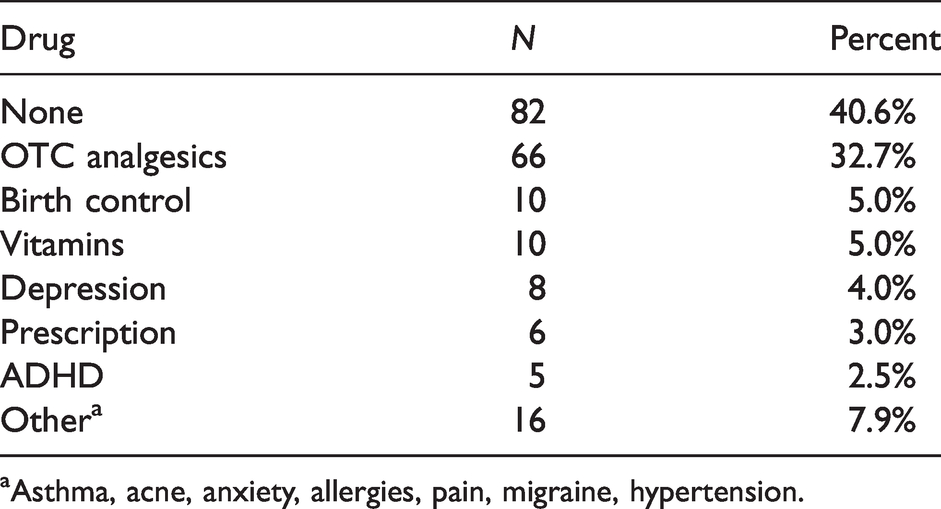
aAsthma, acne, anxiety, allergies, pain, migraine, hypertension.
Measures
Participants completed four measures at their first and last physical therapy appointments: The Symptom Evaluation from the Sport Concussion Assessment Tool versions 3 and 5 (SCAT3/5), the Convergence Insufficiency Symptom Survey (CISS), Dizziness Handicap Inventory (DHI), and the Modified Clinical Test of Sensory Interaction on Balance (mCTSIB). The SCAT is a standardized tool that is used to measure symptoms of concussion.
21
During the time span of the present study, the SCAT3 version was updated to the SCAT5. However, only the Symptom Evaluation, which is included in both versions of the SCAT, was utilized for analysis. It renders two scores: total number of symptoms (0–22) and symptom severity (0–132). Twenty-two symptoms, such as headache, feeling slowed down, sadness, trouble falling asleep, are rated on a 0 (none) to 6 (severe) scale. This symptom scale has been considered reliable and valid for assessing presence and severity of symptoms.
22
A systematic review of concussion symptom checklists indicated an internal consistency (Chronbach α) of .87, and test–retest reliability (Spearman
Treatment description
Participants were provided a course of physical therapy that was multimodal in nature and based on symptom presentation. Table 4 provides an outlined description of treatments. Modalities employed included: 1)
Description of treatments.

The frequency and intensity of the treatment was based on the patient’s presentation and symptoms/limitations. For example, patients with symptoms that primarily included dizziness, imbalance, headache, and/or visual disturbance were treated with vestibular rehabilitation. The intensity and complexity of vestibular rehabilitation increased as the patient’s symptoms/limitations improved. Patients who had a primary or co-complaint of neck pain, neck stiffness, headache, and/or dizziness were treated with manual therapies. Manual therapy interventions were continued until complaints of neck pain and/or neck stiffness were resolved. Patient’s with a primary or co-complaint of visual disturbance, headache, and/or dizziness were treated with neurological rehabilitation in the form of oculo-motor exercises that were progressed in a similar fashion as vestibular rehabilitation.
Clinical decision making involved with each modality was made to promote a patient’s functional recovery and return to previous level of function. With regard to sequencing of modalities within a treatment session, priority was given to manual therapy to help address complaints of neck pain, neck stiffness, headache, and/or dizziness. Thus, improving symptoms thought to be originating from the cervical spine helped to facilitate performance in other modalities (e.g. vestibular rehabilitation requires adequate neck range of motion, cervical afferent input interacts with vestibular and ocular function).
On average, patients were seen once or twice per week depending on symptom presentation and weaned to once per week with improvement. Sessions occurred in the physical therapy offices and each session lasted 45–60 min. Recovery and return to normal functioning was determined on a case by case basis through clinical decision-making that included 1) improvement on the four outcome measures described above, 2) clinical observations of physical functions, and 3) patient report of return to premorbid level of function.
Statistical methods
Analyses were conducted using SPSS, Version 23.
31
Patients were compared for gender differences (chi-square) and age and days spent in treatment (one-way ANOVAs). These comparisons were based on the group variables of months spent in treatment, and on time elapsed between injury and initiation of treatment. Given a small but significant relationship between total days in treatment and number of days between injury and initial evaluation (
Results
Tables 1 and 5 present Patient Demographics. Comparing groups based on months spent receiving post-concussion treatment, chi-square analysis revealed no significant between-groups differences based on gender (
Patient demographics: Time elapsed between injury and initiation of treatment.
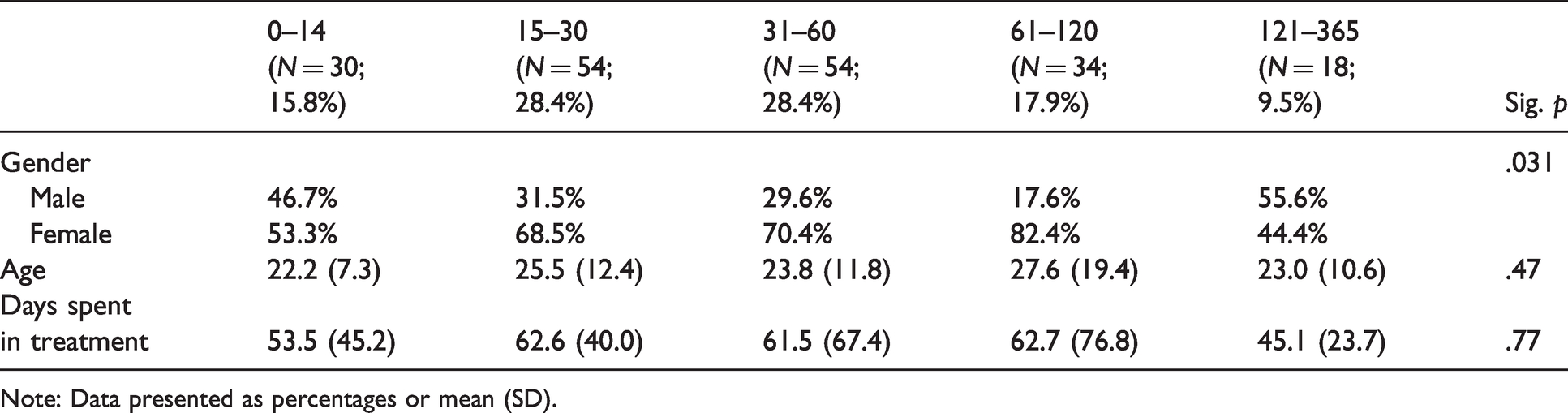
Note: Data presented as percentages or mean (SD).
For the first regression analysis, change scores on the SCAT, CISS, DHI, and mCTSIB were regressed on total days in treatment, with time between injury and initial evaluation entered as a co-variate. Neither time between injury and initial evaluation (
To illustrate the stability of change scores based on time since injury and based on total time in treatment, patients were assigned to independent groups based on time elapsed between concussion and initiation of physical therapy (0–14 days vs. 15–30 days vs. 31–60 days vs. 61–120 days vs. 121–365 days, and number of months spent in physical therapy (1–4 months), and change scores were analyzed using between-groups ANOVAs. There were no significant differences in outcomes for time elapsed since injury on SCAT Symptom Score (
Group differences: Time elapsed between injury and initiation of treatment.
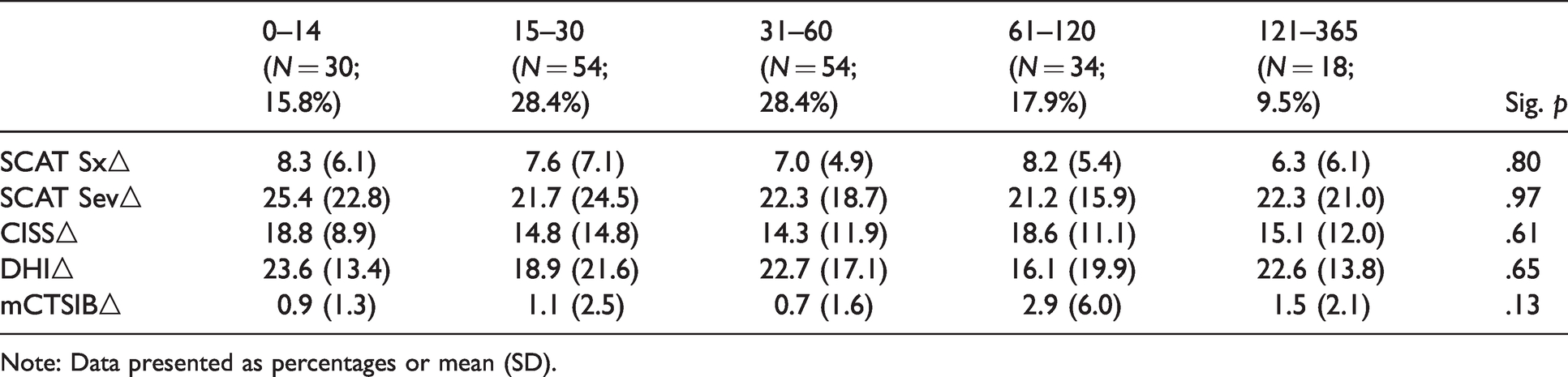
Note: Data presented as percentages or mean (SD).
Group differences: Months spent in treatment.
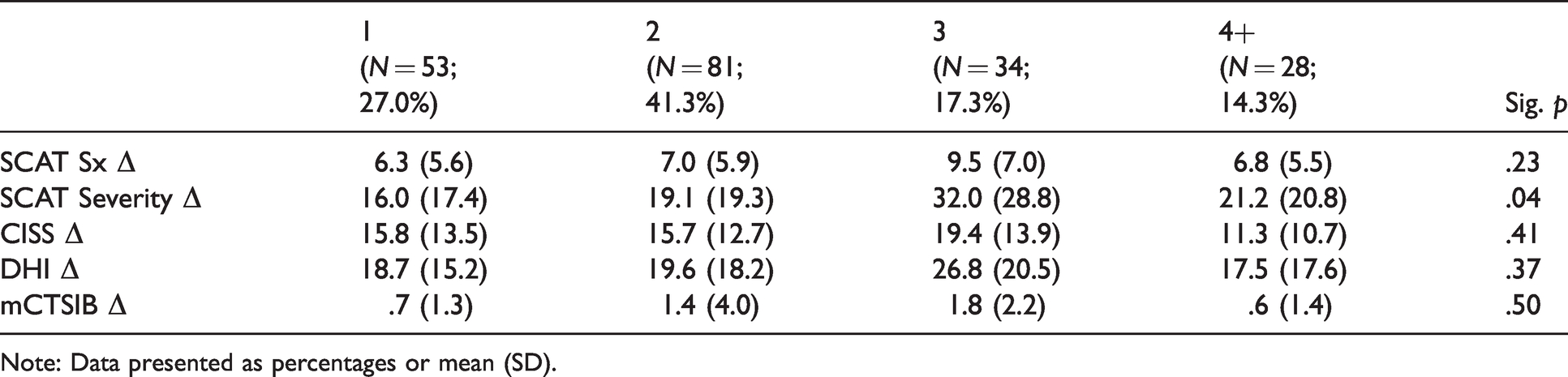
Note: Data presented as percentages or mean (SD).
Outcome scores showed statistically significant correlations (
Intercorrelations between outcome measures.
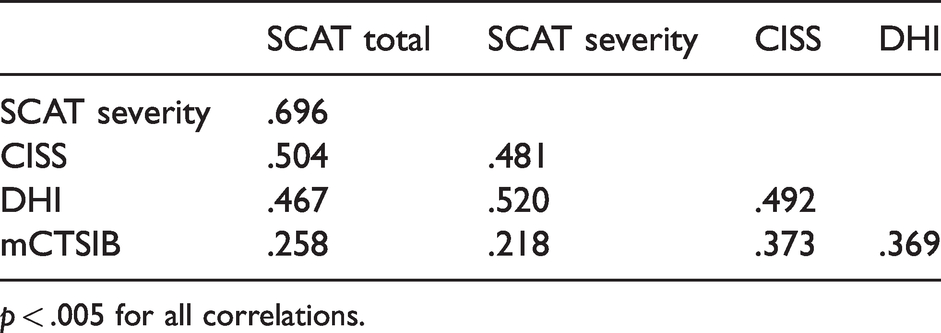
Discussion
These findings suggest that for patients with concussion, whether physical therapy was applied within the first 14 days post-concussion or much later, such as 121–365 days post-concussion, similar improvements were demonstrated. Improvements were documented for the number of reported concussion symptoms, endorsed symptom severity, ocular-motor function, balance, and dizziness. In addition, the duration of therapy, whether for one month or for up to four months, also did not appear to result in any differences in improvements.
These findings bear clinical implications for treatment planning. Since similar improvements were seen whether physical therapy was provided earlier (within 14 days post-concussion) or later, there is no reason to wait to initiate treatment. Early treatment may help accelerate recovery, improve morale, prevent possible adoption of a sick role, and reduce feelings of hopelessness for the patient. Importantly, though, if for some reason a patient is not referred for treatment early, or receives a concussion diagnosis at a late date, initiation of physical therapy appears to still be beneficial, and thus it is never too late to benefit from such therapy. For example, there may be a number of factors that could result in delay of treatment: geographic accessibility, other physical injuries, surgeries, or medical conditions that may have co-occurred independent of the concussion. In such cases, delayed physical therapy could still be of value. These interesting findings on the benefit of physical therapy treatment even if delayed parallel those findings published in other concussion research regarding the delayed application of rest.33–35
These results can inform third party payors who approve health care coverage for physical therapy in concussion patients. Payors should be poised to approve physical therapy services early after the concussion diagnosis, as well as later if the patient has not been referred for treatment in the early post-concussion stage. Importantly, other research has suggested the benefit of applying interventions early, within the first three weeks of concussion. 19
Of note, the present study also revealed that the length of treatment whether for one month or four months did not statistically make a difference in outcomes. That finding may encourage payors to approve briefer durations of physical therapy or in some cases discontinue services after one month. It is not clear why the duration of treatment did not reveal a difference in outcomes. Variables such as patient motivation for treatment, compliance with home assignments, educational level, or severity of the injury were not controlled for in the present study and could impact treatment efficacy and outcome.
Future research may do well to investigate these and other variables that may impact the effectiveness and duration of early or late treatment. Also, might there be an early spontaneous recovery period, after which one would determine whether therapy is even needed and should be initiated? There are many questions yet to be investigated, the answers to which may shed light on treatment decision-making.
It is clear there are significant limitations to the present study. Importantly, it was retrospective in scope, used a convenience sample, and lacked randomization. It also lacked a control/placebo group, thus limiting its generalizability to the clinical population studied. A systematic review of predictors of concussion recovery noted that most youth and young adults who have sustained sport-related concussions will recover clinically within one month 36 and other more specific studies have reported percentages such as 88.8% return to play within 10–21 days post injury 37 and 60.1% return to play within one week. 38 Thus, future studies of physical therapy treatment for concussion should consider the need for randomization, control for self-selection, account for those who improve early and never seek physical therapy, and as noted above consider the notion of spontaneous recovery.
The present sample consisted of a heterogeneous group, a mix of mechanism of injury and individually tailored treatment that were not controlled. As this patient sample spanned four years, it is not known whether treatments were altered over time based on therapist knowledge of the evolution of new international or national guidelines. Furthermore, participants represented one, although multi-centered, physical therapy practice. Finally, the number of days between injury and initial evaluation correlated positively with number of days in treatment. We controlled for this relationship as a statistical covariate (e.g. there was no resultant greater severity or symptom endorsement for patients with lengthier time intervals between injury and initial assessment). However, there may have been other factors or pre-physical-therapy concussion-related issues which were not documented or addressed in a physical therapy setting. Finally, a larger sample size would have also provided more confidence in the present findings.
Nonetheless, although the available research on the efficacy of physical therapy as a treatment for concussion is growing, many studies that have already been published are small in sample size, describe cases or case series, 39 and are without controls. The literature asserts the lack of standardized physical therapy treatment protocols for patients with prolonged concussion symptoms 12 yet recommends tailored, individualized protocols based on symptom presentation of the patient and application of clinical judgement and knowledge. 40 The present study adds to the growing literature on the value of physical therapy in concussion management and provides support for the benefit of such therapy whether early or late in the post-concussion stage. These findings can help guide the decisions of clinicians in the timing of their referrals of patients for treatment as well as apprise third party payors of the benefit of physical therapy early in the post-concussion stage.
Footnotes
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr Vidal is owner of the practice from which data were culled. Dr James was employed in that practice at the time. Dr Moser is owner and director of the Sports Concussion Center of NJ (SCCNJ) and has referred patients to the physical therapy practice that is noted. Dr Schatz is a consultant/research director for SCCNJ and consultant to ImPACT Applications Inc.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
