Abstract
Currently, there is a lack of clear, “gold standard” guidelines for the identification and management of sports-related concussion. This is of concern considering the importance of preventing further injury during game-play. Moreover, a number of assessment measures and tools aim to detect concussion in athletes and help inform return to play decisions, including the assessment of posture and balance, eye-saccades, memory, attention, orientation and post-concussive symptomatology. However, they have often not been widely disseminated for validity studies, and their utility or sensitivity in detecting concussion is limited due to a number of factors. As such, this review will examine current guidelines and sideline assessments measures which aim to inform decisions about return to play following sports-related concussion.
Introduction
Concussion, or mild traumatic brain injury (TBI), is fraught with difficulties with regards to definition, assessment, detection and diagnosis. 1 Throughout the literature and media, sports-related concussion is increasingly becoming a matter of concern. 2 As such, it is important for sports and medical professionals to understand how to diagnose and manage concussion, to prevent the likelihood of a “catastrophic outcome” during game-play. 3 However, disagreements among concussion assessment measures and return to play (RTP) guidelines for athletes have resulted in a lack of a gold standard for concussion management, 4 and there remains relatively little research in examining the efficacy of tools in identifying concussion in sports. 5 What is known is that when assessing concussion for RTP decisions, a comprehensive approach is best. 6 However, most guidelines tend to focus on loss of consciousness (LOC) and post-traumatic amnesia (PTA) as hallmarks for identifying concussion, 7 and there has been argument in the literature regarding the onset of concussive symptoms (e.g. memory) and how to make accurate decisions about managing concussion if some symptoms are delayed or not immediately obvious. 8 This review will outline the relevant literature regarding the most commonly cited and utilized sideline assessment measures for identifying sports-related concussion, and most prominent guidelines for management and RTP decisions.
Methods
A literature search was conducted using Google Scholar, Ovid Medline (1946—March 2017), and PsycINFO (1806—March 2017). The terms “traumatic brain injury” or “concussion” and “guidelines” or “sideline assessment” or “return to play” were used. Manual searching through Google Scholar was also conducted using specific search terms related to the guidelines and assessments under review (e.g. “Balance Error Scoring System,” “Standardised Assessed of Concussion”). Returned articles were screened by title, abstract or full-text accordingly. For brevity of the manuscript, included studies were only those directly relevant to the review: (a) initial validity/reliability studies for assessment measures, (b) original implementation of practice guidelines, (c) review manuscripts examining sideline measures/concussion guidelines. Articles were excluded if they were found to be un-related to the review’s scope and aims (i.e. those that did not include information pertaining to items (a)–(c) above), or were duplicate papers.
Discussion: guidelines
As discussed above, there remains a lack of a universal system of grading concussions to facilitate decisions about sideline assessment and management, and in returning athletes to play. 7 Table 1 outlines and describes the three most prominent guidelines cited throughout the literature—The American Academy of Neurology (AAN) guidelines, the Cantu guidelines, and the Colorado Medical Society guidelines.
Guidelines for grading of concussion and return to play.

LOC: loss of consciousness; PTA: post-traumatic amnesia; RTP: return to play; SAC: standardized assessment of concussion.
AAN guidelines in the management of concussion in sports
The AAN 9 guidelines are presented initially as a sideline concussion grading system, whereby decisions regarding RTP and concussion severity are based on length of LOC and resolution of symptoms before or after 15 min post-injury. 10 The AAN comprehensively examined guidelines for decision-making in the assessment, diagnosis, and management of concussion. 3 They examined a number of factors to help inform sideline assessment guidelines: Risk factors for sports-related concussion, useful and accurate diagnostic tools for concussion, measures and clinical factors important in identifying individuals at risk for ongoing concussion-related deficits, and effective interventions for individuals who suffer ongoing problems. 3
In general, research findings associated with each factor above produce mostly insufficient and inconclusive evidence regarding how to improve and inform sideline assessment guidelines, 3 and inconclusive research findings are often the case in concussion-related work. 1 With regards to risk factors for sports-related concussion, males are identified as higher risk (but only due to the sports they play, e.g. football and soccer present with a higher risk), and also factors including quality of head gear, higher body mass, and lower training time. 3 It is suggested that a combination of measures for the sideline assessment and identification of concussion would be most sensitive; however, research is unclear regarding the best tools to use. 3
Based on their findings, their guidelines were presented under three branches—pre-participation counseling, suspected concussion (use of checklists and screening tools, neuroimaging) diagnosed concussion (RTP risk of recurrent concussion, RTP age effects, RTP concussion resolution, RTP graded physical activity, cognitive restructuring), and retirement of play after multiple concussions (assessment and counseling). 3 It has been argued that issues arise where most emphasis is placed on LOC as an indicator for concussion and marker of severity, rather than number or duration of symptoms, based on findings which indicate that symptoms and memory are better predictors of concussion. 8
Cantu grading system for concussion and guidelines for RTP
The Cantu guidelines 7 provide a practical and directive scheme for grading concussion (grade 1, 2 or 3), which focuses on the presence and severity of LOC, PTA symptoms, and anterograde and retrograde memory difficulties. This grading system then provides step-based decisions on whether or not the athlete should RTP, based on length of time that the athlete has been asymptomatic and the number and severity of concussions incurred. 7 The assessment of anterograde and retrograde amnesia is conducted by a sideline examiner who asks basic questions to the athlete, as outlined in Table 1. Although the guidelines appear straightforward and provide grade-related recommendations for RTP based on severity of concussion, the utility of the assessment is questionable due to the lack of objectiveness of the questions used. Further, more specific guidelines are necessary for how to assess these symptoms, as they can be very subtle in some circumstances, particularly in athletes with mild concussion. Moreover, the authors themselves contend that on the field, LOC usually does not last more than five minutes, and will tend to last for a few brief seconds only. 7 As such, it would take a well-trained assessor to identify LOC in these cases and grade concussion accurately. However, due to the guidelines’ focus on assessing symptoms and changes in memory function, it has been proposed that the guidelines would be more accurate in making decisions about RTP, given that memory and concussive symptoms have been identified as most strongly predictive of severity of injury. 8
Colorado Medical Society Guidelines for the management of concussion in sports
The Colorado Medical Society 11 produced guidelines to compensate for the lack of clear instructions in the management of sports-related concussion in young athletes 12 and emphasized the need for a more comprehensive assessment of the athlete’s mental state in order to detect more subtle effects of concussion, as mentioned above. 12 Similar to Cantu, 7 RTP guidelines were based on a grading system of concussion, as seen in Table 1. The authors’ rationale for the development of this system is the prevention of “catastrophic outcome” including swelling of the brain, neuropsychological deficits, and chronic post-concussion symptoms. 13 Again, grading of concussion and therefore decisions for RTP appear to be based on the presence and duration of LOC and PTA; however, in most circumstances, these can be very brief, particularly for very mild concussion. Moreover, concussive symptoms and difficulties with memory may not manifest for more than 24 h after injury.8,14 Therefore, consensus about the assessment and identification of such a sensitive construct is required to help identify athletes with concussion and help to prevent more severe injury and negligent RTP decisions.
Summary of differences among guidelines
In summary, the aforementioned guidelines for managing sports-related concussion are similar in their procedures for grading severity of concussion and follow-up decisions regarding RTP and medical care. The major difference pertains to terminology (e.g. transient versus brief) and a lack of defining terms used (e.g. asymptomatic, confusion). Moreover, differences exist in length of time for LOC and PTA for each concussion grade among the guidelines. Considering these factors, perhaps the “best practice” approach would be to choose the guidelines which present more clearly defined indicators for each grade of concussion, are more conservative with regards to length of PTA and LOC, and provide more detailed information about management and follow-up. At this time, the Colorado Guidelines would satisfy the above and should be recommended for consultation when considering sports-related concussion.
Discussion: sideline assessment measures
There are multiple measures and tools which claim to assist in identifying athletes with concussion, and aim to help make decisions regarding RTP. Areas of assessment have included balance and posture, eye saccades, neuropsychological or neurocognitive functioning, and comprehensive assessments. Table 2 outlines the assessment measures within this review, including information regarding procedures, psychometrics, and practicality.
Sideline assessment measures for identifying concussion in sports.
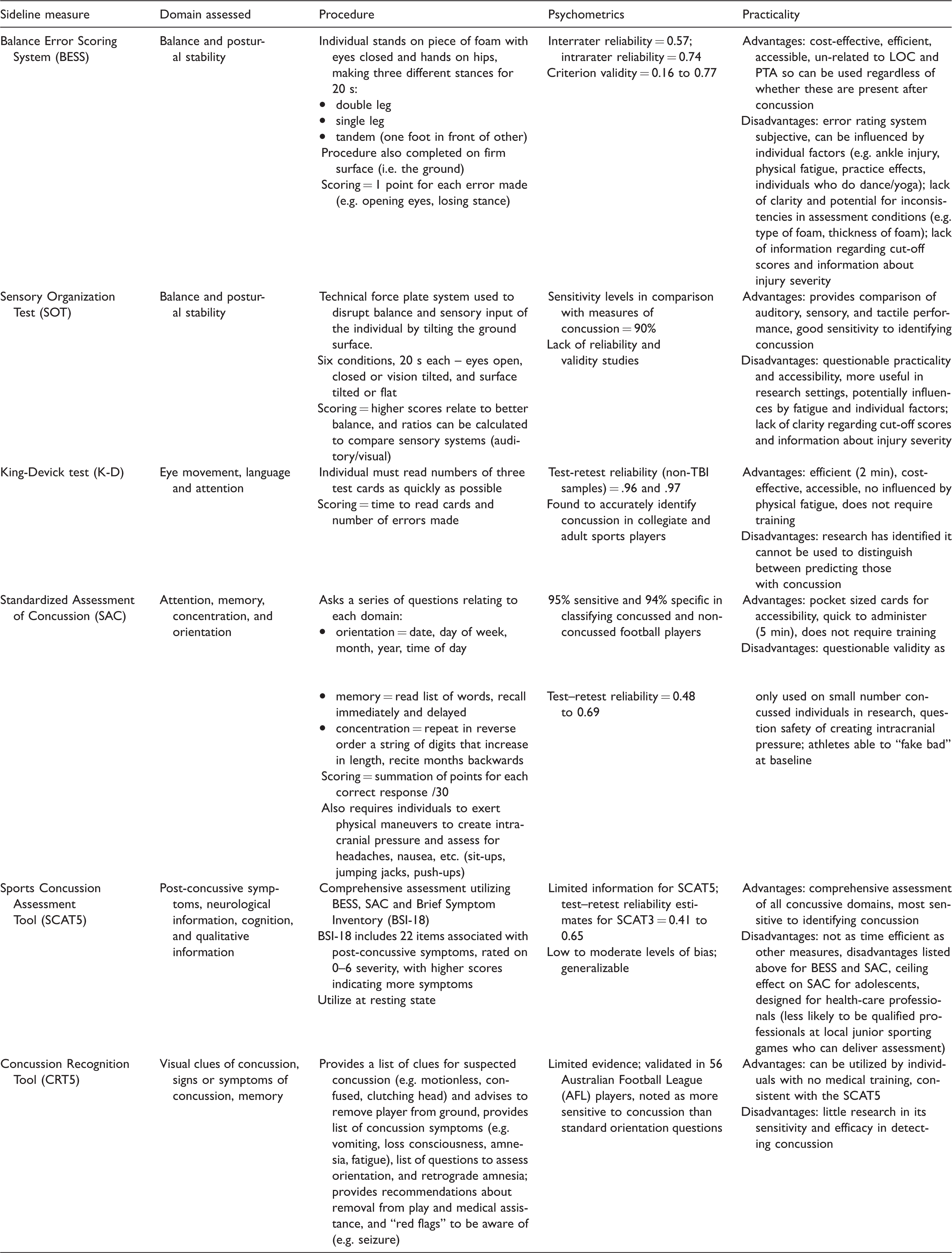
LOC: loss of consciousness; PTA: post-traumatic amnesia; SAC: standardized assessment of concussion.
Balance and postural stability
It is argued that the assessment of balance following concussion is important, as concussions frequently result in postural instability 15 due to the role of the central nervous system in providing feedback to and maintaining equilibrium among the visual, somatosensory, and vestibular systems. 2 More practically, balance is important for movement in sport, 2 and deficits in postural instability have been noted to be evident for significant periods of time post-TBI. 4
Postural instability and balance issues following concussion are likely due to deficits in sensory organization systems. 4 When athletes are concussed, it creates a sensory integration problem where all sensory systems do not communicate as effectively. 4 Considering that posture is mostly dependent on how information from visual, vestibular, and proprioceptive systems are organized and how sensations are processed, 2 it is hypothesized that individuals with concussion may be identified based on poor balance control. Therefore, as a method to assess balance on the sidelines of a sporting game, it has been postulated that manipulation of posture in varying conditions may be useful in providing information about post-concussive impairments.
Balance error scoring system
The balance error scoring system (BESS) has been deemed an inexpensive and practical tool which enables cost-effective, efficient, and accessible assessment of balance, and can be conducted on the sidelines of the game.2,15 It is recommended that pre-season baseline assessments are conducted so that examiners may compare individual errors following concussion. 15 A reliability study utilized three independent scorers who were shown 30 videos of individuals performing the BESS stances (see Table 2), and rated their performance. 15 Two weeks later the same method was repeated with videos viewed in a randomized order, and reliability estimates were quite variable for both inter- and intra-rater scores. 15 As such, the error rating system is quite subjective, as the study indicated, 15 which is likely to affect the sensitivity of the measure in identifying concussion.
Moreover, performance on the BESS may be influenced by a number of individual factors. 2 For example, individuals with an ankle or leg injury would be likely to have impaired balance, and a sport reliant on intense movement of legs (e.g. kicking, running) will result in fatigue and may lead to poorer performance. Alternatively, practice effects and individuals who have naturally better posture and balance (e.g. dancers, individuals who participate in yoga/Pilates) will likely lead to better scores. However, if pre-season baseline assessment scores are derived for each athlete then this likely will negate the above issues.
In support of the measure, there is a significant relationship between the Sensory Organization Test (SOT) (see below) and BESS scores which indicates that the BESS is a good substitute for the SOT on the sidelines. 4 Research also suggests that there is no significant relationship between LOC or PTA symptoms and performance on the BESS or other balance assessments, meaning that the tool can be used regardless of whether or not these symptoms are present or absent after concussion. 4 While this may therefore result in the identification of false positives (identifying concussion where there is none), it may be better to be “safe than sorry.” However, this is less useful in professional sports where an incorrect diagnosis means a player is removed from the game when he does not need to be.
SOT
The SOT also examines balance and posture, with the assistance of a technical force system to disrupt balance and orientation of the individual (see Table 2). 2 Similarly to the BESS, the SOT should also be administered at pre-season for an identification of baseline functioning 6 to avoid the influence of factors such as fatigue and individual differences in balance. The SOT has indicated moderate reliability in healthy individuals when assessing balance deficits 16 ; however, there is a lack of reliability and validity studies for its utility in concussion samples. 16 This highlights its questionable use for identification of sports-related concussion. Moreover, the practicality, accessibility, and associated costs of the measure are not ideal, and it is more likely to be used in research or hospitals, rather than on-field. 2 As such, the BESS is likely a more practical approach for the assessment of balance for sports-related concussion.
King-Devick Test (K-D)
Eye saccades have been noted as an indicator of neurological impairment following concussion, 17 and as such the King-Devick (K-D) test has been administered to athletes for injury assessment (see Table 2). The K-D test is quick, easy to administer, and carry, and does not require a medical professional for administration or scoring. 17 The measure has been utilized in Mixed Martial Arts (MMA) fighting athletes, hockey players, and rugby players, and was found to accurately reflect poor functioning after concussion, such that athletes with concussion had worse performance than baseline. 17 In collegiate football and basketball players, the K-D test also indicated that concussed athletes had longer performance times than non-concussed athletes. 17
However, when the K-D test was used to examine diagnostic validity among individuals with concussion in an emergency department, it was unable to predict group membership (concussion versus no concussion). 18 As such, the sensitivity of the K-D test is debatable, and while it is an efficient measurement tool, it may be influenced by factors such as vision-impairment, language, or fatigue, and would likely not identify individuals with post-concussive symptoms such as headache, nausea, and imbalance.
Standardized assessment of concussion
The standardized assessment of concussion (SAC) was developed in response to AAN practice parameter and Colorado guidelines 19 and was designed to tap into domains of function known to be sensitive to the effects of concussion. As such, evident in Table 2, the SAC examines attention, concentration, orientation, and memory 19 to document objectively the severity of neurocognitive dysfunction or impairment. 19 An initial examination of the utility of the SAC was implemented on football players, where performance on the SAC during practice and also games was compared, with all players who were injured during play assessed with the SAC immediately after. 20 The total SAC score was significantly lower for concussed players who were assessed immediately after injury, than for non-concussed individuals. 20 However, in this study, only six athletes had suspected concussion, and there was no validation conducted with another measurement of concussion to confirm diagnosis. In high school and college football athletes, measurements indicated that concussed players scored significantly lower than controls and performed significantly lower than their baseline measurements, and as such, the SAC was deemed sensitive in detecting individuals with concussion. 19 However, the sample size again was relatively small (33 with concussion, compared to over 500 without), and there was no cross-check with other concussion measures for validity.
Interesting to note is that concussed players scored significantly lower for orientation, immediate memory, concentration, and delayed recall assessments, even though there were no observable deficits, highlighting that an objective measure is necessary otherwise it is likely that athletes with concussion could go undetected and continue to play. 19 Moreover, the assessment can be used with examiners with no prior experience in psychometric testing 19 and is comprehensive yet efficient and accessible.
Sports concussion assessment tool
In developing a comprehensive sideline assessment of concussion, the sports concussion assessment tool (SCAT5) measures cognition, post-concussion symptoms, and balance in addition to other relevant qualitative information, by incorporating the BESS, SAC, and post-concussion checklist.21,22 It is the newest version of the tool following the SCAT3. Modifications in the most recent version include further clarification of assessment guidelines, additional words, and digit strings added to recall and memory tests, a rapid neurological screen, and more explicit information regarding RTP and school. 22 The symptom checklist has been noted as the most sensitive in identifying athletes with concussion, whereas the BESS and SAC are less sensitive. 21 It is noted that baseline or pre-season assessment is necessarily required, and that a comparison to a norm-based sample is just as useful. 21 Also, females tend to report more concussion symptoms at baseline than males, and that athletes with attention-deficit hyperactivity disorder or learning disorders have elevated test scores at baseline. 21 As such, group-based norms would be necessary for evaluating results. However, “healthcare professionals” are required to utilize this tool, which may be feasible in higher-ranked or professional sports, but this limits the utility in local games. Moreover, it is currently unclear what level of training is actually required for using the assessment.
The concussion recognition tool—fifth edition
The pocket concussion recognition tool—fifth edition (CRT5) 23 was developed following a revision of the Pocket SCAT2 which comprised of concussion symptoms, and brief assessment of memory and balance. 5 The Pocket CRT5 expanded the SCAT2 to include more information about symptoms and signs of concussion. 5 The tool is relatively new and not yet widely disseminated, 5 and as such, there is limited evidence for validity and reliability. 24 A benefit of the tool, however, is that it does not rely on medically trained practitioners to deliver the assessment to inform management of concussion, 5 which allows for wider use and accessibility for sporting teams, thereby eliminating limitations outlined above for the SCAT5.
Conclusions
Guidelines
Generally speaking, the AAN, 9 Cantu, 7 and Colorado 11 guidelines are reasonably consistent with regards to decisions about RTP based on grades of concussion severity. However, a number of issues remain suggesting further work is required to develop reliable, “gold standard” guidelines for the management of concussion in sports. For instance, there are disparities across guidelines in the terminology used, such as identifying whether an athlete has any “change in mental state” 9 versus “PTA,”7,11 and it is currently unclear what “transient” or “slight” confusion means or manifests as when assessing grade 1 concussions. With a lack of clear terminology across guidelines, and inevitably different examiners assessing the athlete’s functioning post-injury, it would be difficult to determine reliability and sensitivity of such procedures.
Further, issues remain within the guidelines themselves with regards to identification or diagnosis of concussion based on symptomatology. Across guidelines, some emphasis is placed on the length of LOC to determine grading of concussion and whether or not to RTP.7,9,11 This focus on LOC makes decisions regarding RTP difficult to apply in cases where no LOC is present, as an absence of LOC does not necessarily mean that no concussion has occurred. 25 Moreover, in some individuals, symptoms such as PTA may not be immediately evident, whereas the guidelines focus on short-term resolution of symptoms when making decisions about RTP. The definition of PTA in these guidelines is also unclear. For instance, if PTA is assessed by answering basic questions about the match, they are likely to answer confidently given the contextual information in the environment.
As such, albeit similar in nature, there remains to be subtle variances across the guidelines with regards to determining severity of concussion and decisions about RTP, based on combinations and duration of LOC, PTA/change in mental state and confusion or disorientation. As such, decision-making is difficult with regards to choosing which guidelines to follow to allow for best outcome and least risk of “catastrophic outcome” during play. As such, it would be preferable to have universal grading and decision-making system to allow for consistency. A universal grading system would also serve to increase the utility of sideline assessment measures so that it is clear which grading system they are to follow when making decisions about RTP.
Assessment measures
As is evident in Table 2 of this review, there are a number of strengths and weaknesses inherent in each assessment measure utilized for making decisions based on concussion identification and RTP. Postural stability and balance assessments are useful in that they are not reliant on concussion markers such as LOC and PTA to identify suspected concussion, which may result in a more sensitive means of assessment given that some athletes may not initially present with such symptoms. However, the SOT is not accessible for a sideline assessment tool, and the BESS may be influenced by a number of factors attributed to the individual (e.g. fatigue, pre-existing balance ability, leg injury) and to assessors (e.g. subjective nature of error scoring). Moreover, practical concerns may be raised with the utility of the BESS, including a lack of standardized information regarding the thickness or specific material of the foam used to examine balance. In line with this, while the K-D test may be quick and easy to administer, and has been effective in identifying concussion in MMA fighters and other athletes, 17 it may not be a reliable tool in visually impaired athletes or athletes with reading deficits, unless baseline assessments are conducted. Moreover, validation studies with hospital-based samples identified that the tool was unable to distinguish reliably between individuals with or without concussion. 18
As a whole, more comprehensive or holistic assessments of concussive symptomatology would be beneficial and more sensitive to identifying actual cases of concussion. The SAC 19 is accessible, quickly administered and can be utilized be assessors without training, while also assessing areas known to be affected by concussion (orientation, memory, and concentration). Further, the SCAT5 22 comprises the SAC and also the BESS and Brief Symptom Inventory, enabling assessment and examination across a wide range of function and impairment. Moreover, the CRT5 23 also covers a broad assessment across post-concussive symptoms, orientation, and memory, in line with the SCAT5. Additionally, there is a pocket version for accessibility and can be used by non-medical professionals. 22 These tools allow for the highest level of sensitivity in identifying athletes who have sustained a concussion, and also evaluate symptom severity which is indicated as the most closely associated with accurate classification of concussion. 21 However, the most recent versions of the assessment measures are yet to be widely disseminated and critiqued based on validity, reliability, and sensitivity, and as such, further research in concussive and non-concussive samples are required to evaluate their psychometric properties.
Another consideration to make is evidence of the utility of the measures across different groups, including in female athletes, younger children, or individuals where English is not their first language. Reliability and validity studies which assess the accuracy and efficacy of the above measures to identify concussion appear to focus on collegiate athletes with a predominance of male participants.6,17,19–21,26 There is little evidence of the validity and effectiveness of these measures for young children in sports, who are likely to perform very differently on each of the assessments than in older samples. Additionally, a number of the tools are reliant on the use of English verbal language,5,19,20,22 and it is unclear whether the utility of these tools in non-English samples has been examined.
Final considerations are regarding the utility of baseline assessments of function, which are required to compare any potential impairments following suspected concussion. Research mentions the term “sandbagging” to refer to athletes who purposefully do worse at baseline testing, so to increase their chance of continuing to play if concussion is based on repeated performance on the assessment measure.27,28 As such, an athlete who “fakes bad” or performs poorly at baseline, and performs at their optimal ability following injury, may have their concussion go undetected while they are able to RTP. 29 While one study has highlighted that faking may be difficult to accomplish successfully without the assessor noticing, 27 it should be considered that often during the completion of these assessments, there is pressure from the coach for that athlete to return to the game, and that inevitably sideline measures are associated with some reliance on subjective scoring. Moreover, it is currently unclear how are the measures are used for athletes with multiple concussions, particularly with reference to baseline functioning. It is well documented that multiple concussions can have cumulative effect on impairments and symptoms including poorer cognitive outcomes, more post-concussive symptomatology and prolonged recovery 30 ; however, a new baseline from assessment would be recorded each season, thereby potentially, the baseline level would be lower.
Overall conclusions
Overall, it is best practice to use assessment tools such as the SCAT5 or CRT5 which assess functioning across all suspected areas of impairment for accurate and sensitive identification of concussed athletes. However, validity and reliability studies are required for novel versions of the assessment tools, particularly in sub-groups such as females, young children, and non-English speaking individuals. Moreover, guidelines regarding grading of concussion severity and RTP should be consistent in terminology, and “best practice” could be to consult the Colorado Guidelines which present the most detailed management information. At this point, where there is a lack of clarity or uncertainty, the safest recommendation would be to remove that athlete from play, considering the often subtle effects of minor concussion which will likely continue to inhibit functioning, leaving the athlete vulnerable to further injury.
Regardless, the current guidelines and concussion assessment tools are advancing in terms of implementing procedures for the identification, assessment, and management of concussion in sports. It may also be useful to develop guidelines or education to provide to parents and families at pre-season, including information about the management of concussion and potential warning signs following injury.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
