Abstract
Background
Concussion patients who experience prolonged symptoms may benefit from evidence-based, physician-led, inter-disciplinary care. The success of this approach may depend on a patient’s understanding and adherence to a complex, multi-modal recovery process.
Objectives
We have developed a novel clinical care guide for post-injury concussion caretermed the “Treatment Passport,” intended to facilitate greater communication and understanding among patients, healthcare providers, family members, teachers, and coaches. This study aims to assess whether the Treatment Passport increases patients’ understanding of their concussion care in an inter-disciplinary setting.
Methods
Patients presenting with sports- or recreation-related concussions were randomly assigned to the intervention (
Results
The median age of participants was 20 (range 10–63). Participants in the intervention group showed significant increases in their understanding of inter-disciplinary concussion care when compared to control group members. This was reflected in a 2.1–2.8-fold greater understanding of the cognitive, physical, and vestibular aspects of their care. In addition, 86.7% of control group participants indicated they believed that the Treatment Passport would have helped with their concussion recovery journey.
Conclusion
The Treatment Passport is a novel clinical tool that facilitates the delivery of standardized inter-disciplinary concussion care by increasing patient-caregiver communication and understanding.
Keywords
Introduction
Concussion is a common clinical manifestation of sports-related injuries. 1 The highly variable symptomatic and prognostic nature of concussion presents unique challenges to healthcare providers looking to balance standard-of-care practice with personalized treatment solutions.2–5
While the majority of individuals diagnosed with concussion recover uneventfully within weeks of injury, many patients will experience persistent symptoms that can last months or years. 6 In addition, there is a risk of recurrence or worsening of symptoms when patients prematurely resume normal activities. 7 Patients suffering from prolonged post-concussion symptoms, including various physical, cognitive, and psychiatric co-morbidities, may benefit from a multi-faceted management and treatment approach. 8 Indeed, evidence-based concussion care provided through an inter-disciplinary facility or network of licensed allied healthcare professionals has received considerable attention and has been the driving force behind recent expert consensus guidelines.6,8–11
As guidelines for inter-disciplinary care evolve, the success of this approach will likely depend on a patient’s understanding and adherence to a complex, multi-modal recovery process. 12 Since members of the inter-disciplinary team may employ different styles and/or modes of communication, patients may be unable to understand the relationships among various aspects of their treatment plan. 13 In addition, the lack of standardized treatment plans within inter-disciplinary teams may widen communication gaps between patients and their healthcare providers. Surprisingly, few studies have evaluated the impact of patient understanding or engagement in the decision-making process of concussion care. Given the importance of shared understanding between patients and healthcare providers, 14 a standard-of-care approach that actively engages patients throughout their concussion treatment may facilitate better communication and provide clearer guidelines for the recovery process. 15
We have developed a clinical care guide, termed the “Treatment Passport,” that provides an educational, step-wise concussion management plan, clearly written and depicted via diagrams, for patients and healthcare providers in an inter-disciplinary setting. The Treatment Passport integrates contemporary expert consensus guidelines for concussion care into a personalized clinical practice tool. The tool is intended to engage, educate, and empower concussion patients through increased patient-caregiver communication and understanding. Here, we perform a pilot study to determine whether the Treatment Passport increases patients' understanding of their concussion care in an inter-disciplinary setting.
Methods
Design
This prospective pilot study was approved by the Royal Victoria Regional Health Centre Research Ethics Board (Study No.: R16-006) and conducted at Concussion North, a community-based, tertiary clinic that provides physician-led, inter-disciplinary care for sports- and exercise-related concussions.
Participants
Patients diagnosed with a concussion by a primary care or emergency room physician were referred to a single sports medicine physician at Concussion North for further assessment, diagnosis, and treatment. Concussion North is a tertiary sports injury and concussion center specializing in medical care and the rehabilitation of sports and exercise-related concussions. Patients referred to our center were introduced to the study at the time of their first concussion assessment consultation with the sports medicine physician. Details about the study, voluntary participation, and informed consent and assent were discussed with each patient, including the parents or legal guardians of children under the age of 16 years. Patients were eligible to participate in the study if they were 10 years of age or older and had sustained a sports- or recreation-related concussion. Patients were excluded from the study if they were unable to verbally communicate in English. Patients were sequentially enrolled, and a convenience sample of 33 participants was randomly assigned to the intervention (
Intervention: Treatment Passport
Both intervention and control groups received the same standard-of-care, derived from evidence-based clinical practice guidelines on concussion management and treatment.6,16–19 Concussion North operates as an inter-disciplinary clinic, and all study participants received ongoing written and verbal communication about their symptoms, treatments, and recovery from regulated healthcare providers, including physicians, physiotherapists, athletic therapists, occupational therapists, and neuro-optometrists.
Participants in the intervention group, but not the control group, received the 24-page color Treatment Passport upon providing written informed consent and assent. The Treatment Passport is a novel communication tool intended to guide concussion patients through the process of inter-disciplinary rehabilitation and recovery, using a step-wise clinical management plan clearly written and depicted via diagrams. The Treatment Passport was created by Dr. Shannon Bauman and her clinical team of rehabilitation specialists at Concussion North (MD, Physiotherapists, and Athletic Therapists). With the assistance of a graphic designer and word press editor, Dr. Bauman and her team created this communication tool to guide patients through the detailed care plans they receive during the medical and rehabilitation process at Concussion North. The Treatment Passport is comprised of the following sections (excluding front, back, and inside covers): (1) “Your Journey Starts Now” (Treatment Passport page 1), “Signs & Symptoms” (page 2), “When a Concussion is Suspected” (page 3), “Patient Information” (page 4), “Baseline Testing” (page 5), “ImPACT® Test Post-Injury” (page 6), “Features Of My Concussion” (page 7), “My Concussion Journey” (pages 8–9), “Cognitive Journey: Return To Learn/Earn” (pages 10–11), “Physical Journey: Return To Play” (pages 12–13), “Vestibular Journey” (page 14–15; (Supplementary Figure 1)), “ImPACT® Test Post Injury” (page 16), “Clearance For A Safe Return” (pages 17–18), and “Notes” (pages 19–20). The authors have included ImPACT® in their guide as this was the test being administered at Concussion North at the time of the study; alternative neuro-psychological tests have been validated and may be used by other centers.
Participants in the intervention group reviewed and completed the Treatment Passport together with their circle-of-care providers as they progressed through the treatment program at Concussion North. As the Treatment Passport asks for identifying information (e.g. Name, Date of Birth, Address, Sport, Level, and Position), it was decided for the purposes of this pilot study, each Treatment Passport would be securely locked between appointments at Concussion North (i.e. patients were not permitted to take the Treatment Passport home) to minimize the risk of exposing patient and study information.
Survey
At a four-week follow-up appointment with the sports medicine physician, participants in both groups completed a paper-based, 11-question, 5-level Likert scale survey to evaluate their overall satisfaction and understanding of their ailment, treatment plan, and continued care approach (Table 1). Survey questions were developed through consultation with professional colleagues to assess patients’ understanding of their inter-disciplinary treatment journey. Each participant responded to 1 of 5 levels of agreement or disagreement for each question: “Strongly Disagree,” “Disagree,” “Neutral,” “Agree,” and “Strongly Agree.” Participants in the control group were shown the Concussion North Treatment Passport upon completion of the survey and asked one additional question to evaluate their perceptions of the possible benefits of the intervention by means of a “Yes” or “No” response.
Survey questions.

Control group respondents only.
Statistics
Survey data were coded to capture statistically relevant outcomes. Nonparametric, two-tailed Mann–Whitney U tests were used to identify significant differences in Likert scale responses between intervention and control groups. Independent t-tests and Chi-squared test were used to assess all other statistical outcomes. All analyses were conducted using Graphpad Prism 4.0 (San Diego, CA) and statistical significance set at p < 0.05.
Results
A total of 33 individuals (22 females and 11 males) were sequentially enrolled in the study. The median age of the intervention group was 23 (range: 13–63), and control group was 18 (range: 13–57). Patient demographics and concussion characteristics are provided in Table 2. There were no significant differences in age, gender, number of previous concussions, baseline or final Post Concussion Symptom Score, or duration of treatment between intervention and control groups (data not shown).
Patient demographics and concussion characteristics.
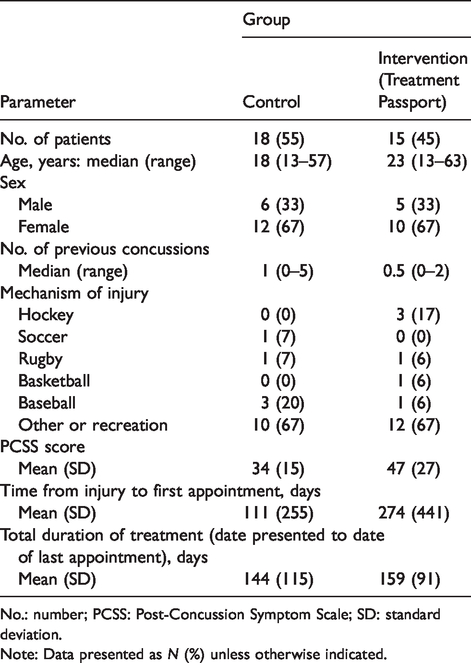
No.: number; PCSS: Post-Concussion Symptom Scale; SD: standard deviation.
Note: Data presented as
For each survey question, the Likert scores from the intervention (
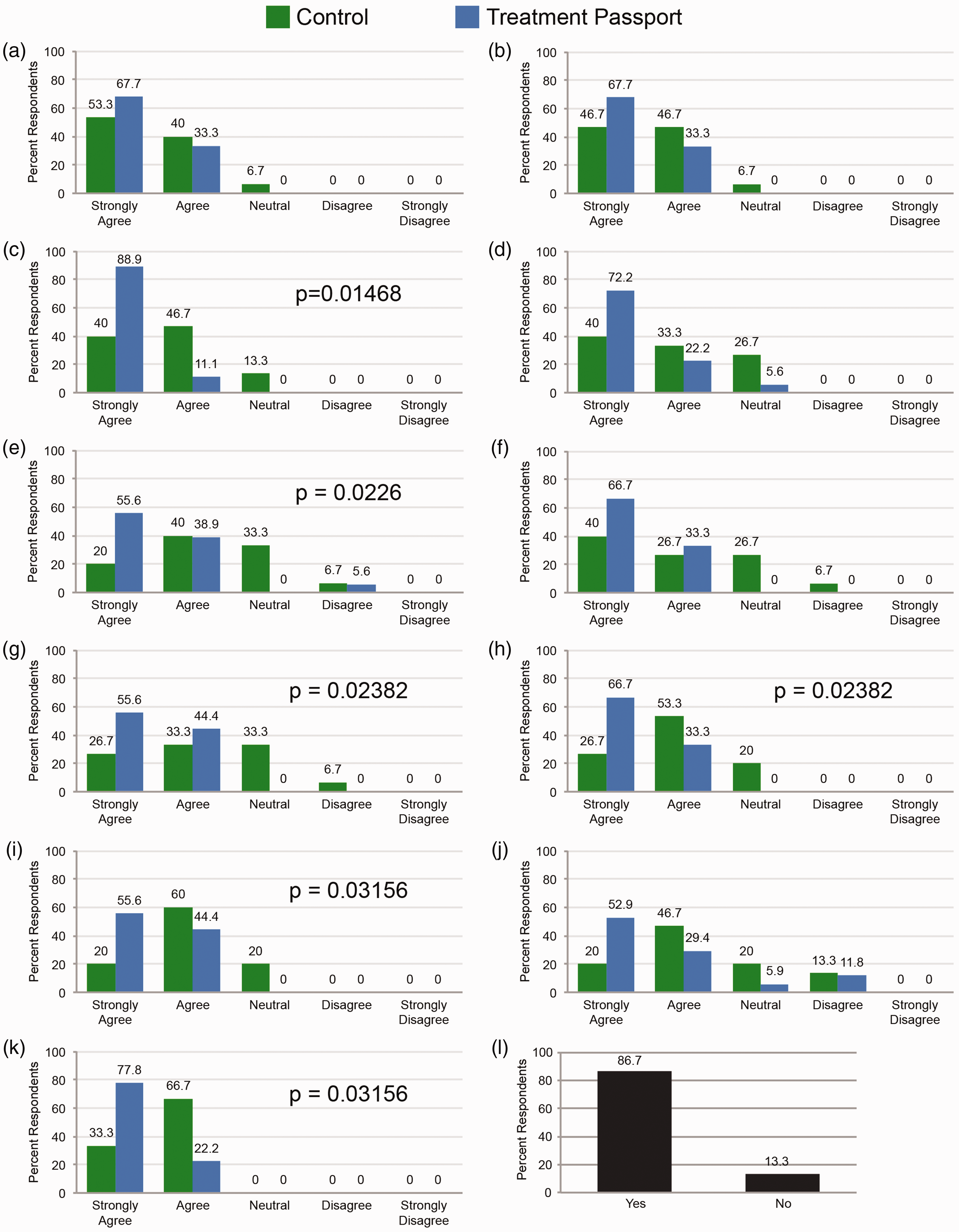
For each question, individual Likert scale responses are presented as a percentage of total respondents (a–k). A non-parametric, two-tailed Mann–Whitney U test identified significant (p < 0.05) differences in 6 of 11 survey questions between intervention (blue) and control groups (green). Participants using the Treatment Passport showed significant increases in their understanding of concussion care for Survey Questions c, e, g, h, i, and k (indicated by p value). Percent respondents from control group indicating that they believed the Treatment Passport would have helped with their concussion recovery journey (l).
Discussion
The mainstay of post-injury concussion care has historically focused on rest, with the expectation that symptoms would recover naturally, thus allowing a gradual return to regular activities. Recently, however, there has been a shift in concussion management to improve outcomes through a more active recovery approach involving physician-led, inter-disciplinary rehabilitation teams, each with expertise in different aspects of concussion care.17–19 In particular, neurocognitive testing, cervical and vestibular rehabilitation, and subthreshold Return-to-Learn and Return-to-Play protocols have been identified as key components in post-injury concussion care that may be effectively delivered by an inter-disciplinary team. 6 As new standards are adopted to support inter-disciplinary approaches to concussion care, 20 patient confusion may arise as a result of their interactions with multiple treatment providers and the added challenge of understanding the role that each provider plays in their recovery process. 21 An effective communication strategy between patients and each member of the inter-disciplinary team may help patients better understand their own clearance parameters and expected recovery timelines as well as facilitate better communication between patients and their families, teachers, coaches, employers, and other stakeholders in recovery. Here, we have shown that the Treatment Passport increases patients’ understanding of the cognitive, physical, and vestibular aspects of their care. Moreover, patients in the control group identified the Treatment Passport as a potentially useful tool in their own care, suggesting that all patients recognize the importance of communicating treatment plans through visual means.
A significant challenge in concussion care management can be the delivery of high quality care to every patient due to the highly variable symptomatic, prognostic, and demographic characteristics of concussion. The Treatment Passport is a novel concussion clinical care guide that may be used by inter-disciplinary teams to help every patient better understand multi-modal assessment, rehabilitation, and recovery processes of their concussion care. This is accomplished by facilitating stronger patient-provider interactions through the visualization of a patient’s post-concussion care journey, including step-wise progressions (“stages”) through each rehabilitative aspect as well as identifying the endpoints required for final clearance. These clearly defined goals allow patients to track their progress, contextualize their level of recovery, and remain actively involved in a multi-modal rehabilitation plan that culminates in their full medical recovery. The Treatment Passport further enables patients to self-advocate for their level of recovery by ensuring their healthcare providers adhere to best practice criteria for safe and complete recovery.
Current guidelines define “recovery” or “clearance” as when a patient is asymptomatic with daily activities, has returned successfully to school and/or work without requiring modifications, or has progressed through a return-to-play protocol without symptoms of concussion.22 Thus, recovery is strongly based on a patient’s own subjective assessment of both symptom resolution and readiness to return to school, work, or pre-contact level of sport or exercise. A study by Ellis et al.8 has recommended that additional objective evaluations, such as neurocognitive tests and treadmill testing, help guide clinical decisions regarding recovery. To our knowledge, the current study is the first to utilize and integrate multi-modal cognitive, physical, and vestibular performance measures to facilitate an objective determination of recovery criteria. The Treatment Passport communicates these criteria and includes a check list to be completed by physicians as part of a comprehensive medical clearance from concussion. It is of note that while “Vision” was included as a “Features of My Concussion,” in the current study, the Treatment Passport has since been revised to include “Vision” as an additional recovery journey, highlighting the potential for the Treatment Passport to evolve as evidence-based practice changes.
While we recognize that our small sample size may have limited our statistical power to identify other relevant outcomes, such as duration of treatment between intervention and control groups, we are currently planning a multi-center study utilizing a web-based digital platform for the Treatment Passport. It is anticipated that a digital version of the Treatment Passport will allow for further customization of the rehabilitation journeys (e.g. sport specific progressions for different types of athletes) and the ability to identify other relevant clinical outcomes as the tool is adopted in different clinical settings. Furthermore, a larger, multi-center study will provide the opportunity to study additional outcomes, such as determining if the use of the Treatment Passport can shorten treatment duration and reduce recovery time after injury for individuals after a concussion. Ultimately, it is our hope that the Treatment Passport may be used not only to engage, educate, and empower patients in their concussion journey, but to provide patients, healthcare providers, family members, teachers, and coaches an integrated communication tool to better understand evolving best practices.
Supplemental Material
CCN886192 Supplemetal Material1 - Supplemental material for A novel clinical practice tool increases patients’ understanding of concussion care within an inter-disciplinary clinic
Supplemental material, CCN886192 Supplemetal Material1 for A novel clinical practice tool increases patients’ understanding of concussion care within an inter-disciplinary clinic by Shannon M Bauman, Julie MacDonald, Carolyn Glatt, Iveta Doktor-Inglis and Jesse McLean in Journal of Concussion
Supplemental Material
CCN886192 Supplemetal Material2 - Supplemental material for A novel clinical practice tool increases patients’ understanding of concussion care within an inter-disciplinary clinic
Supplemental material, CCN886192 Supplemetal Material2 for A novel clinical practice tool increases patients’ understanding of concussion care within an inter-disciplinary clinic by Shannon M Bauman, Julie MacDonald, Carolyn Glatt, Iveta Doktor-Inglis and Jesse McLean in Journal of Concussion
Footnotes
Authors’ note
For access to the full version of the “Treatment Passport” referenced in this manuscript contact the primary author Dr. Shannon M.Bauman. The Treatment Passport (also known as the Concussion North Treatment Passport) is a registered copyright of Concussion North Ltd.
Acknowledgements
We thank Dr. Carrie Esopenko (Rutgers University, Newark, NJ) for helpful discussions and Ms. Karen Pollock (Concussion North, Barrie, ON) for excellent administrative assistance. The authors thank the RVH Foundation for supporting this research.
Authors’ contribution
SMB, JMD, CG, ID, and JM participated sufficiently in the work to take responsibility for the content, and that all those who qualify are listed. Substantial contributions to the conception or design of the work: SMB, JMD, CG, ID, JM; Acquisition, analysis, or interpretation of data for the work: SMB, JMD, JM; Drafting the work or revising it critically for important intellectual content: SMB, JMD, JM; SMB, JMD, CG, ID, and JM accept final approval of the version to be published; AND agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Shannon M.Bauman is the Medical Director of Concussion North and is an independent contractor with no competing interests to this research. Concussion North is independently owned by an immediate family member of Dr. Shannon M.Bauman. Julie MacDonald is employed by Concussion North as a clinician with no competing interests with respect to this research. Carolyn Glatt and Iveta Doktor-Inglis are independent contractors of Concussion North and declare no competing interests.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors thank the RVH Foundation for supporting this research.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
