Abstract
Nursing students commonly engage in clinical education in municipal elderly healthcare. Therefore, it is important to use a pedagogical model that provides the best conditions for nursing students to develop clinical competence. The aim of this study was to describe and interpret nurse preceptors’ experiences of a newly implemented pedagogical model, peer learning, in municipal elderly care home settings. Nine registered nurses from elderly care homes with precepting experience participated. Data were collected through individual interviews, and a thematic content analysis was performed. The study followed the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist. The findings revealed four sub-themes: ‘requiring careful preparation’; ‘contributing control and trust in the learning process’; ‘changing perspectives brings new opportunities and challenges’; and ‘enabling students to believe in themselves’, all interpreted into the main theme of ‘demanding yet supportive and developing’. In conclusion, municipal elderly care homes seemed to be a learning environment well suited for using the peer learning pedagogical model.
Introduction
Clinical education for nursing students needs to be adapted to the knowledge, skills, and competencies required of registered nurses (RNs). In Sweden, healthcare is provided by both regions and municipalities, which means that clinical education for nursing students is also conducted in municipal elderly healthcare facilities, elderly care homes, and home healthcare. Therefore, it is crucial to implement high-quality pedagogical models in these settings.
Nursing care is complex, and the quality depends heavily on the competence of RNs. RNs require the ability to integrate theoretical knowledge and understanding of practical skills, which in turn shape their professional skills. The environment in elderly care homes is challenging 1 and is experienced by nursing students as both complex and diverse.2,3 A literature review 4 describes that nursing students perceive that clinical education in elderly care homes will not contribute significantly to the skills and competencies essential for their future professional practice. This emphasizes the significance of sufficient professional supervision to enable students to connect with the responsibilities associated with the role of a RN in an elderly care home setting. Consequently, enhancing the quality of student learning and professional development in elderly care homes is crucial. 1 Therefore, the choice of pedagogical models for nursing students during clinical education in elderly care homes is of great importance.
Peer learning (PL) is a goal-oriented, student-centered, active learning pedagogical model. 5 The model can be used in both theoretical and clinical education, based on the premise that learning involves social cognition and that experiences, understanding, and knowledge building are shaped by interactions between people. 6 Key concepts in PL are collaboration, support, reflection, critical thinking, and feedback.5,7 PL gives students the opportunity to integrate theory and practice in activities, reflect together, and give and receive feedback regarding patient situations they have experienced. In clinical education, nursing students who participate in PL pair up to discuss and learn from each other 8 and to develop their knowledge and skills. 9 Therefore, the PL pedagogical model differs from traditional models in nursing education, which are based on a ‘preceptor-learning system’, where the quality depends on the preceptor's competence. 10 In PL, learning is student-centered, which means that students actively participate and take responsibility for their own learning. 5 In traditional models, the preceptor is familiar with the routines and culture of the work, and their role is to instruct and demonstrate, while the student constantly follows them in their daily work, thus engaging in a more passive learning process. 11 Using PL stimulates collaboration with peers and the ability to communicate, reflect, and engage in critical thinking. One advantage of using PL is that it contributes to friendship 12 and emotional support 13 between students, which encourages learning from and supporting one other. Other benefits are that students develop independence in their eventual profession as RNs14–16 and that they assume responsibility for their own learning.16,17 In the traditional model, students may have to compete for the preceptor's time in order to develop their leadership skills and collaborate with other staff. This competition has been linked to students’ comparing themselves with one another, which can lead to an awareness of their own learning needs. 7 PL, on the other hand, saves time for the preceptor, sparing them from feeling inadequate and stressed by precepting two students at the same time. 16 In the PL model, a challenge for preceptors may be stepping back to wait for the student to act, 6 or when a group of peers is not at the same level of knowledge, it feels that they are competing in a negative way for care recipients and tasks or are not receiving sufficient individual guidance. 8 PL also entails giving systematic feedback on strengths and ongoing learning needs. In this model, the preceptor has a kind of mentoring role. 16
It is well known that the ageing population is increasing and therefore it is important to provide nursing students with good conditions to gain the skills necessary to meet the healthcare needs of the aging population. As described in the background, clinical education at elderly care homes can provide crucial learning opportunities for the professional development of nursing students. However, a common perception among nursing students is that elderly care home settings will not contribute to the skills and competencies required for their future practice. Therefore, it is important to use high-quality pedagogical models to support nursing students in developing knowledge and professional growth as well as understanding the educational significance of clinical education within elderly care homes. The findings of this study can help develop and improve the use of PL in elderly care homes, thereby increasing the quality of clinical education for nursing students. A review of the literature reveals a lack of studies on the use of PL in municipal elderly care homes from the perspective of preceptors. Thus, the aim of this study was to describe and interpret nurse preceptors’ experiences of a newly implemented PL pedagogical model in municipal elderly care home settings.
Methods
This study adopted a qualitative approach, which enables the investigation of lived experiences. 18 The study is based on nine individual interviews that were subjected to thematic content analysis following Graneheim et al. 19 and Lindgren et al. 20 The study was conducted and reported using the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist. 21
Setting
The study was conducted in elderly care homes in a municipality in northern Sweden, which had a population of approximately 80,000 inhabitants. In this municipality, the PL model had recently been implemented in the clinical education of nursing students in municipal elderly care homes. Before the implementation, RNs who served as preceptors for nursing students were provided with information and training sessions on the PL model. The nursing program included a course in their fourth semester, which involved 5 weeks of clinical education in elderly care homes where peer learning was utilized. In addition to focusing on ethical approaches to relationships and actions, the nursing process, nursing interventions and techniques, and drug treatment, the curriculum also aimed to develop students’ independence and their ability to collaborate with other professionals. Various structured learning activities were included in the clinical education. For instance, students identify specific problems or potential problems in at least two patients by conducting risk assessments according to a national quality register. Another activity involves participating in a knowledge base about palliative care that applies to nursing homes. This is done to better prepare nursing students to care for patients at the end of life.
The term ‘preceptor’ is used to refer to RNs who guide and mentor nursing students in their clinical education. These preceptors engage in teaching, providing feedback, and reflecting on current issues together with the students.
Participants and procedure
The participants were chosen using a purposive criterion-based sampling strategy. The inclusion criteria were as follows; RNs working in elderly care homes, who had experience with both precepting with PL and the traditional models. The age range of the RNs was 28–60 years and they had worked as RNs for 4–20 years. They were recruited with an email invitation that conveyed information about the study and included a reply form to provide informed consent. A contact person from the municipality assisted in the recruitment process. They presented information about the study during a workplace meeting providing both written information and response forms. Nine RNs agreed to participate by returning the reply form via email along with their signed informed consent to participate.
Interviews
Semi-structured individual interviews were conducted with the RNs using an interview guide with open-ended questions, which allowed the RNs to talk freely about their experiences. The interviews began with the open question, ‘Tell me about your experiences of precepting with PL in elderly care homes’. Follow-up questions were asked to encourage the participants to tell more, such as ‘Can you give an example?’ or ‘Can you tell me more?’ Three interviews were performed in person and six by telephone. The interviews lasted 24 −40 min and were digitally recorded and transcribed verbatim.
Analysis
The analysis was performed using a thematic content analysis, following the guidelines of Graneheim et al. 19 and Lindgren et al. 20 Each interview was read several times to gain a sense of the content. Thereafter, units of meaning were selected that corresponded to the aim of the study. No data were excluded from the interviews. The units of meaning were then condensed and labeled with a code describing the content. Next, codes with similar content were sorted into sub-themes by making an abstraction and interpretation of the content, which finally led to four sub-themes. According to Graneheim et al. 19 the analysis can be performed by moving directly from codes to sub-themes, with increasing degrees of abstraction and interpretation. The four sub-themes were interpreted into a main theme, that is, an interpretation that ties the sub-themes together by the common thread underlying its message. 19
Ethical considerations
The study followed the ethical principles of the Helsinki Declaration. 22 All ethical standards, informed consent and right to withdraw were upheld. Before involvement, participants were informed, both orally and in writing, about the study and reassured that their participation was voluntary and that they could withdraw from the study at any time before the data collection was completed. Participants were assured confidentiality and an anonymized presentation of the findings. According to existing Swedish law on the ethical review of human research, no ethical review was required. Nonetheless, ethical guidelines and rules were considered for good measure to prevent harm or risk throughout the research process.
Findings
The findings revealed four sub-themes and one main theme. An overview of the findings is presented in Table 1.
Overview of sub-themes and main theme constructed from the analysis of the interviews.
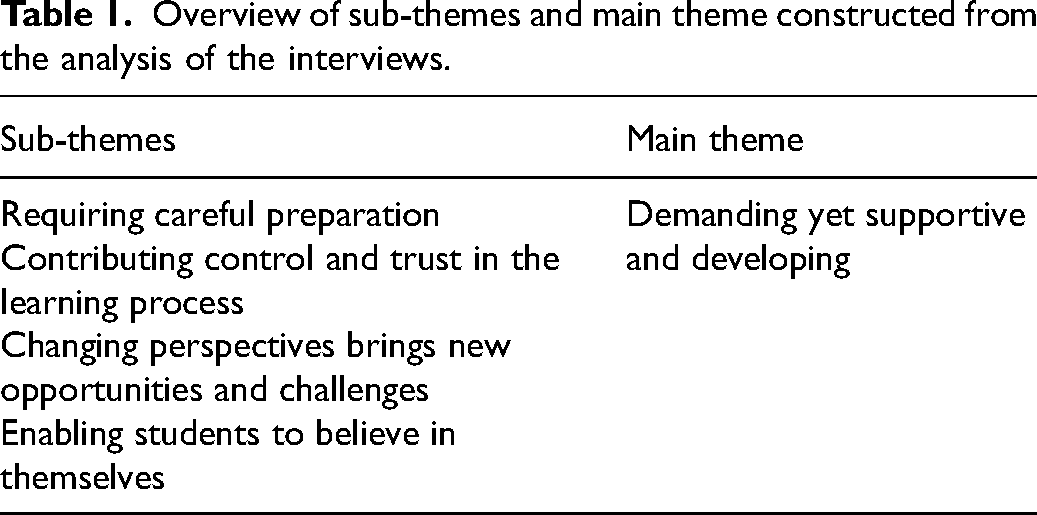
Demanding yet supportive and developing
There seemed to be an incongruence in the use of PL for nursing education in municipal elderly care homes, while PL could be seen as a challenge, it also gave preceptors a sense of security. In other words, the use of PL was demanding yet supportive and developing for those in the role of preceptor. Furthermore, preceptors considered PL to be time- and energy-consuming, but also rewarding and fun, depending on their own attitudes towards PL. Preceptors emphasized the importance of being flexible when using PL in elderly care homes, which was sometimes seen as a challenge. They shared that PL could be demanding due to the uncertainty of precepting in a new way, working with two students simultaneously instead of one.
Requiring careful preparation
Preceptors described the importance of being well prepared before the peers arrived for clinical education in municipal elderly care homes. One reason to prepare carefully was that the preceptors had a lot of initial work to do with the students. They reported that being prepared led to a clearer and better structure for themselves and, more importantly, for the peers, since they could establish a more secure learning environment. To offer good support, they stressed the importance of planning time set aside to work with the peers initially and plan the clinical education. Preceptors shared that it was important to plan for the students to have access to computers and a workspace where they could discuss and reflect together. They stressed that a lack of space in their work environment, manifested as too few computers, confined office space, and high noise levels, could create disorder and complicate precepting. Having several nurses share their workplace in the same room had a negative influence. The space in our office is small, which means that both students cannot be there at the same time if my colleague also has students. My colleague, the students, and I are disrupted by the fact that we are sitting in the same room at the same time. (Interview 5) It would be an advantage if the university made sure to pair them up so that they know each other and that they work well together. (Interview 1)
Contributing control and trust in the learning process
Preceptors in elderly care homes described how, at the beginning of the day, they informed and planned the work together with the peer, which created control in their role as preceptor and established a trusting relationship with the student. Equally important, this practice helped to remove any uncertainty and insecurity for the students.
The interviews also revealed that the conditions in elderly care homes afforded an effective pedagogy in the learning process. In this setting, students are able to have the same preceptor and the same patients during clinical practice, which preceptors believed gave a sense of security to both the student and themselves. Some of them stated that this was the first time they were using PL, and therefore more experience was needed, but the first impression was positive. One of the preceptors said, ‘Peer learning is the melody for the future’. Based on the organization, there is no problem with using the model and it gives structure in the precepting, but I think it would have been more difficult if it had been in a medical department because there is no time for reflection. (Interview 1) It's good that they are two of them in case if I have explained poorly or we have misunderstood each other, which increases my confidence that my information is coming across. (Interview 9)
Changing perspectives brings new opportunities and challenges
Since the PL model is a new way of precepting, preceptors reported that they needed to change their approach. Despite the advantages of PL, they shared that it was not easy to change the way they think and precept because traditional models are so ingrained. It was a difficult transition from precepting one student to two students at the same time, and it took more time, especially at the beginning. On the other hand, using PL also freed up time for the preceptor because the student peers worked together independently.
Some were initially skeptical about using PL but changed their minds after trying the model. It was important for them to develop the pedagogical approach. Ultimately, they described that it was fun to use PL. It also seemed to reduce stress by enabling preceptors to keep up with administrative tasks when the students were working independently with their peers. Preceptors also thought it was important to have an open mind about this new model. They expressed that PL took a lot of energy and involvement, but at the same time it was perceived as an exciting challenge. Some considered it scary and burdensome, especially when students were on different levels in terms of knowledge, which required greater flexibility from the preceptor. In addition, when the peers were not compatible, when one of them took more initiative or when problems arose between the students, preceptors had to exercise a flexible and creative attitude. Regardless, other preceptors maintained that it was not more difficult to precept two students instead of one. When there is a big difference between the students, both students become more insecure; at the same time, the student who takes on more can push on the student who is more withdrawn. (Interview 2) I can only recommend the model; I see nothing negative with it. If there is good personal chemistry between the students, and good cooperation with the management [in their own organization], it is a great tool. (Interview 1) Sometimes, I miss being able to check off with colleagues about how it worked, which is a difference in PL within a municipality in comparison with care in hospital. (Interview 7) The structured activities gave a wider picture not only of what is done but also how to do it based on ethical aspects that could be discussed. (Interview 8)
Enabling students to believe in themselves
All preceptors highlighted that the use of PL in precepting nursing students in elderly care homes equipped students for their future profession as RNs. An advantage was that the peers could ask questions, discuss, and reflect together, which contributed to a sense of security and knowledge development during their clinical education. Preceptors gradually allowed students both in peer groups and individually to take on increasing responsibility, which preceptors said developed students’ independence, self-confidence, and responsibility. Using PL in municipal elderly care nursing was deemed more suitable than in hospital care, because the students had more opportunities to learn from each other, develop independently, and practice collaborating with others for their future as RNs. Other benefits of using PL in a municipal healthcare setting compared with other caring organizations were that students had more time to develop their problem-solving abilities with each other, take on responsibilities, and cooperate with other professionals. The students have the opportunity to perform clinical education quite independently in elderly care homes based on the knowledge they have to date. (Interview 5) They [students] feel secure that they have meaningful activities to do and I need not be present all the time. They do it themselves, take initiative, and are more responsible for their own learning. (Interview 9) When we have time with the students, and they have more time to be near the patients, it implies that they learn a lot. (Interview 6) There are good opportunities within the municipality for the students, such as having time to do their assignments parallel to their practice and get to know their patients, because it is not the same stressful environment as it can be in hospital care. (Interview 3)
Discussion
The aim of this study was to describe and interpret nurse preceptors’ experiences of a newly implemented PL pedagogical model in municipal elderly care homes. The sub-themes and main theme presented a picture of implementing and using PL in municipal elderly care homes that seemed to be supportive for preceptors, but simultaneously challenging and demanding.
The findings of the present study show that using PL in elderly care homes requires preparation before students arrive, which seemed to lead to a clear and better structure in the learning process. This is in line with a study 23 performed in primary healthcare that describes that planning and structure are necessary to ensure quality in the learning process. Another study 3 found that information, teaching, and skill training from the university prepared students better than the clinical placement. This indicates how important a close collaboration between the university and the clinical placement is. In our findings, preceptors believed that elderly care homes allowed more time for reflection, both for the student peers and for the preceptors and students together, than in other caring organizations. One reason for this could be that the management gives preceptors time to give feedback and reflect with the students. 23 Therefore, it is equally important that the management and the nearest chief have knowledge about the PL model and understands its benefit so that they can provide the right conditions for using the model.
Our findings show a lack of physical space for reflection, conversation, and feedback between the students and preceptors. This is consistent with a study conducted in a primary healthcare setting, 23 which found that a lack of physical space and access to computers negatively affected students’ learning process in clinical education. Equally important as the physical space is the learning space for preceptors to pay attention to the students and to the caring attitude, as well as to understand what is happening within the peer group. 24 This shows that using PL is a complex pedagogical process, which, in addition to the above factors, involves planning, adapting to the student's level, applying precepting strategies, and evaluating and assessing students’ knowledge and skills. 25 Despite these challenges, all preceptors in our study agreed that the use of PL in municipal elderly care homes helped develop nursing students for their future profession. This corresponds with a study 26 in a geriatric hospital setting. The study shows that PL with close interaction between patients and staff can create authenticity, ultimately enhancing the professional development of nursing students. The complexity that characterizes elderly care homes offers students to develop a range of nursing skills, encompassing both fundamental and specialized aspects, throughout their clinical education. 3 Studies2,3,27 show that clinical education in elderly care homes provides essential learning opportunities crucial for the professional development of student nurses. Strategies recognized for fostering positive learning experiences for nursing students in elderly care homes involve establishing a robust partnership between academia and nursing homes, delivering thorough student orientation, encouraging positive supervision encounters, and assisting staff in their educational responsibilities. 28
The findings of our study highlight the importance of support from management, colleagues, and the clinical teacher as a significant factor in the use of PL. This is in line with a previous study 29 that pointed out the importance of preceptors receiving support from nurse managers and their colleagues. Another study 30 showed that preceptors desire and need concrete tools and teaching strategies to handle challenges, such as more knowledge and understanding of their role, for instance what responsibilities they have, as well as knowledge of new methods to be more flexible as a preceptor. A study 31 showed how preceptors developed their precepting after completing a preparation course. In that study, before the course, they described a lack of sufficient preconditions, while after they had ways of creating the necessary preconditions. Before, they described the process as teaching, and after, as a learning process for students. This can be interpreted as a sign of understanding and development in their role as preceptors using PL.
The findings of our study indicate that using PL contributes to control and trust in the learning process, which builds a trusting relationship with the students. This is in line with a study 32 performed in a psychiatric setting where preceptors emphasized the importance of developing a trustful relationship with the students. According to Hilli and Sandvik, 33 a caring and supportive relationship is essential to the process of learning and development for nursing students. Trust can be developed over time by creating a relationship between students and preceptors. Frøiland 1 highlighted that this relationship is of utmost importance in influencing a student's learning environment. A literature review 34 exploring student nurses’ learning experience in clinical settings found that nursing students learn best in environments that encourage collaborative learning, trust, and mutual respect, and that a good relationship between student and nurse positively influences the learning experience. Another study 2 showed that nursing students experience nursing homes as a complex and diverse learning arena. However, a significant prerequisite is an interpersonal linkage between the preceptor, nursing student, and patient24,35 that is built on respect towards each other, thus enabling beneficial and supportive interactions. This can lead to deeper relationships with each other 24 and can make preceptors feel more safe and secure. 35 Therefore, it is important that the preceptor and the student have access to a physical space in which to communicate, as well as a trusting relationship to conduct the various components of PL in municipal elderly care homes.
The clinical learning environment plays a factor in students’ learning. One of the criteria of a supportive learning environment is that the students are encouraged to be independent in their learning and are advised to be self-reliant. 34 The learning environment appears to be impacted by the setting in which care is provided. A study 36 conducted in an intensive care unit revealed that preceptors found using PL to be time-consuming. The amount of time they could devote to students depended on the severity of the patient's illness. This highlights the need to adapt the learning outcomes to ensure that nursing students can attain them in the current care setting.
The findings of our study also show that reflection was important, both for the peer groups and together with the preceptor. In previous research, nursing students have reported that reflecting together leads to a sense of responsibility for each other. 37 According to Cooke et al., 4 critical reflection is imperative in developing clinical learning. Knutsson et al. 37 stated that having time for reflection sessions is important to connecting theory to practice and promoting deep learning. Ekebergh 38 argued that reflection facilitates the transformation process during nursing education. Another study 1 highlighted the importance of reflective dialogues and clinical discussions between the preceptor and the students, which revealed students’ theoretical knowledge and helped students to integrate theory and practice. Based on the current findings, the conclusion can be drawn that PL within elderly care homes allows students more time for reflection compared to hospital care.
Our findings show that preceptors strived to change their approach to PL, which brought opportunities but also was challenging. Therefore, preceptors need support in their role when using PL, both from the university and their own colleagues. This is in line with results from a study 39 that found that a good learning environment for nursing students in clinical placements depends on engagement and collaboration between preceptors and university teachers. Husebø 40 found that clinical education in nursing homes is ideal for nursing students to develop nursing competencies and to grow into their new role as a nurse. Furthermore, a good start to the clinical placement depends on a well-prepared nursing home management and staff, who are knowledgeable of the nursing curriculum, educational strategies, and learning goals and who are ready to welcome the students as an asset in nursing older patients. Our findings also show that preceptors wanted to have more information and support. In relation, a study 41 found that mentoring education increased preceptors’ competence in supporting students’ learning processes.
Our findings indicate that preceptors consider elderly care homes to be a well suited, safe, and secure learning environment for nursing students. Beyond the benefits mentioned in our findings, the use of PL has also been found to challenge students’ knowledge in their own learning, encourage critical thinking, and integrate clinical and academic skills, 6 which can be seen as a step towards enhancing their own independence as RNs.
The learning space provided by PL in elderly care homes seems to develop students’ responsibility and cooperation with other professions more independently compared with students who perform clinical education in other caring organizations, such as hospital care. This could be seen as a step towards enabling them to enhance their self-confidence, which in turn develops their self-efficacy as eventual RNs.14,42 Self-efficacy beliefs contribute significantly to human motivation and achievement 43 and relate to a person's belief in their own capacity to achieve a goal in a specific situation. Self-efficacy also positively influences a person's effort and persistence in a situation. 44 Thus, in precepting nursing students, it is important to have effective strategies for strengthening students’ self-efficacy. According to our findings, preceptors believed that using PL in elderly care homes developed students’ ability to become RNs. A high-quality work-based education for nursing students can bring about a sense of self-efficacy, which can be seen as a key component for acting independently and competently as an RN.45,46 In addition, a strong sense of self-efficacy and job satisfaction seem crucial to reducing exhaustion among nursing professions.47,48 Using PL as a pedagogical model for nursing students can provide conditions to increase their competence and independence in their profession. This indicates that self-efficacy could be an indicator for predicting nursing students’ performance in clinical education. Our findings show that collaboration with the university throughout their clinical education was important, in terms of both support and communication between the two parties. High self-efficacy among students has been associated with obtaining higher goals than in students with low self-efficacy. 49 On the other hand, a weak relationship between the university and elderly care homes can adversely influence students’ self-efficacy.39,42 Further, using PL has been found to improve students’ self-efficacy to a greater degree than traditional models.14,50
Methodological considerations
The trustworthiness of this study was assessed according to the aspects of credibility, dependability, confirmability, and transferability. 19 To establish credibility, we focused on analyzing the data without incorporating our personal interpretations, while striving to faithfully portray the preceptors’ experiences. The analysis was conducted by both researchers together, and we discussed our interpretations to reach agreement on the themes. Incorporating representative quotations from the preceptors enhanced both credibility and authenticity. The study was carried out utilizing a comparatively small sample size, a characteristic that could be perceived as a constraint. Nevertheless, the chosen sample size aligned well with the study's objectives. The interviews generated extensive and valuable data. It became evident that data saturation was reached when no new patterns or codes could be identified. What emerged from the data was recurrent and recognizable, indicating a well-suited sample size.19,51 In order to establish dependability, the study's design, methodology, data collection, and analysis were comprehensively detailed. The confirmability was strengthened by both researchers’ extensive experience as RNs, including precepting nursing students, as well as numerous years as senior lecturers within the nursing program. This can also be seen as a limitation; however, we were aware of our pre-understanding throughout the whole research process and strived to use it as a strength. We have clearly outlined the analysis process and made concerted efforts to maintain neutrality, minimizing the potential for biasing the data. In order to enhance transferability, we included comprehensive descriptions and verbatim quotes within the results section.
Conclusion
In summary, the findings of the present study clarify that PL is a suitable pedagogical model to use in an elderly care home setting. Preceptors in municipal elderly care homes reported an overall positive experience using PL. The use of PL was supportive for preceptors but simultaneously challenging and demanding. To prevent and manage challenges that may arise, careful preparation and planning for the nursing students’ clinical education are important. The use of PL in municipal elderly care homes seems to create control and a trusting relationship in the learning process, which in turn can strengthen students’ self-efficacy and provide the conditions for them to become skilled in their eventual profession as RNs.
Other advantages emerged in the use of PL in municipal elderly care homes, including better structure in the role as preceptor, more time to reflect and the opportunity for students to perform tasks independently. Not enough physical space was available, which can impair the learning space and in turn negatively affect the interpersonal linkage between the student and the preceptor. Support in the role as preceptor was considered crucial for the quality of precepting with PL in municipal elderly care homes. Therefore, it is important that preceptors and the university have good communication and that preceptors are offered education and support from the university. Altogether, municipal elderly care homes seemed to be a well-suited learning environment for using PL.
Footnotes
Acknowledgments
The authors want to thank the supervisors for their contribution to this study.
Author contributions
Study design: CN and BL. Data collection: CN. Data analysis and manuscript preparation: CN and BL.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: CN received financial support for the research from the Swedish Nurses’ Association.
