Abstract
Introduction
Wrist hand orthoses are widely used in rehabilitation to improve hand function and alleviate pain. However, their use may restrict wrist motion, causing functional disabilities in activities of daily living (ADLs). This study aimed to evaluate the effects of wrist hand orthoses on upper limb activity during daily life, focusing on differences between padded fiberglass and thermoplastic wrist hand orthoses.
Methods
35 healthy, right-handed adults wore two types of wrist hand orthoses (padded fiberglass and thermoplastic) for 24 h during daily activities. Upper limb activity was measured using accelerometers, while ADL difficulties were evaluated using the Hand20 questionnaire. Activity levels were compared across no-orthosis, fiberglass, and thermoplastic orthosis conditions.
Results
Both wrist hand orthoses significantly reduced upper limb activity (magnitude ratio and use ratio) compared to the no-orthosis condition (p < 0.05). The Hand20 scores indicated greater ADL difficulties under both orthotic conditions, with no significant difference between the two types of orthoses (p > 0.05).
Conclusions
Wrist hand orthoses restrict wrist and forearm motions, reduce upper limb activity, and increase perceived ADL difficulties. No significant differences were observed between fiberglass and thermoplastic orthoses, suggesting comparable effects on daily life. Design modifications can improve user comfort and functionality.
Keywords
Introduction
Wrist hand orthoses are widely used to manage various musculoskeletal and neurological conditions. Their functions vary and may include immobilizing the wrist to improve joint alignment, alleviate pain, and support functional tasks. In the context of rehabilitation, some orthoses are also designed to assist wrist motion to encourage upper limb use during activities of daily living (ADL).1–3 For instance, in cases of wrist drop due to radial nerve palsy, an orthosis supporting wrist extension can facilitate hand use in daily activities. However, even assistive orthoses may impose unnecessary restrictions on wrist or forearm movement depending on their design, potentially leading to functional limitations during ADL and subsequent discontinuation of orthosis use. 4 Therefore, it is crucial to develop and apply wrist hand orthoses that provide the necessary support while minimizing interference with upper limb function in daily life.
Stern and Aranceta-Garza et al.5,6 examined the efficacy and functionality of various commercially available wrist hand orthoses with different shapes and materials, and reported substantial variation in performance across orthosis types. These findings highlight that orthotic design and material characteristics can influence functional outcomes, underscoring the importance of selecting appropriate orthoses for daily use. This underscores the significance of orthosis design and materials in determining functional performance, a topic of interest both domestically and internationally. In Japan, two primary types of wrist hand orthoses are commonly used in rehabilitation: padded fiberglass and thermoplastic wrist hand orthoses. Padded fiberglass wrist hand orthoses are advantageous due to their low cost, high strength, and ease of application. However, they are heavy, poorly ventilated, and less water resistant. In contrast, thermoplastic wrist hand orthoses are lightweight, highly water-resistant, and offer additional benefits. Regarding design, the distal side of padded fiberglass wrist hand orthoses is typically positioned proximally to the thumb palmophalangeal crease, whereas thermoplastic wrist hand orthoses are positioned proximal to the thenar crease. This difference may make thumb opposition more challenging with padded fiberglass wrist hand orthoses, leading to the assumption that thermoplastic wrist hand orthoses interfere less with upper limb use in daily life. However, a previous study 7 reported that in tasks requiring fine motor skills, such as pinch movements, fiberglass wrist hand orthosis posed greater restrictions compared to thermoplastic wrist hand orthoses, while thermoplastic wrist hand orthoses hindered simulated ADL tasks. These findings suggest that the functional impact of wrist hand orthoses varies depending on the task, indicating that no single orthosis is universally suitable for all activities.
Nevertheless, most previous studies have focused on specific tasks or controlled environments, leaving the overall impact of wrist hand orthoses on daily life insufficiently understood. Notably, no comparative studies have been conducted to determine which wrist hand orthosis imposes fewer restrictions on daily life.
Based on these considerations, this study aimed to clarify the impact of wrist hand orthosis use on daily life by evaluating upper limb activity levels as a key indicator. In addition, since upper limb use may vary between seating and standing postures in daily life, this study also explored the posture-specific effects of wrist hand orthosis use as a secondary outcome.
Methods
Ethical considerations
This study was approved by the Ethics Committee of the institution to which the authors belong (approval no. 21-43). Before participation, all participants were provided with a detailed explanation of the study, and written informed consent was obtained. This study was conducted in accordance with the principles of the Declaration of Helsinki.
Participants
The participants were 35 healthy adults (12 males and 23 females, mean age: 20.3 ± 0.5 years) with no history of musculoskeletal disorders, all of whom were right-handed. Participants were recruited through university bulletin boards. All participants were undergraduate students who reported no limitations in daily upper limb use, and none of them dropped out of the study. The study was conducted between September and November 2021. Hand dominance was determined using the Japanese version of the FLANDERS handedness questionnaire, 8 which consists of 10 questions scored on a three-point scale. The sample size was calculated using power analysis with G*Power 3.1, assuming a medium effect size (f = 0.25) based on Cohen’s conventional criteria due to the absence of prior studies with directly comparable experimental conditions. The significance level was set at 0.05, and the statistical power at 0.8.
Wrist hand orthoses
Two types of wrist hand orthoses, fiberglass and thermoplastic, were fabricated for the dominant hand (Figures 1 and 2). To ensure a uniform design, an occupational therapist with over 10 years of hand therapy experience fabricated all orthoses following specific guidelines. Participants were instructed to wear the orthoses continuously, excluding bathing, for 24 h starting the day before data collection, while performing daily activities as usual. A padded fiberglass wrist hand orthosis before fixing (a), after fixing (b). A thermoplastic wrist hand orthosis before fixing (a), after fixing (b).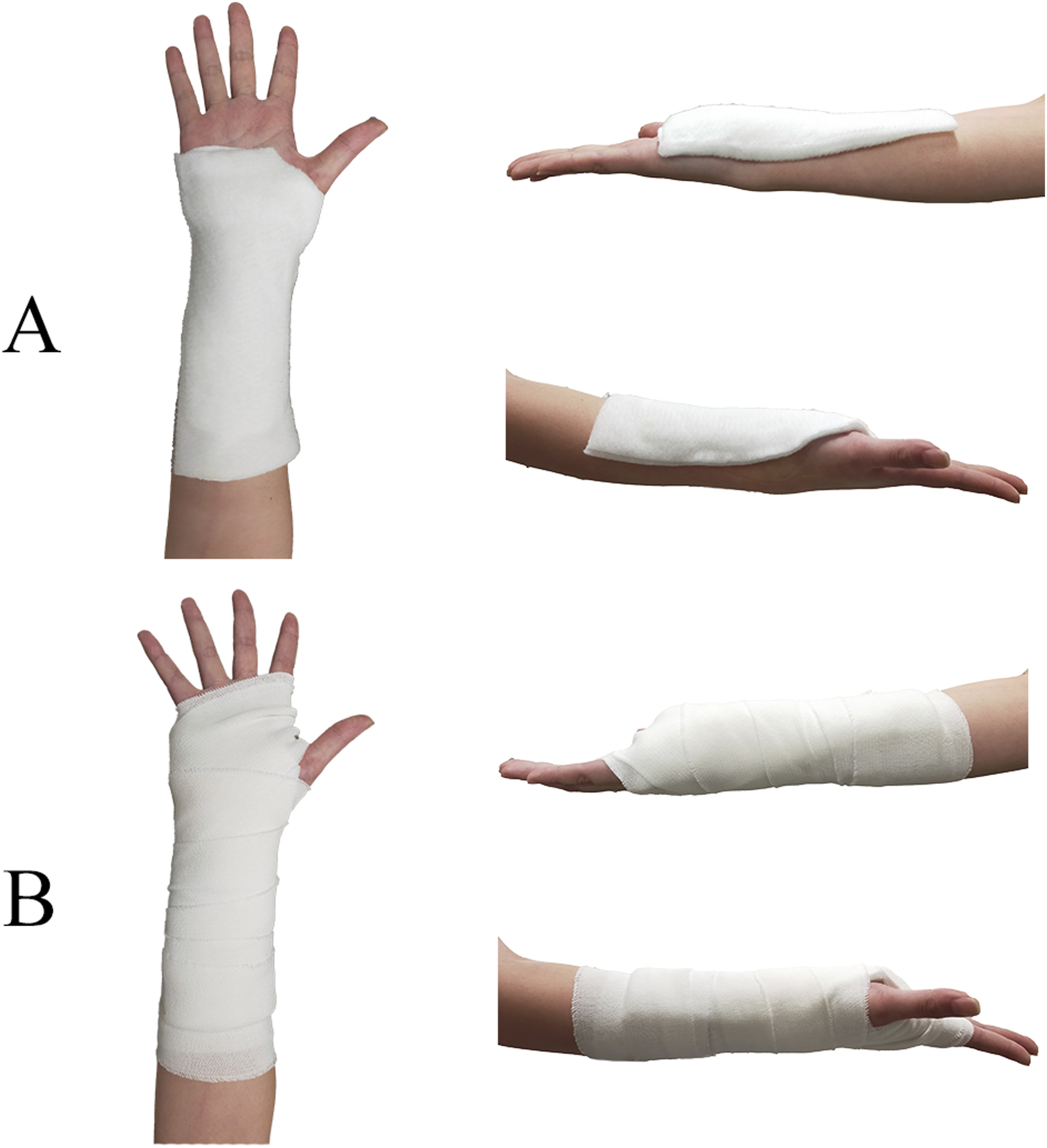

The padded fiberglass wrist hand orthosis was fabricated using ORTHOGLASS® II (BSN Medical Luxembourg, Luxembourg) with the forearm in a neutral position. ORTHOGLASS® II consists of fiberglass coated with hydraulic resin and covered with a non-woven pad. The orthosis covered 2/3 of the forearm proximally, with the distal end 5 mm proximal to the line connecting the radial end of the thenar crease and the ulnar end of the distal transverse palmar crease, and 5 mm proximal to the thumb palmophalangeal crease. The orthosis was secured and fully covered with an elastic bandage.
The thermoplastic wrist hand orthosis was fabricated from a 3.2-mm thick nonsticky solid Taylor orthosis (Smith & Nephew Rolyan Inc., Germantown, WI, USA) with the forearm in a neutral position and matching the front of the forearm. The orthosis also covered 2/3 of the forearm proximally, with the distal end positioned 5 mm proximal to the line connecting the radial end of the thenar crease and the ulnar end of the distal transverse palmar and thenar creases. The orthosis was secured at 2/3 of the palm, wrist joint, and proximal to the metacarpophalangeal joint using a 2.5-cm Velcro hook and loop.
To ensure conformity, the first author used visual inspection and a goniometer to verify that the wrist extension angle was 10°, the orthotic material did not cover the metacarpophalangeal joints of the index to little fingers, and it covered 2/3 of the forearm length, encompassing half its circumference. No pain was reported during the period the participants wore the orthoses.
Experimental procedure
Baseline data were collected from all participants under the no-orthosis condition. Specifically, upper limb activity during daily activities was assessed, and the participants also recorded their activity history. ADL difficulties were also evaluated. Measurements were then obtained while wearing the padded fiberglass and thermoplastic wrist hand orthoses using the same assessment items as in the no-orthosis condition. The testing order was randomized, with a minimum interval of 1 day between conditions to prevent carryover effects. This interval was determined by the authors to be sufficient because each orthosis was worn for only 24 h. Moreover, since the participants were healthy young adults without upper limb impairments, it was considered unlikely that short-term use of the orthoses would result in persistent physical or behavioral changes that could influence subsequent measurements.
Measurements
Upper limb activity during daily activities was assessed, and the participants recorded their activity history for each measurement day. ADL difficulties were also evaluated.
Upper limb activity levels were measured using ActiGraph GT9X-BT accelerometers (ActiGraph, LLC) secured to both wrists with wristbands. Simultaneously, a wGT3X-BT accelerometer (ActiGraph, LLC) was affixed to the right thigh with a belt to measure lower limb activity. 9 Measurements were conducted continuously for 24 h, excluding bathing. Data were sampled at 30 Hz and recorded across three axes (X-axis, Y-axis, Z-axis). Data were processed using ActiLife software (Version 6.0, ActiGraph) and converted to 1 Hz. Vector Magnitude (VM), defined as the square root of the sum of the squares of the three axes, was used to quantify activity intensity. Based on previous research, VM values ≥2 were considered to indicate functional activity, which was defined as a movement or action that helps to accomplish a task (e.g., grasping a can or wiping a tabletop) or has some function, although it does not accomplish a task (e.g., touching the face or moving the arm from one position to another). 10
Movement intensity (Magnitude Ratio) and movement time (Use Ratio) were computed for upper limb data as described in prior research. 11 The magnitude ratio quantified each limb’s contribution to daily activities on a second-by-second basis. For each second, the natural logarithm of the VM of the non-dominant (or affected) limb divided by that of the dominant (or non-affected) limb was calculated. Values >7 and < −7 were replaced with 7 and -7, respectively, to categorize single limb movement. Median values across all epochs were used due to the non-normal distribution of Magnitude Ratio values, confirmed by Kolmogorov–Smirnov tests. A value of 0 indicated equal activity in both limbs; positive values reflected dominant-hand preference, while negative values indicated non-dominant-hand preference.
The use ratio quantified the usage time ratio of each limb, reflecting limb usage balance in daily life. Movement time, defined as the total time with VM ≥2, was summed for both limbs. The dominant limb’s movement time was then divided by that of the non-dominant limb to calculate the use ratio. A value of one indicated equal movement proportions; values >1 indicated dominant-limb dominance, while values <1 indicated non-dominant-limb dominance.
Both the magnitude ratio and use ratio are calculated based on the relative activity between the dominant and non-dominant limbs within each individual. As such, they are inherently normalized and are not influenced by differences in total activity levels or specific daily routines. This allows for meaningful comparisons across participants despite the variability in absolute activity or lifestyle.
Lower limb data were analyzed using an inclinometer to classify postures as standing or seated/lying on a per-second basis.
For activity history, participants logged their daily activities (e.g., eating and cooking) over 3 days, and the percentage of time spent on each activity was calculated.
ADL difficulty was assessed using the Hand20 questionnaire, 12 which includes 20 items evaluating upper limb functional limitations. Items 1–18, focusing on ADLs, were scored on an 11-point Likert scale (0 = no limitation, 10 = impossible). The total scores ranged from 0 to 100, with higher scores indicating greater difficulty. For questions related to upper limb use (Items 1–15, 17, and 18), participants provided explanations if their responses were not 0.
Statistical analyses
Magnitude and Use Ratios were analyzed separately for standing and seated/lying postures. For each posture category, the no-orthosis, padded fiberglass orthosis, and thermoplastic orthosis conditions were compared using Holm-adjusted multiple comparisons. Hand20 scores were similarly analyzed across conditions. Activity history data were compared using chi-square tests. The normality of the data was assessed using the Shapiro-Wilk test. Statistical significance was set at p < 0.05.
Results
Vector magnitude.

Data are shown as median (interquartile range).
Magnitude ratio.

Data are shown as median (interquartile range).
A value of 0 indicated equal movement between both limbs; positive values indicated dominant hand preference and negative values indicated non-dominant hand preference.
Use ratio.

Data are shown as median (interquartile range).
A value of one indicated that both upper limbs moved at the same proportion, while a value >1 indicated dominance of the dominant limb’s movement, and a value <1 indicated dominance of the non-dominant limb’s movement.
Hand20 score.

Data are shown as median (interquartile range).
No significant differences were observed in activity history across the three conditions (p > 0.05).
Discussion
This study investigated the impact of wrist hand orthosis use on upper limb activity during daily life. In the no-orthosis condition, both the Magnitude Ratio and Use Ratio were significantly higher for the right (dominant) hand, indicating that right-handed individuals predominantly use their dominant hand during daily activities. This finding aligns with that of a previous study 13 showing that right-handed adults tend to favor their dominant hand in seated and standing tasks.
In contrast, under wrist hand orthosis conditions, the Magnitude and Use Ratios were significantly lower compared to the no-orthosis condition. No significant differences in activity history were observed among the three conditions, suggesting that the participants maintained consistent daily activity patterns across all conditions. These results suggest that the observed changes in the Magnitude and Use Ratios resulted from wearing wrist hand orthoses rather than variations in daily behavior. It can be inferred that wearing a wrist hand orthosis on the dominant hand reduced both the intensity and duration of its movement.
Franko et al. 4 reported that orthoses restricting wrist motion exacerbate functional disability in simulated ADL tasks and patient-reported outcomes, highlighting the impact of wrist motion restrictions on ADL performance. Similarly, this study found higher Hand20 scores under both orthosis conditions, indicating that participants perceived wrist hand orthoses as impeding ADL tasks. These findings suggest that wrist hand orthoses restrict wrist movement, reducing upper limb use in daily life and hindering ADL performance.
This study also focused on upper limb usage in seated and standing postures. Previous research 14 suggests that individuals use different hands for operating and holding a mobile phone when seated, while using the same hand for both tasks when standing. Seated activities, such as eating or desk work, generally require more upper limb use than standing activities. The degree of functional disability caused by wrist hand orthoses may vary depending on the specific movement, 5 necessitating posture-specific evaluations.
No significant differences in the Magnitude Ratio or Use Ratio were observed between the padded fiberglass and thermoplastic wrist hand orthoses, nor were posture-related effects detected. Similarly, no significant differences in Hand20 scores were found between the two orthoses, indicating comparable daily life impairments. While thermoplastic orthoses are lightweight and water-resistant, potentially reducing fatigue and facilitating water-related tasks, the padded fiberglass orthosis may have introduced psychological burdens, as participants continued tasks despite fatigue or were cautious to avoid getting it wet. However, these psychological influences did not significantly affect upper limb activity. The distal design of the thermoplastic wrist hand orthosis, located proximal to the thenar crease, facilitates thumb opposition more effectively than the padded fiberglass wrist hand orthosis, the distal end of which covers the carpometacarpal joint. However, Hand20 scores revealed that participants primarily reported wrist and forearm motion limitations rather than thumb movement. This suggests that the advantages of thumb opposition in thermoplastic wrist hand orthosis had little impact on movement intensity or time. These findings indicate that material and distal design differences between padded fiberglass and thermoplastic wrist hand orthoses do not significantly affect upper limb activity.
Functional limitations of the upper limb are influenced not only by wrist motion restrictions but also by forearm movement constraints. For conditions such as wrist drop or carpal tunnel syndrome, which do not require restrictions on non-wrist joints, minimizing motion restrictions on other joints could reduce the impact on upper limb use in daily life. Thermoplastic orthoses also offer practical advantages, such as ease of removal and suitability for water-related tasks, which were not evaluated in this study. Future research should consider these practical aspects to develop user-friendly wrist hand orthoses for everyday life.
It should be noted that wrist hand orthoses are often used to intentionally restrict wrist motion for therapeutic or protective reasons, such as pain reduction or joint stabilization. Therefore, the observed decrease in upper limb use and increased perceived ADL difficulty in this study should not be considered to indicate poor orthotic design. Rather, these findings highlight the trade-off between mechanical restriction and functional usability, even in healthy individuals, and suggest the need for context-specific design considerations in clinical settings.
Limitations
This study had several limitations. First, the participants were healthy young adults within a narrow age range and without upper limb impairment, which limits the generalizability of the findings to older populations or individuals with upper limb dysfunction. Second, each condition was assessed over a single day, and longer assessment periods may have yielded more reliable data. Moreover, although a 1-day interval between conditions minimized carryover effects and enhanced feasibility, it may have been insufficient as a washout period. Wearing unfamiliar orthoses continuously for 24 h could have caused discomfort or subtle changes in hand function, potentially influencing participants’ performance on the following day. Future studies should consider including longer washout or adaptation periods to better reflect real-world usage patterns. Third, subjective evaluations, such as user comfort and the psychological effects of wearing wrist hand orthoses, were not addressed. Future research should explore how wrist hand orthoses influence subjective experiences, including discomfort and psychological stress, and their impact on upper limb activity.
Footnotes
Ethical considerations
This study was conducted with the approval of the Ethics Review Committee of Kawasaki University of Medical Welfare [approval number: 21-43]. This study was conducted according to the principles of the Declaration of Helsinki.
Contributorship
JH conceived the study. JH and KI developed the statistical analysis plan and conducted the statistical analyses. MY contributed to the interpretation of the results. JH drafted the original manuscript. KI supervised the study. All authors reviewed the manuscript draft and revised it critically for intellectual content. All authors approved the final version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is supported by the Grants-in-Aid for Scientific Research of Japan Society for the Promotion of Science, Grant Number JP19K19627.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Guarantor
JH
