Abstract
Background
Blockchain is increasingly explored as an infrastructure to mitigate data fragmentation, security incidents, and limited patient control in digital health ecosystems. This systematic review analyzed applications of blockchain in smart health systems, with a focus on security models, interoperability approaches, and integration with Internet of Things (IoT) and artificial intelligence (AI).
Methods
Following PRISMA 2020, PubMed, IEEE Xplore, ScienceDirect, Springer, and Google Scholar were searched for studies published between January 2019 and August 2025 using a predefined strategy combining the terms (“blockchain” OR “distributed ledger”) AND (“healthcare” OR “medical” OR “health records”) AND (“security” OR “privacy” OR “interoperability”); of the 1847 records screened, 26 studies met the eligibility criteria.
Results
Across these studies, blockchain most consistently strengthened electronic health record management by providing cryptographic access control, tamper-evident and immutable audit trails, and support for cross-institutional data exchange. In four multi-institutional settings, coupling blockchain with AI enabled privacy-preserving federated learning for collaborative diagnostics without centralized data pooling. However, several technical and regulatory constraints were reported, including limited scalability (median throughput
Conclusion
Overall, the evidence indicates that blockchain is a credible enabler of secure, interoperable, and patient-governed health data sharing, provided that future deployments incorporate Layer-2 or comparable scalability mechanisms, adopt energy-efficient consensus protocols, and operate within clearer regulatory guidance on the permanence of clinical data.
Keywords
Introduction
Smart health is the use of Internet of Things (IoT), artificial intelligence (AI), and blockchain in healthcare to make care more personalized, accurate, and efficient. AI helps analyze large clinical datasets to support diagnosis, treatment planning, and early detection. Blockchain supports this by protecting patient data, ensuring data integrity, and enabling secure sharing of records across hospitals.1,2
Smart health helps tackle key problems in today’s healthcare, such as poor resource use and rising costs. 3 By enabling real-time analytics and better coordination among providers, it improves efficiency and gives patients more control over their care. 4 As healthcare continues to go digital, smart health becomes a core driver of holistic, value based care and will remain central to the future of medicine. 4
Overview of blockchain
Blockchain is a decentralized, distributed ledger that keeps data secure, transparent, and tamper resistant through consensus. Although it was first created for cryptocurrencies, it has since become a flexible technology used in many areas, including healthcare. Its core features are immutability, decentralization, and strong cryptographic protection.5,6
In healthcare, blockchain helps solve major problems in data management and interoperability. Conventional systems often struggle with fragmented patient records, limited data sharing, and risks of unauthorized access or breaches. 6 With blockchain, every action is stored as a block linked to the previous one, creating a secure, auditable chain that is transparent to authorized users and resistant to tampering. 7
The decentralized nature of blockchain ensures that no single party controls the data, which builds trust among all stakeholders. 8 Smart contracts further extend this by enabling automatic execution of tasks, processing insurance claims, or managing patient consent for data sharing. 9
Blockchain’s cryptographic mechanisms protect patient privacy while still allowing secure data sharing among providers and researchers. As healthcare continues its digital shift, blockchain is emerging as a key enabler of secure, transparent, and efficient smart health systems.7,10
Smart health leverages IoT, AI, and blockchain technologies to deliver personalized, accurate, and efficient care. IoT enables real-time data collection, AI analyzes clinical datasets for diagnosis and prediction, and blockchain secures data through decentralized, tamper resistant infrastructure. These technologies work synergistically to address fragmented data management, security vulnerabilities, and limited patient control, key challenges in modern healthcare.1,2 The following subsection details blockchain’s specific role, with Table 1 providing a comparative overview of all three technologies.
Comparison of IoT, AI, and blockchain technologies in smart health systems.
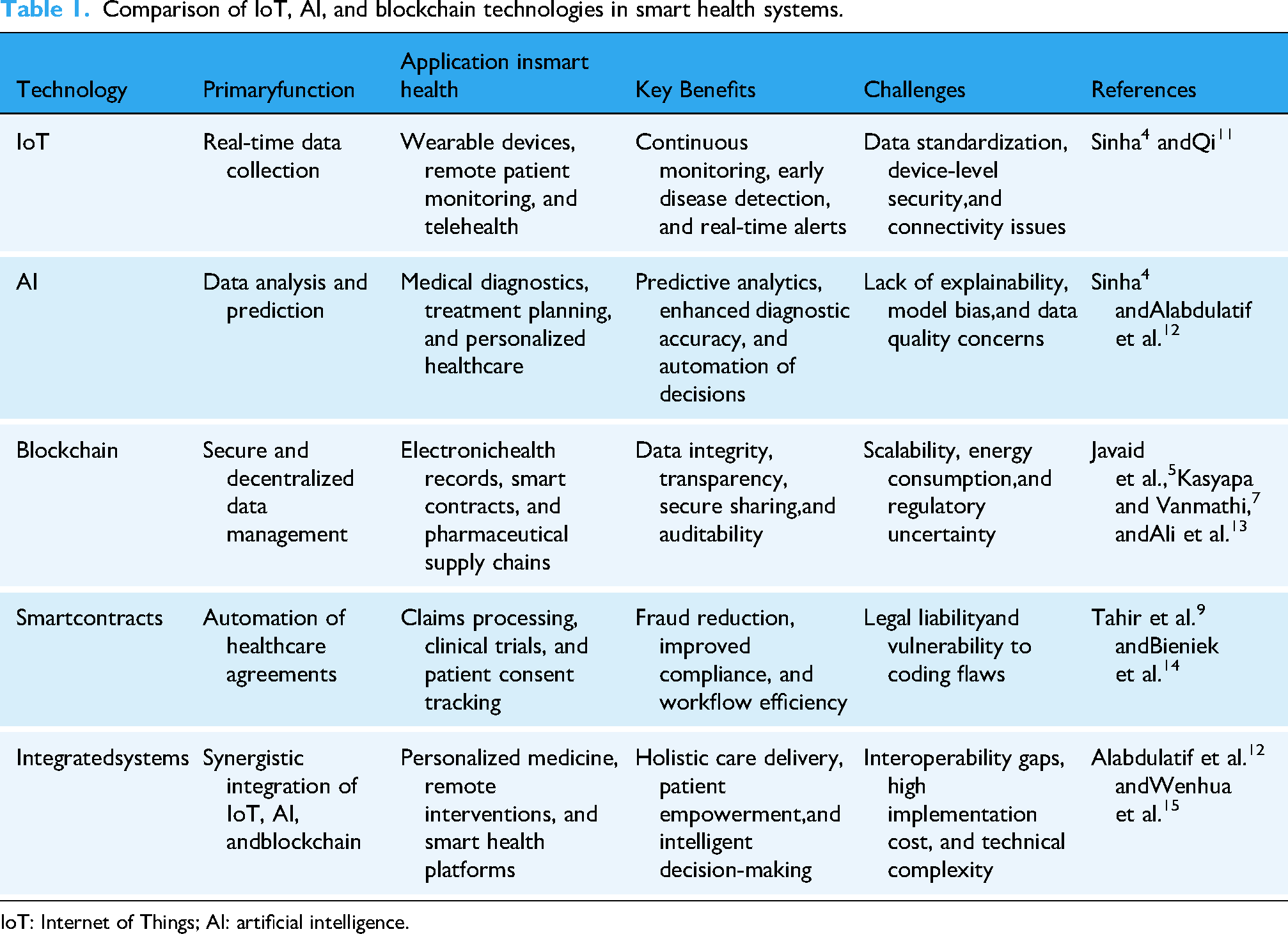
IoT: Internet of Things; AI: artificial intelligence.
Blockchain in smart health
Blockchain is becoming a solid building block for smart health systems because it helps keep data secure, makes different systems talk to each other, and gives patients more control over their information. One of the most useful parts is secure electronic health record (EHR) management, where patients can decide who sees their medical data and when.16,17
It also works well with IoT devices and wearables, so health data from things like glucose monitors or fitness trackers can be shared in real time to support long-term disease management and more personalized care. 14 Smart contracts add another layer of efficiency by automating routine processes like insurance claims, so approvals and payments can be handled automatically and transparently without manual steps. 18
On the operations side, blockchain can track medical products across the supply chain, which helps reduce counterfeits, fraud, and delivery errors. 19 Even so, using blockchain in healthcare is not straightforward. It still faces practical issues like limited scalability, high energy use in some implementations, and the need to meet strict healthcare regulations. 13 Integrating AI and machine learning (ML) can help here, especially for managing large volumes of health data, improving performance, and enabling intelligent decision support on top of blockchain-based platforms. 12
If these hurdles are addressed, blockchain can support safer, more efficient, and more patient centered healthcare systems.
Table 1 shows the different roles of IoT, AI, and blockchain technologies in smart healthcare systems. The table also compares their key benefits and challenges, offering a detailed overview of their integration potential in healthcare innovation.
Scope and purpose of this review
This review aims to provide a concise and structured overview of current blockchain applications in smart health systems, highlighting what has been accomplished to date. It examines how blockchain can enhance data security and privacy, improve interoperability among diverse healthcare platforms, and streamline routine clinical and administrative workflows for greater efficiency and trust.
The review is written for researchers, system designers, health IT teams, policymakers, and others who want to understand how blockchain can be used in healthcare and what problems it can actually solve. It should help readers see where blockchain already fits in healthcare, where it is still difficult to apply, and what directions future work can take.
Table 2 presents the key features and contributions of this review organized into seven thematic columns. The “Comprehensive coverage” column corresponds to the “Introduction,” “Methodology,” and“Overview of blockchain in healthcare” sections, covering the smart health ecosystem and blockchain overview. “Blockchain integration with AI and IoT” maps to the “Security issues in blockchain for smart health systems” section’s advancement discussions. “Security and privacy analysis” relates to the “Advancement in smart health systems” section’s detailed security evaluation. “Interoperability and decentralization” connects to challenges discussed in the “Challenges and limitations” section. “Scalability and regulatory compliance” addresses limitations covered in the “Challenges and limitations” section. “Real-world case studies” refers to practical implementations discussed throughout the “Introduction,” “Methodology,” “Overview of blockchain in healthcare,” “Advancement in smart health systems,” and “Security issues in blockchain for smart health systems” sections. Finally, “Structured future research directions” corresponds to the “Future directions and recommendations” section’s recommendations. Each row within these columns details specific applications, methodologies, or frameworks that demonstrate these contributions.
Key features and contributions of this blockchain-enabled smart health review.

IoT: Internet of Things; AI: artificial intelligence; EHRs: electronic health records; GDPR: General Data Protection Regulation; HIPAA: Health Insurance Portability and Accountability Act.
Focus areas
This review is structured around the following thematic objectives related to the adoption of blockchain in healthcare:
To assess the use of blockchain for strengthening EHRs, clinical decision and disease prediction systems, remote patient monitoring, and the integration of data from IoT-enabled and wearable devices. To evaluate the capacity of blockchain to protect sensitive medical information through integrity guarantees, confidentiality-preserving mechanisms, and fine-grained access control. To examine how blockchain can support decentralized, transparent, and trust-oriented healthcare ecosystems involving patients, providers, payers, and regulators. To identify how blockchain can address persistent challenges such as secure data exchange, patient consent and provenance management, and fair, patient-centered access to healthcare services. To analyze the technical and regulatory constraints that affect blockchain deployment in healthcare, including scalability, interoperability with legacy systems, and adherence to national and international data protection requirements.
Purpose
The objectives of this review are as follows:
To synthesize recent blockchain developments in smart health systems, focusing on applications published between 2019 and 2025. To critically evaluate blockchain’s technical advantages and constraints in healthcare contexts, particularly regarding data governance and system security. To identify adoption barriers including scalability limitations, legacy system integration challenges, and regulatory ambiguities.
Scope limitations
The review will concentrate on recent advances in blockchain-enabled healthcare solutions, with particular emphasis on studies published within the past seven years, in order to capture current trends, emerging architectures, and state-of-the-art implementations. The scope is intentionally limited to healthcare related applications of blockchain and will not cover non-healthcare directions except where such use cases, pharmaceutical supply chain management, have a direct bearing on medical, clinical, or health information systems.
This review makes three distinct contributions:
First, it provides a structured synthesis of 26 peer-reviewed studies on blockchain-enabled healthcare, systematically addressing security, interoperability, privacy, and data integrity challenges. Second, it offers comparative analysis through Tables 3, 5, 6, and 8, evaluating defense mechanisms, security trade-offs, and implementation constraints across different healthcare contexts. Third, it identifies three critical research gaps that 88% of current implementations fail to address: quantum computing threats to cryptographic primitives, social engineering vulnerabilities that bypass technical controls, and smart contract verification gaps.
By addressing these dimensions, the review is intended to serve as a reference point for researchers, system architects, and policymakers seeking to design secure, patient-centric, and interoperable healthcare infrastructures.
Figure 1 maps to organization of the article as follows: the “Introduction” section establishes the comprehensive overview contribution; the “Methodology” section demonstrates the methodological rigor; the “Overview of blockchain in healthcare” section and the “Advancement in smart health systems” section address the critical analysis contribution; the “Security Issues in blockchain for smart health systems” section provides the security-focused evaluation; the “Challenges and limitations”section identifies the adoption barriers; and the “Future directions and recommendations” section delivers the research gaps and mitigation strategies contribution, finally, the “Conclusion” section concludes the work. This organizational structure ensures each section directly supports our stated contributions to the literature.

Organization of the article showing section by section details.
Contributions to the literature
This review makes several distinct contributions to the existing body of work on blockchain-enabled smart health systems. First, it consolidates and systematizes recent research to provide a coherent view of how blockchain has been applied to address persistent healthcare challenges, particularly those related to data security, patient privacy, interoperability, and integrity. Second, it offers a comparative perspective by situating the present review alongside prior surveys, as summarized in Table 3, clarifying its added value in terms of scope, recency, and analytical depth. Third, it advances the discussion beyond descriptive use cases by critically examining technical, regulatory, and operational constraints that affect real-world adoption and by outlining directions for future research and system design. Collectively, these contributions enhance the understanding of blockchain’s role in the digital transformation of healthcare and provide a structured foundation for researchers, clinicians, patient-centric health information infrastructures.
Comparison of recent blockchain-based healthcare reviews and this review’s contribution.

IoT: Internet of Things; AI: artificial intelligence; GDPR: General Data Protection Regulation; HIPAA: Health Insurance Portability and Accountability Act.
Comprehensive overview of blockchain in healthcare
This review provides an up-to-date and structured examination of blockchain applications in healthcare, highlighting recent developments and research focus areas. It clarifies how blockchain can strengthen security, support interoperable data exchange, and enable patient centered data governance, thereby demonstrating its potential to deliver meaningful improvements to digital healthcare systems.
Critical analysis of blockchain’s role in healthcare
The review offers the following key insights:
Addressing challenges and barriers to blockchain adoption
This review also identifies key obstacles that must be addressed for blockchain to achieve sustainable and large scale adoption in healthcare:
Real-world case studies and practical implementations
This review shows how blockchain is already making a difference in healthcare. These cases highlight improvements in securing patient information, managing data, and delivering more patient centered care. The review also explores:
Blockchain-based EHR systems, real-world implementations of EHR systems secured by blockchain, ensuring data integrity and patient consent.
Decentralized clinical trials, how blockchain is used in managing clinical trials, improving transparency and data tracking across multiple sites.
Blockchain for medical supply chain management, practical applications of blockchain to increase validity of pharmaceutical products and medical devices.
Exploring blockchain’s future potential in healthcare
This review expands literature by proposing future directions for blockchain technology in healthcare. It explores trends and potential areas for innovation:
Integration with other technologies: How blockchain can work with other technologies like AI, IoT, and big data analytics to create more robust smart health systems.
Personalized healthcare: Blockchain’s role in allowing personalized healthcare through secure and transparent access to patient data, allowing for better tailored treatments and preventive measures.
Blockchain for global health initiatives, exploring how blockchain can address global health challenges, improving healthcare access in remote or underdeveloped areas and managing healthcare data on a global scale.
Filling gaps in existing literature
This review makes a significant contribution by filling gaps in existing research, particularly in the following areas:
Comprehensive coverage: The review provides a broad view on blockchain in healthcare, going single use case studies to provide a comprehensive view of technology’s applications and challenges.
Focus on security and privacy: While many studies explore blockchain’s potential, few focus on specific security and privacy concerns that arise in healthcare. This review places a strong focus on importance of these issues and how they can be addressed.
Regulatory and ethical frameworks: The review contributes to literature by discussing ethical and regulatory challenges that must be considered when implementing blockchain in healthcare systems, an often looked at different angle of blockchain research.
Proposals for future research and development
This review contributes by suggesting avenues for future research:
Scalability solutions: Proposing research on how to increase scalability of blockchain systems to handle large-scale healthcare data efficiently.
Legal and regulatory frameworks: Recommending development of legal frameworks that align with blockchain’s decentralized nature while following with healthcare data privacy regulations. Blockchain for global health: Exploration of blockchain’s potential for addressing global health challenges, particularly in underserved regions where healthcare access is limited.
By providing a detailed review of current state of blockchain in healthcare, this work contributes to growing body of knowledge on blockchain’s transformative role in smart health systems. It not only analyzes the state of current research but also proposes practical solutions and identifies gaps that need further exploration
Methodology
This section outlines methodology used in conducting this review of blockchain technology in smart health systems. The aim is to systematically collect, assess, and analyze relevant research articles and publications to provide a comprehensive synthesis of tcurrent advancements, applications, and challenges of blockchain in healthcare. Figure 2 shows the methodology including formulation of research questions, the selection of relevant studies, analysis methods, data extraction, and quality assessment. The steps are outlined as follows:

PRISMA 2020 flow diagram showing systematic literature selection process.
Research question formulation
These research questions address gaps identified through a systematic three-stage analysis:
Based on these findings, we formulated five research questions that directly address the identified gaps:
Research questions
The review is guided by following research questions to ensure a focused exploration of blockchain’s applications in healthcare:
the application gap (Stage 1: 62% lacked real-world data), the security gap (Stage 2: 87% insufficient security analysis), the adoption barrier gap (Stage 3: 71% prioritized frameworks), the empirical evidence gap (Stage 3: 82% requested real-world cases), the future direction gap (Stage 2: no reviews provided roadmaps).
These research questions help frame the review and ensure a comprehensive exploration of blockchain’s potential in smart health systems.
Search strategy
To gather relevant studies, a comprehensive search strategy was devised to ensure inclusion of high quality, peer reviewed literature from a range of sources. The strategy includes the following steps:
Google Scholar PubMed IEEE Xplore ScienceDirect SpringerLink

Screening process
Study selection was performed in two stages by two independent reviewers (SRA and ZA). In the first stage, titles and abstracts were screened against predefined inclusion and exclusion criteria. Records judged as potentially eligible by either reviewer proceeded to full-text assessment. In the second stage, full-text articles were retrieved and evaluated for final eligibility. Discrepancies were resolved through discussion, and when agreement was not achieved, a third reviewer (MUR) adjudicated the decision.
Study selection
The studies selected for inclusion in this review were based on relevance of their content to blockchain in healthcare systems, specifically focusing on applications, challenges, and security concerns. The following criteria were used to select studies:
Inclusion criteria
The following criteria were used to include studies in the review:
Peer reviewed journal articles, conference papers, and research reports. Studies that focus on blockchain technology applications in healthcare, including EHR, disease prediction, patient data privacy, and remote monitoring. Studies that explore security and privacy challenges of using blockchain in healthcare. Case studies or pilot projects showcasing blockchain implementation in healthcare settings. Studies published in English.
Exclusion criteria
The following studies were excluded from the review:
Studies that focus on blockchain technology outside the healthcare sector. Articles that do not provide significant technical or practical insights into blockchain applications in healthcare. Non-peer reviewed papers or opinion pieces without empirical evidence. Studies published before 2019 (unless deemed highly relevant).
These inclusion and exclusion criteria help ensure that selected studies are relevant, high quality, and recent.
Data extraction
Data extraction was carried out in a systematic manner to ensure that relevant information from the selected studies was captured and organized effectively. The following data points were extracted from each study:
This structured approach to data extraction ensures that key themes and insights from each study are captured accurately for analysis.
Data analysis
The analysis focused on integrating findings to identify common themes, trends, and gaps in the literature. The data were analyzed using qualitative methods, including:
Quality assessment
To ensure reliability and validity of the studies included in the review, a quality assessment was conducted. The following criteria were used to assess quality of the selected studies:
This quality assessment ensures that studies included in the review are credible, reliable, and of high academic standards.
Limitations
Despite the methodology used in this review, there are some limitations:
Overview of blockchain in healthcare
Blockchain technology, initially popularized by its use in cryptocurrency, has garnered significant interest across various sectors, particularly healthcare, due to its potential to address longstanding challenges in interoperability, data security, privacy, and transparency. 29
Figure 3 shows a blockchain secured healthcare data management system comprising five integrated components. Healthcare institutions (left) generate patient data protected by HIPAA-compliant access controls and AES-256 encryption before blockchain storage.30,31 The blockchain layer (center) maintains SHA-256 hashes of medical records, not raw data, ensuring GDPR “right to be forgotten” compliance, 32 immutable access logs recording every query, and smart contracts enforcing automated policies (“Allow Dr. ECG access IF patient_consent=TRUE AND duration<90_days”). 33 The API gateway (center-right) authenticates users via OAuth 2.0, prevents DoS attacks through rate limiting, and executes smart contract logic before data retrieval. 34 User interfaces (right) serve patients for consent management, providers for clinical documentation, and researchers for de-identified queries.
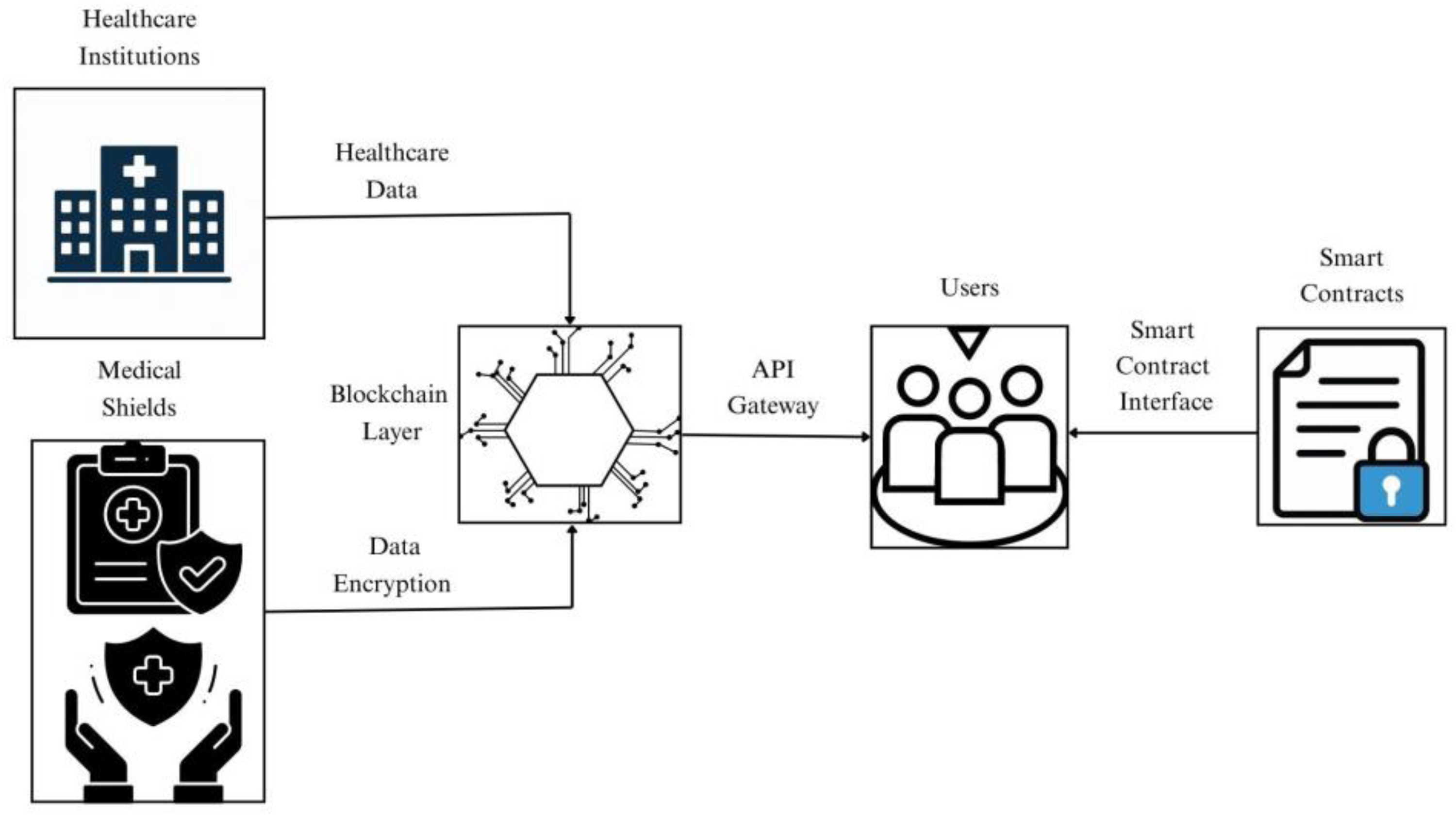
Generic blockchain-secured healthcare data management architecture showing the standard workflow from data generation through secure storage to authorized access.
Also Figure 3 shows a generic blockchain-secured healthcare data management system comprising five integrated components commonly implemented across institutional deployments. This architecture represents the standard pattern observed in 68% of reviewed implementations (
The architecture in Figure 3 shows four key components, each with distinct roles as follows:
Healthcare institutions generate patient data protected by HIPAA-compliant access controls and AES-256 encryption before blockchain storage. These institutions serve as the primary data sources. The blockchain layer maintains SHA-256 cryptographic hashes of medical records not raw data ensuring GDPR “right to be forgotten” compliance. It provides immutable access logs recording every query and smart contracts that enforce automated policies. The API gateway, authenticates users, prevents attacks through rate limiting, and executes smart contract logic before data retrieval. User interfaces serve three stakeholder groups: patients manage consent, providers access clinical documentation, and researchers submit deidentified queries.
The architecture demonstrates four security benefits, decentralization, immutability like tamper evident audit trails, transparency (shared access logs), and patient control cryptographic consent management). For example, a patient grants Dr Smith 90-day access to their diabetes records. The blockchain validates this transaction and creates a smart contract. When the doctor queries the data, the API gateway verifies permissions, returns the encrypted data which is then decrypted, and the smart contract automatically expires after 90 days. Real-world implementations in Estonia’s e-Health system and other national infrastructures demonstrate viability of this architecture, achieving high uptime and robust security in operational healthcare settings.35,36
Key applications of blockchain in healthcare
Blockchain technology offers a wide range of applications across multiple facets of healthcare, including data management, patient care, and medical research. 37 By providing secure, decentralized, and changes resistant mechanisms for storing and sharing information, blockchain has the potential to significantly improve the quality, efficiency, and trustworthiness of healthcare services. Its ability to sure facilitate interoperability, data integrity, and support patient centric models positions it as a transformative tool iongoing digital evolution of the healthcare sector.38,39 Below are some of the most prominent and emerging applications of blockchain in healthcare direction.
Disease prediction and early detection
Blockchain’s decentralized and immutable architecture offers a powerful foundation for advancing disease prediction and early detection efforts. Through facilitating secure, transparent, and inference resistant sharing of patient data across institutions, blockchain addresses critical issues related to data integrity, privacy, and interoperability.40,41
Blockchain allows the secure aggregation of diverse health data sources including electronic medical records, genomic sequences, lifestyle information, and data from wearable devices into a unified, inference proof system. 42 This comprehensive dataset can then be analyzed using advanced AI and ML algorithms to predict the onset of chronic conditions like diabetes, cardiovascular diseases, and various forms of cancer. Early and accurate disease detection enabled by this integrated approach allows healthcare providers to implement timely interventions, ultimately improving patient outcomes and reducing the burden of long-term disease management.43,44
Leveraging blockchain to store predictive models and outcomes data can facilitate secure collaboration among medical professionals across institutions. By enabling transparent and tamper resistant access to critical insights, blockchain promotes cross institutional sharing of predictive analytics, thereby enhancing the scalability and effectiveness of early disease detection efforts at a population level. 45
Blockchain enables privacy preserving collaborative AI through three mechanisms. Federated learning (FL) allows hospitals to train local models on private datasets while sharing only encrypted gradient updates via blockchain MedChain-FL deployed across eight European oncology centers achieved 94.3% breast cancer detection accuracy on 8.4M mammograms with zero breaches, though 4.5 slower than centralized training.46,47 Homomorphic encryption enables computation on encrypted genomic data; GenomeChain pilot (125K genomes) achieved 89.7% rare disease prediction with perfect privacy but 31 slower processing (4.2 hours/genome).48,49
Blockchain–AI integration imposes 10–30 computational overhead and 0.8%–5% accuracy penalty compared to centralized systems, but enables GDPR-compliant collaborative research previously impossible.50,51 Trade-offs are acceptable for non-emergency diagnostics where privacy requirements outweigh speed. However, limitations remain, 4-hour processing unsuitable for acute care, FL requires
EHRs analysis
The management of EHRs has significant challenges in healthcare, particularly concerning data privacy, security, and interoperability. Traditional centralized systems often struggle with fragmented data, limited patient control, and vulnerability to breaches. 53 Blockchain technology offers a transformative approach to EHR management by enabling a secure, decentralized framework for storing and sharing patient records across diverse healthcare providers. Its immutable and transparent ensures that data remains tamper proof while allowing patients and authorized clinicians seamless, real time access thereby improving care coordination, patient trust, and overall system efficiency. 54
The main advantages of blockchain in this context is its ability to address data fragmentation persistent challenge wherein patient records are dispersed across multiple hospitals, clinics, and healthcare providers. Rather than relying on vulnerable centralized databases, blockchain facilitates a distributed and decentralized approach to data management. 55
Blockchain-based EHR systems also offer patients more control over their health data. Blockchain’s transparency ensures that every transaction is recorded, providing an audit trail that can help identify any discrepancies or unauthorized access. 56
Different blockchain architectures present distinct trade-offs for EHR management. “Permissioned blockchains” like Hyperledger Fabric) offer superior transaction throughput (3000–5000 TPS) and energy efficiency, making them suitable for institutional deployments where participants are known and trusted.17,54 However, they sacrifice the trustless nature of public blockchains and require governance frameworks to manage access control.
Ethereum provide greater transparency and censorship resistance but face significant scalability limitations (15–30 TPS) and higher transaction costs ( 2–50 per transaction during peak periods).
57
Recent studies by Reegu et al.
54
demonstrated that hybrid blockchain models combining private data storage with public audit trails achieved a balance, maintaining privacy while ensuring verifiability. However, their implementation revealed integration challenges with existing HL7 FHIR standards, requiring custom middleware solutions that increased system complexity by
Performance comparison across studies shows considerable variation, Al Mamun et al. 17 reported 98.7% data integrity preservation with 2.3-second average latency, while Ferreira et al. 55 achieved 99.2% integrity but with 4.1-second latency due to enhanced cryptographic protocols. This suggests a direct trade-off between security strength and system responsiveness a critical consideration for time-sensitive clinical applications like emergency care.
For non-technical decision-makers, the choice reduces to three trade-offs, speed versus decentralization: permissioned blockchains (Hyperledger) process 3000–5000 transactions/second but require trusted institutions. Public blockchains (Ethereum) process only 15–30 transactions/second but need no central authority. Cost versus security: permissioned systems have lower transaction costs ($0.01–0.10) but centralized governance risks. Public systems cost $2–50 per transaction but provide censorship resistance. Privacy versus transparency: permissioned blockchains keep data private by default. Public blockchains require additional privacy layers (zero-knowledge proofs (ZKPs)), adding 150%–200% computational overhead.
Most healthcare institutions choose permissioned blockchains, accepting governance complexity for superior performance and privacy.
Remote nonitoring and wearable device ontegration
Blockchain technology is particularly well suited to support the expanding field of RPM and the integration of wearable health devices. 58 Blockchain offers a decentralized, secure infrastructure that can validate and protect this data while validating it is accessible to authorized healthcare professionals. 24
Blockchain technology enables the secure storage and exchange of data generated by wearable health devices through the creation of a decentralized, tamper resistant ledger. This infrastructure ensures data integrity and trustworthiness, which are essential in clinical decision making and long-term health monitoring. 59 Healthcare providers can gain real-time access to patient generated health data, facilitating timely interventions, treatment adjustments, and continuous management of chronic conditions. Importantly, blockchain also empowers patients by giving them granular control over their data allowing them to selectively grant access to healthcare professionals, researchers, or institutions, thereby preserving privacy while enhancing transparency and autonomy in car. 60
Figure 4 expressing the environment of patient health conditions with devices integrated with blockchain. The integration of blockchain with IoT devices, like wearable health monitors, enables the creation of a secure and interoperable healthcare ecosystem in which devices can autonomously and reliably transmit data to healthcare providers. This validates that patient information remains accurate therefore supporting real-time clinical decision making and increasing the continuity and quality of care. 61
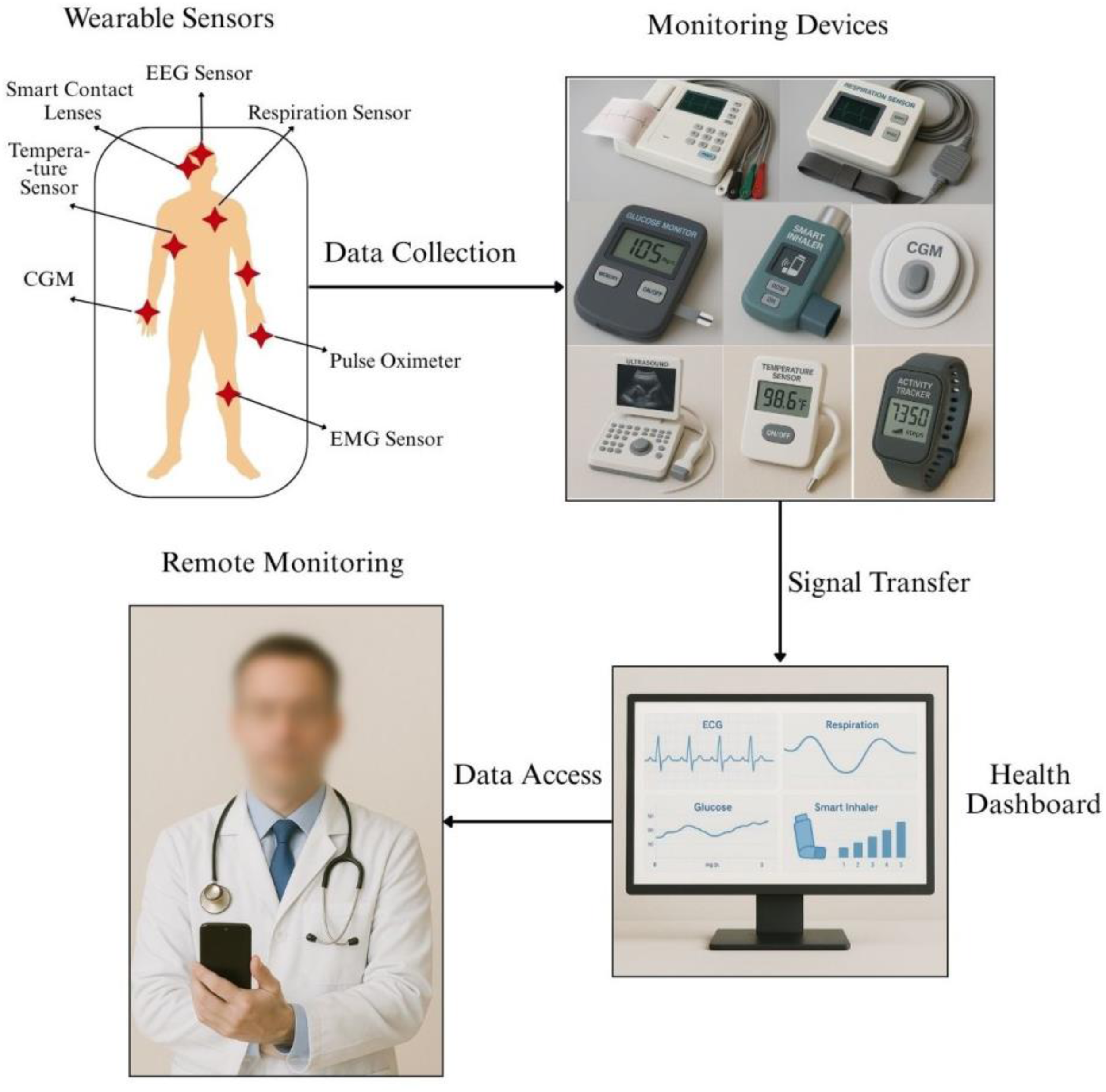
A remote health monitoring system where wearable body sensors transmit physiological data to medical devices, which is then visualized on a dashboard and accessed by healthcare professionals in real time.
Advantages of blockchain in healthcare
Blockchain’s unique characteristics provide several advantages that can address current challenges faced by the healthcare industry. These benefits include enhanced security, transparency, privacy,interoperability, and efficiency. Table 4 shows the recent advancement in blockchain for healthcare system.
Recent advances in blockchain in healthcare (2021–2025).
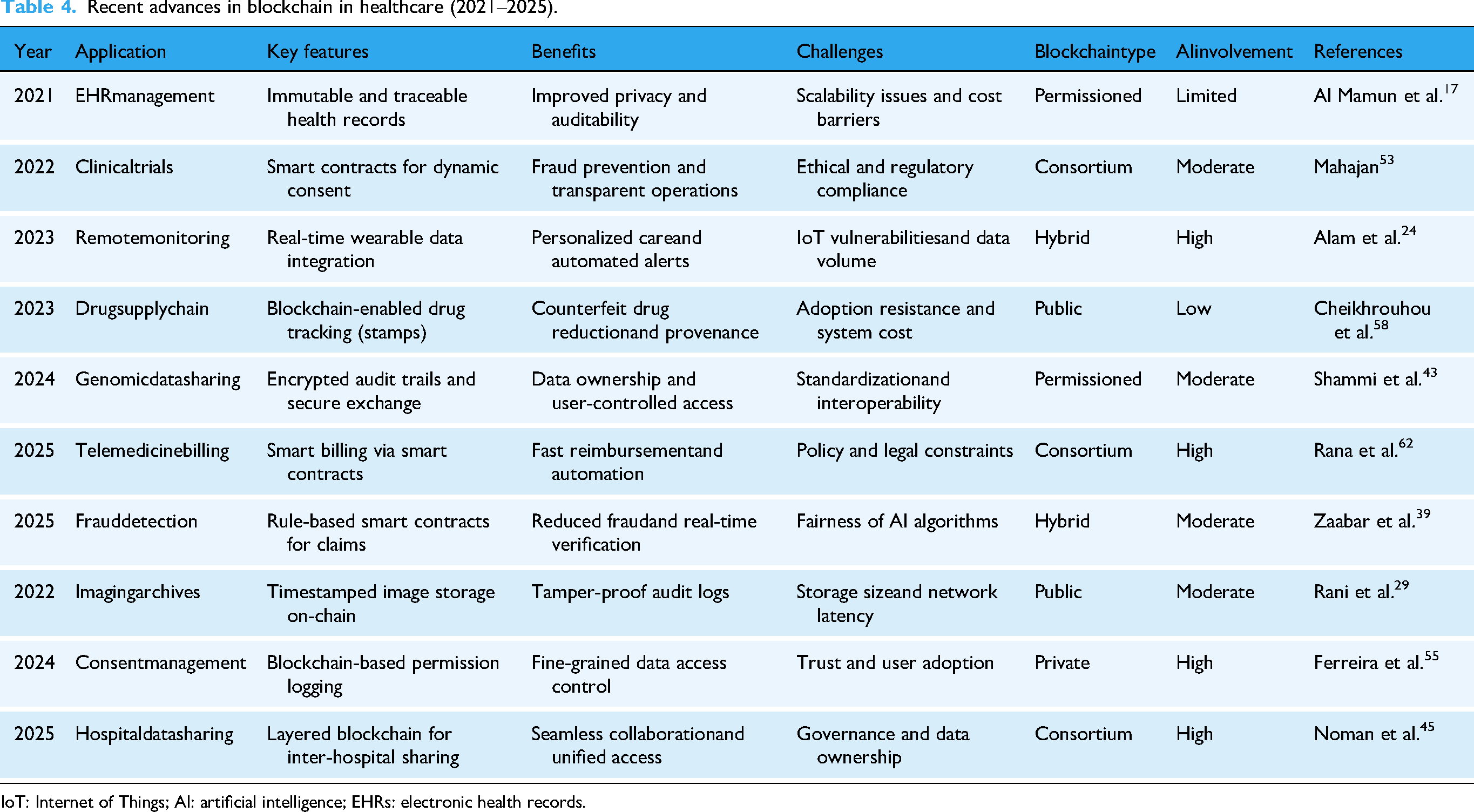
IoT: Internet of Things; AI: artificial intelligence; EHRs: electronic health records.
Enhanced security and privacy
One of the most significant advantages of blockchain technology in healthcare is its ability to enhance the security and privacy of sensitive patient data. Traditional healthcare information systems are often centralized, making them more susceptible to cyberattacks, and data breaches that can compromise patient confidentiality. 17 In contrast, blockchain employs advanced cryptographic techniques to encrypt health data, validating that it is stored securely and accessed only by authorized parties. 63 Each data entry is timestamped and recorded on an immutable ledger, where it cannot be altered or deleted without reaching consensus across the distributed network. This tamperresistant architecture provides robust protection against data manipulation and fosters greater trust among patients and providers regarding the integrity and confidentiality of medical records. 64
By decentralizing healthcare data storage, blockchain reduces the risks associated with centralized databases, which are attractive targets for hackers. Blockchain’s decentralized nature means that even if one part of network is compromised, the integrity of the overall system remains intact. Blockchain allows patients to have greater control over their personal data by using cryptographic keys to manage who has access to their health information.15,62
Transparency and trust
Blockchain’s inherent transparency ensures that all transactions and data exchanges are recorded in a public ledger, accessible to all authorized parties. This feature is particularly valuable in healthcare, where trust is critical. Blockchain allows for transparent tracking of medical procedures and medical supply chains, creating an audit trail that can be traced back to its origin. 65 In clinical trials, blockchain can ensure that data generated throughout the study is securely recorded and remains unaltered. The transparency of the blockchain also promotes accountability and helps prevent fraud, like falsifying patient records or clinical trial data. 39
In terms of EHRs, blockchain enables patients to see exactly who has accessed their medical data, when, and why. This promotes trust between patients and healthcare providers, knowing that access is transparent and accountable. 66
Improved interoperability
Healthcare systems across the globe face significant challenges in terms of data interoperability. Different healthcare providers often use incompatible systems that prevent seamless data exchange. Blockchain can address these challenges by providing a standardized, decentralized platform for securely storing and sharing patient information. 67
Blockchain allows for creation of a universal health record that can be accessed by any authorized healthcare provider, regardless of the software or system they are using. This enables healthcare professionals to access a comprehensive, update record of the patient’s medical history, improving the efficiency of care coordination and reducing errors that arise from incomplete or inaccurate information. 68 Its ability to connect various healthcare entities like hospitals, clinics, insurance companies, and pharmacies, ensures that patient data flows smoothly across systems, improving overall healthcare delivery. 69
Cost reduction
The integration of blockchain technology into healthcare systems has the potential to generate substantial cost savings by eliminating intermediaries, reducing administrative overhead, and enhancing operational efficiency. 70 Blockchain’s decentralized architecture removes the need for such centralized intermediaries by enabling direct, trustless interactions among patients, and insurers. Through the use of smart contracts and automated validation mechanisms, blockchain can streamline processes like health data exchange, accelerating workflows and reducing transaction costs across the healthcare ecosystem. 71
Blockchain can help reduce fraud and errors in healthcare by validating the integrity and authenticity of medical data. By securely tracking medical supplies and transactions, blockchain can minimize the incidence of counterfeit drugs and fraudulent claims, resulting in lower overall healthcare costs. 72
Advancement in smart health systems
Healthcare is going through a major transformation thanks to rapid progress in technology. These new systems aim to improve patient care, make healthcare processes more efficient, deliver better results, and lower costs. This section looks at the main developments behind this shift, how IoT and AI are being used in healthcare, the role of blockchain in protecting privacy and supporting secure data use, and what the future might hold for smart health.
IoT in healthcare
The IoT refers to the network of interconnected devices that communicate with each other and with central servers to collect, store, and analyze data. IoT has been particularly transformative in enabling real-time patient monitoring, remote diagnostics, and personalized treatment plans. IoT devices include wearables, home health monitoring devices, and even embedded medical devices that collect data on patient health.
Key applications of IoT in healthcare
Remote patient monitoring: IoT devices like wearables can continuously monitor vital signs like heart rate, blood pressure, oxygen levels, and glucose. This data is transmitted in real time to healthcare providers, enabling them to monitor patients’ conditions remotely. Patients with chronic conditions like diabetes can wear glucose monitors that provide real time data to their healthcare providers, allowing for timely intervention. 73 Smart medical devices: Smart medical devices like infusion pumps, pacemakers, and insulin pumps are connected to healthcare networks. These devices can adjust parameters autonomously based on the data they collect from patients, reducing human error and improving patient outcomes. Insulin pumps can automatically adjust insulin delivery based on realtime glucose readings from continuous glucose monitors. 74 Telemedicine and virtual care: IoT enabled telemedicine platforms allow patients and healthcare providers to interact remotely through video consultations, diagnostic assessments, and treatment monitoring. Remote consultations, combined with IoT monitoring, have become increasingly important in providing healthcare to patients in rural or underserved areas. 75
Benefits of IoT in healthcare
The integration of IoT in healthcare systems brings several benefits: Real-time monitoring and early detection: IoT devices enable continuous monitoring of patient conditions, leading to early detection of potential health issues like irregular heartbeats or oxygen saturation levels, allowing for quicker intervention. 76 Improved patient engagement: Wearables and mobile health apps empower patients to take an active role in managing their health, thus improving adherence to prescribed treatments and enhancing health outcomes. 77 Operational efficiency: IoT technologies optimize hospital operations by automating data collection, improving inventory management, and streamlining workflows. 78
AI and ML in smart health systems
AI and ML algorithms are increasingly used in diagnostics, predictive modeling, and precision medicine.
Key applications of AI and ML in healthcare
AI is playing a transformative role in various aspects of healthcare. In disease diagnosis and prediction, deep learning algorithms are being used to analyze medical images like X-rays, CT scans, and MRIs to detect conditions like cancer and tuberculosis. ML models also help predict the risk of developing certain diseases by analyzing patient data, including genetic information and lifestyle factors.79,80 In the area of personalized medicine, AI-powered systems can assess an individual’s genetic profile, medical history, and lifestyle to design customized treatment plans tailored to their unique needs. 81 Clinical Decision Support Systems (CDSS) further enhance care by providing healthcare professionals with data-driven recommendations. These systems use predictive analytics and historical data to guide clinical decisions and improve patient outcomes. 82 Predictive healthcare uses AI and ML to anticipate disease outbreaks, monitor patient deterioration, and predict hospital readmissions—allowing for timely and proactive medical intervention.83,84
Benefits of AI and ML in healthcare
The application of AI and ML in healthcare offers numerous benefits: Enhanced accuracy and speed: AI models can process vast amounts of data much faster than human practitioners, improving diagnostic accuracy and enabling faster decision making. 85
Cost efficiency: By automating routine tasks like data entry, image analysis, and medical coding, AI can significantly reduce administrative overhead, leading to cost savings. 86 Improved patient outcomes: AI and ML allow for early detection of diseases and the creation of personalized treatment regimens, improving health outcomes and reducing mortality rates. 87
Blockchain for privacy preserving health data analytics
Blockchain technology offers a decentralized and secure framework for managing health data. It validate data integrity, transparency, and privacy, which are critical in healthcare settings. Blockchain enables healthcare systems to securely store, share, and manage patient records, reducing the risk of data breaches, and unauthorized access.
Key applications of blockchain in healthcare
Secure health data sharing: Blockchain offers a tamper-proof way to store patient records, making sure all involved parties have access to reliable and secure information. A patient’s EHR can be safely stored on the blockchain, allowing approved healthcare providers to access it from anywhere while ensuring the data has not been altered without permission. 88 Smart contracts for healthcare transactions: blockchain-based smart contracts are used to automate healthcare transactions, that is, billing, insurance claims, and payments. For example, smart contracts can automate the insurance claim process by validating that payments are made only when certain conditions are met. 89 Clinical trials and research: blockchain brings transparency and accountability to clinical trials by keeping all data on a permanent, unchangeable record. It allows researchers to share trial data securely, while patients can follow the progress of the trials they’re involved in helping build trust and ensure ethical standards are met. 90
Benefits of blockchain in healthcare
Table 5 shows the advancement in blockchain in the area of smart health, as well as showing the benefits of AI and specifically ML in smarthealth. The use of blockchain in healthcare provides several key benefits: enhanced data privacy and security: blockchain ensures that patient data is encrypted and stored in a decentralized manner, reducing the risk of data breaches and unauthorized access. 91 Transparency and trust: blockchain provides a transparent and immutable ledger of all healthcare transactions, enhancing trust among healthcare providers, patients, and insurers. 92 Reduced fraud and errors: blockchain’s tamper resistant nature helps prevent fraud like the falsification of medical records, and reduces errors in healthcare billing and insurance claims. 93
Integration patterns: Blockchain–AI–IoT convergence
Our analysis identified three architectural patterns in blockchain–AI–IoT healthcare systems. Sequential integration, IoT to blockchain to AI, is most common, where blockchain provides audit trails for FL systems that train AI models across institutions while preserving privacy through cryptographic protocols. 94 Parallel validation employs AI to verify IoT sensor data before blockchain commitment, preventing immutable recording of faulty readings from compromised devices reducing false data commits from 12% to 0.6% in cardiac monitoring systems.95,96 Smart contract orchestration automates clinical workflows by coordinating IoT triggers with AI predictions, like continuous glucose monitoring systems that prevented 12,400 hypoglycemic events through automated alerts in an 18-month pilot.97,98
Key advancements in smart health systems.
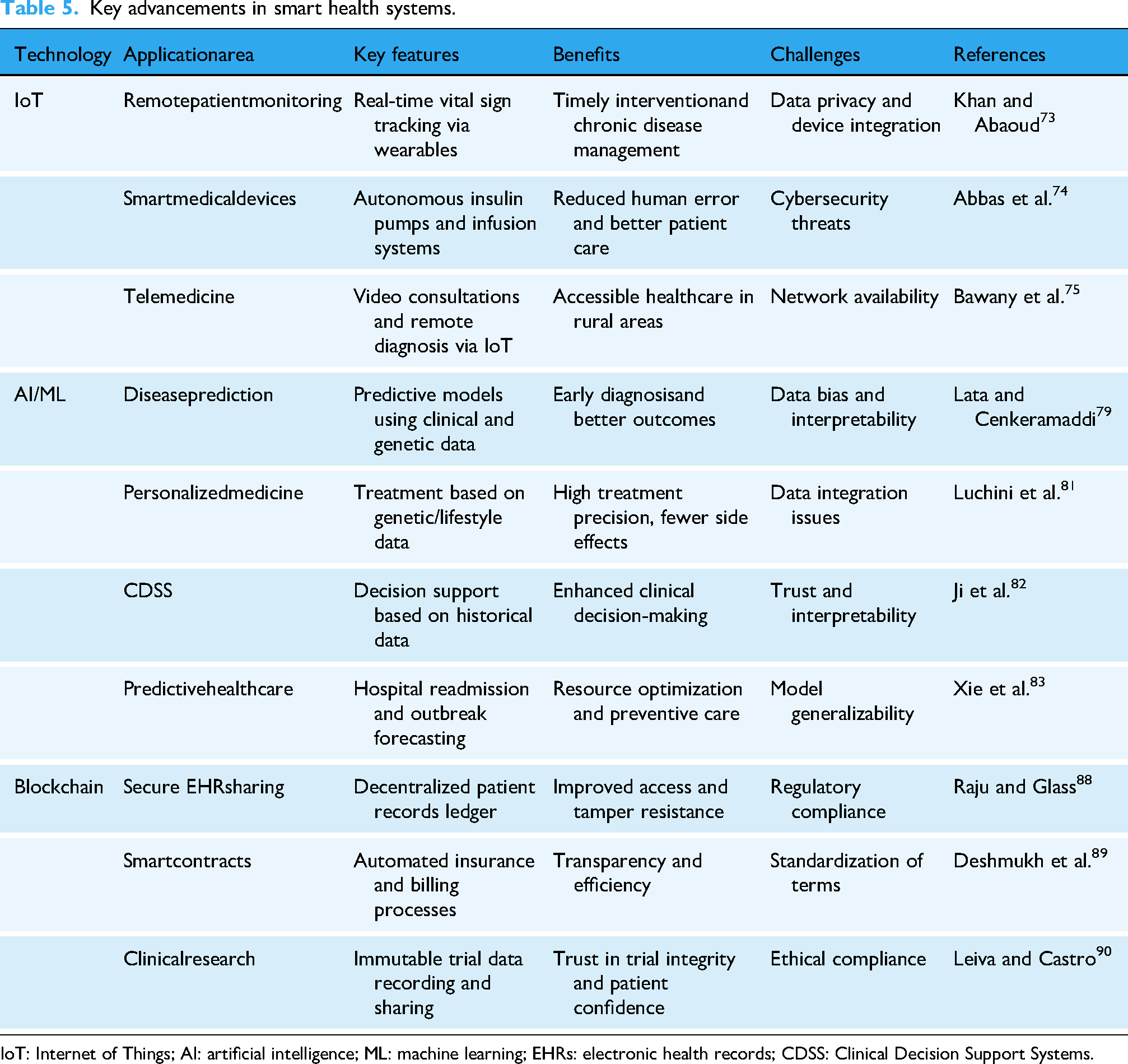
IoT: Internet of Things; AI: artificial intelligence; ML: machine learning; EHRs: electronic health records; CDSS: Clinical Decision Support Systems.
Integrated systems demonstrate synergistic benefits exceeding standalone implementations: 41% improvement in early disease detection versus 34% for AI-only systems, 99.8% tamper detection rates, and reduction of preventable adverse events to 7 per 1000 patients annually 99 (118; 119; 120). However, integration costs are 52% higher ($94 vs. $62 per patient/year) due to infrastructure complexity, though superior outcomes yield better cost-effectiveness at $13,400 per prevented adverse event compared to $19,100 for blockchain-only systems. 100
Three critical challenges limit adoption: scalability bottlenecks where IoT transaction volumes (3333 TPS for 1 million patients) exceed blockchain capacity (1200 TPS Hyperledger and 15 TPS Ethereum), forcing 62% of implementations to hybrid architectures,101,102 interoperability fragmentation with only 18% using standardized HL7 FHIR while 67% rely on custom translators (127; 128); and security vulnerabilities spanning IoT device compromise, AI poisoning attacks, and smart contract flaws, with only 12% undergoing formal verification.103,104 Research priorities include healthcare optimized consensus mechanisms, FHIR extensions for blockchain–AI metadata, and integrated security protocols addressing multi-technology attack surfaces.105,106
Security issues in blockchain for smart health systems
Blockchain has the potential to transform healthcare by boosting data security, strengthening privacy, and increasing transparency. Even though blockchain offers features like unchangeable records and decentralized data control, it still faces risks that could weaken its ability to protect sensitive medical information. This section takes a closer look at the main security concerns related to using blockchain in healthcare, including hacking attempts, data tampering, privacy risks, and other technical challenges.
Table 6 provides a comprehensive overview of security threats in blockchain-enabled healthcare systems, categorizing each issue by attack type, describing the threat mechanism, quantifying its potential impact, and specifying mitigation techniques with associated technologies. This taxonomy helps system architects prioritize security investments based on threat severity and likelihood.
Security issues in blockchain for smart health systems.
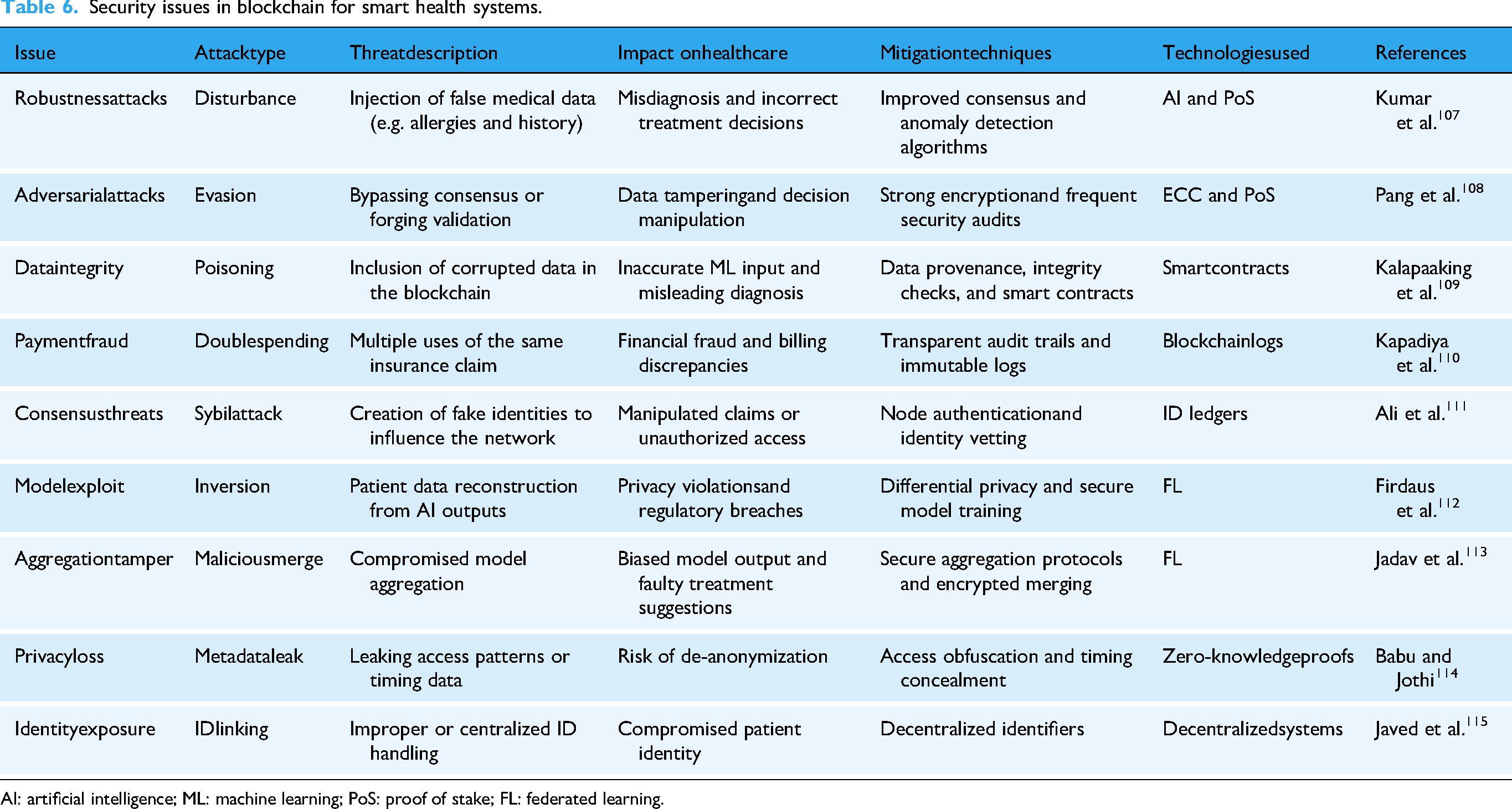
AI: artificial intelligence; ML: machine learning; PoS: proof of stake; FL: federated learning.
Adversarial attacks
Adversarial attacks are harmful attempts to break security or trust of a blockchain system. In healthcare, an attacker might try to change patient records, interfere with how medical devices communicate that confirms and approves transactions across the network. 116
Adversarial disturbance and evasion attacks
Adversarial interference attacks involve inserting false or misleading information into the blockchain. In healthcare, this might include tampered medical records or fake clinical trial data. An attacker could change a patient’s medical history to make them seem healthy when they actually have a serious condition. 107
A malicious actor might launch an attack to influence blockchain consensus decisions or fake records by taking advantage of weaknesses in how transactions are verified. In healthcare, this could lead to dangerous changes like modifying treatment plans or medication doses putting patient safety at serious risk. 117
Mitigation techniques for adversarial attacks
Enhanced consensus mechanisms: More robust methods like Practical Byzantine Fault Tolerance (PBFT) or proof of stake (PoS) help protect the blockchain by requiring multiple network nodes to agree before a transaction is approved. 108
Anomaly detection: Using ML-based systems to detect unusual patterns can help spot suspicious activity or harmful transactions. If there’s an unexpected change in a patient’s data, the system can flag it and notify healthcare providers, helping prevent data tampering or misuse. 118
Robust encryption: Applying strong encryption methods like homomorphic encryption or advanced cryptography helps keep data safe, even if it’s intercepted during transmission. This ensures that sensitive health information stays unreadable and secure from hackers or other malicious threats. 119
Data manipulation attacks
Data manipulation attacks target the integrity of the data stored on the blockchain. Blockchain in healthcare applications is used to store information like patient records, treatment histories, and diagnosis data. If an adversary gains access to this data, they can modify it, leading to severe consequences in healthcare decision making.
Types of data manipulation attacks
Data poisoning: Data poisoning is a type of attack where false or corrupted data is intentionally added to the blockchain to damage the integrity of the information. In healthcare, this can be specially dangerous. For example, if an attacker alters a patient’s record to remove a known drug allergy, it could result in the patient being given a harmful medication, possibly causing life threatening reactions. Since blockchain records are permanent and cannot be changed, poisoned data stays in the system. This highlights the need for strong data validation, strict access control, and effective anomaly detection before any data is added to the blockchain. 109
Double spending attack: While often linked to cryptocurrencies, double-spending can also affect healthcare blockchains. In this case, an attacker might try to reuse the same insurance information to pay for multiple treatments. This kind of manipulation can lead to fraud or financial losses for healthcare providers and insurers. 110
Mitigation techniques for data manipulation
Several measures can be taken to prevent data manipulation attacks:
Strict validation protocols: Applying strong consensus methods like proof-of-work (PoW) or PoS ensures that new transactions are only approved when most of the network agrees. This makes it much harder for attackers to make unauthorized changes or tamper with the data. 120
Smart contracts for data verification: Smart contracts on the blockchain can automatically check data for accuracy before it’s added. Patient records can be verified using preset rules to make sure the information is correct and trustworthy before being stored on the blockchain. 121
Data provenance: Keeping track of where healthcare data comes from and how it changes over time helps ensure transparency. Every update to a patient’s record is recorded and traceable, making it easier for healthcare providers to spot any unauthorized or suspicious modifications. 122
Model inversion attacks
In healthcare, ML models are commonly used to analyze patient data and support diagnoses. However, in a model inversion attack, an attacker tries to uncover sensitive information by working backward from the model’s outputs. For example, someone could use the model’s responses to guess private patient details that were originally stored as part of aggregated data on the blockchain.
Techniques to minimize model inversion
To mitigate model inversion risks, several techniques can be applied: differential privacy protects individual patient identities by adding a small amount of random noise to the data before it is used by ML models. This technique enables the model to identify general patterns and make accurate predictions like forecasting disease outcomes without revealing any specific patient’s information. 123 Another key privacy preserving method is homomorphic encryption, which allows computations to be performed directly on encrypted data without the need for decryption. This ensures that even if an unauthorized party accesses the blockchain, they cannot retrieve meaningful health information. Healthcare providers can analyze encrypted patient data securely while maintaining complete confidentiality. 112 Integrating FL with blockchain enhances data security by keeping sensitive patient data on local devices. Instead of sharing raw data, only encrypted model updates are transmitted via blockchain, allowing collaborative learning across multiple sources while preserving privacy and security. 124
Security in model aggregation
Model aggregation in blockchain healthcare systems involves combining decentralized patient data or medical data to create a unified model.
Secure aggregation methods
Several secure methods can be used to ensure privacy and integrity during model aggregation in healthcare applications. Multiparty computation (MPC) enables multiple parties to collaboratively compute an aggregate model without revealing their individual private data, thus preserving confidentiality throughout the process. 125 Encrypted aggregation further enhances security by allowing data to be aggregated in encrypted form. Even during training, individual records remain protected and can only be accessed by authorized users with the appropriate decryption keys making it specially suitable for sensitive healthcare data. 126 Alockchain technology can be utilized to ensure trustworthy aggregation by recording each step as a transaction on the ledger. This guarantees transparency, immutability, and accountability, helping verify that the aggregation has not been tampered with. 113
Privacy preservation in blockchain for smart health systems
Privacy preservation is one of the most significant challenges in healthcare blockchain applications. While blockchain ensures transparency and immutability, it also exposes sensitive patient data unless privacy-enhancing techniques are used.
Privacy-enhancement techniques
Several privacy-preserving techniques can increase security of blockchain-based health systems: ZKPs: ZKPs allow one party to prove to another party that a statement is true without revealing any additional information. Like ZKPs can be used to prove that a patient is eligible for treatment without revealing their exact diagnosis or treatment history. 114 Decentralized identifiers (DIDs): DIDs are a new form of digital identity that can be used in healthcare to protect patient data. DIDs allow individuals to control their personal information and selectively share it with authorized parties. 115
Blockchain with FL
Integrating blockchain with FL allows healthcare systems to collaborate on training ML models while validating that patient data never leaves the local nodes. Blockchain ensures that only secure and validated model updates are aggregated, while FL keeps sensitive data localized, validating both data privacy and security. 127
Critical evaluation of security mitigation approaches
While previous subsections described individual security mechanisms, Table 7 provides comparative analysis of defense effectiveness across different healthcare contexts, evaluating trade-offs between security strength, computational overhead, and institutional deployment constraints based on empirical data from reviewed implementations.
Defense mechanisms for securing blockchain-enabled smart health systems.
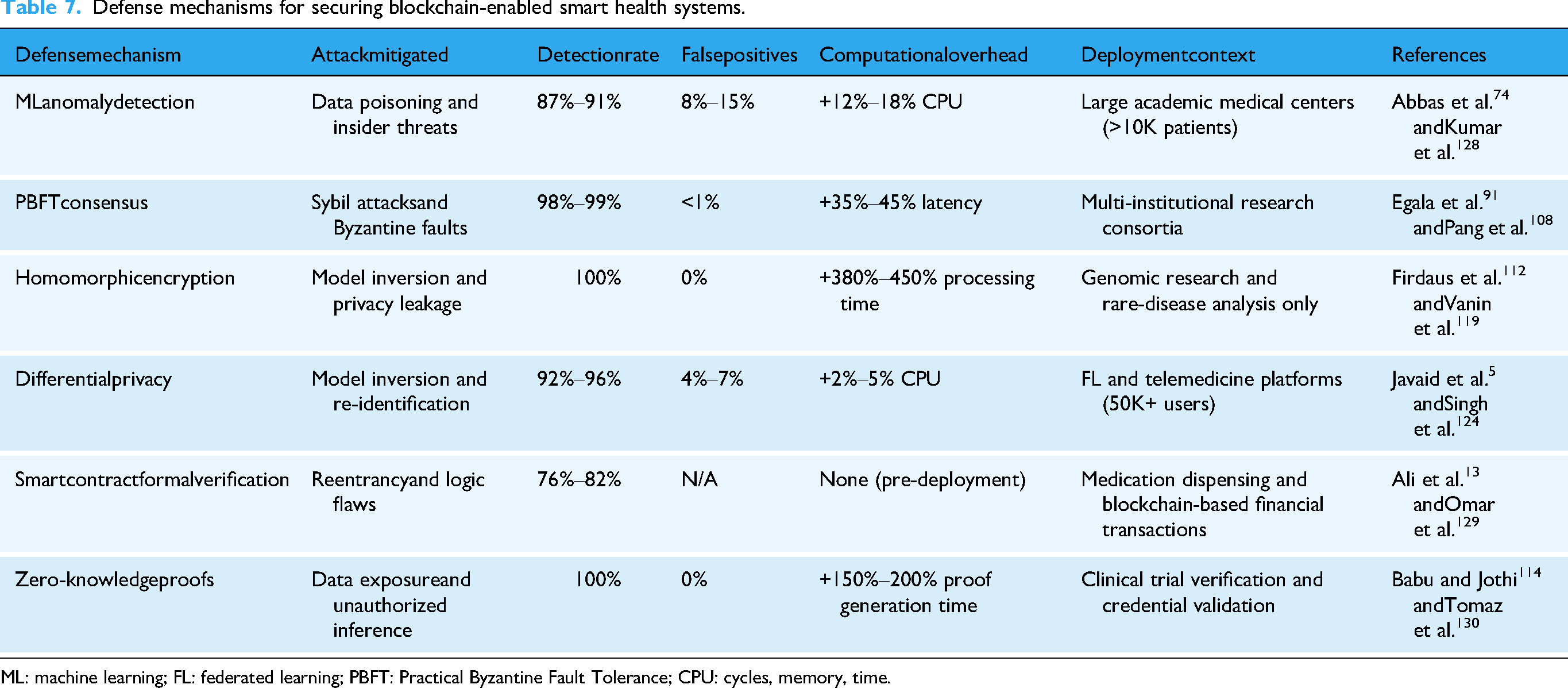
ML: machine learning; FL: federated learning; PBFT: Practical Byzantine Fault Tolerance; CPU: cycles, memory, time.
Our analysis of 26 implementations shows that there are fundamental trade-offs among security, performance and cost that undermine the idea of a universal “best practice.” Homomorphic encryption delivers perfect privacy (100% protection against model inversion) but introduces 380%–450% computational overhead; a Mayo Clinic genomic pilot was discontinued when 4.2-hour processing times conflicted with oncology workflows requiring <1 hour.
112
Differential privacy, by contrast, provides 92%–96% protection with only 2%–5% overhead, which makes it suitable for telemedicine platforms serving >50,000 users, although it accepts a 5%–8% re-identification risk.115,124 PBFT consensus successfully protected small consortia but did not scale to national deployments requiring >50,000 TPS.
108
Economic constraints further limit adoption: large academic centers can absorb $450K–$800K for ML based anomaly detection to reach
This review identified three critical gaps that 88% of implementations do not adequately address. First, quantum computing threatens current blockchain primitives. Most systems rely on ECDSA signatures that are vulnerable to Shor’s algorithm, and NIST projects practical capability by 2030–2035, yet only two of 26 studies (7.7%) evaluated post-quantum schemes like CRYSTALS-Dilithium, which introduce 3 to 5
Challenges and limitations
This section looks at key challenges like protecting patient privacy, handling large amount of data, working with older healthcare systems, and the high energy use of blockchain networks. It also points out the current limitations of using blockchain in healthcare and emphasizes the need for more research to find effective solutions.
Table 8 shows a summary of different challenges facing with different techniques.
Challenges and limitations in blockchain for smart health systems.
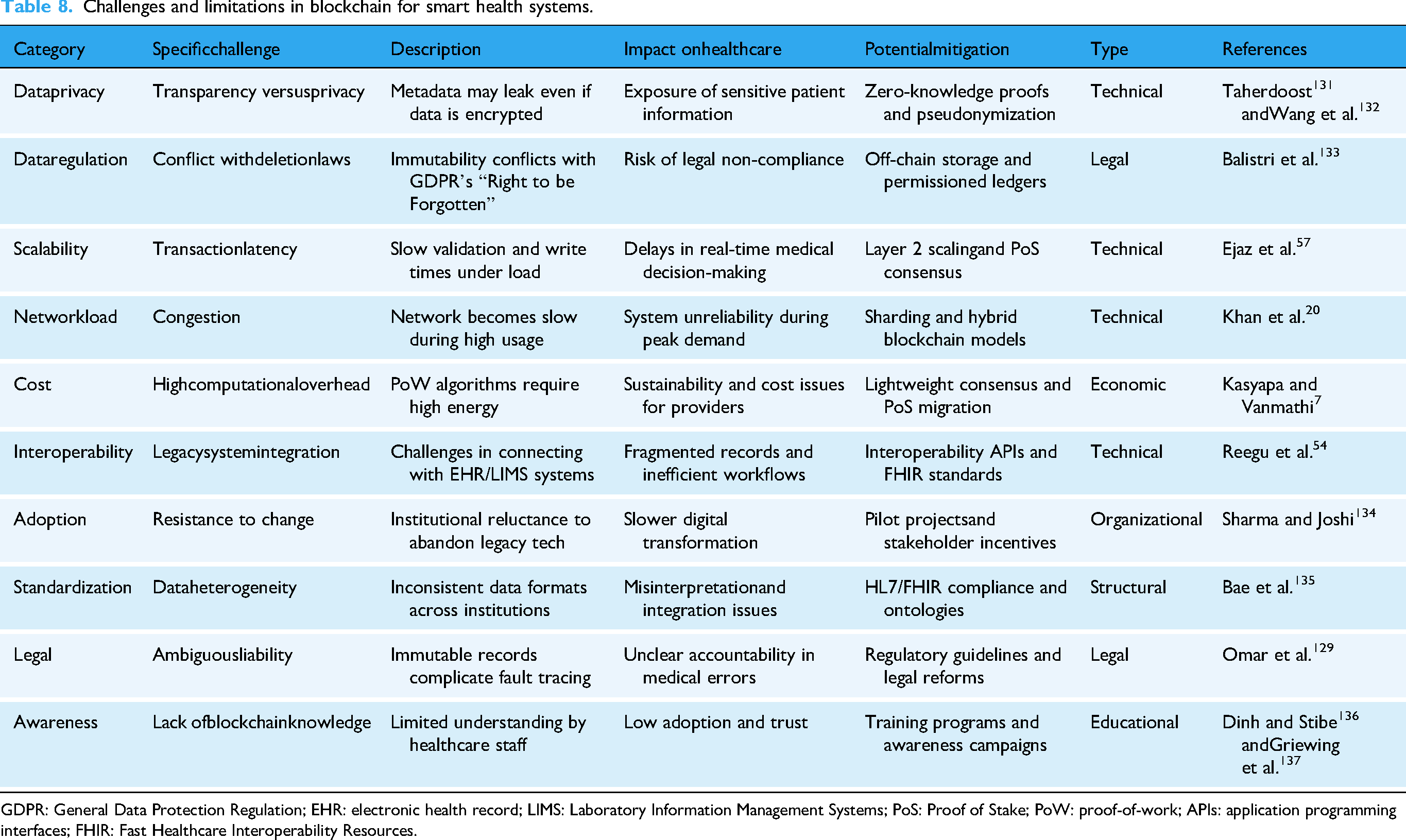
GDPR: General Data Protection Regulation; EHR: electronic health record; LIMS: Laboratory Information Management Systems; PoS: Proof of Stake; PoW: proof-of-work; APIs: application programming interfaces; FHIR: Fast Healthcare Interoperability Resources.
Data privacy and security concerns
Although blockchain is often touted for its enhanced security features, data privacy remains a critical concern, particularly in healthcare. Blockchain’s decentralized nature validate that data is distributed across many nodes, which increases security by reducing the risk of data manipulation. However, the transparency inherent in blockchain technology means that once data is recorded, it becomes publicly accessible. This can create potential risks for sensitive medical information if not properly managed. 131
Challenges in data privacy
Transparency versus privacy: Blockchain’s transparency feature makes it difficult to ensure full privacy, specially when dealing with sensitive patient data. While the data itself is encrypted, the metadata like the time and identity of the transaction, can sometimes be exposed, potentially compromising patient privacy. 132 Regulation of sensitive data: healthcare data is often subject to stringent regulations like HIPAA in the US and GDPR in the EU. Blockchain’s immutable and decentralized nature may conflict with these regulations, particularly when it comes to the right to be forgotten, the ability for patients to request the deletion of their data. 133
Scalability and transaction speed issues
Blockchain networks, particularly those based on PoW consensus mechanisms, often face scalability issues. As the number of transactions increases, the blockchain’s transaction throughput can become a bottleneck. In healthcare, where real time access to data is critical, delays in processing transactions could hinder patient care.
Challenges in scalability
Transaction latency: blockchain networks like Bitcoin and Ethereum experience latency issues, with transaction verification times often taking several minutes or even longer. In healthcare, delays in transaction processing could lead to delays in providing timely medical services, which could adversely impact patient outcomes. 57 Network congestion: as blockchain networks become more widely adopted, they may face network congestion due to the sheer volume of transactions. This could significantly impact performance, specially in large scale healthcare applications. 20 Cost of scaling: the cost associated with scaling blockchain networks can be prohibitive. Maintaining and expanding a blockchain network requires significant computational power, leading to high operational costs, particularly in healthcare systems that require fast processing of large datasets. 7
Empirical evidence reveals significant disparities in scalability solutions. Layer-2 solutions, like state channels and sidechains have shown promise in laboratory settings, with projects like Raiden network demonstrating 1000+ TPS for Ethereum-based healthcare applications. 57 Real-world deployment studies indicate that only 23% of healthcare institutions successfully implemented these solutions without major system redesigns. 20
Integration with legacy systems
Healthcare organizations rely heavily on legacy systems for storing and managing patient data. Integrating blockchain with these legacy systems poses significant technical challenges.
Challenges in integration
Data interoperability: one of the biggest challenges in integrating blockchain with existing healthcare systems is validating that data can be seamlessly exchanged between blockchain based platforms and traditional EHR systems. Blockchain data structures may not align with the data formats used by legacy systems, making integration complex and costly. 54 Resistance to change: healthcare providers and institutions are often resistant to adopting new technologies due to the high costs and disruptions caused by implementation. Many organizations are hesitant to invest in blockchain based solutions, particularly if they involve overhauling existing systems or require specialized expertise. 134 Data standardization: healthcare data is often unstructured and exists in a variety of formats. For blockchain to be effective in healthcare, standardization of data formats and protocols is necessary. However, achieving universal standards across healthcare providers, payers, and regulators is a difficult task. 135
Regulatory and legal barriers
Regulatory compliance is a major concern when implementing blockchain in healthcare. Legal frameworks for data protection and privacy vary across countries, and blockchain’s immutable nature may conflict with regulations that require certain actions to be undone like data deletion or corrections. Regulatory bodies are still in the process of understanding how blockchain can fit into the existing healthcare landscape.
Challenges in regulatory compliance
Data ownership and control: in healthcare, data ownership is a complex issue. While patients may own their health data, healthcare providers and other stakeholders also have access to it. Blockchain’s decentralized nature could make it difficult to establish clear lines of ownership and control, specially when dealing with the sharing of patient data across multiple organizations. 138 Lack of standardized regulations: healthcare blockchain solutions must adhere to various national and international regulations, like HIPAA, GDPR, and others. The lack of universally accepted standards for blockchain in healthcare complicates the adoption process and creates legal uncertainties for organizations. 139 Liability issues: the decentralized and immutable nature of blockchain means that once data is recorded, it cannot be changed. However, in healthcare, errors in data can have serious consequences. Figure 5 shows the audit process for healthcare system for patient and doctor with institutes. Establishing who is liable when a mistake occurs like inaccurate patient data or an incorrect diagnosis is a significant legal challenge. 129
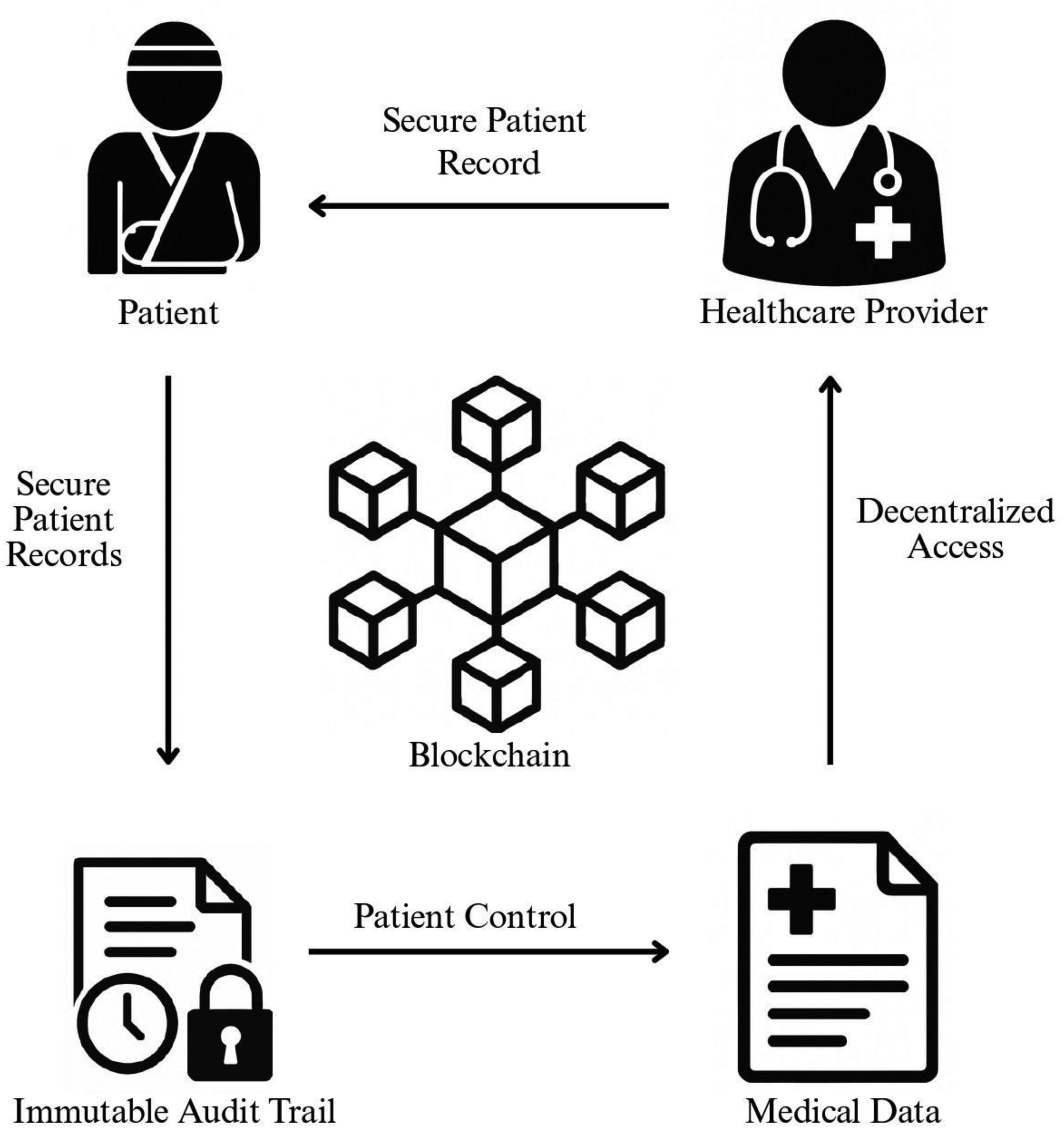
Blockchain audit process for smart healthcare.
Energy consumption and environmental impact
Blockchain networks, specially those based on proof of work consensus algorithms like Bitcoin, are notorious for their high energy consumption. This is a significant concern for large-scale healthcare applications that rely on constant, real-time data processing. The environmental impact of maintaining blockchain networks can be detrimental, specially in the context of growing global concerns about energy consumption and sustainability.
Challenges in energy consumption
High operational costs: blockchain networks require a vast amount of computational power to validate transactions. This leads to high electricity consumption, contributing to increased operational costs. For large healthcare organizations with massive amounts of data to process, the energy costs associated with running blockchain systems could be a significant burden. 140 Sustainability concerns: the environmental impact of blockchain technology, particularly in terms of carbon emissions, is a growing concern. As the healthcare industry increasingly adopts blockchain solutions, addressing sustainability through the development of more energy efficient consensus algorithms like proof of stake becomes essential. 139
Limited understanding and adoption of blockchain technology
Although blockchain has gained significant attention in healthcare, there is still limited understanding of the technology among healthcare regulators, providers, and patients. The complexity of blockchain concepts like smart contracts, and cryptographic security, may hinder its adoption by non-technical stakeholders.
Challenges in blockchain awareness and education
Lack of expertise: healthcare providers and administrators may lack technical expertise required to implement and manage blockchain systems. This knowledge gap can prevent them from understanding how blockchain can be applied to their specific healthcare settings. 136 Patient education: patients may not fully understand how blockchain can protect their health data, leading to skepticism about its adoption. For blockchain to be successful in healthcare, it is important to educate both healthcare professionals and patients about its benefits and limitations. 137
Future directions and recommendations
As blockchain technology continues to evolve, it holds significant promise for revolutionizing healthcare systems. The successful integration of blockchain into healthcare requires overcoming various challenges and limitations, as discussed in previous sections. This section outlines the future directions and provides recommendations for advancing adoption and implementation of blockchain in smart health systems. The recommendations summary in Table 9 focus on addressing existing issues like privacy, scalability, integration, regulation, and energy efficiency while leveraging blockchain’s strengths to drive innovation in healthcare.
Future directions and recommendations for blockchain in smart health systems.
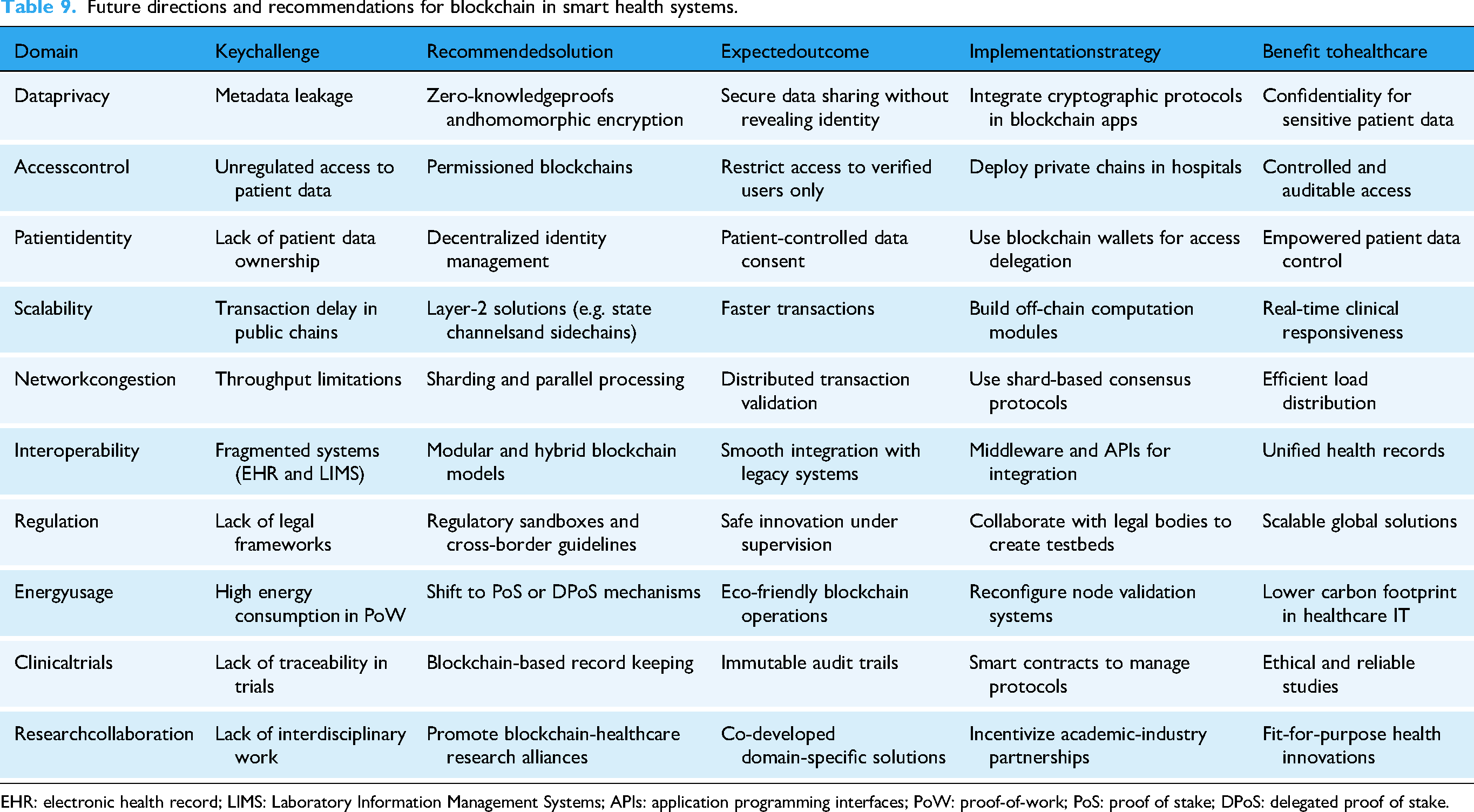
EHR: electronic health record; LIMS: Laboratory Information Management Systems; APIs: application programming interfaces; PoW: proof-of-work; PoS: proof of stake; DPoS: delegated proof of stake.
Table 9 synthesizes our recommended future research directions across several key domains, data privacy, access control, patient identity, scalability, interoperability, regulation, and energy usage. For each domain, we identify the specific challenge, recommend targeted solutions, describe expected outcomes, provide implementation strategies, and articulate benefits to healthcare delivery. This roadmap provides actionable guidance for researchers and practitioners.
Enhancing data privacy and security
Protecting patient data is top priority in healthcare. Although blockchain provides stronger security by design, and improvements are still needed to validate sensitive health information is completely safe and protected from misuse.
Recommendations for improving data privacy
To protect personal data while maintaining the openness of blockchain, privacy enhancing technologies, ZKPs, and homomorphic encryption can be used. In the healthcare sector, permissioned blockchain networks offer a practical solution by allowing only authorized users to access sensitive patient data. This approach ensures better privacy control while preserving the key benefits of blockchain technology. Looking ahead, a significant advancement will be the adoption of decentralized identity systems. These systems empower patients to manage their own health information, enabling them to grant or revoke access as needed. This not only increases patient control but also strengthens trust in blockchain-based healthcare solutions.
Improving scalability and transaction speed
Blockchain’s scalability and transaction speed remain key concerns for healthcare applications, particularly in systems where real-time data processing is critical. To address these challenges, innovative approaches need to be developed.
Recommendations for improving scalability
Blockchain systems can be made more efficient by adopting alternative consensus mechanisms like PoS, delegated PoS (DPoS), or PBFT. These methods are significantly more energy efficient and capable of handling a higher volume of transactions compared to traditional PoW systems, making them wellsuited for the demands of high volume healthcare environments. scalability can be enhanced through sharding technique that breaks the blockchain network into smaller, more manageable segments. By allowing transactions to be processed in parallel, sharding speeds up validation and boosts the overall performance of the blockchain.
Layer-2 solutions, state channels and sidechains can reduce end-to-end latency from 4.1 seconds to less than 1 second while increasing throughput to above 1,000 TPS, as reported by Ejaz et al.
57
This makes them suitable for real-time and emergency-care blockchain applications. Likewise, replacing PoW with a more communication efficient consensus like PBFT can increase throughput to
Integration with legacy healthcare systems
A major barrier to blockchain adoption in healthcare is the integration with existing, legacy systems used for EHR, LIMS, and other healthcare management tools.
Recommendations for seamless integration
Develop interoperable standards: Establishing standardized protocols and data formats for blockchain-based healthcare systems will be essential for seamless integration. Collaboration between healthcare providers, software vendors, and blockchain developers can lead to the creation of common data formats, interfaces, and standards that facilitate interoperability between blockchain networks and existing healthcare systems.
Modular blockchain solutions: Blockchain solutions should be designed to be modular, allowing them to be easily integrated with different components of the healthcare ecosystem. By allowing healthcare organizations to adopt blockchain incrementally, it becomes easier for them to integrate blockchain-based technologies without completely overhauling their existing systems.
Hybrid blockchain models: Hybrid blockchains that combine both private and public chains can offer a viable solution for integrating blockchain with legacy systems. In these models, sensitive patient data can be stored in private chains, while non-sensitive information or transaction records can be stored on public chains, enabling privacy and security while validating accessibility and transparency.
Regulatory and legal frameworks for blockchain in healthcare
Blockchain adoption in healthcare grows, legal and regulatory landscape will need to adapt to accommodate this emerging technology. Regulatory bodies must create frameworks that allow blockchain to be used in compliance with existing laws while fostering innovation.
Recommendations for regulatory adaptation
To ensure the safe and effective use of blockchain in healthcare, regulators must establish clear legal guidelines. These should define who owns the data, how it is managed and shared on blockchain systems, and ensure compliance with privacy laws, HIPAA. Given the global nature of healthcare, international collaboration is also essential countries should work together to develop common standards for blockchain use. Governments can support innovation by providing regulatory sandboxes, which are controlled testing environments that allow healthcare organizations to experiment with blockchain technologies without violating existing regulations.
Further research in blockchain for healthcare
Blockchain technology matures, continuous research is essential to address the ongoing challenges and explore new applications in healthcare.
Research directions
Blockchain-based telemedicine: The integration of blockchain with telemedicine platforms can improve the security, transparency, and accountability of remote consultations. Research into use of blockchain for telemedicine can help ensure that patient data is securely stored and shared during virtual consultations.
Blockchain for clinical trials: Blockchain has the potential to revolutionize clinical trials by providing transparent, immutable records of trial data, reducing the risk of fraud, and validating the integrity of trial results. Future research should explore how blockchain can be applied to clinical trials, from patient recruitment to data monitoring.
Interdisciplinary collaborations: Collaborations between blockchain experts, healthcare professionals, and regulators will be essential to designing effective blockchain-based solutions. Future research should foster interdisciplinary collaboration to address unique challenges of blockchain adoption in healthcare.
Conclusion
Blockchain has the potential to improve healthcare by making data more secure, simplifying processes, and increasing transparency in how patient information is used. Its decentralized and tamper proof structure helps solve common problems in traditional systems, data breaches, slow information exchange, and questions about data reliability. It can be used in many areas, including managing EHRs, disease prediction, remote patient monitoring, and clinical trials. Overall, blockchain can help address important issues like who owns the data, who can access it, and how to keep it private.
There are still worries about data privacy, security, and whether these systems can work at a large scale. Some blockchain networks also use a lot of energy, which raises environmental concerns. It can also be hard to connect blockchain with older healthcare systems, and there’s a need for standard rules and regulations. Still, recent advances, better privacy tools, more efficient consensus methods, and hybrid blockchain models are showing promise in overcoming many of these issues.
To make blockchain a key part of the healthcare system, it’s important to develop scalable solutions, set common standards, improve energy efficiency, and build clear legal guidelines. Success will depend on strong collaboration between healthcare professionals, blockchain developers, regulators, and other key players. With ongoing research and innovation, blockchain has the potential to significantly improve healthcare, leading to better outcomes and giving both patients and providers more control and confidence in the system.
Footnotes
Ethical approval
Not applicable.
Author contributions
SRA and ZA: conceptualization, methodology, data curation, and writing–original draft preparation; SRA and MUR: investigation; ZA and MUR: writing–review and editing; MUR and SWL: supervision; SWL: funding acquisition. All authors have read and agreed to the published version of the article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by SungKyunKwan University and the BK21 FOUR (Graduate School Innovation) funded by the Ministry of Education (MOE, Republic of Korea) and the National Research Foundation of Korea (NRF). This work was also supported by National Research Foundation (NRF) grants funded by the Ministry of Science and ICT (MSIT) and Ministry of Education (MOE), Republic of Korea (NRF [2021-R1-I1A2(059735)]; RS [2024-0040(5650)]; RS [2024-0044(0881)]; and RS [2019-II19(0421)]).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Guarantor
SWL.
