Abstract
Background
The development of artificial intelligence (AI), machine learning (ML) and deep learning (DL) has advanced rapidly in the medical field, notably in trauma medicine. We aimed to systematically appraise the efficacy of AI, ML and DL models for predicting outcomes in trauma triage compared to conventional triage tools.
Methods
We searched PubMed, MEDLINE, ProQuest, Embase and reference lists for studies published from 1 January 2010 to 9 June 2022. We included studies which analysed the use of AI, ML and DL models for trauma triage in human subjects. Reviews and AI/ML/DL models used for other purposes such as teaching, or diagnosis were excluded. Data was extracted on AI/ML/DL model type, comparison tools, primary outcomes and secondary outcomes. We performed meta-analysis on studies reporting our main outcomes of mortality, hospitalisation and critical care admission.
Results
One hundred and fourteen studies were identified in our search, of which 14 studies were included in the systematic review and 10 were included in the meta-analysis. All studies performed external validation. The best-performing AI/ML/DL models outperformed conventional trauma triage tools for all outcomes in all studies except two. For mortality, the mean area under the receiver operating characteristic (AUROC) score difference between AI/ML/DL models and conventional trauma triage was 0.09, 95% CI (0.02, 0.15), favouring AI/ML/DL models (
Conclusions
This review demonstrates that the predictive ability of AI/ML/DL models is significantly better than conventional trauma triage tools for outcomes of mortality, hospitalisation and critical care admission. However, further research and in particular randomised controlled trials are required to evaluate the clinical and economic impacts of using AI/ML/DL models in trauma medicine.
Introduction
Technological innovation has been at the forefront of recent global development. Arguably the fastest rate of development has been in the field of artificial intelligence (AI), especially in the medical profession. 1 AI refers to the capability for inhuman systems to make decisions based on input data (Figure 1). 2 Machine Learning (ML) is a branch of AI that aims to create decision-making algorithms that gradually improve as they are exposed to data. 2 The algorithms are then able to recognise vital data motifs for given outcomes which are subsequently stored in model parameters—set values which determine how the model stores and processes data. Deep learning (DL) is a further subset which creates models capable of learning and applying complex data patterns.2,3

Diagrammatic representation of the relationship between artificial intelligence, machine learning and deep learning. AI: artificial intelligence; ML: machine learning; DL: deep learning.
Most AI models are created using a specific structure, beginning with inputting data from a large database to develop a model with the ability to generate a useful output. This is often used to solve a pre-defined objective. In medicine, these objectives can be patient diagnosis or prognosis, 4 drug discovery 5 or note transcription. 6 AI is commonly employed in visually oriented specialties, such as dermatology, to assist clinicians in detecting skin cancer4,7; ophthalmology, for identification and grading of diabetic retinopathy; or radiography, to analyse chest radiographs.8–10 However, an underexplored area in which AI may be able to play a major role is in trauma triage.
Triage is the categorisation of patients by healthcare professionals based on the severity of their injuries. 11 This ensures patients are at the right location with the right resources, at the right time, and are given the correct management.12,13 Patients with the greatest risk of preventable adverse outcomes are categorised as Priority 1 (P1); therefore urgent and accurate identification of such patients is vital. 12 Optimal triage limits preventable disability and death and avoids the overburdening of emergency departments. 14 Incorrect triage leads to over-triage, when non-critically injured patients are transferred to higher level facilities or under-triage, when critically injured patients are not transferred to a specialised trauma team.15,16 Either consequence results in poor patient outcomes, misallocation and overwhelming of emergency and surgical resources. 17
Currently, conventional triage tools such as the National Early Warning Score, Modified Early Warning Score, Revised Trauma Score (RTS), Trauma and Injury Severity Score (TRISS) and many more are used by physicians depending on hospital guidance.18,19 All triage tools require basic physiological data such as respiratory rate, systolic blood pressure, heart rate, capillary refill time and Glasgow Coma Scale.12,19 Physicians are then able to merge this knowledge with diagnostic reasoning to determine the patient's potential trauma outcomes and triage destination. This is commonly through the analytical reasoning approach, combining previous knowledge and experience with existing data to make decisions. 20
However, a limitation of using triage tools is the dependence on the physician's decision making. Whilst this is often accurate, it can be compromised due to the high levels of stress common in trauma care. In addition, certain triage tools require detailed physical examinations or history taking, which may be susceptible to physician variability. 21 This creates a system where the accuracy of triage tools is dependent on a physician's level of experience and skill.
Utilising the prognostic predictive abilities of AI, ML and DL, combined with the increasing availability of large trauma databases such as the Trauma Audit & Research Network 22 may offer an avenue to overcome the limitations of conventional triage tools. Whilst there is a review by Liu, 2014 which evaluates ML for predicting outcomes in trauma, 23 there are no systematic reviews to date which analyse the effectiveness of various AI, ML and DL models in trauma triage. Therefore, this systematic review aimed to critically appraise the effectiveness of AI, ML and DL models at predicting outcomes in trauma triage. A meta-analysis was further performed to assess the accuracy of AI, ML and DL models predicting outcomes of mortality, hospitalisation and critical care admission compared to conventional triage tools.
Methods
Search strategy and selection criteria
This systematic review and meta-analysis was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines. 24 The systematic review was not registered in PROSPERO or any other database.
Two reviewers (OA and ZA) independently searched PubMed, Ovid MEDLINE, ProQuest and Embase databases for primary research published from 1 January 2010 to 9 June 2022. The search was performed on 9 June 2022. A tailored systematic search strategy consisting of Medical Subject Headings (MeSH) including keywords such as ‘triage’, ‘artificial intelligence’, ‘deep learning’ and ‘machine learning’ was created for each database. The full search strategy for all the databases is found in Table 1. OA also examined the bibliographies of relevant articles identified during the initial search for additional studies.
Search terms for all databases.

The inclusion criteria were studies which evaluated the use of AI, ML or DL models for trauma triage and compared their effectiveness to conventional trauma triage tools or other AI/ML/DL models. Studies which used AI/ML/DL models for other uses except trauma triage or studies which only developed AI/ML/DL models without validation or testing were excluded. This review was limited to human studies regardless of age, gender, ethnicity or primary presenting complaint. Randomised controlled trials, observational studies, cohort studies and case series were included. Studies with animal subjects or presenting duplicate data were excluded. A detailed selection criteria can be found in Table 2.
Detailed inclusion and exclusion criteria.

After removal of duplicate studies; title and abstract screening of remaining studies was performed by OA and ZAB based on the selection criteria, followed by full-text screening. Any disagreements over study selection were resolved through discussion with ZA
Data analysis
The following data was then extracted for all included studies using a data extraction spreadsheet: study design, location, study population, study size, AI/ML/DL model, primary outcomes and secondary outcomes and the comparison trauma triage tool(s) or AI/ML/DL model(s).
The primary outcome for this review was prediction of in-hospital mortality. The main secondary outcomes were the prediction of critical care admission and in-patient hospitalisation. The primary effect measure collected for all outcomes was the area under the receiver operating characteristic (AUROC). It was chosen as it is a quantitative value typically used to evaluate the predictive performance of algorithms. 25
A risk of bias assessment was conducted using the Risk of Bias in Non-randomised Studies of Interventions (ROBINS-I) tool. 26 Three reviewers (OA, ZA, ZAB) independently gave a risk of bias score (Low, Moderate, Serious, Critical) for each of the tool's seven domains for all included studies. The overall risk of bias score for a study was based on the highest score received in any of the seven domains. Any disagreement was resolved through discussion with the senior author (ZA).
Assessment of heterogeneity was conducted by examining the differences across studies for methodological heterogeneity. We used Review Manager (RevMan 5.3, Cochrane Informatics & Technology, London, UK) to determine the
Role of the funding source
There was no funding source for this study.
Results
The initial search from all databases yielded 114 results, with two additional studies identified from other sources. After removal of duplicates, 87 studies underwent title and abstract screening, with 39 subsequent studies undergoing full-text screening. After full-text screening, a further 25 studies were excluded, resulting in 14 studies being included in this review for analysis.27–41 The PRISMA diagram including reasons for exclusion is shown in Figure 2.

PRISMA study selection flow chart.
All included studies were retrospective observational cohort studies, published between August 2014 and July 2022. The studies all compared specific AI/ML/DL models to either current triage tools, other AI/ML/DL models or a combination of both. The total study size across all studies for both the development and validation of the AI/ML/DL models and trauma triage tools was 29,966,339 patients. The population in all studies was trauma patients who were admitted to the emergency department. Three out of 14 studies utilised data exclusively from paediatric patients (<18 years old),27,32,36 whilst the other studies utilised data from only adult trauma patients. An overview of the study characteristics is included in Table 3.
Overview of study characteristics.

Seven studies included in-hospital mortality as an outcome,30,33,35–39 six studies analysed hospitalisation as an outcome29,32,35–37,39 and five studies examined critical care admission as an outcome.34–37,39 Meta-analysis was feasible for all three outcomes of mortality, hospitalisation and critical care admission as more than two studies examined each of these outcomes. All studies performed external validation using a different dataset and used similar numerical outcome measures. 41 The best-performing AI/ML/DL model was compared to non-AI/ML/DL tools for all studies in the meta-analyses for mortality, hospitalisation and critical care admission.
Due to the range of data available on the various trauma databases used to develop the AI models, the studies were able to analyse multiple outcomes. Other outcomes analysed by the studies include prediction of shock, need for early major haemorrhage control surgery, need for early massive transfusion, prediction of injury severity and prediction of the need for life-saving interventions.28,31,40 These outcomes were not eligible for meta-analysis as most were only analysed by one study. The best-performing AI/ML/DL models outperformed their comparator trauma triage tools in all outcomes for all studies analysed except for two studies. The same outcome of mortality was assessed and the same triage tool, and the TRISS was used in both studies in which the trauma triage tool outperformed the AI/ML/DL models.30,38 An overview of all study outcomes and results can be found in Table 4.
Overview of the study outcomes.

Five of the seven studies assessing our primary outcome of mortality reported greater AUROC scores in the best-performing AI/ML/DL model compared to the best-performing conventional trauma triage tools.33,35–37,39 Four of those five studies reported statistically significantly greater AUROC scores in the AI/ML/DL group compared to the non-AI/ML/DL triage group (

Meta-analysis comparing mortality prediction with AI/ML/DL and non-AI/ML/DL tools. AI: artificial intelligence; ML: machine learning; DL: deep learning.
For the secondary outcome of hospitalisation, all six studies reported greater AUROC scores in the best-performing AI/ML/DL model group compared to the conventional trauma triage group.29,32,35–37,39 The AUROC scores in the AI/ML/DL group compared to the non-AI/ML/DL group was statistically significant for four of the six studies (
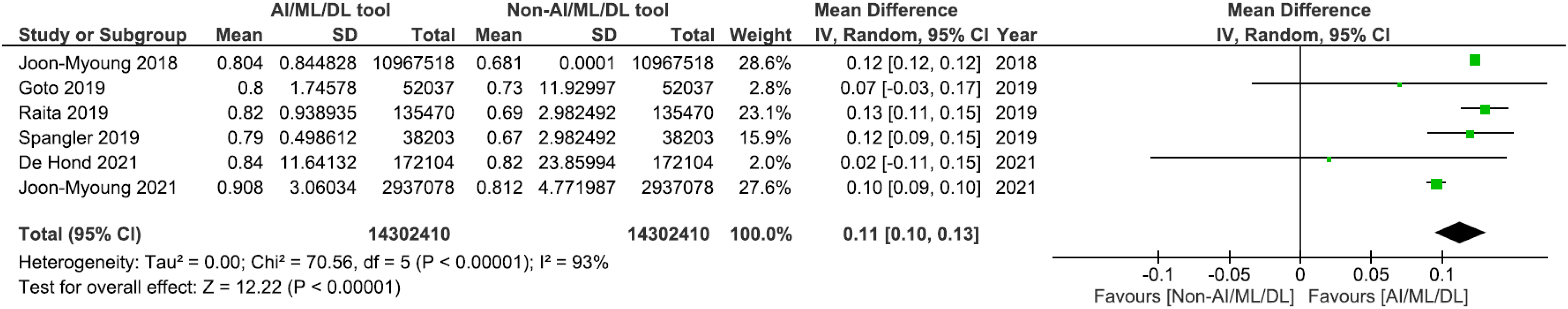
Meta-analysis comparing hospitalisation prediction with AI/ML/DL and non-AI/ML/DL tools. AI: artificial intelligence; ML: machine learning; DL: deep learning.
For the other secondary outcome of critical care admission, all five studies reported greater AUROC scores in the best-performing AI/ML/DL model group compared to the conventional trauma triage group.34–37,39 Three of the five studies reported significantly greater AUROC scores in the AI/ML/DL group compared to the conventional trauma triage tools group (
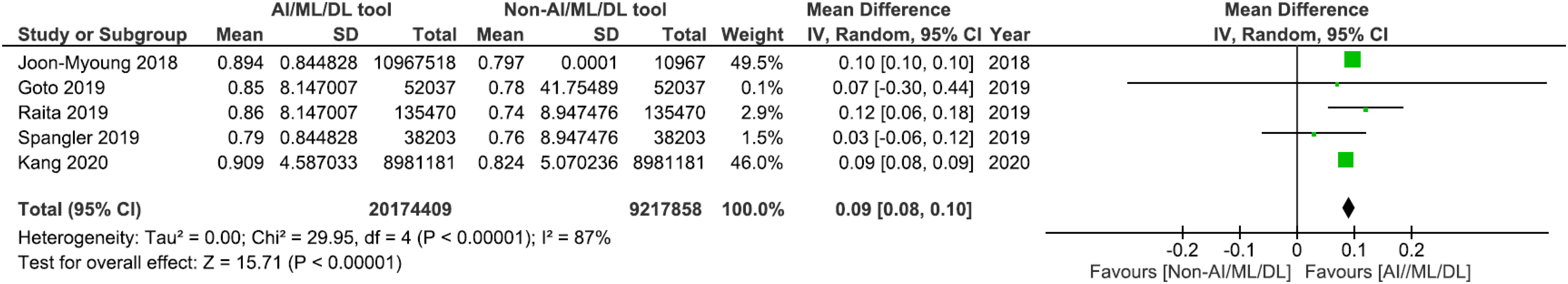
Meta-analysis comparing critical care admission prediction with AI/ML/DL and non-AI/ML/DL tools. AI: artificial intelligence; ML: machine learning; DL: deep learning.
Risk of bias assessment was performed for all 14 studies across the seven domains using the ROBINS-I tool. 26 Overall, 65% studies were judged as having a moderate risk of bias (Figure 6A). All domains except bias due to deviations from the intended interventions had some studies with a moderate risk of bias. Individually, nine studies had a low risk of bias as bias was accounted for through the use of appropriate regression and standardisation (Figure 6B). In particular, the risk of selection bias was counteracted in these studies by comparing patient characteristics and actual outcomes in the derivation/development (non-analytic) cohort and the external validation (analytic) cohort. Five studies were found to have a moderate risk of bias, commonly misclassification bias due to incorrect data imputation/coding errors or confounding bias as a result of inappropriate/lack of regression.

Risk of bias assessment. (a) Summary diagram to show % of articles with bias over the seven domains. (b) Risk of bias in individual studies depicted using the ROBINS-I traffic light plot.
High heterogeneity, due to varying ages, different populations and different AI/ML/DL models in the meta-analyses of all three outcomes was accounted for using random effects models which counteracted both intra-study and inter-study variance. 42 This increased the weighting distribution more evenly compared to using the fixed-effects model.
Discussion
This systematic review and meta-analysis evaluated the ability of AI/ML/DL models to accurately predict trauma outcomes, specifically mortality, hospitalisation and critical care admission. Our results demonstrate that AI/ML/DL models display a better predictive ability for trauma outcomes, particularly mortality, hospitalisation and critical care admission compared to conventional trauma triage tools. Our comprehensive meta-analysis revealed that the difference in predictive ability was statistically significant for all of our outcomes of mortality, hospitalisation and critical care admission. To our knowledge, this is the first systematic review and meta-analysis appraising AI/ML/DL models in comparison to conventional triage tools in the context of mortality, hospitalisation and critical care admission outcomes. These results, therefore, offer a great foundation for the adoption and regular use of AI/ML/DL models in clinical trauma environments.
The overall mean AUROC score differences for the chosen outcomes of mortality, hospitalisation and critical care admission significantly favoured the AI/ML/DL groups compared to the conventional triage tools groups; however, it is important to recognise the difference from the null value was objectively minimal. This suggests the difference between the use of AI/ML/DL for trauma triage at predicting these outcomes is currently statistically significant; however, it is objectively only slightly better compared to the current triage tools. Our meta-analysis for all three outcomes shows that current AI/ML/DL technologies for trauma triage are most effective at predicting hospitalisations as this outcome had the greatest mean AUROC score difference. It can be argued that the ability to predict the other outcomes of critical care admission and mortality have a greater effect on a patient's prognosis.
The results of the meta-analysis for our chosen outcomes signify the potential of a future which has an increased reliance on these AI/ML/DL technologies at predicting mortality, hospitalisation and critical care admission in trauma patients. However, the use of AI/ML/DL for trauma triage is still considered to be in its infancy compared to other well-established methods such as RTS or TRISS.9,10 Given there is still a high probability for improvement of these technologies given the speed of recent advancements in AI, it can be surmised the ability of AI/ML/DL models to predict these outcomes with greater accuracy will vastly improve in the future.
A positive finding of this review was the clear improvement in implementation and utilisation of trauma databases globally. 43 This has been expediated by advancements in health policies, particularly in developing countries, with the establishment of simple, low-cost, electronic trauma databases such as the Nigerian Trauma Registry. 44 Trauma databases are already well proven to provide vital data which can help guide resource allocation, influence injury prevention approaches and monitor changes in an hospital's trauma system performance. 45 This combined with the ability of AI/ML/DL models to process and understand large quantities of data rapidly suggests it is feasible to develop, validate and test AI/ML/DL models tailored to different healthcare systems on a large scale. Before this can become fully widespread, implementation of trauma databases both in developed and developing countries must increase. This requires the promotion of a well-defined population, appropriately trained physicians, a reliable data-collection system and the capacity to analyse, report and validate this data. 46 To accomplish these measures; adequate funding, updated healthcare policies and appropriate resources would be needed, often from government healthcare authorities. Therefore, a future hindrance to the development and implementation of clinical AI/ML/DL models may be a lack of trauma databases.
It is important to highlight that the effectiveness of AI/ML/DL model development is dependent on the choice and type of data acquired from trauma databases. 47 This was particularly evident in the study by Spangler et al. which found that the AI/ML/DL model developed using ambulance data (patient information acquired from the ambulance team) performed better in all outcomes of hospitalisation, mortality and critical care admission compared to the AI/ML/DL model developed using dispatch data (patient information acquired from the original emergency call) (see Table 2). 37 This highlights the importance of having trauma databases with high-quality data as this translates to higher quality AI/ML/DL models. This is vital to account for in customised clinical AI/ML/DL models such as in the study by Nederpelt et al., as the regulation in development may be less stringent. 28 Therefore, it is vital to ensure only the highest quality data is used in model development.
Future development of the best AI/ML/DL systems may require an amalgamation of high-quality conventional triage tools and AI/ML/DL models. This was evident in the study by Kang et al. which assessed a custom DL model, conventional triage tools and a specialised combination of both the custom DL model and conventional triage tools (Ensemble) for the outcome of critical care admission. 34 It was discovered that whilst the custom DL model outperformed the conventional triage tools, the Ensemble models outperformed both the conventional triage tools and the custom DL model in terms of predictive ability for the study's outcome (see Table 2). Utilisation of this notion may be highly effective when AI/ML/DL are combined with conventional triage tools which appear to offer a high predictive ability such as the TRISS triage tool, the only triage tool from all studies which outperformed the AI/ML/DL models.30,38 This introduces the notion that the future of trauma triage may lie not just in the utilisation of AI/ML/DL models but creating methods to integrate the computing power found in these models and the principles of the best-performing conventional triage tools.
This systematic review and meta-analysis has shown that the use of AI/ML/DL models for trauma triage reduces the complexity associated with conventional trauma triage tools which require detailed history taking, physical examinations (e.g. pain score) and physician judgement based on clinical experiences.21,48 Most AI/ML/DL models only require imputation of patient variables such as age, sex, primary complaint, trauma type, comorbidities or mental status to determine potential outcomes. This informs patient triage and ideally leads to better patient outcomes.
Another advantage is the fact that the input variables are basic information which can be quickly collected and therefore do not require clinician judgement as this is all processed by the AI/ML/DL models. This would offer clinicians more time to direct towards performing uniquely human skills such as empathy, communication and broad-view problem solving. This also relieves trauma clinicians of time-consuming duties in a speciality in which many physicians are often over-worked and face burnout.49,50 This would ultimately lead to improved patient outcomes as clinicians would have more time to perform urgent clinical duties and manage patients to the best of their ability.
It is important to note that whilst this systematic review suggests that AI/ML/DL models can predict trauma patient outcomes with greater accuracy compared to current conventional triage tools, it may not yet be met with confidence from clinicians. This can be due to a lack of education on how AI/ML/DL algorithms work. Therefore, educating trauma physicians on the capabilities and the impact AI/ML/DL models can have and would be an important future step to promote widespread implementation of these models.
A vital consideration for future medical AI/ML/DL models is ensuring that they are transferrable to different hospitals or clinical scenarios. However, this presents a conundrum, similar to the “No Free Lunch” theory for optimisation from Wolpert 51 which suggests that if an algorithm is optimised for one situation, it may be difficult for it to produce good results in another situation. When applied to our study, it can be inferred if AI/ML/DL models are developed using a particular dataset in a certain environment; it may limit the transferability of that model to a different environment. A way to account for this is through the implementation of internal and external validation in AI/ML/DL algorithms.
All studies in this systematic review were discovered to have undergone validation, with most studies undergoing external validation, using an independent database. In the context of this systematic review, validation should occur after AI/ML/DL model development and can be repeated multiple times with various databases to improve model performance before testing. 23 A limitation discovered by our systematic review was that there is inconsistency regarding the terminology of validation in various studies. In some studies, the term was used to describe the testing of the final AI/ML/DL models whilst other studies referred to validation as external tuning of the AI/ML/DL models using either an internal or external database.
For future models and studies, we recommend that data cohorts should be clearly distinguished into a development set (to train and develop the AI/ML/DL model), an external validation set (to fine-tune the model using an independent database) and a test set (to assess the performance of the AI/ML/DL model). For external validation to be feasible, data sharing between trauma databases and AI/ML/DL models must be encouraged especially due to the speed at which information evolves on a global scale. However, actions should be taken to ensure the de-identification and anonymisation of patient data in all instances.
Data validation, ideally external, is important as it ensures AI/ML/DL models are able to showcase the same predictive abilities in diverse populations. This could then lead to the creation of specific trauma triage AI/ML/DL models which can be applied to various populations, similar to AI models used in dermatology to assist clinicians in skin cancer diagnosis.52,53 Applying the combination of using trauma databases for AI/ML/DL development, internal/external validation and the testing of the models should lead to the creation of a general medical AI/ML/DL algorithm. A custom diagram detailing a template for the creation of future trauma AI/ML/DL algorithms can be found in Figure 7.

AI/ML/DL algorithm template. AI: artificial intelligence; ML: machine learning; DL: deep learning.
In terms of progression from the results of this systematic review and meta-analysis, the next steps for future research should be a comparison of individual AI, ML and DL models. This review categorised all models together to enable a better comparison against conventional triage tools. However, it would be important to assess if either AI, ML or DL offer greater predictive ability of outcomes in trauma triage. There are already a wide array of models available such as gradient boosting (XGBoost), a ML algorithm where numerous weak learning classifiers are trained to combine together whilst learning from the results of previous combinations to produce better results or random forest, where learning is gained sequentially and is based on the performance of the previous stages. Different AI/ML/DL use different methods to achieve their specified outcomes. Therefore, it will be of high value to contrast the different methods and analyse for the most effective method.
Methodological deficiencies in this systematic review are primarily due to most studies being retrospective. A result of this means the data collected was not originally meant for research purposes, some databases in studies had missing data which may predispose the studies to confounding bias. However, this was mitigated by these studies through the exclusion of participants with missing data from the AI/ML/DL model development. In addition, the differences between each study created large heterogeneity with the results of our meta-analyses for all three outcomes. This was alleviated by using a random effects model in the meta-analyses. A common limitation of retrospective studies is the requirement of large sample sizes for rare events to be effective. This was easily managed in the studies due to the computing power of AI/ML/DL models which enables processing of large amounts of data.
Another limitation may have been in the effect measure of AUROC due to its deficiency in computing rare events with imbalanced data (where the number of negatives outweighs the positives) such as in-hospital mortality and critical care admission. 39 When using AUROC, the false-positive rate (false positive/total actual negatives) does not dramatically decrease when the total negatives are large.39,54 A more suitable effect measure for imbalanced data would be the area under the precision-recall curve (AUPRC) as it considers the fraction of true positives in positive predictions therefore making it a more precise measure.25,54 However, AUPRC values and graphs are harder to interpret and do not consider true negatives at all, an important consideration for AI research, therefore making it a less popular option for AI/ML/DL researchers.
Thirdly, the differences in variables used in the development of various AI/ML/DL models were another limitation from this review. Whilst key variables such as age, sex and primary complaint were constant in all models, some studies included other variables to contribute to the learning of their AI/ML/DL models. This makes it difficult to ascertain the effect of the different variables on the predictive ability of AI/ML/DL models and how this ability could also change depending on the outcome being tested. Future research should be undertaken to evaluate models developed using different variables and whether this leads to better AI/ML/DL predictive ability for trauma outcomes, in addition to identifying the variables with the greatest impact on predictive ability.
Conclusions
This systematic review and meta-analysis shows that AI/ML/DL models display greater accuracy at predicting key outcomes of mortality, hospitalisation and critical care admission compared to most conventional trauma triage tools. This is still an emerging and improving area of medicine which requires greater research, specifically in the form of prospective studies and randomised controlled trials. In order to benefit clinical policy and improve patient care, aims for future research on the use of AI/ML/DL models in trauma triage should be tailored to evaluating the clinical and economic effects and the potential creation of guidelines for the use of AI/ML/DL in trauma medicine.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076231205736 - Supplemental material for Exploring the effectiveness of artificial intelligence, machine learning and deep learning in trauma triage: A systematic review and meta-analysis
Supplemental material, sj-docx-1-dhj-10.1177_20552076231205736 for Exploring the effectiveness of artificial intelligence, machine learning and deep learning in trauma triage: A systematic review and meta-analysis by Oluwasemilore Adebayo, Zunira Areeba Bhuiyan and Zubair Ahmed in DIGITAL HEALTH
Footnotes
Contributorship
OA conceptualised and designed the study. OA, ZA and ZAB contributed to the literature search. OA and ZAB screened articles for inclusion and performed data extraction. OA performed the data analysis, interpretation, synthesis of findings and wrote the manuscript. OA and ZA performed the statistical analysis. OA and ZAB performed the risk of bias assessments. ZA supervised the paper and contributed to revision of the manuscript. All authors had full access to all the data in the study and have approved the final version.
Declaration of conflicting interests:
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data sharing
All data for this review were obtained from published research. Data extracted for this Review and database search strategies will be made available on reasonable request. For access, please email the corresponding author.
Ethical approval
None
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Guarantor
OA.
Informed consent
Informed consent was not required for this study. All data for this review were obtained from published research which had deidentified all patient information prior to analysis.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
