Abstract
Background
The metaverse, an emerging digital ecosystem that integrates virtual reality (VR) and augmented reality (AR), is gaining increasing attention in the healthcare industry. In Alzheimer's disease and related dementias (AD/ADRD) care, the metaverse offers transformative solutions for cognitive assessment, remote monitoring, caregiver education, and patient engagement.
Objective
A comprehensive scoping review was conducted following the PRISMA Extension for Scoping Reviews (PRISMA-ScR) guidelines to systematically identify, select, and synthesize relevant literature exploring how emerging digital solutions, including digital health and metaverse applications, are addressing clinical challenges associated with AD/ADRD.
Methods
Searches were conducted across online databases including PubMed, IEEE Xplore, ACM Digital Library, and Google Scholar (with a restricted search strategy due to the high volume of available literature), yielding a total of 160 hit results. Of these, 18 relevant articles were selected for in-depth analysis.
Results
Findings highlight that immersive virtual environments enable individuals with AD/ADRD to engage in cognitive training programs and simulations, aiding memory and cognitive function. Additionally, VR-based telemedicine enables patients to consult with healthcare professionals from the comfort of their homes, reducing travel burdens and ensuring continued medical care despite geographical constraints. Beyond direct patient benefits, the metaverse supports caregivers through virtual training, educational resources, and peer networks that help them navigate the complexities of dementia care. Virtual spaces promote social interaction, reducing isolation and enhancing well-being. However, adoption barriers include technological unfamiliarity, cognitive and physical limitations, caregiver concerns, privacy and cost-related challenges.
Conclusion
Personalized technology design, structured learning environments, and caregiver training can enhance adoption and effectiveness. To maximize impact, addressing barriers through education, improved accessibility, and tailored interventions is essential. Future research should explore scalable implementation strategies, assess long-term patient outcomes, and evaluate cost-effectiveness to support widespread adoption.
Keywords
Introduction
Alzheimer's disease and related dementias (AD/ADRD) represent a global health crisis with profound individual, societal, and economic implications. Characterized by progressive cognitive and functional decline, these conditions primarily afflict older adults, impairing memory, thought processes, and daily functioning. In the United States alone, an estimated five million individuals currently live with AD/ADRD, with prevalence expected to triple by 2050 as the population ages.1,2 Worldwide, over 55 million people are affected, and this figure is projected to double every 20 years. 3 Beyond the staggering numbers, the burden on caregivers, often family members, entails significant physical, emotional, and financial strain, compounded by the need for assistance with activities of daily living and the management of behavioral symptoms as the disease progresses.
Given the profound societal and economic implications of AD/ADRD, national and global efforts have emerged to develop policies and care models aimed at addressing these challenges. The National Institute on Aging (NIA) and initiatives such as the National Plan to Address Alzheimer's Disease (NAPA) seek to create sustainable service delivery systems to meet the needs of both patients and caregivers.4,5 Despite these strides, significant gaps remain in understanding the diverse experiences of individuals with AD/ADRD, particularly within underrepresented populations, where research is sparse. 6 The challenges of AD/ADRD care extend beyond clinical boundaries, encompassing significant barriers to education, diagnosis, and patient engagement. While interventions such as Therapeutic patient education (TPE) have been widely adopted in neurodegenerative disease management for conditions such as Parkinson's disease and multiple sclerosis, its implementation in AD/ADRD care remains limited. The progressive cognitive decline in dementia patients presents unique challenges, as patients may struggle with retaining health information, following structured self-management programs, and engaging in traditional educational interventions. 7 To address these gaps, innovative and less formalized educational strategies are needed to empower patients and caregivers with actionable knowledge, self-management skills, and psychosocial support tailored to their unique circumstances.
Digital health innovations offer unprecedented opportunities to overcome the limitations of conventional care models, including inadequate caregiver support, logistical constraints, and patient engagement barriers. By leveraging real-time data capture, AI-driven insights, and remote monitoring, digital tools can provide a window into the lived experiences of patients and caregivers to enhance care coordination. These innovations align with the goals of initiatives like DATAcc's Core Digital Measures, which connect technology to meaningful patient and caregiver experiences.8,9 Digital health solutions can empower caregivers with actionable insights, alleviate burdens, and ultimately transform the AD/ADRD care continuum. As the global burden of dementia continues to grow, embracing digital measures as part of a comprehensive strategy will be essential in advancing equitable, effective, and sustainable solutions for those affected by AD/ADRD. This review aims to explore how digital health technologies, including cutting-edge innovations like the metaverse, address the clinical, educational, and caregiving challenges associated with AD/ADRD. A scoping review was conducted to methodically present the existing research in this area, the benefits, limitations, and potential of digital health tools to transform care delivery, enhance patient outcomes, and reduce caregiver burden.
Challenges faced by AD/ADRD patients and caregivers
AD/ADRD present multifaceted challenges that impact patients, caregivers, and healthcare systems. The gradual cognitive decline associated with AD/ADRD affects patients’ memory, language, and ability to perform daily activities independently. 10 This deterioration necessitates extensive caregiving support, often placing an immense strain on families. For instance, in 2018 alone, approximately 16.3 million informal caregivers provided 18.6 billion hours of assistance, valued at $244 billion, to individuals with AD/ADRD. 2 The physical and emotional toll of caregiving often leads to neglect of caregivers’ own well-being. The continuous need for vigilance and support highlights the urgent need for interventions that address the unique challenges faced by caregivers of individuals with AD/ADRD.
The economic implications of AD/ADRD are another critical concern. The financial strain includes medical costs, non-medical expenses, and lost productivity among caregivers. 11 Communication deficits present a further obstacle which significantly impact patients’ quality of life affecting language use, functional communication, and social interactions. Studies have shown that both pharmacological treatments (e.g., memantine and cholinesterase inhibitors) and non-pharmacological approaches (e.g., cognitive-linguistic stimulation) have shown promise in addressing these issues.12–14 However, caregivers also highlight barriers to accessing respite care and maintaining consistent communication with healthcare providers. Addressing these gaps requires proactive support models that integrate caregivers into care planning, provide tailored resources, and enhance communication with healthcare professionals. 15 In this context, digital technologies offer a promising solution, enabling more efficient care coordination and real-time support. These innovations not only alleviate caregiver burden but can also provide cognitive offloading, automation, remote monitoring, emotional support, and significant patient independence. 16
Advancing care through a virtual health system
As digital health technologies continue to evolve, an integrated virtual health system could further enhance support for caregivers by centralizing resources, improving coordination, and reducing caregiving burden (Figure 1). To fully support caregivers and streamline AD/ADRD care, a comprehensive virtual health system could be developed, integrating key features tailored to their needs:
Centralized Caregiver Platform: A dedicated virtual health system should offer a centralized dashboard where caregivers can access patient medical information, track medication schedules, and receive reminders. This would improve organization and coordination between caregivers, patients, and healthcare providers. Social & Emotional Support: The platform should feature peer support groups, forums, and virtual meetups where caregivers can connect, share experiences, and seek guidance. Mental health resources, such as teletherapy and guided stress-relief exercises, can further help caregivers manage emotional strain. AI-Driven Education & Guidance: A built-in AI-powered assistant can provide caregivers with personalized content, educational videos, and condition-specific guidance, helping them make informed decisions. This ensures they stay updated on best practices without overwhelming them with excessive information. Integrated Communication Tools: Seamless communication between caregivers, healthcare professionals, and patients is essential. The system should support emergency response features for critical health events, support secure messaging and video calls with doctors, and provide automated updates and alerts for medication and appointments. Caregiver-Enabled Patient Management: The platform should allow caregivers controlled access to the patient's digital health records, enabling them to review medical history, track vital signs through wearable health devices and set up medication and appointment reminders. A well-designed virtual health system integrating these elements would bridge the gap between caregivers, patients, and healthcare providers, reduce their stress, and ultimately improve patient outcomes. Such a system would enhance adherence to treatment and foster emotional support.
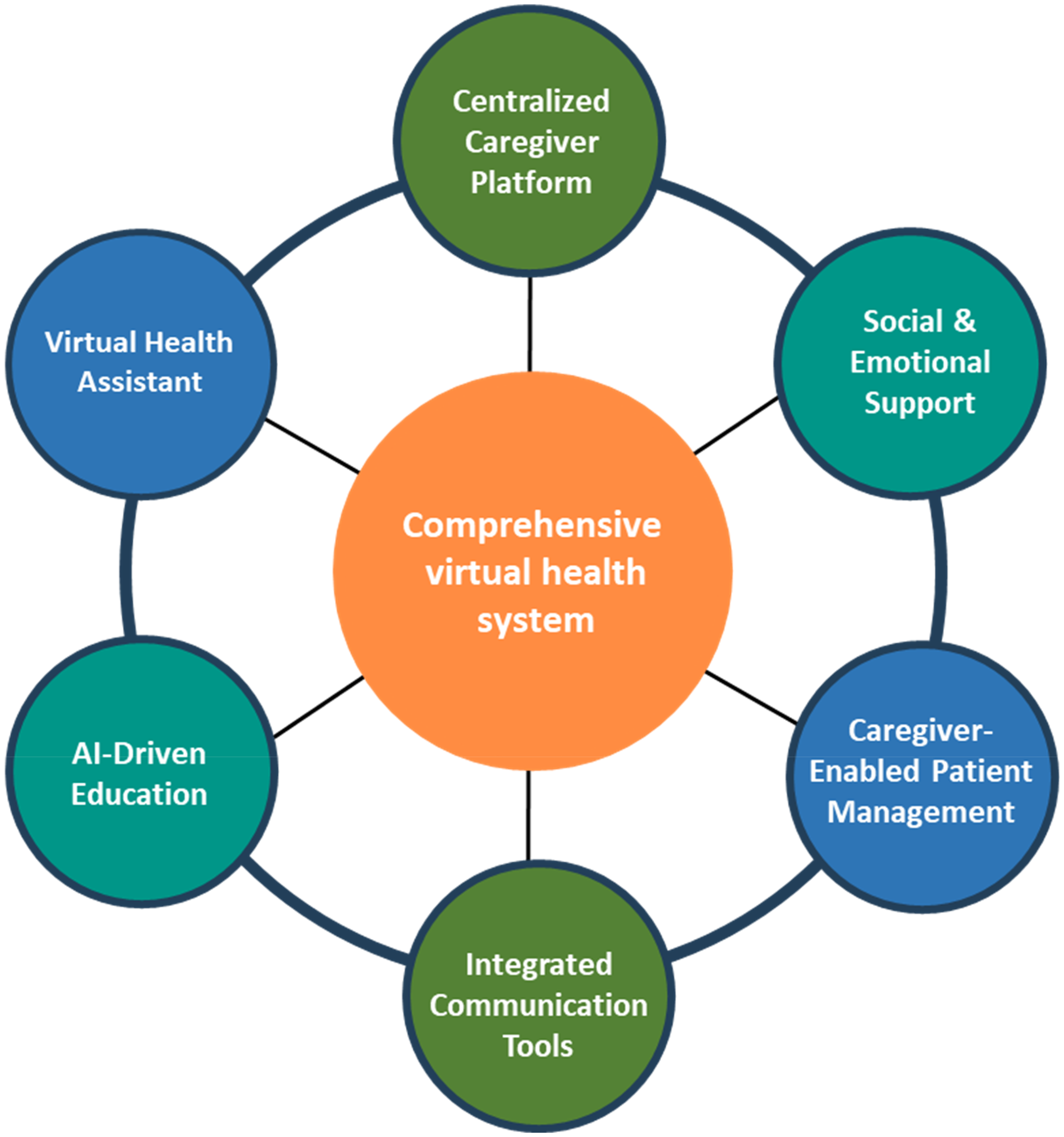
Infographic representing the virtual health ecosystem bridging the gap between caregivers, patients, and healthcare providers like a centralized dashboard, social support, AI-driven assistance, communication tools, and patient management.
The metaverse: a new frontier in dementia care
Beyond conventional digital health tools, the metaverse is emerging as a transformative technology that integrates artificial intelligence (AI), augmented reality (AR), virtual reality (VR), blockchain, and the Internet of Things (IoT) to create immersive, interactive, and interconnected digital environments. 17 Initially conceptualized for entertainment and social interactions, its applications have expanded across various domains, including education, business, and healthcare. By seamlessly blending digital and physical realities, the metaverse facilitates real-time, multisensory experiences that redefine communication, collaboration, and service delivery. 18
The rapid advancement of metaverse technology is driven by several key factors, including technological convergence, the rise of remote interactions during the COVID-19 pandemic, and the increasing demand for immersive learning experiences. 19 In academic and professional training, metaverse-based AR and VR simulations enhance learning experiences, skill acquisition, and collaborative problem-solving. 20 Beyond these technical applications, the metaverse addresses pressing societal challenges such as loneliness, which affects nearly two billion individuals worldwide. By fostering virtual communities, it enhances social engagement and psychological well-being. 21
Healthcare is one of the most promising domains for metaverse integration, where it offers solutions for medical education, telemedicine, patient monitoring, and personalized care. By merging the Internet of Medical Things (IoMT) with VR/AR technologies, the metaverse enables real-time interactions between virtual specialists, cloud-based medical experts, and terminal users, optimizing healthcare accessibility and efficiency. 19 In medical training, VR-based simulations facilitate surgical practice, remote dissections, and AI-powered clinical education. 17 Telemedicine is further enhanced through VR-enabled consultations, bridging geographical barriers and improving patient-centered care. 22 Additionally, virtual environments support cognitive therapies and social engagement, particularly for individuals with neurodegenerative conditions. 21
The metaverse holds significant promise for AD/ADRD, benefiting both patients and caregivers. VR-based reminiscence therapy immerses patients in familiar past environments, stimulating memory recall and improving emotional well-being. Virtual like CareCompanion can provide personalized support for daily tasks, navigation, and social connectivity, enhancing independence and quality of life for ADRD patients. 23 IoT-integrated wearable devices continuously monitor cognitive and physiological markers, allowing for early detection of disease progression and timely intervention. Furthermore, metaverse provides an interactive platform for caregivers, offering educational resources, peer support, and real-time consultations to alleviate the burden of caregiving.
Research objectives and contributions
We recognize the potential of the metaverse to enhance patient care, cognitive support, and caregiver assistance, and seek to explore how emerging digital solutions are addressing the clinical challenges associated with AD/ADRD. The effective integration of these technologies into dementia care necessitates a thorough examination of their capabilities, applications, and limitations.
To fulfil this objective, this research endeavors to present a scoping review that examines the opportunities, advancements, and challenges in leveraging digital health and metaverse applications for AD/ADRD management. Given the increasing relevance of these technologies in healthcare innovation, this study will analyze recent key developments marked by accelerated digital transformation in response to the pandemic. More specially, Table 1 displays the scoping review questions addressed in this study.
Scoping review research questions addressed in this study.
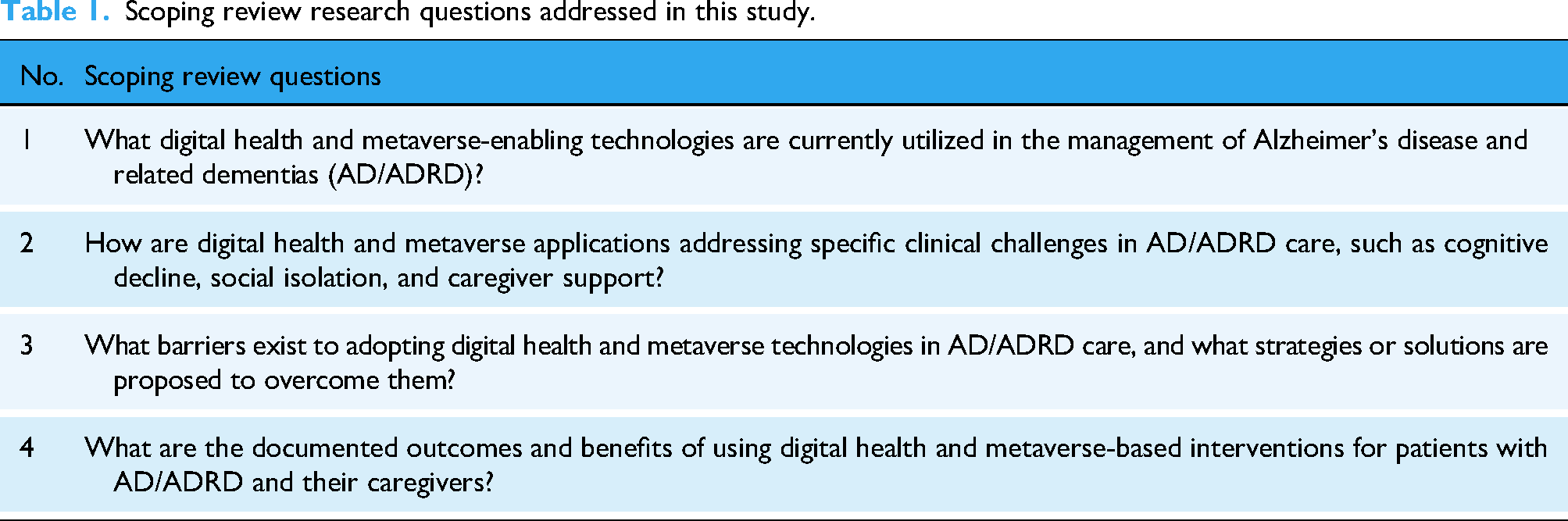
The contributions of this study include:
Identification and analysis of digital health and metaverse technologies currently applied in AD/ADRD management. Evaluation of how these technologies address clinical challenges such as cognitive decline, social isolation, and caregiver burden. Identification of barriers to adoption and assessment of strategies to enhance the implementation of digital health and metaverse-based interventions. Assessment of documented outcomes and benefits for patients and caregivers, providing insights into the effectiveness and future potential of these innovations.
Paper organization
The rest of the paper is organized into sections reporting the methodology, results and discussion. The next section explains the research methodology we adopted in this study. In the result section, we discuss digital health and metaverse-enabling technologies available for AD/ADRD care as identified in literature. The application of these technologies to address associated clinical challenges is also explored. We then identify barriers to adoption of the metaverse and provide strategies to enhance the implementation of metaverse-based interventions. In the discussion section we address security, ethical, and privacy concerns before discussing the limitation, future direction and provided the conclusion for this study.
Methodology
To address the research questions outlined in this study, we conducted a comprehensive scoping review following the PRISMA Extension for Scoping Reviews (PRISMA-ScR) guidelines. 24 This methodological approach ensures a systematic and transparent process for identifying, selecting, and synthesizing relevant literature related to digital health and metaverse-enabling technologies in the management of AD/ADRD.
Search strategy
A structured search was performed across multiple academic databases, including PubMed, Scopus, IEEE Xplore, ACM Digital Library, and Google Scholar (Table 2). The search queries incorporated a combination of Medical Subject Headings (MeSH) terms and keyword variations to ensure comprehensive retrieval of relevant studies. To refine the search results, automatic filters were applied based on publication date, language, and relevance. Google Scholar results were screened for relevance, with the first 125 studies selected for inclusion due to the high volume of available literature. The search covered studies published between January 1, 2015, and January 31, 2025. Database searches were conducted between January 31 and February 4, 2025, with each database accessed on the specific dates summarized in Table 2.
Number of articles retrieved from the electronic search of databases.

Screening process and eligibility criteria
The selection process was carried out in stages. The first author conducted the initial review, and the second author verified the article sources to ensure consistency and agreement. A total of 160 published papers were retrieved from the electronic search databases (Figure 2). Table 2 shows the number of articles retrieved from each publication database. To refine the results, we applied additional search restrictions, including filtering for peer-reviewed journal articles and conference proceedings, removing non-English publications, and including studies published within the last 10 years (2015–2025). As a result, 114 ineligible articles were removed. Additionally, two duplicate entries were identified and excluded. A total of 44 studies retrieved from the initial search were first screened based on their titles and abstracts. 20 articles that did not explicitly discuss digital health or metaverse applications in AD/ADRD care were excluded. 24 eligible studies from the title and abstract screening phase were then assessed based on full-text availability. Studies were excluded if they only briefly mentioned metaverse technologies without a substantive discussion of their application in AD/ADRD management. After applying the inclusion and exclusion criteria, we identified and retained 18 of the most relevant studies for detailed analysis. Table 3 shows the publication venue of selected papers.

PRISMA flow chat of the included studies.
Publication journal of selected papers.

A summary of the exclusion criteria applied:
Studies not published within the last 10 years. Non peer reviewed publication (grey literature). Non-English publications. Duplicate or more than one article entry. Articles that did not explicitly discuss digital health or metaverse applications in AD/ADRD care. Conference abstracts, theses or dissertations.
A summary of the inclusion criteria applied:
Studies published within the last 10 years (2015–2025). Peer reviewed studies with full-text availability. Studies targeting individuals with cognitive decline or AD/ADRD. Studies that discuss applications digital health and metaverse-enabling technologies to address AD/ADRD challenges. Studies that discuss existing barriers to the adoption of digital health tools and propose solutions to overcome them in AD/ADRD care.
Data extraction
The authors have reported the data charting process in a supplementary excel file. During screening for the 44 articles by reviewing titles and articles, 18 articles were selected as relevant (see supplemental file). The sheet titled “data charting” contained the descriptive variables of the 18 selected studies (author name(s), publication year, journal name, region and research questions) and information addressing the use of digital health and metaverse enabling technology in AD/ADRD care, the challenges observed with the technology adoption and proposed strategic solutions.
Results
State of the art: Digital health and metaverse-enabling technologies in AD/ADRD management
The reviewed studies emphasize the growing digital health and metaverse-enabling technologies applicable in AD/ADRD care (Table 4). The majority were published in Sage journal and frontiers of public health (Table 3). Most studies discussed VR, AR, digital twin technology and the IoT.
Overview of identified studies exploring metaverse applications in AD/ADRD management.

VR and AR
VR applications provide immersive environments for memory and cognitive training, while AR enhances real-world interactions, aiding in patient education and engagement. Six studies emphasize the role of VR in cognitive assessment, rehabilitation, or caregiver education. VR systems vary from non-immersive desktop-based applications to fully immersive environments using head-mounted displays, such as the Oculus Rift DK2, providing interactive simulations for spatial navigation training and therapeutic engagement.25–29 Vienna et al. explored just five eligible studies on VR exposure therapy as a tool for anxiety treatment and neuropsychological assessment in participants living with dementia with symptoms ranging from early to severe stages. The feasibility for utilizing both semi and fully immersive VR technology to increase alertness and pleasure in early stages of dementia was confirmed when performed outside the hospital setting. 25 However, one study reported an increase in fear and anxiety with the use of VR in dementia, hence raising concerns about safety and ethical implications of its use for dementia patients. Additionally, AR and VR are recognized for their role in sensory input customization and cognitive engagement. 28 These technologies enable the development of personalized, immersive, and controlled sensory experiences, optimizing interventions for individuals with sensory modulation challenges and dementia. Through gamified cognitive exercises and virtual reminiscence therapy, AR fosters cognitive stimulation and emotional well-being in aging populations. Additionally, therapists can leverage these advancements to tailor sensory inputs, enhance intervention efficacy, and precisely monitor patient progress.
Digital twin technology and AI in AD diagnosis
Digital twins particularly when integrated with cloud computing and AI, offer transformative tools for enhancing patient care and monitoring. Currently, digital twins are used to construct dynamic, bi-directional virtual models of real-world hospital environments, equipment, and processes. These models are updated using real-time data from physical sources, such as sensors, medical records, and wearable devices, and are being applied to areas like outpatient and inpatient services, operating rooms, and emergency response systems. These virtual replicas can leverage real-time data from wearable devices to track vital signs such as blood pressure, heart rate, and temperature, and provide continuous monitoring, from wearable devices.30,31
In AD care, AR tools embedded within digital twin platforms enhance usability by overlaying patient-specific data onto physical environments, assisting healthcare providers during diagnosis and treatment. For example, emergency scenarios such as falls or strokes, common in elderly patients, can be simulated in virtual environments using digital twin models that reflect real ambulance layouts, clinical workflows, and virtual representations of physical objects, patients and medical environments. However, despite these promising applications, the use of digital twins in AD care remains in its early stages of development. Limitations include high construction costs, lack of unified data standards, challenges in integrating multimodal data, and constraints in XR device usability. These challenges highlight the need for gradual, collaborative integration across healthcare sectors to build interoperable and effective digital health ecosystems.
Wearable devices and IoT-enabled monitoring for AD/ADRD care
The IoT, alongside wearable health devices, facilitates continuous health monitoring by ensuring real-time data collection, and personalized interventions.28,32 These devices support remote patient tracking, promoting early detection of cognitive decline and ensuring patient safety. Furthermore, telehealth expanded access to dementia care, particularly benefiting individuals with limited mobility or those in remote locations. As illustrated in Figure 3, IoT applications relevant to AD/ADRD care include:
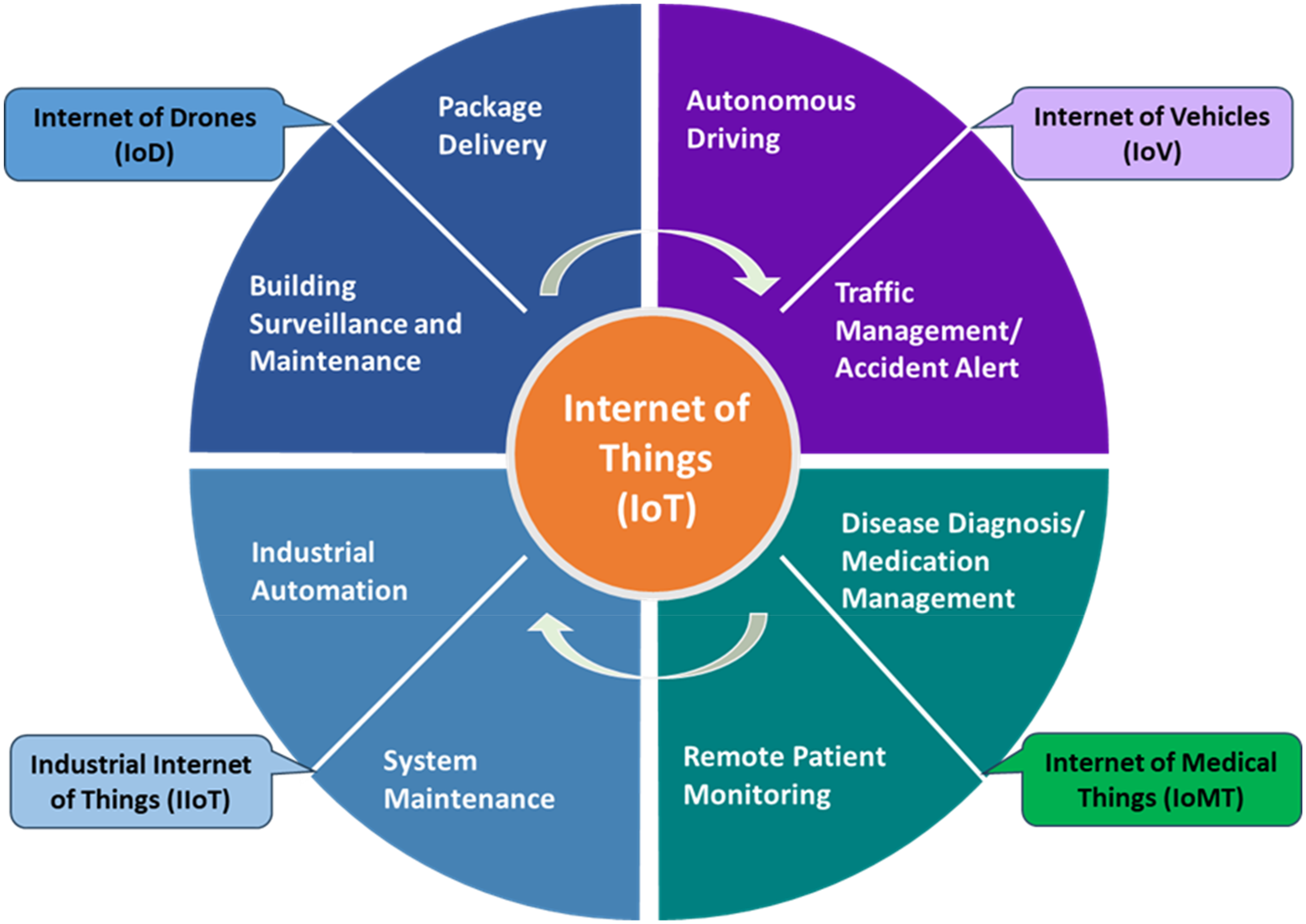
IoT applications for AD/ADRD care.
Internet of medical things (IoMT):
Enables remote patient monitoring, disease diagnosis, and medication management, ensuring patients receive timely interventions while minimizing hospital visits. Smart medical devices, including wearable biosensors, smartwatches, and home-based monitoring systems, track vital signs, sleep patterns, and cognitive function, alerting caregivers to abnormalities in real time 33
Internet of vehicles (IoV)
Supports autonomous driving and intelligent traffic management, providing safe transportation solutions for individuals with cognitive impairments and reducing accident risks. IoV-powered navigation assistance can help AD/ADRD patients maintain mobility while enhancing safety and independence. 34
Internet of drones (IoD)
Supports automated package delivery for medications, medical supplies, and assistive devices, ensuring timely access to essential healthcare resources, particularly for individuals in remote or mobility-restricted areas. Building surveillance and maintenance can also enhance patient security in smart city environments. 35
Industrial internet of things
Contributes to smart home automation and system maintenance, optimizing ambient-assisted living for AD/ADRD patients. Smart home technologies, including AI-powered voice assistants, fall detection sensors, and automated lighting/heating systems, can create a safe and adaptive living environment tailored to the needs of dementia patients. 36
Beyond these applications, the integration of IoT with AI, federated learning, edge-cloud computing, and blockchain are improving the security, efficiency, and scalability of IoT-based dementia care. AI-powered cognitive models, memory-aid devices, and assistive technologies improve daily living activities, promoting patient independence and safety. Additionally, telehealth platforms, video conferencing tools, and remote screening technologies enhance access to dementia care, particularly benefiting individuals with limited mobility or those in remote locations.
E-learning platforms and caregiver education
Digital education tools are vital in supporting caregivers of AD patients. Two studies37,38 reported that e-learning platforms, mobile learning applications, webinars, and MOOCs (Massive Open Online Courses) provide accessible training opportunities for adult learners. The blended learning approach which incorporates the on-site (face to face) learning and online component created a more balanced and effective learning experience. Likewise, VR-enhanced caregiver training, highlighted in studies, demonstrates the growing preference for metaverse-based education to overcome traditional barriers such as time constraints and limited accessibility.26,38 Innovative metaverse applications, such as dementia villages in virtual environments, simulate familiar settings to support reminiscence therapy and social engagement. Serious games and cognitive training programs also promote mental stimulation and improve cognitive functions among older adults demonstrating the metaverse's transformative potential in AD/ADRD care.
Applications of the metaverse to address AD/ADRD challenges
Addressing cognitive decline with VR and spatial navigation training
One of the most pressing challenges in AD/ADRD care is cognitive decline. Three identified studies examined the emerging metaverse technologies, particularly VR-based cognitive training programs, which demonstrated significant potential in slowing disease progression and enhancing cognitive engagement.25–27 These tools, especially when VR-based spatial navigation assessments are combined with AI-powered personalization, can significantly enhance the overall diagnostic experience. Not only do these assessments provide richer data for clinicians, but they also offer a more engaging experience for patients, potentially improving participation and compliance during the cognitive evaluation process. 39 Similarly, digital gaming technologies have been reported to promote mental stimulation and lifelong learning, counteracting cognitive deterioration. 40 As illustrated in recent studies, VR-based wayfinding games, such as Labyrinth VR, offer immersive experiences that challenge and strengthen the hippocampus, the brain region responsible for memory and spatial navigation. 41 Similar to how open-world video games encourage natural exploration and map learning, Labyrinth VR places participants in a virtual city, requiring them to complete real-world tasks like locating a grocery store or navigating to a friend's house. This type of cognitive training has been shown to improve spatial memory recall and enhance long-term memory retrieval in older adults. This training also encourages neuroplasticity, which may counteract age-related hippocampal shrinkage. Notably, older adults who engaged with Labyrinth VR demonstrated significant improvements in memory retrieval, with some participants achieving performance levels comparable to nondemented older patients, while complementing pharmaceutical treatments. 41
In addition to VR, the metaverse ecosystem supports various assistive technologies designed to enhance daily living and cognitive function.
Reducing social isolation
Social isolation is a significant concern in AD/ADRD care, as patients often experience reduced social interactions due to cognitive impairments. Digital health interventions such as VR-based social engagement platforms and ICT-enabled communication tools have been instrumental in fostering social connections.25,27 Studies exploring the use of assistive technology in dementia care reported that multiplayer VR platforms provide interactive virtual environments where patients can engage with caregivers, family members, and peers, reducing feelings of loneliness.28,42 Platforms like Rendever offer virtual trips and reminiscence therapy, allowing seniors to explore new places or revisit past events, potentially boosting their cognitive function and well-being. 43 As a leading VR solution designed for senior living communities and healthcare organizations, Rendever's immersive experiences foster group engagement and meaningful social connections. These VR applications create shared experiences, enhancing social interaction and emotional well-being among individuals with AD/ADRD. 43
Additionally, VR-based reminiscence therapy, where patients interact with familiar and emotionally significant virtual environments, has also been reported to improve emotional well-being and reduce feelings of disconnection. 38
Supporting caregivers
Caregivers play a crucial role in AD/ADRD management, and digital health solutions have been developed to ease their burden and enhance their caregiving skills. Two studies have reported VR-based caregiver training simulations provide immersive experiences that improve caregivers’ understanding of dementia and equip them with effective caregiving strategies.38,44 These training programs enable caregivers to practice responding to real-life scenarios in a controlled virtual environment, thereby increasing their competence and confidence. 38 Additionally, telehealth applications and remote monitoring tools allow caregivers to track patients’ conditions in real time, facilitating timely interventions and reducing stress.28,42,45 ICT-based on-the-job training (OJT) has also been identified as a crucial resource for equipping novice caregivers with the necessary knowledge and skills, improving their ability to provide high-quality care. 46
Advancements in AI-driven Large Language Models (LLMs) present new opportunities for digital caregiving strategies. By analyzing existing caregiving education materials and mobile application descriptions, LLMs can help align key caregiving tasks with digital tools across different stages of AD progression. 47 These tasks, ranging from behavior monitoring and daily assistance to direct supervision and ensuring a safe environment, can be supported by digital aids such as memory-enhancing apps, GPS tracking, and voice-controlled devices. Furthermore, digital health platforms offer educational resources tailored to caregivers’ needs, addressing time constraints and accessibility issues. Studies have shown a strong interest among caregivers in using metaverse-based educational tools, highlighting their potential in enhancing caregiver knowledge and preparedness while attending to ADRD patients.27,40 The availability of virtual communities and peer support networks further alleviates caregiver stress, providing them with emotional support and opportunities for shared learning.29,38
Barriers to adopting digital health and metaverse technologies in AD/ADRD care
Technological familiarity and complexity
Many individuals with dementia have limited or no prior exposure to digital technologies, including gaming platforms, VR, or even basic digital health tools.28,37,40 This unfamiliarity creates a learning curve that can deter them from engaging with these technologies. For some, the complexity of new digital tools further exacerbates their reluctance. Even caregivers, who may have the technical knowledge, can struggle to understand the best ways to support technology use with their loved ones, especially when the tools are not intuitive or when they are not tailored to the cognitive abilities of people with dementia.28,47
Cognitive and physical limitations
Individuals with AD/ADRD may experience cognitive decline and physical impairments, which make certain digital health tools or metaverse technologies difficult to engage with. For instance, several digital games or VR environments require cognitive flexibility, quick responses, a certain level of physical mobility, which may be challenging for people with dementia. 28 In particular, high-paced digital programs or those requiring complex interactions might alienate users who are dealing with physical limitations such as mobility issues or fine motor difficulties. 28
Caregiver concerns, preconceptions, stigma and misconceptions
Caregivers, often the gatekeepers to adopting digital technologies, may hold concerns about whether technologies are appropriate or beneficial for people with dementia. Many caregivers worry that the cognitive decline associated with dementia makes it impossible for patients to benefit from digital interventions. The stigma surrounding dementia often leads to the marginalization of dementia patients, fostering negative societal perceptions that they are incapable of engaging with new technologies.28,37,40,45 This stigma, both societal and within families, can undermine the self-worth of individuals with dementia and deter them from accessing supportive technologies. 48 Additionally, some caregivers fear the technologies may be too complex for individuals with dementia, thus discouraging their introduction. 48 These preconceptions can prevent the adoption of technologies that could significantly enhance care.
Time constraints for caregivers
In addition to concerns about the suitability of digital technologies, caregivers often face a lack of time to learn, implement, or manage new technological interventions. 38 Their busy caregiving responsibilities, often exacerbated by work commitments, make it difficult to participate in training or education programs about new digital health tools. This barrier could create reluctance to adopt technologies, even if they have the potential to improve care.
Accessibility and cost-related barriers
Cost-related barriers also limit the widespread implementation of VR and AR in AD/ADRD care. The high cost of these technologies may exclude some healthcare providers, particularly those with limited resources. Older adults, especially those from lower socioeconomic backgrounds, may not have access to the necessary devices or internet connectivity needed for digital health solutions. 37 Additionally, digital health technologies often require ongoing software updates and maintenance, which can be expensive and challenging to manage for both individuals and healthcare institutions. 37
Lack of tailored solutions
While digital health and metaverse technologies have great potential, many are not designed with the unique needs of individuals with dementia in mind. 29 Technologies that do not account for cognitive decline, physical limitations, and emotional needs may be ineffective or frustrating for users, further discouraging their adoption. Standardized technologies may fail to engage people with dementia in a meaningful way, particularly when those technologies are not adaptable to varying cognitive abilities.
Strategies and solutions to overcome barriers
Promoting awareness, education, and reducing stigma
A major barrier to the adoption of digital health technologies is the stigma surrounding dementia. Public education campaigns that challenge misconceptions about the abilities of individuals with dementia can foster acceptance and encourage engagement with these technologies.37,40 Similarly, targeted training programs for caregivers and healthcare providers can address preconceptions and equip them with the knowledge to support technology use effectively.28,38,48 By creating a more informed and supportive environment, individuals with dementia are more likely to feel empowered to explore digital solutions.
Creating supportive learning environments
Studies highlight the importance of structured and supportive environments which can enhance engagement with digital health technologies.28,37 Community-based programs, such as “Tech Clubs” or peer-assisted learning initiatives, provide personalized support and practice time, allowing users to build confidence and competence. 37 These structured sessions allow participants to engage with digital tools in a low-pressure setting, reducing the fear of failure and encouraging exploration, while also improving long-term adoption rates.
Personalized and tailored approaches
Adapting digital health and metaverse technologies to an individual's cognitive abilities, interests, and physical limitations is critical for successful integration. A personalized approach, where the technology is adjusted based on an individual's needs, can enhance their experience and reduce feelings of frustration.28,37 Innovations such as custom input devices (e.g., a wheelchair-adapted VR interface) have shown promise in making VR experiences more intuitive for elderly users. 26 Designing more familiar and simplified user interfaces, such as touch-based interactions or voice commands, can help improve adoption rates.28,37 This approach can significantly increase the likelihood that individuals will continue using the technology.
Fostering independence and lifelong learning
Encouraging lifelong learning and promoting the independence of individuals with dementia can also overcome many barriers. Studies suggest that when individuals are provided with the resources and encouragement to continue learning and using digital technologies, they can regain a sense of control over their care and improve their well-being. 28 The use of simple, intuitive digital tools that are easy to learn and gradually adapt to an individual's evolving needs could help foster a sense of autonomy and reduce dependency on caregivers.
Ensuring affordability, accessibility, and data security
Financial constraints remain a significant barrier to technology adoption. Developing cost-effective digital health and VR solutions, alongside funding support from governmental and non-governmental organizations, can improve accessibility across different socioeconomic groups.33,44 Additionally, concerns about privacy and data security in remote care settings must be addressed. Implementing robust data protection measures, such as encryption, secure authentication, and decentralized data-sharing mechanisms, can foster trust and encourage broader adoption of digital health technologies.
Discussion
Digital innovation and immersive solutions for AD/ADRD care
The reviewed studies highlight a growing interest in leveraging digital health and metaverse-enabling technologies (Figure 4) for AD/ADRD management, reflecting a trend toward immersive, intelligent, and connected care systems, incorporating tools such as VR, AR, digital twin technologies, AI, and IoT. VR and AR technologies were especially prominent, supporting cognitive assessment, training, and therapy. VR-based spatial navigation training, such as Labyrinth VR, demonstrated potential in strengthening hippocampal function, aiding memory recall, and improving neuroplasticity in older adults. 41 Similarly, another study found that VR-based physical and cognitive training improved global cognition, verbal memory, instrumental activities of daily living, and neural efficiency in older adults with mild cognitive impairment (MCI). 49 However, researchers should consider the challenges of using VR with older adults, such as potential sensory-motor incongruences, while recognizing its benefits for experimental control and ecological validity in spatial navigation research. 50 While some findings affirmed the feasibility of using immersive VR systems even outside clinical settings, others reported increased anxiety among some dementia patients, raising concerns about safety, emotional impact, and appropriate use cases. 25 Digital twin technologies further extend the capabilities of immersive care by integrating real-time data from wearables and sensors to simulate and monitor clinical environments. These systems can replicate hospital workflows, simulate emergency responses, and support diagnosis by providing a virtual mirror of patient conditions and care environments. The integration of sensor technologies, IoT, and AI in smart environments further enhances healthcare delivery through remote patient monitoring and real-time data sharing. 51

The metaverse enabling technologies.
Importantly, digital platforms are also transforming caregiver education and support. E-learning tools, virtual simulations, and VR-enhanced training programs empower caregivers with the skills to handle complex dementia scenarios, reducing stress and improving care quality. 52 Despite their promise, adoption is challenged by high infrastructure costs, fragmented data standards, and limitations in device usability. Moreso, technological unfamiliarity, cognitive and physical limitations, stigma, and financial constraints hamper widespread adoption. Many tools are not tailored to the specific needs of dementia patients, and caregivers often lack time or resources for training. To overcome these challenges, studies emphasize the need for awareness campaigns, supportive learning environments, personalized design, and investment in affordable, secure technology infrastructure.
Ensuring ethical integrity and safety in metaverse-enabled dementia care
The adoption of metaverse technologies for AD/ADRD care raises critical concerns around ethical conduct, data protection, psychological safety, and legal accountability. These concerns are particularly pressing given the cognitive vulnerabilities and consent-related limitations common among people living with dementia. A core ethical challenge lies in the collection and handling of sensitive data. Immersive VR/AR platforms often rely on biometric, behavioral, and physiological inputs collected through wearables and extended reality devices. Without adequate safeguards, this sensitive data is at risk of misuse, surveillance, or cyberattacks. To mitigate these threats, studies recommend implementing end-to-end encryption, granular access controls, and transparent data governance frameworks.18,53
Informed consent remains a complex issue in dementia care. Cognitive impairments may limit patients’ ability to comprehend or retain information necessary for meaningful consent. Simplified, tiered consent models, combined with caregiver involvement and real-time digital prompts, are critical for preserving autonomy while ensuring ethical compliance. 42 The risk of identity fraud and impersonation is amplified in metaverse spaces that support avatars and digital clones. Another emerging concern is the risk of identity fraud in virtual environments. Metaverse platforms that support avatars and digital clones could be exploited by malicious actors. As a result, robust identity verification mechanisms such as biometrics and voice recognition are needed. However, these tools must be designed to accommodate the physical and cognitive limitations commonly found in AD/ADRD populations.
The psychological effects of immersive interventions also demand careful evaluation. Reminiscence therapies and virtual dementia villages show potential to improve mood and memory. However, poorly designed or culturally insensitive environments may lead to disorientation, distress, or reinforcement of false memories. Therapeutic content must be validated, individualized, and context-appropriate to avoid unintended harm. 42
Legal uncertainties further confound the deployment of metaverse tools in healthcare. Issues such as intellectual property, malpractice liability, and jurisdictional authority introduce considerable uncertainty. 54 Without targeted regulatory frameworks, patients and providers face unclear rights and responsibilities in digital care environments. Additionally, open metaverse spaces are vulnerable to harassment, misinformation, and exploitation. Solutions such as content moderation, smart contracts, and decentralized autonomous organizations (DAOs) have been proposed to enforce ethical standards and enable community-driven oversight. 18
Blockchain technologies may offer a path forward by enabling secure, consent-driven, and interoperable data exchange
Security and social issues in metaverse-based dementia care
While the metaverse holds promise for enriching dementia care and offering new ways to connect and heal. its safe implementation depends on robust cybersecurity and ethical design. Table 5 outlines key metaverse security risks and corresponding mitigation strategies.
Key security risks of the metaverse and mitigations.

Authentication and access control risks
A fundamental challenge in is ensuring that only authorized individuals, such as patients, caregivers, and healthcare professionals, can access sensitive virtual environments and data. Traditional authentication mechanisms, such as passwords or personal identification number (PINs), are often inadequate in immersive, multi-device settings. Risks include avatar impersonation and unauthorized data access. Advanced identity verification methods such as decentralized identity systems and biometric authentication can enhance traceability and prevent impersonation.55,56
Smart contracts and blockchain risks
The metaverse often relies on blockchain technology and smart contracts to automate transactions and manage data sharing. While these technologies offer transparency and efficiency, they are not without significant risks. Smart contracts, which are self-executing pieces of code used to automate transactions and data sharing in the metaverse, are prone to several critical vulnerabilities such as reentrancy attacks or integer overflows. These flaws can be exploited by attackers to drain funds, manipulate outcomes, or compromise the integrity of sensitive health data. Blockchain platforms themselves are subject to scalability issues, particularly when handling the large volumes of real-time data generated in healthcare settings. There is also the reported risk of 51% attacks, where a group of malicious actors controls a majority of the network and can disrupt or reverse transactions.57,58 Additionally, integrating blockchain with traditional healthcare systems poses technical challenges and requires specialized expertise, which is often in short supply.
Virtual asset security
Virtual assets, such as non-fungible tokens, representing medical records or therapy tools, and cryptocurrencies used for transactions within the metaverse, are attractive targets for cybercriminals. If compromised, attackers can steal both digital assets and sensitive health information. Vulnerabilities in smart contracts governing asset management can also allow for unauthorized transfers or destruction of virtual property. 59
Social and psychological risks
Beyond technical threats, metaverse environments must safeguard against psychological harm and social exploitation. The immersive nature of the metaverse involves continuous data collection on users’ movements, speech, and behaviors. Additionally, avatars could be used to impersonate trusted individuals or manipulate vulnerable users, increasing the risk of social engineering attacks and psychological harm.55,56 This points out the need for ethical design and informed interaction protocols.
Study limitations and future directions
While digital health and metaverse technologies offer unprecedented opportunities to enhance AD/ADRD care, significant challenges remain in ensuring equitable access, effectiveness, acceptability, and real-world application of these technologies. First, most studies reviewed were conducted in high-resource settings with access to advanced healthcare infrastructure, limiting the generalizability of findings to diverse populations, including low- and middle-income countries. Socioeconomic disparities, digital literacy, and cultural differences in caregiving approaches may impact the adoption and effectiveness of these technologies. Future research should focus on cross-cultural validation and implementation strategies tailored to resource-limited settings to ensure equitable access to these innovations.
Second, VR and AR applications, while promising, have been associated with increased anxiety, fear, and disorientation in some AD/ADRD patients. Many digital tools are not designed with cognitive impairments in mind, making them difficult for patients to navigate. Future research should prioritize safety assessments and optimize sensory inputs to minimize negative effects. In addition, adaptive user interfaces, voice-activated controls, and AI-driven personalization could enhance usability for individuals with varying levels of cognitive decline. While scalable, easy-to-use training modules and AI-assisted guidance systems should be developed to support caregivers in integrating these tools into daily care routines.
Furthermore, a major challenge in evaluating digital health interventions for AD/ADRD is the lack of standardized outcome measures across studies. Many studies had small sample sizes (ranging between 24 and 319 participants),38,46 lacked control groups, or relied on observational data, making it difficult to establish causal relationships between digital interventions and cognitive improvement. Several studies rely on different cognitive scales, behavioral assessments, and digital biomarkers, making it challenging to compare results. The absence of universal criteria for measuring effectiveness leads to inconsistencies in findings and limits meta-analyses. Future research should focus on defining consistent clinical endpoints for digital interventions, such as changes in cognitive decline progression, quality of life, or caregiver burden. Also essential is developing harmonized protocols for assessing usability, accessibility, and long-term engagement with digital tools. 60
Conclusion
The adoption of digital health and metaverse technologies demonstrates a pivotal shift in the management of AD/ADRD. The reviewed studies suggest benefits for enhancing patient monitoring, caregiver support, patient safety and reducing care burdens. However, current evidence supporting their widespread use remains preliminary, as these technologies are still in the early stages of clinical validation. Significant gaps remain in understanding their long-term effectiveness, safety, cost-efficiency, and real-world applicability across diverse populations. Many digital interventions have yet to be tested through rigorous, large-scale studies using standardized outcome measures. Without this evidence base, routine integration into dementia care pathways should proceed with caution. Challenges related to accessibility, digital literacy, and stigma must be actively addressed. Nevertheless, the adaptability of these tools positions them as potentially valuable components of future patient-centered care models. To fully realize this potential, future research must prioritize inclusive, interdisciplinary approaches that address usability, accessibility, and ethical concerns. Digital health innovations should be co-designed by clinicians, technologists, researchers, and policymakers to ensure they are equitable, evidence-based, and responsive to the complex needs of aging populations, not only in dementia care, but also in managing other chronic conditions where remote engagement and caregiver support are increasingly essential.
Supplemental Material
sj-xlsx-1-dhj-10.1177_20552076251365002 - Supplemental material for Digital health and metaverse for Alzheimer's disease and related dementia: A scoping review
Supplemental material, sj-xlsx-1-dhj-10.1177_20552076251365002 for Digital health and metaverse for Alzheimer's disease and related dementia: A scoping review by Uchenna Esther Okpete and Haewon Byeon in DIGITAL HEALTH
Supplemental Material
sj-docx-2-dhj-10.1177_20552076251365002 - Supplemental material for Digital health and metaverse for Alzheimer's disease and related dementia: A scoping review
Supplemental material, sj-docx-2-dhj-10.1177_20552076251365002 for Digital health and metaverse for Alzheimer's disease and related dementia: A scoping review by Uchenna Esther Okpete and Haewon Byeon in DIGITAL HEALTH
Footnotes
Notations
Authors’ contributions
Uchenna Esther Okpete contributed to conceptualization, methodology, validation, writing‒original draft preparation, writing‒review and editing, and visualization. Haewon Byeon contributed to conceptualization, methodology, validation, formal analysis, writing‒review and editing, supervision, project administration, and funding acquisition.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (NRF-RS-2023-00237287).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability
The data presented in this study are provided at the request of the corresponding author.
Supplemental Material
Supplemental material for this article is available online.
