Abstract
Early detection, accurate diagnosis, and effective treatment of liver diseases are of paramount importance for improving patient survival rates. However, traditional methods are frequently influenced by subjective factors and technical limitations. With the rapid progress of artificial intelligence (AI) technology, its applications in the medical field, particularly in the prediction, diagnosis, and treatment of liver diseases, have drawn increasing attention. This article offers a comprehensive review of the current applications of AI in hepatology. It elaborates on how AI is utilized to predict the progression of liver diseases, diagnose various liver conditions, and assist in formulating personalized treatment plans. The article emphasizes key advancements, including the application of machine learning and deep learning algorithms. Simultaneously, it addresses the challenges and limitations within this domain. Moreover, the article pinpoints future research directions. It underscores the necessity for large-scale datasets, robust algorithms, and ethical considerations in clinical practice, which is crucial for facilitating the effective integration of AI technology and enhancing the diagnostic and therapeutic capabilities of liver diseases.
Introduction
Liver diseases are a major global health concern, accounting for ∼ 2 million deaths each year and contributing to 4% of all deaths (one out of every 25 deaths worldwide). 1 These diseases are characterized by their complexity and diversity, encompassing a wide range of conditions such as viral hepatitis, metabolic dysfunction-associated steatotic liver disease (MASLD), cirrhosis, and hepatocellular carcinoma (HCC). Epidemiological data reveals an upward trend in the incidence of cirrhosis and HCC, particularly in developing countries. This increase is exacerbated by factors including hepatitis virus infections, alcohol abuse, and MASLD.2,3 In 2019, cirrhosis resulted in 1.48 million deaths, representing an increase of 8.1% compared to 2017. 4 Moreover, with the changing lifestyle patterns, the incidence of liver diseases has also risen significantly among the younger populations, presenting an even greater challenge to public health. 5 Liver diseases not only cause physical suffering to patients but also impose a substantial economic burden on families and society. Consequently, early detection and effective intervention are of utmost importance in reducing the morbidity and mortality associated with liver diseases. However, due to the high heterogeneity of liver diseases and the complexity of their pathological processes, traditional diagnostic and therapeutic approaches have notable limitations in sensitivity and specificity.
Artificial intelligence (AI) refers to the technology that simulates human intelligence via computers, enabling machines to, reason, and self-correct. In recent years, the potential applications of AI in the medical field, especially in early disease diagnosis, personalized treatment, and patient management, have drawn extensive attention. AI can aid doctors in making more accurate diagnostic and treatment decisions by analyzing a vast amount of medical data. 6 With the rapid development of AI, its application in the prediction, diagnosis, and treatment of liver diseases has shown great promise. In the management of liver diseases, AI can be utilized in areas such as image recognition, data mining, and predictive modeling to enhance the accuracy and efficiency of diagnosis. 7 The application of AI in liver diseases is not only limited to improving diagnostic accuracy but also extends to predicting disease progression, evaluating patient prognosis, and formulating personalized treatment plans. 8
With the unceasing progress of technology, the role of AI in the management of liver disease will become even more crucial. It has the potential to revolutionize the way we diagnose and treat liver diseases. This article aims to explore the current status and future prospects of AI in the prediction, diagnosis, and treatment of liver diseases.
Early screening of liver diseases
Limitations of traditional screening approaches
Traditional screening methods for liver diseases mainly depend on imaging examinations (such as ultrasound, computed tomography [CT], and magnetic resonance imaging [MRI]) and the measurement of serum biomarkers (such as alpha-fetoprotein [AFP]). However, these methods have certain limitations. Firstly, the sensitivity and specificity of imaging examinations are limited, particularly in the detection of early-stage HCC and liver fibrosis. They often result in false-negative and false-positive results. 9 Secondly, serum biomarkers lack specificity. Many patients may not show notable biomarker alterations in the early stages. 10 Moreover, traditional screening methods typically demand substantial medical costs and resource investments, especially when multiple follow-ups and repeated tests are required, making it economically unfeasible. 11 Finally, as the etiology of liver diseases evolves (e.g. from viral hepatitis to metabolic liver diseases), traditional screening methods also encounter challenges in identifying high-risk populations. 12 Consequently, there is an urgent need for innovative screening methodologies to improve the effectiveness and accuracy of early detection.
Development and application of AI-assisted screening tools
With the progress of AI, AI-assisted screening tools have shown great potential in the early screening of liver diseases. These tools leverage machine learning and deep learning algorithms to extract features from a vast quantity of imaging data, thus enhancing the accuracy of liver disease detection. 13 For example, AI can analyze liver ultrasound images to automatically identify signs of liver tumors and fibrosis. This not only reduces the workload of doctors but also improves the efficiency and consistency of diagnosis. 14 Moreover, AI can integrate clinical data and biomarkers for risk assessment and personalized screening, aiding doctors in formulating more precise screening strategies. 15 Currently, multiple studies have indicated that AI-assisted tools outperform traditional methods in the early screening for liver diseases, especially when screening high-risk populations, which significantly boosts the early detection rates. 13
Case study: Application of AI in the early screening of HCC
In the practical applications of early screening of HCC, AI has showcased its unique advantages. For example, a study employed deep learning algorithms to analyze liver MRI images and successfully identified early-stage HCC patients with significantly higher accuracy compared to traditional imaging assessments. 14 Furthermore, AI has been applied in the development of liquid biopsy techniques. These techniques analyze circulating deoxyribonucleic acid and exosomes in the blood to identify HCC-related signatures for early detection. 11 These studies indicate that AI not only improves the efficiency of early HCC screening but also offers a more comprehensive patient risk assessment by integrating multiple data sources. In conclusion, the application of AI in early screening of HCC shows great potential, potentially improving patient prognosis and survival rates, especially in high-risk populations. 15
Application of AI in the risk stratification and prediction of liver diseases
Development and validation of risk assessment models
The application of AI in the risk assessment for liver diseases, especially in the development and validation of risk assessment models, has drawn growing attention. AI, especially machine learning, constructs efficient risk assessment models for liver diseases by comprehensively analyzing a wide range of clinical data, including age, gender, alcohol consumption habits, body mass index, and liver function indicators. These models can not only predict the risk of liver disease onset but also provide recommendations for early intervention in personalized health management. In recent years, researchers have leveraged AI, especially machine learning algorithms, to develop various risk assessment models for liver diseases, such as MASLD, liver fibrosis, and HCC.16–18 Typically based on large-scale clinical datasets, these models utilize patients’ clinical characteristics, imaging results, and laboratory test findings to forecast the occurrence and progression of diseases. For example, a study employed a multilayer perceptron model to successfully identify specific preoperative risk factors associated with HCC recurrence, providing a foundation for personalized interventions. 19 Moreover, another systematic review demonstrated that AI-assisted non-invasive techniques are comparable to human experts in the accuracy of detecting and staging liver fibrosis, highlighting the potential of AI in the risk stratification for liver diseases. 20 The validation of these models is usually carried out through cross-validation and independent validation sets to ensure their reliability and effectiveness in clinical applications. Through continuous optimization and validation, AI risk assessment models are anticipated to play a crucial role in future clinical practice.
Application of AI in the prediction of liver diseases
AI-driven prediction tools have demonstrated promising potential in clinical applications related to liver diseases. For example, automated diagnosis and staging systems for MASLD have been validated in multiple studies.21–23 Study has also indicated that these AI-based tools showcase excellent performance in accuracy, sensitivity, and specificity. 24 Moreover, in the research on MASLD, AI has been utilized to develop repeatable, quantitative, and automated methods to enhance the accuracy of patient stratification and uncover new biomarkers and therapeutic targets. 25 In the management of HCC, AI models can not only predict the recurrence risk but also assist doctors in formulating personalized follow-up and intervention strategies. This effectively reduces the recurrence probability for patients. 19 These clinical application cases illustrate that AI has significant clinical value in the risk stratification and management of liver diseases, enabling the formulation of more precise treatment plans for patients and improving their prognosis. With the continuous progress of technology, it is anticipated that more AI tools will be applied in the early detection and intervention of liver diseases in the future.
Application of AI in the diagnosis and treatment of liver diseases
Medical imaging analysis and interpretation
Medical imaging is one of the core approaches for diagnosing liver diseases. AI, especially convolutional neural networks (CNNs) in deep learning, has exhibited exceptional performance in imaging analysis.26–28 By training deep neural networks, AI can automatically extract features from ultrasound, CT, and MRI to detect and quantify liver lesions. Compared with traditional imaging diagnosis, AI not only has significant advantages in accuracy and efficiency but also reduces subjective variations arising from manual interpretation.
In recent years, AI has achieved progress in liver imaging, as presented in Table 1. The application of AI in liver imaging not only improves diagnostic accuracy but also alleviates the workload of doctors, demonstrating a promising clinical application prospect.
AI application in liver disease diagnosis.

AI: artificial intelligence; HCC: hepatocellular carcinoma; MASLD: metabolic dysfunction-associated steatotic liver disease; CNN: convolutional neural network.
Assistive diagnostic systems
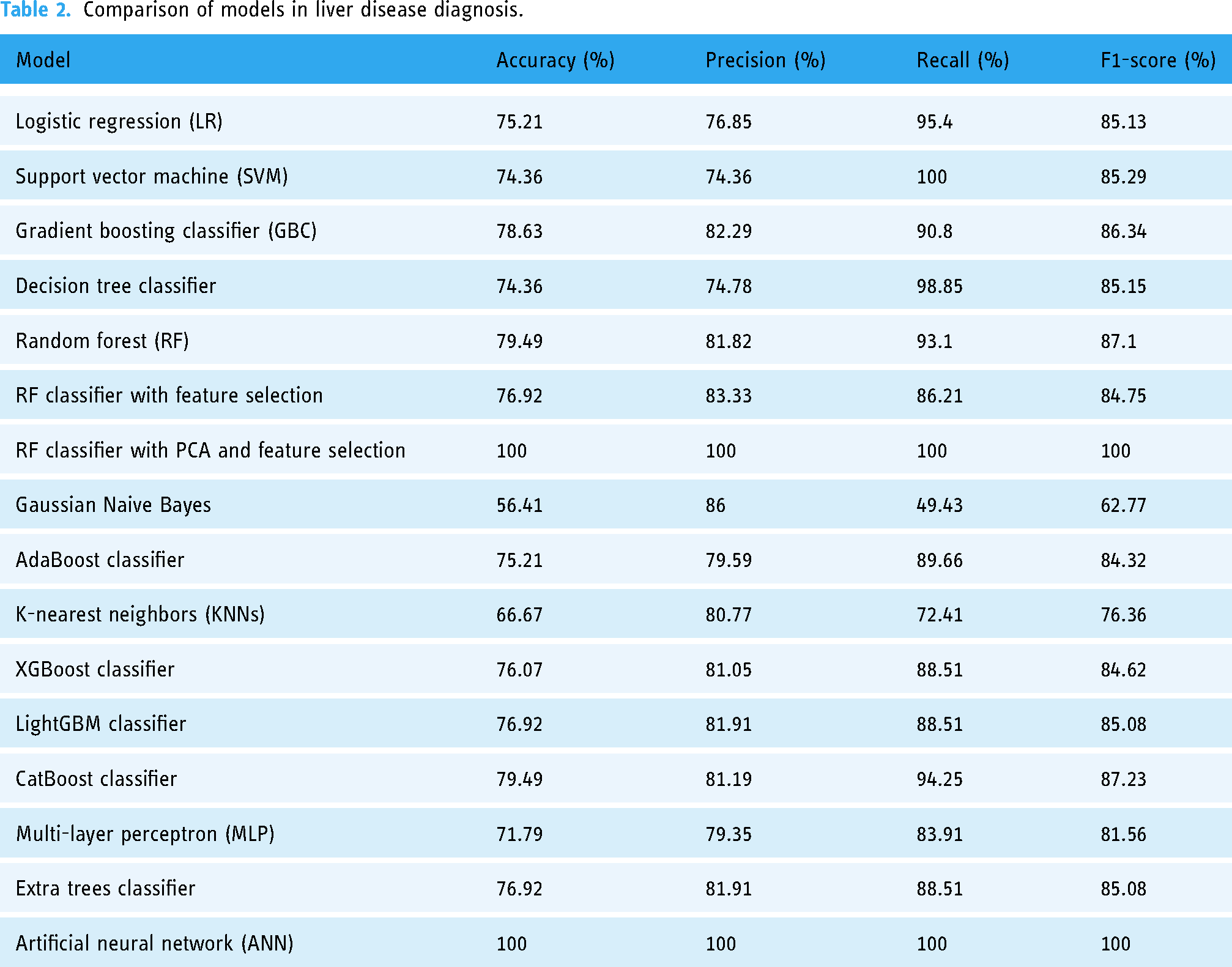
AI offers robust assistive diagnostic support to clinicians by comprehensively analyzing clinical data, medical images, and pathological slice information.39–41 AI systems based on natural language processing (NLP) technology are capable of extracting information related to liver diseases from electronic health records (EHRs) and generating diagnostic suggestions by integrating laboratory and imaging data. These assistive diagnostic systems possess notable advantages in improving diagnostic speed and accuracy, especially in the diagnosis of complex cases. Some researchers have compared multiple machine learning models to improve the early diagnosis capabilities for liver diseases, as shown in Table 2. 42 The assistance of AI can decrease the incidence of misdiagnosis and missed diagnosis.
Comparison of models in liver disease diagnosis.
Personalized treatment and treatment response prediction
Application of AI in personalized treatment planning
Precision medicine assumes a crucial role in the management of liver diseases, especially in the formulation of personalized treatment plans. The heterogeneity of liver diseases gives rise to substantial differences in the pathophysiological states of individual patients. Consequently, traditional one-size-fits-all treatment approaches frequently fail to meet the individual needs of patients. The application of AI has expanded from disease diagnosis to precision medicine. By integrating patients’ genomics, proteomics, and metabolomics data, AI can identify key biomarkers associated with liver disease progression, thus facilitating the development of personalized treatment plans for patients. 43 For example, MASLD, which is closely related to metabolic syndrome, exhibits notable disparities in pathological features and clinical manifestations among patients. Studies have shown that stratifying and classifying patients according to their specific pathophysiological characteristics can significantly improve treatment outcomes and patients’ quality of life. 44 Moreover, for autoimmune liver diseases (AILD), personalized treatment is of particular significance due to their complex etiology and pathological mechanisms. Through precision medicine approaches, patients can undergo genetic analysis and clinical manifestation assessment to formulate more suitable treatment plans, thereby improving therapeutic efficacy and minimizing side effects. 45 In the case of HCC, AI assists doctors in choosing the most appropriate targeted therapies or immunotherapy regimens by analyzing the molecular characteristics of the tumor.46,47 In conclusion, the formulation of personalized treatment plans not only enhances patient treatment outcomes but also reduces the waste of medical resources, enabling more efficient medical management.
Application of AI in drug response prediction
The application of AI in drug response prediction is developing rapidly, especially in personalized medicine. By analyzing patients’ genomic data, clinical histories, and biomarkers, AI can provide accurate predictions of drug responses. For example, a study has indicated that AI models can predict the response of specific drugs in cancer cells, thereby assisting doctors in selecting the most appropriate treatment plans. 43 By integrating multiple data sources, these models can identify key genes and molecular pathways that impact drug responses, thus enhancing the accuracy of predictions. Additionally, AI can analyze large-scale clinical trial data through machine learning algorithms to identify potential differences in patient responses to various drug treatments. 48 This approach not only improves the effectiveness of treatment but also minimizes unnecessary side effects, providing robust support for personalized medicine.
AI-assisted monitoring and evaluation of treatment effects
AI has shown great potential in monitoring and evaluating the treatment effects of liver diseases. By comprehensively analyzing patients’ biomarkers, imaging data, and clinical parameters, AI can monitor real-time changes in patients’ conditions and assess treatment efficacy. For example, AI can utilize image recognition technology to analyze liver images, assisting doctors in accurately determining the degree of liver fibrosis and fat deposition, which provides a basis for subsequent treatment decisions. 49 Additionally, AI can analyze large amounts of clinical data through machine learning algorithms to identify key factors that influence treatment efficacy, enabling personalized monitoring and evaluation of patients. 50 This AI-based monitoring method may not only improve the accuracy of assessments but also enable doctors to adjust treatment plans promptly to optimize treatment effects. With the continuous progress of technology, the application of AI in liver disease management is expected to hold even greater promise, potentially providing patients with more precise and efficient treatment options.
Application of AI in liver surgery
Surgical assistance and robotic surgery
In recent years, the application of AI in surgery has become increasingly widespread, especially in real-time image guidance. By analyzing real-time imaging data, AI can provide more precise anatomical structure recognition and surgical navigation. The integration of surgical robots and AI is revolutionizing the realm of surgical procedures. Modern surgical robots not only feature high-precision manipulation capabilities but also achieve intelligent analysis and feedback of the surgical process through AI. Research has indicated that AI-driven robotic systems can analyze imaging data in real-time during surgery, optimize instrument movement, and alleviate surgeon fatigue. 51 Moreover, these systems can automate certain surgical steps, such as suturing and tissue cutting, thereby improving the consistency and safety of surgical procedures. 52 When combined with robotic-assisted surgical systems (e.g. da Vinci surgical robot), AI further enhances the precision and safety of surgical procedures. Real-time image guidance and force feedback control provide surgeons with precise operational guidance, minimizing surgical trauma and expediting postoperative recovery. However, despite the significant potential shown by the application of AI in surgical robots, challenges such as high development costs and reliance on data quality still persist. 53 In the future, with continuous technological advancements and data accumulation, the application of AI in surgical robots is expected to become more extensive, further improving the efficiency and safety of surgical procedures.
Application of intraoperative decision support systems (DSSs)
Intraoperative DSSs are emerging as crucial elements in modern surgery. By integrating multiple data sources, these systems offer real-time decision-making support for surgeons. DSS leverage machine learning and data analysis techniques to process real-time information during surgery, including imaging data and patient physiological parameters, to aid surgeons in their decision-making processes. 54 For example, research has shown that by combining imaging data with other information during the operation, DSS can effectively forecast potential risks and provide corresponding countermeasures. 55 Although current research indicates promising prospects for the intraoperative application of DSS, several challenges remain to be addressed, including system reliability, accuracy, and adaptability in different surgical environments. 56 In the future, with the continuous development of technology, intraoperative DSS will provide more comprehensive and intelligent support for surgical procedures, thus enhancing surgical success rates and ensuring patient safety.
Application of AI in postoperative complication prediction
AI is playing an increasingly significant role in predicting postoperative complications. Leveraging machine learning and data analysis, AI can extract valuable information from vast amounts of clinical data. This enables doctors to more effectively identify and anticipate the risks of complications during the postoperative phase. For example, AI can analyze patients’ physiological data, including heart rate, blood pressure, and laboratory test results, to monitor their health status in real-time and promptly detect potential complication risks. 57 This predictive capability not only improves the accuracy of clinical decision-making but also facilitates personalized postoperative management.
Data analysis and patient follow-up management
Data analysis plays a pivotal role in the postoperative follow-up management of patients. By conducting a systematic analysis of postoperative data, medical teams are able to more accurately assess patients’ recovery progress and the risk of complications. The integration of mobile health (mHealth) technology enables patients to continue receiving monitoring and support even after discharge. A study concentrating on elderly patients has demonstrated that the use of mobile applications and activity trackers for postoperative remote monitoring is highly feasible, accompanied by good patient compliance and satisfaction rates. 58 Moreover, research indicates that data analysis can identify key factors that influence postoperative recovery, thus providing more precise follow-up strategies for clinical practice. 59 The combination of these technologies not only improves the efficiency of patient follow-up but also provides more decision-making support for healthcare professionals.
Application of machine learning in long-term prognosis assessment
The application of machine learning in long-term prognosis assessment is increasingly prevalent, especially in the management of complex diseases. By analyzing patients’ long-term data, machine learning models are capable of identifying significant factors that impact patients’ prognosis. For example, in a study regarding liver surgery, machine learning models were employed to predict postoperative complications and patient survival rates. The results showed a substantial correlation between specific clinical characteristics and adverse prognosis. 60 Additionally, machine learning has been applied to forecast the risk of postoperative cancer recurrence. By integrating multiple biomarkers and clinical data, the prediction accuracy of these models has been significantly improved. 61 This data-driven approach to prognosis assessment not only deepens the understanding of patients’ long-term outcomes but also serves as a foundation for the development of personalized treatment plans.
Integration of clinical CDSs
AI is playing an increasingly prominent role in CDSs. Many existing CDS tools are plagued by problems such as alert fatigue and lack of interoperability among systems, which restricts their effective utilization in clinical practice. 62 By analyzing vast amounts of medical data, AI can assist doctors in making more utilization diagnostic and treatment decisions. For example, AI aids clinicians through various methods, such as image diagnosis, pathological classification, and treatment option selection. This not only reduces medical errors but also enhances patient safety. 63 In the field of oncology, AI applications have achieved sophisticated human–machine interaction, providing data-driven insights in clinical decision making and optimizing the selection of treatment options. 63 Additionally, AI can analyze laboratory data using machine learning algorithms, thereby improving the efficiency of clinical laboratories and enhancing patient treatment outcomes. 64 With the continuous development of AI, its role in clinical decision-making will become even more crucial, enabling doctors to make more effective decisions in complex clinical scenarios.
Challenges and limitations of AI
AI holds immense potential for application in the medical field. However, its implementation encounters numerous challenges and limitations. These issues not only impact the popularity and effectiveness of AI but may also pose risks to patient safety and privacy. Therefore, a thorough analysis of these challenges and limitations is essential for promoting the healthy development of AI.
Data privacy and ethical issues
With the rapid development of AI in the healthcare field, data privacy, and ethical concerns have emerged as increasingly significant issues. Traditionally, the protection of patient data relies on legal frameworks. However, with the intrusion of commercial interests, especially when profit-oriented companies acquire medical data, patient privacy is confronted with new challenges. Research has indicated that such data sharing may result in the misuse of patient information, particularly with a significantly increased risk of commercial exploitation targeting vulnerable populations. 65 Moreover, the application of AI has prompted in-depth deliberations on data ethics, such as how to foster openness in scientific research and data sharing while safeguarding data privacy. 66 Therefore, establishing robust ethical norms and legal frameworks to ensure that data is not misused during sharing is a crucial issue that demands urgent attention. Researchers suggest enhancing patients’ trust in data sharing through transparency in data use and stringent requirements for patient-informed consent. 67 Meanwhile, as the use of synthetic data becomes increasingly common, ensuring the accuracy and reliability of these data, as well as reconciling the conflict between data sharing and privacy protection, presents new ethical challenges. 68 Therefore, while promoting the development of AI, it is essential to establish strict data protection regulations and ethical standards to guarantee that patients’ privacy is fully protected. 69
Limitations of AI in clinical applications
Despite the significant potential exhibited by AI in clinical applications, such as improving the accuracy of disease diagnosis and optimizing treatment plans, it still encounters various limitations in practical use. Firstly, the development and validation processes of AI systems frequently lack sufficient support from randomized controlled trials, which may affect their broad applicability in clinical settings. 70 The application of AI in the diagnosis of liver diseases hinges on the trust of patients. The absence of transparency and ethical supervision may lead patients to be skeptical of AI recommendations, thereby affecting their acceptance. 38 Secondly, the lack of transparency and interpretability of AI systems makes it challenging for doctors to comprehend the basis of AI-made decisions during use, which may undermine doctors’ trust and acceptance. 71 Additionally, the diversity and complexity of data pose challenges to the training and application of AI models, especially in dynamic environments such as emergency medicine. 72 Data bias issues can also result in suboptimal performance of AI in specific populations, thus affecting the fairness and effectiveness of treatment. 73 Therefore, future research should concentrate on improving the interpretability of AI systems, enhancing system interoperability, and addressing clinicians’ acceptance of these tools to provide more effective clinical decision support. Finally, a special concern is accountability. When AI products are actually implemented, they are typically developed and operated jointly by different organizations or departments. The entities responsible for data collection, model training, and deployment may vary. Once problems arise with AI-based decisions, the division of responsibilities often descends into complex disputes. This ambiguity in responsibilities also dampens enterprises’ motivation for building transparency. 74
Suggestions for improvement and future potential research directions
To address the ethical challenges, several measures should be adopted to fortify data privacy and enhance algorithmic transparency. First of all, federated learning should be implemented. This approach enables AI models to be trained on local servers without the need to transfer patient data, thus ensuring a higher level of privacy protection. 75 Furthermore, blockchain-based encryption techniques can effectively safeguard medical data from unauthorized access and enhance data security. 76 Moreover, promoting the transparency and explainability of AI is of utmost importance. Developers should integrate explainable AI (XAI) frameworks such as SHAP (Shapley additive explanations) and LIME (local interpretable model-agnostic explanations) to improve the model interpretability of models. Thus enable clinicians to comprehend the reasoning underlying AI-based decisions. 77 Additionally, regulatory authorities should establish regular auditing mechanisms for AI models to evaluate their fairness, accuracy, and potential biases, ensuring compliance with ethical standards.
To surmount the challenges encountered in clinical applications, a multidisciplinary approach, innovative data annotation methodologies, and the advancement of more rigorous AI techniques and models are imperative. Firstly, the regulation and governance of medical AI require the implementation of standardized and safe AI practices, along with the establishment of a transparent reporting system for the performance of AI systems. This policy can alleviate clinicians’ skepticism and boost their reliance on AI-assisted decision-making. Simultaneously, it ensures that clinicians do not relinquish control over patient care due to potentially incomprehensible AI outcomes. 74 Secondly, researchers propose enhancing the diversity and representativeness of data collection during the development of AI systems, conducting sufficient clinical trials, and establishing corresponding regulatory mechanisms to guarantee the safety and effectiveness of AI. 78 Meanwhile, educating and training healthcare workers to understand and effectively use AI tools is also a crucial aspect of future development. 78 Furthermore, given the increasing significance of big data and AI in healthcare and precision medicine, the enactment of robust data protection legislation is of paramount importance for safeguarding individual privacy. Countries around the world have promulgated laws to protect the privacy of their citizens. For example, the United States has introduced the Health Insurance Portability and Accountability Act (HIPAA), while Europe has implemented the General Data Protection Regulation (GDPR).79,80 Through these improvement measures, AI can be more seamlessly integrated into clinical practice, thereby enhancing the quality of patient care.
AI holds great promise in improving the outcomes of liver diseases. However, its clinical application remains limited. The demographic characteristics of the liver disease patient population are highly heterogeneous. If the training data fails to represent the broader population, the generalizability of the model in real-world settings will be substantially diminished. Consequently, when most current models are prospectively evaluated with real-world data, their performance is likely to deteriorate. 81 Therefore, there is a need for more large-scale, multicenter, prospective studies that employ standardized omics data acquisition techniques to ensure the continued development of AI methods in liver diseases and ultimately contribute to alleviating the global burden of liver diseases.
Future outlook: Collaborative models between AI and clinicians
Looking to the future, collaborative models between AI and clinicians are poised to become the mainstream in clinical decision support. By integrating AI's computational prowess with clinicians’ clinical experience, the two parties can establish a synergistic working relationship, thereby enhancing the quality and efficiency of decision-making. 82 This collaborative model not only enables doctors to make more accurate decisions in complex situations but also continuously optimizes the performance of AI models through real-time feedback and learning mechanisms. 82 For example, in the field of radiology, AI can assist radiologists in identifying lesions and providing decision support. Meanwhile, doctors can evaluate and adjust AI's recommendations, achieving a mutually beneficial outcome for both humans and machines. 83 Additionally, with the advancement of data sharing and standardization, future AI systems will be better equipped to integrate information from diverse sources, providing clinicians with more comprehensive decision support. In conclusion, the collaboration between AI and clinicians will bring both new opportunities and challenges to CDSS, driving continuous improvements in healthcare services.
Discussion
In recent years, the application of AI in liver disease prediction has attracted extensive attention. By analyzing big data, AI can effectively integrate various clinical information, thereby enhancing the early detection rate and the accuracy of risk stratification for liver diseases. Particularly in the diagnosis of complex liver diseases such as MASLD, cirrhosis, and liver cancer, AI showcases its unique advantages by providing clinicians with more accurate decision-making support. This not only contributes to improving patient prognosis but also optimizes the allocation of medical resources in resource-constrained environments, alleviating the burden on the healthcare system. Moreover, AI holds significant promise in disease monitoring and follow-up. Leveraging wearable devices and intelligent medical systems, AI can monitor patients’ physiological parameters in real-time, assisting doctors in intervening before the progression of the disease, thus facilitating comprehensive patient management. The AI-based full-lifecycle health management model is expected to further reduce the recurrence rate of liver diseases and improve patients’ quality of life. Looking ahead, the application of AI in liver disease management will become more personalized and precise. By integrating AI with other cutting-edge technologies such as gene editing, regenerative medicine, and immunotherapy, the management of liver diseases is on the verge of achieving a qualitative leap. For example, gene editing technology can repair gene mutations associated with liver diseases, while regenerative medicine holds the potential to repair damaged liver tissue through stem cell technology. When combined with AI's accurate predictions and optimized treatment plans, the integration of these frontier technologies will provide patients with a novel treatment experience, significantly improving treatment outcomes and prognosis.
However, despite the significant potential exhibited by AI in the prediction, diagnosis, and treatment of liver diseases, it encounters multiple challenges in practical applications. Firstly, the development of AI models necessitates a substantial amount of high-quality, accurately annotated data. In the medical domain, acquiring large-scale datasets is difficult due to issues related to data privacy protection and data standardization. Moreover, data heterogeneity and imbalance impede the performance of AI models, especially when dealing with populations from different races and regions, thereby affecting the models’ generalization capabilities. Securing sufficiently diverse and balanced datasets to ensure broad applicability across various groups is an urgent issue that demands attention. Secondly, the “black box” characteristic of AI models restricts their interpretability in clinical scenarios, which may undermine the trust of medical staff and patients in AI-assisted decision-making. Clinical decisions typically require interpretable and traceable evidence. However, the intricate algorithms and numerous parameters in AI models make their output results difficult to explain, thus hampering the extensive application of AI in clinical practice. To address this, future research should place greater emphasis on the development of explainable AI technologies, introducing transparent model structures to enable clinicians to comprehend and trace the decision-making process of AI, thereby enhancing trust and better integrating AI with traditional medical practices. Furthermore, the legal and ethical issues associated with AI in medical applications must be addressed promptly. For example, striking a balance between data privacy protection and information sharing, as well as determining the attribution of potential medical liability stemming from AI decisions, are crucial factors that impede the large-scale clinical application of AI technology. Therefore, establishing reasonable legal frameworks and ethical guidelines to regulate the application of AI in the medical field and safeguard patients’ rights and privacy is a direction that cannot be ignored in future development. To address these challenges, breakthroughs are required in data-sharing mechanisms and privacy protection. This involves promoting medical data standardization and cross-institutional collaboration to acquire more diverse data for model development and validation. Simultaneously, by introducing explainable AI, the transparency of models can be enhanced, making their decision-making processes more explicit and thus increasing the trust of medical staff in AI. Additionally, AI should be deeply integrated with doctors’ professional judgments to form a patient-centered full-lifecycle health management system, achieving comprehensive coverage from prevention, early screening, to precision treatment and long-term management.
Looking to the future, the development directions of AI in liver disease management mainly encompass multi-modal data fusion, the optimization of CDSS, and the development of real-time monitoring and early warning systems. These advancements will further boost the feasibility and effectiveness of AI in clinical applications. Simultaneously, with the continuous iteration and development of AI, its potential impact on personalized medicine, precision treatment, and full-course disease management will become increasingly prominent. Through rational policy guidance and multi-party cooperation, AI is expected to assume a more important role in the field of liver diseases, thereby driving the overall improvement of medical care.
In summary, the significance of AI in liver disease prediction cannot be underestimated. Its application prospects in risk stratification, as well as precision diagnosis and treatment, are extensive. However, to fully realize this potential, continuous efforts are required to drive the development of related technologies and surmount the current challenges. In this process, interdisciplinary collaboration will be crucial for the advancement of AI. Researchers, clinicians, and data scientists should collaborate closely to integrate their respective expertise, ultimately achieving a qualitative leap in liver disease management. Only through unceasing research and innovation can we ensure that the application of AI in this field brings tangible clinical benefits, thereby improving patients’ quality of life.
Conclusion
AI is driving innovations in liver disease management. Through its applications in disease prediction, diagnosis, and personalized treatment, it offers novel solutions for precision medicine. Despite the numerous challenges it faces, the application prospects of AI in the liver diseases domain remain extensive. By enhancing the interpretability of AI models, promoting greater data sharing and standardization, and establishing more stringent ethical and legal frameworks, AI is set to play an increasingly crucial role in the diagnosis and treatment of liver diseases. With the continuous refinement of AI algorithms, advancements in data acquisition and processing technologies, and in-depth interdisciplinary research, AI will assume a pivotal position in improving the efficiency of liver disease diagnosis and treatment and enhancing patient prognosis. The deep integration of AI and traditional medicine will trigger comprehensive innovations in the diagnosis and treatment of liver diseases. This will provide patients with more precise, efficient, and personalized medical services, thereby contributing to better health outcomes and an improved quality of life. Moreover, the integration of AI with other advanced medical technologies will further promote the comprehensive management of liver diseases, providing optimal health protection for patients throughout the entire process, from early prevention to long-term follow-up. In the future, with the profound integration of AI and medicine, we are on the verge of entering a new era of precision medicine, bringing better prognoses and higher quality of life to patients with liver diseases.
Highlights
Given that the rapid advancement of AI technology has significantly impacted the medical field, this article aims to systematically explore the current application status of AI in liver disease prediction, diagnosis, and treatment, analyze its actual effects in clinical practice, and look forward to future development directions. By summarizing current research findings, we hope to provide valuable references for clinicians and inspiration for future research.
Footnotes
Acknowledgements
Not applicable.
Contributorship
All authors contributed to set the concept and design of the research. BG led the writing of the manuscript and WDD participated in drafting the manuscript. All authors read the manuscript critically and participated in revising the manuscript.BG contributed to subsequent revisions. All authors approved the final manuscript to be published and agreed to be accountable for all aspects of the work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
