Abstract
Objective
Electronic patient-reported outcome (ePRO) systems hold promise for revolutionizing communication between cancer patients and healthcare providers across various care settings. This systematic review explores the multifaceted landscape of ePROs in cancer care, encompassing their advantages, disadvantages, potential risks, and opportunities for improvement.
Methods
In our systematic review, we conducted a rigorous search in Scopus, Web of Science, and PubMed, employing comprehensive medical subject heading terms for ePRO and cancer, with no date limitations up to 2024. Studies were critically appraised and thematically analyzed based on inclusion and exclusion criteria, including considerations of advantages, disadvantages, opportunities, and threats.
Findings
Analyzing 85 articles revealed 69 themes categorized into four key areas. Advantages (n = 14) were dominated by themes like “improved quality of life and care.” Disadvantages (n = 26) included “limited access and technical issues.” Security concerns and lack of technical skills were prominent threats (n = 10). Opportunities (n = 19) highlighted advancements in symptom management and potential solutions for technical challenges.
Conclusion
This review emphasizes the crucial role of continuous exploration, integration, and innovation in ePRO systems for optimizing patient outcomes in cancer care. Beyond traditional clinical settings, ePROs hold promise for applications in survivorship, palliative care, and remote monitoring. By addressing existing limitations and capitalizing on opportunities, ePROs can empower patients, enhance communication, and ultimately improve care delivery across the entire cancer care spectrum.
Keywords
Introduction
Cancer remains a formidable global health challenge, responsible for approximately 10 million deaths in 2020. 1 Beyond physical symptoms, cancer profoundly impacts patients’ psychological well-being and quality of life, necessitating effective reporting of the patient’s condition and the application of management strategies for treatment.2,3 Traditional paper-based reporting approaches encounter limitations in real-time data collection, integrity, and accessibility, prompting a transition to electronic reporting systems. The burden on cancer patients to report outcomes consistently and regularly through traditional methods is especially high, and failing to collect that data could hurt the completeness of studies essential for regulatory approval.4,5 While paper-based approaches can report complications and outcomes, they face numerous limitations such as physical space constraints, data loss, and limited access for care providers to vital data when and where needed due to the accumulation of vast amounts of nonreal-time data.6,7 Consequently, paper-based approaches to collecting patient-reported data may result in untimely, illegible, illogical, or incomplete data, ultimately impacting the quality of patient care and treatment adversely. To address these challenges, recent advancements in information technology have spurred the design and development of various electronic systems in this domain. Moving towards the electronicization of outcome reports will enhance warnings and reminders, improve data quality compared to paper-based methods, reduce data access time, and facilitate data comparison and clinical research.6,8
Electronic patient-reported outcome (ePRO) systems have great potential to solve various problems in cancer care. These systems can facilitate real-time data collection, improve the reporting of side effects and outcomes, enhance patient engagement, and provide timely alerts and personalized feedback to patients and healthcare providers.9–11 ePRO systems are advanced digital platforms designed to collect real-time data directly from patients regarding their health, symptoms, and quality of life. Utilizing various technologies such as websites, mobile applications, and portals, ePROs provide a dynamic and accessible means of tracking patient-reported information, contributing to more comprehensive and timely assessments in cancer care10,11 Furthermore, the remote monitoring capabilities of ePROs could prove beneficial in situations where frequent in-person visits are challenging or geographically restricted. 12 Moreover, ePRO systems present a promising avenue for enhancing cancer care through improved patient engagement, real-time symptom tracking, and personalized care. 13
Several studies have highlighted the potential benefits and challenges of ePRO systems in cancer care, including improved health-related quality of life14–16 enhanced patient engagement 17 and favorable cost-effectiveness. 18 Additionally, ePRO systems are effective in providing longitudinal monitoring of treatment and symptoms, facilitating better communication with specialists, 19 and they are providing a more comprehensive and meaningful clinical insight regarding screening, diagnosis, and response to treatment.14–16 These systems, characterized by user-friendly interfaces and personalized feedback mechanisms, contribute not only to efficient reporting but also to heightened patient satisfaction.20,21 However, challenges such as methodological limitations, feasibility concerns, and technical barriers need to be addressed for their widespread adoption.22–24
Highlighting the critical need for ePRO in cancer, previous studies have shown their efficacy in assessing symptom burdens and improving patient well-being. However, a comprehensive assessment of the advantages, disadvantages, and implementation strategies of ePRO systems in cancer care is lacking.25–27 While Merit et al. conducted a thorough review focusing on electronic patient-reported outcome measures (ePROM) benefits and disadvantages, 28 our study surpasses this scope by including all ePRO measurements and systems, as well as analyzing opportunities and threats. This systematic review aims to address this gap, providing valuable insights into the benefits and challenges of ePRO, guiding evidence-based oncology practices, and aiding stakeholders in effective integration. By systematically evaluating the role of ePRO systems in enhancing patient outcomes and cancer care quality, our study benefits healthcare providers, researchers, and policymakers, informing decision-making processes and ultimately improving patient care and engagement.
The research questions for our systematic review could be formulated as follows:
What are the advantages of integrating ePRO systems into cancer care? What are the disadvantages and potential threats associated with implementing ePRO systems in oncology practices? What opportunities do ePRO systems present for improving patient outcomes and enhancing the overall quality of cancer care? What are the potential threats and challenges that need to be addressed for the successful integration of ePRO systems in diverse oncological settings?
These research questions will help in systematically evaluating the advantages, disadvantages, opportunities, and threats of ePRO systems in cancer care, and in identifying the most effective approaches for their successful implementation and widespread adoption.
Methods
We conducted a systematic review of all academic articles pertaining to ePRO for diagnostic and treatment outcomes in cancer. The study unfolds within a digital landscape, utilizing a meticulously crafted data extraction form as the primary instrument for collecting valuable perspectives. Following full-text screening and quality appraisal, a total of 85 articles met the inclusion criteria. Subsequently, data extracted from these pertinent articles will undergo thorough narrative analysis and be presented in organized tables and diagrams. Our final report will adhere to the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA). 29 This study covers five main steps including search strategy, inclusion and exclusion criteria, study selection, quality appraisal, and data extraction and synthesis. 29
Search strategy
We searched for articles published in electronic databases without time limitation, using three databases: Scopus, Web of Science, and PubMed. The searches used the following keywords and medical subject heading (MeSH) terms in various combinations. We derived two broad themes that were then combined with the Boolean operator “AND.” The first theme in Mesh “electronic Patient Reported Outcomes” was created by the Boolean operator “OR” to combine text words (e.g., “electronic Patient-Self Reporting,” OR “electronic Patient Reported Measures”). The second theme “Cancer” was the broad aspect created for the search strategy. Additionally, a backward snowball search will be employed to ensure comprehensive coverage of relevant articles. In the next step, all studies were imported into EndNote software and accordingly, we could remove duplicates.
Inclusion and exclusion criteria:
The inclusion criteria for this study were papers published in English, related to electronic patient-reported outcomes and measures, and various research types like quantitative, qualitative, and mixed methods. The exclusion criteria were non-English language articles, inaccessible full-text articles, studies exclusively focused on technical infrastructure, and those emphasizing paper-based or manual patient-reported outcome (PRO) versions, books, protocols, standards, framework, and guidelines, conference proceedings, dissertations, conference abstracts, reviews, short reports, posters, newspapers, editorials, and commentary. Furthermore, unrelated subjects were excluded such as feasibility, paper vs. electronic, terminology criteria, clinical alerts, health equity, perspective, experiences, and perception, data and machine learning, models, associations, not related and not cancer, editorial, biology, telemedicine, ethical principles, wearables, gamification, system design, and technical innovations, oncology informatics, precision oncology, validity and reliability, and economic. Studies lacking indicators or outcomes for cancer, not using the system as the intervention tool, or with insufficient and vague information were also excluded.
Study selection
Two reviewers (Hosna Salmani and Somayeh Nasiri) independently checked the title and abstract of the papers, and in case of disagreement, a third person (Maryam Ahmadi) was used. The irrelevant studies were removed, and the reasons for inclusion and exclusion were identified. One reviewer (Hosna Salmani) conducted data extraction, and other reviewers (Maryam Ahmadi and Somayeh Nasiri) rechecked the accuracy of the results. The same researchers read and reviewed the entire text to make the final decision.
Quality assessment
The selected articles underwent a rigorous quality assessment using the Mixed Methods Appraisal Tool, comprising components for qualitative, quantitative (clinical trials), quantitative (nonclinical trials), descriptive, and mixed methods, incorporating 25 questions. Each affirmative response contributes to a 25% score. Articles surpassing the average in the number of positive responses or fully specified items are categorized as high quality. Those with positive responses ranging from 25% to 50% are classified as medium quality, while those falling below 25% are considered low quality.
Data extraction
An initial data extraction form was developed at this stage of the review, which included advantages, disadvantages, opportunities, and threats. One reviewer extracted the data, and data elements were organized into two sections: general items (author, year, country/state, objective, and participants) and specific items (advantages, disadvantages, threats & opportunities, and cancer type). The selected papers were summarized in the final step of our methodology, and important factors were identified. The statistical results of systematic reviews were described for outcomes reported in the studies (see Table A1).
Data synthesis
The data were analyzed descriptively due to the heterogeneity of the study characteristics in ePRO. Thematic analysis was conducted to combine similar findings, with the themes recorded and categorized into organizations and individuals. The themes were then grouped and further analyzed. To ensure the validity of the thematic extraction process, the papers were cross-checked and discussed by the two authors of this study. 30 In the final step of the methodology, the selected papers were summarized, and major factors were found. The frequencies and percentages were calculated for all the results with respect to each of the items, and the comprehensive results, including Table 1 and Table A1 and Figures 1–2, were presented. The study’s findings contribute to a better understanding of the advantages, disadvantages, threats, and opportunities of electronic reporting systems in cancer care, informing the development of evidence-based, patient-centric oncology practices.
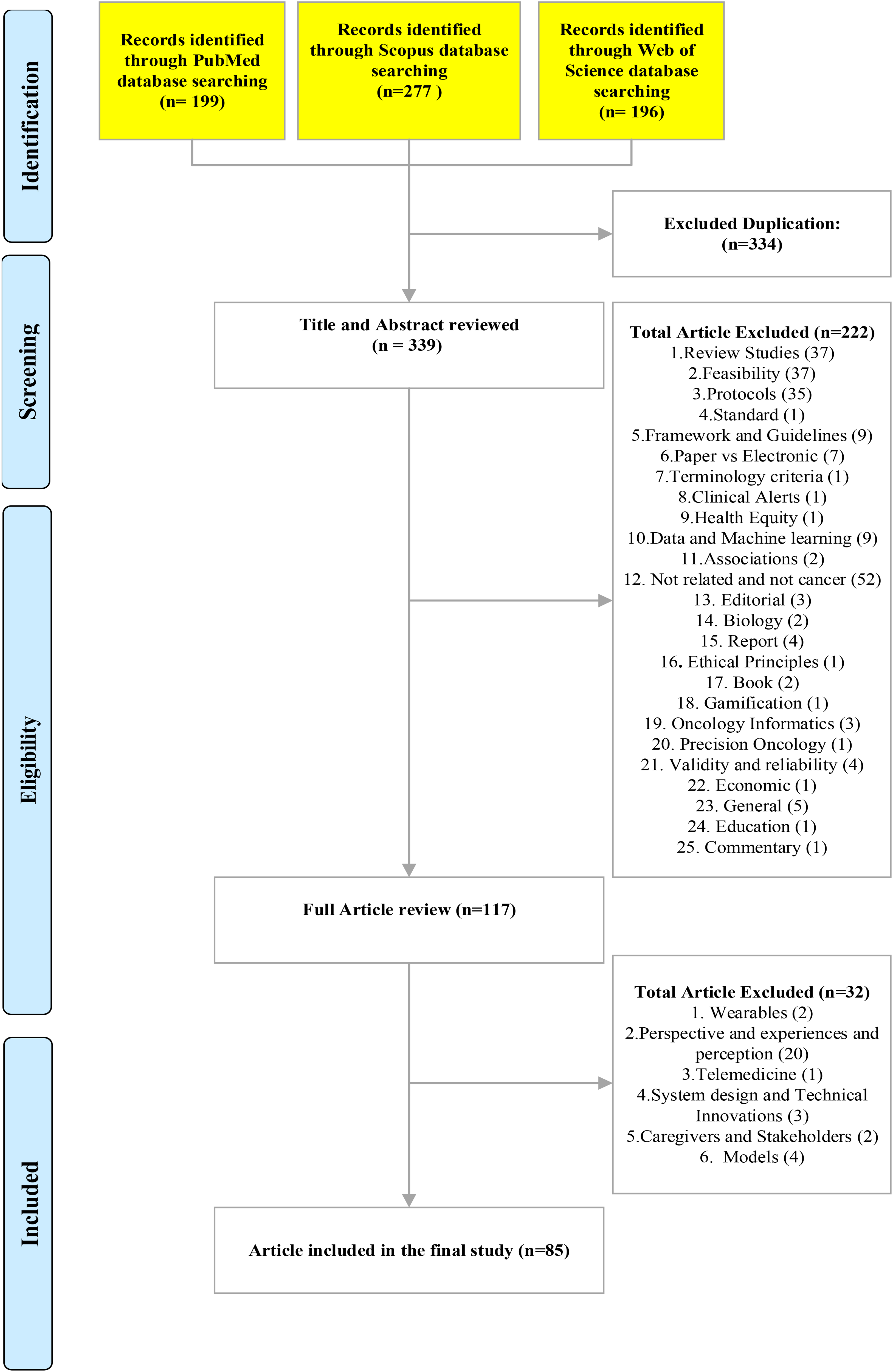
PRISMA diagram of our review process.
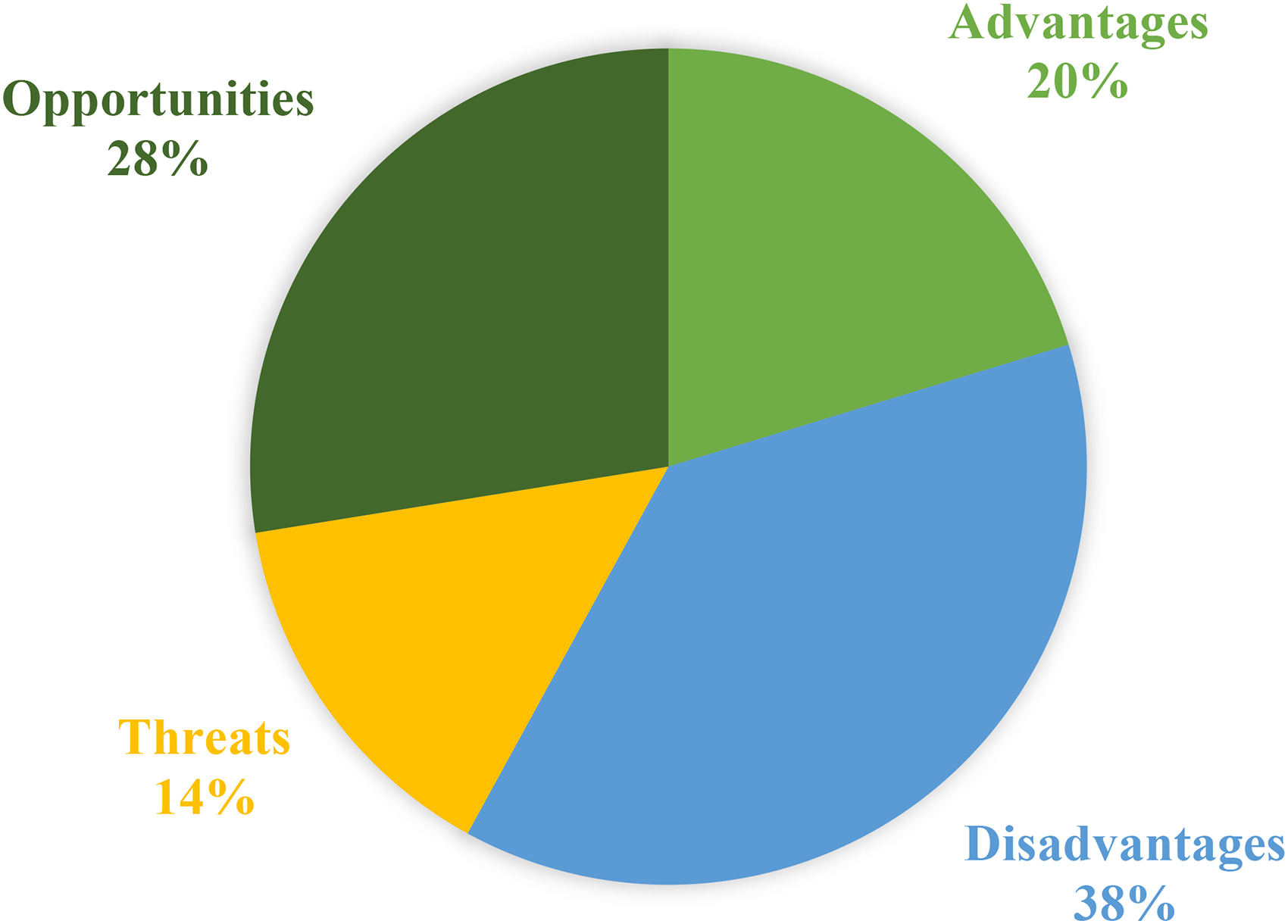
The frequency distribution of ePRO systems related to advantages, disadvantages, threats, and opportunities in selected studies.
The classification of advantages, disadvantages, threats, and opportunities in ePRO.
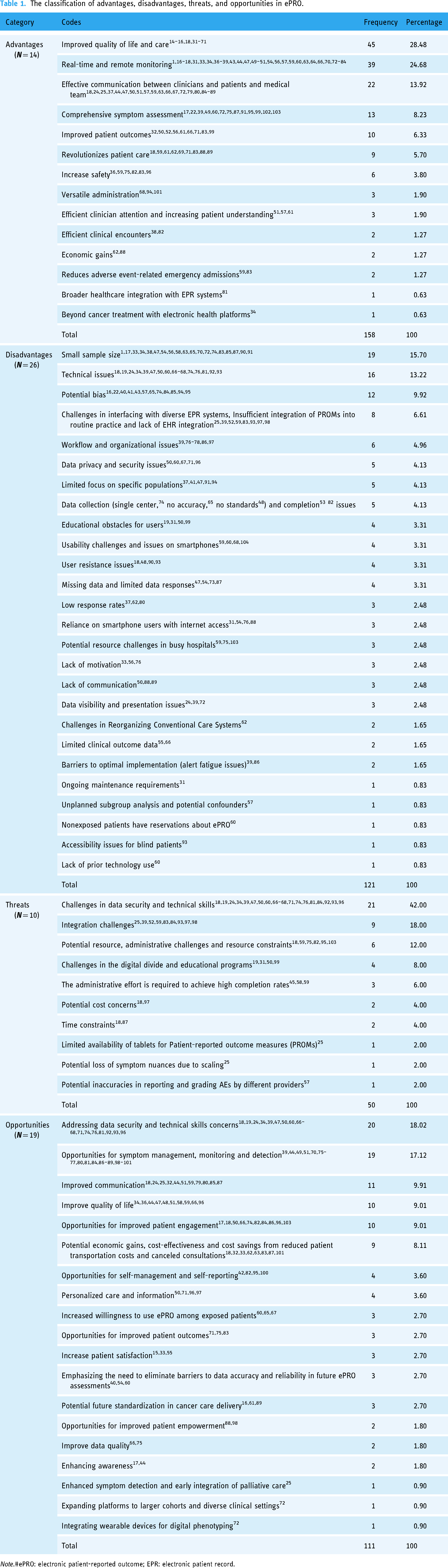
Note.#ePRO: electronic patient-reported outcome; EPR: electronic patient record.
Results
General findings
In our systematic review, we identified 672 papers, out of which 85 academic papers were included in our systematic review, providing a comprehensive exploration of electronic health platforms for cancer care. Figure 1 presents a PRISMA diagram illustrating our review process, showcasing the systematic selection and inclusion of relevant academic papers.
In the following sections, after summarizing all articles, we classified them based on their advantages, disadvantages, opportunities, and threats. The study revealed a comprehensive spectrum encompassing a total of 69 instances, including 14 advantages (20%), 26 disadvantages (38%), 10 threats (14%), and 19 opportunities (28%). The frequency distribution of ePRO systems, as illustrated in Figure 2, provides a comprehensive overview of the diverse aspects related to advantages, disadvantages, threats, and opportunities observed in the selected studies.
Main findings
Our systematic review of ePRO systems in cancer unveiled several significant findings. Table 1 displays the distribution of studies addressing the advantages, disadvantages, threats, and opportunities associated with ePRO in cancer. After identifying these factors within the ePRO system, we categorized and summarized common themes into distinct categories.
Advantages
According to Table 1, The advantages of ePRO were found to be diverse, with “Improved Quality of Life and Care” being the most prominent, cited in 45 studies (28.48%).14–16,18,31–71 This was followed by “Real-time and Remote Monitoring” with 39 references (24.68%), highlighting its significance in real-time health monitoring, which can significantly impact patient outcomes1,16–18,31,33,34,36–39,43,44,47,49–51,54,56,57,59,60,63,64,66,70,72–84 and “Effective Communication Between Clinicians and Patients” with 22 articles (13.92%), emphasizing the critical role of communication in improving collaboration and patient understanding.18,24,25,37,44,47,50,51,57,59,63,66,67,72,79,80,84–89 Conversely, the minimum count within the advantages is represented by “Broader Healthcare Integration with electronic patient record (EPR) systems” and “Beyond Cancer Treatment with Electronic Health Platforms,” each featuring only one study.34,81
Other advantages included “Comprehensive Symptom Assessment,” “Improved Patient Outcomes,” “Revolutionizes Patient Care,” “Increased Safety,” and “Versatile Administration,” among others. The advantages of ePROs were found to significantly impact patient outcomes, facilitate efficient clinical encounters, and increase safety, among other benefits.
Disadvantages
On the other hand, the review also identified several disadvantages associated with electronic Patient Reported Outcome Measures (ePROMs). The most prevalent disadvantage was “Small sample size,” cited in 19 studies (15.70%), reflecting a common challenge in research methodologies that may limit the generalizability of findings,1,17,33,34,38,47,54,56,58,63,65,70,72,74,83,85,87,90,91 followed by “Technical issues” with 16 references (13.22%), highlighting the challenges posed by technology in the implementation of electronic health platforms18,19,24,34,39,47,50,60,66–68,74,76,81,92,93 and “Potential bias” with 12 references (9.92%), emphasizing the need for researchers to address and mitigate bias in participant selection, data extraction and reporting.16,22,40,41,43,57,65,74,84,85,94,95 In contrast, the minimum counts are assigned to “Ongoing maintenance requirements,” “Unplanned subgroup analysis and potential confounders,” “Nonexposed patients have reservations about ePRO,” “Accessibility issues for blind patients,” and “Lack of prior technology use,” each with only one reference.31,57,60,93 Other disadvantages included challenges in interfacing with diverse EPR systems, workflow, and organizational issues, data privacy and security issues, limited focus on specific populations, and educational obstacles for users, among others. These disadvantages highlighted potential challenges in the implementation and utilization of ePROs in cancer research (see Table 1).
Threats
In terms of threats, the review identified “Challenges in data security and technical skills” as the most prevalent threat, cited in 21 studies, (42.00%) reflecting the growing concern around data security and the importance of technical expertise in managing electronic health platforms,18,19,24,34,39,47,50,60,66–68,71,74,76,81,84,92,93,96 followed by “Integration Challenges” with nine references (18.00%), indicating the complexities associated with seamlessly integrating these platforms into existing healthcare systems.25,39,52,59,83,84,93,97,98 and “Potential Resource, Administrative Challenges and Resource Constraints” with six references, (12.00%) indicating the complexities associated with seamlessly integrating these platforms into existing healthcare systems.25,39,52,59,83,93,97,98 The minimum counts within threats are assigned to “Limited availability of tablets for PROMs,” “Potential loss of symptom nuances due to scaling,” and “Potential inaccuracies in reporting and grading AEs by different providers,” each featuring only one reference.25,57 Other threats included challenges in the Digital Divide and Educational Programs, the administrative effort required to achieve high completion rates, potential cost concerns, and time constraints, among others. These threats indicated the potential barriers and challenges in the effective integration and utilization of ePROs in clinical practice. The data is shown in Table 1.
Opportunities
Finally, the review also highlighted various opportunities associated with ePROMs. The most prevalent opportunity was “Addressing data security and technical skills concerns,” cited in 20 studies (18.02%), indicating the recognition of these concerns as potential areas for improvement and advancement,18,19,24,34,39,47,50,60,66–68,71,74,76,81,92,93,96 followed by “Opportunities for symptom management, monitoring and detection” with 19 references (17.12%), emphasizing the potential for technological advancements to enhance symptom management and monitoring,39,44,49,51,70,75–77,80,81,84,86–89,98–101 and “Improved communication” with 11 references (9.91%), reflecting the recognition of enhanced communication as a valuable opportunity for better patient outcomes.18,24,25,32,44,51,59,79,80,85,87 The minimum counts within opportunities are attributed to “Enhanced symptom detection and early integration of palliative care,” “Expanding platforms to larger cohorts and diverse clinical settings,” and “Integrating wearable devices for digital phenotyping,” each with only one reference.25,72 Other opportunities included improving quality of life, improved patient engagement, potential economic gains, opportunities for self-management and self-reporting, personalized care and information, increased willingness to use ePRO among exposed patients, and opportunities for improved patient outcomes, among others. These opportunities emphasized the potential for ePROs to enhance patient care, improve communication, and provide valuable insights for clinical decision-making.
Discussion
Our systematic review examined the intricate landscape of ePRO systems in cancer care, exploring their Advantages, Disadvantages, Threats, and Opportunities. The variations in counts within each category shed light on the diverse focus areas within the literature, informing researchers and practitioners about the depth of exploration in each domain.
Advantages
According to our findings, we found several significant advantages of ePRO systems in cancer care: “Improved Quality of Life and Care,” “Real-time and Remote Monitoring,” and “Effective Communication Between Clinicians and Patients.” The most prominent advantage identified was the “Improved Quality of Life and Care”.14–16,18,31–71 This finding is consistent with the study by Gressel et al., which emphasized the prevalence of web-based ePRO systems for long-term monitoring and patient empowerment. 101 Similarly, Moradian et al.’s exploration of an eHealth tool for capturing and analyzing immune-related adverse events in cancer treatment 31 and Helissey et al.’s assessment of the effectiveness of electronic patient reporting outcomes in prostate cancer care further contributed to understanding the benefits of ePRO systems in cancer care. 34 These findings align with the broader literature, emphasizing the positive impact of ePRO systems on the quality of life and symptom management.
“Real-time and Remote Monitoring,” emerges as another salient advantage.1,16–18,31,33,34,36–39,43,44,47,49–51,54,56,57,59,60,63,64,66,70,72–83 emerged as a crucial aspect in our exploration of ePRO systems. This aligned with our overarching objective of examining the broader applications of ePRO systems. Moreover, the studies by Macanovic et al., 72 Holch et al., 73 Wickline et al., 37 and Tang et al. 37 provided valuable perspectives into the advantages of ePRO systems in cancer care. Macanovic et al. investigated the implementation of a remote patient monitoring system using an ePRO platform in a tertiary cancer center, highlighting the potential for improved symptom management and high compliance rates with weekly symptom assessments. 72 Holch et al. focused on the electronic patient self-Reporting of Adverse-events: Patient Information and aDvice (eRAPID) system, which aimed to improve the monitoring and management of symptoms in patients with prostate, lower gastrointestinal, and gynecological cancers. 73 Wickline et al. examined the usability and acceptability of the electronic self-assessment and care (eSAC) program in advanced ovarian cancer, emphasizing the importance of real-time feedback for symptom management and the potential for early integration of palliative care. 37 and Tang et al. implemented symptom management follow-up using an ePRO platform in outpatients with advanced cancer, demonstrating the feasibility of incorporating daily app-based ePRO surveillance for patients undergoing radiotherapy 75 which led to increased reporting of cancer-specific symptom burden and significantly improved several domains of patient satisfaction.
“Effective Communication Between Clinicians and Patients,” emerged as a critical advantage,18,24,25,37,44,47,50,51,57,59,63,66,67,72,79,80,85–89 enhancing collaboration and improving patient understanding. Additionally, the studies by Brant et al., 87 Zylla et al., 80 and Peltola et al. 47 contributed to our discussion on effective communication between clinicians and patients through ePRO systems. Brant et al.’s study on patient and provider use of electronic care plans generated from patient-reported outcomes demonstrated improved confidence when asking patients to complete assessments and describing the assessment tool, 87 Zylla et al.’s exploration of the collection of electronic patient-reported symptoms in patients with advanced cancer using Epic MyChart surveys highlighted the potential benefits of ePROs in improving patient-doctor interaction through feedback on reported symptoms. 80 Peltola et al.'s study on a novel digital patient-reported outcome platform (Noona) for clinical use in patients with cancer assessed suitability, demonstrating improved survival rates, enhanced quality of life, decreased anxiety levels, better physical health status, increased adherence to therapy, fewer visits to the emergency room, reduced hospital admissions, improved patient self-belief and confidence, and collaborative and personalized cancer care. 47 These studies showed the pivotal role of ePRO systems in improving patient outcomes, enhancing symptom management, and improving collaboration between clinicians and patients. The findings from these studies align with the broader literature, emphasizing the consistent and favorable outcomes associated with the incorporation of ePRO systems in cancer care.
The identification of limited references associated with “Broader Healthcare Integration with EPR Systems” and “Beyond Cancer Treatment with Electronic Health Platforms,” served as a critical signal prompting further exploration in the academic study.34,81 Each reference, confined to a single citation, directed scholarly attention toward specific areas that merited more comprehensive investigation.
This insight indicated the imperative to broaden the scope of ePRO systems, contributing substantively to the theoretical underpinnings within the domain of digital health platforms. This discernment was particularly evident in studies such as Richards et al.'s pilot investigation on real-time electronic symptom monitoring for postsurgery patients 81 and Helissey et al.'s study on the effectiveness of electronic patient reporting outcomes in prostate cancer care. 34 The singular reference in each study accentuated less-explored facets, thereby signaling the potential for future academic research to advance the integration of ePRO systems into broader healthcare contexts, transcending the confines of cancer treatment. It is suggested that more studies on the effect of ePRO systems on broader healthcare integration and beyond cancer treatment be conducted experimentally.
Disadvantages
The systematic review revealed several challenges associated with ePRO systems in cancer care, with “Small sample size,” “Technical issues,” and “Potential bias” being the most common drawbacks. “Small sample size” was the most frequently mentioned challenge.1,17,33,34,38,47,54,56,58,63,65,70,72,74,83,85,87,90,91 This finding aligned with broader challenges in research methodologies and emphasized the need for innovative approaches to surmount limitations and enhance generalizability. Doolin et al. implemented ePRO for patients with new oral chemotherapy prescriptions at both an academic site and a community site. The study's small sample size and the lack of random allocation in the comparison group limited the ability to control for confounding factors. 17 Howell et al. implemented personalized symptom management through a quality improvement collaborative that focused on the implementation of PROs in real-world oncology multisite practices. 91 These studies, each with its specific focus, contributed to the broader understanding of challenges and solutions associated with ePRO systems in cancer care and are consistent with our goal of study.
“Technical issues” were identified as a significant disadvantage in ePRO systems.18,19,24,34,39,47,50,60,66–68,74,76,81,92,93 This indicated the challenges posed by technology in the implementation of electronic health platforms. The findings resonated with the broader literature, emphasizing the need for robust technological solutions and supporting the overarching goal of identifying challenges in the implementation of ePRO systems to examine studies on technological enhancements for the advancement of digital health platforms. Similarly, Judge et al. identified the implementation issues and evaluated the efficacy of an electronic patient self-reporting pain device in community-based cancer clinics. They found the staff resistance to change and technical integration issues with electronic medical records. 93 combined with Dronkers et al.'s evaluated the implementation of an ePROs system, in the routine care of head and neck cancer patients. In their study a sustainable technical environment was essential and also organizational and workplace adjustments were needed. 18 These studies discussed the technical challenges and potential solutions in the implementation of ePRO systems within the context of cancer care.
“Potential bias” emerged as a notable disadvantage, highlighting the need for researchers to address and mitigate bias in participant selection.16,22,40,41,43,57,65,74,85,94,95 This indicated the critical need for researchers to address and mitigate participant selection bias, aligning with a broader emphasis on enhancing the reliability and validity of study findings. The findings contributed substantially to a comprehensive understanding of biases in ePRO studies, aligning with the overarching goal of thoroughly exploring drawbacks and providing insights for refining study designs. Girgis et al. evaluated the effectiveness of the PROMPT-Care web-based system in a diverse population of cancer patients by reducing emergency department presentations; In their study, the response rate was low, possibly contributing to recruitment bias. 95 and Patt et al. evaluated the impact of ePROs on adverse events and total cost of care among patients with metastatic cancer and they found the potential bias due to differences in intervention and control groups 16 each added unique perspectives, considering the potential biases and refinements in ePRO system studies in cancer care.
In contrast, several factors such as “Ongoing maintenance requirements,” “Unplanned subgroup analysis and potential confounders,” “Nonexposed patients have reservations about ePRO,” “Accessibility issues for blind patients,” and “Lack of prior technology use” were each mentioned only once, where challenges were identified but may necessitate further exploration.31,57,60,93 These findings indicated the importance of targeted research in these specific domains, aligning to identify less-explored areas within the study on novel challenges in the implementation of ePRO systems. The studies by Niska et al. 57 and Hartkopf et al., 60 each focusing on ePRO in head-and-neck cancer radiotherapy and adjuvant/metastatic breast cancer patients, contributed significant insights to the broader understanding of challenges associated with ePRO systems, emphasizing the need for continued exploration and focused research in the identified areas.
The analysis of these findings showed that a small sample size was consistently mentioned as a challenge across various studies. However, technical issues were also prevalent, indicating that robust technological solutions are needed to address these challenges. Additionally, potential selection bias was highlighted as an important consideration, emphasizing the need for researchers to address and mitigate participant selection bias. Further research is recommended to address these challenges, including innovative approaches to surmount limitations related to small sample sizes, robust technological solutions to address technical issues, and targeted research to explore less-explored areas within the literature.
Threats
Our study identified several significant threats in ePRO systems, with the most prevalent being challenges in “data security and technical skills” and “Integration.” Data security threats18,19,24,34,39,47,50,60,66–68,71,74,76,81,92,93,96 in ePRO systems include potential breaches, unauthorized access, and data loss. To address these threats, robust security measures such as encryption, access controls, and regular security audits are essential.60,66,67 On the other hand, technical skills and training are low, which poses a significant challenge. The lack of experts and technical training can hinder the effective implementation and management of ePRO systems.19,60 Perspectives from various studies collectively highlighted the understanding of these challenges and potential solutions in the realm of ePRO systems. Gabrielle et al. adopted a remote symptom monitoring intervention developed in research settings for implementation in real-world clinical settings at two cancer centers and they found challenges related to the technology platform and workflow were encountered during the Zhang et al. 39 , followed by patient-reported health status changes over time in Chinese advanced cancer patients and explore the risk factors affecting their health status. They found potential technical issues with the ePRO system, and data security concerns 74 and Nordhausen et al. evaluated the implementation of ePRO in inpatient radiation oncology. They found Technical and organizational issues, such as Wi-Fi problems and interruptions in assessment completion. Moreover, Staff turnover and time constraints were barriers to implementation. Also, Challenges in making the collected data actionable within the clinical workflow and motivating clinical staff to use the results. 76 These studies focusing on the adaptation of remote symptom monitoring, changes in patient-reported health status in advanced cancer patients, and the implementation of electronic assessment of patient-reported outcomes in inpatient radiation oncology, respectively, consider the understanding of challenges and solutions in the concept of ePRO systems in cancer.
One of the known threats in the review study was “system integrity.” Despite this, few studies have paid attention to this issue.25,39,52,59,83,93,97,98 System integrity is considered a threat because it refers to the trustworthiness and reliability of the system. For instance, if the system is compromised, it can lead to inaccurate data collection and reporting, which can significantly impact patient care and decision-making.52,98 The findings resonated with overarching complexities in health system integration, highlighting the need for strategic planning and collaboration to address these hurdles effectively. Our research significantly contributed to the broader literature on integration challenges, aligning with our primary goal of comprehending and addressing potential threats to the successful implementation of ePRO systems. Several studies on “system integrity” have addressed the challenges of the ePRO system. For example, Sandhu et al. found Limited adoption due to integration regarding the incorporation of ePROs into routine cancer care at an academic center 52 and Biran et al. evaluated the acceptability and appropriateness of an ePRO intervention for patients with relapsed and refractory multiple myeloma and explored the lack of data integration into clinic workflow, highlighting the challenges and opportunities in the real-world implementation of ePRO systems. 98
The examination of threats within ePRO systems revealed minimal counts associated with specific challenges: “Limited availability of tablets for PROMs,” “Potential loss of symptom nuances due to scaling,” and “Potential inaccuracies in reporting and grading Adverse Events by different providers,” each supported by only one reference25,57 These findings indicated identified challenges that necessitated further exploration for the development of targeted solutions. The research contributed to the identification of less-explored threats, aligning with the objective of pinpointing areas for subsequent research and improvement in the landscape of ePRO systems. Furthermore, Warnecke et al. compared the information provided by ePROMs and nurse-reported assessments to identify overlaps and differences in the assessment of current symptom burden among oncological inpatients. 25 and Niska et al. assessed changes in quality of life and adverse events during radiotherapy for head-and-neck cancer using electronic patient-reported quality-of-life data. They found Potential for inaccuracies in adverse event reporting and grading by different providers. 57 These findings identified challenges that necessitated further exploration for the development of targeted solutions. Furthermore, studies provided valuable real-world insights, providing practical perspectives on challenges and potential solutions within the ePRO landscape.
In summary, while data security and technical skills are the most prevalent threats in ePRO systems, it is crucial to address system integrity to ensure the trustworthiness of the data collected. Robust security measures and ongoing technical training are essential to mitigate these threats and ensure the effective implementation and management of ePRO systems.
Opportunities
Our study identified several significant opportunities in ePRO systems, with the most prevalent being opportunities in “Addressing data security and technical skills concerns,” “Opportunities for symptom management, monitoring, and detection” and “Improved communication.”
“Addressing data security and technical skills concerns” emerged as a prominent opportunity.18,19,24,34,39,47,50,60,66–68,71,74,76,81,92,93,96 This highlighted the recognition of these concerns as potential areas for improvement and advancement in the implementation of ePRO systems. The findings aligned with the broader literature, emphasizing the need to address data security concerns and enhance technical skills in the deployment of digital health platforms. Studies by Graf et al. analyzed the acceptance and evaluation of a tablet-based ePRO app for breast cancer patients and found the Potential for improving health care. 19 and Duregger et al. developed a concept and implemented a prototype for introducing ePRO into the existing neuroblastoma research network and the data quality, patient engagement, and remote monitoring were improved. 66 These studies provided practical insights into enhancing data security and technical skills within the ePRO landscape.
“Opportunities for symptom management, monitoring, and detection,”39,44,49,51,70,75–77,80,81,84,86–89,98–101 emphasizing the potential for technological advancements to enhance patient care. Our findings examined the realm of technological progress that holds the promise of significantly elevating standards in patient care. This exploration seamlessly aligned with our overarching objective of comprehensively understanding the diverse and impactful opportunities presented by ePRO systems. Notably, studies conducted by Lee et al. identified factors associated with the adoption and compliance of ePROM among cancer patients in a real-world setting and they found the opportunity to improve patient-doctor interaction through feedback on reported symptoms 99 and Daly et al. assessed the clinical value of daily ePROs for cancer patients undergoing antineoplastic treatment and they found the potential for improved virtual supportive care delivery and optimized remote symptom monitoring. 77 These studies provided significant perspectives that further enriched the ongoing academic study on strategically leveraging ePRO systems to enhance symptom management and, consequently, raise the overall quality of patient care in clinical settings.
“Improved communication,” underlining the recognition of enhanced communication as a valuable opportunity for improved patient outcomes.18,24,25,32,44,51,59,79,80,85,87 This consistency aligns with the emphasis on effective communication between clinicians and patients as a critical advantage. Our findings resonated with the broader literature, highlighting the significance of communication in cancer care. Studies by Mohseni et al. developed a smartphone-based app for electronic reporting of outcomes by patients with prostate cancer and they found improvements in Reporting complications and side effects, communication between patients and specialists 32 and Lapen et al. developed a remote system for toxicity assessment and management of acute breast radiation side effects using ePROs and they found enhancement in patient-clinician communication. 79 These studies contributed valuable insights, reinforcing the academic studies on leveraging ePRO systems for improved communication and, consequently, enhancing patient outcomes in the realm of cancer care.
In our exploration of ePRO systems, we discovered significant opportunities, with three areas displaying minimal counts yet harboring significant potential: “Enhanced symptom detection and early integration of palliative care,” “Expanding platforms to larger cohorts and diverse clinical settings,” and “Integrating wearable devices for digital phenotyping,” each substantiated by a single reference.25,72 These realms, though less explored, present untapped possibilities for further research and innovation, aiming to elevate cancer care. Our findings not only contribute to identifying overlooked opportunities but align seamlessly with our overarching goal of pinpointing areas for future investigation and advancement. Warnecke et al. found enhancement in symptom detection, improved communication, and early integration of palliative care 25 and Macanovic et al. found opportunities for expanding the platform to a larger cohort and other clinical settings and integration of wearable devices for digital phenotyping. 72 These studies provided valuable perspectives on optimizing cancer care through innovative approaches within ePRO systems.
In future research, it is suggested to integrate the ePRO system with the electronic health record to improve the quality and cost-effectiveness of cancer care. This integration can result in avoiding repeated activities, promoting care coordination, and improving communication between healthcare providers across care settings. A protocol for guidance and action should be developed to ensure the successful implementation of this integration. Additionally, future studies should examine the impact of ePRO intervention in conjunction with other technologies such as artificial intelligence and wearables. It is also recommended to include other types of papers such as opinion pieces, editorials, viewpoints, and publications in languages other than English to provide a more comprehensive overview of all studies and all cancers around the world. Finally, it is essential to evaluate the financial and clinical impact of ePRO systems frequently to ensure their effectiveness in delivering patient care and promoting information systems.
Implications
Our study had several strengths. Firstly, by providing a comprehensive overview of the advantages, disadvantages, threats, and opportunities associated with ePRO systems, our study serves as a springboard for future research endeavors. This groundwork facilitates targeted investigations to address knowledge gaps and refine implementation strategies to maximize the potential benefits for patients and healthcare providers.
Furthermore, recognizing the pivotal role of ePRO systems in healthcare organizations highlights the imperative for concerted efforts to seamlessly integrate these technologies into clinical practice. As facilitators of timely information access, care coordination, and communication among healthcare stakeholders, prioritizing the adoption and optimization of ePRO platforms can significantly enhance the delivery of cancer care.
Additionally, the emphasis on evaluating the impact of ePRO on quality and cost-effectiveness underscores the importance of evidence-based decision-making in healthcare. By assessing the efficacy of ePRO implementation in improving patient outcomes and optimizing resource utilization, healthcare organizations can make informed choices regarding technology adoption and investment, thereby enhancing overall healthcare value.
Moreover, the actionable guidance provided for managers and policymakers enables more effective planning and implementation of ePRO initiatives. Leveraging these insights to inform strategic decision-making processes facilitates streamlined implementation efforts, resource allocation, and the resolution of potential adoption barriers, accelerating the integration of ePRO systems into routine clinical practice.
Lastly, identifying opportunities for improvement in ePRO implementation emphasizes the need for ongoing innovation and collaboration. Focusing on enhancing symptom management, patient empowerment, and patient-doctor communication improves continuous improvement in ePRO platforms, ensuring they remain responsive to the evolving needs and preferences of cancer patients and healthcare providers.
Limitation
This review study had several limitations that provide valuable insights for future research. First, due to time constraints, we surveyed published papers on three main databases. Therefore, this study can be a landscape for prospective studies. Second, in this review, the impact of ePRO intervention was included, but documents related to other technologies such as artificial intelligence, and wearable technologies were not examined in this research. Third, we excluded other types of papers such as reports, brief reports, books, textbooks, thesis and dissertation, editorials, letters perspective articles, symposiums, posters, brief communications, and unpublished working papers. Fourth, the study did not include types of reviews such as systematic reviews and Fifth, we excluded publications in languages other than English. These limitations suggest the need for future studies to provide a more comprehensive and inclusive analysis of ePRO systems in cancer care.
Conclusions
In conclusion, our systematic review provided a comprehensive analysis of the advantages, disadvantages, opportunities, and threats of ePRO systems in cancer care. The study discovers the diverse focus areas within the literature, informing researchers and practitioners about the depth of exploration in each domain. The advantages of ePRO systems, such as improved quality of life and care, real-time monitoring, and effective communication, aligned with the broader landscape of studies emphasizing the positive impact of technology in cancer care. However, the disadvantages and threats indicated the challenges that need to be addressed for the successful implementation of ePRO systems, including small sample sizes, technical issues, data security concerns, and integration challenges. The opportunities highlighted areas for improvement and innovation in cancer care, such as addressing data security concerns and enhancing symptom management.
While our review offers valuable insights, it is not without limitations. The restriction to published papers on three main databases due to time constraints suggests the need for broader exploration in future studies. Additionally, our focus solely on ePRO interventions excludes consideration of other pertinent technologies like artificial intelligence and wearables, highlighting avenues for further investigation. Furthermore, the exclusion of certain types of papers and non-English publications may have limited the scope of our analysis, emphasizing the importance of inclusivity in future research efforts. Moving forward, we recommend integrating ePRO systems with electronic health records to optimize cancer care delivery, exploring combined interventions with emerging technologies, broadening the scope of literature review, and continuously evaluating the financial and clinical implications of ePRO systems. By addressing these recommendations, future research can enhance our understanding of ePRO systems’ role in cancer care and inform strategies for improving patient outcomes. Our study contributes to the dynamic landscape of cancer care and research, emphasizing the need for continued exploration and innovation in leveraging electronic health platforms for the benefit of cancer patients.
Footnotes
Acknowledgements
We thank Iran University of Medical Sciences for supporting this study.
Contributorship
HS, SN and MA served as a lead for conceptualization, methodology, and resources. HS served as a lead for formal analysis, data curation, writing–original draft preparation, and visualization. SN and MA served as a lead for writing–review and editing and supervision. MA served as a lead for project administration. All authors have read and agreed to the published version of the manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was obtained from the Research Ethics Committee of Iran University of Medical Sciences, Tehran, Iran (IR.IUMS.REC.1402.105).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Guarantor
Not Applicable.
Appendix
Summary characteristics of articles included.

| Number | cAuthor | Year | Country/state | Objective | Participants | Advantages | Disadvantages | Opportunities and threats | Cancer type |
|---|---|---|---|---|---|---|---|---|---|
| 1. | Natalie R Dickson, et al. 84 | 2024 | United States | To evaluate the utilization and clinical impact of an ePRO tool in patients with solid tumors undergoing IO therapy | 538 patients in the HC cohort, and 1014 patients in the ePRO cohort, with 319 ePRO users and 695 nonusers | DoT and OS, enhanced patient-provider communication, proactive symptom management, ease of use for patients | Challenges in differentiating the impact of the platform from other changes affecting outcomes, potential selection bias among ePRO users, reliance on self-reported data | O: Enhanced patient engagement, better symptom management, real-time monitoring of treatment efficacy T: Reliability of patient-reported data, technological challenges, system integration issues |
Solid tumors (NSCLC, melanoma, renal cell carcinoma, bladder cancer, head and neck cancer) |
| 2. | David Riedl, et al. 14 | 2023 | Austria | To investigate the ability of adult patients of different age ranges to complete routine ePRO assessments and to identify factors associated with completion and the need for assistance. | 5571 patients (mean age: 60.3 years, range 18–93 years) in Inpatient Rehabilitation setting | ePRO assessment feasible for older individuals, Touchscreen devices are potentially attractive, Quick completion time, Potential learning effect for faster completion | Decreased completion rate with age, Gender disparity in assistance requirement, Potential challenges in first-time portal access | -O: -Potential to refine portal access procedures, Gender-based assistance requirement considerations, and Learning aids for older patients -T: N/A |
Various cancer types (breast, hemoblastoses, prostate, uterine/ovarian, colon, head/neck, lung, stomach, rectum) |
| 3. | Tanja Sprave, et al. 15 | 2023 | Germany | -Investigate the feasibility of integrating ePROs in the treatment surveillance pathway for HNC patients during radiotherapy. -Assess the impact of app-based ePRO monitoring on global and disease-specific quality of life and patient satisfaction. |
100 enrolled, 93 evaluable | Demonstrated feasibility of incorporating daily app-based ePRO surveillance for patients with HNC undergoing radiotherapy. Increased reporting of HNC-specific symptom burden and significantly improved several domains of patient satisfaction. | Potential limitations due to limited cohort size, patients’ awareness of trial participation, and monitoring of department-owned devices. | -O: Further investigations are required for patient telemonitoring using patient-owned mobile devices and to assess the transferability of the findings outside the clinical trial context. Improved patient satisfaction, early detection of symptoms -T: Higher symptom burden reported, and potential sensitization effect. |
HNC (oropharynx, larynx, hypopharynx, nasopharynx, and parotid glands) |
| 4. | Debra A. Patt, et al. 16 | 2023 | United States | To evaluate the impact of ePROs on adverse events and total cost of care among patients with metastatic cancer enrolled in the Centers for Medicare and Medicaid Services OCM program | Initially, 1630 patients with cancer; 831 met the selection criteria, 458 matched patients were identified | Reduced adverse events, hospitalizations, emergency room visits deaths, and decreased total cost of care. |
Potential bias due to differences in intervention and control groups, limited sample size, influence of COVID-19 pandemic, limitations in addressing socioeconomic factors | -O: Enhancing value-based care, potential future standardization in cancer care delivery -T: N/A |
Metastatic Breast, Chronic leukemia, Lung, Lymphoma, Multiple myeloma, Prostate, and Small intestine/colorectal cancer |
| 5. | Andrew Harper, et al. 22 | 2023 | Canada | 1. Describe symptom severity among AYA with cancer at diagnosis and 1 year after diagnosis. 2. Identify demographic and clinical risk factors for higher symptom severity. 3. Evaluate symptom trajectories among AYA with cancer during the year following diagnosis. 4. Compare symptom severity and trajectories with older adult patients with cancer. |
937 adolescents and young adults; 473 at diagnosis, 322 at 1 year after diagnosis | - Comprehensive study covering various cancer types in AYA. - Identification of key risk factors for moderate to severe symptoms. - Comparison with older adult patients for unique insights. |
- Use of single-item indicators and dichotomizing symptom scores may introduce measurement error. - Potential volunteer bias as completion of the patient-reported outcomes questionnaire is not mandatory. | - O: Insights into the unique needs of the AYA population for targeted interventions. - T: Potential type I errors due to the assessment of multiple explanatory factors and symptoms |
Various cancer types, including Breast, Central nervous system, Endocrine, Gastrointestinal, Genitourinary, Gynecologic, Head and neck, Hematologic, Intrathoracic, Melanoma, Sarcoma, etc. |
| 6. | Eva Oldenburger, et al. 23 | 2023 |
Belgium | Explore the opinions of HCP active in radiation oncology in Belgium on using ePROMs for symptom follow-up after palliative radiotherapy. | 128 respondents, including radiation oncologists, nurses, radiation therapy technologists, clinical support managers, and quality managers. | - 84% considered ePROMs beneficial for patients’ health and symptom knowledge. - 75% willing to implement and use ePROMs. - Suggested a dedicated nurse navigator for ePROM promotion and follow-up. |
- 75% agreed that the implementation of ePROMs would result in additional workload - Concerns about the feasibility of ePROMs for palliative patients. |
-O: - Dedicated personnel for ePROM implementation and follow-up can increase success. - T: - The majority willing to review ePROMs before clinical consultation |
N/A |
| 7. | Williams LA, et al. 94 | 2023 | United States | To rapidly develop, launch through an electronic patient portal, and provide initial validation for a PRO measure of COVID-19 symptom burden in patients with cancer. | 600 participants diagnosed with both cancer and COVID-19 | Comprehensive assessment of symptom burden, rigorous development process, versatile administration | Low response rate, potential selection bias, limited focus on specific population | -O: Importance of longitudinal research -T: Consideration of COVID-19 variants, |
Various types of cancer in individuals also diagnosed with COVID-19 |
| 8. | Warnecke E, et al. 25 | 2023 | Germany | To compare the information provided by ePROMs and nurse-reported assessments in order to identify overlaps and differences in the assessment of current symptom burden among oncological inpatients. | 230 inpatients | Identification of underestimation of distress by nursing staff - Focus on psychological symptoms - Real-time feedback for symptom management - Potential for early integration of palliative care |
- Limited availability of tablets for PROMs - Potential loss of symptom nuances due to assessment scaling - Insufficient integration of PROMs into routine practice |
-O: Enhanced symptom detection, improved communication, early integration of palliative care - T: - Limited tablet availability, - Potential data loss due to assessment scaling |
Soft-tissue sarcoma, Lung, Uveal melanoma, Gastrointestinal, Hepatobiliary and pancreatic cancer |
| 9. | Moradian S, et al. 31 | 2023 | Canada | To develop an eHealth platform for cancer patients to manage symptoms and interact with healthcare professionals. | N/A | Improved survival rates, enhanced quality of life, decreased anxiety levels, better physical health status, increased adherence to therapy, fewer visits to the emergency room, reduced hospital admissions, improved patient self-belief and confidence, and collaborative and personalized cancer care. | Limited to smartphone users with internet access, ongoing maintenance is required for timely notifications, usability testing needed, and educational obstacles for some users. | N/A | Various types of cancer in individuals |
| 10. | Mohseni M, et al. 32 | 2023 | Iran | Develop a smartphone-based app for electronic reporting of outcomes by patients with prostate cancer | Specialists (n = 15), Patients (n = 21) | The system can potentially lead to improvements in patient outcomes, reduce costs, and improve patient access to healthcare services. Further research on cost-effectiveness and data integration is recommended. | Limited number of participants, reliance on patient’s self-reporting, | -O: -Reporting complications and side effects, communication between patients and specialists -quality of life assessment questionnaire - cost-effectiveness and data usefulness need further research - T: N/A |
Prostate cancer |
| 11. | McMullan C, et al. 24 | 2023 | United Kingdom | To assess the usability of the ChemoPRO® app among people with lived experience of cancer. | 10 participants with lived experience of cancer. | Participants found the app acceptable, easy to use, and useful for recording symptoms and communicating with clinicians. | Some technical issues such as missing information and unclear pop-up messages. -Participants suggested simplifying certain features and improving data presentation |
- O: -improving patient-clinician communication through the app. -Future testing should include clinical settings and diverse populations. T: N/A |
Leukemia, breast, multiple, myeloma, stomach, bowel, rectal, sarcoma |
| 12. | Bojan Macanovic et al. 72 | 2023 | Ireland | To investigate the feasibility of implementing a remote patient monitoring system using an ePROs platform in a tertiary cancer center in the Republic of Ireland. | 13 patients and 5 staff | - High compliance rate with weekly symptom assessments. - Positive patient and clinician satisfaction. - Potential for improved symptom management. |
- Small sample size. - Limited to oral chemotherapy patients. - Gender imbalance among participants. |
O: Opportunities for expanding the platform to a larger cohort and other clinical settings. - Integration of wearable devices for digital phenotyping. T: N/A |
Breast Melanoma Colorectal Lung |
| 13. | Patricia Holch, et al. 73 | 2023 | United Kingdom | Establish feasibility and acceptability of the eRAPID system | 167 (73.2% consented and randomized) | Integration into hospital EPR systems, codesign with patients and clinicians | Baseline score imbalances, missing data in gynaecological patients, and lower online adherence at 12 and 24 weeks. | Improve the monitoring and management of symptoms | Prostate, lower gastrointestinal, and gynaecological cancers |
| 14. | Silvia Hofer et al. 33 | 2023 | Switzerland | To assess the impact of treatment on HRQoL and patient-reported outcomes in palliative STS treatment. | The study was terminated early due to the COVID-19 pandemic, and only 11 patients were randomized and 10 evaluated. | - ePRO allowed real-time monitoring of symptoms and interactions. - High patient adherence rate for ePRO questionnaires. - Early detection of deterioration. - Assessment of treatment satisfaction and expectations. |
- The study had to be terminated early due to low enrollment during the COVID-19 pandemic. - Small number of participants. - Limited generalizability due to the small sample size. |
O: Regulatory recognition of PRO data and potential cost savings. T: The need for data security and limited patient motivation for prolonged ePRO assessments. |
STS |
| 15. | Helissey. et al. 34 | 2023 | Helsinki
and France |
Effectiveness of electronic patient reporting outcomes, by a digital telemonitoring platform, for prostate cancer care: the Protecty study | 61 patients | Feasibility of remote monitoring for prostate cancer patients, high compliance (72% during the first month), potential correlation between treatment tolerance (health status) and survival. | Limited generalizability, small sample size, relatively short follow-up period (8 months), single-center study. | -O: monitoring of compliance and adverse events in real-time, improving the quality of patient care. -T: Technical or connectivity issues experienced by patients, patient adherence to telemonitoring platforms, and interpretation of data in clinical practice. |
Prostate cancer |
| 16. | Franziska Geese, et al. 35 | 2023 | Switzerland |
Explore the potential of ePROMs in clinical practice for assessing the quality of life, functionality, needs, fear of progression, distress, and care quality in sarcoma centers | 55 patients from three sarcoma centers | ePROMs provide relevant patient information, evaluate care quality, reflect APNs service impact | Lengthy questionnaires, potential user dropout due to extensive items | -O: N/A -T: Barriers in recruiting for rare diseases, differences in sarcoma center structures impacting patient experiences |
Sarcoma |
| 17. | Andrew Gvozdanovic, et al. 92 | 2022 |
United Kingdom | To assess the feasibility of Vinehealth integration into brain tumor care | Six patients were initially recruited, and four engaged with the Vinehealth application throughout the study period. | Collection of real-world data, positive participant feedback, and subjective improvement in care reported by all participants using Vinehealth. | Technical issues impacting completion rates of specific assessments | -O: -Potential adverse events in mHealth technology, the need for larger, more comprehensive studies to evaluate the tool’s impact, and the challenge of usability, especially for older adults. -T: N/A |
Brain tumors include glioblastoma, metastasis from triple-negative breast carcinoma, and haemangioblastoma. |
| 18. | Yening Zhang et al.l 74 | 2022 | China | To track patient-reported health status changes over time in Chinese advanced cancer patients and explore the risk factors affecting their health status. | 103 patients completed a baseline survey (T = 0) and two follow-up surveys (T1 = 14 days, T2 = 28 days). | Effective for recording health status, capturing changes over time, and identifying risk factors for deteriorating health status. - Longitudinal study design provides insights into health status changes over time. - Use of validated measurements (EQ-5D-5L, MDASI-C, HADS). - Electronic data collection through the ePRO system. - Inclusion of demographic and medical data for comprehensive analysis. |
Small sample size, single-center study, no comparison group. - Limited sample size (103 patients). - Data collected only from a single cancer hospital. - Potential recall bias in self-reporting. The study does not investigate the effectiveness of interventions. |
-O: Efficient data collection, real-time monitoring, and improved patient engagement, Improving health status monitoring and supportive care. -T: Potential technical issues with the ePRO system, and data security concerns. |
Advanced stages of cancers, including Stage III without curative treatment chance and Stage IV) Lung, gastric, oesophageal, liver, colorectal, and breast cancer |
| 19. | Liyan Zhang, et al. 36 | 2022 | China | To compare the efficiency between ePRO and traditional follow-up models in cancer immunotherapy. | 278 patients (141 in the intervention group, 137 in the control group) | - Reduced incidence of serious irAEs - Fewer emergency department visits - Lower rate of treatment discontinuation - Higher quality of life - Less time needed for follow-up |
N/A | -O: -Improving patient safety and quality of life by detecting and responding to irAEs more efficiently. -Reducing the burden on healthcare providers and improving work efficiency. -T: Issues related to technology access and patient compliance. |
Gastric, Esophageal, Lung, Pancreatic, Colorectal, Breast, Brain, Liver, Kidney, and others |
| 20. | Wickline, et al. 37 | 2022 | United States | Usability and acceptability of the eSAC program in advanced ovarian cancer | Total sample (N = 134); device interview sample (n = 18); usability interview sample (n = 19) in ambulatory setting: | - eSAC was found to be acceptable and useful for patients and clinicians. - Improved patient-clinician communication. - Enhanced symptom management and quality of life. - The flagging system for palliative care referrals was successful. - Increased palliative care referrals and communication between providers and patients. - Facilitated discussions on sensitive topics like sexual function. - Provided a way to see subjective symptoms objectively. - Patients enjoyed participating in research and found a sense of purpose. |
- Findings may not generalize to diverse populations or cancer types. - AES is not offered to participants completing fewer than three reports. - Reports occasionally seemed outdated by the time of clinical review. - Low response rates for clinician surveys and focus groups. |
-O: Compatibility with devices, technological support, and patient comfort with technology were associated with patient acceptance. - Opportunities for broader implementation of PROs in ovarian cancer care and research. -T: N/A |
Advanced ovarian cancer |
| 21. | Tolstrup,et al. 38 | 2022 | Denmark | -To examine the impact of using ePRO with triggered alerts as an add-on to standard care on the HRQoL of melanoma patients receiving checkpoint inhibitors. -To investigate the association between irAEs severity and HRQoL. |
Patients (N = 138) | Patients in the intervention group had a significantly better HRQoL compared to the control group at 48 weeks. Patients felt more involved in their treatment and care, and alerts were seen as reassuring. | The study had a relatively small sample size. Some nonrespondents at week 48 could have completed questionnaires but chose not to. The threshold for triggers may have been too low. | -O: The increased focus on irAEs may have a long-lasting effect on HRQoL. There’s potential for more proactive interventions and routine physician monitoring of patient reporting. -T: N/A |
Melanoma |
| 22. | Tang et al. 75 | 2022 | China | To describe the implementation process and evaluation of an ePRO platform for symptom management in cancer patients, share experiences, and assess feasibility, safety, and efficacy. | A total of 161 patients with advanced cancer were enrolled in the study, although completion rates varied across the seven follow-up assessments. | - The ePRO platform demonstrated high completion rates and low drop-off rates during follow-up assessments. - Real-time alerts were sent to both patients and doctors, enhancing patient security. - The system featured a user-friendly interface, automatic reminder notifications, and standardized data collection and management, contributing to data quality. - The system facilitated symptom management and provided convenience for patients outside the hospital setting. |
N/A | -O: -The potential for improving symptom management in outpatient cancer care, which could lead to better patient outcomes and resource utilization T: N/A |
Patients with advanced cancer, including lung, liver, gastric, oesophagal, colorectal, and breast cancer. |
| 23. | Gabrielle B. Rocque, et al. 39 | 2022 | United States | To adopt a remote symptom monitoring intervention developed in research settings for implementation in real-world clinical settings at two cancer centers. | Phase I: 23 patients; Phase II: 35 patients (myeloma and acute leukemia) | - Improved symptom control, quality of life, length of time on treatment, hospitalization rates, and overall survival. - Well-received by nurses and oncologists (healthcare professionals found the intervention valuable for patient care and documentation) |
- Technical and workflow barriers: Challenges related to the technology platform and workflow were encountered during the implementation. - Alert fatigue: Nurses expressed concerns about the volume of alerts generated and the need for appropriate responses. - Data visibility issues: Physicians requested improved visibility of data and integration with the EHR. - Variability in patient education: There were inconsistencies in educating patients about the program, leading to differences in the enrollment process. |
–O: Cancer: Identifying patients who would benefit most from remote symptom monitoring, especially those with advanced-stage cancer, posed challenges. T: -Difficulty discerning advanced-stage vs. early-stage - Potential underutilization of the Intervention Despite its benefits, the intervention was underutilized outside of controlled research trials, indicating a need for broader implementation. |
Lymphoma, breast, gastrointestinal, genitourinary, myeloma, acute leukemia |
| 24. | David Riedl et al. 40 | 2022 | Austria | To assess the impact of multidisciplinary inpatient rehabilitation on the HRQoL and physical fitness of pediatric cancer survivors. | 236 pediatric cancer survivors aged 5–21 years and 478 parents (as proxy respondents). | - Statistically significant improvements were observed in most HRQOL scales postrehabilitation. - Enhanced physical activity and functional status postrehabilitation. |
- The lower agreement between children’s and parents’ HRQOL ratings before rehabilitation, suggests potential biases in proxy reporting. - Proxy overestimation of patients’ symptom scores and underestimate functioning |
-O: -The use of performance scores improved the alignment between children’s and parents’ ratings. -T: -Future studies should explore this approach for more accurate assessments. |
leukemias, lymphomas, CNS tumors brain, bone, soft tissue, blood and immune system and others. |
| 25. | Nordhausen, et al. 76 | 2022 | Germany | To evaluate the implementation of e-PRO in inpatient radiation oncology | The study involved a total of 568 patients. | - Most patients were willing to complete e-PRO assessments. - e-PRO assessment identified more symptoms compared to clinical records. - Patients completing e-PRO assessments were more likely to receive supportive measures. |
- Some patients faced barriers like health-related issues (e.g., high symptom burden, mild cognitive impairment) or lack of motivation. - Technical and organizational issues were barriers, such as Wi-Fi problems and interruptions in assessment completion. - Staff turnover and time constraints were barriers to implementation. |
-O: Potential benefits in symptom management and improving cancer care. -T: Challenges in making the collected data actionable within the clinical workflow and motivating clinical staff to use the results. |
Patients with various cancer |
| 26. | Mangyeong Lee et al. 99 | 2022 | Korea | To identify factors associated with the adoption and compliance of ePROM among cancer patients in a real-world setting | 580 cancer patients | Efficient symptom capturing, potential for improving patient outcomes and reducing unexpected clinical visits | Relatively low compliance rate, potential fatigue from extensive questionnaire, need for better education and support for user engagement | -O: -Improving patient-doctor interaction through feedback on reported symptoms -T: Challenges in user engagement, |
Various cancers (e.g., breast, lung, gastric, colorectal, lymphoma, head and neck, others) |
| 27. | Fay J. Hlubocky, PhD, MA, et al. 41 | 2022 | United States | To examine the prevalence of psychosocial factors affecting quality of life in ovarian cancer survivors using an ePRO platform | 174 out of 300 ovarian cancer survivors | Feasible for identifying unique psychosocial factors affecting HRQoL in ovarian cancer survivors, can be done remotely, potentially valuable for interventions. | Selection bias due to online participation, limited psychosocial staff support for distress referrals, one-time assessment, and potential underrepresentation of certain populations. |
-O: -To address unmet psychosocial needs of ovarian cancer survivors, -potential for future interventions, T: -Threat of selection bias and limited generalizability. |
Ovarian cancer |
| 28. | Joachim Graf, et al. 19 | 2022 | Germany | To analyze the acceptance and evaluation of a tablet-based ePRO app for breast cancer patients and examine its suitability, effort, and difficulty in the context of HRQoL and sociodemographic factors. | 106 women with adjuvant or advanced breast cancer at 2 major university hospitals in Germany. | - Patients regarded the ePRO assessment as more suitable, less stressful, and less difficult than ePRO. - Majority of patients stated that ePRO assessment improves health care in hospitals. |
N/A | -O: Potential for improving health care. -T: Patients with lower education and technical skills may face barriers to using ePRO apps; more studies are needed to address these needs. |
Breast Cancer |
| 29. | Afaf Girgis, et al. 102 | 2022 | Australia | To evaluate the processes and success of implementing the PRM system in the routine care of patients diagnosed with lung cancer. | 48 patients diagnosed with lung cancer completed 90 assessments during the 5-month implementation period. | - Every assessment identified patient concerns. - PRMs patients had significantly fewer visits to the cancer assessment unit for problematic symptoms. - Staff reported improved confidence when asking patients to complete assessments and describing the assessment tool. |
N/A | N/A | Lung cancer |
| 30. | Bobby Daly, et al. 77 | 2022 | United States | Assess the clinical value of daily ePROs for cancer patients undergoing antineoplastic treatment | 217 patients (median age 66, 103 women, and 114 men) | - Provides real-time symptom monitoring - Can detect severe symptoms without prior signs - Allows for continuous symptom management |
- May require changes in clinical staff workflow - Limited to a single-site cancer center - Subjective alert threshold levels |
- O: - Potential for improved virtual supportive care delivery - Optimize remote symptom monitoring T: - Risk of inadequate engagement due to competing demands |
Breast, head and neck, gastrointestinal, genitourinary, gynecology, lymphoma, melanoma, thoracic, and soft cancers |
| 31. | James Convill, et al. 42 | 2022 | United Kingdom | - Investigate the level of agreement between clinician-reported and self-reported patient smoking status during the first visit to a cancer center. - Examine the self-reported frequency of smoking cessation after the diagnosis of lung cancer. |
195 patients were included in the primary analysis. | - Most cases showed concordance between clinician- and self-reported smoking status. - Supports the use of ePROMs as a helpful tool to assess smoking status and identify patients for smoking cessation referral. |
- Some patients demonstrated discordance between clinician- and self-reported smoking status. - Reasons for discordance were not explored. - Limited consultation time may affect reporting. - Limited data on exact numbers for some criteria. |
-O: -Improving ePROM wording to increase self-referrals. -T: -Discordance between clinician and self-reporting highlights the need for additional support and follow-up for smoking cessation. |
Lung cancer |
| 32. | S. Boeke, et al. 43 | 2022 | Germany | To assess patient acceptance of PA monitoring in an outpatient setting during radiotherapy and to correlate changes in PA with toxicity and changes in QoL. | 23 patients |
High patient acceptance of activity trackers, availability of step-count data on 92% of treatment days, correlation between changes in PA and patient-reported side effects and QoL | Small number of participants, potential selection bias, limitations in step count measurements as a surrogate for aerobic exercise |
-O: - Remote monitoring of patients’ physical activity for early intervention. -T: Small sample size and potential biases. |
Breast Head and Neck, Lung Anal, Esophageal, and Pancreatic cancer |
| 33. | Adeola Bamgboje- Ayodele, et al. 103 | 2022 | Australia | To detail the development and implementation of ICPs forePROs in lung cancer patients in oncology settings | 96 staff members participated in engagement activities across three hospitals. | - Alignment with existing workflows - Utilizing available staff - Minimizing staff and patient burden - Maximizing patient engagement |
- Limitations in multilanguage PRM system, impacting patient reach -Unfamiliarity of care coordinators with new visualization of reports |
-O: -Strong stakeholder engagement and resource availability -T: -Patient population limitations due to language barriers |
Lung Cancer |
| 34. | Laura Takala, et al. 44 | 2020 | Finland | Assess the usefulness of ePROs during adjuvant RT in patients with early breast cancer. | 253 patients with breast cancer receiving RT | High response rates (82.6%), improved patient-clinician communication, enhanced symptom monitoring, and increased patient satisfaction. | Some symptoms are not discussed during appointments. For example, psychological symptoms (e.g., anxiety, fatigue) often under-recorded in EPR | -O: -Improved symptom detection, enhanced patient awareness, positive impact on patient-clinician communication, and potential positive effect on patients’ quality of life. -T: N/A |
Breast cancer |
| 35. | Olga Strachna, et al. 78 | 2021 | United States | To develop an ePROs program for head and neck cancer patients and evaluate its feasibility and impact. | 4154 patients | - Integration of ePROs into clinical care is feasible - Provides valuable data for assessing outcomes and counselling patients - Captures subsite/treatment modality HRQoL effects |
- Survey fatigue for patients - Limited clinician adoption (12%) - Barriers to EMR integration |
-O: - Potential improvements in content, workflow, data visualization, and health informatics - Data can be used for assessing outcomes and counselling patients -T: N/A |
Head and neck cancer |
| 36. | Dag Rune Stormoen et al. 85 | 2021 | Denmark | To describe PROs from patients with mCRPC receiving oncological treatment and compare them with adverse events from registration studies |
54 patients with mCRPC receiving medical oncological treatment | - PROs provide information about adverse effects and symptom burden during treatment. - Helps in understanding symptoms not previously reported. - Supports shared decision-making between clinicians and patients. - Provides real-world evidence complementing clinical studies. |
- Small sample size. - The study does not include a control group. - Potential bias due to multiple reports from the same patient. - Limited generalizability due to the study’s focus on mCRPC patients in Denmark. |
-O: PROs can improve communication and decision-making in cancer treatment. Real-world evidence can complement clinical studies. -T: -Potential bias due to small sample size and multiple reports from the same patients. Limited generalizability. |
mCRPC |
| 37. | Cathrine Lundgaard Riis, et al. 45 | 2021 | Denmark | To examine the impact on service use, workflow, and workload after introducing ePRO-based individual follow-up for early breast cancer treatment. | Initially, 129 women were assessed, 64 in SFU, and 60 in PIFU; the final assessment included 47 participants for PREMs. | Reduction in unnecessary consultations, potential for tailored care, positive patient-reported experience measures | The increased administrative workload in handling ePROs, potential technology adoption limitations among patients, and response rate of around 70% for questionnaires. | -O: N/A. -T: Feasibility challenges for all patients, the potential for service re-allocation, the need for larger-scale studies, technology barriers among patients, and administrative challenges. |
Early-stage breast cancer |
| 38. | Sissel Ravn, et al. 46 | 2021 | Denmark | To evaluate the effect of a follow-up supported by ePRO on PA and PI in patients undergoing intended curative complex surgery for advanced cancer. | 187 patients who had undergone intended curative complex surgery for advanced cancer at two different departments at Aarhus University Hospital. | ePRO-supported consultations provided a wider scope of dialogue and encouraged patients to ask questions and share their experiences and concerns during follow-up. | ePRO did not improve PA and did not lead to a statistically significant change in PAM scores over time. | -O: Improving patient involvement and promoting dialogue. -T: Contextual factors, clinician’s role, and patient characteristics. |
Patients with metastases to the peritoneal surface undergoing intended curative complex surgery for advanced cancer. |
| 39. | Maria Kristiina Peltola, et al. 47 | 2021 | Finland | To assess the suitability of the Noona ePRO application for patients with cancer, nurses, and doctors at Helsinki University Hospital | - Patients: 44 - Health care professionals: 17 |
- High ease of use and reliability reported by both patients and professionals, indicating user-friendliness. - Potential to improve symptom management and early detection of adverse events. |
- Limited generalizability due to a sample of participants with good digital literacy, which may not represent the broader population. - Small sample size, which may limit the statistical power of the study. - Lack of a control group for comparison, making it difficult to assess the effectiveness of Noona compared to other methods. | - O: Noona has the potential to improve patient satisfaction, quality of life, and clinical management by enabling early detection of adverse events during cancer treatments. - T: Limited application to patients with lower digital literacy, potential technical issues, and a need for further evaluation in more diverse populations. |
Various solid tumor types |
| 40. | Debra Patt, et al. 86 | 2021 |
United
States |
To determine the feasibility of real-world implementation of ePROs among patients with cancer at a large community oncology practice. | 4375 patients |
- High and durable compliance rates - Easy for patients to understand and use - Relevant to patient care - Improved patient satisfaction - Reduced emergency room visits and hospitalizations |
- Compliance declined over time - Barriers to optimal implementation included the absence of additional reminder text or e-mail prompts and changes in workflow due to the COVID-19 pandemic |
- O: -Optimizing engagement strategies and alert mechanisms for clinical staff and patients. -T: -Increased work burden during the pandemic and deprioritization of symptom management due to competing priorities. |
Breast cancer, Chronic leukaemia, Lung cancer, Lymphoma, Multiple myeloma. and Prostate cancer, Small intestine/colorectal cancer |
| 41. | Thomas Licht, et al. 48 | 2021 | Austria | Investigate cancer survivors’ HRQoL, specific deficiencies related to underlying disease or treatment, and benefits of rehabilitation in a variety of cancer entities. | 4401 cancer survivors |
- Significant improvement in HRQOL, psychological distress, and symptoms. The large number of participants. Rehabilitation programs showed effectiveness in improving the quality of life in various cancer entities |
- Nonrepresentative representative study of all cancer survivors, but restricted to those persons who were capable of and felt the need for rehabilitative measures. -No standardized documentation of medical history and socio-demographic data. Severely disabled patients and those in a palliative setting were excluded. No information on the specific rehabilitation program. |
-O: -The rehabilitation program aims to improve the quality of life of cancer survivors by addressing physical and psychosocial needs. The study highlights the opportunity to design specific rehabilitation programs tailored to the unique needs of cancer patients based on their underlying malignancies. -T: N/A |
Various cancer entities, including head and neck, esophageal, gastric, colon, rectal, liver, pancreatic, lung, skin, breast, uterine, ovarian, prostate, testicular, renal, bladder, brain, thyroid, malignant lymphomas, multiple myeloma, leukaemias, and other cancer types |
| 42. | Jeeyeon Lee, et al. 90 | 2021 | South Korea | To evaluate the degree of depression and anxiety in patients with breast cancer during the treatment period and short-term follow-up. | 137 patients with breast cancer | Provides continuous and easily accessible assessment of depression and anxiety. Minimizes the time spent on statistical analysis. | Limited sample size. Did not assess the effect of specific treatments on depression and anxiety. | -O: -Provides valuable data for mental health assessment in breast cancer patients. Can help identify candidates for psychotherapeutic management. -T: N/A |
Breast cancer |
| 43. | Kaitlyn Lapen, et al. 79 | 2021 | United States | Develop and study the implementation of a remote system for toxicity assessment and management of acute breast radiation side effects using ePROs | 678 patients | - Improved patient-clinician communication - Enhanced symptom management - Potential reduction in unnecessary clinic visits | - Weekly surveys could be burdensome for some patients - Alerts generated for symptoms that were already addressed or resolved |
- O: To enhance patient-clinician communication -T: Not understanding the purpose of ePROs |
Breast cancer |
| 44. | M. Kay M. Judge, et al. 93 | 2021 | United States | To identify implementation issues and evaluate the efficacy of an electronic patient self-reporting pain device in community-based cancer clinics. | 178 cancer patients (33 in the pilot phase and 145 in the RCT phase) in community-based clinics |
- Feasible in community oncology clinic settings - Satisfactory time efficiency for comprehensive pain assessment - Data automatically recorded and easily accessed by clinicians - Can help meet regulatory and policy requirements - Empowers patients in the data acquisition process |
- Staff resistance to change - Some elderly patients required assistance with using the technology - Lack of integration with electronic medical records - Accessibility issues for blind patients |
-O: Improved pain assessment, documentation, and analgesic prescription, as well as meeting regulatory requirements. -T: Staff resistance to change and technical integration issues with electronic medical records. |
Various types of Cancer patients |
| 45. | Olga Generalova, et al. 97 | 2021 | United States | Feasibility, implementation, and healthcare utilization outcomes of an ePRO application for cancer patients at an academic medical center. | 72 patients | - Support from organizational leadership and clinical teams at all levels. - Staged implementation allowed for specific action items to be addressed and modified as needed. - Implementation was feasible and acceptable, with high satisfaction rates for ease of use. - Exposure to ePRO did not increase healthcare utilization. |
- Lack of EHR integration. - Possible increased workflow for staff and clinicians. - Patient burden of logging symptoms and issues with the platform. - Lack of integration directly with the primary patient-facing portal. |
-O: N/A -T Concerns about data privacy and security. - Increased healthcare provider burden. - Overdocumentation of symptoms from patients. - Potential cost concerns (estimated at $100 per patient, depending on the scope of services). - Patient trust in reporting personal information. - Potential expansion to patients receiving less frequent care or using telemedicine. |
Patients with advanced cancer in the thoracic, gastrointestinal, and genitourinary oncology groups |
| 46. | Jim W. Doolin, et al. 17 | 2021 | United States | To assess the implementation of an ePRO system for patients starting oral chemotherapy at a cancer center improving patient monitoring, and symptom assessment. | 62 patients who started a new oral chemotherapy regimen agreed to receive online ePROs, and 25 of them completed the ePRO (40% completion rate). A historical cohort of 50 patients was also used for comparison. | - The ePRO system improved time to symptom assessment. - The majority of responses resulted in clinical outreach to manage concerns. |
- The completion rate of ePROs was 40%, indicating challenges in patient engagement. - The need for a project manager to coordinate sending ePROs and track follow-up added administrative demands. - The study’s small sample size and the lack of random allocation in the comparison group limited the ability to control for confounding factors. |
- T: Enhancing providers’ awareness of patients’ concerns when starting new oral chemotherapies. - O: Improving patient engagement with ePROs and evaluating long-term impacts for patients on oral chemotherapy. |
N.A |
| 47. | Kate Absolom, et al. 49 | 2021 | United Kingdom | To evaluate the impact of eRAPID on symptom control, healthcare use, patient self-efficacy, and quality of life in a patient population predominantly treated with curative intent during chemotherapy | 508 consenting patients and 55 health professionals | -Improved physical well-being at 6 and 12 weeks. -Increased patient self-efficacy. -No increase in hospital workload. - Reduction in hospital visits. - Supporting patients with cancer experiencing mild to moderate symptoms. 6 - Feasibility for remote technology-enabled care. |
Patient adherence to weekly symptom reporting was 64.7% and it was limited. | -O: -Reducing hospital visits. -Supporting patients with mild to moderate symptoms-Feasibility for remote technology-enabled care. -T: Limited patient adherence. |
Colorectal, breast, or gynaecological cancers |
| 48. | Dylan M. Zylla, et al. 80 | 2020 | United States | To assess the feasibility of using ePROs for symptom monitoring in patients with advanced cancer | 80 patients with stage IV nonhematologic malignancies on chemotherapy | - Patients found the MyChart survey easy to use and helpful for addressing their symptoms. - The ePRO system allowed for better communication between patients and their oncology care team. - Symptom tracking in real-time facilitated appropriate care for concerning symptoms. |
- Response rates via MyChart were relatively low (46%). - Some symptoms did not result in urgent triage follow-up because they were already being addressed. - Challenges in full automation of ePROs were observed. |
- O: The system provides the potential for improving communication, symptom management, and overall patient satisfaction. - T: Low response rates and challenges in implementation may hinder the full potential of the system. |
Stage IV nonhematologic malignancies include lung, colorectal, prostate, pancreas, head and neck, oesophagal and stomach, breast, ovarian, cervical, endometrial, liver/bile duct, and kidney cancers. |
| 49. | Christine Tran, et al. 50 | 2020 | United States | To explore the feasibility and acceptability of collecting ePROs using validated HRQoL questionnaires for prostate cancer. | 29 patients in total; 1 patient excluded from analysis | High compliance rate, easy to use, facilitated communication between patients and caregivers, value of emotional support and wellness, patients desired personalized engagement tools | Technical issues reported, lack of increased communication with healthcare providers, need for educational support on self-monitoring and management of cancer, potential issues with privacy and data control | - O: Potential for more personalized questions and predictive analytics to increase engagement and participation - T: Privacy and data control concerns |
Prostate cancer |
| 50. | Lærke K. Tolstrup, et al. 51 | 2020 | Denmark | Assess the electronic tool’s impact on reducing severe adverse events by 50% in melanoma patients undergoing immunotherapy. | 146 melanoma patients participated in the study. | Patients in the intervention group called more frequently, indicating increased attention to adverse events. The study also reported high patient and clinician satisfaction with the intervention. | No significant difference was observed between the two groups in the number of Grades 3 or 4 adverse events or the overall number of adverse events. Some patients declined to participate due to a lack of computer skills or perceived demands of the study. A relatively small proportion of patients received combination therapy, where the risk of developing severe adverse events is higher. | -O: The potential to improve patient communication, early relapse detection, symptom monitoring, and quality of life. -T: -The possibility that less technologically adept patients may be excluded from this kind of intervention. The intervention may not have been adequately tailored to detect certain types of adverse events, such as laboratory abnormalities. |
Metastatic melanoma patients receiving immunotherapy. |
| 51. | Sahil Sandhu, et al. 52 | 2020 | United States | To gain insights into oncologists’ perspectives regarding the incorporation of ePROs into routine cancer care at an academic center | 16 oncologists with diverse subspecialties and experience in various cancer types | - Improved patient outcomes. The enhanced quality of life - Reduced emergency department utilization - Prolonged survival - Enhanced patient-centered care - Increased clinic efficiency |
- Limited adoption due to integration difficulties - Concerns about information overload - Patient response rates - Timing of survey distribution - Response validity |
- O: Improving patient-centered care, clinic efficiency, and enhanced documentation for billing support - T: Potential information overload and low patient response rates. |
Genitourinary, Breast, GI, Sarcoma, Urologic, Thoracic, |
| 52. | Cathrine L. Riis, et al. 100 | 2020 | Denmark | Evaluate patients’ satisfaction with care provided using ePROs to individualize follow-up care for women with early breast cancer receiving adjuvant endocrine therapy |
134 women | - Reduced number of consultations, -High patient satisfaction, - Patient-initiated follow-up program customized to the needs of the individual |
- Some patients were excluded due to psychosocial comorbidity, cognitive impairment, or lack of computer skills, - Underpowered for some outcomes |
-O: -Feasibility of ePROs use, customization of follow-up care, potential for tailored self-management advice, and symptom surveillance in cancer care -T: N/A |
Early breast cancer |
| 53. | H. S. Richards, et al. 81 | 2020 | United Kingdom | To evaluate the feasibility of a real-time electronic symptom monitoring system for patients after discharge following cancer-related upper gastrointestinal surgery | 40 participants in the study | - High response rates for symptom reports - Reassurance and valuable support for patients - Enhanced understanding of patients’ experiences for clinicians |
- Technical issues and downtime - Influence of weekly interviews on data completion - Limitations in data pooling from two hospital centers |
-O: -Extending symptom monitoring beyond the acute phase -T: - The need for further refinement to avoid erroneous symptom alerts |
Cancer-related upper gastrointestinal surgery (oesophageal, gastric, hepato-pancreato biliary cancer) |
| 54. | Florence D Mowlem, et al. 53 | 2020 | United Kingdom | To understand the impact of anticancer treatment on oncology patients’ ability to use ePRO. | Seven individuals with cancer diagnosis and treatment experience. | - Participants preferred electronic PROs over paper completion - Mobile devices were seen as helpful for staying connected during illness - Positive attitude towards using technology for assessments |
- Peripheral neuropathy of the hands affecting device interaction - Fatigue and concentration issues impacting ePRO completion - Changing health status based On the treatment cycle, which would impact their device use |
- O: Flexibility in survey completion, larger buttons, pause functionality, and BYOD options for patients to complete ePROs on their own devices. - T: Potential missing data due to symptoms and impairments |
Breast, Prostate, and Colon/bowel |
| 55. 184 | Christina karamanidoua, et al. 96 | 2020 | Greece | To develop a novel ePRO-based palliative care intervention for cancer patients by eliciting end-users’ needs judgments of the MyPal system, and recommendations for improvement. | Nine patients with CLL | Valued contact with the healthcare team, freedom of reporting symptoms, validity and reliability of information | Concerns about the reliability of collected data, interpretation of collected data, privacy, and digital safety of collected data | -O: Opportunities include improving patient engagement and providing personalized information. -T: Threats include potential data quality issues, incorrect data interpretation, and privacy concerns. |
CLL and MDS |
| 56. | Doris Howell, et al. 91 | 2020 | Canada | To implement electronic Patient Reported Outcomes (e-PROs) in “real-world” oncology practices for personalized management of generic and targeted symptoms of pain, fatigue, and emotional distress (depression, anxiety). | Over 6000 patients completed e-PROs | - Increased e-PRO completion rates - Acceptability of e-PROs by patients (76%) and clinicians (80%) - Improved patient experience - Significant reduction in anxiety - Higher levels of patient activation - Reduced hospitalization rates |
- Varying baseline rates of e-PRO use at different sites - Limited sample sizes - Heterogeneity and potential within-site clustering in pre/post population cohort comparisons - Complex implementation challenges |
-O: - Opportunity to use e-PROs as performance metrics and in value-based care -T: - Challenges in facilitating implementation across multiple disease site teams - Health system restructuring in Montreal, Quebec - Implementation challenges in “real-world” oncology practices |
Lung and sarcoma cancer |
| 57. | Afaf Girgis, et al. 95 | 2020 | Australia | Evaluate the effectiveness of the PROMPT-Care web-based system in a diverse population of cancer patients by reducing emergency department presentations and other health service outcomes. |
328 patients received the intervention, and 1312 patients were matched as controls. | - Reduced emergency department service by 33% among patients receiving the intervention compared to controls. - Emphasized automated triggers for reviewing elevated patient report results and highlighted nurses’ crucial role in managing alerts. - Provided patients with resources to support guided self-management. |
- The response rate was low, possibly contributing to recruitment bias. - Limited follow-up and engagement with the system. - Challenges in balancing screening burden and timely alerts |
-O: The system can help reduce the high demand for health services, provide targeted systematic care to patients in need, and support patients’ self-management. -T: Treats include reaching underserved patient populations, assessing PROs in languages other than English, and cultural adaptation of resources. |
Patients with solid tumors |
| 58. | Emilie A. C. Dronkers, et al. 18 | 2020 | Netherlands | To evaluate the implementation of an ePROs system, in the routine care of HNC patients. | -Quantitative: HM group (45 patients), Standard care group (46 patients) - Qualitative: Interviews with 15 HM patients |
- Improved doctor-patient communication - Increased efficiency of the consultation using HM. - Patients felt better prepared. - Enhanced focus on critical issues. - Graphical display of results aids in systematic monitoring of symptoms. - Patients can actively participate in their care. |
- Implementation of HM required significant time and energy. - Organizational and workplace adjustments were needed. - A sustainable technical environment was essential. - Extra costs were not reimbursed by health insurers or the government. - Some patients found the questionnaires unclear or irrelevant. |
- O: Improved patient care, better data for research, increased patient engagement, potential cost-effectiveness, improved doctor-patient communication. - T:Time and resource constraints, resistance to change, and costs not reimbursed. -Dedication and support from all team members were necessary |
Head and neck cancer |
| 59. | Noa Biran, et al. 98 | 2020 | United States | Evaluate the acceptability and appropriateness of an ePRO intervention for patients with RRMM and explore its impact on clinic workflow | 11 patients with RRMM were recruited, and 9 patients completed the study | - High completion rate for weekly guided sessions - Patients found the app easy to use and understand - Increased patient awareness of symptoms - Potential for improving clinical research and care |
- Clinic staff found app alerts to be too numerous and redundant - App alerts couldn’t differentiate between chronic and acute symptoms - Lack of integration of the intervention data into routine care |
-O: - Encouragement for patients to stay in therapy - Improved symptom management - Increased patient empowerment - T: -A high volume of alerts can burden clinic staff -Alert logic may need refinement - Lack of data integration into clinic workflow |
RRMM |
| 60. | Lorraine Warrington, et al. 82 | 2019 | United Kingdom | To field test the eRAPID system, an online tool for monitoring and managing adverse events in patients with cancer during treatment. | 12 patients receiving chemotherapy for early breast cancer and 10 health professionals (oncologists and specialist nurses). | - Patients found eRAPID easy to use and valued the self-management advice. - Potential to improve patients’ self-efficacy, knowledge, and confidence in managing symptoms during treatment. - Positive patient feedback, describing eRAPID as “reassuring” and a “safety net.” |
- Some patients forgot to routinely complete the weekly report. - Notifications for severe symptoms could be triggered for resolved symptoms, leading to patient worry. - Variability in staff engagement with patient-reported data in clinical encounters. |
-O: - Potential to increase patient self-efficacy and engagement in care. - Improving patient self-management and reducing hospital resource utilization. - Enhancing patient activation in their healthcare. -T: - Notifications for resolved symptoms could cause unnecessary patient worry. |
Patients with early breast cancer were tested in the field usability study. The eRAPID system is being evaluated in a larger population, including patients with breast, gynecology, or colorectal cancer. |
| 61. | Hilde Krogstad et al. 104 | 2019 | Norway | To evaluate the usability of the EirV3 system used for PROMs in cancer care | 37 patients, 17 physicians | - Easy to use by patients and physicians in various care settings - Relevant for different cancer diagnoses and treatments |
- Some irritant and moderate usability issues identified - Limited ability to address severe usability issues |
-O: -Potential integration of EirV3 into daily clinical practice -T: N/A |
Breast, Gastrointestinal, Lymphomas, Prostate, Gynecological, Lung, Malignant melanoma, and Testicular cancers |
| 62. | Yuichiro Kikawa, et al. 54 | 2019 | Japan | Evaluation of HRQoL monitoring from home among MBC patients using the CHES | 16 MBC patients who received outpatient chemotherapy or endocrine therapy, both with and without targeted therapy. | - Acceptable compliance with electronic HRQoL data collection (84.6%). - Potential for real-time home monitoring to improve overall HRQoL. |
- Small sample size. - Participants needed access to the Internet. - Wide range of compliance between patients. - Disease progression and forgetting were common reasons for missing data. |
-O: -Beneficial for MBC patients, but the impact may vary in different healthcare systems and regions. - Increased access to hospitals in Japan due to the national health insurance system may affect the survival benefit of using ePRO. -T: -Future research is needed to explore its usefulness further. |
MBC |
| 63. | Sanna Iivanainen, et al. 55 | 2019 | Finland | Investigate whether symptoms collected by the Kaiku Health ePRO tool on cancer patients receiving ICI | 37 patients | - Good adherence to ePRO follow-up. - Strong correlation with symptoms seen in clinical trials. |
- Low response rate for QoL questionnaires. - Limited clinical outcomes data. |
-O: N/A -T: Correlations between symptoms may reflect therapeutic efficiency, side effects, or tumor progression and should be further investigated. |
Various types of cancer |
| 64. | Gregory M. Gressel. et al. 101 | 2019 | United States | To establish feasibility and acceptability of PROMIS ePRO integration in a gynecologic oncology outpatient clinic and assess if it can help identify severely symptomatic patients and increase referral to supportive services. | 336 patients in the Gynecologic Oncology Clinic: |
- PROMIS ePRO administration is feasible and acceptable to gynecologic oncology patients. - It can help identify severely symptomatic patients for referral to ancillary support services. |
- Language limitation (only available in English). - Lack of information about the follow-up of referrals and whether symptom scores improved postreferral. |
-O: To improve symptom identification and support for gynecologic cancer patients. -T: - Barriers that patients face in the referral process need further investigation. The cost-effectiveness of implementing these instruments should be explored. |
Gynecologic cancer |
| 65. | Jeannine M. Brant, et al. 87 | 2019 | United States | To determine the perception of patients and providers from patient-reported outcomes | 121 women (51 with gynecologic cancer and 70 with breast cancer) | - Patients reported the usefulness of CPs. - CPs improved team communication, helped find needed resources and managed symptoms. - Provider satisfaction with customization of patient recommendations. |
- Small sample size. - Missing data due to disease progression and nonresponse. - Overwhelming of patients at the beginning of treatment. |
-O: Improved symptom management, communication, and potentially cost reduction. -T: -Time constraints, perceptions of PROs as intrusive, lack of knowledge on how to address information, and issues related to liability. |
Breast Cancer, Gynecologic Cancer |
| 66. | Kerry N. L. Avery, et al. 83 | 2019 | United Kingdom | To develop a hospital EHR-integrated ePRO system to improve the detection and management of complications postdischarge following cancer-related surgery | Phase 1: 18 patients, Phase 2: 59 participants who provided 444 complete self-reports | - Integration into hospital her - Real-time symptom monitoring - Clinical algorithms for alerting clinicians - Tailored self-management advice - Web-based access - Improved symptom control and patient safety |
- Limited sample size - Developed in a single center - Integration issues with her - Potential IT problems - Limited generalizability |
-O: Improved patient outcomes, reduced emergency admissions, and healthcare cost savings. -T: Integration issues, IT problems, limited generalizability. |
Cancer-related major abdominal surgery |
| 67. | Sasja A. Schepers, et al. 56 | 2016 | Netherlands | Determine the fidelity of the KLIK method as implemented in outpatient pediatric cancer care | 205 children with newly diagnosed cancer | - Enhanced discussion of psychosocial functioning - Better detection of HRQoL problems - Higher HCP-reported satisfaction with care |
- Barriers related to organizational issues - Decreasing adherence to completion of HRQoL questionnaires over time - Barriers related to the user’s motivation and the KLIK method itself |
-O: N/A -T: Challenges in a complex clinical setting, such as pediatric oncology during the early stages of treatment - The need for tailored implementation strategies to address specific barriers |
Pediatric cancer: Leukemias/lymphomas, Solid Tumors, and Brain Tumors |
| 68. | Joshua R. Niska, et al. 57 | 2017 | United States |
To assess changes in QoL and AEs during RT for head-and-neck cancer using electronic PROQOL data. | 65 patients | - Real-time ePROs collection allowed for systematic monitoring of QOL and AEs during RT. - Could potentially improve physician-patient communication. - Clinically meaningful changes were color-coded in the tabular format to capture the attention of clinicians. - Electronic data collection added only an average of 2.9 additional minutes to the clinical encounter. |
- Small sample size (N = 65) with limited power. - Unplanned subgroup analysis of CCRT and RT-alone patients. - Potential confounders due to unbalanced CCRT and RT-alone groups. - Retrospective collection and grading of AEs from medical records. - Possible ascertainment bias in AE data extraction. |
- O: Real-time ePROs can help detect and address patient concerns and mitigate AEs. Further studies can explore the role of PROs in addressing patient needs and reducing AEs during head-and-neck RT. - T: Potential for inaccuracies in AE reporting and grading by different providers. |
Head and neck cancer |
| 69. | Steven M. Lucas, et al. 58 | 2017 | United States | To report on the establishment of a unified, electronic PRO infrastructure and | 773 eligible patients, with 688 (89%) enrolled preoperatively | High enrollment rate, high completion rate, ability to collect PROs electronically, immediate access to survey responses during clinic visits, and opportunities for quality improvement. | Approximately 25% of patients still required paper responses, limited sample size and short-term follow-up, MID not yet described for the survey. | -O: - Opportunities include improved surgical care, quality improvement, risk-adjustment techniques, and better patient counseling. -T: Threats include the administrative effort required to achieve high completion rates. |
Prostate cancer |
| 70. | P. Holch, L, et al. 59 | 2017 | United Kingdom | To develop a system for patients to self-report and manage AE during and after cancer treatment | Patient advocates (N = 9), patients (N = 13), and staff (N = 19) participated in usability testing | - Patients can report AE from home - Immediate self-management advice for low or moderate AE - Email notifications for severe AE - Integration with EPR - Real-time access to patient data for clinicians - Secure data transfer through NHS network |
- Requires training for staff and patients - Integration challenges in different NHS settings - Usability on smartphones could be improved |
-O: - Opportunity to improve patient care, safety, and quality of life by reducing AE-related emergency admissions and enhancing communication between clinicians and patients -T: - Challenges in interfacing with different EPR systems. - Potential resource and administrative challenges in busy hospitals |
Breast, gynaecological, colorectal, pelvic radiotherapy, upper gastrointestinal surgery |
| 71. | Andreas D. Hartkopf, et al. 60 | 2017 | Germany | To investigate the willingness, and assess specific needs, and barriers of aBC and mBC patients in nonexposed and exposed settings before implementing digital ePRO | 202 participants (nonexposed group: 96, exposed group: 106) | - Increased willingness to use ePRO among exposed patients. - Reduction of barriers in the exposed group, such as data security and technical skills. |
- Concerns about data privacy and technology usage. - Lack of prior technology usage. |
O: N/A -T: - Emphasizing the need to address and eliminate barriers to data accuracy and reliability in future ePRO assessments. - Exposure to ePRO appears to increase willingness to use and reduce barriers. |
Breast cancer |
| 72. | Kate Absolom, et al. 61 | 2017 | United Kingdom | To improve the safe delivery of cancer treatments, enhance patient care, and standardize AE documentation | Internal pilot phase with 87 participants, full trial target sample of 504 participants | - Empowers patients to self-report symptoms and side effects of cancer treatments from the comfort of their home - Provides immediate access for clinical teams to AE reports via the EPR - Enhances systematic AE reporting, ensuring early detection and intervention - Provides patient advice on managing mild AEs, improving the patient’s ability to self-manage - Reduce healthcare costs through better AE management - May improve patient outcomes and quality of life during cancer treatment - Can extend to long-term survivorship care, providing long-lasting benefits |
Not specified | - O: May have broader applications beyond the cancer treatment context. - Opportunity: Could lead to improved standardization of AE documentation across healthcare systems - T: Potential system usability issues not explicitly mentioned in the article |
Breast, colorectal and gynaecological cancer |
| 73. | Liv Marit Valen Schougaard, et al. 62 | 2016 | Denmark | To implement telepatient-reported outcomes (telePRO) as the basis for follow-up in chronic and malignant diseases using the generic PRO system AmbuFlex | AmbuFlex was implemented in nine diagnostic groups in Denmark. A total of 13,135 outpatients from 15 clinics have been individually referred. -Response rates for the initial questionnaire ranged from 81% to 98% in different patient groups |
- Improved quality of care by flagging important symptoms and producing better documentation of patient information -Promotion of patient-centered care with a focus on patient’s needs and knowledge about their disease -Optimization of healthcare resource utilization -Use of PRO data for research and hospital quality assurance |
Potential challenges may include low response rates, clinician reluctance, and the need for training programs for clinicians | - O: Economic potential related to canceled consultations, reduced reimbursement of patient transportation costs, and reduced need for the destruction of medicine in cancer treatment The need for reorganization of conventional care in the healthcare system -T: N/A |
Prostate, colorectal cancer |
| 74. | Maria K. Peltola, et al. 63 | 2016 | Finland | Assess the suitability of Kaiku® (an ePRO application) for collecting PROs related to early side effects of radiotherapy and health-related quality of life in HNC patients. | Nine HNC patients were approached, and five consented to participate. | - High patient compliance with the system. - Patients found the system easy to use. - Efficient monitoring of side effects and quality of life. - Potential for early detection of symptoms and improved patient management. |
- Limited sample size, preventing statistical analysis. - Suitability was assessed only by patient compliance. - Symptoms were reported on a nonvalidated scale. - No process for providing feedback to patients based on self-reported symptoms. |
- O: -Cost-effective way to organize individualized follow-up for HNC survivors. - T: Limited patient acceptance due to information technology issues. |
HNC |
| 75. | Beate Mayrbäurl, et al. 64 | 2016 | Austria | To assessHRQoL in patients with advanced colorectal cancer across different lines of palliative chemotherapy | 100 consecutive patients with colorectal carcinoma | - Provides insights into the longitudinal course of HRQOL across different chemotherapy lines in patients with advanced colorectal cancer. - Provides data on how HRQOL changes over time during palliative chemotherapy. - A lower symptom burden and better QOL than those with progressive disease. |
- The study may have limitations due to a decrease in the number of patients across treatment lines, affecting the analysis of patients receiving three or more chemotherapy lines. - Timing and frequency of HRQOL assessments can be challenging. - Compliance with follow-up assessments may be lower in clinical practice compared to clinical trials. |
- O: -Considering HRQOL in the treatment of patients with metastatic colorectal cancer. - Routine evaluation of HRQOL during all chemotherapy lines is recommended to aid in comparing treatment options and making informed decisions. -T: N/A |
Colorectal cancer |
| 76. | J. Graf, E. et al. 65 | 2016 | Germany | To determine the extent to which existing computer skills, disease status, health-related quality of life, and sociodemographic factors affect patients’ willingness to use electronic methods of data collection (ePRO) | 96 | Provides insights into patient preferences for electronic vs. paper-based surveys, potentially improving data collection in breast cancer patients | Limited sample size, potential selection bias, and self-reported data may not be entirely accurate | -O: - Providing support and improving the user-friendliness of ePRO applications. -T: Identifying barriers to the use of electronic surveys, particularly in older patients and those with lower quality of life. |
Breast cancer |
| 77. | Katharina Duregger, et al. 66 | 2016 |
Austria | To develop a concept and implement a prototype for introducing ePRO into the existing neuroblastoma research network by applying NFC and mobile technology. | N/A | - Improved data collection through ePRO. - Enhanced patient empowerment. - Potential for remote patient monitoring and treatment. - Integration with existing research networks. - Increased data security through pseudonymization. - Usability and ease of patient registration for physicians. |
- The prototype was not fully functional, requiring further development. - The exact number of participants was not specified in the article. - Limited data on patient outcomes or system performance. - Challenges in managing lost ID cards or forgotten PINs in the long term. |
-O: Improved data quality, patient engagement, and remote monitoring. -T: Prototype status, potential technical challenges in full implementation, and the need for a complete back-end system. |
Neuroblastoma (the primary focus of the study), but the system’s applicability extends to other pediatric cancers and rare diseases. |
| 78. | Renee A. Cowan, et al. 88 | 2016 |
United States | The assessment, and feasibility of acceptability and satisfaction of a Web-based system for capturing PROs in the immediate postoperative period in gynecologic cancer surgery patients. | 96 eligible patients | - Most patients found STAR easy to use and useful. - Patients reported a positive experience with the system and would recommend its use. - Collecting PROs in the immediate postoperative period can enrich preoperative teaching, help identify complications earlier, and improve symptom control. |
- Clinical personnel found that the STAR system increased their current workload without enhancing patient care. - Some patients found the program too rigid and the questions didn’t account for actual conditions. - A few patients felt isolated due to the technology limiting communication. |
-O: - Potential for increased patient empowerment. - Could facilitate clinical research. - Symptom reports could be summarized and printed for provider review before appointments, making postoperative appointments more efficient. - Requires further research to improve clinician satisfaction and the system’s usefulness. - T: -Applicability may be limited by the need for technology-savvy patients and economic factors (home computer and internet access). |
Gynecologic cancer |
| 79. | L. M. Wintner, et al. 67 | 2015 | Austria | Assessment, and the feasibility of routine clinic-ePRO/home-ePRO with the CHES software. | - 113 patients for clinic-ePRO - 45 patients for home-ePRO |
- High willingness of patients to participate in routine clinic-ePRO assessments (94.7% of clinic-ePRO patients) - Patients’ preference for electronic data entry (67.2% of clinic-ePRO patients) - High satisfaction with the graphic display of the questionnaire (91% of clinic-ePRO patients) - Perceived usefulness of PRO data for informing physicians (64.6% of clinic-ePRO patients) |
- Some patients perceived clinic-ePRO as too impersonal (57.5% of clinic-ePRO patients) - Not allowing for individual situations (30.1% of clinic-ePRO patients) - Technical issues and complexity (4.1% combined) - Concerns about data security (mentioned by one patient) |
- O: Improving familiarity with and acceptance of ePRO assessments -T: - Digital divide affecting older and computer-illiterate patients - Need for educating patients about the complementary nature of PROs |
Gastrointestinal, glioma, gynaecological, lung, neuroendocrine, and testicular cancers |
| 80. | Lynne I. Wagner, et al. 89 | 2015 | United States | To integrate ePRO assessment into the EHR and clinical workflow for symptom screening in ambulatory cancer care. | 636 women receiving gynecologic oncology outpatient care | - Immediate EHR integration for real-time assessment results. - Automated triage for psychosocial, informational, and nutritional concerns. - Precise and robust measurement of symptoms. |
- The response rate for completing the entire assessment was lower when patients had to initiate the assessment. - Limited generalizability to patients with EHR patient electronic communication accounts. |
-O: Improved symptom and psychosocial management, meeting emerging accreditation standards. -T: Limited patient participation, and potential differences between participants and nonparticipants. |
Ovarian, Uterine, Cervical, Other female genital malignancy |
| 81. | Erqi L. Pollom, et al. 68 | 2015 | United States | To evaluate the feasibility of eQOL data collection using a touch-screen tablet device in patients undergoing treatment for head and neck cancer | 50 patients | - High compliance rates during and at the end of treatment. - Reasonable average time to complete the survey (9.8 min). - Utilization of tablet devices already available in the clinic. |
- Usability challenges for elderly patients (70 years old). - Some patients required assistance with electronic forms. - Potential for technical difficulties during survey administration. |
- O: Efficient data collection, improved mobility, and reduced data entry errors. - T: Challenges related to patient acceptance, usability, and potential technical issues. |
Head and neck cancers |
| 82. | Sophia K. Smith, et al. 69 | 2014 | United States | Demonstrate how an ePRO system can aid in distress management in oncology. | 17,338 | - Cost-effective and efficient symptom score collection - Multidisciplinary approach to distress management - Streamlined triage process for psychosocial care referrals. |
- Lack of detailed psychosocial screening questions - No electronic upload of PRO data to medical records. | -O: Expansion to other disease groups, development of a web-based ePRO system. T: N/A |
Breast, lung, and gastrointestinal cancer patients |
| 83. | L M Wintner, et al. 70 | 2013 | Austria |
To assess the QoL of lung cancer patients undergoing CT across multiple treatment lines. | 187 | - The study provides insights into QOL in lung cancer patients undergoing CT across multiple treatment lines. - It suggests that CT itself did not negatively impact QOL, with most QOL aspects remaining stable during CT. - QOL assessments can be effectively conducted |
- Sample size decreased across CT lines, potentially affecting the generalizability of results. - The study included both nonsmall cell lung carcinoma (NSCLC) and small-cell lung carcinoma (SCLC) patients, which may introduce heterogeneity. - The variety of administered cytotoxic agents may confound the results. |
-O: -The system provides the potential for close-meshed routine QOL monitoring, which could facilitate early recognition of symptom aggravation and timely intervention. - T: Data may be influenced by the specific CT regimen used, and the variety of CT agents could be a confounder. |
Lung cancer |
| 84. | August Zabernigg, et al. 1 | 2012 | Austria | To investigate QOL trajectories from adjuvant treatment to palliative third-line therapy | 80 patients (pancreatic cancer and cancer of the bile ducts) | Frequent assessments, short intervals for QOL data, real-world clinical practice data | Limited statistical power due to a relatively small sample size, heterogeneity in the patient population | - O: - Providing more robust QOL information in clinical trials, the potential for identifying influential factors on patients’ QOL -T: N/A |
Pancreatic cancer and Bile duct Cancer |
| 85. | Abernethy, Amy P. MD, et al. 71 | 2010 | United States | Demonstrate a rapid learning healthcare model in an academic oncology clinic using ePROs as foundational data | Metastatic breast cancer (n = 65) and gastrointestinal cancer (n = 113) patients in Duke Cancer Clinics | Real-time research-quality data collection, acceptance of e/Tablets, linkage of ePRO and other datasets | Technological challenges, data privacy concerns, potential for data compatibility issues | -O: Potential for CER, personalized medicine, improving patient outcomes -T: N/A |
Breast and gastrointestinal cancer |
Note. O: opportunity; T: threats; ePRO: electronic patient-reported outcome; IO: immuno-oncology; HC: historical control; DoT: duration of therapy; OS: overall survival; NSCLC: nonsmall cell lung cancer; HNC: head and neck cancer; OCM: oncology care model; AYA: adolescents and young adults; HCP: healthcare providers; HRQoL: health-related quality of life; STS: soft tissue sarcoma; APNs: advanced practice nurses; eSAC: electronic self-assessment and care; irAEs: immune-related adverse events; CNS: central nervous system; PA: physical activity; QoL: quality of life; ICPs: integrated care pathways; RT: radiotherapy; EPR: electronic patient record; PROs: patient-reported outcomes; mCRPC: metastatic castration-resistant prostate cancer; PI: patient involvement; PAM: patient activation measurement; CLL: chronic lymphocytic leukemia; MDS: myelodysplastic syndromes; HNC: head and neck cancer; RRMM: relapsed and refractory multiple myeloma; PROMs: patient-reported outcome measures; CHES: computer-based health evaluation system; ICI: immune checkpoint inhibitors; AEs: adverse events; aBC: adjuvant breast cancer; mBC: metastatic breast cancer; BYOD: bring your own device); RRMM: relapsed and refractory multiple myeloma; MBC: metastatic breast cancer; PROQOL: patient-reported QOL; MID: minimum important clinical difference; NFC: near field communication; ePROMs: electronic patient reported outcome measures; eRAPID: electronic-patient self-reporting of adverse-events: patient information and aDvice; AES: adverse events; HM: healthcare monitor.
