Abstract
The growing and ubiquitous digitalization trends embodied in eHealth initiatives have led to the widespread adoption of digital solutions in the healthcare sector. These initiatives have been heralded as a potent transformative force aiming to improve healthcare delivery, enhance patient outcomes and increase the efficiency of healthcare systems. However, despite the significant potential and possibilities offered by eHealth initiatives, the article highlights the importance of critically examining their implications and cautions against the misconception that technology alone can solve complex public health concerns and healthcare challenges. It emphasizes the need to critically consider the sociocultural context, education and training, organizational and institutional aspects, regulatory frameworks, user involvement and other important factors when implementing eHealth initiatives. Disregarding these crucial elements can render eHealth initiatives inefficient or even counterproductive. In view of that, the article identifies failures and fallacies that can hinder the success of eHealth initiatives and highlights areas where they often fall short of meeting rising and unjustified expectations. To address these challenges, the article recommends a more realistic and evidence-based approach to planning and implementing eHealth initiatives. It calls for consistent research agendas, appropriate evaluation methodologies and strategic orientations within eHealth initiatives. By adopting this approach, eHealth initiatives can contribute to the achievement of societal goals and the realization of the key health priorities and development imperatives of healthcare systems on a global scale.
The background of eHealth initiatives: the digitalization of processes and the process of digitalization
Global digitalization trends have been rapidly evolving in recent years, with various information and communication technologies (ICTs) and innovations shaping our societies and economies. In the era of digital transformation, the field of healthcare has witnessed a remarkable surge in the adoption of high-profile digital novelties. 1 Digitalization in healthcare, often referred to as eHealth or digital health, is revolutionizing the operation of the healthcare ecosystem, its structure and the roles and relationships between the stakeholders. eHealth initiatives encompass the use of internet technologies, digital solutions and data in their efforts to enhance healthcare delivery, improve patient outcomes and advance the efficiency of healthcare providers and the healthcare system in general. 2 The evolution of eHealth initiatives has been driven by the rapid advancement of various digital tools, which have enabled the collection, storage and exchange of vast amounts of healthcare data. From electronic health records and telemedicine to mobile health applications and artificial intelligence-based diagnostics, eHealth initiatives involve a wide range of digital solutions with the aim of transforming healthcare systems worldwide. These initiatives have the potential to bring significant impacts and benefits to the healthcare sector. Here is a short outline of some of the most important implications of eHealth initiatives.
Improved efficiency and productivity: eHealth solutions can streamline healthcare processes, thereby reducing paperwork and administrative burdens. Electronic health records, telemedicine and remote monitoring tools enable efficient data exchange, faster decision-making and improved coordination among healthcare providers, leading to better management of care and work efficiency. 3
Enhanced access to care: eHealth solutions, such as telemedicine and mobile health apps, can overcome geographical barriers and improve access to healthcare services, particularly in remote or underserved areas. 4 Patients can receive timely consultations, follow-ups and health information regardless of their location.
Empowered patients: eHealth solutions have the potential to empower patients by providing them with access to their health information, educational resources and self-management tools. 5 This can lead to increased patient engagement, shared decision-making and better adherence to treatment plans.
Improved healthcare outcomes: eHealth solutions can contribute to better health outcomes by facilitating early detection and intervention, reducing medical errors and improving care coordination. 6 Real-time monitoring and data analytics enable proactive healthcare interventions and personalized treatments.
Cost savings: eHealth solutions have the potential to reduce healthcare costs by minimizing hospital readmissions, preventing unnecessary diagnostic tests and optimizing resource allocation. 7 Remote consultations and telemedicine can also reduce travel, accommodation and other expenses for patients.
Research and population health: eHealth solutions generate vast amounts of data that can be utilized for research, population health analysis and public health planning. 8 Aggregated data from diverse sources can help identify trends, track disease outbreaks and support evidence-based policymaking.
eHealth initiatives, aimed at leveraging ICTs to enhance healthcare systems and healthcare service delivery, have promised numerous benefits and profits for all stakeholders as described above. However, in a general wave of enthusiasm, these promises often triggered excessive and unfounded expectations among the public, mass media and numerous high-ranking individuals in the medical and political spheres.9–11 Amidst the hype surrounding eHealth initiatives, it is essential to critically examine their implementation and capacities, and assess the validity of the claims made. While eHealth initiatives hold significant promise, it is crucial to recognize the prevailing failures and fallacies that can hinder their successful realization. One very common misconception is the notion that technology alone can solve complex healthcare challenges and issues. Although ICTs provide valuable tools, their effectiveness depends on various factors, including the sociocultural context, education and training, the organization of healthcare, regulatory frameworks and the involvement of end users, be they patients or healthcare professionals.12,13 Moreover, a range of other failures and fallacies stem, on the one hand, from the misallocation of resources, over-optimistic expectations or inadequate planning, resulting in unrealized benefits or unintended consequences, resistance to change, or, on the other hand, from technological or healthcare data areas, in terms of inadequate ICT infrastructure, interoperability and standardization issues, data privacy and security concerns. Neglecting these crucial elements can lead to the overall downfall of eHealth initiatives, rendering them inefficient or even counterproductive.
By shedding light on the failures and fallacies inherent in eHealth initiatives, this article seeks to contribute to a more realistic and evidence-based approach to their planning and implementation. Figure 1 illustrates the architecture of the Slovenian eHealth project, encompassing ambitious categories such as patients/citizens, healthcare professionals, healthcare informatics, education and training, promotion, strategic tasks, operational tasks and international integration. However, in practice, stakeholder cooperation and task implementation are notably deficient. Engagement of policymakers and promotion of eHealth is limited, sociocultural determinants of health professionals and patients are inadequately considered, user education and training are at a low level, and normative regulation in the entire field is inconsistent, relying on intermittent political interests and arbitrary decisions. On the other hand, the majority of issues arise from complex substantive matters, which necessitate attention through a range of systemic measures and additional resources (primarily human). Enhanced cooperation between sectors (health, education and digital industry) could lead to an increased number of competent experts. This, in turn, could contribute to a better understanding of the wider context of eHealth, and facilitate the resolution of specific contextual and professional challenges outlined above, and lay the groundwork for more efficient and expedited development of eHealth in the future.
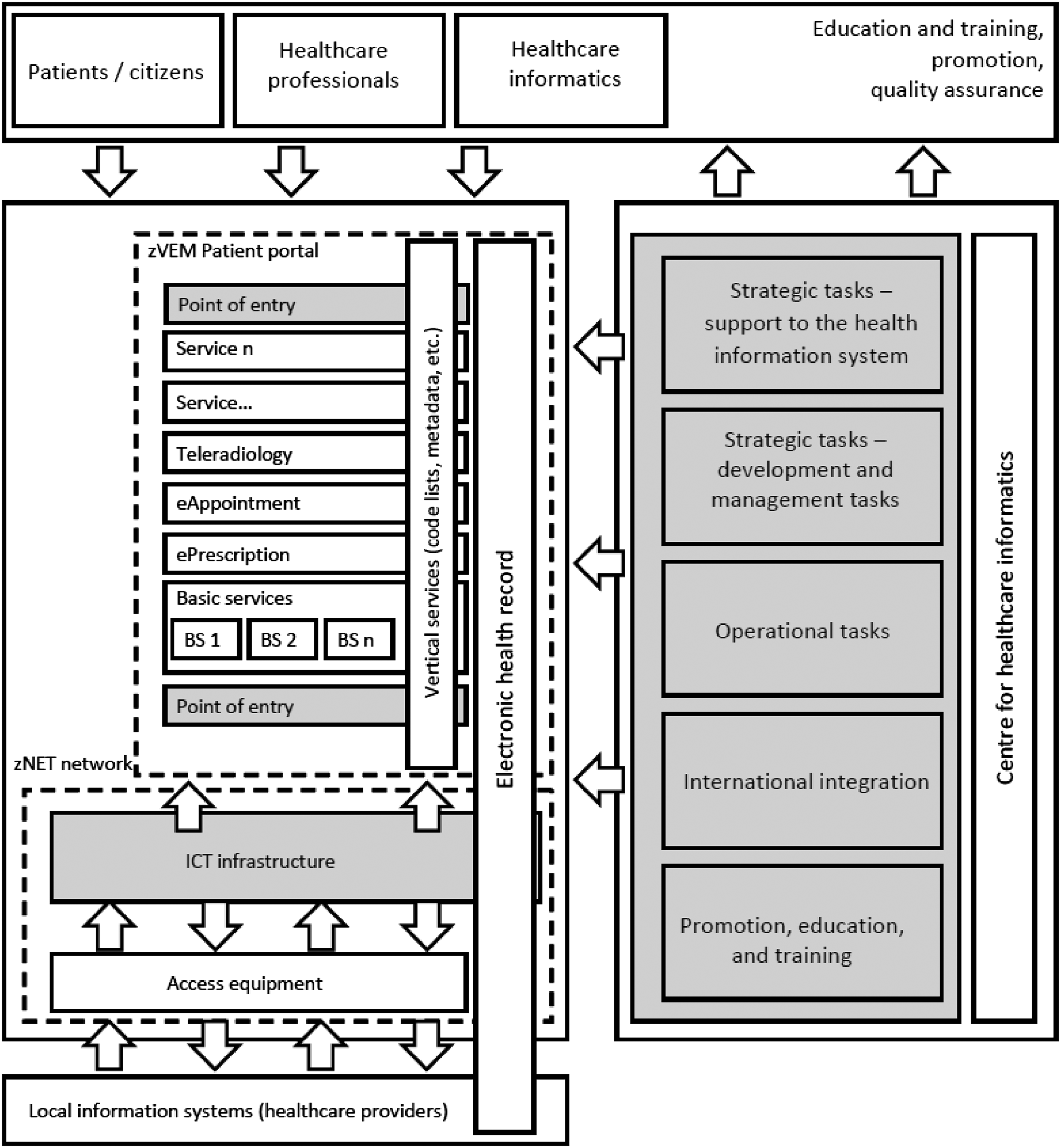
Architecture of the Slovenian eHealth project.
Despite these limitations, substantial progress has been achieved in recent years in implementing and utilizing eHealth solutions in Slovenia. The hope is that recent developments in eHealth signify an increased awareness among decision-makers, and especially users, about the significant impact that digital solutions can have on public health, providing crucial support to decision-making, planning and overall health system management.14,15
Certainly, questions arise about the potential achievements in the entire field of eHealth during this period if the approach to implementing eHealth initiatives had been more comprehensive and had garnered greater support from critical ecosystem stakeholders and factors.16,17 Addressing these challenges is crucial for the effective utilization of eHealth initiatives, ensuring that they fulfill their potential to improve healthcare outcomes and enhance patient-centered care on a global scale.
Most jurisdictions that already have well established eHealth programs, including Slovenia, face similar challenges in the aforementioned areas. In addition to systemic, sociocultural, educational, normative, organizational and other concerns, the most significant issue is the severe shortage of professionals possessing the requisite competencies and experience at the intersection of medicine and informatics. They represent the primary catalyst for the beneficial and effective further development of eHealth. In view of this, it is imperative to enact the necessary changes and comprehensively address the outlined challenges, particularly concerning human resources, which have profound implications for all other factors. This endeavor will be very intricate as it demands close collaboration among various social subsystems and a long-term approach.
Methodological considerations
The rapid proliferation of ICTs in the recent period and the growing need for effective digital solutions throughout the operation of the healthcare system have triggered research interest in studying the numerous and diverse aspects of eHealth initiatives and individual digital solutions. 18 As a result, the research in the field is relatively extensive and on the rise today. Given the complex nature of eHealth initiatives, such research focuses on various features and challenges concerning this phenomenon. 19 Studies sometimes tend to be too general, on the one hand, or too particularized and narrow, on the other, making it hard to create an objective narrative and gain a wider sense of the most significant factors and characteristics of eHealth initiatives, which to a large extent pre-determine the success as well as the disappointment of these large sociotechnical projects. Although several literature reviews, case studies, expert interviews, international comparisons and other analyses and assessments of eHealth initiatives were performed in the past, there has been no compelling observation or evaluation of the potential benefits of eHealth solutions in a broader systemic sense, let alone in a global context. Research often addresses technological/technical, user, organizational, financial, data, process, security, semantic and other—sometimes more peripheral or isolated—aspects of eHealth initiatives, without reflection on broader societal goals and the key health priorities and development imperatives of today's healthcare systems.
It is evident that from the initial eHealth initiatives around the year 2000 up to the present day, consistent research agendas and appropriate guidelines for the evaluation (ex ante and ex post) of eHealth initiatives have not been established.20–22 The lack of a unified methodological framework—to a certain degree including relevant indicators and metrics, which could represent an applicable platform to analyze usability, effectiveness, and, if possible, other broader and possibly longer-term implications of eHealth initiatives—has enabled arbitrary observations and evaluations in this field. Investing a certain amount of effort and resources and attempting to create a consistent and balanced evaluation framework could be instrumental in the targeted promotion of more effective and faster progress in the field of eHealth. Such a framework would, at least at the overall level, strive to assess the development, applicability and other impacts of eHealth solutions, thereby outlining strategic directions for global eHealth development and stimulating other required changes, including allocation of resources. The absence of strategic orientations and the insufficient definition of priority areas within eHealth initiatives have often resulted in the scattered, aimless and erratic development of eHealth solutions in both national environments and at the global level.23,24 In such a fuzzy environment, it is very difficult to create stable research and methodological foundations that could enable the identification and delineation of the failures and fallacies that have appeared in eHealth initiatives since their inception. Certain failures and fallacies of eHealth initiatives can thus be attributed to the perfunctory research attempts and flawed methodological approaches used to research this phenomenon over the past two decades.
Inconvenient findings
While eHealth initiatives undeniably offer various and palpable benefits to all stakeholders, it is essential to acknowledge the missed opportunities and contexts where these initiatives could be further improved. Here are some failures and fallacies that have emerged and, to a certain extent, characterized the development and progress of eHealth initiatives thus far:
Technological solutionism: One of the prominent fallacies surrounding ICTs and eHealth initiatives is the belief that technology alone can address complex social problems, including public health issues and healthcare system challenges.25–27 While ICTs offer tremendous potential in healthcare, their successful implementation and usage depend on various factors beyond the technology itself, such as the human, organizational and contextual aspects of healthcare delivery. The sociocultural context, regulatory frameworks, healthcare workforce engagement and user acceptance are critical elements that must be considered.28,29 Resistance to change and limited user adoption have emerged as some of the most significant barriers in healthcare digitalization initiatives. Healthcare professionals, who play a vital role in the delivery of care, may encounter challenges in embracing and fully utilizing digital tools. 30 Factors such as disruption to established workflows and procedures or skepticism regarding the effectiveness of ICTs can hinder their adoption. Some eHealth solutions are developed as standalone solutions that operate independently of existing clinical information systems at healthcare providers. This limited integration can lead to data silos, the duplication of efforts and the fragmentation of care. 31 eHealth solutions may not always prioritize a user-centric design, leading to systems that are difficult to navigate, lack user-friendly interfaces or do not meet the specific needs of healthcare professionals and patients. A lack of user involvement in the design process can hinder the adoption and limit the effectiveness of eHealth solutions. 32 Experience shows that the full potential of eHealth solutions can only be realized when they are user-centric and seamlessly integrated with the broader healthcare ICT infrastructure at healthcare providers.
Similarly, patients may face barriers in accepting and using digital health solutions, including information asymmetry, long-standing habits and discomfort with digital interfaces. Overcoming these resistance barriers and ensuring widespread user adoption are pivotal to successful digitalization efforts. 33 Neglecting these factors can lead to the failure of eHealth initiatives, as technology alone cannot overcome systemic barriers and deficiencies or address deeply rooted social and healthcare issues.
Interoperability, ICT infrastructure and resources: Interoperability, that is, the seamless exchange of information between different systems and platforms, has been a persistent challenge. Many healthcare organizations and systems operate with disparate electronic health records and technologies that do not effectively communicate with one another, thus impeding the flow of vital patient information. 34 The customized implementation of digital solutions, non-compliance with data standards and technical barriers often prevent the efficient sharing of patient data, thereby hindering care coordination and compromising the continuity of care across healthcare settings. Lack of interoperability and standardization may ultimately result in inaccurate and incomplete data, which can induce erroneous judgments, leading to adverse healthcare treatment procedures, longer delays in the implementation of healthcare services and various inefficiencies on the part of both individual healthcare providers and the decision-makers at the level of healthcare policy. 35 Inadequate ICT infrastructure and resource allocation pose further obstacles to the digitalization of healthcare. Many healthcare systems, particularly those in resource-constrained settings, face challenges in developing the necessary technological infrastructure, such as reliable internet connectivity, hardware and software systems, network equipment and security products. Understandably, eHealth initiatives heavily rely on technology infrastructure, software and connectivity. However, technical failures, system outages or cyber-attacks can disrupt healthcare services and compromise patient care, especially in underserved healthcare environments. 36 Overdependence on technology without adequate backup plans or alternative solutions can leave patients and healthcare providers vulnerable. Additionally, limited investments and resource allocation for digitalization initiatives can impede progress, leaving healthcare organizations without adequate human resources and ill-equipped to leverage the full potential of digital solutions.
Universal access and healthcare disparities: Assuming universal access to technology and digital infrastructure is a common fallacy associated with eHealth initiatives. While internet penetration rates have increased globally, significant disparities persist, particularly in low-resource settings and marginalized populations.37,38 Overlooking the digital divide can exclude vulnerable communities from reaping the benefits of eHealth initiatives, further exacerbating existing healthcare and socioeconomic disparities. While technology has the potential to bridge gaps and improve healthcare access, it can also inadvertently widen disparities if not implemented thoughtfully. 39 The increased use of eHealth solutions, such as telemedicine, may lead to a more impersonal healthcare experience. The absence of face-to-face interaction with healthcare providers can result in a reduced sense of empathy and understanding, potentially affecting the quality of patient care, and consequently access to healthcare services. 40 Socioeconomic, cultural and infrastructural factors can influence the reach and effectiveness of eHealth interventions. It is essential to consider these points and elements during project planning, tailoring interventions to address specific needs and ensuring that marginalized communities are not left behind. Ensuring equitable access to technology and addressing infrastructural challenges should be prioritized to avoid perpetuating inequities in healthcare delivery. Healthcare systems must acknowledge the diverse needs, beliefs and social, cultural and economic determinants that influence the acceptance and adoption of digital healthcare solutions.
Digital literacy and user training: The fallacy of assuming widespread digital literacy and user readiness poses a significant challenge to eHealth initiatives. It is crucial to recognize that individuals (patients and healthcare professionals) may vary in their digital skills and level of comfort in using technology for healthcare purposes. 41 eHealth solutions can introduce additional administrative tasks and documentation requirements for healthcare providers. The increased workload and challenges associated with learning and adapting to new technologies may contribute to burnout and decreased job satisfaction among healthcare professionals. 42 Neglecting the importance of user training and support can result in low adoption rates, limited engagement and suboptimal outcomes. Investing in digital literacy programs and providing comprehensive user training are essential to empowering individuals to effectively utilize eHealth tools and derive maximum benefit. 43 Moreover, a long-term perspective demands a user-centered design and training curriculums and courses that consider the needs and capabilities of diverse populations. This includes providing education and support to healthcare professionals and patients to ensure that they can effectively and confidently utilize digital tools. 44 Infrastructure investment and resource allocation must be prioritized to bridge the digital divide and enable equitable access to digital healthcare solutions for all populations.
Data privacy and security: Ensuring robust data privacy and security measures is another critical failure often overlooked in eHealth initiatives. With the collection and storage of sensitive healthcare data, concerns about privacy breaches, unauthorized access and potential misuse become paramount. 45 Neglecting to promote the value and implications of healthcare data and omitting to implement appropriate safeguards can erode public trust in eHealth initiatives and hinder the willingness of individuals to share their health information. Incorporating privacy-by-design principles, robust encryption and adherence to established data protection regulations are vital to maintaining data security and preserving patient confidentiality. 46 Regulatory frameworks worldwide are often not adequately adapted to rapid changes and novel business paradigms introduced by digital solutions, so important questions regarding the protection of personal data often arise. 47 In view of this, maintaining effective privacy and security frameworks to protect patient data remain a critical challenge that requires ongoing attention and investment. However, striking a balance between utilizing data for individual and public health benefits and safeguarding data privacy and security principles will remain a complex challenge in the future.
The processing of personal data within eHealth solutions should be precisely defined within an appropriate regulatory framework. Relevant data protection acts at the national level and the General Data Protection Regulation (GDPR) must provide detailed specifications regarding the purpose and scope of data processing, data types, retention periods, lawful controllers, eligible users, data sources and interlinking between various databases. 48 In compliance with legal provisions, comprehensive organizational, logical and technical measures should be in place to prevent unauthorized processing of personal data, aligning with the requirements in Article 32 of the GDPR.
The institution processing personal health data should take steps to inform individuals about data collection purposes and related data protection rights under the GDPR. Regular audits, including a data protection impact assessment (DPIA) for the eHealth information system, should be conducted to enhance data protection. The DPIA aims to ensure GDPR compliance, identify risks to data protection and security and define measures to mitigate these risks, especially given the extensive processing of personal health-related data in large national eHealth databases. The GDPR's direct applicability in all Member States contributes to a harmonized EU-wide data protection framework, fostering mutual trust. Addressing healthcare data issues necessitates a multi-faceted approach, combining technological solutions, regulatory compliance and a commitment to ethical data practices. By doing so, healthcare organizations can harness the benefits of data, while safeguarding patient privacy and trust.
Among the areas where eHealth initiatives have failed to meet expectations, or were characterized by failures and fallacies, it is probably possible to list additional technological, organizational, user, educational, legal and other aspects. However, in this article, the author wanted to focus mainly on the most critical areas, which also have the greatest impact on patient benefits and the further development of eHealth initiatives.
Analyzing both successful and unsuccessful eHealth initiatives can provide valuable insights for future implementations. Identifying the key factors that have contributed to the outcome of eHealth initiatives, such as stakeholder engagement, robust evaluation frameworks, adaptive project management and scalability, can inform best practices, improve future implementations and help avoid the repetition of past mistakes. 49 Policymakers, healthcare professionals, technology experts, patients and other relevant professionals and representatives with expertise and experience in large national ICT projects engage in multidisciplinary collaboration and consultations on a daily basis. However, the mechanisms of their collaboration are not adequately defined, the project activities are not effectively planned and their collaborative actions are not institutionalized and supported by all the necessary resources and procedures. Such poorly managed, organized and system-supported groups can hardly formulate useful guidelines and provide informed decisions about the necessary steps for the successful implementation of eHealth initiatives. This collaboration must be based on knowledge exchange and the sharing of effective strategies from different fields, taking into account the inherent particularities of eHealth initiatives, the outlined factors and national specificities. Sharing lessons learned from different contexts and disseminating knowledge can foster a culture of evidence-based implementation and the continuous improvement of eHealth initiatives.
The article provides a comprehensive systematization of existing knowledge and experience concerning the shortcomings of current development approaches and the limited impacts of eHealth initiatives. In this sense, the article represents one of the few contributions in this field, if any in the recent period. Namely, research into the root causes of the limited success of eHealth initiatives to date is often fragmented, concentrating on individual narrow aspects or only a few listed factors in the best case. This approach hampers a broader and deeper understanding of the issue and impedes progress in overcoming existing obstacles and accelerating the implementation and utilization of eHealth solutions.
Certain positions expressed in the article may be considered personally biased and could raise thought-provoking questions, potentially making the research findings arguable. These points should be thoroughly addressed in further research aimed at conducting a comprehensive analysis of eHealth initiatives, focusing on their developmental aspects and untapped potentials. However, it is worth noting that many international organizations and academics offer similar findings and opinions in their research on eHealth.50–57 These cited sources discuss one or more factors, which have been highlighted in the article as critical for the successful development and effective utilization of digital health solutions in the future.
Conclusions
The article aims to consolidate and categorize the failures and fallacies of eHealth initiatives in one place, shedding light on their background and implications, which are topics that are not frequently discussed. The identification of these failures and fallacies relies, on one hand, on a literature review, incorporating findings from other researchers. On the other hand, it is grounded in the author's expertise and experience that have accumulated in the field of eHealth over the last 20 years. The author advocates for a more comprehensive and evidence-based approach to planning and implementing eHealth initiatives, positing that this would enhance the quality of solutions, increase their utilization and provide better added value for all stakeholders. Despite the apparent shift away from a technology-centered perspective in some research and documents over the last years, the article observes that political and public perceptions often remain entrenched in outdated patterns, treating all eHealth initiatives as exclusively technical projects. Such an interpretation obscures real problems and demonstrates a narrow technical view of extensive sociotechnical projects such as eHealth, which greatly reduces the chances of their ultimate success.
The failures and fallacies encountered in healthcare digitalization initiatives serve as important reminders of the challenges faced in the quest to improve healthcare systems and public health. While significant progress has been made in leveraging ICTs to transform healthcare, critical hurdles still exist that require our attention and collective wisdom. In our efforts to pave the way for successful and instantaneous digital transformation, it is quite obvious that we have overlooked many important factors and aspects, which to a large extent inhibit faster progress in this area and evidently require more comprehensive, thoughtful and gradual approaches to the digitalization of healthcare.
In conclusion, the identified failures and fallacies do not, in any way, represent a discouraging act or a call for the termination of development activities in the field of eHealth. On the contrary, they underscore the need for a new perspective that will improve the chances of success for all existing and upcoming eHealth initiatives. By critically examining the progress in this field, considering the lessons learned and related challenges and explicitly addressing the outlined failures and fallacies, we can navigate the complexities of healthcare digitalization more effectively and adopt a more realistic and evidence-based approach to their planning and implementation. Through consideration of sociocultural context, education and training, expert collaboration, stakeholder engagement, regulatory frameworks and a commitment to ethical and inclusive principles, we can achieve a digitally transformed healthcare landscape that delivers improved outcomes, more equitable access and patient-centered care on a global scale. Our collective wisdom and determination are essential to ensuring the success of healthcare digitalization initiatives and creating a future where technology serves as a catalyst for positive change in healthcare worldwide.
Footnotes
Acknowledgements
The author would like to thank the colleagues at the National Institute of Public Health of the Republic of Slovenia for their help and support.
Contributorship
DS initially reviewed the literature and conceptualized the study. DS conclusively drafted, wrote and edited the final version of the article.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
According to the guidelines of the National Institute of Public Health's Commission on Deontological and Ethical Issues, this article is exempt from ethics approval since it contains information freely available in the public domain. Patient consent was not required, as the conducted research did not involve human or animal subjects.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Guarantor
DS.
