Abstract
Case series summary
This study describes three cases of feline Mycobacterium bovis infection diagnosed in Buenos Aires, Argentina. Cats presented with variable clinical signs, including lymphadenopathy, respiratory distress, and granulomatous retinopathy. Diagnosis was confirmed by cytology, culture, PCR and spoligotyping, identifying two distinct patterns (SB0140 and SB1780). All cats received a combination therapy of rifampicin, clarithromycin and doxycycline, achieving full recovery in two cases and treatment failure in one. The consistent diagnostic protocol allowed molecular epidemiological characterization. A raw meat diet was identified as a potential source of infection in one case.
Relevance and novel information
This report provides a comprehensive clinical, molecular and therapeutic description of feline M bovis infection, emphasizing its zoonotic relevance and the need for One Health collaboration.
Plain language summary
Tuberculosis is an infectious disease that can affect both animals and people. In cats, it is uncommon but can cause serious illness and may pose a risk to public health. This article describes three pet cats from Buenos Aires, Argentina, who were diagnosed with tuberculosis caused by Mycobacterium bovis, a bacterium commonly associated with cattle. The cats showed different clinical signs, including swollen lymph nodes, breathing difficulties, eye lesions and general illness. A combination of laboratory tests, including microscopic examination, bacterial culture and molecular techniques, was used to confirm the diagnosis and to identify the type of bacteria involved. Two different bacterial patterns were found, which helps improve understanding of how this disease circulates in the region. All cats were treated with a combination of three antibiotics commonly used to manage mycobacterial infections. Two of the cats responded well to treatment and fully recovered, while one did not survive despite therapy. In one case, feeding raw meat was identified as a possible source of infection. These cases highlight the importance of considering tuberculosis as a possible diagnosis in sick cats, especially in areas where M bovis is present. The findings also emphasize the need for cooperation between veterinarians and public health professionals to reduce the risk of transmission between animals and humans.
Introduction
Tuberculosis caused by Mycobacterium bovis remains a global concern. Domestic cats are susceptible to infection and may develop variable clinical manifestations. 1 Most feline cases have been reported in the UK,2 –4 but infections have also been documented in other parts of Europe,5 –7 New Zealand, 8 Argentina9 –11 and the USA. 12
The aim of this work was to describe the clinical presentation, diagnosis and treatment of three cats with M bovis infection at a veterinary referral center in Buenos Aires, Argentina.
Case series description
Case 1
A 1-year-old, neutered female domestic shorthair cat was rescued from the outskirts of Buenos Aires, Argentina, at 2 months of age. The cat was up to date with vaccinations according to World Small Animal Veterinary Association (WSAVA) recommendations, 13 was fed a commercial balanced diet (kibble) and lived strictly indoors. At 8 months of age, during elective ovariohysterectomy, an enlarged and firm left inguinal lymph node was detected. A biopsy sample was collected for histopathology, which revealed lymphadenitis with acid-fast bacilli (AFB) using Ziehl–Neelsen (ZN) staining. Samples were submitted for mycobacterial culture and molecular typing.
Additional diagnostic tests included abdominal ultrasonography, which was unremarkable, and thoracic radiographs showing increased pulmonary radiodensity with a diffuse, non-structured interstitial to peribronchial pattern, more pronounced in the left caudal lung lobe, with mild alveolar involvement (Figure 1). However, no abnormalities were identified on physical examination at the time of consultation after the biopsy.

Right lateral thoracic radiographic views. (a) At diagnosis: generalized increase in pulmonary radiodensity due to an unstructured interstitial pattern; increased radiodensity over the cranial mediastinal region, without abnormalities observed in other projections, likely corresponding to fat deposits. (b) After treatment: overall improvement in pulmonary aeration; mild persistence of increased bronchial markings
Case 2
A 1-year-old, neutered male domestic shorthair cat was rescued from the streets in the outskirts of Buenos Aires, Argentina, at 3 months of age. The cat was up to date with vaccinations according to WSAVA recommendations, 13 was fed a commercial balanced diet and lived strictly indoors. The patient was presented with a 1-month clinical history of intermittent hemorrhagic diarrhea, lymphadenopathy of the inguinal and prescapular lymph nodes, fever and lethargy (Figure 2). Cytologic examination of a fine-needle aspirate from the right inguinal lymph node revealed AFB with ZN staining. Samples were collected for mycobacterial culture and molecular typing. Abdominal ultrasonography revealed enlarged jejunal and iliac lymph nodes with irregular borders and a mildly heterogeneous hypoechoic pattern, suggestive of infiltrative adenopathy

Edema of both hindlimbs was observed, likely secondary to the marked inguinal and abdominal lymphadenopathies
Case 3
A 2-year-old, neutered male domestic shorthair cat was adopted at 45 days of age from the outskirts of São Paulo, Brazil, and, since 3 months of age, had lived in Buenos Aires, Argentina. The cat had an exclusively indoor lifestyle, cohabited with another cat and a dog, and had been fed a commercial raw diet for most of his life; for the last 6 months, his diet had been switched to kibble. The patient was presented to the veterinary hospital with marked dyspnea, fever and progressive anorexia. Thoracic imaging revealed a severe, diffuse interstitial–peribronchial pattern with multifocal nodular changes (Figure 3). The patient was admitted to the intensive care unit for oxygen therapy and intravenous hydration, received metamizole as an antipyretic and low-dose dexamethasone (0.3 mg/kg IV), and was stabilized within 24 h to undergo bronchoalveolar lavage (BAL). Cytologic examination revealed AFB using ZN staining (Figure 4). Samples obtained from the BAL were submitted for mycobacterial culture and molecular typing.

Right lateral thoracic radiographic views. (a) At diagnosis: generalized increase in pulmonary radiodensity due to a mixed interstitial pattern, predominantly micronodular, interspersed with areas of a more unstructured appearance. (b) After treatment: overall improvement in pulmonary aeration; persistence of an interstitial–bronchial pattern with suspected evidence of bronchiectasis, consistent with chronic degenerative changes
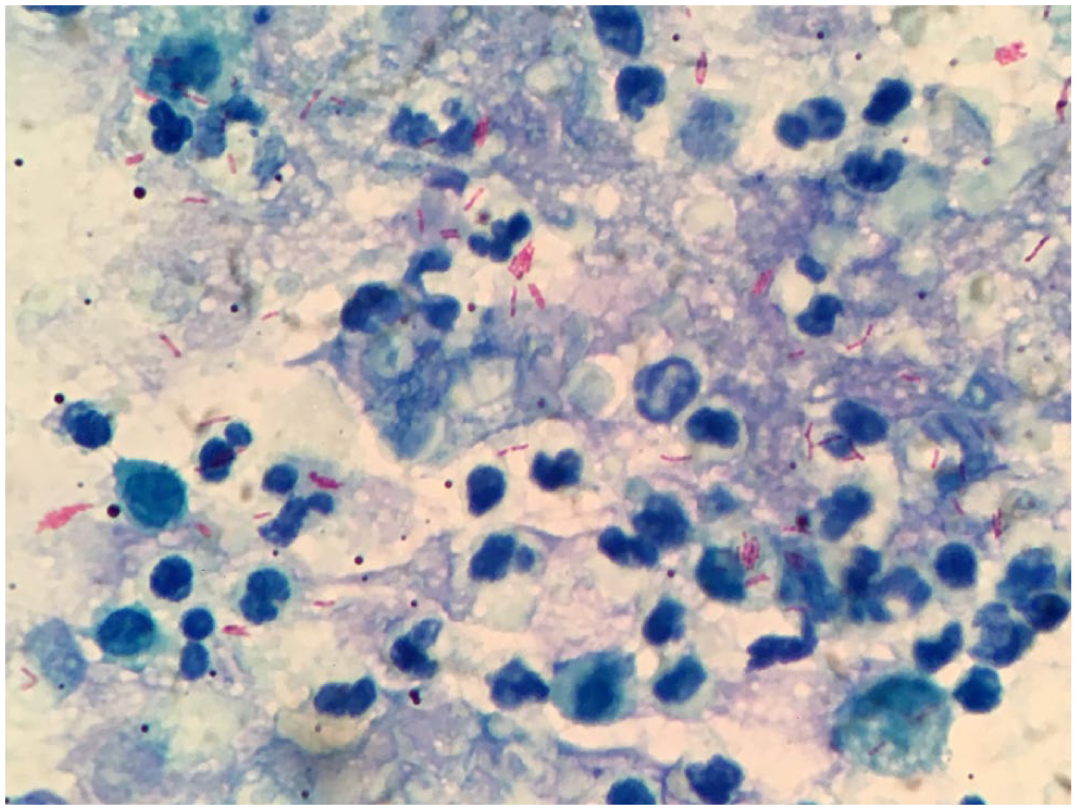
Cytologic smears were well preserved and contained abundant material composed predominantly of numerous neutrophils, a moderate number of macrophages and occasional erythrocytes. The macrophages exhibited abundant, strongly basophilic and finely granular cytoplasm, with oval nuclei showing loose chromatin and inconspicuous nucleoli. Surrounding these cells, an amorphous, pink, reticular material compatible with proteinaceous substance was observed. Ziehl–Neelsen staining revealed numerous strongly stained, acid-fast bacilli, both free among the inflammatory cells and within the cytoplasm of macrophages (600 ×)
In addition, the cohabiting animals (one dog and one cat) were examined through hematology, abdominal ultrasonography and thoracic radiography, with no pathologic findings detected at that time.
Laboratory findings
Hematologic and biochemical parameters are summarized in Table 1. Case 2 showed marked leukocytosis (52.2 × 109/l), characterized by severe neutrophilia with a left shift, monocytosis and mild non-regenerative anemia. In contrast, cases 1 and 3 had hematologic values within or close to reference intervals.
Hematological and biochemical parameters for each cat at the time of diagnosis

A:G = albumin:globulin; ALP = alkaline phosphatase; ALT = alanine aminotransferase; RI = reference interval; WBC = white blood cell
Biochemical abnormalities included mild to moderate increases in alanine aminotransferase (ALT) activity in all cats, hypoalbuminemia in case 2 and hyperglobulinemia with a decreased albumin:globulin ratio in case 3.
All cats tested negative for feline leukemia virus (FeLV) and feline immunodeficiency virus (FIV) using a SNAP Duo FIV/FeLV test (Virbac Laboratories).
Diagnosis of M bovis
Diagnosis of M bovis was achieved through bacteriological culture and molecular identification, followed by genotyping using the spoligotyping technique. Samples were first decontaminated using Petroff’s method and then cultured in duplicate in Stonebrink medium and in Löwenstein–Jensen medium. 14 Cultures were kept up to 3 months with weekly observation; when colonies were observed, ZN staining was performed. Positive ZN colonies were put in sterile water (300 µl) and thermal lysis was performed in a dry block heater (95°C for 40 mins). Samples were centrifuged (12,000 rpm; ~13,400 × g) for 10 mins, and the supernatant was used for further molecular analyses. For molecular confirmation of isolates from the M tuberculosis complex, IS6110-PCR was performed using the primers (INS1 and INS2) and the cycling from Hermans et al 15 (Table 2). IS6110-positive isolates were genotyped by spoligotyping according to the method described by Kamerbeek et al. 16 The resulting patterns were identified by comparison with the international database www.mbovis.org (VISAVET Health Surveillance Centre of Universidad Complutense). The prior occurrence of these spoligotypes in Argentina was assessed by comparison with the IABIMO-INTA-CONICET database.
Primers used in IS6110-PCR

Treatment
All three cats received a combined therapy consisting of rifampicin (10 mg/kg PO q24h), clarithromycin (10 mg/kg PO q12h) and doxycycline (10 mg/kg PO q24h). Despite the absence of initial clinical signs in case 1, treatment was instituted after diagnostic confirmation and the presence of thoracic radiographic abnormalities. In this cat, rifampicin was discontinued after 45 days because of the development of erythematous and pruritic cutaneous lesions, which resolved completely after withdrawal; treatment was continued with clarithromycin and doxycycline. Cases 2 and 3 showed initial clinical improvement within the first 48 h. Supportive care, including oxygen therapy or anti-inflammatory treatment, was provided when indicated.
Clinical outcome and follow-up
Case 1 achieved complete radiographic resolution after 4 months, and therapy was maintained for an additional 60 days. 17 Two months after starting therapy, the owners reported partial vision loss. Ophthalmologic assessment revealed bilateral anisocoria secondary to granulomatous retinopathy, which resolved by continuing the tuberculosis and topical treatment (Figure 5). Case 2 showed initial clinical improvement but relapsed after 3 months, presenting with fever, anorexia and progressive lymphadenopathy; as a result of clinical deterioration and lack of response, euthanasia was elected. Case 3 exhibited full clinical recovery after 30 days and complete radiologic resolution after month 5; treatment was continued for 60 days beyond radiographic cure.
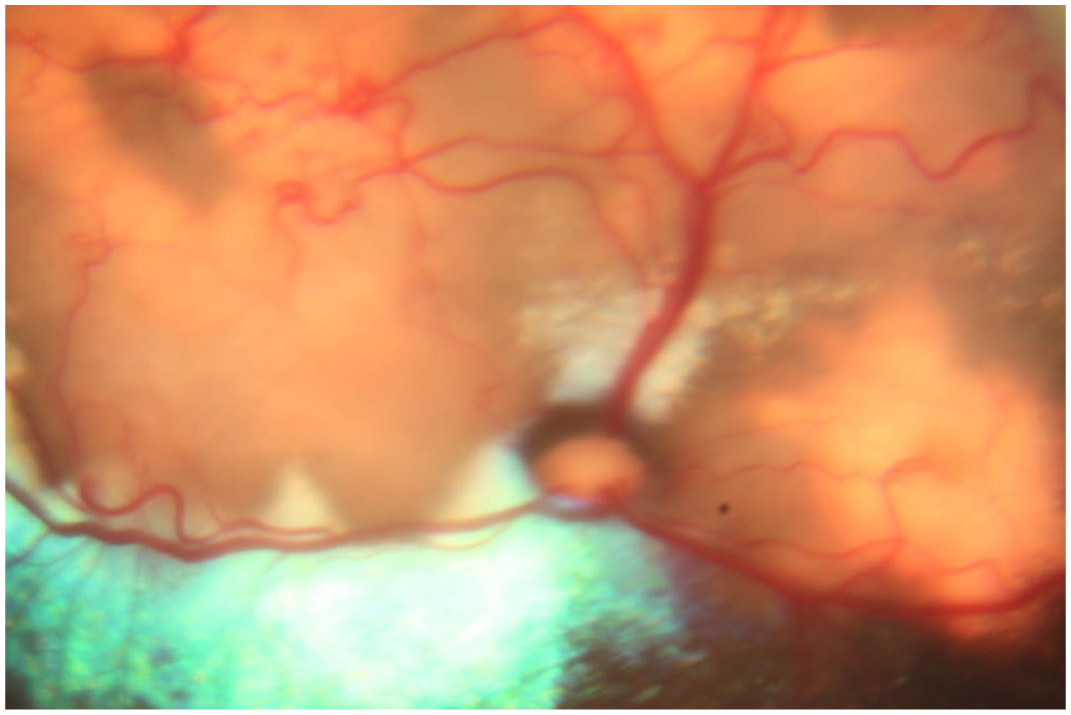
Funduscopic image showing granulomatous lesions in the tapetal area with associated retinal detachment and marked neovascularization
After-treatment evaluations at 3, 6 and 12 months, including clinical examinations, laboratory testing, thoracic radiography and/or abdominal ultrasound, confirmed sustained remission in the surviving cats.
Discussion
This study provides a comprehensive description of feline tuberculosis in Buenos Aires, Argentina, integrating clinical, molecular, therapeutic and follow-up characterization. Although feline M bovis infection has been previously reported in Argentina, most earlier cases involved stray or semi-domiciled cats, often originating from feline colonies, with limited clinical evaluation and no standardized therapeutic follow-up.
All cats had lived strictly indoors since adoption. In this case, molecular epidemiology contributed to understanding the possible routes of infection. Spoligotyping is a molecular technique that enables differentiation within and between species of the M tuberculosis complex. 16 It is based on the detection of the presence of spacers in the Direct Repeat (DR) region. This is very useful when trying to determine outbreak origins and possible transmission. For cases 1 and 2, the infection was most likely acquired before adoption, while the cats were still outdoors. This assumption is supported by published evidence of cat-to-cat transmission3,18,19 in shared environments and by the identification of spoligotype SB0140, which has already been reported in feline cases from Argentina 11 and is the most frequently identified spoligotype in cattle and wildlife.9,11 However, other potential routes of transmission cannot be excluded, including hunting and/or the ingestion of raw meat before adoption. 1 Spoligotype SB1780 was identified in case 3 and was previously detected in bovine populations (personal communication, Dr Zumárraga, IABIMO-INTA-CONICET). Given that M bovis is endemic in Argentine cattle, despite the existence of a national eradication program (SENASA, Resolution 128/12), and considering that raw diets in Argentina are primarily based on bovine meat, dietary exposure cannot be excluded.
Interestingly, the median age of the affected cats in this series was 1.3 years, which is lower than that reported in previous studies, where the median age was approximately 3 years.1,2 This finding may suggest early exposure or a higher susceptibility of younger animals under certain epidemiologic conditions.
Regarding the clinical signs, two cases exhibited fever and progressive weight loss. The occurrence of hyperthermia associated with superficial and/or deep lymphadenopathy should raise suspicion of feline tuberculosis in endemic areas. Unlike other studies, where the presence of cutaneous nodules is commonly reported,1,19 such lesions were not observed in the cats described here. Case 1 was characterized by pneumonia associated with granulomatous retinopathy, illustrating the variable clinical manifestations that M bovis infection can produce, even within the same individual. In some cases, leukocytosis with marked neutrophilia and hyperproteinemia were observed; 1 although expected in feline tuberculosis, these findings are not pathognomonic.
Diagnosis was performed using the same methodology in all cases: ZN staining, bacteriological culture PCR and genotyping. This approach enabled the identification of different spoligotypes, providing valuable information from a molecular epidemiology perspective.
The therapeutic management of feline tuberculosis remains challenging because of limited drug availability, variable host immune response and the requirement for long-term caregiver commitment. The antibiotic protocol implemented included rifampicin, clarithromycin and doxycycline. The treatment was based on a triple therapy regimen, as previously reported in other studies.1,17 The combined use of rifampicin and clarithromycin constitutes the first-line therapy for feline tuberculosis; however, doxycycline is not part of the standard treatment. Doxycycline was included owing to the unavailability of pradofloxacin in Argentina and considering its reported immunomodulatory benefits in human tuberculosis, 20 together with its documented use in the management of other mycobacterial infections.1,17 In case 1, the patient was able to receive rifampicin for only 45 days because of the development of an adverse reaction. Nevertheless, maintenance therapy with clarithromycin plus doxycycline, along with specific treatment for retinopathy, resulted in sustained clinical remission. To ensure complete recovery, clinical, laboratory and radiologic evaluations were performed throughout the course of treatment. Once both clinical and radiologic resolution were achieved, therapy was continued for an additional 60 days to consolidate recovery. In case 2, despite receiving the same therapeutic regimen and sharing the same spoligotype as case 1, no favorable clinical response was observed. This finding reinforces that clinical outcome depends not only on antimicrobial therapy but also on the host’s specific immune response.17,21
Because tuberculosis in companion animals is a notifiable disease in Argentina and there is a low risk of M bovis transmission from cats to humans,7,11,22 all owners underwent latent tuberculosis screening, with negative results. Considering the prolonged antimicrobial treatment and the use of drugs also indicated for human tuberculosis, written informed consent was obtained before initiating treatment.
Conclusions
This report describes feline M bovis infection in Argentina, providing clinical, molecular and therapeutic characterization of three cases. The identification of two spoligotypes contributes to the understanding of feline tuberculosis epidemiology, while the adapted triple antimicrobial regimen showed potential efficacy, highlighting both therapeutic challenges and zoonotic implications.
Footnotes
Acknowledgements
Thanks to Francisco Zapata (Dimerolab), Roxana Paul (INEI – ANLIS ‘Dr Carlos G Malbran’), Gustavo Martinez (Instituto de Zoonosis Luis Pasteur), Florencia Pastorino (Zoonosis Urbanas – Buenos Aires), Martin José Zumarraga (IABIMO-INTA-CONICET) and Agustina Covini (ICU Unit, Wellvet Veterinary Clinic).
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognized high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS Open Reports. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers, tissues and samples) for all procedure(s) undertaken (prospective or retrospective studies). For any animals or people individually identifiable within this publication, informed consent (verbal or written) for their use in the publication was obtained from the people involved.
