Abstract
Case summary
A 16-year-old male castrated domestic shorthair cat was referred for investigation of a 2-week history of lethargy, hyporexia, and intermittent diarrhoea and constipation. CT revealed a colo-colonic intussusception associated with a fat attenuating non-contrast enhancing mass measuring 4.5 × 2.6 cm, arising from the ventral aspect of the intussuscipiens, causing partial obstruction. Surgical intervention involved manual reduction of the intussusception, colectomy with 3 cm margins and end-to-end anastomosis. Histopathological examination identified the mass as a lipoma, composed of well-differentiated adipocytes originating within and expanding into the submucosa of the intestine, with an ulcerated and necrotic luminal surface. The cat was discharged 3 days postoperatively and had fully recovered at the 10-day follow-up. At 9 months postoperatively, the patient continued to do well with no recurrence of clinical signs.
Relevance and novel information
To the best of our knowledge, this is the first reported case of a colonic lipoma and the first reported case of a colonic submucosal lipoma leading to intussusception in a cat. This case highlights the importance of considering colonic lipomas as a differential diagnosis in feline patients presenting with constipation, diarrhoea or an acute abdomen.
Plain Language Summary
A 16-year-old castrated male domestic shorthair cat was referred for further investigation after 2 weeks of low energy, reduced appetite, and occasional diarrhoea and constipation. A CT scan showed that part of the large intestine had telescoped into another section of the colon, a condition called a colo-colonic intussusception. This was caused by a 4.5 × 2.6 cm fatty mass (a lipoma) inside the bowel wall, which was partially blocking the intestine. The cat underwent surgery to gently pull the intestine back into its normal position. The affected part of the colon was then removed with a small margin of healthy tissue and the two ends were rejoined. Laboratory analysis confirmed that the mass was a lipoma, a benign (non-cancerous) fatty growth. It had developed within the inner layer of the bowel wall and expanded into the surrounding tissue. The surface of the mass was ulcerated and contained some dead tissue, likely due to friction or pressure inside the intestine. The cat recovered well after surgery and was discharged from the hospital 3 days later. At a checkup 10 days after the procedure, he had fully recovered. At a 9-month follow-up, he continued to do well, with no signs of the problem returning.
Introduction
Lipomas are benign, non-epithelial, adipose tumours commonly seen in dogs, typically arising from subcutaneous tissues; however, they are rare in cats and even more unusual when associated with gastrointestinal structures. 1 In human medicine, lipomas of the large intestine are the third most frequently occurring benign tumour, after hyperplastic and adenomatous polyps. 2 They are usually asymptomatic and often diagnosed incidentally, although intussusception has been reported. 3 In humans, clinical symptoms may occur when lesions exceed 2 cm, and giant lipomas (>4 cm) are more likely to be symptomatic.4,5 Little information is available in the veterinary literature regarding feline gastrointestinal lipomas. To the best of our knowledge, this is the first report of a colonic lipoma resulting in an intussusception in a cat.
Case description
A 16-year-old, 4.6 kg, male castrated domestic shorthair cat was referred for evaluation of a 2-week history of lethargy, hyporexia, and intermittent episodes of small intestinal diarrhoea alternating with constipation and occasional dyschezia. The cat had lost 0.5 kg over the preceding 3 months. Before referral, empirical treatment had been initiated with a gastrointestinal diet, maropitant and a probiotic supplement (Fortiflora; Purina), without clinical improvement.
Physical examination revealed a non-painful mass in the caudal abdomen, and the cat had a body condition score of 4/9. The remainder of the examination was unremarkable. Haematology and biochemistry profiles, including serum cobalamin and total thyroxine concentrations, were performed, revealing marked leukocytosis with lymphocytosis, monocytosis and granulocytosis (Table 1).
Summary of laboratory results
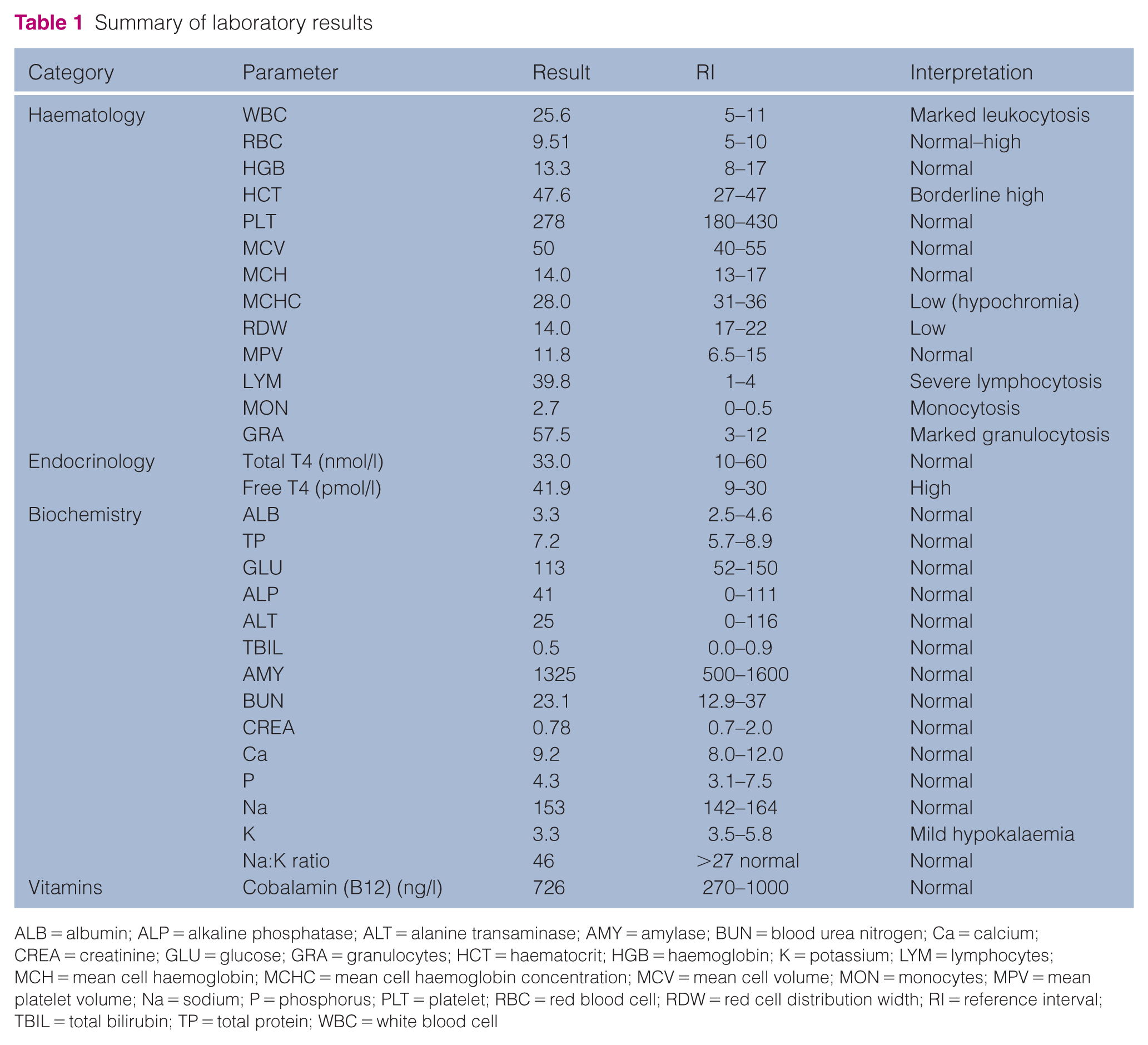
ALB = albumin; ALP = alkaline phosphatase; ALT = alanine transaminase; AMY = amylase; BUN = blood urea nitrogen; Ca = calcium; CREA = creatinine; GLU = glucose; GRA = granulocytes; HCT = haematocrit; HGB = haemoglobin; K = potassium; LYM = lymphocytes; MCH = mean cell haemoglobin; MCHC = mean cell haemoglobin concentration; MCV = mean cell volume; MON = monocytes; MPV = mean platelet volume; Na = sodium; P = phosphorus; PLT = platelet; RBC = red blood cell; RDW = red cell distribution width; RI = reference interval; TBIL = total bilirubin; TP = total protein; WBC = white blood cell
Abdominal ultrasound revealed a well-demarcated, hypoechoic intramural colonic mass acting as a lead point for an intussusception. The affected colonic segment displayed preserved wall layering with concentric rings typical of intussusception. There was no evidence of intestinal obstruction; however, a mild to moderate hyperechoic peritoneal reaction was present, consistent with regional inflammation. Ultrasound images were not saved at the time of the examination and therefore could not be included in this report. The cat was premedicated with medetomidine (2 µg/kg IV) and methadone (0.2 mg/kg IV), anaesthesia was induced with propofol (4 mg/kg IV) and the cat was maintained on inhalant isoflurane. Intravenous contrast-enhanced CT of the thorax and abdomen was performed. Thoracic CT was unremarkable. Abdominal CT revealed a large colonic intussusception of approximately 10 cm in length. Arising from the left ventral aspect of the intussuscipiens, a 4.5 cm × 2.6 cm heterogeneous fat and soft tissue attenuating, non-contrast enhancing mass was identified, resulting in dorsal displacement of the faecal content (Figure 1).

Multiplanar reconstruction CT images showing a heterogeneous fat and soft tissue attenuating, non-contrast enhancing fusiform mass arising from the left ventral aspect of the intussuscipiens (yellow arrowheads), displacing the faecal content dorsally
After routine aseptic preparation, cefazolin (20 mg/kg IV) was administered perioperatively. A ventral midline celiotomy extending from the xiphoid to the pubis was performed. No free fluid was observed within the abdominal cavity. Surgical intervention included reduction of a colo-colonic intussusception. The colonic tissue appeared viable after reduction; however, owing to the presence of an intraluminal mass, a colectomy was performed. Margins of 3 cm of grossly normal colon were resected orad and aborad to the lesion. An end-to-end anastomosis was subsequently performed using 4-0 polydioxanone suture in a simple interrupted pattern (Figure 2). A broad-based intraluminal mass measuring 4.5 × 3 cm was identified within the descending colon, approximately 7 cm aborad to the caecum. The mass caused significant proximal invagination and marked luminal narrowing. An enlarged mesenteric lymph node was identified and biopsied. No other abnormalities were detected upon inspection and digital examination of the remaining intra-abdominal organs within the field of view. The omentum was placed over the anastomosis site, the peritoneal cavity lavaged with warm saline and the abdominal incision closed routinely.
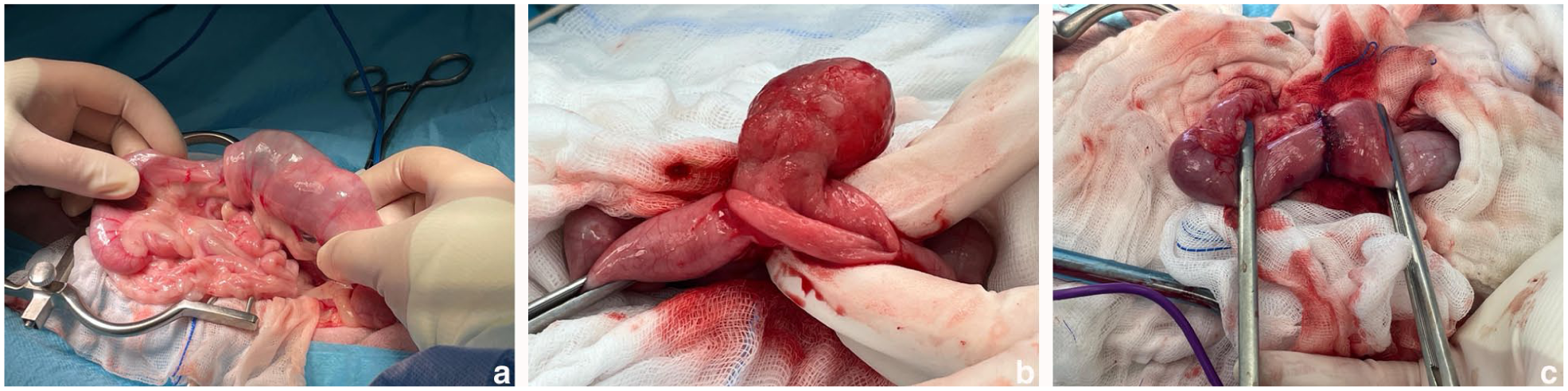
(a) Intussusception, (b) intraluminal lipoma after enterotomy and (c) colonic anastomosis
The cat recovered uneventfully and remained hospitalised for 72 h postoperatively. During this period, maintenance intravenous fluids were administered, and analgesia and antimicrobial therapy were provided with buprenorphine (0.02 mg/kg IV q6h), amoxicillin–clavulanate (20 mg/kg IV q8h) and metronidazole (10 mg/kg IV q12h). Upon discharge, the cat was prescribed oral medications, including amoxicillin–clavulanate (20 mg/kg PO q12h for 7 days), meloxicam (0.1 mg/kg PO q24h for 5 days) and metronidazole (10 mg/kg PO q12h for 7 days).
On histopathology, the mass was diagnosed as a lipoma. The lesion consisted of well-circumscribed submucosal adipose tissue composed of mature adipocytes. The adipocytes were arranged in a lobular pattern with scattered lymphocytes and occasional plasma cells within the surrounding stroma (Figure 3). The mass was surrounded by compressed smooth muscle, and there was a focal area of necrosis and ulceration of the luminal surface, which was covered by granulation tissue and debris. Cranial sections of the colon showed mild mucosal oedema and prominent submucosal lymphoid aggregates. No evidence of malignancy or invasive behaviour was noted, and the surrounding tissue appeared unremarkable. There was no significant inflammatory response outside the immediate area of the mass. The lymph node exhibited moderate reactive lymphoid hyperplasia with a prominent population of parafollicular lymphocytes.

Histological examination of resected mass revealing a well-circumscribed submucosal mass composed of well-differentiated adipocytes with scattered lymphocytes and collagen. The mass was surrounded by compressed smooth muscle, with an ulcerated, necrotic luminal surface covered in debris and granulation tissue. Courtesy of Isobel Gibson, IDEXX Laboratories
A follow-up examination 10 days postoperatively revealed that the cat had a good body condition score, with normal defecation reported by the owners. There was a notable weight gain of 0.5 kg. At 9 months post-operatively, a follow-up telephone call indicated that there had been no recurrence of clinical signs, and the cat had made a full recovery, returning to normal health.
Discussion
Gastrointestinal lipomas are benign adipose tumours of mesenchymal origin. In human medicine, they are relatively rare, accounting for only a small percentage of all gastrointestinal tumours.6,7 Colonic lipomas, first described by Bauer in 1757, are the third most common benign intestinal tumour in humans, after hyperplastic and adenomatous polyps.3,5 Although uncommon in both humans and other animals, these tumours may produce clinical signs when they grow large enough to cause obstruction or other complications.2,6
In humans, gastrointestinal lipomas are histopathologically classified as intramuscular, subserosal or submucosal. 8 Approximately 90% originate from the submucosa, while the remaining 10% arise from the subserosal or intramuscular layers. 9 Surgical resection is generally the treatment of choice for symptomatic patients. In the present case, the cat’s lipoma was classified as submucosal, consistent with most human cases.
In humans, colonic lipomas typically grow slowly, are often asymptomatic and are most commonly discovered incidentally during routine colonoscopy or autopsy.5,10,11 Clinical signs usually arise when the lipoma exceed 2 cm in size. Lipomas greater than 4 cm are classified as ‘giant lipomas’, and approximately 75% of these become symptomatic. 3 Common clinical manifestations of giant colonic lipomas include abdominal pain, diarrhoea, constipation and gastrointestinal bleeding.10,11 In human medicine, colonic lipomas most often present as solitary masses, although multiple lipomas can occur in 6–25% of cases.12,13
Malignant transformation of lipomas is exceedingly rare in humans, with only isolated cases reported, such as those involving intraosseous lipomas. 14 These instances are exceptional, and lipomas are generally considered benign neoplasms with little to no risk of malignant transformation. Surgical resection is typically curative, and recurrence after resection is uncommon.15,16
In feline medicine, the incidence of gastrointestinal lipomas is extremely uncommon. Although fatty infiltration of the gastric mucosa has been described, only a single case of an incidental, asymptomatic gastric submucosal lipoma has been reported. 17 To date, to our knowledge, there have been no published reports of colonic lipomas or symptomatic gastrointestinal lipomas in feline patients.
Colonic lipomas can be detected using various radiological techniques. Large lesions may appear as a fat opacity causing a mass effect, with or without intestinal mechanical obstruction, on plain radiographs. Ultrasound of the abdomen may reveal a hyperechoic lesion without internal vascularity.13,17 CT typically reveals an intraluminal mass with uniformly ovoid-shaped sharp borders and characteristic homogeneous fat attenuation (–40 to –120 Hounsfield units). 13 Finally, CT colonography combined with a barium enema may reveal a cavity-filling defect with well-defined borders. 13
This report highlights the clinical parallels between a giant colonic lipoma in a cat and those observed in human medicine. In humans, giant colonic lipomas (>4 cm) are more likely to cause clinical signs and complications such as intussusception. 5 Similarly, in this case, the cat presented with a 2-week history of lethargy, hyporexia, weight loss, and intermittent episodes of diarrhoea and constipation. CT imaging revealed a colonic mass with intussusception, a finding commonly reported in human patients with giant colonic lipomas. 6
Colonic lipomas may be under-recognised in veter-inary medicine, particularly when they remain asymptomatic. In human medicine, these tumours are often detected incidentally during routine colonoscopy or autopsy-diagnostic opportunities that are less frequently applied to clinically normal animals. Although post-mortem examinations in cats can identify such lesions, it rema-ins possible that smaller or subclinical lipomas are overlooked.
In this case, the duration of growth is uncertain, but the development of clinical signs only 2 weeks before presentation suggests that smaller lipomas may remain asymptomatic in cats, as has also been reported in humans.
This case has some limitations. The use of three different antimicrobials peri- and postoperatively does not reflect current guidelines for colonic surgery. In addition, follow-up was limited to a telephone call, and no postoperative imaging was performed.
Surgical intervention resulted in a favourable long-term outcome. To the authors’ knowledge, this represents the first reported case of a colonic lipoma causing intussusception in a cat. This case demonstrates that gastrointestinal lipomas can occur in cats, may lead to clin-ical signs and that surgical intervention can be curative.
Conclusions
Colo-colonic intussusception should be considered a potential cause of acute abdomen in patients presenting with ileus, diarrhoea or constipation. This case underscores the importance of including colonic lipomas in the differential diagnosis, given their capacity to cause serious complications such as intussusception. Prompt identification and appropriate surgical management are key to achieving favourable clinical outcomes.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognised high standards (‘best practice’) of veterinary clinical patient care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS Open Reports. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers, tissues and samples) for all procedure(s) undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
