Abstract
Background:
The growing emphasis on low-carbon, sustainable health care systems is driving the integration of environmental sustainability into clinical practice and research. This shift necessitates clinician literacy in health care sustainability, particularly in methodologies for assessing environmental impacts.
Objective:
To introduce health care professionals to life cycle assessment (LCA) as a tool for evaluating environmental impacts in clinical contexts and to illustrate its application through a case study on hemodialysis therapies.
Design:
A qualitative assessment of LCA methodology, including its fundamental principles, stages, and applications in health care.
Setting:
Hemodialysis materials were collected from In-Centre and Home Dialysis units at Vancouver General Hospital.
Patients/Sample/Participants:
No patients are directly involved in this work; samples of unused hemodialysis materials were collected for process assessment. The target audience is health care professionals, particularly those involved in kidney care, who need to interpret LCA results for informed decision-making.
Methods:
Overview of LCA, an internationally standardized methodology that evaluates the environmental impacts of products and processes over their entire life cycle, is presented. The 4 stages of LCA, the key environmental impact categories it assesses, and guidelines for appropriate interpretation and use are explored.
Results:
Life cycle assessment provides numerous midpoint data, mechanisms by which damages occur to endpoints, including human health and environments. The case study comparing home versus in-center hemodialysis demonstrates how LCA findings can inform decision-making in kidney care.
Limitations:
The interpretation of LCA results requires an understanding of its methodology and limitations. The accuracy of LCA outcomes depends on the quality and scope of data used in the assessment.
Conclusions:
As LCA is increasingly applied in clinical settings, health care professionals must develop the skills to critically evaluate and apply its findings. This primer equips kidney care professionals with essential knowledge of LCA methodology, supporting the integration of environmental sustainability into clinical practice.
Trial Registration:
Not applicable
Introduction
Climate change, pollution, and biodiversity loss are collectively disrupting both natural and human systems. 1 Between 2030 and 2050, an additional 250 000 deaths annually are expected from malnutrition, malaria, and heat stress, all of which can cause or worsen kidney disease. Declining air quality may also worsen chronic kidney disease (CKD), with air pollution currently associated with more than 3.28 million incident CKD cases annually. 2 More than 80 countries have committed to strengthen climate resilience and/or reduce greenhouse gas (GHG) emissions in health systems, 3 and the United Nations has declared a healthy environment a basic human right. 4
Health services delivery has environmental costs that adversely affect health. Nagai et al demonstrate rising emissions as CKD stage advances, 5 and in one health region in the United Kingdom, GHGs from dialysis were found to be 18 times higher than from general health care. 6
There are increasing calls for, and inclusion of, environmental impact assessment in clinical trials in kidney and wider health care literature.7-9 Life cycle assessment (LCA) is defined by rigorous international standards (ISO 14040 and 14041) and is the gold standard environmental impact assessment methodology, evaluating a broad range of impacts of a product, process, or service throughout its life cycle. The quality of health care LCA publications has been “inadequate,” while lacking standardized approach, reporting, data quality, and interpretation. 10
An overview of LCA methodology, analysis, and interpretation is herein presented, illustrated with a case study in kidney care, to assist clinicians and health care decision makers in the understanding and application of this emerging tool.
Methods
Conducting an LCA in Kidney Care
Life cycle assessment provides detailed environmental impact assessments of individual products or processes, and enables comparisons between functionally equivalent alternatives. Life cycle assessment is conducted in 4 stages (Figure 1). Life cycle assessment design has similarities to clinical outcomes research: the goal is determined (akin to primary and secondary outcomes), the scope or “boundary” is precisely defined (similar to inclusion/exclusion criteria), data are collected, results analyzed, and findings interpreted.

Stages of life cycle assessment.
Numerous software programs are available for sustainability assessments, including SimaPro, GaBi, and OpenLCA. These tools rely on inventory databases such as Ecoinvent, IDEA, USEEIO, Agri-footprint, ELCD, and GaBi Database. However, their lack of medical-specific datasets can pose challenges in accurately assessing the environmental impacts of health care processes.
To illustrate the process of LCA, a case study (using published but non-peer-reviewed data, ongoing analysis in progress) is presented in a series of text boxes 11 (Box 1).

Goal and scope
The LCA’s purpose, intended application and audience, and scope of study are first defined. A system boundary is established in which it is determined which life cycle stages will be considered (Figure 1), and which material and/or energy flows will be included (Figure 2). The most comprehensive assessment, a “cradle-to-grave” analysis, involves capture of material and energy inputs throughout a product’s entire life cycle, from extraction to disposal. Examples of processes for which more targeted assessments may be appropriate include evaluation of the environmental impacts of a pharmaceutical’s production, or impacts of peritoneal dialysis plastics, where, respectively, cradle-to-gate, or gate-to-grave scope could be employed.

A simplified system boundary for conducting an LCA evaluating hemodialysis.
A functional unit is a quantifiable measure of a product’s function, used to standardize inputs and outputs. A well-defined functional unit enables consistent assessment of environmental impacts across different products or processes (eg, hemodialysis [HD], home hemodialysis, and peritoneal dialysis) (Box 2).

Life cycle inventory
Process flow mapping transforms a simplified boundary diagram into a detailed process map, ensuring that all steps in a life cycle stage are comprehensively accounted for. Data are then collected to precisely quantify all inputs (eg, material type, mass, and energy) and outputs (eg, waste, emissions). These are collectively referred to as activity data and can include measured inputs or outputs (preferred), or data gleaned from published literature or manufacturers. Life cycle inventory (LCI) is the most demanding and time-consuming task in an LCA (Box 3).

Life cycle impact assessment
Activity data are inputted into LCA software, which translates LCI results into quantitative environmental impacts. Lifecycle assessment software programs use pre-existing datasets and impact assessment methods to quantify these impacts. At this stage, impacts can be assessed across 2 broad types of indicators: midpoint and endpoint.
Results
Midpoint indicators quantify specific environmental impacts at an intermediate stage, between initial environmental loads (eg, emissions, resource use) and final impacts on endpoints. Endpoints include human and/or ecosystem health and resource depletion, providing an aggregated assessment of overall harm.
Midpoint Indicators
Midpoint indicators can be thought of as the mechanisms by which endpoint damages occur. Each midpoint indicator is a well-established environmental impact known to affect human and ecosystem health. For example, damages to human health can transpire via global warming, ozone depletion, or air pollution, among others. A detailed description of midpoint indicators is presented in Table 1. Selected midpoint results for HD are shown in Figure 3A. Figure 3B is a “hotspot analysis” that highlights the dialysis process (consumables use), patient and staff travel, and supply transport as the highest sources of emissions (Box 4).
Overview of Life Cycle Assessment Midpoint Indicators and Their Description.

Note. kg = kilogram, CO2 = carbon dioxide, eq = equivalent, CFC-11 = chlorofluorocarbon-11, GHG = greenhouse gases, CH4 = methane, CFCs = Chlorofluorocarbons, mol H+ = mole of hydrogen ion, NMVOC = non-methane volatile organic compounds, PO4 = phosphate, N = nitrogen, m³ H2O = cubic meter of water, Sb = antimony, MJ = megajoule, LC50 CTUh = lethal concentration 50, comparative toxicity unit for humans, LC50 CTUe = lethal concentration 50, comparative toxicity unit for ecosystems, PM10 = particulate matter (particles less than 10 micrometers in diameter).

(A) Midpoint analysis showing selected impact categories. (B) Process contributions to total GHG emissions.

Presentation of all midpoint and endpoint categories ensures data transparency and allows discussion of trade-offs, in which one environmental impact may be more immediately relevant to a given region or population than another.
Endpoint Indicators
Endpoint indicators estimate the ultimate impacts of a product or process (Figure 4). These are derived by aggregating midpoint indicators according to their relative contributions to human health, ecosystems, and resource availability. For example, GHGs are converted into disability-adjusted life years using established models that estimate the health impacts of climate change.
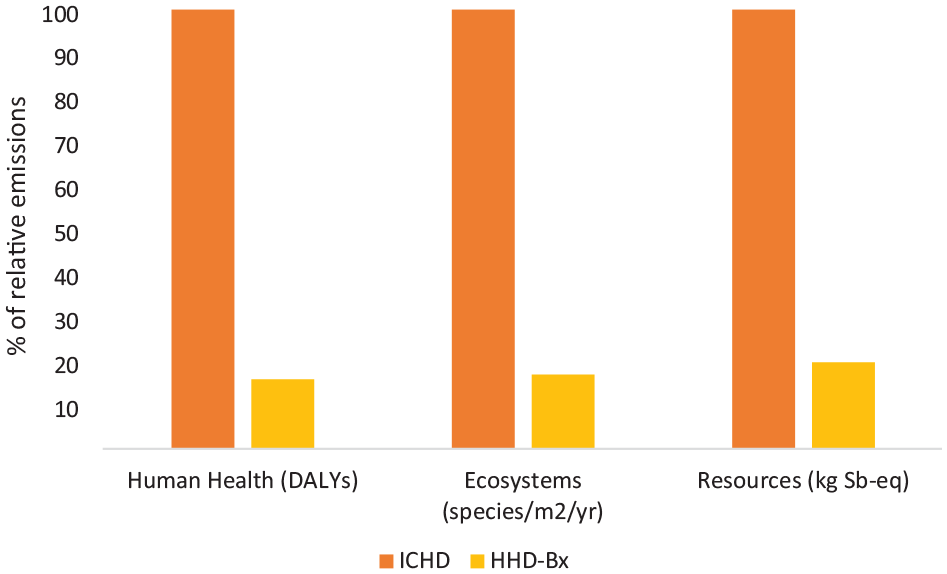
Comparative endpoint impacts of hemodialysis therapies.
Discussion
Interpretation of LCA involves the selection and reporting of contextualized results (Box 5).

Generalizability of LCA results must be considered in the context of regional variability in clinical practices, energy sources, types and provenance of consumables, and staff and patient travel distances. Sehgal et al describe a 3-fold variation in emissions from HD facilities within a single organization due to differences in natural gas consumption and transportation distances. 12 Hernández-de-Anda et al highlight the difference in annual HD GHG emissions based on number of dialysis sessions provided (6.6 tons CO2e with 96 treatments, 10.3 with 144). 13 These examples illustrate that no single LCA will provide globally applicable data. Lifecycle assessment replication in different geographic and clinical contexts can help users apply the findings to their settings and optimize care processes (Box 6).

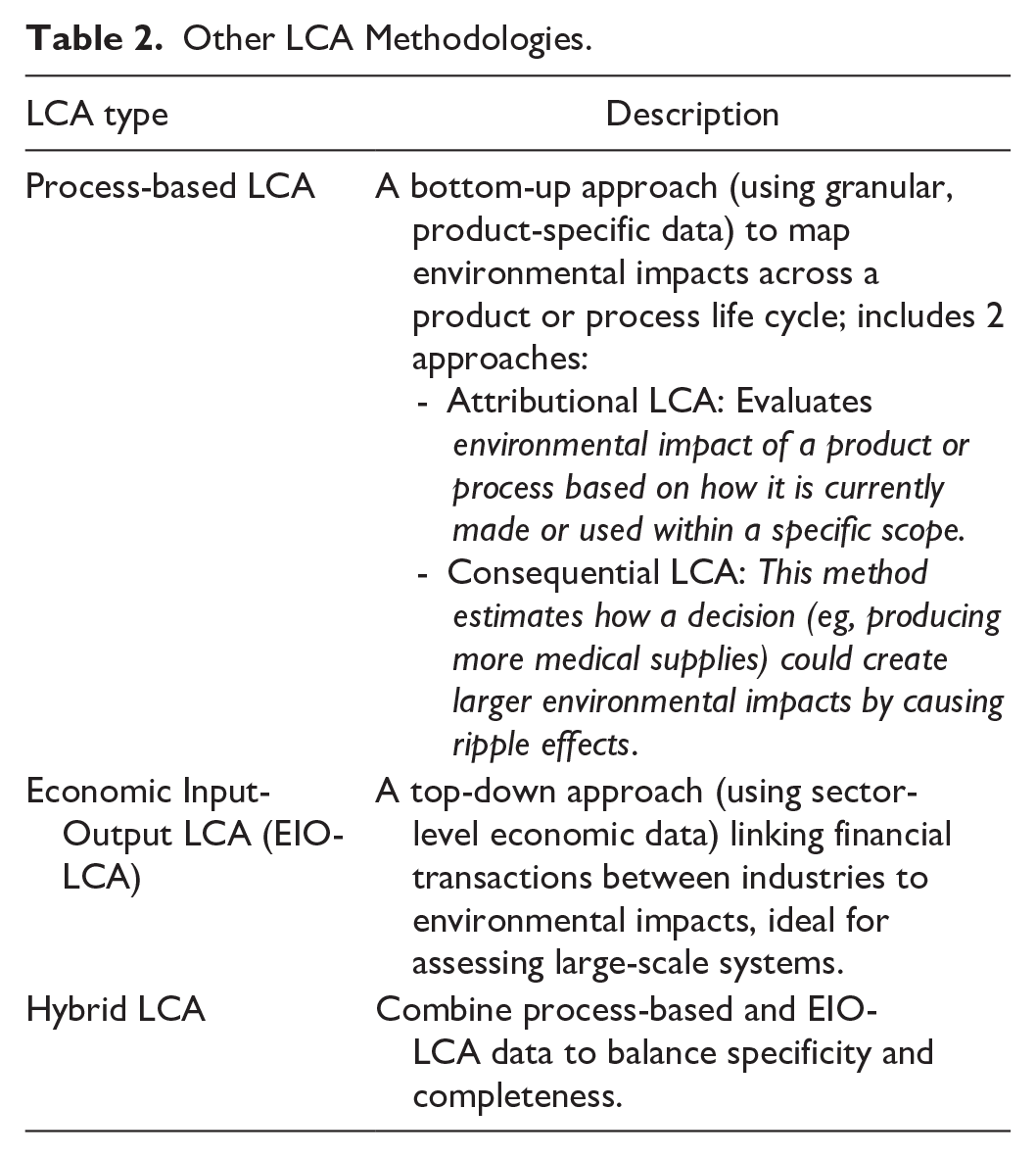
This manuscript describes the conduct of a process-based LCA. Additional LCA methodologies can be used in specific contexts or using alternate data sources, as outlined in Table 2.
Other LCA Methodologies.

Limitations
Although LCA is considered the gold standard for environmental impact assessment, the level of rigor and expertise may be unnecessary or impractical for some clinical questions and settings. Approximations of GHG emissions, or data collection for known highly emitting GHGs areas (eg, travel for HD, supply transport, consumables use), could still offer valuable insights. Data for these areas can be gathered through direct measurements, activity-based estimates, or by using established emission factors to identify the primary sources of emissions. Tools such as the in-center hemodialysis (ICHD) carbon calculator (available at ichdcarbon.org) are available, but may have limited generalizability (the ICHD calculator has only been validated in the United Kingdom). Lifecycle assessment is well suited to guide environmental performance improvement of individual modalities and to allow comparison between clinically equivalent alternatives, where knowledge of environmental performance might favor uptake of one therapy over another. However, primary data for dialysis consumables are limited, often requiring secondary sources. This limitation underscores the need for improved data collection efforts and alternative approaches.
Conclusion
Lifecycle assessment provides comprehensive environmental impact data across the life cycle of a product, process, or service. LCA allows specific comparisons between alternate therapies, including those that may not be obviously comparable operationally or environmentally, and highlights “hotspots” within a product or process for targeted improvement. Kidney care professionals will benefit from knowledge of LCA methodologies, limitations, and applicability as this technique is increasingly adopted in the clinical realm.
Footnotes
Acknowledgements
Special thanks are extended to Saba Saleem for her provision of the sample LCA case.
List of Abbreviations
CKD, chronic kidney disease; GHG, greenhouse gas; HD, hemodialysis; HHD, home hemodialysis; ICHD, in-center hemodialysis; ISO, International Organization for Standardization; LCA, lifecycle assessment; LCI, lifecycle inventory; LCIA, lifecycle impact assessment.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is supported by BC Renal and the Life Cycle Management Lab (LCML) at UBC Okanagan, we thank them for their invaluable support for this research. CES is gratefully supported by the Marcia Bell Research Scholar Award.
Ethical Considerations
Data for the sample LCA case were collected from primary sources under The University of British Columbia Research Ethics Board study protocol REB#H22-02433.
Consent to Participate
Not applicable.
Consent for Publication
Consent for publication was obtained from all authors.
Data Sharing Statement
Raw data that supports the findings of the case example in this primer can be accessed upon request from the corresponding author, in accordance with applicable regulations and ethical guidelines.
