Abstract
As humanity's marked effects on Earth's natural systems become increasingly apparent, we witness with alarm the impact on health and healthcare delivery. In this review, interrelationships between climate change, kidney health, and peritoneal dialysis (PD) therapies are described, and expansion of duty of care to the environment while maintaining the highest-quality healthcare is explored. Practical, high-yield actions that can be undertaken by patients and providers through the principles of sustainable care are introduced, including medication and single-use plastic consumables optimization, incremental PD, remote health monitoring, innovative PD effluent drainage, waste optimization, and importantly, patient empowerment as partners in sustainability. To ensure sustainable practices are embedded in clinical care, creation of a network of green champions, alignment with low carbon sustainable health systems more broadly, and appropriate uptake of emerging innovations in PD therapy that may be offered through sustainable procurement and regional or point of care dialysate production are crucial.
Case vignette
A gentleman with end-stage kidney disease recently started automated peritoneal dialysis (APD). He was immediately surprised by the plastic waste and single-use items consumed, and the frequent home deliveries and storage requirements. Each day, he discarded empty dialysate bags, drainage bags, plastic tubing, and APD cassettes, as well as their plastic and cardboard packaging (Figure 1). These materials accumulated quickly, filling numerous bags that exceeded his home rubbish removal allowance. Concerned about the environmental and financial impact of this waste, he explored whether his treatment could be more sustainable. However, he was unsure which items could be recycled, as he read that medical waste should not be placed in recycling or household bins. He highlighted his concerns to his peritoneal dialysis (PD) nurse during a clinic visit. The nurse later addressed this in a multi-disciplinary meeting with the home dialysis team. Together, they discussed practical steps to make PD more sustainable in their centre.

Image depicting waste generated from one day of continuous ambulatory peritoneal dialysis therapy. This image was provided by a patient who has provided consent for its use to be shared in this paper.
This vignette highlights patient and staff roles in advancing sustainable practices, emphasizing the need for educational resources on minimizing waste, conserving resources and encouraging sustainable options in kidney care.
Take-home points
Reducing the environmental impact of PD is a vital component of health systems transition to sustainability.
Environmentally sustainable PD can be achieved by operationalizing the Centre for Sustainable Healthcare's sustainability framework: health promotion, patient empowerment, lean resource management, low-carbon alternatives and operational resource use.
Institutional culture change driven by education and green champions, and incentives are critical to implementing environmentally sustainable kidney care.
Kidney care providers must collaborate with policymakers to accelerate widespread adoption of sustainable practices, and both can work with industry to aid the development of novel supply delivery systems and technologies that minimize resource use.
What is climate change, and what effects does it have on kidney health, and kidney health systems?
Climate change refers to the consequences of planetary warming on Earth's natural systems, including rising sea levels from melting glacial and polar ice, altered rainfall patterns, and extreme weather, all driven by human-caused increases in greenhouse gas (GHG) emissions, primarily due to the combustion of fossil fuels. The 2023 report of the Intergovernmental Panel on Climate Change warns that climate change threatens all life on Earth, while highlighting the rapidly closing opportunity to secure a liveable and sustainable future. 1 Despite 196 nations signing the legally binding Paris Accord, a treaty that seeks to hold average global temperature rise well under 2 °C from pre-industrial levels, temperatures throughout 2024 exceeded the agreement's aspirational 1.5 °C warming limit.2,3 In January 2025, average global temperatures reached 1.75 °C above pre-industrial levels, concerning climate experts that a new phase of accelerated planetary warming might now be occurring. 4
Ecological changes significantly impact human health, with 24% of deaths worldwide related to the environment. 5 Heat-related illnesses, water- and vector-borne diseases, food insecurity due to reduced crop yields, injuries from extreme weather, and increased non-communicable diseases including acute and chronic kidney diseases (CKD) are occurring. 6 Recent data reveal the links between kidney disease, heat and impaired air quality. Researchers in the United Kingdom (UK), a region known for its temperate climate, reported an odds ratio of 1.6 for acute kidney injury on days when temperatures reached 32 °C compared to 17 °C. They further highlighted an odds ratio of 1.02 per 1 °C increase in temperature above 17 °C. 7 In 2017, over 3.2 million incident and 122 million prevalent CKD cases were attributable to small particulate matter air pollution, alarming numbers considering that 99% of people globally reside in regions exceeding World Health Organization (WHO) air quality guideline limits.8,9 Not all are equally affected. Whilst contributing the least to climate change, and frequently struggling with underfunded health systems, 3.3 to 3.6 billion people reside in vulnerable low- and middle-income regions.1,10 The highest projected growth in the number of people with kidney failure is in the global south. 11
Extreme weather events disrupt healthcare delivery, posing risks to patients dependent on life-sustaining kidney replacement therapies.12,13 Climate- or disaster-related water scarcity presents a challenge for dialysis care, particularly in the context of haemodialysis. For PD, climate-related disruption can impact access to, or availability of, healthcare infrastructure (both human resources and clinic or hospital facilities), medications and PD supplies. 12 In 2024, Hurricane Helene caused severe flooding at the Baxter International manufacturing site in North Carolina, United States (US), temporarily halting operations and necessitating patients to adopt emergency PD supply conservation strategies. 14
The healthcare sector has a moral and ethical responsibility to minimize its environmental impact, not only to protect health through mitigating environmental impact of healthcare activities, but also to contribute to a liveable future. Kidney care providers must mobilize in a sectoral approach to low carbon and climate resilient care, including for PD therapies.
How does PD contribute to environmental harm?
The healthcare sector is responsible for 5.2% of global GHG emissions, and therefore contributes to climate change. 15 PD is a highly resource-consuming therapy. PD fluid, consisting of water, salts and sugar, is filled into steam-sterilized PVC bags, then packaged in High-Density Polyethylene over-pouches and cardboard boxes. The manufacturing facility requires electricity (energy sources vary from low-carbon renewables such as solar, wind and hydropower to high-carbon fossil fuels such as coal or natural gas) and water to operate. PD fluids and consumables (tubing, drainage bags, cycler cassettes) are transported either by land, sea, or air freight, depending on the location, to regional warehouses before being delivered to patients’ homes. Used materials are either sent for recycling, landfill or incineration. PD drainage fluid is disposed through wastewater systems. This process is summarized in Figure 2. Plastic in landfills may decompose into microplastics that can enter leachate. 16
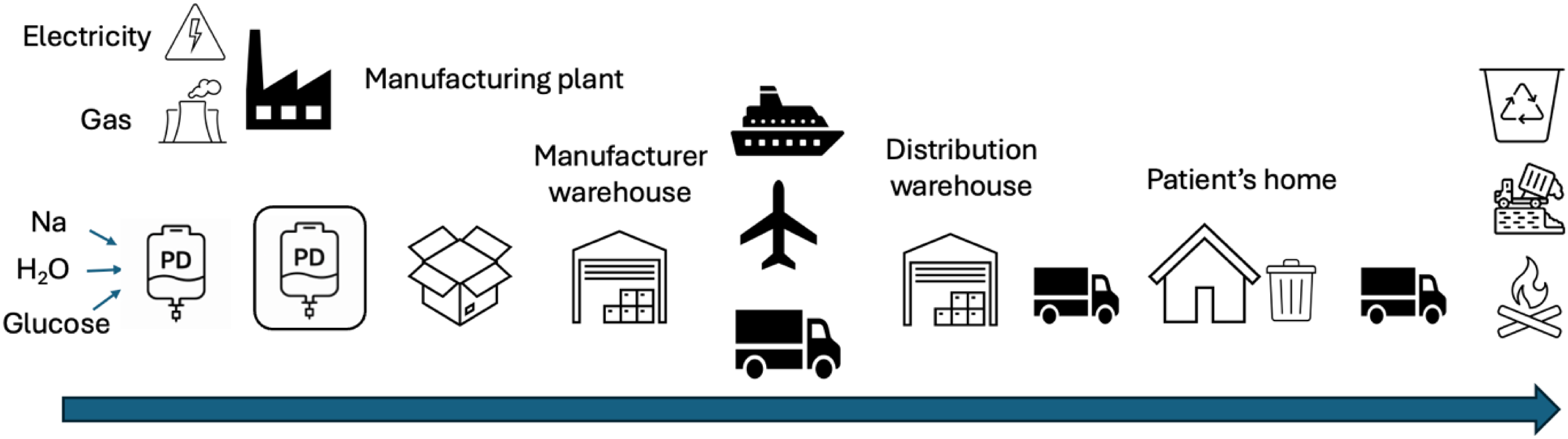
The production to waste of peritoneal dialysis fluid and consumables. Na: sodium, H2O: water
GHG emissions are reported in carbon dioxide equivalents (CO2e), a standard measure of atmospheric heat-trapping of different GHG. 17 GHG emissions for APD range from 11.8 to 15.0 kg CO2e per day (a 7-day prescription translates to 4.3 to 5.4 tonnes CO2e per year), while continuous ambulatory peritoneal dialysis (CAPD) emissions range from 3.5 to 4.8 kg CO2e per day (1.3 to 1.8 tonnes CO2e per year), depending on the country. 18 Emissions differ by region and country due to variations in energy sources, staff and patient transportation distances, and supply transport distances.16,18 Some variability is also due to differences in methodological approaches used in the life cycle analyses, such as whether certain processes were included within the system boundary, and whether proxy data were used. By comparison, the carbon footprint of in-centre haemodialysis (ICHD) ranges between 20.9 and 43.9 kg CO2e per session and home haemodialysis from 15.6 to 33.6 kg CO2e per session. 18 Similarly, a recent Australian study found ICHD emits 4.8 tonnes CO2e per patient per year, higher than both APD (3.3 tonnes CO2e) and CAPD (2.0 tonnes CO2e). 19 To contextualize these emissions, the global average annual CO2e emitted per person in 2023 was 4.7 tonnes (ranging from 0.3 to 38.8 tonnes CO2e per person, highlighting massive inequality in global resource use, hence emissions). 20
Energy required for operating the automated cycler, waste management, and dialysate production were the main contributors to APD emissions in Italy. In contrast, in the US, plastics were the primary drivers of GHG emissions. 18 APD had higher emissions compared to CAPD due to increased emissions in the manufacturing and disposal of APD consumables and their higher overall weight, leading to greater transport emissions.16,19
What is sustainable kidney care, and how can it improve the health of people with and at risk of kidney disease?
Sustainable healthcare maintains high-quality care whilst expanding duty of care to the environment, aiming to steward Earth's natural systems and resources for the betterment of all. The GREEN-K initiative (Global Environmental Evolution in Nephrology and Kidney Care) of the International Society of Nephrology has called for the systematic creation and implementation of environmentally sustainable kidney care (ESKC) by promoting low-carbon, resource-efficient kidney care through education, procurement and infrastructure improvements and sustainable clinical pathways. 21
A study in Japan found that the environmental impact of kidney care increases with declining kidney function, especially with rapid eGFR loss in CKD stages G3a and G3b or worse, reaching up to 1270–1440 kg CO2e versus 280–300 kg CO2e in CKD stage G1 or G2. 22 This is due to increased healthcare utilization, both outpatient and hospital-based, as CKD worsens. 22 Early identification and CKD risk factor modification, not only reduces kidney disease, but also lessens its environmental toll. 21 The alignment of better clinical outcome with lowest environmental impact for CKD preventive therapies was recently demonstrated in a secondary analysis of the CREDENCE trial. A 20% reduction in emissions with the addition of canagliflozin to routine therapy for people with type 2 diabetes and proteinuric CKD was demonstrated through avoidance of higher emitting dialysis and hospital care. 23
Early reports support transplantation having a significantly lower environmental impact than dialysis, hence improving the uptake of kidney transplantation, as well as extending graft survival, are key components of ESKC. To date, data of a direct comparison of the environmental impact between dialysis modalities and transplantation is lacking. A life cycle analysis estimated that up to 789.9 kg CO2e and 2022.3 kg CO2e are produced by living donor transplantations and deceased donor transplantations respectively. 18 This analysis did not consider the associated immunosuppressive therapy and follow-up care. The environmental impact of transplantation is likely highest in the immediate postoperative period but is expected to decline with stable graft function, making it reasonable to assume that transplantation would have overall lower GHG emissions compared to dialysis. Additionally, transplantation improves survival and quality of life compared to dialysis, making access to transplantation a key priority in quality kidney care.21,24
How can the environmental impact of PD be reduced?
The principles of sustainable healthcare, as defined by the Centre for Sustainable Healthcare, provide a useful approach to explore sustainability improvements in PD. These principles include disease prevention and health promotion, patient empowerment, lean healthcare delivery, low-carbon alternatives and operational resource use. 25 Figure 3 illustrates these principles applied to PD, including their interconnections. Table 1 summarizes the possible interventions and resources.
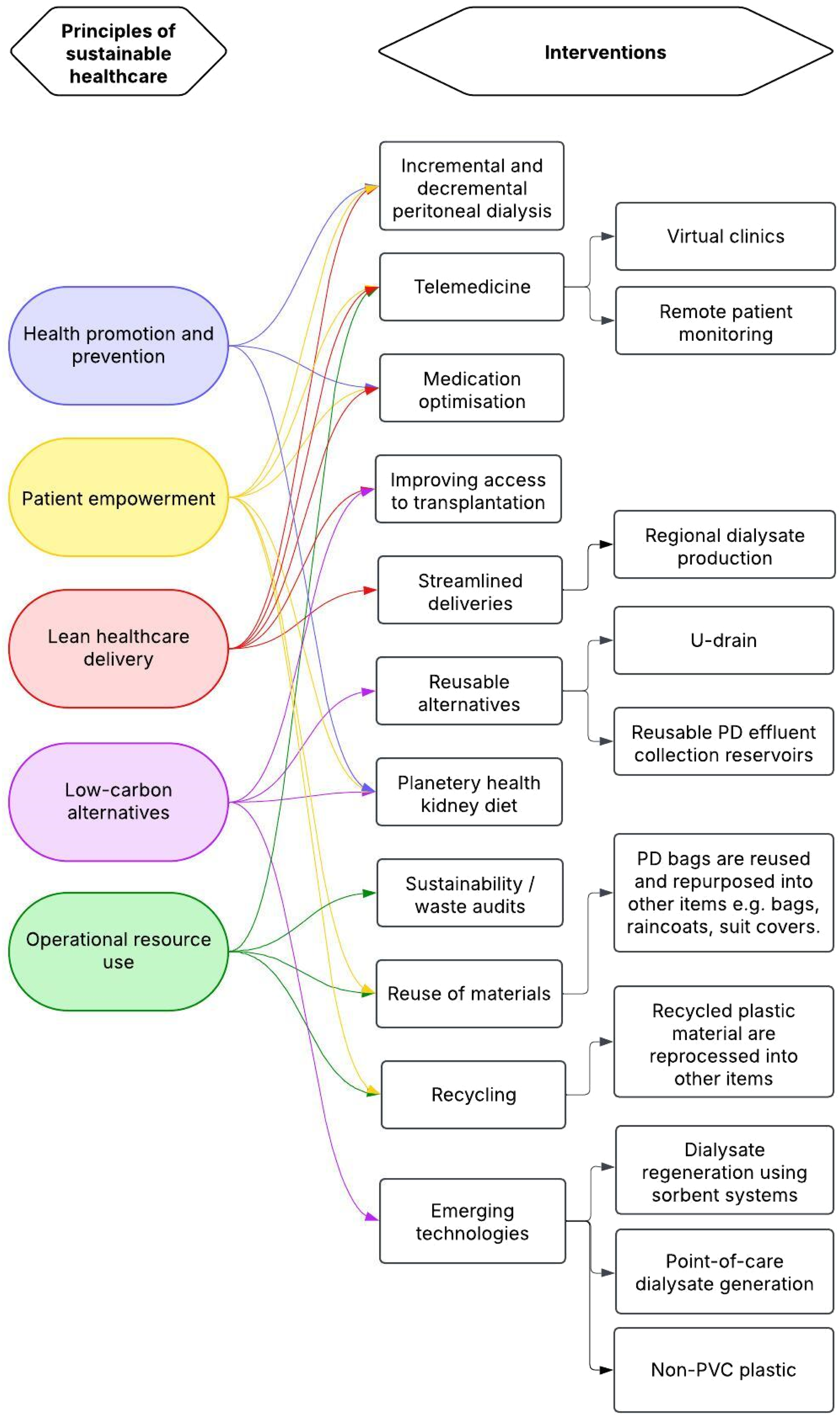
Possible interventions to reduce the environmental impact of peritoneal dialysis. PD: peritoneal dialysis. Driver diagram adopted using The Centre for Sustainable Healthcare principles of sustainable clinical practice. 25
A summary of selected sustainable interventions in peritoneal dialysis.
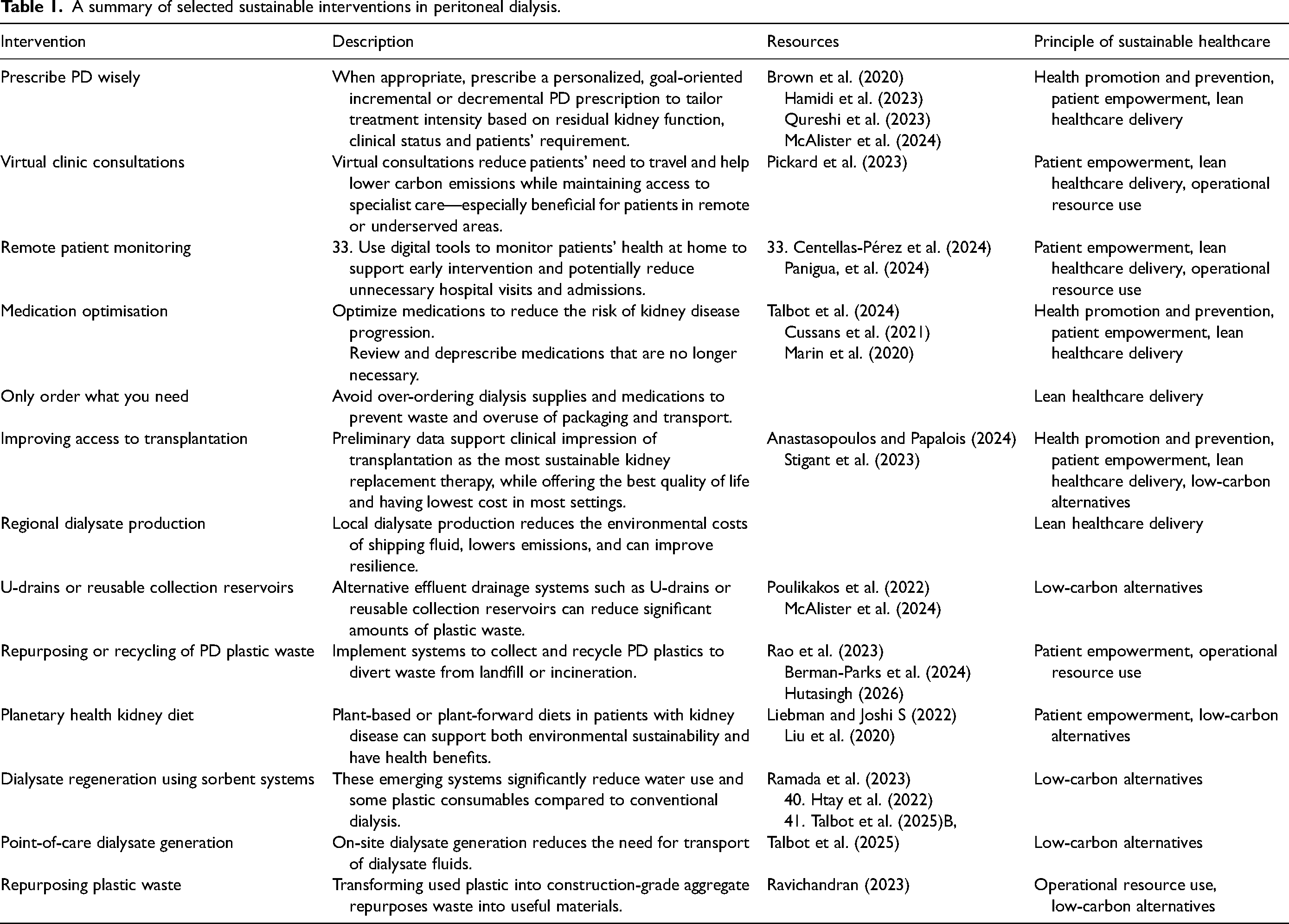
Sustainable PD treatment options are explored below. Their appropriateness requires consideration of clinical factors, ideally through shared decision-making with patients and/or their carers. These strategies were selected for their accessibility and reduced health care resource use.
Prescribe PD wisely
PD can be started at lower estimated glomerular filtration rates in appropriately selected patients, without significant compromise in clinical outcomes when initiation is timely and supported by adequate pre-dialysis care. 26 Incremental PD is initiating patients on PD with a less than ‘standard dose’ dialysis. The dialysis prescription is increased as residual kidney function declines. 27 Similarly, decremental PD involves reducing an established ‘standard’ prescription to a lower dose, as may be appropriate with improvement in residual kidney function, or a change in patient status with reduced solute clearance requirement (i.e. as may occur with weight loss, lower food, especially protein, intake). 28 Incremental and decremental PD prescriptions involve fewer exchanges, lower dialysate use and lower disposal needs.16,29 This, in turn, has cost benefits, 29 while improving patients’ quality of life by easing treatment burden, and aligning with the International Society of Peritoneal Dialysis guidelines. 27
Optimize medication use
In the UK, it is estimated that £300 million worth of prescribed medicines are wasted annually. Reducing half of that wastage could avoid 23.4 million kg CO2e emissions. 30 In a Canadian study, PD patients averaged 16.7 prescribed medications, four of which were potentially inappropriate. 31 Medication reviews and deprescribing can reduce medication wastage. 32 Shared decision-making supports patients in expressing their understanding of their condition and educates them on proper medication adherence. 30
Only order what you need
Ensuring that patients receive the right quantity of PD supplies requires regular reviews of usage patterns, considering any changes in prescription and compliance. Overordering can lead to burdensome supply presence in the home setting, and product expiry or non-use if interim prescription change occurs, with associated financial and environmental costs. PD providers should implement inventory management systems, conduct routine supply audits, and engage with patients to track their actual needs. 32 Encouraging patient-provider communication about supply levels can prevent surplus deliveries while ensuring continuous and uninterrupted care. 33
Optimize use of virtual care and monitoring technologies
When appropriate and available, virtual consultations, via telephone or video, significantly reduce GHG emissions associated with travel for in-person appointments. Lower impact is particularly observed in rural or underserved areas where travel for in-person appointments can be substantial. 34
Certain APD machines have a functionality of remote patient monitoring, allowing healthcare providers to remotely track treatment data and proactively manage patients. Such monitoring can facilitate early detection of complications, allowing timely intervention that in some settings has been shown to reduce hospitalization rates and improve technique survival.35,36 Reducing adverse events and hospital admissions bring significant environmental benefit. Additionally, remote monitoring supports treatment adjustments without requiring patients or providers additional travel to clinic, thereby reducing transportation-related emissions. 37
Adopt a planetary health kidney diet
When appropriate and desired, patients can enhance sustainability by adopting a plant-based or plant-forward diet such as the EAT-Lancet planetary health diet. 38 While research on plant-based diet in the PD population remains limited, several potential advantages have been demonstrated, including less constipation, volume and sodium overload, hypertension and metabolic acidosis. 39 One study suggests that a diet with higher plant-based protein is associated with lower mortality in PD patients compared to individuals on a lower plant-based protein diet. 40 Despite these benefits, careful nutritional planning is essential. A plant-based diet may pose challenges in maintaining adequate protein and energy intake, as well as managing serum potassium and phosphate levels, which could be elevated due to high mineral content of certain plants and food additives. 39 Regular dietary monitoring and consultation with kidney dietitians can help mitigate these risks.
Steward use of PD consumables
Single-use drainage bags in PD generate up to 148.6 kg of plastic waste and 155.1 kg CO2e emissions per year. 16 Alternative drainage systems can reduce plastic waste and improve convenience for patients. In the UK, U-drains allow PD effluent to be drained directly into a household plumbing system, eliminating the need for disposable drainage bags. The system simplifies PD setup and clearing post-dialysis, reduces plastic waste and minimizes storage space for consumables without increasing peritonitis incidence. 41 Utilizing a 25-litre drum as a reusable collection reservoir is another drainage option that has been demonstrated to reduce GHG emissions and save costs. 16
In 2020, Fresenius Medical Care received approval from the US Food and Drug Administration for their PD solutions to be packaged in PVC-free Biofine® bags. These bags are reported to be 60% thinner than conventional PVC tubing, hence require less material for production. 42 However, there are currently no widely known established recycling pathways for these Biofine® bags. Hence, novel plastics, including Biofine® and bioplastics, warrant further study to better define any anticipated environmental benefit.
Recycle eligible PD materials
Performing four CAPD exchanges generates 58.76 and 222.88 g of recyclable polypropylene and PVC plastic, respectively, per day. An APD treatment of four exchanges at night with a day fill generates 75–89 g of recyclable polypropylene plastic and 272–323 g of PVC plastic waste daily. Globally, recyclable polypropylene and PVC PD waste exceed 7 million kg and 30 million kg, respectively. 43 Recycling PVC could potentially reduce emissions by up to 30% for CAPD and 14% for APD. 16
Major barriers to recycling plastic waste in PD are the classification of healthcare waste as ‘hazardous’ hence non-recyclable, or when recycling programmes are unavailable. 32 There are several successful recycling initiatives that have helped to reduce plastic waste. In Mexico, a pilot recycling program allowed patients to return used PD bags for recycling. 44
Manufacturers should be urged to support recycling by expanding take-back programs, such as Baxter's PVC recycling program in Australia, New Zealand, and Malaysia.44,45 These examples illustrate how patient empowerment, industry collaboration, and linkage with local waste management infrastructure play a major role in reducing our plastic waste in PD.
What are the future directions of sustainable PD?
Emerging PD technologies offer enhanced portability and dialysate regeneration using sorbent systems. Viva Kompact, previously known as Automated Wearable Artificial Kidney (AWAK) and Wearable Artificial Kidney (WEAKID) are PD devices based on the REDY (REcirculating DialYsis) sorbent system.46–48 This has the potential to reduce water and plastic use for PD significantly, but benefits must be weighed against the carbon footprint of sorbent production and recycling. 46 A preliminary safety study in 15 patients demonstrated no serious adverse events, though many patients experienced abdominal bloating and abdominal pain during recirculation. 47
Another emerging development of interest is the point-of-care dialysate generation system. One example, the Ellen Medical Devices Point-of-Care (EM-POC) system, includes a portable pure water distiller and a plastic bag containing a proprietary blend of electrolytes and sugars. Sterile water from the distiller reconstitutes PD fluid at home. A regimen of four 2-litre bags daily, amounting to 3 tonnes annually, can be reduced to 230 kg with EM-POC PD bags. 49 Further environmental benefit could be realized through reduction of dialysate transport GHG emissions.
Turning PD plastic waste into aggregates for construction material is another potential to enhance sustainability in both the healthcare and construction sectors. 50
How can we improve the culture toward sustainable PD care?
Talk about climate change
Speaking to colleagues and patients about climate change and its impacts on health and health systems can be challenging at first, especially in clinical settings that often prioritize immediate needs. In climate science, tipping points refer to a threshold in Earth's systems that causes sudden, irreversible changes to major systems when exceeded. 1 By complementary analogy, social tipping interventions are small actions at individual, organizational or global levels that can accumulate to catalyze broader awareness and shifts in practice. 51 Nephrologists and other professionals have an important role in driving these social tipping interventions, framing climate action as a component of quality care that embeds sustainability and enhances resilience while protecting planetary health. 52
Empower patients to adopt sustainable practices
In this case vignette, the patient was overwhelmed by the vast quantity of waste produced by his treatment. As described in Verdin et al. (2025), ‘Ask us where the waste is generated—we will tell you!’ but it is rare that the kidney team raises the topic of waste reduction with the patient. 32 PD providers can address this by integrating sustainability education into patient training sessions, such as covering topics like waste management, responsible disposal and signposting to recycling programmes if available. For example, the ‘Jom Recycle’ plastic recycling programme in Malaysia educates patients on how to separate recyclable materials from non-recyclable medical waste. 45
It is also our responsibility as health care professionals to educate patients on broader environmental health topics and encourage them to advocate for sustainable healthcare. This can build a sense of ownership and responsibility for environmental health whilst contributing to their own kidney care.
Medical education
The Royal College of Anaesthetics in the UK exemplifies this by including sustainability in its training curriculum. 53 A similar approach in nephrology training could encourage early adoption of sustainable practices. The GREEN-K initiative provides an online curriculum for sustainable kidney care. 54 Integrating sustainability modules into formal training, beginning with medical and nursing curricula, would help future professionals consider the environmental impacts of healthcare delivery, incorporating sustainable practices into everyday services.
Green champions
In the UK, the Centre for Sustainable Healthcare's Kidney Centre Sustainability Champion Scheme encourages units to designate a Green Champion, a staff member dedicated to advocating and implementing sustainable kidney best practices care. 55 Within the PD team, the Green Champion can engage with the multidisciplinary team and patient representatives to drive awareness, promote sustainability and inspire colleagues to adopt sustainable daily practices.
Incentives including financial savings
Integrating sustainability into healthcare practices improves financial efficiency, system resilience and patient outcomes. 56 Incentivizing sustainability initiatives through financial savings could drive further change in culture. A successful example is seen in the Bradford Haemodialysis unit, where 20% of the savings from installing central dialysate acid delivery, which reduced dialysate and plastic waste, were returned to the kidney department. 57 Additionally, the unit used the prize money from the British Journal of Renal Medicine Innovation in Renal Medicine award in 2011 to upgrade to more energy-efficient lighting in their unit. 58 In Thailand, the Friends of Kidney-Failure Patients club uses the proceeds of the sale of repurposed plastic waste from PD to fund the care of dialysis patients. 59
Charitable incentives could boost participation in recycling and waste reduction programmes, especially among those less motivated by environmental issues. Studies show that individuals with lower environmental values are more inclined to recycle if it benefits others, while those with strong environmental values recycle consistently, regardless of the outcome recipient. 60
Sustainability audits
ESKC PD specific key performance indicators (KPIs) should be defined, routinely collected and used for iterative process improvement. These KPIs should address key areas such as energy and water consumption, packaging and supply chain efficiency, and waste generation and disposal. By embedding these metrics within a continuous audit process, healthcare providers can systematically identify opportunities to reduce environmental impact whilst maintaining high standards of patient care.
Waste audits improve purchasing, waste segregation and recycling, ensuring recyclables are processed correctly and non-infectious medical waste is diverted from biohazard bins for incineration, reducing financial and environmental costs. Audit results can help units set measurable goals and engage staff in sustainability, fostering a culture of continuous, sustainable quality improvement. 61
To promote positive culture change, the topic of sustainability should be a standing agenda item in governance and departmental meetings, ensuring continuous assessment, accountability and improvement.
How can the global kidney care community work together to improve the environmental sustainability of Peritoneal Dialysis?
Globally, all regions are confronted with sustainability challenges in PD care, highlighting the need for a sectoral and collaborative approach that involves all stakeholders, including PD providers, patients, industries, administrators and policymakers to develop solutions that are locally appropriate and globally aligned (Figure 4). The GREEN-K initiative of the International Society of Nephrology seeks to align kidney care globally with planetary health principles. 21 It is developing resources and a sustainable procurement strategy to promote global procurement of innovative kidney care processes, services, and products that are environmentally friendly, climate-adapted and affordable, that reduce health inequalities. 21 Kidney societies worldwide are encouraged to develop their own sustainable care programmes and join the global effort to improve kidney health while safeguarding Earth's natural systems. Since much of PD's carbon emissions originate from the production and transportation of consumables, the role of industry, including manufacturers, logistics and distribution organizations, in reducing the environmental impact of this therapy is significant. System-level policies and procurement frameworks can encourage industry to prioritize sustainability throughout the supply chain. Meaningful emissions reductions will require engagement with industry to develop resource-efficient technologies, minimize single-use plastics, reduce packaging and transport distances, and establish take-back or recycling schemes.
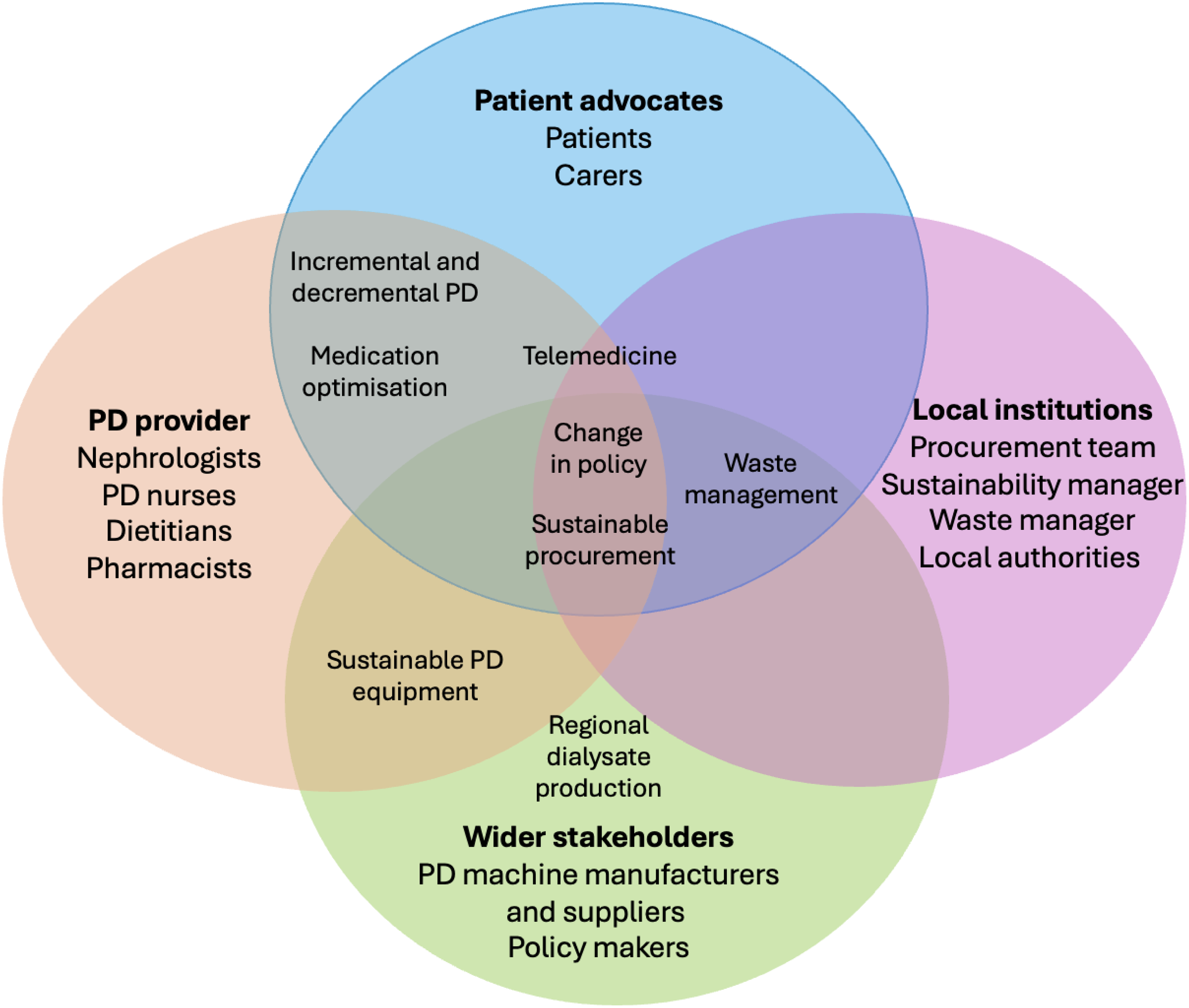
Key stakeholders and their influence on sustainable PD initiatives.
Alongside industry partnerships, advocating for sustainable procurement policies within government agencies and hospitals can ensure that healthcare systems prioritize low-carbon and environmentally friendly dialysis products. This includes striving for regulations that incentivize green manufacturing practices and integrating sustainably sourced materials in hospital procurement decisions, similar to the sustainability efforts promoted by the GREEN-K initiative. 21
Integrating sustainability into PD guidelines, professional training programmes and conferences through collaboration with kidney societies is essential and ensures environmental concerns are embedded into dialysis care. Patients and carers provide a powerful voice for sustainability in healthcare. Engaging patient organizations and charities, like the UK's National Kidney Federation, and publishing their insights, can amplify patient voice, influence policy and share best practices for greener care.32,62
Through partnership, innovation, practice improvement, advocacy and broad system engagement, a more sustainable future for PD can be achieved, ensuring environmentally responsible, cost-effective and effective dialysis care for future generations.
Conclusion
By focusing on the five principles of sustainable healthcare – health promotion, patient empowerment, lean resource management, low-carbon alternatives and operational resource use – healthcare providers can significantly lessen the environmental impact of PD while maintaining the highest standards of patient care.
Footnotes
Acknowledgements
We are grateful to the patient for their voluntary contribution of a photograph documenting a full day of waste generated from continuous ambulatory peritoneal dialysis. Their photograph has supported the educational value of this work.
Declaration of conflicting interests
SC and MP have no conflicting interests. CS has the following conflicts: Speaker’s bureau Otsuka Canada; received honoraria for environmentally sustainable kidney care talks from University of Manitoba, McGill Institute of Cardiology, and Queen’s University; steering Committee member, ISN GREEN-K initiative (non-remunerated position); Chair, Canadian Society of Nephrology ‘Sustainable Nephrology Action Planning’ Committee (non-remunerated position); Medical Lead, Planetary Health Working Group, British Columbia Renal Agency (salaried position); and received salary support from Marcia Bell Distinguished Scholar Award, University of British Columbia.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval was not required for this review.
Informed consent to participate
Not applicable.
Informed consent to publish
Not applicable.
Trial registration
Not applicable.
Author contributions
SC and MP conceived and designed the review article. SC researched and drafted the manuscript. CS and MP critically reviewed and revised the manuscript. All authors approved the final version of the manuscript.
