Abstract
This report describes a patient with Vertical Maxillary Excess without open bite in whom surgical orthodontic treatment to reduce lower facial height remarkably improved function and facial esthetics. The patient was a 22-year-old male whose main concern was crowding and temporomandibular joint clicking sounds. The clinical and radiological findings led to the diagnosis of Vertical Maxillary Excess with a mild skeletal class II malocclusion. The proposed treatment plan comprised a bimaxillary surgery without premolar extractions. LeFort I osteotomy was planned to reposition the maxilla superiorly by 7–8 mm. This surgery was combined with a bilateral sagittal split osteotomy for mandibular anterior derotation to adjust the mandible to the occlusal and anteroposterior change. Postoperatively, the mandibular plane angle (GoGn-SN) was decreased by 4° and skeletal class I was achieved (ANB, 4°). In addition, lip incompetence was corrected and the excessive gingiva exposure upon smiling was significantly improved. The patient was satisfied with the treatment result and reported the temporomandibular joint clicking sounds disappearing after surgery.
Introduction
Vertical Maxillary Excess (VME) is a developmental deformity presenting skeletal, dento-alveolar, and facial characteristics, notably an excessive vertical growth of the maxilla. This typically results in lip incompetence and excessive exposure of maxillary incisors at rest with or without a gummy smile. 1 There are two different types of VME: with open bite and without open bite. The lower third of the face is considerably increased in both types of VME which accounts for the steep mandibular plane and the retrognathic appearance of the mandible especially in individuals with open bite. However, the main skeletal difference between the two types of VME is in ramus height; the ramus of the open bite type is normal or slightly reduced, whereas the ramus of the non-open bite type is increased. 2 To achieve balanced facial proportions and optimal functional occlusion, a combined surgical-orthodontic approach is generally indicated. The down fracturing or LeFort I maxillary osteotomy for superior repositioning of the maxilla is considered the gold standard surgical treatment for VME. 3 It involves the separation of the tooth-bearing portion of the maxilla from the rest of the maxillary bone then displacing it in the desired position. 2 In certain cases, the LeFort I osteotomy can be combined with a bilateral sagittal split osteotomy (BSSO) for mandibular anterior derotation and advancement to correct a skeletal class II malocclusion which is common in patients with VME. 3 The aim of this article is to report the orthodontic and surgical treatment of a patient who had VME without open bite. A bimaxillary surgery was performed.
Case presentation
Clinical examination and diagnosis
The patient is a 22-year-old male who sought orthodontic treatment with the chief complaint of crowding in both dental arches. He also reported having temporomandibular joint (TMJ) clicking sounds when opening and closing his jaw.
The facial photographs (Figure 1) showed an oval, slightly tapered form with an increased lower third height of the face. The nose was narrow and the cheekbones were flat. Excessive exposure of the maxillary incisors and increased interlabial distance were evident. In profile, the nose was prominent, the nasolabial angle was within normal limits, and the chin was retrusive.

Pretreatment facial photographs.
The intraoral photographs (Figure 2) revealed considerable crowding in both arches with a high vaulted narrow palate. A unilateral class II canine relationship was noted on the left side with a 2 mm shift of the mandibular midline to the left. A class I molar and canine occlusion was present on the right side.

Pretreatment intraoral photographs.
On the panoramic radiograph (Figure 3(a)), root lengths and periodontium appeared normal. The Cephalometric radiograph (Figure 3(b)) revealed a mild skeletal Class II relationship (ANB = 6°). Both sella-nasion-A point (SNA) and sella-nasion-B point (SNB) were decreased (SNA = 76°, SNB = 70°) suggesting a maxillary and mandibular retroposition relative to the cranial base. Mandibular plane angle showed a hyperdivergent craniofacial pattern (SN-GoGn = 42°) with a convex profile (Angle Z = 65°). In addition, incisor angulation was within normal limits for the upper and lower teeth (IMPA = 91°, I/F = 115°). The cephalometric measurements are shown in Table 1.

Pretreatment radiographs. (a) Panoramic radiograph. (b) Anteroposterior cephalometric radiograph.
Cephalometric measurements.

ANB: A point-nasion-B point; angle Z of Merrifield: Frankfort horizontal-profile line; FMA: Frankfort horizontal-mandibular plane; Jarabak’s ratio: ArGo/NMe: articular gonion-nasion menton; SD: standard deviation; SNA: sella-nasion-A point; SNB: sella-nasion-B point; SN-GoGn: sella nasion-gonion gnathion; WITS appraisal: Witwatersrand appraisal.
The clinical and cephalometric findings led to the diagnosis of VME without open bite, moderate skeletal class II and Angle class II right subdivision.
Treatment objectives and treatment plan
The main treatment objectives were to achieve normal maxillary incisor exposure at rest (2 mm) and to attain lip seal without straining of the mentalis muscle by reducing the overall face height. Correcting lip incompetence would have both esthetic and functional benefits since this condition is commonly linked to mouth breathing. Other treatment objectives included resolving the crowding in both arches, establishing a class I occlusion with normal overbite and overjet, and correcting the midline shift.
A LeFort I osteotomy was elected to reposition the maxilla superiorly and raise the occlusal plane. The impaction of the maxilla will allow a counterclockwise rotation of the mandible which will further decrease the height of the lower face and cause the chin to be slightly more prominent. Based on the amount of incisor exposure at rest, we were able to determine that, approximately, a 7 mm maxillary impaction was necessary to achieve esthetically pleasing results. In addition, the autorotation of the mandible also meant that the maxilla would need to be moved slightly anteriorly to maintain the same occlusal relationship. In our case, the LeFort I osteotomy was combined with a BSSO for mandibular anterior derotation to accommodate the occlusal and anteroposterior change without placing excessive pressure on the TMJ especially since the patient presented with TMJ disorder (TMD) symptoms preoperatively.
Treatment alternatives
Extraction of the upper and lower second premolars. This treatment option would aid in resolving the crowding, especially since the lower left second premolar is lingually tipped. However, it would not correct the lip incompetence.
Temporary anchorage devices can be used as an alternative to maxillary surgical impaction to correct the gummy smile. However, the amount of intrusion achievable with mini-screws is insufficient, in this case, to correct the VME and establish lip seal.
Treatment progress
Surgical-orthodontic treatments are generally conducted in three phases: (1) preoperative orthodontic treatment, (2) surgical intervention, and (3) postoperative orthodontic phase. One of the main goals of presurgical orthodontics is to eliminate dental interferences and simplify the surgery. For this patient, presurgical orthodontic care was initiated after extraction of the third molars to level the teeth, resolve the crowding, and coordinate the arches mainly by expanding the maxillary arch. Basically, any orthodontic movement that can potentially open the bite is performed during this phase.
On the day of appliance placement, orthodontic bands were adjusted on the upper and lower first and second molars. Roth prescription brackets were bonded on the remaining dentition except the LL 5. The slot sizes were 0.022 × 0.028-in (GAC™ Thin Arch Mini brackets Dentsply GAC Germany). The following sequence of Nickel Titanium (NiTi) archwires was used to align the teeth in both arches: round section archwires with a diameter of 0.014-in and then 0.016-in followed by a rectangular archwire with a diameter of 0.016 × 0.022-in. When the mandibular archwire was changed to a 0.017 × 0.025 Stainless Steel (SS) wire, an open coil spring was placed to create space for the lingually positioned left second premolar mostly by derotating and tipping the first molar distally (Figure 4). Once all teeth were aligned, a set of 0.019 × 0.025 SS archwires were ligated and crimpable hooks were adjusted along each one of them to allow for the intraoperative intermaxillary fixation (IMF). The presurgical orthodontic phase lasted approximately 7 months. Maxillary arch expansion and distal tipping of mandibular left molars resulted in a slight open bite that was planned to be corrected, along with the unilateral class II occlusion and midline deviation, during the surgical intervention. Presurgical facial and intraoral photographs are shown in Figure 5.

Intraoral photographs during orthodontic treatment.
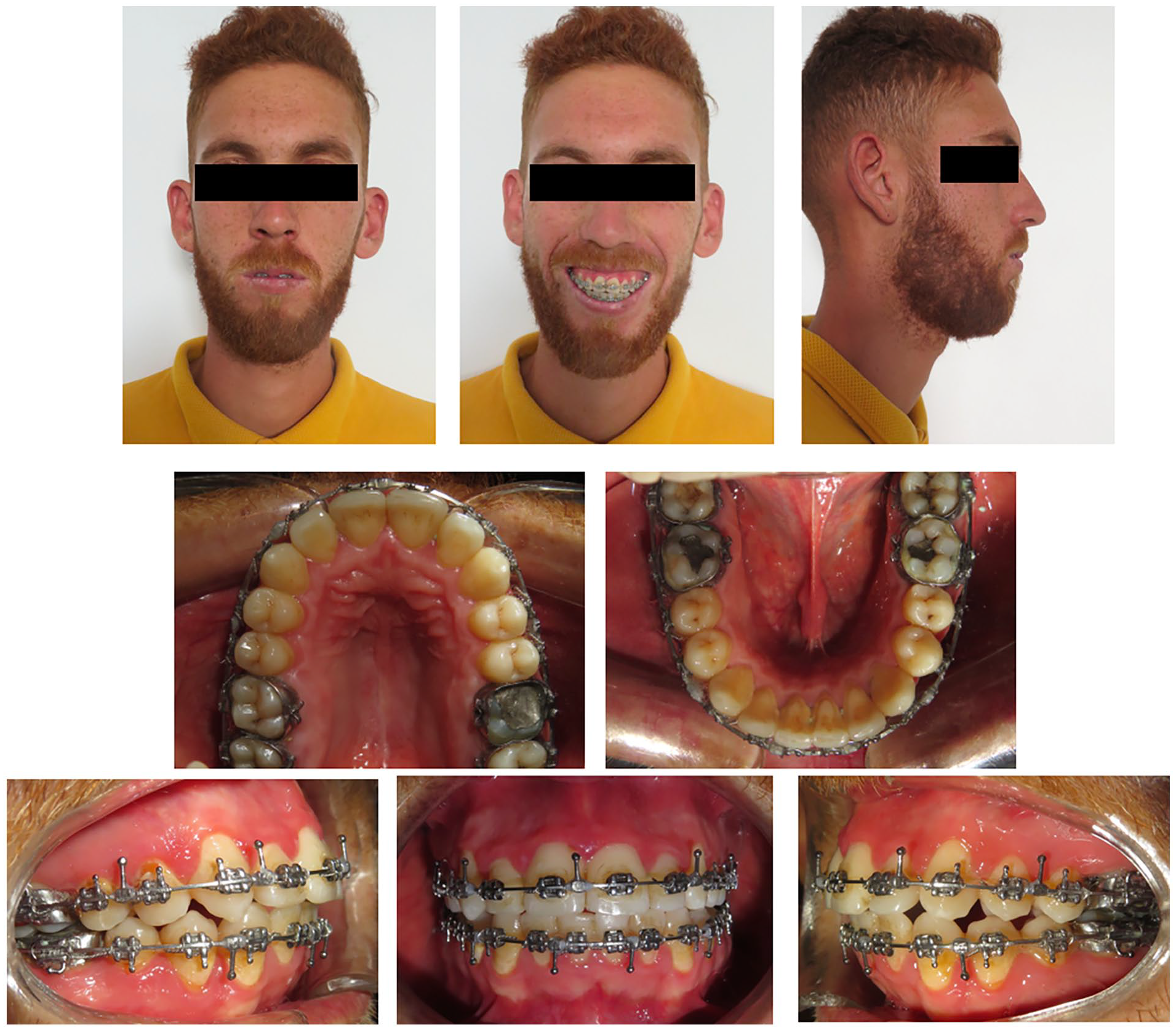
Presurgical facial and intraoral photographs.
Preoperative cephalometric predictions indicated that a 7–8 mm impaction of the maxilla would allow the mandible to autorotate upward and forward by 4–5 mm assuming the radiographic condyle as center of rotation. The prediction of the mandibular autorotation is done by rotating the mandible in the sagittal view while keeping the point located at the center of the mandibular condyle. Taking into consideration the autorotational movement of the mandible, the maxilla would also have to be surgically moved slightly forward to maintain the same occlusal relations. After the cephalometric surgical planning, maxillary and mandibular casts were mounted on a semi-adjustable articulator using a face bow and a check bite. Vertical and horizontal reference lines were made on the bases. The maxillary cast was trimmed according to the amount of superior movement and then was luted to the mandibular cast in an optimal occlusion using sticky wax and the articulator was closed. Two acrylic splints were made and used as the occlusal key during surgery. A LeFort I osteotomy with impaction of 7–8 mm was combined with a BSSO for mandibular anterosuperior movement with slight rotation to the left to correct the unilateral Class II malocclusion and midline deviation. The patient remained in IMF for 6 weeks. Orthodontic refinement was accomplished after the IMF phase to improve interdigitation using elastics.
Treatment results
The duration of orthodontic treatment was approximately 24 months. The appliance was removed 6 months after surgery and bonded retainers were placed in both arches. Recall visits occurred at 3-month intervals during the first year.
The treatment results were documented in Figure 6. The posttreatment radiographs are shown in Figure 7. The cephalometric tracings before and after treatment were superimposed in Figure 8, with the measurements listed in Table 1.

Posttreatment facial and intraoral photographs.

Posttreatment radiographs. (a) Panoramic radiograph. (b) Anteroposterior cephalometric radiograph.

Cephalometric superimposition. Black line: pretreatment. Red line: posttreatment.
Post-operative examination showed a functional and esthetic improvement with decreased overall face height and well-proportioned facial thirds. Normal lip seal was achieved and the position of maxillary incisors was in good balance with the upper lip. Teeth and gingiva exposure upon smiling was also decreased. In addition, it was evident that the superior repositioning of the maxilla widened the base of the nose and elevated its tip. Occlusally, the arches were well rounded and crowding was resolved. A Class I occlusion was established with ideal overjet and overbite, and coincidence of midlines.
The posttreatment panoramic radiograph (Figure 7(a)) revealed satisfactory parallelism between the teeth with minimal signs of root resorption in the maxillary and mandibular incisors. It was evident from the posttreatment lateral cephalogram (Figure 7(b)) that the mandibular plane angle was decreased after surgery (GoGn-SN, 38°) which improved the chin projection and reduced the convexity of the facial profile (Angle Z, 79°). Jaraback’s ratio (SGo/NMe ×100) was within normal limits (64.4%). 4 However, it demonstrated an increase from 63% to 64.5% following surgery, attributable to the reduction in the NMe distance. Both SNA and SNB angles increased while ANB angle decreased from 6° to 4° as a result of the anterior derotation of the mandible, thus establishing a skeletal class I. The anteroposterior inclination of the maxillary and mandibular incisors had increased (IMPA, 98°, I/F, 120°). Superimposition of the pretreatment and post-surgical cephalometric tracings demonstrated the superior repositioning of the maxilla and the anterosuperior derotation of the mandible, which both decreased the height of lower facial third. We observed an upward movement of both the anterior and posterior nasal spines, each by approximately 6 mm. This change is expected given the nature of the horizontal maxillary impaction procedure. Point A shifted upward by 6–7 mm and forward by 4 mm, aligning with the extent of the maxillary advancement surgery performed in association with the impaction. The mandibular skeletal changes were evidenced by shifts in the positions of the landmarks B, pogonion (pog), and menton (Me) in both horizontal and vertical dimensions. These points advanced forward by 11–12 mm and upward by 6–7 mm, consistent with the mandibular anterosuperior derotation performed during surgery to accommodate the changes of the maxilla. The soft tissues are affected by the changes in the underlying skeletal structures, as reflected in the upward and forward shifts of cutaneous Pog and Me by 7 mm upward and 11–12 mm forward, respectively. In addition, post-surgery assessments indicate that while the length of the lower lip remained unchanged at 65 mm, the upper lip length decreased by approximately 5 mm, from 29 to 24 mm, directly attributable to the superior repositioning of the maxilla.
Discussion
VME is a developmental deformity that results due to overgrowth of the maxilla. Clinically, it manifests with lip incompetence and excessive exposure of the maxillary incisors and the gingiva when smiling. 5 The length of the upper lip is normal but may appear short due to the full exposure of the upper front teeth when the lips are in repose. 2 Class II malocclusion with or without open bite is also common in individuals with VME. Radiologically, the mandibular plane angle (MP-SN) is increased in both types of VME, noticeably more so in the open bite group. In addition, the ramus height is short in patients with open bite whereas it is long in those without open bite, as is the case of our patient. Shortening a long face of an individual with VME is challenging and generally requires an approach combining both orthodontic treatment and orthognathic surgery.6,7 The literature has revealed that surgical impaction of the maxilla aids in the correction of VME, anterior open bite, and in obtaining a competent lip seal.8,9 The superior repositioning of the maxilla following LeFort I osteotomy is considered the most stable orthognathic surgical intervention,10,11 and it was initially performed by Converse in 1952 12 by posterior intrusion for the management of patients with open bite. However, it can also be performed anteriorly in patients presenting with a gummy smile. 13 Since treating lip incompetence and excessive teeth exposure is a priority in patients with VME, it is important to determine the amount of maxillary impaction necessary to achieve optimal functional and esthetic results. In a previous study, it was shown that approximately 2 mm of maxillary incisors are visible with the lips at rest. 14 In addition, it is predicted that the upper lip moves upward one-fifth or 20% the amount of the superior repositioning of maxillary incisors during surgery.2,3 In our case, the distance between the upper lip and upper central incisor edge was approximately 8 mm. Thus, the maxillary incisors must be moved 6 mm upwardly leaving 2 mm of tooth showing after surgery. However, since the upper lip will be shortened roughly by 1.2 mm, we have decided to perform a maxillary impaction by 7–8 mm. The superior repositioning of the maxilla and upper teeth results in a counter-clockwise rotation of the mandible thereby shortening the facial profile still further and making the chin more prominent. 3 The autorotation of the mandible associated with the maxillary impaction was initially advocated by Schendel et al., 15 Bell et al., 7 and Fish et al. 2 Mandibular autorotation following a maxillary surgical impaction is associated with the projection of the chin forward and shortening of the lower face. It was observed that the amount of mandibular autorotation is proportional to the amount of maxillary impaction; with every 1 mm of maxillary superior repositioning, the chin would move 0.6 mm vertically and 0.2 mm horizontally. 13 Another study revealed that an average of 5 mm-maxillary impaction would lead to a 2 mm advancement and 1.2 mm shortening of the chin when using the condyle as center of rotation for mandibular autorotation in the cephalometric predictions. 16 In our case, the maxillary impaction was combined with a BSSO for mandibular anterosuperior movement to further shorten the lower face and improve chin projection. Subsequently, the maxilla had to be repositioned slightly forward during surgery to maintain the same occlusion. In the medical literature, there is still controversy concerning the effects of orthognathic surgeries (OGS) on the TMJ. The signs and symptoms of TMD are more prevalent in patients with dentofacial anomalies than normal population. This prevalence can be explained by different factors including stress, functional impairments between the components of the masticatory apparatus and parafunctional habits such as grinding or clenching. 17 OGS particularly those involving mandibular osteotomy can directly affect the TMJ. 18 A previous study 19 showed that patients with preexisting TMD undergoing orthognathic surgery are expected to have appreciably improved signs of TMD as is the case of our patient who reported the disappearance of clicking sounds after surgery. Different factors can account for this improvement in TMD symptoms post-operatively notably the correction of malocclusion, the decrease in emotional stress related to skeletal deformity, 19 and the benefits of surgical procedure on muscles of mastication. 20 The etiology of TMD is multifactorial with malocclusion being a risk factor. Although, the role of occlusal factors in the development of TMD is minor (10%–20%), 21 establishing occlusal stability with good intercuspation of teeth after surgery can help explain the favorable effect of OGS on TMD symptoms. Other possible explanations include improvement in disc–condyle relationship, increase in neuromuscular coordination, and improvement in psychological status due to better function and appearance. 17 While orthognathic correction of dentofacial anomalies can ameliorate the symptoms of TMD, few studies have reported the worsening in TMD after surgery.17–19 Therefore, the relief or deterioration of TMD symptoms cannot be predicted before surgery. 20 However, placing excessive pressure of the articular disc by placing the condylar head in a posterior–superior position during surgery can potentially result in the onset of TMJ symptoms or the worsening of preexisting TMD. 18 Orthodontically induced apical root resorption (OIRR) is an undesirable and often inevitable complication of orthodontic tooth movement. When severe, it can lead to an unfavorable crown-to-root ratio of the teeth. Research indicates that OIRR arises from a combination of individual susceptibility and mechanical factors. In our case, apical root resorption (RR) was observed in the upper and lower anterior teeth. Several investigators have suggested, that OIRR most frequently affects the upper incisors especially the laterals because they often have small or pipette-shaped roots.22–24 A previous study 25 found that 74% and 82% of the central and lateral incisors exhibited clinically significant root resorption (more than 1 mm) after 12 months of active treatment. In our case, treatment variables associated with RR were most likely treatment time and the use of rectangular archwires. First, the prolonged duration of treatment can increase the risk of root resorption.22,26,27 For our patient, the treatment time was extended due to the postponement of surgery for several months as a result of the COVID-19 pandemic. This delay inadvertently prolonged the duration of orthodontic treatment, potentially exacerbating the risk of root resorption. Second, the use of heavy stainless steel wires during the IMF phase may have contributed to the observed root resorption. These archwires exert greater forces on the teeth, which can lead to increased stress on the root surfaces and subsequent resorption.
Conclusion
Maxillary impaction via LeFort I osteotomy has proved to be the treatment of choice for the management of individuals with VME. Combining this surgery with a BSSO for mandibular anterosuperior derotation allowed the reduction of lower facial height and helped establish a good balance between upper lip and maxillary incisors. As a result, the lip incompetence was corrected and the gummy smile was significantly improved. In addition, the TMD symptoms were resolved after surgery and the patient’s facial proportions looked more balanced.
Footnotes
Acknowledgements
Not applicable.
Author contributions
The authors confirm contribution to the paper as follows: M.B. contributed to data collection and writing the draft manuscript; S.T., R.M. contributed to supervision and validation; A.B.A., I.D., W.B.A. contributed to supervision, review and editing.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for his anonymized information to be published in this article.
