Abstract
Employing percutaneous nephrolithotomy to manage a complex renal calculus has always been challenging due to the blood transfusion requirement and the frequent necessity of using multiple access tracts. We report a novel treatment modality in the case of a 65-year-old male with a complex, large-volume renal calculus who was successfully treated by vacuum-assisted miniaturized endoscopic combined intrarenal surgery using the combination of a thulium fiber laser in retrograde fashion with a holmium:YAG laser in antegrade fashion. The kidney stone was entirely cleared, and the patient fully recovered with no adverse event.
Introduction
To date, treatment strategies in the management of urolithiasis are mainly based on minimally invasive procedures, with a preference for endourologic techniques, which include extracorporeal shock wave lithotripsy, retrograde intrarenal surgery, and percutaneous nephrolithotomy (PCNL).1,2 PCNL is the procedure of choice for eliminating large (>2 cm) and complex renal stones, but achieving complete stone clearance in a single approach may require using multiple access tracts.3,4 The large number of tracts and the need for renal parenchymal manipulation leads to more kidney parenchymal injuries, requires PRC transfusion, and sometime contributes to various serious complications, such as uncontrolled hemorrhage and massive hemothorax.5,6
As a result of better quality of vision technology, miniaturization of instruments, and the implementation of artificial intelligence, the procedure to remove a complex kidney stone has evolved.7,8 Miniaturized endoscopic combined intrarenal surgery (mini-ECIRS) is a new surgical treatment that has won increasing acceptance globally. To the best of our knowledge, we report the first known case of complex renal stone management using vacuum-assisted mini-ECIRS with a combination of two laser types—a holmium:YAG (Ho:YAG) laser and a thulium fiber laser (TFL)—to take optimal advantage of the distinct characteristics of the two lasers in the same procedure.
Case report
A 65-year-old male patient presented at our clinic with intermittent left flank pain. His mental and physical health were excellent. A urine examination revealed no pyuria and negative urine cultures. The blood creatinine level was 1.0 mg/dL. Computerized tomography revealed a large renal pelvis calculus measuring 37 × 30 × 18 mm (Figure 1(a)) with one group of small, lower-pole calyceal calculi of 14 × 15 × 16 mm in size (Figure 1(b)). The average density of the stones was 1500 Hounsfield units. Following a comprehensive discussion of the treatment plan, the patient was scheduled for a vacuum-assisted mini-ECIRS procedure using a combination of TFL and Ho:YAG lasers.

Computerized tomography scan illustrating a (a) renal pelvis calculus (b) lower pole calculus.
Intravenous cefuroxime was administrated as a prophylactic antibiotic during the induction phase of general anesthesia. The patient was arranged in the Galdakao-modified supine Valdivia (GMSV) position, with his left flank raised by placing two 500 ml saline bags behind his chest and buttocks and his leg fixed in an asymmetrical lithotomy position. Two urologists used two operating instruments simultaneously; one used a miniature nephroscope and the other a flexible ureteroscope (fURS).
The first urologist began performing retrograde pyelography cystoscopically to delineate the ureter and pelvicalyceal system. A single-use digital fURS (Scivita Medical Technology, Jiangsu, China) was introduced without difficulty into the kidney through the access sheath. To prevent injury, the second urologist performed ultrasonography to detect organs possibly located between the puncture site on the skin and the kidney. The lower calyx was punctured using an 18-gauge nephrostomy needle, employing the triangulation technique under fluoroscopic guidance. Tract dilation was achieved over the guidewire using a single-step dilator, establishing a working route with a 16 Fr ClearPetra disposable nephrostomy sheath (Well Lead Medical Co., Ltd, Guangzhou, China). Laser lithotripsy was performed using the fragmentation technique through a 12 Fr nephroscope MIP-M system (Karl Storz, Tuttlingen, Germany) with a 120 W Ho:YAG laser (Lumenis, San Jose, CA, USA) and a 550 μm core laser fiber with an energy of 1.5 J and a rate of 30 Hz (Figure 2(a)). The fURS laser lithotripsy was performed with a 60 W thulium fiber system (SOLTIVE, Olympus, MA, USA) and a 200 μm laser fiber with the settings of 1.5 J and 30 Hz (Figure 2(b)). The stone fragments were removed with graspers or were evacuated and washed out using a suction system through the nephrostomic sheath. At the end of the procedure, a 6 Fr ureteral stent was placed retrogradely. The operation lasted 80 min and the laser time was 15 min. An abdominal x-ray was obtained to identify residual fragments and confirm the appropriate positioning of the ureteral stent (Figure 3). The patient made an uneventful postoperative recovery. The stent was removed cystoscopically at 6 weeks after discharge. The patient’s 3-month follow-up showed no clinical abnormalities.

(a) Miniature nephoscope view of the renal calculus; (b) Flexible ureteroscope view of the renal calculus.
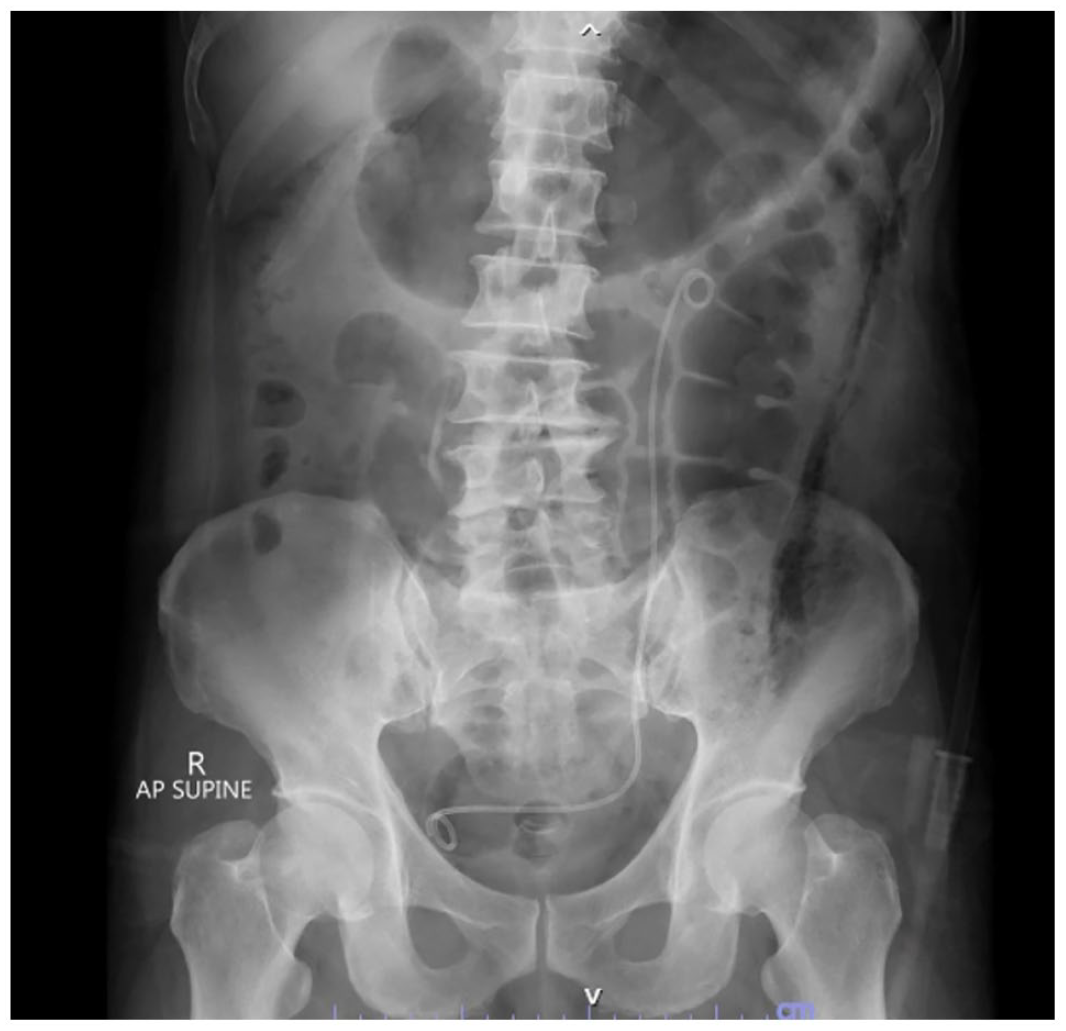
Postoperative abdominal plain radiography showing no evidence of residual calculi.
Discussion
Mini-ECIRS that combines miniature PCNL and retrograde intrarenal surgery is gaining popularity worldwide for the treatment of complex upper urinary tract calculi. This synergistic approach can effectively retrieve any urolithiasis while arranging the patient in only the GMSV position and accessing the organ only once.9,10 Furthermore, implementing the endo-vision puncture technique using fURS enables surgeons to directly visualize and adjust the percutaneous puncture of the desired calyx and to monitor the access tract and ensure sufficient dilatation. This approach is associated with shorter hospital stays, reduced postoperative pain, and fewer postoperative adverse events compared to using PCNL alone.11,12 In our case, we also performed a tubeless procedure, which promoted the patient’s early ambulation and quick, safe discharge on the third post-operative day.
The Ho:YAG laser with no pulse modification remains the gold standard laser in daily urological practice, but the TFL, which uses a long silica fiber doped with elemental thulium to generate the laser beam, is a novel laser technique with ideal physical properties for use in stone lithotripsy and prostate enucleation. 13 When directly compared with Ho:YAG, the TFL technology contributes a more efficient laser energy in terms of dusting, with an ablation rate up to three times higher and a retropulsion value around three times lower. 14 The TFL exhibits a significantly higher absorption coefficient for water and a more concentrated beam. Additionally, it enables a higher maximum pulse repetition rate of up to 2000 Hz, allowing for faster, more precise treatment, making the TFL very useful when incorporated with fURS. In terms of peak power and pulse shape, the Ho:YAG’s peak power is greatly variable and still high, whereas the TFL demonstrates an almost rectangular flat-top pulse shape with a nearly fixed low peak power in various settings. 15 For breaking a stone using a miniature nephroscope, fragmentation lithotripsy remains a mandatory technique for which Ho:YAG may be superior in this setting. Thus, our patient received the optimized benefit of two types of laser as shown by the short laser time.
Conclusion
This report described an optimum use of both TFL and Ho:YAG lasers to break a complex kidney stone in vacuum-assisted mini-ECIRS, a technique that yielded a successful outcome in terms of complete stone clearance, short laser time, and a favorable safety profile for the patient.
Footnotes
Acknowledgements
The authors appreciate Yada Phengsalae for aiding in manuscript preparation.
Author contributions
All authors contributed equally to the article and read and approved the final version of the article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval to report this case was obtained from institutional review board (COA. MURA2023/502).
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Consent for publication
Written informed consent was obtained from the patient to publish this report in accordance with the journal’s patient consent policy.
