Abstract
Congenital proximal radioulnar synostosis limits prono-supination and is often well tolerated. Only one publication in the literature describes a fracture associated with this malformation. We report a case of radius and ulna shaft fractures in a 35-year-old patient with well-tolerated bilateral proximal congenital proximal radioulnar synostosis.
Introduction
Congenital synostosis of proximal radius and ulna (CRUS) is a rare malformation caused by failure of normal prenatal separation of the radius and ulna. 1 Patients commonly present in early childhood with functional deficits because of limited forearm rotation and fixed positioning of the forearm. Compensatory motion and hypermobility are frequently observed at the wrist and shoulder, which may predispose these joints to overuse injury. 2 In most of the cases, this malformation is well tolerated. However, it makes the antebrachial frame vulnerable to torsional trauma.
Case presentation
We report a case of diaphyseal fracture of both left forearm bones in a 35-year-old patient with well-tolerated bilateral proximal congenital radioulnar synostosis. The patient fell from a height of 1 m with a mechanism of forced supination of the forearm. Upon examination, we found an obvious deformity of the forearm, with protrusion of the bony ends without cutaneous effraction.
Range of motion was measured on the uninjured limb and found: 40° pronation, 130° flexion, and full extension. The patient had full active range of motion of both his shoulder and wrist. There was no sign of neurological or vascular compromise. Probing about history revealed previous prono-supination limitation of both forearms, known since childhood, to which he had adapted well. The X-ray showed an oblique fracture of both forearm bones in their middle third, type A3-1 of the AO (Arbeitsgemeinschaft für Osteosynthesefragen) classification. It also revealed a proximal radioulnar synostosis and mainly a tapered aspect to the diaphysis, with agenesis of the radial head (Figure 1). Anatomical reduction and open osteosynthesis using two compression plates were performed. The ulna was approached, first, via a posterior approach and the radius via an anterior Henry approach (Figure 2). Fracture reduction was tricky due to synostosis, which made the proximal fragments poorly mobile. The ulnar shaft was small in diameter with a very narrow medullary cavity. Therefore, we were very careful in the use of holding forceps. Exposure of the radius was difficult and hampered by the impossibility of placing the proximal segment in supination.
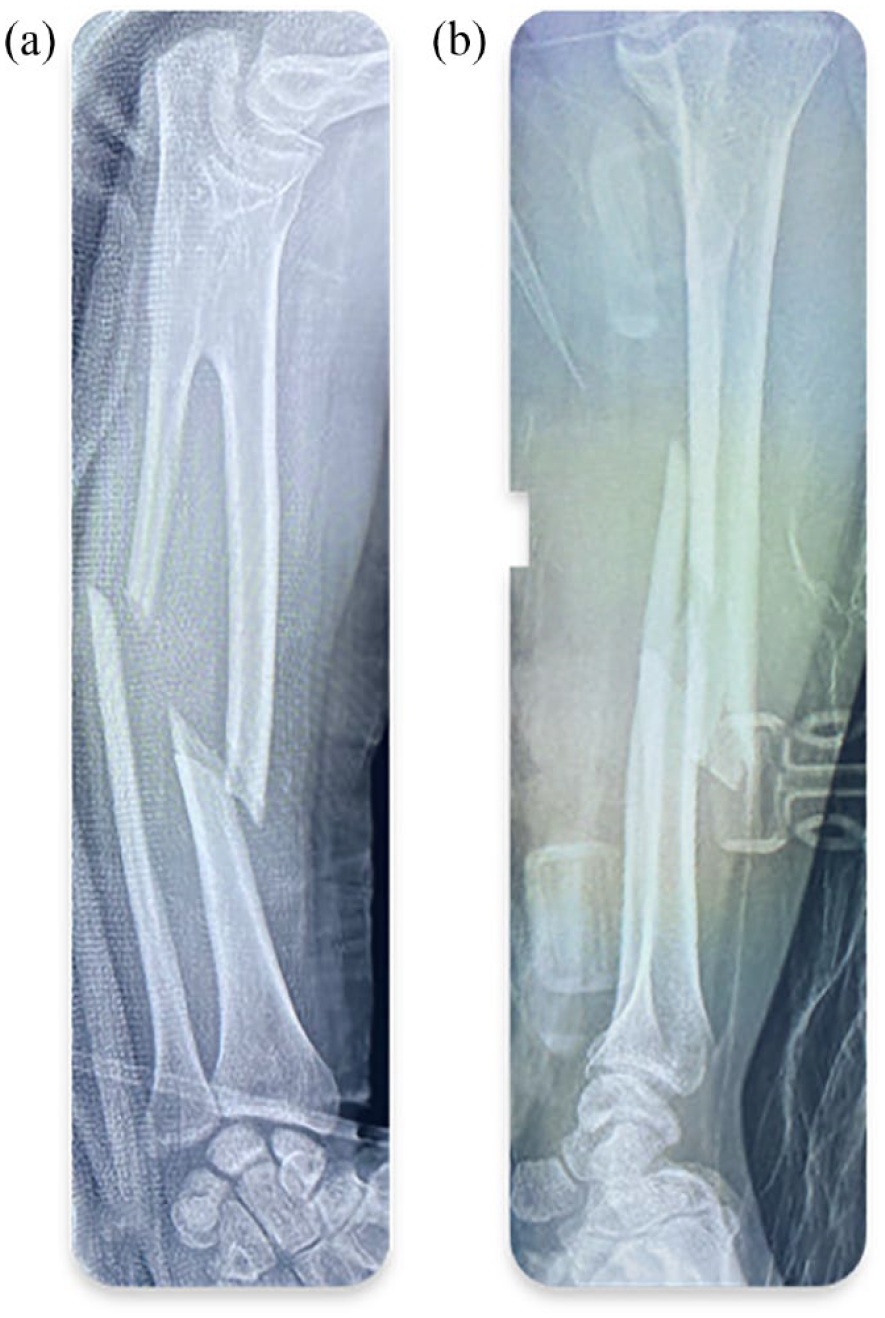
Oblique fracture of the radius and ulna. (a) Front view. (b) Profile view.

Postoperative radiographs.
The limb was immobilized with a posterior elbow splint for 4 weeks, followed by rehabilitation. Postoperative follow-up was simple. Consolidation was obtained after 3 months. The patient regained his initial joint amplitudes: 40° pronation, 130° flexion, and full extension.
Discussion
The first case of radioulnar synostosis was described in 1796 by Mital 3 and fewer than 400 cases have been reported in the literature. The persistent connection between the radius and ulna is nearly always proximal; while distal radioulnar synostosis is extremely rare. 4
CRUS malformation leads to a limitation of prono-supination. The wrist is fixed in variable degrees of pronation with no possibility of supination.
When the forearm is fixed at less than 30° of pronation, there is little functional limitation, due to compensation by rotation around the shoulder and wrist. 5 Beyond 30° of pronation, limitations are individual dependent. In our case, the patient had refused surgical correction because he has no objective or functional limitations of movements in spite of having severe degree of synostosis. Treatment options for CRUS are limited to surgery but the indications remain not clear. 6 However, most clinicians agree that any forearm fixated beyond 70° of pronation must be operated early in childhood. 7 The most dependable option is rotational osteotomy through the synostosis. 8 More recently, Mal-Lawane performed 12 percutaneous rotation osteoclasis procedures of the antebrachial skeleton in young children. They had very satisfactory esthetic outcome with no cases of vascular or nervous complications. 9 In a recent systematic review, Barik S noted that most of the complications occurred above the threshold of 65–70° of correction and in children 7 years and above. 10
CRUS appears to be a benign malformation. Though, it makes the antebrachial frame both rigid and vulnerable to torsional stress. To our knowledge, only one case of CRUS, associated with a fracture of both forearm bones, has been described. 11 In our case, the trauma was of low kinetic energy, resulting in fracture of both diaphysis, which were narrow and fragile. The fracture was treated with a solid compression plate after anatomical reduction.
No attempt should be made to recover further joint amplitude, but it is recommended that the forearm be returned to its ankylotic position.
Patients with CRUS are at high risk of forearm fractures resulting from minimal trauma. It is therefore preferable to avoid contact sports in these patients, especially activities requiring prono-supination.
Conclusion
CRUS is a rare malformation, causing variable functional discomfort and a risk of fracture during torsion movements. The tapered nature of the diaphysis and poor exposure make the treatment of forearm fractures associated with CRUS challenging.
Footnotes
Author contributions
A. N. researched literature. S. Y. wrote the first draft of the article. M. S. B. reviewed and edited the article and approved the final version of the article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
This case report received ethical approval from our institution. The patient was given consent form before the surgery.
Informed consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Trial registration
Not applicable.
