Abstract
Renal papillary hypertrophy is a rare variation that mimics upper tract urothelial carcinoma. This is the ninth case in literature. It causes hematuria and pain, or it could be asymptomatic. It is important to distinguish this variation from malignant masses since misdiagnosis leads to unnecessary radical surgery. Flexible ureteroscopy helps distinguish malignant from benign masses, particularly in cases where there is not a consensus on the exact pathology of the mass. We present a 46-year-old female who came with hematuria and was planned to undergo radical nephroureterectomy under the impression of renal cell carcinoma based on imaging studies. After flexible ureteroscopy, renal papillary hypertrophy was confirmed and radical nephroureterectomy was prevented.
Introduction
Distinguishing benign and malignant masses mimicking upper tract urothelial carcinoma (UTUC) is important since standard management of UTUC is radical surgery, and misdiagnosis may lead to unnecessary radical nephroureterectomy (RNU). Renal papillary hypertrophy is a rare cause of hematuria that mimics UTUC, with only a few reported cases.1,2 Flexible ureteroscopy (F-URS) is a procedure that involves a flexible scope inserted inside the urethra that can help to diagnose (diagnostic or d-URS) and treat upper urinary tract problems, including stones and suspicious masses. It provides urologists with precise information about the number, size, and location of masses, so it helps distinguish benign from malignant ones, especially when other studies remain inconclusive. 3 We report a female patient who came in with hematuria. The plan was to undergo RNU based on imaging studies. F-URS was done to assess the mass and renal papillary hypertrophy was the final diagnosis; hence, radical surgery was not performed.
Case presentation
A 46-year-old heavy smoker female came with a complaint of painless intermittent gross hematuria and occasional flank pain. Her past medical history was unremarkable and had no family history of the genitourinary or malignancy-related disease. She did not take any medication. UA (Urinalysis) was unremarkable except for 5–10 red blood cells (RBCs). Both urine culture and urine cytology came as negative. Imaging studies such as sonography, magnetic resonance imaging (MRI), intravenous pyelogram (IVP), and computed tomography (CT) scan were done. CT scan showed a solid nodular iso-dense mass in the middle calyx of the left kidney with the interpretation of highly suspicious transitional cell carcinoma (TCC; Figure 1a and b). MRI showed a round mass or cyst being either Squamous Cell Carcinoma (SCC) or parapelvic cyst (Figure 2). Sonography showed a hypodense mass in the middle of the left kidney being either TCC or reninoma (Figure 3). IVP showed a noninvasive mass with the interpretation of renal cell carcinoma (RCC). The patient was planned to undergo RNU in another center with suspicion of RCC to which she did not agree. Finally, she was referred to our center, and based on the inconclusiveness of imaging studies, we decided to perform an f-URS with a 9.4-F ureteroscope. Ureteroscopy showed multiple masses with small blood clots in the middle calyx of the left kidney (Figure 4) https://www.aparat.com/v/0LS9l. Biopsies were taken from the tumor-like mass (Figure 5); however, the pathologist could not find any tissue so instead reported the cytology, which was negative. Therefore, she did not receive further treatment. Fifteen months after f-URS, the patient is alive, asymptomatic, and no growth was seen in her last follow-up sonography. Informed consent was obtained in both written and verbal format from the patient to report this case.

(a) CT scan. The 17 × 12 mm solid nodular iso-dense mass in the middle calyx of the left kidney (shown by an arrow), (b) CT scan, coronal cut (17 × 12 mm mass).

MRI image of the mass (12 × 11 × 13 mm); the dimensions are reported in the MRI report.
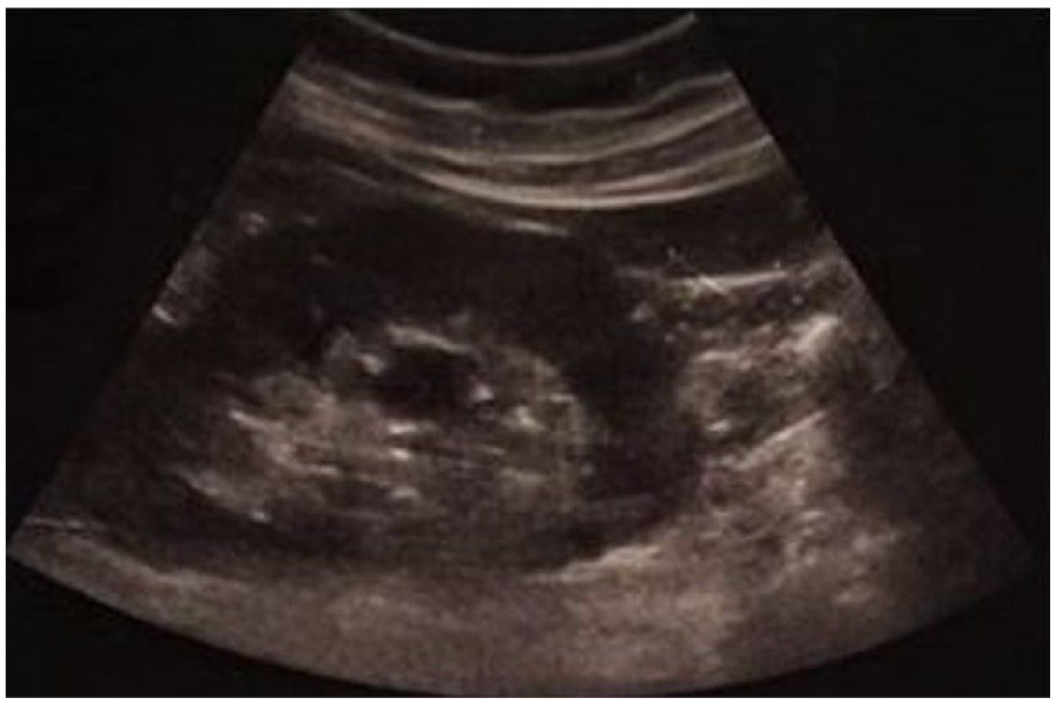
Sonography showing the 18 × 13 mm hypoechoic mass.
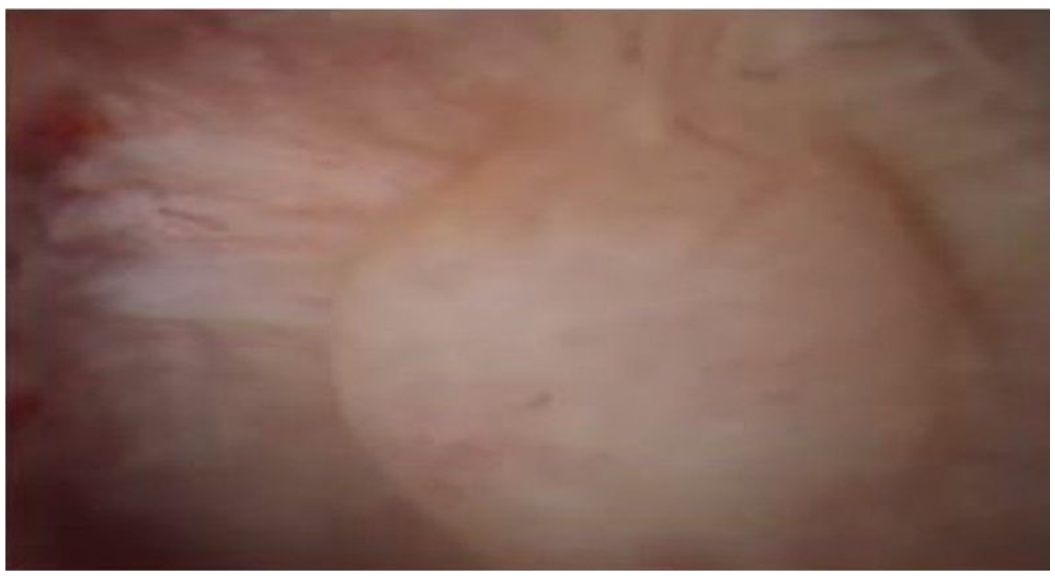
One of the multiple masses seen on ureteroscopy.

Taking a biopsy from one of the masses.
Discussion
Renal papillary hypertrophy is a rare variation, causing filling defects with concave impressions on the surrounding calyx which mimics UTUC.1,2 So far, only nine cases have been reported. 1 In pathological studies, hyperplasia of the renal papilla with normal histology is seen. 1 Also, nodular calcified papillary structures were seen. 4 They can be multiple, bilateral, or unilateral. Its main symptom is hematuria, gross, or microscopic; others include flank or loin pain; or it could be asymptomatic. 1 Other cases reported normal ultrasound; however, ours was hypoechoic. It affects people from 9 months to 30 years old; however, our patient was 46 years old. By far, seven females and two males have been reported. There seems to be an association between this condition and the use of contraceptive medication; however, the data are inconclusive.1,4 Our patient was a heavy smoker which may contribute to this condition. Hematuria may be a result of dilated thin-walled veins at the angle of affected calyces. 1
Studies show biopsy could be omitted if there are multiple masses with negative cytology and no other abnormal findings. 1
Management includes laser ablation with holmium–yttrium-aluminum-garnet (YAG) or thallium-YAG in symptomatic patients or close follow-up for asymptomatic patients. 4 Previous cases recommended follow-up every 4 months plus CT or MRI twice in the first year. 4 If the patients become symptomatic or a change in size is detected, laser ablation or retrograde intrarenal surgery is recommended. 4 The symptoms may resolve by themselves.
Radiologists and urologists should be familiar with this variation as it can prevent unnecessary radical surgery. Other benign conditions that mimic UTUC include clots, renal papillary necrosis, cystic pyelonephritis, fibroepithelial polyp, wall thickening due to inflammation, and urogenital tuberculosis (TB). 2 Shin et al. reported that 17% of the resected tumors were benign, and the resection was indicated by CT imaging. CT scan identified almost 35% of benign masses as highly suspicious RCC. They also stated a significant difference between preoperative CT diagnosis and final histopathological findings. 5 When there is a lack of consensus between different studies, a d-URS biopsy is recommended, as data show it can prevent unnecessary RNU and is significantly associated with lower rates of RNU and misdiagnosis. Also, d-URS has similar sensitivity and greater specificity compared with CT scans. 3 Our case shows the importance of using f-URS in cases where other studies including imaging remain inconclusive on the pathology of the UTUC mimicking mass.
Conclusion
This case shows the importance of f-URS and d-URS in distinguishing malignant and benign masses, especially when radiological studies are inconclusive, and a wrong diagnosis can lead to unnecessary radical nephrectomy.
Footnotes
Acknowledgements
We would like to thank Kasra Hospital for providing us with the needed documents.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The case report is adhered to CARE guideline to report the case, and our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Informed consent was obtained in both written and verbal format from the patient to report this case.
