Abstract
Microblading is a novel method of semi-permanent makeup, which has achieved popularity in the last few years. We present the case of a patient who developed cutaneous sarcoidosis after microblading of her eyebrows. A 45-year-old female presented with a 6-month history of pruritic erythematous granulomatous plaques on bilateral eyebrows corresponding to the site of microblading 1.5 years prior. A tissue biopsy was preformed which was consistent with cutaneous sarcoidosis. An extensive work-up including assessment by respirology, rheumatology, and ophthalmology did not reveal any evidence of systemic sarcoidosis. The patient was treated with intralesional triamcinolone injections and tacrolimus ointment twice daily, with complete resolution. To our knowledge, this is the first case of cutaneous sarcoidosis associated with microblading in the literature. Dermatologists should be aware of popular and novel cosmetic procedures and the potential complications that arise from these interventions.
Introduction
Microblading, also known as eyebrow feathering/eyebrow embroidery, is a method of semi-permanent makeup, which has achieved popularity in the last few years. 1 Using this technique, pigment is introduced into the skin until the level of the papillary dermis using linear rows of needles.1,2 This technique results in the appearance of natural feathery-appearing hairs.1,2 Although most commonly used for eyebrow pigmentation, this technique has also been employed in scalp pigmentation for alopecia. Unlike traditional permanent tattooing, pigmentation lasts 1–3 years, largely due to the shallower depth of pigment deposition.1–3 Several risks have been associated with this cosmetic procedure including allergic contact dermatitis and skin and soft tissue infections. 2 We present the case of a patient who developed a cutaneous sarcoidosis to microblading of her eyebrows.
Case report
A 45-year-old female presented with a 6-month history of a pruritic erythematous granulomatous plaques on the bilateral eyebrows corresponding to the site of microblading 1.5 years prior (Figure 1). She had a prior medical history of hypothyroidism and migraines which were being managed with levothyroxine and eletriptan, respectively. Physical examination showed firm erythematous to beige granulomatous linear plaques affecting the length of bilateral eyebrows. A punch biopsy was performed to evaluate differential diagnoses which included sarcoidosis or allergic contact dermatitis. Tissue biopsy showed sarcoidal granulomas throughout the dermis with multinucleated giant cells. There was stippling of exogenous pigment throughout, which was more prominent within superficial macrophages. Spongiosis was also identified in the epidermis. The patient was also referred for allergic patch testing using Chemotechnique diagnostics’ North American 80 Comprehensive series, which identified a 2+ reaction to 4-tert-butylphenol formaldehyde resin. This allergen is a shoe adhesive used to glue leather parts together and is unrelated to dyes used in microblading. Her presentation was consistent with cutaneous sarcoidosis, and the patient was treated with intralesional triamcinolone 2.5 mg/mL injections and tacrolimus 0.1% ointment twice daily as needed, with complete resolution (Figure 2).

Baseline photos before treatment on 9 October 2019.

Photos after treatment on 4 November 2020.
A work-up for systemic sarcoidosis was subsequently preformed. The patient denied symptoms of systemic sarcoidosis including fever, night sweats, chills, ocular irritation/dryness, oral ulcers, chest pain, or shortness of breath. However, she endorsed arthralgia in wrists with morning stiffness lasting longer than 30 min. The results of hematological, biochemical, and inflammatory tests were unremarkable aside from Anti-ds DNA, which was found to be borderline positive with titer of 5. She had normal renal function, and there was no evidence of hypercalcemia. Imaging results including chest X-ray, echocardiogram, and X-rays of the hands, knees, ankles, and feet were unremarkable, suggesting no systemic involvement. She was seen by respirology who found no evidence of pulmonary sarcoidosis. She had normal pulmonary function tests (PFTs) with Diffusion Capacity of the Lungs for Carbon Monoxide (DLCO). She was referred to ophthalmology who found no evidence of ocular sarcoidosis. She was seen by rheumatology who found no evidence of internal or joint involvement. At one-year follow-up, there were still no signs of systemic sarcoidosis.
Discussion
Cutaneous sarcoidosis following tattooing has been described numerous times in the literature. 4 We performed a literature review of cases of cutaneous eyebrow sarcoidosis in the context of permanent or semi-permanent cosmetic tattooing. The results of this review are summarized in Table 1. In total, there were 21 cases (15 studies) identified in the literature. All of the identified cases occurred after permanent eyebrow tattooing. There were no cases of cutaneous sarcoidosis described following microblading (semi-permanent method) of the eyebrows. Onset of tattoo sarcoidosis from permanent or semi-permanent pigmentation varied significantly from 4 months to 25 years. There were also several cases which developed after multiple tattoo applications.
Summary of literature describing cutaneous sarcoidosis in permanent or semi-permanent cosmetic eyebrow tattoos.
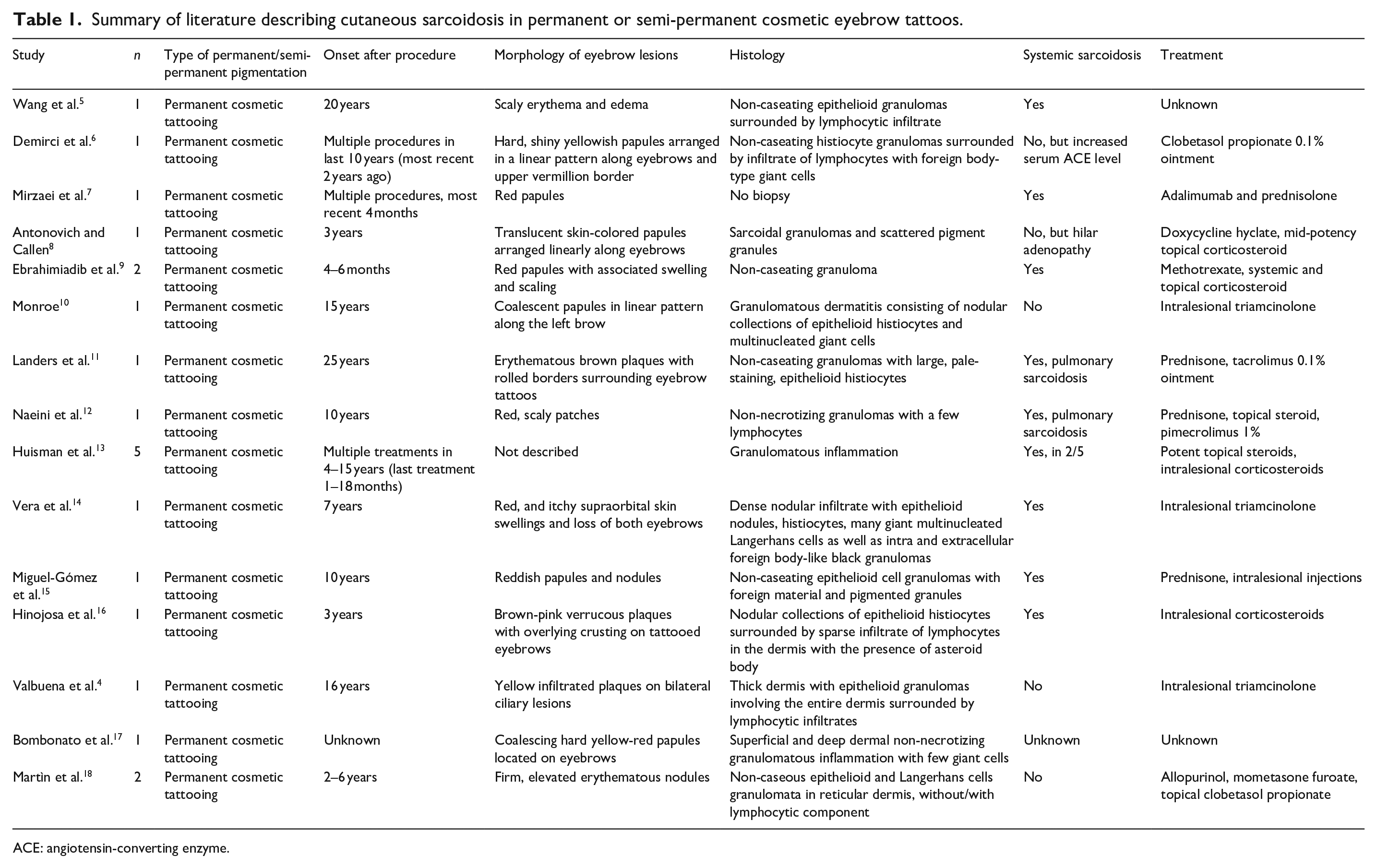
ACE: angiotensin-converting enzyme.
Of the 21 patients with cutaneous eyebrow sarcoidosis, 10 were found to have systemic sarcoidosis, or to subsequently develop systemic sarcoidosis. After full work-up of our patient, there was no evidence of systemic sarcoidosis, which persisted at 1-year follow-up. Nonetheless, several patients with permanent tattoos developed systemic sarcoidosis years after initial presentation with cutaneous sarcoidosis. This may possibly be due to an immune response to ongoing exposure to foreign materials in the skin, which is a known etiology of systemic sarcoidosis.6,12,19,20 However, because the pigmentation in microblading is non-dispersible, and hence difficult to retain for more than a few years, the theoretical risk of this is less than in permanent tattoos.1,21 Nevertheless, in patients who have granulomatous reactions to microblading, it may be reasonable to recommend against future pigmentation to avoid the risk of developing systemic manifestations of sarcoidosis.
To our knowledge, this is the first case of cutaneous sarcoidosis associated with microblading in the literature. With the expansion of the cosmetic procedure industry, dermatologists should be aware of popular and novel cosmetic procedures and the potential complications that arise from these interventions to facilitate appropriate management.22,23 It is also important to note that there is significant influence of social media on the public’s interest in cosmetic procedures. 24 As such, the focus of future research should be to characterize social media and public interest in cosmetic procedures and to outline the medical considerations for these procedures.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Patient provided written informed consent to publish case report and images.
