Abstract
Background:
Scabies is one of the major neglected tropical diseases among children in deprived communities. Studies conducted among schoolchildren in Africa are limited and inconsistent. Thus, the aim of this study is to estimate the pooled magnitude and predictors of scabies in African schoolchildren.
Methods:
The pooled prevalence estimate with 95% confidence intervals was performed using a random-effects model. Heterogeneity between studies was assessed using the I2 statistic. Subgroup analyses and sensitivity analyses were performed to explore potential sources of heterogeneity. Publication bias was evaluated using the funnel plot, Begg’s, and Egger’s tests.
Results:
A total of 28,482 subjects from 19 studies were included. The pooled prevalence of scabies among African schoolchildren was 10.81% (2459/28482) with (95% CI: 7.10–14.51). Factors such as being male (aOR = 1.86; 95% CI: 0.72–3.01), children who have a history of sharing clothes with their family (aOR = 1.76; 95% CI: 0.62–2.91), having illiterate parents (aOR = 0.96; 95% CI: 0.51–1.41), having history of contact with skin itching cases/scabies (aOR = 3.37; 95% CI: 1.70–5.03), infrequent cloth wash (aOR = 5.30; 95% CI: 1.26–9.34), sharing common sleeping beds/fomites (aOR = 2.13; 95% CI: 0.04–4.22), family member with itchy signs/scabies (aOR = 5.83; 95% CI: 1.45–10.21), and not taking a bath with water and soap (aOR = 8.51; 95% CI: −4.14 to 21.15) were factors associated significantly with scabies.
PROSPERO registration:
CRD42024542762.
Conclusion:
In the present scenario, scabies ranges from 2.0% to 17.80% and is higher in Cameroon. Therefore, policymakers and health planners should put a great deal of emphasis on the implementation of relevant prevention and control measures.
Introduction
Human scabies is a parasitic skin infection caused by tiny mites called Sarcoptes scabiei var. hominis that burrow into the skin and cause itching and a rash.1,2 Scabies can cause rashes on different parts of the body, with the specific areas affected varying depending on a person’s age.2–5 Scabies is a prevalent skin disease that affects a large number of people globally but is most common in developing nations and tropical regions, impacting individuals of all ages, from babies to the elderly. Children and older people in resource-poor areas and tropical countries with high population density are at increased risk.
Symptoms of scabies infestations include superficial burrows, severe itching, which worsens during the night, and a widespread rash that can cover a large part of the body or be contained to specific areas like finger webspaces, the wrist, elbow, armpit, penis, nipple, waist, and buttocks. 6 Bacterial superinfection is common in scabies skin lesions and, if left untreated, it can lead to infection of deep structures, septicemia, rheumatic fever, and renal failure. 7 Moreover, scabies causes intense itchiness in school kids, which can create significant emotional and health challenges like feelings of embarrassment, exclusion, fatigue, school absenteeism, loss of performance at school, lack of concentration or memory, intellectual disability, bipolar disorder, trouble focusing, and sleep disturbances.8,9 Scabies and its associated problems have a substantial financial impact on individuals, families, communities, and healthcare systems.10,11
Globally, over 200 million people are affected, with a prevalence ranging from 0.2% to 71.4%. 12 Reports from schools in Malaysia, 13 Turkey, 14 and Thailand 15 yielded a prevalence of 31%, 33%, and 87.3%, respectively, and 61%–62% in Bangladesh. 16 Several pieces of evidence from the literature show that the prevalence of scabies in African countries is persistently high. Scabies research carried out at schools showed 4% in Mali, 17 0.7% in Malawi, 17 and 8.3% in Kenya. 18 Moreover, the prevalence of scabies is 5.2% in Guinea-Bissau, 19 15.9% in Gambia, 20 2.9% up to 65% in Nigeria,21,22 and 2.5% to 78.4% in Ethiopia.23,24
Epidemiological studies have shown the associated factors with the prevalence of scabies infestations are poor hygiene, poverty, overcrowded living conditions, family history of scabies, sharing beds or clothes, younger age, male sex, big families, lack of knowledge about scabies, parent illiteracy, low household income, residency in rural areas, the existence of livestock or rodents at home, seasonal conditions, and movement to contaminated areas.25,26 In Africa, scabies is driven by events like flooding, drought, civil war and conflict, poor water supply and sanitation, and overcrowding living conditions. 27
Africa’s unique geographical location, climate, and cultural features create ideal conditions for various parasites to thrive. 28 Understanding the burden and distribution of scabies is crucial for developing effective prevention strategies. In recent years, there has been a rise in research on scabies epidemiology, with a meta-analysis in Ethiopia revealing a prevalence of 14.5%. 29 However, no systematic review specifically focusing on the prevalence of scabies among schoolchildren in Africa has been carried out. To address this gap, the current study aims to analyze existing data to provide up-to-date and reliable estimates that can inform prevention and control measures across the continent.
Methods
Design and protocol registration
This systematic review and meta-analysis was designed to estimate the continental pooled prevalence of scabies among schoolchildren in Africa. The result was reported following Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guideline 30 (see Supplemental File 1). The review protocol was registered in the International Prospective Register of Systematic Reviews (PROSPERO) under registration number CRD42024542762.
Search strategy
Five databases (PubMed (Medline), Google Scholar, Scopus, Science Direct, and African Journals Online) were used to retrieve published and unpublished works. Language and time restrictions were not taken during the search for studies, and all published and unpublished studies up to June 2024 were included. We looked through reference lists of articles to find studies that were not accessed in online databases. We searched studies using different terms alone or together, using words like “OR” or “AND.” The search keywords used were “prevalence,” “associated factors,” “contributing factors,” “predictors,” “Sarcoptes scabiei,” “scabies,” “child,” “schoolchildren,” “children,” “Africa,” “Nigeria,” “Ethiopia,” “Egypt,” “Democratic Republic of the Congo (DRC),” “Tanzania,” “South Africa,” “Kenya,” “Uganda,” “Sudan,” “Algeria,” “Morocco,” “Angola,” “Ghana,” “Mozambique,” “Madagascar.” “Côte d’Ivoire,” “Cameroon,” “Niger,” “Mali,” “Burkina Faso,” “Malawi,” “Zambia,” “Chad,” “Somalia,” “Senegal,” “Zimbabwe,” “Guinea,” “ Rwanda,” “Benin,” “ Burundi,” “Tunisia,” “South Sudan,” “Togo,” “Sierra Leone,” “Libya,” “Congo,” “Central African Republic,” “Liberia,” “Mauritania,” “Eritrea,” “Gambia,” “Botswana,” “Namibia,” “Gabon,” “Lesotho,” “Guinea-Bissau,” “Equatorial Guinea,” “Mauritius,” “Eswatini,” “Djibouti,” “Comoros,” “Cabo Verde,” “Sao Tome and Principe,” and “Seychelles,”
Inclusion and exclusion criteria
To determine which articles to include in this study, we considered a specific set of criteria: (1) observational findings; (2) studied in Africa and reported the prevalence or magnitude of scabies among schoolchildren; and (3) published from 24 February 2015 to 1 June 2024. The exclusion criteria include (1) reviews and case reports; (2) confusing or unclear analysis results; (3) studies out of scope (schoolchildren); (4) studies reporting other skin diseases; and (5) inaccessible works.
Study selection and quality appraisal
All retrieved articles were imported into EndNote X8 (Thomson Reuters, USA). After excluding duplications, the titles and/or abstracts of articles were independently screened by two authors (IA and KT). The authors resolved their dispute by talking it out with AG. A full-text appraisal was conducted on articles that met our research question’s criteria and were considered sufficiently valid. JBI critical appraisal checklist for simple prevalence, 31 case-control, 32 and randomized controlled clinical trials (RCTs) 33 studies were used for quality appraisal using 9, 10, and 13 criteria, respectively. For each question, a score was assigned (yes “for reported,” no for “not reported” or “not applicable,” unclear for “confused reports”); the scores were summarized across the items to achieve a total score of 0–9, 0–10, and 0–13 for simple prevalence, case–control, and RCT studies, respectively. Based on the points they received, the studies were sorted into low, medium, and high-quality categories. Only articles classified as medium or high quality were considered in the meta-analysis (see Supplemental File 2).
Data extraction
Data from studies meeting the necessary criteria were extracted and recorded in an Excel spreadsheet. Information such as the name of the first author, publication year, country, study area (setting), study design, sampling method, sample size, cases, prevalence, and response rate were extracted from the eligible studies (Table 1).
Detailed characteristics of eligible studies.
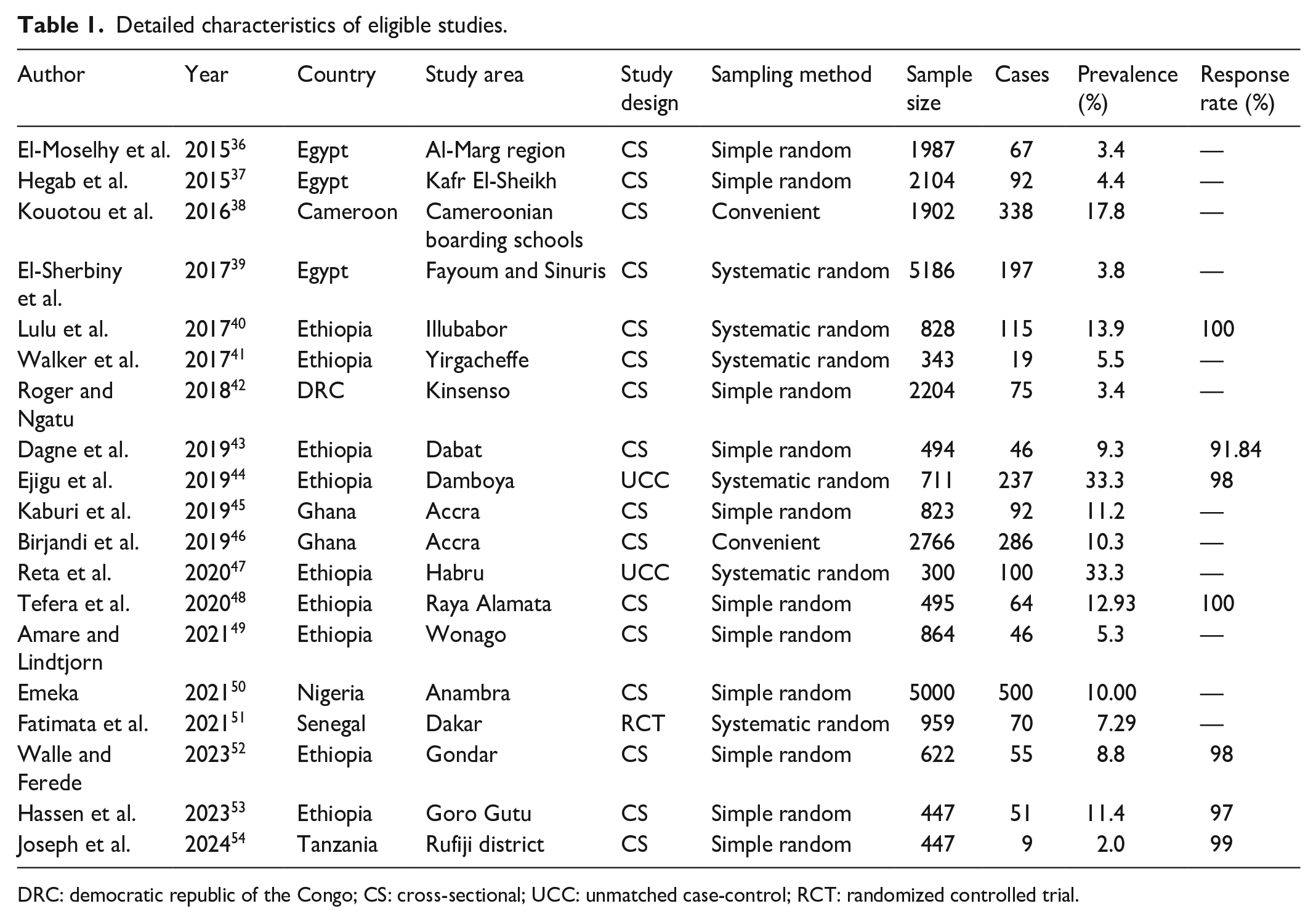
DRC: democratic republic of the Congo; CS: cross-sectional; UCC: unmatched case-control; RCT: randomized controlled trial.
Data analysis
For this meta-analysis, the study utilized STATA version 14 software (StataCorp LLC, College Station, Texas, USA). A random effects model was employed to determine the overall prevalence of scabies, with a 95% confidence interval (CI). The I2 statistics were utilized to gauge the level of heterogeneity among the collected data. A value of 25, 50, or 75 for I2 signifies low, moderate, or high heterogeneity, respectively. 34 Additional examinations were conducted, such as subgroup and sensitivity analyses, to identify potential sources of heterogeneity. To evaluate publication bias within the collected articles, a funnel plot, and Begg’s and Egger’s tests were used. A p-value of less than 0.05 in Begg’s and Egger’s tests indicates a statistically significant presence of publication bias. 35
Results
Selection of studies
The selection process of this study is shown in Figure 1. A total of 1274 articles were retrieved from the five electronic databases. The first 365 articles were removed due to duplicates. Then, 525 articles were excluded after evaluating the title and/or abstract. Another 178 studies were excluded after the full text evaluation. Furthermore, a total of 187 articles were removed due to review articles (n = 20); qualitative studies (n = 23); other skin diseases among schoolchildren (n = 65); out-of-schoolchildren studies (n = 74); and correspondence, proceedings, and letters to the editor (n = 5). In the end, a total of 19 articles were identified as meeting the necessary requirements and were subsequently incorporated into the systematic review and meta-analysis.

Flow diagram summarizing the selection of eligible studies.
Characteristics of included studies
The detailed characteristics of the included studies are summarized in Table 1. The 19 eligible studies were studied in 8 countries. Ethiopia had the highest number of eligible studies (9), followed by Egypt (three studies). Ghana has two studies, and one study was conducted in Nigeria, Senegal, Cameroon, the Democratic Republic of the Congo (DRC), and Tanzania. Sixteen studies were cross-sectional, two were case-controls, and the remaining one was a randomized clinical trial. All studies are school-based, and a total of 28,482 children were involved. The sample size among schoolchildren in the included studies ranged from 300 to 5186.
Pooled prevalence of scabies
The pooled prevalence of scabies among schoolchildren in Africa is 10.81% (95% CI: 7.10–14.51), obtained from 2459 scabies-infested schoolchildren. Substantial heterogeneity was observed in the studies (I2 = 94.7%, p < 0.001) (Figure 2).

Forest plot displaying the pooled magnitude of scabies among schoolchildren in Africa.
Subgroup analysis
A subgroup analysis was conducted due to notable heterogeneity within the data, and the results are shown in Table 2 and in Supplemental File 3. The pooled prevalence of scabies among studies conducted using sample sizes of less than 900 (13.25%; 95% CI: 7.72–18.78) was higher than >900 sample sizes (6.96%; 95% CI: 3.91–10.01). Among African countries, Cameroon had the highest prevalence (17.80%; 95% CI: 12.00–23.60), followed by Ethiopia (14.79%; 95% CI: 8.23–21.34), Ghana (11.01%; 95% CI: 7.45–14.58), Nigeria (10.00%; 95% CI: 2.30–17.70), Senegal (7.29%; 95% CI: 4.14–15.19), Egypt (3.83%; 95% CI: 1.45–6.20), and the DRC (3.40%; 95% CI: −0.65 to 7.45). While the lowest prevalence was observed in Tanzania at 2.00% (95% CI: −0.60 to 4.60). A high overall estimate was observed in case–control studies (33.30%; 95% CI: 30.26–36.34) as compared to cross-sectional studies (7.77%; 95% CI: 5.75–9.78) and randomized clinical trial studies (7.29%; 95% CI: 4.14–10.44). The pooled prevalence estimate of scabies was greater in studies using the systematic random sampling method (16.12%; 95% CI: 5.85–26.38) than in studies utilizing the convenient (14.54%; 95% CI: 7.25–21.82) and simple random sampling methods at 7.05% (95% CI: 4.76–9.34). The pooled prevalence of scabies increases from 6.98% (95% CI: 3.69–10.27) during the period between 2015 and 2018 to 12.90% (95% CI: 7.41–18.39) in the next 6 years (2019–2023). Overall, 19 studies are included in this systematic review and meta-analysis with a total sample size of 28482.
Subgroup analysis on the pooled prevalence of scabies among schoolchildren in Africa.

DRC: democratic republic of the Congo; CS: cross-sectional; UCC: unmatched case-control; RCT: randomized controlled trial.
Quality assessment and publication bias
Details on the quality assessment of each study are found in Supplemental File 2. Briefly, 100% of the included studies were of high quality (low risk of bias). Publication bias was apparent in the included studies since the funnel plot showed asymmetry (Figure 3(a)). In the same way, both Begg and Egger tests, which are based on regression analysis (see Supplemental File 4), indicated that there is a significant presence of publication bias, with a p-value of 0.001. Due to the heterogeneous nature of the studies, we conducted a sensitivity analysis by excluding each study individually to evaluate how each one affected the overall effect size. In the study on scabies among African schoolchildren, the research by Ejigu et al. 44 and Reta et al. 47 played a significant role in affecting the overall outcome. The pooled estimates of 7.67 (6.83–8.51) were recorded after eliminating individual studies at a time, specifically those studies conducted by the abovementioned authors (Ejigu et al. 44 and Reta et al. 47 ). After completely removing those two studies, as indicated in Figure 3(b), the estimate becomes 6.65 (5.80−7.51).

(a) Funnel plot representing evidence of publication bias; (b) Sensitivity analysis result of the involved studies that assessed the effect of individual studies on the overall prevalence of scabies.
Factors associated with scabies infestation among schoolchildren
In this work, parent education and family members with itchy signs or scabies were reported in 8 articles; sharing history of cloth with family in six articles; male sex and having history of contact with skin itching cases or scabies in five articles; sharing common sleeping beds/fomites in four articles; infrequent cloth washing in three articles; and avoiding bathing with soap and water in two articles were significantly associated with scabies among schoolchildren in Africa (Table 3).
Several factors associated with the magnitude of scabies among schoolchildren in Africa.

However, family size was reported in five articles, students not attending grade level in four articles, wealth or income status, infrequent baths, and rural residence were reported in three articles. Furthermore, sharing clothes with a scabies case, family or caregiver poor knowledge about scabies, and having animals inside the house were reported in two articles, but according to this systematic review and meta-analysis, none of these factors mentioned above was significantly associated with scabies among schoolchildren in Africa (Table 3).
Discussion
Scabies is a significant global health problem, disproportionately affecting children in developing countries, especially in Africa. The current work aimed to assess the pooled magnitude of scabies and its drivers among schoolchildren in Africa. In the current study, 19 studies with 28,482 subjects were included.
The current pooled data reveals that scabies affected 10.81% of the schoolchildren. A consistent result was reported in Nigeria (10.5%). 55 However, as compared to the current finding, a higher prevalence was reported in Australia (16.5%), 56 Malaysia (31%), 13 Turkey (33%), 14 Solomon Islands (54.3%), 57 Bangladesh (61%–62%), 16 Sierra Leone (67%), 58 and Thailand (87.5%). 15 Conversely, our result was higher than studies conducted in Taiwan (1.4%), 59 and Australia (8.2%). 60 These variations could be due to sociodemographic characteristics, data collection season, population of the participant in the study, sample sizes, methodology used, and economic status.
This meta-analysis revealed that children who have a history of sharing clothing with family were 1.76 times more vulnerable to scabies infestation than children who did not share their clothing with family. Previous studies also reported similar results.37,38,61,62 This might be due to the consequences of living in impoverished conditions.
Children from families with illiterate parents in the study had scabies at a rate 0.96 times greater than those with parents who could read and write. The current result is in line with several previous studies conducted elsewhere.37,40,44,53,63–65 This could be explained by the fact that children from educated families have better opportunities to earn more money and better personal and environmental sanitation, in addition to better health-seeking behavior than others. 40
The other associated predictor was sharing common sleeping beds/fomites with others. Schoolchildren who shared common sleeping beds/fomites were 2.13 times more likely to be infested with scabies than their counterparts. This finding is in line with studies conducted elsewhere.37,38,66–69 Close contact while sleeping in the same bed with a person who has scabies might be a cause of acquiring the disease. However, previous research conducted in Ethiopia did not find a significant association between scabies and the sharing of sleeping beds or fomites.26,70,71
Boys are almost twice as likely as girls to acquire scabies, with this gender difference being statistically significant. This finding is consistent with the studies done in the southern Ethiopia,44,49 northern Ethiopia,47,69 and Cameroon. 38 A Cameroonian boarding schools study, 38 reported that boys were more likely to share sleeping beds, had higher rates of close contact with individuals experiencing itching, practiced less frequent handwashing with soap, and had longer fingernails compared to girls. These factors may contribute to increased scabies infestation among boys. Additionally, close skin-to-skin contact during play, fights, or sports can facilitate scabies mite transmission in males. Conversely, the findings from studies conducted in Ghana 46 and Gambia 20 demonstrated a higher prevalence of scabies among females. These contrasting results highlight the potential influence of cultural and geographical factors on scabies epidemiology.
Children with a history of contact with itchy skin or scabies are 3.37 times more likely to get scabies. Additionally, children with family members with itchy signs or a history of scabies were 5.83 times more likely to have scabies. This finding is supported by several studies.38,44,48,61 This is expected because scabies is a disease transmissible by contact. If there was a family history of scabies, the transmission rate might be high since there is a high probability of contact within the family.
In this study, infrequent cloth washing and not taking a bath with soap and water were significantly associated with scabies infestation. This finding revealed that children whose cloth was not frequently washed had a 5.30 and those who took baths only with water had an 8.51 times greater chance of being infected with scabies compared to those who frequently washed their cloth and their bodies with both water and soap. Although hygiene standards are not effective against mites and do not modify the likelihood of contracting scabies,72,73 our study and others23,26,53,74,75 confirmed that scabies and poor personal hygiene are associated risk factors. Other studies do not confirm this association.76,77
The study found differences in the prevalence of scabies in children according to country, with Cameroon having the highest prevalence (17.80%) and Tanzania having the lowest prevalence (2.0%). This difference might be due to differences in lifestyle and health-care-seeking behavior.
The pooled prevalence figure of scabies increased over time from 6.98% in 2015–2018 to 12.90% in 2019–2024. This variation could be attributed to the difference between the advancement of diagnostic tools, differences in the study season, increased accessibility to health facilities, and education and awareness of skin diseases, including scabies, which could result in a decrease in the number of scabies cases.
Strengths and limitations
The unique aspect of this systematic review and meta-analysis is that it is the first to report the pooled magnitude of scabies in African schoolchildren. Furthermore, the pooled risk factors associated with scabies infestation were identified. However, this review has its own limitations. Variations in data collection methods and sample sizes across various studies could be the reason for the observed heterogeneity in the current review. In general, this study did not consider all countries in Africa due to the lack of availability of articles; therefore, the estimate may not fully represent the continent’s prevalence of scabies infestation.
Conclusion
The pooled prevalence of scabies among the published studies included, increased from 6.98% during 2015−2018 to 12.90% between 2019 and 2023. Regardless of the cause, the increase in scabies prevalence has the potential to negatively impact the health and well-being of schoolchildren. Policymakers and health planners should put a great deal of emphasis on the implementation of relevant prevention and control measures. Further in this population, extensive research is needed across different African countries to understand the nature, dynamics, and risk factors associated with scabies.
Supplemental Material
sj-docx-1-smo-10.1177_20503121241274757 – Supplemental material for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis
Supplemental material, sj-docx-1-smo-10.1177_20503121241274757 for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis by Abayeneh Girma, Indiris Abdu and Kasaye Teshome in SAGE Open Medicine
Supplemental Material
sj-docx-2-smo-10.1177_20503121241274757 – Supplemental material for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis
Supplemental material, sj-docx-2-smo-10.1177_20503121241274757 for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis by Abayeneh Girma, Indiris Abdu and Kasaye Teshome in SAGE Open Medicine
Supplemental Material
sj-docx-3-smo-10.1177_20503121241274757 – Supplemental material for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis
Supplemental material, sj-docx-3-smo-10.1177_20503121241274757 for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis by Abayeneh Girma, Indiris Abdu and Kasaye Teshome in SAGE Open Medicine
Supplemental Material
sj-docx-4-smo-10.1177_20503121241274757 – Supplemental material for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis
Supplemental material, sj-docx-4-smo-10.1177_20503121241274757 for Prevalence and determinants of scabies among schoolchildren in Africa: A systematic review and meta-analysis by Abayeneh Girma, Indiris Abdu and Kasaye Teshome in SAGE Open Medicine
Footnotes
Acknowledgements
None.
Author contributions
AG, IA, KT were actively engaged in conceptualization, resources, data curation, methodology, software, formal analysis, investigation, validation, visualization, and supervision, writing—original draft and writing—review and editing. All authors read and approved the final version of the manuscript.
Availability of data and materials
The datasets generated and analyzed during the current study are available from the corresponding author upon reasonable request.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
