Abstract
Background:
Methods:
The PubMed database was searched using “recurrent
Results:
Compared with placebo, VOS following standard-of-care antibiotics for CDI significantly reduced risk of recurrence at 8 weeks (relative risk, 0.32 (95% CI: 0.18–0.58);
Conclusions:
Clinical care of patients with rCDI now includes Food and Drug Administration-approved therapeutics to address microbiome restoration. Clinical trial evidence supports use of VOS following antibiotics and importance of microbiome restoration in rCDI.
Introduction
Moreover, up to 25% of patients with an initial CDI episode will experience recurrent CDI (rCDI), which most commonly occurs in the first 8 weeks following antibiotic therapy.4,5 Patients with rCDI are more likely to experience subsequent episodes than those with an initial CDI episode, which is often attributed to persistent microbiome disruption.4,6 Patients with rCDI critically have significantly higher morbidity and mortality rates than those with primary CDI. 7 Additionally, rCDI has a negative impact on health-related quality of life (HRQoL), with over 40% of patients believing they would never be rid of CDI symptoms. 8 Patients bear a substantial economic burden, primarily driven by repeated CDI-related hospitalizations, and over 80% of patients with rCDI had a CDI-related hospitalization within 12 months after their first recurrence. 9
The treatment of all CDI episodes requires the use of standard-of-care (SOC) antibiotics to resolve active infection. Guideline recommendations for treating an initial episode of CDI or a first or second episode of rCDI include fidaxomicin (200 mg twice daily for 10 days or 200 mg twice daily for 5 days, then once every other day for 20 days) or oral vancomycin (125 mg 4 times daily for 10 days or in a tapered/pulsed regimen).10,11 However, these agents do not eradicate
In this systematic review, we aim to highlight the role of the microbiome in CDI development and recovery and discuss newly approved microbiota-based LBPs, with a specific focus (using a systematic approach) on fecal microbiota spores, live-brpk (VOWST™; formerly SER-109 and hereafter referred to as VOS for Vowst Oral Spores).
Pathophysiology and diagnosis of CDI
Risk factors for CDI encompass a variety of factors that influence the host immune system and/or disrupt gastrointestinal microbiota including cumulative antibiotic exposure, older age (>65 years), comorbidities (e.g., immunosuppression, inflammatory bowel disease, or chronic kidney disease), proton pump inhibitor use, and most significantly, a history of CDI recurrence.16,19 Prior hospitalization is a key risk factor for rCDI, as the rate of recurrence is consistently higher in patients with healthcare-associated CDI versus community-associated CDI. 2
Therapeutic strategies for the prevention of rCDI
Because SOC antibiotic therapy for rCDI is often ineffective for correcting the gut microbiota dysbiosis underlying recurrence, restoration of host defenses with microbiome therapeutics following the use of SOC antibiotics has emerged as a promising treatment strategy to break the cycle of recurrence.13,17,18 Current treatment guidelines for patients with three or more episodes of CDI unresponsive to SOC antibiotics include fecal microbiota transplantation (FMT).10,11,15 FMT involves the transfer of stool from a screened healthy donor to a recipient via colonoscopy, enema, or duodenal infusion.10,15 However, FMT is not FDA-approved, preparation and administration of FMT is not standardized, and cases have been reported of FMT being associated with hospitalization and death due to the transmission of pathogenic agents, including drug-resistant bacteria.20,21 Thus, there had been a need for standardized, effective, and safe products to prevent future CDI recurrences. 13
There are two types of FDA-approved therapies for this purpose with differing underlying strategies: administration of a toxin-targeting monoclonal antibody or administration of gastrointestinal microbiota.22,23 Bezlotoxumab (Zinplava™), a monoclonal antibody that binds to
The two FDA-approved LBPs are fecal microbiota, live-jslm (REBYOTA™; formerly RBX2660; now RBL), and fecal microbiota spores, live-brpk (VOWST™; formerly SER-109; now VOS) (Table 1).11,15,26,27 RBL was approved first in November 2022; it is considered a whole-stool product and is administered via rectal enema. 24 In contrast, VOS is about 1% of the total mass of donor materials following a manufacturing process that yields a product enriched with purified Firmicutes spores administered orally in a capsule formulation. 28 VOS was approved in April 2023 and will serve as the focus for the remainder of this review. 22

CDI:
VOWST™ Oral Spores
VOS is an FDA-approved orally administered human donor-derived microbiome therapeutic containing Firmicutes bacterial spores indicated to prevent the recurrence of CDI in adults following antibacterial treatment for rCDI.22,31 The proposed mechanism of action of the Firmicute spores in VOS is modulation of the conversion of primary bile acids to secondary bile acids in the gastrointestinal tract, resulting in the restoration of host defenses against bacterial pathogens and inhibition of

VOS is manufactured in accordance with Good Manufacturing Practice regulations and uses samples from healthy human donors who have completed extensive health examinations, laboratory testing, and health-related questionnaires. 31 Donor samples undergo a thorough series of manufacturing steps, including ethanol-based purification, to remove 99% of fibers and fecal solids and isolate Firmicute spores. 34 These rigorous manufacturing steps also rapidly inactivate potential bacterial, viral (including SARS-CoV-2), parasitic, and fungal pathogens, thereby mitigating the risk to patients beyond donor screening alone, while providing beneficial Firmicutes to reduce the risk of rCDI.28,34 Because Firmicutes spores are resistant to oxygen, heat, and gastric acid, they can be administered orally with a low pill burden and can be stored at room temperature.31,34
Product labeling for VOS instructs patients take a single dose of a laxative (i.e., 10 oz of magnesium citrate or, in patients with renal impairment, 250 mL GoLYTELY) on the day before and at least 8 h prior to taking the first dose of VOS to wash out any residual antibiotics that may remain in the gastrointestinal tract, which could otherwise inactivate VOS dose species.12,22 VOS is taken as a single daily dose of 4 oral capsules on an empty stomach for 3 consecutive days within 2–4 days following the completion of SOC antibiotic treatment for rCDI.12,22 Each capsule of VOS contains between 1 × 106 to 3 × 107 Firmicutes spore colony-forming units (CFUs) in 92% ± 4% (w/w) glycerol in saline. 22
Systematic review search methods
A systematic review was conducted with the aim of evaluating and summarizing all clinical trial evidence for the use of VOS. The PubMed database was searched for clinical trials using the terms “recurrent
Results of PubMed search.

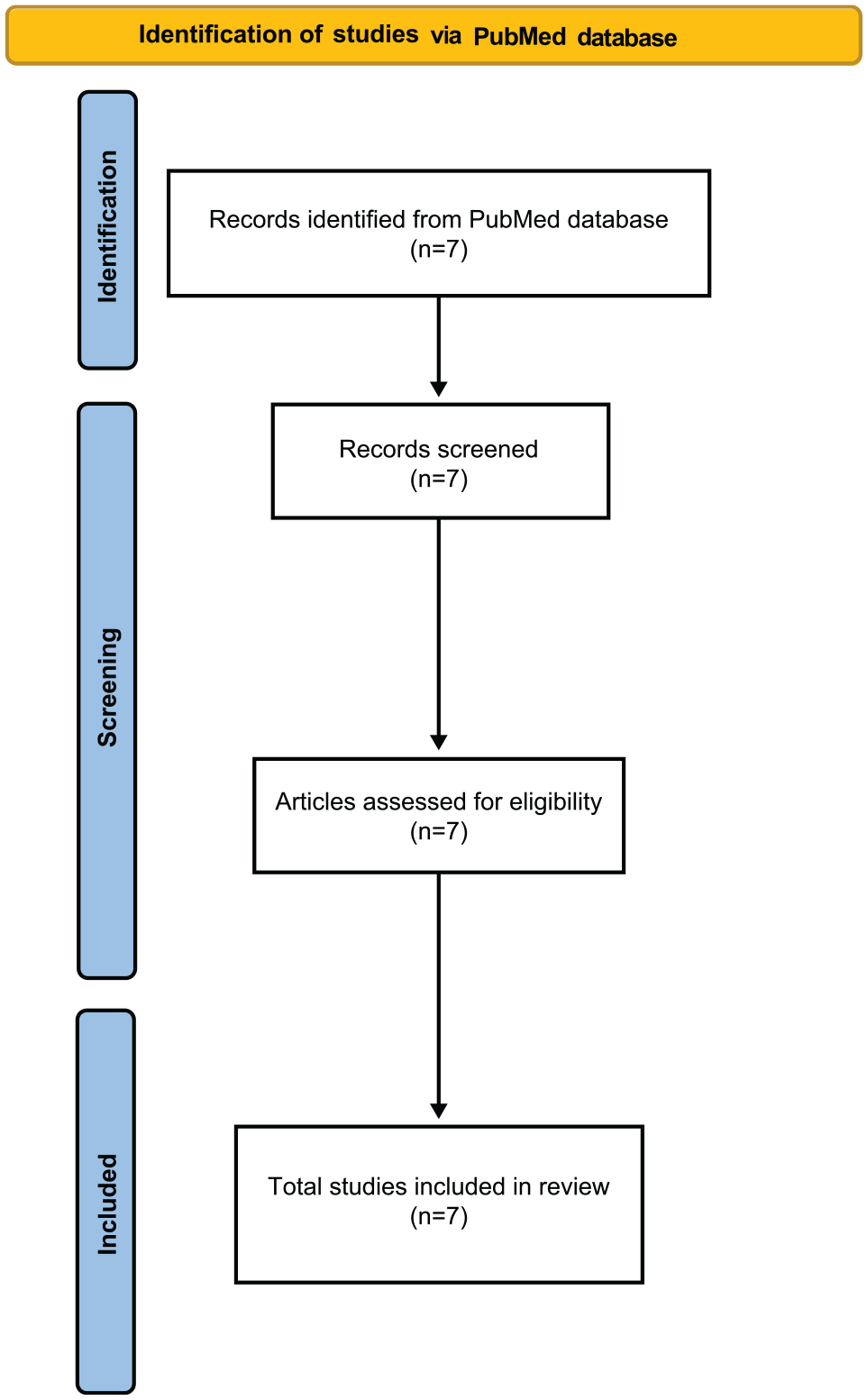
PRISMA flow diagram of study selection.
Results
Study design and patient population
Eligibility criteria and efficacy/safety endpoints across the identified clinical trials were similar (Table 3). In the pivotal, randomized, double-blind, placebo-controlled, Phase 3 ECOSPOR III clinical trial, patients with an established diagnosis consistent with rCDI, a positive

CDI:
Recurrence of CDI was defined as three or more unformed stools per day for two consecutive days, any positive result of a
Characteristics of patients enrolled in VOS clinical trials were reflective of those with greatest risk of recurrence.16,19 Most patients enrolled across these three clinical trials were White, female, aged ⩾ 65 years, and had a history of multiple CDI recurrences (Table 4).12,32,35 The SOC antibiotic was selected by the investigator, with vancomycin being the most common antibiotic regimen administered for the most recent qualifying episode of CDI (Table 4).12,32,35 A post hoc analysis of the ECOSPOR III trial reported that patients who received VOS in ECOSPOR III had a mean (standard deviation) Charlson Comorbidity Index (CCI) score of 4.1 (2.4); 32.4% had cardiovascular disease, 18.1% had malignancy, and 14.8% had renal impairment or failure.
36
Additionally, 13.7% of patients in ECOSPOR III took non–CDI-targeted antibiotics after treatment with VOS or placebo and 40.7% of patients were taking acid suppressive medications at baseline (proton pump inhibitor,
Efficacy
Efficacy was assessed across all three clinical trials based on the rate of rCDI and recurrence-free rates at Weeks 8 and 24, respectively (Table 5). The ECOSPOR III trial met the primary endpoint of superiority of VOS compared with placebo in reducing the risk of CDI recurrence through Week 8 after initiating therapy (relative risk reduction of VOS following antibiotic therapy for CDI vs placebo following antibiotic therapy for CDI: 0.32 (0.18–0.58);
In ECOSPOR III, a greater proportion of patients who received VOS, compared with placebo, were recurrence-free at Weeks 8 and 24, respectively (Week 8: 88% vs 60%; Week 24: 79% vs 53%). 33 ECOSPOR IV results demonstrated similarly high recurrence-free rates for patients who received VOS at Weeks 8 and 24 (91% and 86%, respectively). 32
A post hoc analysis of ECOSPOR III demonstrated that VOS-treated participants had a lower relative risk of CDI recurrence at Week 8 compared with placebo across all high-risk demographic subgroups that were analyzed (including age, sex, number of prior episodes, creatinine clearance at baseline, non-CDI antibiotic usage, use of acid suppressive medications at baseline, and CCI score categories of 0, 1–2, 3–4, and ⩾5). 36 Rates of rCDI at Week 8 were analyzed across relevant patient subgroups (i.e., age and antibiotics) and found to be consistent with rCDI rates in the overall population. Although patients who were ⩾65 years had numerically higher rates of recurrence in both Phase 3 clinical trials at Week 8 compared with those <65 years, the treatment effect of VOS was consistent across all age groups in both the ECOSPOR III (relative risk (95% CI), 0.36 (0.18–0.72) for ⩾65 years vs 0.24 (0.07–0.78) for <65 years) and ECOSPOR IV (rCDI rate (95% CI), 13% (8%–20%) for ⩾65 years vs 4% (1%–9%) for <65 years) trials. Similarly, although recurrence rates were numerically higher among patients who received vancomycin versus those who received fidaxomicin in the ECOSPOR III and ECOSPOR IV trials, the treatment effect was consistent between subgroups (ECOSPOR III: relative risk (95% CI), 0.41 (0.22–0.79) for vancomycin vs 0.09 (0.01–0.63) for fidaxomicin; ECOSPOR IV: rCDI rates (95% CI), 9% (5%–14%) for vancomycin vs 8% (3%–17%) for fidaxomicin).
Subgroup analyses comparing rates of CDI recurrence and recurrence-free rates in patients with first recurrence (history of 2 CDI episodes) versus those with multiple recurrences (history of ⩾3 CDI episodes) were also conducted in ECOSPOR IV. Results indicate that similarly low rates of CDI recurrence at Week 8 (rCDI rate (95% CI), 7% (2%–15%) for first recurrence vs 10% (6%–15%) for multiple recurrences) and recurrence-free rates at Week 8 (relative risk (95% CI), 94% (86%–98%) for first recurrence vs relative risk (95% CI), 90% (85%–94%) for multiple recurrences) were observed between subgroups, which were consistent with the findings of the overall population. 32
Compositional and metabolic shifts in the microbiome
In ECOSPOR III, stool specimens were collected at baseline, and at Weeks 1, 2, and 8, after dosing; in the ECOSPOR Phase 2 study, stool samples were collected at baseline, and at Weeks 1, 4, and 8, after dosing. Samples were analyzed for changes in species composition and bile acid concentrations, using whole metagenomic sequencing and liquid chromatography-mass spectrometry, respectively.12,31 Engraftment was quantified as the number of VOS dose species detected in posttreatment stool samples that had not been present at baseline.12,31 The metagenomic analyses conducted in ECOSPOR III demonstrated that patients who received VOS had a higher number of engrafting VOS dose species compared with placebo at Weeks 1 and 8. In the ECOSPOR Phase 2 study, patients who received VOS had significantly more VOS dose species than those who received placebo at Weeks 1, 4, and 8 (
Safety/Tolerability
Across all three clinical trials, most treatment-emergent adverse events (TEAEs) were mild or moderate in intensity, self-limiting, and gastrointestinal in nature.12,32,33,35 Of the 182 patients included in the safety population of the ECOSPOR III trial, 168 (92%) experienced TEAEs. The most common TEAEs reported for VOS versus placebo, respectively, were flatulence (70% vs 76%), fatigue (59% vs 63%), and abdominal distension (54% vs 53%). 12 In ECOSPOR IV, 141 (54%) of the 263 patients enrolled (all patients received study drug) experienced TEAEs; the most commonly observed TEAEs up to Week 8 were diarrhea (23%), flatulence (8%), and nausea (8%). 32 In the ECOSPOR Phase 2 trial, 66 (74%) of the 89 patients enrolled experienced TEAEs. Gastrointestinal disorders were the most reported TEAEs with similar occurrence rates across both treatment arms (VOS, 55% vs placebo, 45%). In ECOSPOR III, 51% of VOS- and 52% of placebo-treated patients experienced TEAEs that were considered treatment-related or possibly treatment-related. 12 In the safety analysis population of ECOSPOR IV, 12.2% of patients experienced TEAEs that were considered related or possibly related to VOS. In the ECOSPOR Phase 2 trial, 17% of patients (VOS, 18% vs placebo, 14%) experienced TEAEs considered related or possibly related to treatment. 32
No patients in the VOS arms of ECOSPOR III and ECOSPOR IV experienced a serious TEAE leading to study withdrawal. None of the serious AEs or deaths reported across the three trials were deemed to be related to treatment.12,32,35 Patients in the placebo arm of the ECOSPOR III trial experienced more serious TEAEs than those in the VOS arm (16% vs 8%, respectively); most of the serious TEAEs were diarrhea related to on-study CDI recurrence. In ECOSPOR III, no serious TEAEs related to VOS occurred through Week 8; three deaths occurred in the VOS arm.
12
In ECOSPOR IV, 33 (13%) of 263 patients experienced serious TEAEs and 8 (3%) patients experienced TEAEs leading to death.
32
Of the 89 patients in the ECOSPOR Phase 2 study, 12 (13%) experienced a serious TEAE (VOS,
HRQoL
An exploratory aim of ECOSPOR III was to evaluate the validity of the
Discussion
Clinical care for patients with rCDI has entered a new era with the availability of FDA-approved, microbiome-targeted interventions.22,24,26 These novel drugs were evaluated in comprehensive clinical development programs that reported significant reduction in the risk of CDI recurrence compared with placebo.22,24 Our review focuses on VOS, the only orally administered member of this novel class of drugs, and aims to support healthcare professionals and their patients in making informed treatment decisions to reduce the burden of CDI recurrence.
In Phase 3 studies, VOS reduced the relative risk of rCDI by 68% versus placebo, following antibiotic treatment in patients with rCDI, with low rates of rCDI enduring through 24 weeks.12,32,33 Reduced rates of rCDI were consistent regardless of the risk factors for rCDI (e.g., age) and prior antibiotic therapy for the qualifying CDI episode.12,32 Most AEs observed in patients treated with VOS were gastrointestinal in nature and were mild or moderate in intensity. 12 Patients who received VOS also demonstrated greater improvements in disease-specific HRQoL. 37
This review is limited in that it only includes published articles and data; unpublished data and results could not be accessed for reporting or inclusion. Considering that this review is primarily focused on summarizing VOS clinical evidence from reputable and peer-reviewed sources, we believe that this methodology is accurate in capturing all currently available and relevant studies related to VOS. Another limitation is the heterogeneity of the clinical studies evaluated, including the differences in inclusion criteria and study design (i.e., number of CDI episodes and double-blind vs open-label).12,32,35 Additionally, not all studies used the FDA-approved dose across trials; however, doses in the Phase 3 trials were adjusted based on the efficacy findings from the Phase 2 trial.12,22,32,35
A proposed mechanism by which the VOS treatment effects may be conveyed is based on observations that patients treated with VOS had a higher number of newly appearing dose species in their microbiome and greater concentrations of secondary bile acids than patients treated with placebo; engraftment of dose species and increased concentrations of secondary bile acids were seen as early as 1 week after VOS treatment, demonstrating early microbiome restoration.12,14,35
Relevance to patient care and clinical practice in comparison with existing drugs
The use of antibiotics alone to treat recurrent
Conclusion
Emerging evidence supports that the management of rCDI should follow a two-step approach, which includes treating the active infection with SOC antibiotics followed by a live biological product, such as VOS, to address the underlying pathophysiology of microbiome disruption, improve host defenses, and protect against
Footnotes
Acknowledgements
The clinical development program for VOS was sponsored by Seres Therapeutics. Writing, editorial, and submission assistance for this manuscript was provided by Stevin Joseph, PharmD, and Cheryl Casterline, MA (Peloton Advantage, LLC, an OPEN Health company), and funded by Nestlé Health Science. The authors confirm that they have authorized the submission of the manuscript via third party and have approved all statements or declarations (e.g., conflicting interests, funding) therein.
Author contributions
Kerry LaPlante, Robert Stevens, and Anne J Gonzales-Luna contributed to conception and design, contributed to acquisition, analysis, or interpretation of data, critically revised the manuscript for important intellectual content, gave final approval, and agree to be accountable for all aspects of work ensuring integrity and accuracy.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Kerry LaPlante has served as a consultant for Ferring Pharmaceuticals and Seres Therapeutics. Robert Stevens is a current employee and shareholder of Seres Therapeutics, Inc. Anne J Gonzales-Luna has served as a consultant for Ferring Pharmaceuticals and Innoviva Specialty Therapeutics and has received research grants from Seres Therapeutics and Paratek Pharmaceuticals.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The clinical development program for VOS was sponsored by Seres Therapeutics.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Availability of data and materials
All data are from published materials that are referenced, and there are no new samples or models.


