Abstract
Objective:
To evaluate the status of medication adherence in diabetic patients and its effective factors.
Methods:
A cross-sectional descriptive study was conducted with 170 diabetic patients in Iran. Participants were assessed for medication adherence, self-efficacy, and social support. Descriptive statistics, bivariate analyses, and multiple stepwise regression were conducted to explore predictors for medication adherence.
Results:
Regression analysis showed that 48% of medication adherence changes stemmed from the four variables including social support, self-efficacy, income, and education levels, (R2adj = 0.480, F = 39.943, p < 0.001). According to the model, the highest effects were related to income level (β = 0.332, t = 5.493, p ⩽ 0.001) and self-efficacy (β = 0.330, t = 4.789, p ⩽ 0.001), respectively. Based on the final model, only the social support variable showed no significant relationship with adherence (β = 0.002, t = 0.032, p = 0.947).
Conclusion:
Social support and self-efficacy were related to medication adherence in diabetic patients, and social support can improve medication adherence in patients with diabetes by affecting self-efficacy. Healthcare workers who interact with individuals with diabetes should take into account the factors mentioned above when designing health promotion interventions to address the needs of these individuals.
Introduction
Diabetes as a chronic and non-communicable metabolic disorder is considered a global health emergency in the 21st century.1,2 The global prevalence of DM in adults will increase to 10.2% in 2030 and to 10.9% in 2045.2–4 According to the statistics, the prevalence of the disease triples every 15 years, 5 and developing countries experience a higher prevalence than other countries. 6 In Iran, the prevalence of type 2 diabetes was estimated to be 8.4% in 2013, and it is anticipated to reach 12.3% by 2035.7,8 Diabetes leads to numerous physical and mental complications such as cardiovascular disease, diabetic nephropathy, amputation, feelings of rejection, worry about the future of the disease, as well as marital, family, and occupational problems.9,10 The management of diabetes is challenging, 11 but medication adherence plays a vital role in mitigating symptoms and preventing complications. 12 Evidence shows that medication adherence is among the most critical factors in diabetes management and control, and non-adherence leads to disease worsening. 13 Medication adherence improves blood sugar control, resulting in reduced disease complications and relevant costs. 14 Various studies indicate that many patients with diabetes have poor medication adherence.15–17 Various factors, including factors related to the health system and healthcare workers, factors related to the patients themselves, and factors related to personal traits, can affect the level of medication adherence in chronic diseases, such as diabetes.18,19 However, the presence of factors influencing medication adherence can be different in different societies.19,20 Research has reported that medication adherence is associated with self-efficacy and social support in renal21,22 and previous vascular patients.22,23 Based on the literature review, patients with a high sense of self-confidence in self-care function more successfully in controlling their disease.20,24 A study on elderly people with heart disease indicated that individuals with higher self-efficacy had higher levels of disease management, including taking medication according to the doctor’s prescription and controlling diet and stress. 25 On the other hand, individuals with poor self-efficacy had poorer self-care adherence; thus, as reported, self-efficacy is one of the most robust determinants of health-related behavior.22,26,27 Studies have analyzed the effects of self-efficacy and social support on blood sugar control; however, the associations between these variables are not clear yet. 13 It is essential to examine other predictive factors in patients and their contributions to medication adherence. For example, researchers have dealt with the positive effect of social support and regarded paying attention to the patient’s perception and their attitude toward the received support as an important factor in their ability for disease control and self-care. 12 Given that following treatment recommendations can culminate in patients’ recovery or disability and affect the therapeutic achievements, awareness of the current status can also affect planning and implementing the required interventions. The present study seeks to investigate the relationships between self-efficacy and social support with medication adherence in patients with diabetes and to evaluate the effect of self-efficacy and its mediation role on the relationship between social support and medication adherence.
Method
Study design and setting
The current research was a hospital-based cross-sectional study conducted from April to September 2022 in two hospitals in the city of Tabriz, Iran, named Shahid Madani Hospital and Imam Sajjad Hospital, both teaching and academic hospitals. These two hospitals have specialized diabetes clinics. We have followed the Strengthening the Reporting of Observational Studies in Epidemiology Guidelines when preparing the manuscript.
Sample size, sampling, and study participants
The sample size was estimated at 152 cases using the mean formula and based on the medication adherence score reported by Mehrtak et al. 28 However, considering an increase in the accuracy of the study by 10%, the final sample size was calculated as 170 cases.
Study parameter: alpha = 0.05, power = 0.80, m = 2.96, SD = 1/89, d = 10%M
Qualified participants were selected using the convenience sampling method. The participants included individuals over 18 years old with reading and writing ability diagnosed with type 2 diabetes who received medication for at least 6 months. Individuals were excluded from the study in case of acute life-threatening conditions, such as coma or mental disorder, which limited their cognitive ability to participate.
Instruments
Socio-demographic and patient characteristics: It consists of the socio-demographic variables of age, gender, educational levels, occupation, monthly family income, and duration of disease.
The Morisky Medication Adherence Scale MMAS-8 questionnaire: Was designed by Morisky and Wood, 2008. The 8-item Morisky Medication Adherence Scale (MMAS-8) is a structured self-report measure of medication-taking behavior. The scale provides information on behaviors related to medication use that may be unintentional (e.g., forgetfulness) or intentional (e.g., not taking medications because of side effects). This questionnaire consists of seven questions of two options (with yes or no) and a question as an answer. The overall scores range from zero to eight, with scores divided into three categories: poor drug compliance (score greater than 2), moderate adherence (score 1 and 2), and high adherence (0 score). 29 The reliability and validity of the MMAS-8 have been assessed by Mohammadpour et al. in Iran. Internal consistency was acceptable with an overall Cronbach’s coefficient of 0.697 and test–retest reliability showed good reproducibility (r = 0.940); p < 0.001. 30
The multidimensional scale of perceived social support: The perceived social support questionnaire designed by Zimet et al. 31 encompasses 12 items. The questionnaire evaluates three domains, a: perceived support from the family (four items), b: perceived support from friends (four items), and c: significant other (four items). The items are scored based on a seven-point Likert scale from “completely disagree” (score: 1) to “completely agree” (degree: 7) where the minimum and maximum scores are 12 and 84, respectively. 32 The instrument validity and reliability were confirmed in Iran and its validity was confirmed through content analysis and reliability in various studies was established using Cronbach’s alpha coefficient (α = 0.86–0.9 for the subscales and 0.86 for the whole instrument). 33 In the current study, social support is broadly defined as the provision of emotional (e.g., caring), or informational (e.g., notifying someone of important information) support, instrumental (e.g., helping with housekeeping), tangible (e.g., practical support like financial aid), and/or psychological support for somebody by the social network of family members, friends, or community members. 34
Self-efficacy questionnaire: The self-efficacy was measured using the General Self-Efficacy Scale of Sherer et al. 35 This scale consists of 17 items, scored based on a Likert scale which was rated from completely disagree to completely agree, and each item is scored from 1 to 5. 36 As a result, the maximum and minimum scores are 85 and 17, respectively. The validity and reliability of the questionnaire were approved in Iran by Asgharnejad et al. 37 with Cronbach’s alpha of 0.83 which confirms the high reliability of the tool and its reliability coefficient is 0.92.
Statistical analysis
Data analysis was conducted using Statistical Package for the Social Sciences version 24 software and included descriptive statistics such as mean, standard deviation (SD), frequency, and percentage. The independent t-test and the analysis of variance (ANOVA) were used to assess the relationship between the study’s demographic variables and main variables. Furthermore, Pearson’s correlation test was used to assess the relationship between the study’s main variables (medication adherence, social support, and self-efficacy); finally, univariate and multivariate linear regression analyses were used to predict the effect of independent variables on the dependent variable of medication adherence. p-values < 0.05 were considered significant. The missing value was replaced by the mean.
Results
Sample characteristics and their relationships with main variables
The participants included 170 individuals with diabetes (mean age = 58.79 years; SD = 13.03; age range = 22–87); 92.4% were in the age group above 40 years, of which 48.8% belonged to the age group above 60 years. More than 58% of the participants were male, 56.5% were employed, and 38.2% had a diploma and higher education levels. Assessing the relationship between the study’s demographic variables and main variables, including medication adherence, self-efficacy, and social support, indicated that only the two variables of income level and education level were significantly related to the main variables (Table 1).
Baseline characteristics of the diabetic participants (n = 170).
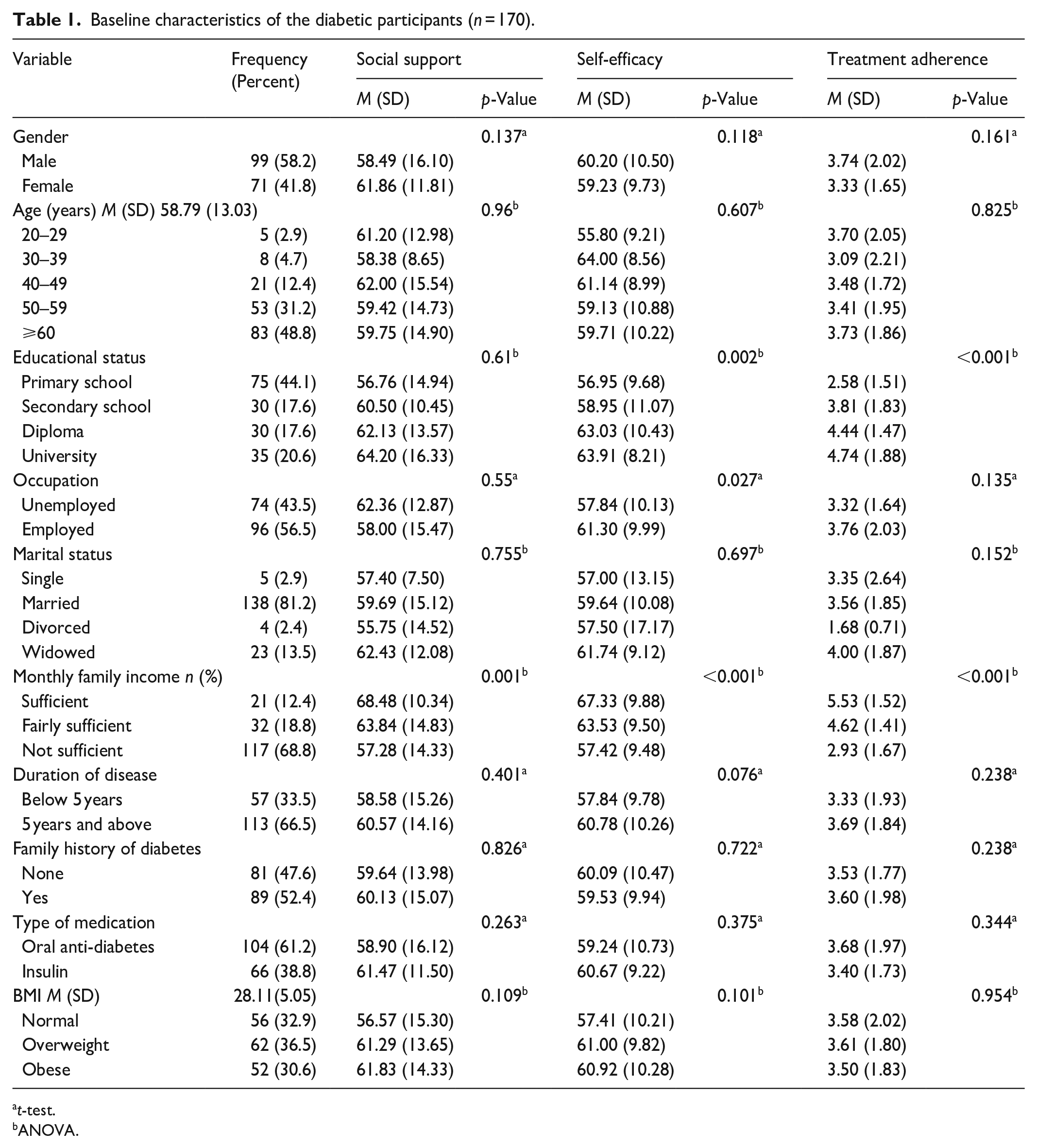
t-test.
ANOVA.
According to Table 2, the data analysis indicated that individuals with diabetes had low scores on medication adherence, and based on the categorization of the majority of cases, 151 people (88.8%) had low medication adherence (scores obtained from the questionnaire less than six). In terms of social support, moderate to high scores were reported. According to the categorization, only 18.2% of people (n = 31) had lower social support, and 52.9% (n = 90) and 28.8% (n = 49) reported moderate and high social support, respectively. The mean (SD) scores of the areas of social support from friends, family, and other key individuals were 15.95 (9.45), 21.86 (6.10), and 21.76 (6.17), respectively. The highest and lowest scores were related to the areas of support from family and friends. Furthermore, in terms of the categorization of self-efficacy, although the mean scores were moderate, most participants reported a high level of self-efficacy. In addition, Pearson’s correlation analysis showed a positive and significant relationship between self-efficacy and medication adherence (r = 0.531, p < 0.001) and also between social support and medication adherence (r = 0.331, p < 0.001).
Descriptive statistics and correlations among primary study variables (N = 170).
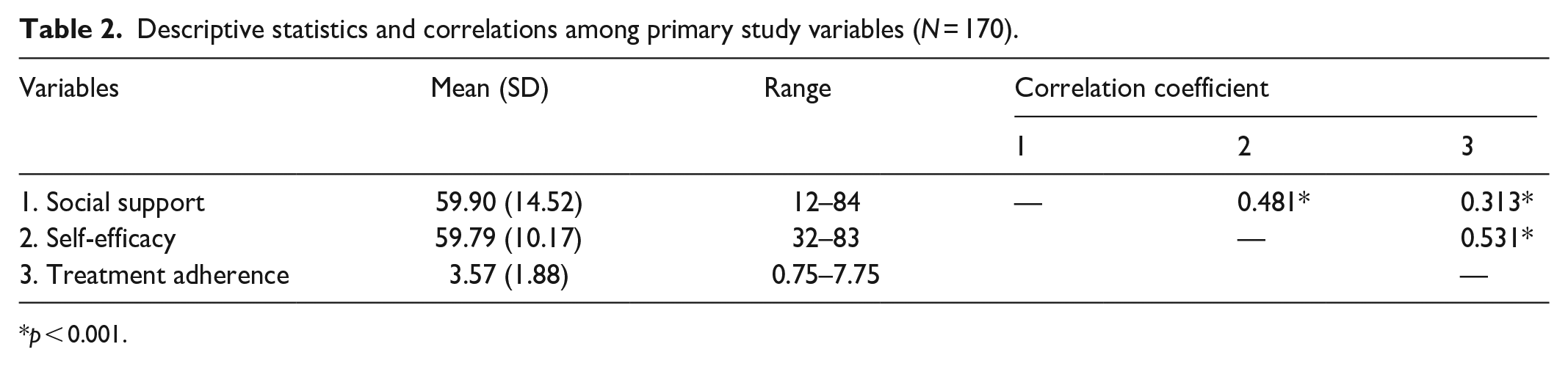
p < 0.001.
Social support and medication adherence
Regression analysis revealed a significant relationship between high social support and higher levels of medication adherence (β = 0.313, t = 4.276, p < 0.001) and that 9.3% of the dependent variable’s changes could be explained by social support (R2adj = 0.93, F = 18.287, p < 0.001). Also, assessing the effect of the income level variable on social support indicated that a high-income level was significantly associated with a high self-efficacy level (β = 0.218, t = 3.801, p < 0.001) and that 7.4% of the self-efficacy variable’s changes were related to income level (R2adj = 0.074, F = 18.287, p < 0.001).
Self-efficacy and medication adherence
Regression analysis showed that a high self-efficacy level was significantly associated with higher levels of medication adherence (β = 0.513, t = 8.132, p < 0.001) and that 27.8% of the dependent variable’s changes could be explained by self-efficacy (R2adj = 0.278, F = 66.122, p < 0.001). Also, assessing the effects of social support, income level, and education level on self-efficacy indicated that high social support (β = 0.386, t = 5.688, p < 0.001), income (β = 0.215, t = 3.145, p = 0.002), and education (β = 0.164, t = 2.445, p = 0.016) levels were significantly related to high self-efficacy levels and that 29.8% of self-efficacy variable’s changes were related to social support, income level, and education level (R2adj = 0.298, F = 24.949, p < 0.001).
Social support, self-efficacy, income, education status, and medication adherence
Regression analysis to assess the effect model of the two variables of self-efficacy and social support on medication adherence revealed that both variables could explain 27.8% of the dependent variable’s changes (R2adj = 0.278, F = 66.122, p < 0.001). In this model, self-efficacy showed a positive and significant relationship with medication adherence (β = 0.495, t = 6.646, p < 0.001), but social support had no significant relationship with medication adherence (β = 0.075, t = 1.011, p = 0.313). Path analysis indicates that social support generally has an indirect effect of 0.191 on medication adherence.
Finally, by assessing the effect model of the social support, self-efficacy, income level, and education level variables on medication adherence, regression analysis showed that 48% of medication adherence’s changes stemmed from the variables above (R2adj = 0.480, F = 39.943, p < 0.001). According to the model, only the social support variable showed no significant relationship with adherence (β = 0.002, t = 0.032, p = 0.947), and the highest effects were related to income level (β = 0.332, t = 5.493, p ⩽ 0.001) and self-efficacy (β = 0.330, t = 4.789, p ⩽ 0.001), respectively; education level showed significant and positive relationship with medication adherence (β = 0.311, t = 5.295, p ⩽ 0.001).
Discussion
The aim of managing diabetes is to regulate blood glucose levels and ultimately enhance the well-being of individuals with diabetes. 25 Current studies deal with a more comprehensive understanding of how social support and self-efficacy function as two main psychological constructs that may help diabetic patients in medication adherence. The results of this research show that while social support and self-efficacy were associated with medication adherence, self-efficacy mediated the relationship between social support and medication adherence. These findings suggest that self-efficacy is a critical mechanism through which social support may affect adherence behavior.
First, the results of the current study indicated that the participants’ medication adherence level was low. However, they had a more appropriate status in terms of social support perception and self-efficacy. Unfortunately, nearly 89% had non-optimal medication adherence. Numerous studies have been conducted on medication adherence, indicating low medication and treatment acceptance in chronic diseases. 15 Various studies showed that 57% 16 and 42.7% 17 of patients did not have good medication adherence. The results of Ghanei Gheshlagh et al.’s 38 study in Iran are also consistent with our study. In the research of these researchers, only a limited number of individuals (7.4%) had reported scores of medication adherence higher than 6. Another study in Iran also revealed that about 60% of individuals had poor medication adherence, 15 which was not consistent with the report of other studies conducted in other countries, such as Nigeria 39 and the United Arab Emirates, 40 as well as with the study conducted in Iran. 41 However, different findings can be due to the implementation of different disease control programs by the health sectors in different countries. 19 Moreover, the value of most of these studies has been restricted because of the challenge of measurement tools for medication adherence.
By investigating the relationship between socio-demographic variables and medication adherence, individuals with high education and income levels had higher levels of medication adherence and based on regression analysis, income status was a stronger predictive factor compared to other variables. The findings of this study are matched with the findings of other studies conducted in Iran and other countries.19,42,43 Patients with a higher education level seem to have a higher awareness of their treatment, medications, and complications of treatment non-adherence and also gain more knowledge of the importance of medications in controlling their disease and preventing disease complications. 44 Some studies conducted in America 42 showed no relationship between education level and medication adherence. 45 Other researchers have also reported that having a higher income level affects optimal medication adherence, which is consistent with the findings of this study.15,42,46 It seems that individuals with higher income levels, in addition to the public sector’s services, can also benefit from the private sector’s services and easy access to medicines and other health services.
Investigating the relationship between the study’s main variables indicated a positive and poor-to-moderate relationship between social support and medication adherence. According to Badrizadeh et al.’s 47 report, the correlations between the areas of social support and its total score with medication adherence are −0.342, 0.044, and 0.277, respectively. In this study, social support alone could explain 12.9% of medication adherence changes, almost in line with our study. Furthermore, additional research has also recognized the presence of this correlation.48,49 Researchers believe that patients with diabetes, particularly those who also have complications, need frequent visits to the doctor, and doctors and healthcare workers can play a supportive role in providing the necessary support and required training to the patients. 50 It has been shown that support programs such as providing appointment and disease management reminders, motivational messaging, and education with cell phones can improve chronic disease management and reduce visits among low-income, vulnerable populations.51,52 In addition, the use of consumer health information technologies and technological surrogate nursing in supporting medication adherence appears to have potential benefits for patients’ self-management of diabetes.53–55
Assessing the relationship between the two variables of self-efficacy and medication adherence indicated the presence of a moderate-to-high relationship between the two variables. The literature review shows that self-efficacy is an important prerequisite for patients’ self-management and plays a critical role in diabetic individuals’ self-care. A study conducted in India has revealed that self-efficacy is an important predictor of performing self-care behaviors in patients with diabetes. 56 In another study, self-efficacy played a crucial role in adherence to self-care behaviors, such as physical activity and having a healthy diet. 57 However, other researchers58,59 reported no significant relationship among diabetic patients’ self-efficacy, self-management, self-care behaviors, and medication adherence. One of the reasons for such inconsistency can be cultural and social factors.
However, finally, the mediating role of self-efficacy in the relationship between social support and medication adherence was an important finding in our study. By investigating the mediating role of self-efficacy in the relationship between social support and medication adherence in patients with previous failure in America, Maeda et al. 60 after controlling demographic variables, such as age, gender, and education, emphasized the mediating role of self-efficacy. Also, Xie et al. 22 reported the same results among patients with coexisting type 2. Self-efficacy might be a key target for implementing interventions to improve self-care behaviors in these patients. It has also been found that self-efficacy mediates the relationship between social support and medication adherence in rheumatoid patients 61 and hypertension 24 has also had a mediating effect.
This research has some limitations. First, self-reporting can lead to bias, and using questionnaires to assess medication adherence can affect the results; this challenge can be removed by checking blood sugar levels. Since cross-sectional studies cannot express the cause-and-effect relation, conducting studies with a longitudinal design and trials with a strong design is recommended. Further, conducting qualitative studies can also be useful in explaining the role of other moderators. Despite these limitations, this research is the first study to discover the relationship between social support and self-efficacy and how they affect medication adherence in diabetic patients. Future research is warranted to investigate the barriers to and facilitators of medication adherence among these patients.
Conclusion
Social support and self-efficacy were related to medication adherence in diabetic patients, and social support can improve medication adherence in patients with diabetes by affecting self-efficacy. Given the consequences of non-adherence in patients with diabetes, implementing interventions affecting medication adherence will facilitate the likelihood of correct treatment use, reduce costs, and lead to improved health outcomes. Diabetes educators may take into consideration these factors in planning health promotion interventions to meet the needs in this regard. In summary, clinicians can focus on interventions that enhance patients’ confidence in managing their health and adhering to prescribed medications. Educational programs, counseling, and regular follow-up discussions can be beneficial in building and sustaining self-efficacy, and adjustments to treatment plans and support strategies can be made based on changes in the patient’s socioeconomic factors, self-efficacy, and educational background over time.
Supplemental Material
sj-doc-1-smo-10.1177_20503121231221446 – Supplemental material for The mediating effect of self-efficacy on the relationship between social support and medication adherence in adults with type 2 diabetes
Supplemental material, sj-doc-1-smo-10.1177_20503121231221446 for The mediating effect of self-efficacy on the relationship between social support and medication adherence in adults with type 2 diabetes by Khadijeh Khalili Azar, Amirreza Mirzaei, Ali-Reza Babapour and Azita Fathnezhad-Kazemi in SAGE Open Medicine
Footnotes
Acknowledgements
We thank the women who participated in the study. We also appreciate the support from the Islamic Azad Medical Sciences University.
Authors’ contributions
Concept: A. Fn-K, A. Kh. K.A; Data collection &/or processing- Kh. K.A, AR. B.P; Analysis and/or interpretation- A. Fn-K.; Literature search- A. M, AR. B.P; Writing- AR. B.P, Kh. K.A; Critical review- A. Fn-K, A. Kh. K.A.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest for the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval for this study was obtained from * the Ethics Committee of the Islamic Azad University, Tabriz Medical Sciences, Tabriz, Iran (code number: IR.IAU.TABRIZ.REC.1400.046).
Informed consent
Written informed consent was obtained from all subjects before the study.
Trial registration
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

