Abstract
Introduction:
Stroke is the second-leading global cause of death next to ischemic heart disease. The burden of stroke mortality, morbidity, and disability is increasing across the world. In Ethiopia, evidence on the survival status of adult stroke patients is insufficient. The purpose of this study is to estimate in-hospital mortality and its predictors among adult stroke patients.
Methods:
Institution-based retrospective follow-up study was conducted on adult stroke patients who were admitted to Debre Markos Comprehensive Specialized Hospital from 1 November 2015 to 31 October 2020. Through simple random sampling, 382 patient charts were selected from 1125 stroke patients for 5 years follow-up period. Data were entered using EpiData™ version 4.1 and exported to Stata/SE™ version 14 for cleaning, coding, categorizing, and analysis. Predictor variables were selected using 95% confidence interval with a corresponding adjusted hazard ratio.
Results:
In this study, 219 (57.33%) males and the mean (standard deviation) age of 57.65 ± 14.3 years. The in-hospital mortality rate of stroke was 12.8%; the median (interquartile range) time to mortality and Glasgow Coma Scale were 7 (4–13) days and 14 (11–15), respectively. The incidence of in-hospital mortality was 29/1000, 11/1000, 8/1000, and 13.6/1000 person-days in the first, second, third, and end of follow-up weeks, respectively. Pneumonia (adjusted hazard ratio = 3.51 (95% confidence interval = 1.86, 6.61)), hemorrhagic stroke (adjusted hazard ratio = 2.03 (95% confidence interval = 1.03, 3.99)), moderate impairment Glasgow Coma Scale (9–12) (adjusted hazard ratio = 2.16 (95% confidence interval = 1.08, 4.29)), severe impairment Glasgow Coma Scale (3–8) (adjusted hazard ratio = 2.38 (95% confidence interval = 1.01, 5.67)), history of hypertension (adjusted hazard ratio = 2.01 (95% confidence interval = 1.08, 3.74)), and increased intracranial pressure (adjusted hazard ratio = 2.12 (95% confidence interval = 1.10, 4.07)) were statistically significant predictors for in-hospital mortality.
Conclusion:
In-hospital mortality of stroke was relatively high, and the median time to mortality was 8 days. Pneumonia, hemorrhagic stroke, Glasgow Coma Scale, history of hypertension, and increased intracranial pressure were identified predictors.
Introduction
A stroke is a sudden onset of focal or global disturbance of cerebral function lasting 24 h or longer, resulting from disruption of blood supply to the brain tissue caused by an inadequate supply of oxygen and nutrients. 1 Individuals with this condition frequently exhibit unilateral motor or sensory deficits, speech disturbances, altered mentation, headache, and/or vertigo.2–4 Stroke accounts for 11.8% of total death worldwide, ranking as the second-leading cause of mortality after ischemic heart disease and being a major cause of permanent disability.3,5–7 In the absence of public health response, stroke is expected to exceed 23 million new cases and 7.8 million mortalities per year by 2030. 8
The in-hospital mortality of stroke patients in developed countries ranges from 3% to 11%, whereas in low- and middle-income countries, it increases to 7%–15%. 9 In sub-Saharan African (SSA) countries, it was three to four times higher than that of developed countries ranging from 11% to 43.4%. 10 Based on severity, older age, comorbidities, treatment effectiveness, and complications, nearly 38% of hemorrhagic strokes are fatal compared to 8%–12% of ischemic strokes. 11 At 30 days, hemorrhagic stroke has a nearly 40% case-fatality rate due to intracerebral hemorrhage. 12
The previous evidence revealed 3.1% in Taiwan, 13 7.13% in Spain, 14 4.9% in Germany, 15 and 33.3% in Tanzania 14 in-hospital stroke mortality. More than half (62%) of stroke patients died within a 10-year follow-up in the Netherlands. 16 In China, the mortality rate for ischemic and hemorrhagic stroke was 15.9% and 20.4%, respectively, 13 22% of patients died within 30 days in Azerbaijan, 17 and 41% of stroke mortality reported was in Ghana. 18 In Uganda, evidence revealed that 6.3% died within 7 days and 26.8% died within 30 days of stroke onset, with a mean survival point in time of 25.7 days and an average hospital stay of 8.9 days. 19 Similarly in Burkina Faso, the intra-hospital mortality rate was 12.7% on day 7, 21% on day 14, and 28.7% at the end of follow-up on a mean hospital length of stay of 13.2 days. 20 According to the Global Burden of Disease (GBD) report 2015 in Ethiopia, hemorrhagic stroke was the fifth leading cause of mortality, accounting for 62.7 mortalities per 100,000 people. 21 World Health Organization (WHO) 2017 report, stroke mortality in Ethiopia reached 6.23% of total mortalities, ranked as the sixth leading cause of mortality with an age-adjusted death rate of 89.82 per 100,000 population. 22 In a study conducted at St. Paul’s Millennium Medical College in Ethiopia, the median length of hospital stay was 9 days, with an intra-hospital mortality rate of 14.7% (23.5% hemorrhagic and 6.1% ischemic) stroke. 23 The average length of stay of the patient was 6.7 ± 2.5 days in Shashemene Hospital, 24 and the intra-hospital mortality rate was 11% (59.3% due to hemorrhagic stroke) in Felege Hiwot Referral Hospital, Ethiopia. 10
Modifiable factors like aspiration pneumonia, urinary tract infection, level of Glasgow Coma Scale (GCS), increased intracranial pressure (ICP), atrial fibrillation, abnormal laboratory findings (i.e. hemoglobin level, creatinine level, random blood sugar level), duration of symptom onset and length of hospital stay, pre-existing chronic illnesses, and behavioral risk factors are known predictors.10,13,20 Non-modifiable (age, sex, family history, illiteracy, without spouse, and race/ethnicity) were risk factors for stroke mortality.16,19,25,26 Currently, stroke is becoming a public health problem in developing countries including Ethiopia with huge consequences in terms of lost productivity, premature deaths, and long-term disability.27–30 Recently, the Ethiopian Federal Ministry of Health (FMOH) focused on non-communicable diseases (NCDs) with a sustainable strategy of prevention, treatment, and care. 31 In-hospital stroke mortality is an excellent tool for measuring the quality of hospital management and acute stroke case-fatality rates. Evidence on stroke mortality can be used to monitor disease trends and design appropriate public health interventions. This finding contributes to reducing patient mortality, stroke complications, and further disabilities, as well as improving care quality in high-risk patients through targeted interventions. There is a paucity of evidence on stroke survival status and its predictors. Hence, this study aims to estimate in-hospital mortality and its predictors among adult stroke patients admitted to Debre Markos Comprehensive Specialized Hospital, Ethiopia.
Methods
Study design and eligibility criteria
A hospital-based retrospective follow-up study was conducted from 1 November 2015 to 31 October 2020. Data were collected from 1 October 2020 to 30 November 2020. The study was conducted at Debre Markos Comprehensive Specialized Hospital (DMCSH), Debre Markos Town. It is located 295 km away from Addis Ababa, the capital city of Ethiopia, and 265 km from Bahir Dar, the capital city of Amhara National Regional State. The hospital has 213 admission beds and 456 health staff (196 nurses, 49 physicians, and 211 other professionals); it serves more than 3.5 million people in its catchment area. In the hospital, blood tests, clinical examinations, and recently introduced brain computed tomography (CT) scans are used to diagnose patients, and chemotherapies, complications management, and rehabilitation are available treatments for stroke. Furthermore, observing cerebrospinal fluid pressures during the lumbar puncture procedure and pupillary examinations (dilatation, edema, and weak reflexes) were used to diagnose increased ICP, and laboratory blood investigations, chest X-ray, and clinical features were used to diagnose pneumonia. 32 All adult (⩾18 years old) patients diagnosed with stroke by clinically or brain imaging and admitted to DMCSH during the study period were a source population. Patient charts with missing important baseline variables (i.e. age, date of admission, and date of discharge) were excluded from the study.
Sample size determination and sampling procedure
The sample size was calculated using Stata/SE™ version 14 using sample size determination formulas for survival analysis. It is calculated by 95% confidence interval (CI), 80% power, and the Freedman principle approach, which assumes equal allocation between these groups, p = q = 0.5, P(event) = 0.5, event = 164, s1(t1) = 0.58, and hazard ratio (HR) = 1.55 hemorrhagic stroke of the previous study in Iran, 2018 33
The probability of the event = 1 − (ps1(t) + qs2(t)). 34
where Zα/2 is the significance level two side (5% the values 1.96); Zβ has the value of 80% power (0.84); p is the proportion of the population allocated for the first group (0.5); q is the proportion of the population allocated for the second group (0.5); s1(t) is the survival function in the first group at the time t1 (0.58).
For this study, the largest final required sample size was 382 including a 5% non-response rate. To select samples, a simple random sampling technique was used. Within 5 years of the study period, 1125 admitted adult stroke patients were registered in the Health Management Information System (HMIS) at the hospital. While the study cases were chosen to be representative of each study year, the samples were assigned to each year in proportion to their size. Finally, each year of the study period, study participants were selected by computer-generated technique.
Operational definitions
Event: all in-hospital stroke mortality from all types of stroke occurred in the follow-up period.
Censored: those patients who were referred to another hospital or discharged from the hospital without developing the event are considered.
Survival time: the time in days from dates of admission to the date of event ascertainment (death due to stroke) or time of censor.
Time to mortality: time from the first day of admission to the occurrence of adult stroke death during the study period.
GCS: it measures the level of consciousness categorized as normal/mild impairment GCS (13–15), moderate impairment GCS (9–12), and severe impairment GCS (3–8). 35
Hypertension: it is defined as a persistent elevation of systolic blood pressure (SBP) ⩾140 mm Hg and/or diastolic blood pressure (DBP) ⩾90 mm Hg following repeated measurement.36,37
Pneumonia: this is a severe form of acute respiratory infection known to affect the lung alveoli filled with fluid resulting from a decrease in the amount of oxygen and pain.38,39
ICP: it is defined as sustained ICP greater than 20 mm Hg for greater than 5–10 min in a patient who is not being stimulated.40,41
Diabetes: it is the condition of fast plasma glucose ⩾7.0 mmol/L (126 mg/dL) or 2 h of plasma glucose ⩾11.1 mmol/L (200 mg/dL) during an oral glucose tolerance test. 42
Data collection procedure and quality assurance
The recorded review technique was employed to collect important data among eligible medical records in the individual patient charts. The data extraction checklist, adapted from previous related studies, was prepared in English to maintain consistency with the patient chart,19,25,26 and the 2019 WHO stepwise approach stroke surveillance manual. 2 Data quality was maintained by following a careful checklist design, training data collectors and supervisors, and providing close supervision and monitoring throughout the data collection period.
Ethical consideration
This study was approved by the Debre Markos University, College of Health Sciences ethical review committee (HSC/R/C/Ser/Co/42/13/13). The need of informed consent was waived by the ethics committee of Debre Markos University. All methods were performed in accordance with the relevant guidelines and regulations.
Statistical analysis
Data were entered into the EpiData ClientEntry™ version 4.2 statistical software and exported to Stata/SE™ version 14 for cleaning, recoding, categorizing, and analysis. All descriptive statistics were presented by mean value, median, standard deviation (SD), frequency tables, graphs, and charts for important descriptive variables. The Cox proportional hazard model was done to estimate the independent effect of predictors on the occurrences of stroke mortality. Model fitness was checked by log-log plot graphical, proportional hazard assumptions test, and the Schoenfeld test. The final goodness of fit was checked using the Cox–Snell residual analysis (Supplemental Figure 1). Variables were selected with P ⩽ 0.25 in bivariable to multivariable Cox proportional hazard regression analysis. Finally, in the multivariable Cox regression model at P < 0.05, 95% CI, the corresponding adjusted hazard ratio (AHR) was used to identify statistically significant predictors for stroke mortality.
Results
Socio-demographic characteristics
In this study, 382 adult stroke patients were included with 219 (57.33%) of them being males. The majority (i.e. 350 (91.62%)) of patients were Orthodox religion followers, and the mean age of study participants was 57.65 ± 14.3 (SD) years. About 270 (70.68%) were married, 219 (57.33%) of rural residents, and 173 (45.29%) of stroke patients who could not read and write (Table 1).
Socio-demographic characteristics of adult stroke patients admitted in DMCSH Northwest Ethiopia, 2020.
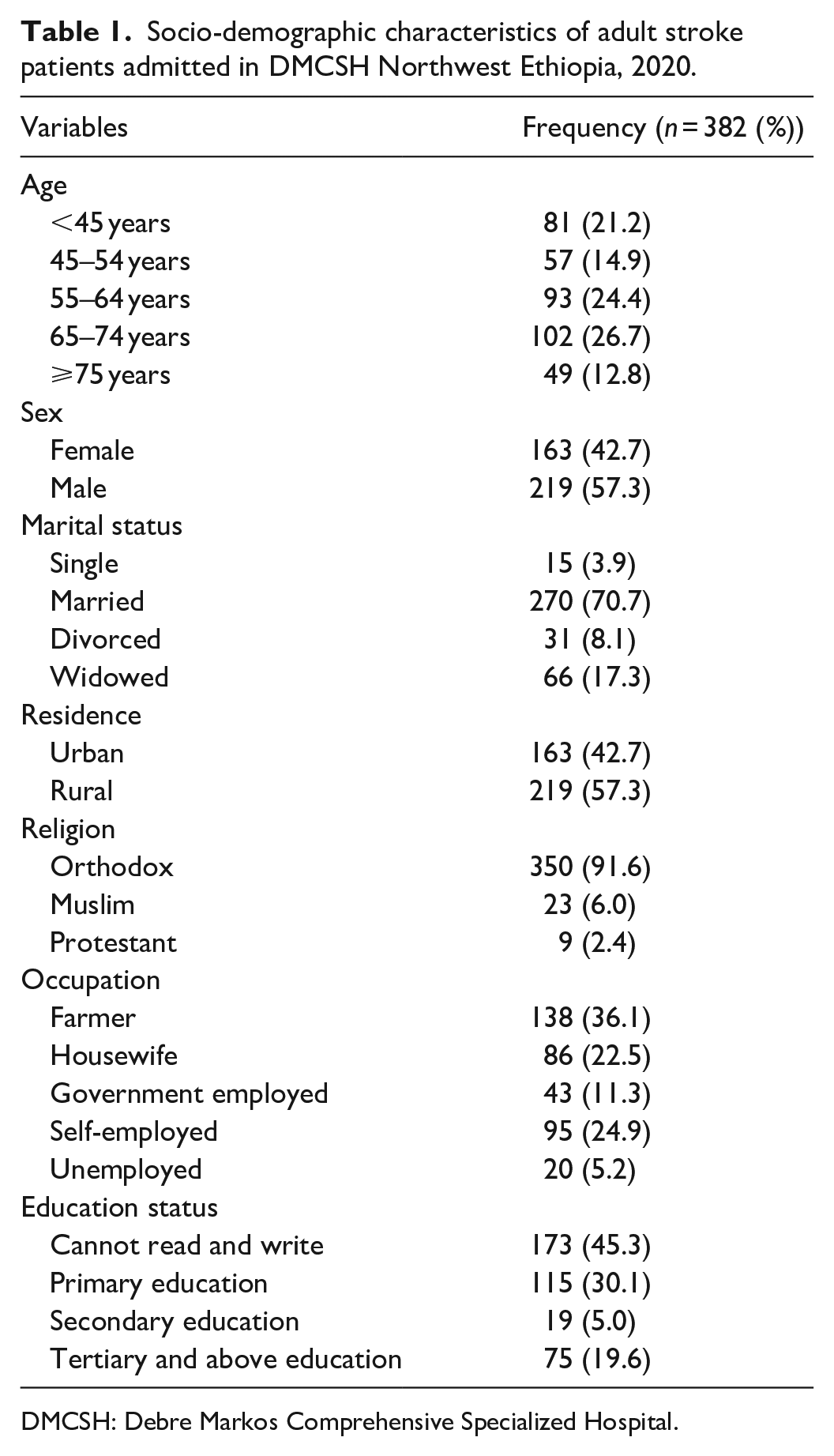
DMCSH: Debre Markos Comprehensive Specialized Hospital.
Baseline clinical parameters, history of chronic illnesses and patient risk behaviors
One-third (66%) of patients were diagnosed with ischemic stroke. the maximum systolic blood pressure, pulse, and respiratory rate of the patient were 240 mm Hg, 160 beats/minute, and 38 breaths/minute, respectively. The median (interquartile range (IQR)) of the GCS was 14 (11–15). The mean (SD) duration of a delay from symptom onset to hospital arrival was 2.72 ± 4.24 days and 252 (66%) of patients had normal/mild impairment GCS levels at the time of hospital admission. Among the study participants, only 68 (17.8%) and 9 (2.4%) of them had a history of alcohol and cigarette use, respectively; whereas about 101 (26.44%) of study patients had a diagnosed history of hypertension (Table 2 and Figure 1).
Baseline clinical parameters associated with stroke patients admitted in DMCSH Northwest Ethiopia, 2020.

DMCSH: Debre Markos Comprehensive Specialized Hospital; GCS: Glasgow Coma Scale; ICP: intracranial pressure.

History of diagnosed chronic illnesses among adult stroke patients admitted in DMCSH Northwest Ethiopia, 2020.
Mortality status and time to mortality among stroke patients
In this study, the in-hospital stroke mortality rate was 12.8% (with 25 (6.5%) hemorrhagic and 24 (6.3%) ischemic stroke) and 51.8% of stroke patients improved after treatment in the 3589 person-days follow-up times (Figure 2). The median (IQR) time to death from the entire cohort was 7 (4–13) days. The mean survival time for admitted stroke patients was 27.7 days (95% CI = 25.40, 29.73). The incidence of stroke mortality was the highest in the first and second weeks of follow-up time, and then decreases in subsequent days of the follow-up time, 29 per 1000 person-days in the first week, 11 per 1000 person-days in the second week, 8 per 1000 person-days in the third week, and 13.6 per 1000 person-days observation at the end of follow-up (Supplemental Figure 2).

In-hospital clinical outcomes of stroke patients admitted in DMCSH, Northwest Ethiopia, 2020.
Predictors of stroke mortality
In bivariable Cox proportional hazard regression, variables like age, sex, pneumonia complication, stroke type, admission GCS level, admission body temperature, admission respiratory rate, history of hypertension, history of cardiovascular disease (CVD), admission increased ICP, admission creatinine level, and admission diastolic blood pressures were selected for multivariable analysis. Whereas in the multivariable Cox proportional hazard regression model, only six variables are identified as statistically significant. Stroke patients with pneumonia complications are at higher risk for mortality. Stroke patients who had pneumonia complications were 3.51 (AHR = 3.51 (95% CI = 1.86, 6.61)) times more risk of mortality compared to those who had no pneumonia complications. Diagnosed stroke type was found to be a statistical predictor of stroke mortality. Patients who had hemorrhagic type stroke were twofold (AHR = 2.03 (95% CI = 1.03, 3.99)) at higher risk of mortality compared to ischemic type stroke. Likewise, the level of GCS score at the time of hospital admission has positively been related to stroke patient mortality. Stroke patients with severe impairment GCS (3–8) were 2.38 (AHR = 2.38 (95% CI = 1.01, 5.67)) times more at risk of mortality compared to normal/mild impairment GCS (13–15), and patients with moderate impairment GCS (9–12) had more than twofold (AHR = 2.16 (95% CI = 1.08, 4.29)) the risk of mortality compared to normal/mild impairment GCS (13–15). Those stroke patients with a history of hypertension at admission were at a twofold (AHR = 2.01 (95% CI = 1.08, 3.74)) higher risk of mortality compared to non-hypertensive stroke patients. Finally, in this study, increased ICP was identified as a statistically significant factor. Those stroke patients who experienced increased ICP were 2.12 (AHR = 2.12 (95% CI = 1.10, 4.07)) times more likely to experience mortality compared to their counterparts without increased ICP (Table 3 and Figures 3–5).
Multivariate Cox regression analysis for predictors of mortality among adult stroke patients admitted in DMCSH, Northwest, Ethiopia, 2020.

GCS: Glasgow Coma Scale; CVD: cardiovascular disease; ICP: intracranial pressure.

The Kaplan–Meier survival curves compare the survival time of adult stroke patients with categories of pneumonia in DMCSH, Northwest Ethiopia, 2020.

The Kaplan–Meier survival curves with log-rank test compare survival time of adult stroke patients with categories of increased ICP in DMCSH, Northwest Ethiopia, 2020.

The Kaplan–Meier survival curves with log-rank test compare survival time of adult stroke patients with categories of hypertension history in DMCSH, Northwest Ethiopia, 2020.
Discussion
This study provided evidence on the mortality of adult stroke patients and its predictors of admitted to DMCSH. In this study, the mortality rate was 12.8% (95% CI = 9.6, 16.6) with a total of 3589 person-days follow-up times. This finding is comparable with 11% in Felege Hiwot Comprehensive Specialized Hospital, 10 12% in Ayder Referral Hospital, 43 13.3% in Shashemene Referral Hospital, 24 14.7% in Hawassa University Referral Hospital, 44 Ethiopia, and 13% in Saudi Arabia. 17 This finding is lower than studies conducted in Azerbaijan 22%, 13 Tanzania 33.3%, 14 and Ghana 41%. 18 This low rate of mortality may be due to differences in socioeconomic status, follow-up time, and study setup. But, it is higher than studies in Taiwan 3.1%, 13 in Spain 7.13%, 14 and in Germany 4.9%. 15 This variation may be due to differences in development status, level of awareness of the population on risk factors of stroke and its mortality, and differences in sample size. In developing countries such as Ethiopia, deteriorating patients remaining at home against medical advice resulted in out-of-hospital mortality and may have contributed to an underestimated mortality rate of stroke patients.
The in-hospital mortality from hemorrhagic stroke was slightly higher at 6.5% than from ischemic stroke at 6.3%. In this study, 62 (16.2%) stroke cases were referred to higher-level hospitals for further evaluation, management, and immediate decisions. As a result, this comparable and low in-hospital mortality of hemorrhagic stroke could be attributed to referral cases (i.e. lack of neurosurgery and brain imaging) in the hospital may be underestimated. This was comparable with studies in Hawassa 44 and St. Paul’s Medical College, Ethiopia. 23 The median (IQR) time of death was 7 (4–13) days, and this was found to be comparable with 4.5 days found in a study done in Hawassa 44 and 4 days encountered at Ayder Comprehensive Specialized Hospital as the median time of death among adult stroke patients after admission. 45
In this study, stroke with pneumonia complications was found to be a predictor factor for stroke mortality. Those patients who had pneumonia complications were 3.51 times more at risk of mortality compared to those who had no pneumonia complications. This finding is consistent with studies conducted in Nigeria, Hawassa, and St. Paul’s Medical College, Ethiopia.23,44,46 Post-stroke pneumonia is the most common complication of all stroke patients within 7 days of admission leading to mortality and poor clinical outcome as a result of disturbed neurological function recovery, and reduced activities of daily living.47–49
Diagnosed stroke type was found to be a statistical predictor of mortality. Patients who had hemorrhagic type stroke were at a twofold higher risk of mortality compared to those with ischemic. This was supported by a study conducted in London, 50 but the difference is from a study conducted in Ayder Hospital, Ethiopia. 45 The possible difference may be due to a difference in sample size and/or study setting.
Likewise, the level of GCS score at the time of hospital admission was positive with stroke patient mortality. Stroke patients with severe impairment GCS were at 2.38 times greater risk of mortality compared to normal/mild impairment GCS; whereas patients with moderate impairment, GCS had 2.16 times more risk of mortality compared to normal/mild impairment GCS. This finding was in line with studies in Saudi Arabia, 17 Iran, 33 South London, 50 and Ayder Comprehensive Specialized Hospital, Mekele, Ethiopia. 45 The possible explanation could be patients with decreased GCS or comatose patients had a higher probability of developing acute phase neuro-medical stroke complications, which possibly predisposes them to a high risk of death.
In addition, those stroke patients with a history of hypertension at admission were twofold higher risk of mortality compared to non-hypertensive stroke patients. This finding is consistent with studies done in Saudi Arabia, 17 Egypt, 51 and Felege Hiwot Referral Hospital, Ethiopia. 10 The possible reason may be poor adherence to anti-hypertension medication due to poor health-seeking behaviors resulting in uncontrolled blood pressure which may increase the likelihood of death.
Finally, in this study, increased ICP was identified as a statistically significant factor. Those stroke patients who have increased ICP were at 2.12 times higher risk of mortality compared to stroke patients without increased ICP. This finding is similar to studies done in Saudi Arabia, 17 St. Paul’s Medical College, Ethiopia, 23 and Ayder Comprehensive Specialized Hospital, Ethiopia. 45 This finding can be explained by the effect of stroke-related depressed immunity, depressed gag-reflex, and delayed mobilization of admitted patients probably increasing mortality compared to non-ICP cases.49,52,53
Limitations of the study
The retrospective nature of this study, incomplete or missing variables, may have introduced random errors. Hospital-based studies may not reflect the true picture or may underestimate the number of stroke patients who were critical and died before hospitalization, as well as the number of mild cases which may have not been reported to the hospital. Stroke patients who are discharged against medical advice and referred cases to a higher level may have an impact on the in-hospital mortality rate. Patients diagnosed without brain imaging took part in this study, which misdiagnosed stroke type as a limitation.
Conclusion
In this study, the in-hospital mortality rate of stroke was relatively high. The median time to death was 8 days for stroke patients. In this study, presence of pneumonia complication, hemorrhagic type of stroke, decreased level of GCS, history of hypertension, and increased ICP at time of admission were found to be significant predictors of in-hospital mortality for stroke patients. Early identification, treatment of complications, and other co-morbidities along with strict follow-up are required to reduce in-hospital stroke mortality. Designing appropriate strategies to control modifiable risk factors and strengthening diagnosis and treatment facilities in the context of Ethiopia will be important. Prospective community-based studies with a large sample size were recommended to estimate the exact burden of stroke mortality.
Supplemental Material
sj-docx-1-smo-10.1177_20503121221122465 – Supplemental material for In-hospital mortality and its predictors among adult stroke patients admitted in Debre Markos Comprehensive Specialized Hospital, Northwest Ethiopia
Supplemental material, sj-docx-1-smo-10.1177_20503121221122465 for In-hospital mortality and its predictors among adult stroke patients admitted in Debre Markos Comprehensive Specialized Hospital, Northwest Ethiopia by Maru Admas, Muluken Teshome, Pammla Petrucka, Animut Takele Telayneh and Nakachew Mekonnen Alamirew in SAGE Open Medicine
Footnotes
Acknowledgements
The authors thank Debre Markos Comprehensive Specialized Hospital for the permission to conduct this study and Debre Markos University for all unreserved support to accomplish this research. The authors also thank all data collectors and individuals who contributed to this work.
Author contributions
M.A. contributed to the conceptualization. M.A., M.T., N.M.A., and A.T.T. contributed to the formal analysis. M.A., N.M.A., M.T., and P.P. contributed to the development or design of methodology. M.A., A.T.T., and N.M.A. contributed to the entering data into computer software. M.T., A.T.T., and P.P. contributed to the supervision and validation. M.A., N.M.A., and M.T. contributed to the writing original draft. M.A., A.T.T., and P.P. writing review and editing. All authors read and approved the final article.
Availability of data and materials
The data sets used and/or analyzed during this study are available from the corresponding author upon reasonable request.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was approved by the Debre Markos University, College of Health Sciences ethical review committee (HSC/R/C/Ser/Co/42/13/13).
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
The need of informed consent was waived by the ethics committee of Debre Markos University because all these data were obtained from secondary data source of patient charts.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

