Abstract
Objective:
Undernutrition in the elderly has adverse effects on physiological functions and various clinical outcomes. In Ethiopia, similar to many developing countries, there is a dearth of epidemiological data on the nutritional status of the elderly. This study aimed to assess the magnitude of undernutrition and associated factors among the elderly population enrolled in the Public Servants Social Security Agency in Harar, eastern Ethiopia.
Method:
A cross-sectional study was carried out among 337 elderly adults from June to August 2020. The Mini Nutritional Assessment Tool Short Form assessed the nutritional status of the elderly. Data were entered in Epi Data software version 3.1 and transferred to SPSS version 20 for analysis. Ordinal logistic regression assessed factors associated with undernutrition, using variables with a p value less than 0.05 as statistically significant.
Result:
The magnitude of undernutrition was 16.6% and 45.1% were at risk of undernutrition. Being unable to read and write (odds ratio (OR) = 3.64; 95% confidence interval (CI), 1.98–6.72), elderly with morbidities (OR = 2.05; 95% CI, 1.15–3.64), low dietary diversity score (OR = 3.52; 95% CI, 1.63–7.60), and elderly who were food insecure (OR = 0.59; 95% CI, 0.37–0.95) were significantly associated with undernutrition.
Conclusion:
The magnitude of undernutrition among the elderly is a public health issue. Independent predictors include educational status, morbidity, dietary diversity, and food insecurity. Intervention programs need to focus on the elderly’s nutrition, access to healthy foods, and other health issues.
Introduction
According to the World Health Organization, the elderly is defined as persons above 60 years. The number of elderly is projected to increase from 900 million to 2 billion between 2015 and 2050, going from 12% to 22% of the total global population. 1 Overall, in Africa, the life expectancy at birth has increased to approximately 65 years in 2015, this group accounts 3.5% (40 million) of the total population. 2
Malnutrition in the elderly is defined as a state of insufficient nutritional status; undernutrition is characterized by inadequate dietary intake, poor appetite, muscle wasting, and weight loss, adversely affecting physiological functions and clinical outcomes such as quality of life, infection rates and complications, muscle wasting, hospitalization outcomes and mortality rates.3–5
Malnutrition prevalence estimates vary substantially depending on the population considered, the healthcare setting, and the tool used for assessment. For example, over half (51.8%) of the elderly were at risk of malnutrition in sub-Saharan Africa, and 35.7% were malnourished. 6 On the other hand, more than a quarter (28.3 %) of the elderly in Ethiopia were malnourished, and 62.4 % were at risk of malnutrition. 7
Malnutrition is associated with reduced muscle function, bone mass, and cognitive function. In addition, malnutrition is often associated with anemia, immune system dysfunction, slow wound healing, and delayed surgery recovery, consequently increasing morbidity and mortality.4,8–10 Malnutrition is also linked with delayed disease recovery, resulting in more convalescent periods. Therefore, malnourished patients have significantly longer hospital stays with more infectious and non-infectious complications, an increased rate of unplanned readmissions, and higher health resource utilization in the outpatient setting. This results in an increased economic burden for the individuals and the healthcare system. 11 A recent prospective study in the elderly showed that adjusted healthcare costs were 714 € per year greater in malnutrition patients than in well-nourished patients, mainly due to hospital admission costs. 12
Most nutritional intervention programs are directed toward infants, young children, adolescents, and pregnant and lactating mothers. These dietary interventions often neglect the elderly, even with the proven benefits, including improved quality of life. A timely assessment of those at risk of malnutrition is essential for appropriate intervention to be taken. Having a database to assist with initiating vital programs and formulation of policies, evaluating nutritional status is necessary. 13
In Ethiopia, like other developing countries, most nutritional studies focus on children, particularly infants and preschool children, although elderly people appear to be equally affected. As a result, there are limited epidemiological data regarding the nutritional status of elderly individuals. Because of this, this study aimed to assess the magnitude of undernutrition and its associated factors among the elderly enrolled in the Public Servants Social Security Agency in Harar town.
Methods and Materials
Study setting and population
A cross-sectional study was conducted among the elderly population enrolled in the Ethiopian Public Servants Social Security Agency in Harar town from June to August 2020. Harar is the capital of Harari National Regional State, one of the regional states of the Federal Democratic Republic of Ethiopia. Harar is located 515 km east of Addis Ababa, the capital city of Ethiopia. The town had a projected total population of 203,438 (M:F = 102,369:101,069) in 2010.
Study participants were elderly individuals who collect their retirement pension payments monthly from the Public Servants Social Security Agency. The agency is a governmental organization that collects pension contributions from every government employer, which individuals receive monthly once they retire. Currently, 3000 (428 females and 2572 males) individuals are enrolled and receiving services from the Public Servants Social Security Agency Harar branch. This branch includes four districts (Hakim = 700, Abadir = 900, Aboker = 600, Shenkor = 800) 14 (Figure 1). Therefore, the study population included all elderly people enrolled in the Harar branch of the Public Servants Social Security Agency receiving services from one of the four districts. All study participants were living in home, not in a social/health care institution.

Map of the study area.
Inclusion and exclusion criteria
Participants >60 years of age were included. Those participants unable to respond and those on nutritional therapy were excluded from the study.
Sample size determination and sampling procedure
The single proportion formula (n = (z α/2)2 * p(1 − p)/d²)) was used to calculate the sample size, using a 95% confidence interval (CI), 5% margin of error, and 28.3% undernutrition prevalence among the elderly from a previous study in Hawassa. 7 Therefore, the final calculated sample size was 343, with addition 10% non-response rate. There were 2687 individuals eligible for the study (Hakim = 630, Abadir = 814, Aboker = 532, Shenkor = 711). The sample size (343) was proportionally allocated to the four sites based on the number of participants in each district. Next, computer-generated simple random sampling was used to select study participants from each site.
Data collection methods
Independent variables included socioeconomic data such as age, sex, religion, marital status, educational status, current employment status, monthly income, family size, farmland ownership; health and behavioral factors comprised of morbidity, taking medications, receiving support from others, currently smoking or using alcohol, currently chewing khat, physical activity; diet-related factors included food insecurity and dietary diversity.
A structured pretested questionnaire prepared by reviewing related literature,7,11,13,15,16 was administered through an interviewer to collect the socioeconomic data, dietary, behavior, and health-related factors.
The nutritional status was determined using the Mini Nutritional Assessment-Short Form (MNA-SF), 17 which has a maximum of 14 points, consisting of six questions on food intake, weight loss, mobility, psychological stress or acute disease, presence of dementia or depression, and body mass index (BMI). If the height or weight could not be assessed, the calf circumference was used instead of the BMI using an alternate scoring. MNA-SF scores of 12–14 were considered normal nutritional status (well-nourished); 8–11 indicated at risk of undernutrition, and 0–7 were undernutrition.
Anthropometric measurements (weight and height) were measured as part of the MNA-SF. Weight was recorded to the nearest 0.1 kg using an electronic weight scale with the participants in light dress and no shoes. Additionally, height was measured to the nearest 0.1 cm using a stadiometer with the participant standing vertical and looking straight ahead with heels, buttocks, and shoulders pressed against the stadiometer. BMI was calculated as the body weight in kilograms divided by the square of height in meters. If participants were unable to stand on the stadiometer, the demi-span measurement was measured from a distance between the midline of the sternal notch to the web between the middle and ring finger along the outstretched arm. Then height was calculated using the standard formula (female height in cm = (1.35 × demi-span in cm) + 60.1 and male height in cm = (1.40 × demi-span in cm) + 57.8). 20
Individual dietary diversity scores the previous 24 h were used to assess overall nutritional diversity. Food eaten by the respondents were classified into 12 food groups: cereals, oils/fats, sweets/sugar, legumes, white roots and tubers, fruits, vegetables, meat and meat products, milk and milk products, eggs, fish and seafood, spices, condiments, and beverages. An individual dietary diversity score was calculated by adding all food groups consumed over the previous 24 h. A high dietary diversity refers to respondents with a personal dietary diversity score greater than or equal to the mean individual dietary diversity score (⩾6 food groups). While a low dietary diversity refers to respondents with an individual nutritional diversity score below the mean individual dietary diversity score (<6 food groups). 18
The individual food insecurity status of the participants was assessed using the Household Food Insecurity Access Scale 19 developed by the Food and Nutrition Technical Assistance project, which was adapted to the individual level. It consisted of nine questions regarding food insecurity, with three possible responses including never, rarely, sometimes, or often and a total score of 27. Each of the questions were asked using a 4-week (30 days) recall period. First, the respondents were asked an occurrence question about whether the condition in the question happened at all in the past 4 weeks (yes or no). Then, if the respondent answered “yes” to the occurrence question, a frequency-of-occurrence question was asked to determine whether the condition happened rarely (once or twice), sometimes (3–10 times), or often (more than 10 times) during the preceding 4 weeks. Finally, the score was added and dichotomized into two categories: food insecure and food secure. Any participant was considered food insecure if they answered affirmative to two or more questions on the food insecurity scale. 19
The participants were classified as physically active when they reported regular aerobic exercise (walking, jogging) at least 30 min every 5 days or its equivalent, or if their occupation required physical force daily. 20
Data quality control
Data collectors and supervisors were trained for 2 days on data collection methods. Then, a pre-test was done on 5% of the study participants in Dire Dawa. Appropriate modifications were made to the questionnaire based on the pre-test results such as time modification, skipping pattern arrangement, wording, and phrases. The questionnaire was initially prepared in English, then translated to local languages, namely Amharic and Oromiffia, by different language experts to ensure the consistency of the questions before actual data collection. All of the anthropometric measurements were performed using standard procedures and calibrated equipment. The overall data collection processes were controlled and checked by the investigator.
Statistical analysis
Data were entered into Epi Data software version 3.1 and transferred to SPSS version 20 for analysis. Each completed questionnaire was checked for completeness and cleaned. Descriptive analysis, such as mean, standard deviation (SD), and proportion of the studied variables, was calculated. MNA-SF 12-14 points (normal nutritional status) was coded as “0,” 8–11 points (at risk of undernutrition) coded as “1” and ⩽7 points (undernutrition) coded as “2.”
A multi-collinearity test was performed to check the correlation between independent variables using collinearity statistics (variance inflation factors >5 was considered suggestive of multi-collinearity). Goodness of fit was checked using Hosmer–Lemeshow test; in addition, the assumption of proportional odds was checked. The nine variables (sex, marital status, educational status, whether received support from others, currently chewing khat, dietary diversity, food insecurity status, having morbidity, and currently on medication) that fulfilled the assumption of proportional odds and model fit were included in the ordinal logistic regression analysis. Next, the ordinal logistic regression analysis was performed to assess factors associated with nutritional status; those variables with a p value less than 0.05 were considered as statistically significant.
Results
Socioeconomic characteristics
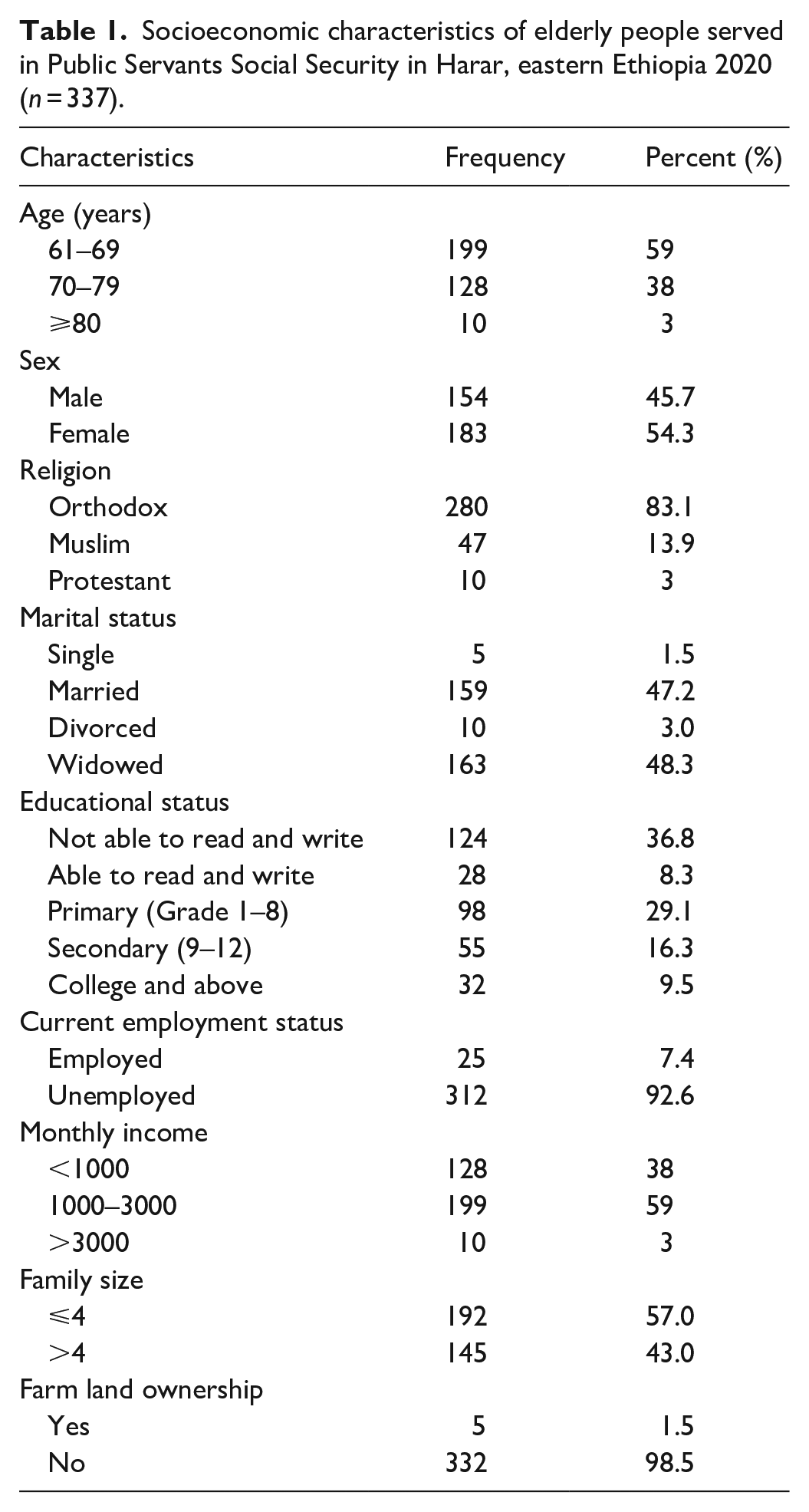
The study involved a total of 337 elderly individuals aged >60 years, which was a 98.3% response rate. The participants’ mean (±SD) age was 68.10 (±5.210) with a range of 61–82 years. In all, 199 (59.1%) elderly were between 61 and 69 years. Females account for more than half (54.3%) of the study subjects. The majority (83.1%) were Orthodox Christians. In total, 163 (48.4%) were widowed, 124 (36.8%) were unemployed, and 199 (59.1%) earned within the range of 1000–3000 birr per month (Table 1).
Socioeconomic characteristics of elderly people served in Public Servants Social Security in Harar, eastern Ethiopia 2020 (n = 337).
Behavior and diet-related factors
In all, 35 (10.4%) of the participants reported that they received support. All (100%) support was obtained from relatives, and financial support (100%) was the only type participants received. Among the participants, 20 (5.9%), were smokers; in addition, 91 (27%) used alcohol. In all, 109 (32.2%) were khat chewers. In all, 45 (13.4%) of the participants performed physical exercise. In total, 214 (63.5%) had a low dietary diversity score, and 243 (72.1%) were food insecure (Table 2).
Behavior, diet, and health-related factors of the elderly people served in Public Servants Social Security Agency in Harar, eastern Ethiopia 2020 (n = 337).

Health-related factor
In all, 213 (63.2%) of the participants had a chronic disease. Among them, 56 (26.3%), 40 (18.8%), and 26 (12.2%) had hypertension, gastritis, and diabetes mellitus, respectively (Figure 2). Among the total participants, 177(52.5%) were taking medications; the mean pill burden was 2.3, with a minimum of one and a maximum of six pills.

Types of morbidities among elderly people served in Public Servants Social Security Agency 2020.
Nutritional status
The magnitude of undernutrition among the elderly in the present study area determined by the mini nutritional assessment was 16.6%. About 45.1% were at risk of undernutrition, and 38.3% were normal.
Factors associated with undernutrition
Nine variables (sex, marital status, educational status, receiving support from others, currently chewing khat, dietary diversity, food insecurity, having a chronic illness, and currently taking medication) fulfilled the assumption of proportional odds and fit of the model were included in ordinal logistic regression analysis. Finally, educational status, dietary diversity, food insecurity, and having chronic illness were independent predictors of undernutrition.
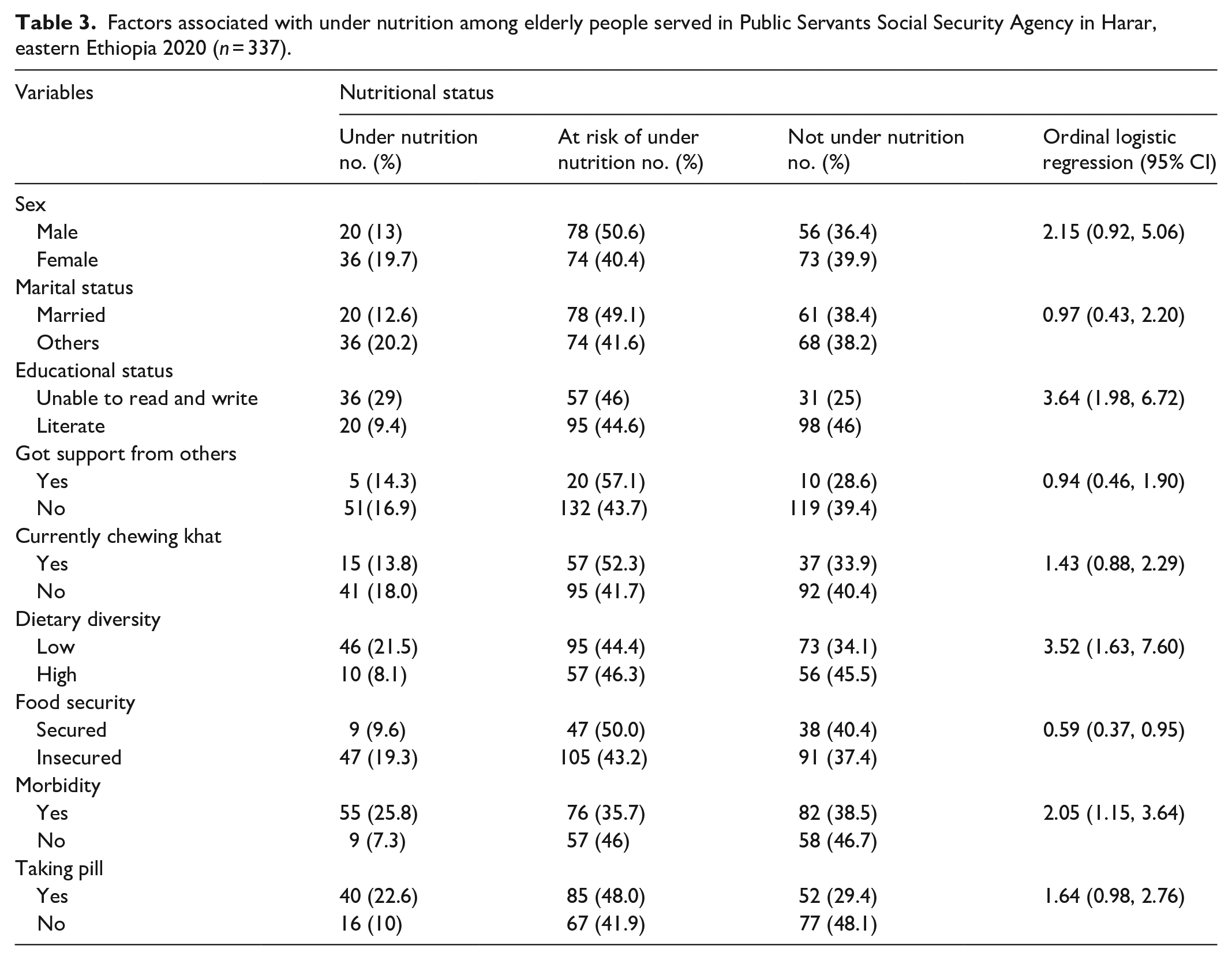
Those participants unable to read and write were 3.6 times more likely to be undernourished compared to those who were literate (odds ratio (OR) = 3.64; 95% CI, 1.98–6.72). Older adults with low dietary diversity scores were 3.5 times more likely to be undernourished when compared to those with high dietary diversity scores (OR = 3.52; 95% CI, 1.63–7.60). Those elderly who were food secure were 41% less likely to be undernourished when compared to those who were food insecure (OR = 0.59; 95% CI, 0.37–0.95). The elderly with morbidities were two times more likely to be undernourished than those with no chronic illnesses (OR = 2.05; 95% CI, 1.15–3.64) (Table 3).
Factors associated with under nutrition among elderly people served in Public Servants Social Security Agency in Harar, eastern Ethiopia 2020 (n = 337).
Discussion
The overall undernutrition prevalence among elderly individuals in this study was 16.6%. In addition, nearly half (45.1%) of study participants were at risk of developing undernutrition. Being illiterate, low dietary diversity, food insecurity, and elderly with morbidities were independent predictors of undernutrition.
The prevalence of undernutrition in the study area was 16.6%. A similar finding was reported in Kamrup District, India (15%), 13 South-Central Nepal (19.8%), 21 and Sodo Zuriya District, Ethiopia (17.1%). 15 However, the extent of undernutrition in our study was less than what was reported from similar studies in Nepal (24.8%), 22 Lagos State, Nigeria (35.7%), 6 Gondar town, Northwest Ethiopia (21.9%), 16 Hawassa City, Southern Ethiopia (28.3%), 7 and Debre Markos Town, Northwest Ethiopia (22.7%) 11 ; however, higher than studies reported in Pakistan (5.53%) 23 and Malaysia (7.3%). 24 The differences may be due to variations in study subjects. In this study, participants included elderly individuals receiving a pension; however, the other studies included elderly individuals in the community and the nursing home. In addition, there may be socioeconomic and health-related differences, such as illness and medications.
Educational status was significantly associated with undernutrition. In this study, participants unable to read and write were 3.6 times more likely to be undernourished compared to those who were literate. This is similar to other reported studies in the aging population in Northwest Ethiopia 16 and Sodo Zuriya District Wolaita zone, Ethiopia. 15 Education is an essential factor in improving health status; educated individuals develop habits, skills, resources, and the ability to achieve a better life, 24 increasing the likelihood of better feeding practices and nutrition.
Dietary diversity was found to be significantly associated with undernutrition. According to this study, older adults with a low dietary diversity score were 3.5 times more likely to be undernourished when compared to those with a high dietary diversity score. This result is comparable to the study performed in Gondar town, Northwest Ethiopia. 16 This might be due to low calories and protein content of less diversified foods as compared to high diversified foods.
The present study revealed more than two-thirds of the elderly were food insecure; food insecurity is an independent predictor of undernutrition among the elderly. The elderly who were food secure were 41% less likely to be undernourished than those who were food insecure. The studies in Malaysia 24 and Aykel Town Administration, Amhara Regional State, Northwest Ethiopia, 25 reported similar findings. Food insecurity is linked to low income, low educational status, social isolation, living alone, and functional impairments. 24 This could ultimately result in limited access to adequate quantity and quality of foods, resulting in adverse nutritional outcomes among elderly individuals.
The elderly with chronic illness were two times more likely to be undernourished compared to their healthy counterparts. A study in Nigeria reported similar findings. 6 This could be explained by the following: chronic illnesses of the gastrointestinal system are often related to poor food intake and nutrient malabsorption; side effects, such as anorexia, nausea, dry mouth, and constipation, from medications used to treat chronic illnesses, can result in malnutrition 26 ; the cost of treatment for chronic diseases often competes with the money needed for food. The other reason could be chronic illnesses, such as diabetes, hypertension, heart disease, treated with dietary restrictions that affect food intake. Since sugar, salt, and fat contribute to the food taste, dietary restrictions may make food unpalatable, reducing food intake.
Limitation of the study
The design used in this study may not show a causal relationship between predictor and outcome variables. Dietary diversity score and food security were assessed employing a 24-h and 30-day recall, respectively. Since the accuracy of both the tools largely depends on the respondent’s memory, they are subject to errors and biases. Additional limitations of this study include the study’s findings cannot be generalized for all elderly, those who are not enrolled in the Public Servants Social Security Agency.
Conclusion
The study revealed the magnitude of undernutrition among elderly individuals was lower than most studies carried out in Ethiopia: however, it is still a public health issue. In addition, it was found that educational status, dietary diversity, food insecurity, and having chronic illness were independent predictors of undernutrition among the older population.
Therefore, intervention programs supported by government and non-governmental organizations in this area should consider prevention, early detection and treatment of comorbid illness, and economic empowerment to increase access to diversified foods and improve food insecurity. Lastly, educating this population on healthy eating would minimize nutritional problems. Further research, including the possible unaddressed factors of undernutrition in the present study, is also recommended.
Supplemental Material
sj-docx-1-smo-10.1177_20503121221108615 – Supplemental material for Undernutrition and associated factors among elderly people served in Public Servants Social Security Agency in Harar, Eastern Ethiopia
Supplemental material, sj-docx-1-smo-10.1177_20503121221108615 for Undernutrition and associated factors among elderly people served in Public Servants Social Security Agency in Harar, Eastern Ethiopia by Gizeshwork Mulugeta, Tariku Dingeta, Habtamu Mitiku and Fitsum Weldegebreal in SAGE Open Medicine
Footnotes
Acknowledgements
We would like to acknowledge all study participants for providing information and the data collectors for their patience during the data collection process. We would also like to acknowledge the Institutional Health Research Ethics Review Committee (IHRERC) of Haramaya University for enabling us to have ethical clearance. Our deepest gratitude goes to Dr. Tara Wilfong (MD, MPH) who thoroughly edited the language of this manuscript.
Author contributions
GM contribute to the inception of idea, proposal development, data collection, analysis, interpretation, and final write up and also writing the manuscript. TD, HM, and FW designed the work, edited the proposal and critical review of the manuscript. All authors read and approved the final manuscript.
Availability of data
The authors declare that all the necessary data are fully described within the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval for this study was obtained from the Institutional Health Research Ethics Review Committee of Haramaya University (Ref. No. IHRERC/103/2020).
Informed consent
Written informed consent was obtained from all subjects before the study. Those study participants who were unable to read and write, the participants information sheet and informed voluntary consent form was read by the data collectors and then the participant finger print signatures were obtained.
Trial registration
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
