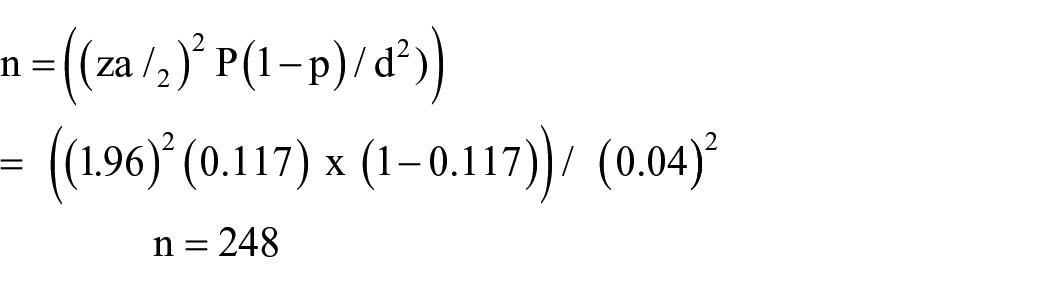Abstract
Objective:
This study aimed to assess the prevalence and associated factors of depressive symptoms among adults attending anti-retroviral therapy follow up at Debre Markos Comprehensive Specialized Hospital.
Methods:
Institution-based cross-sectional study was conducted, and a systematic sampling technique was used to select the 266 participants. Depressive symptoms were assessed by using patient health questionnaire 9. A binary logistic regression analysis with an odds ratio and a 95% confidence interval was used to assess the strength of associations in SPSS version 20 and a p-value < 0.05 was considered as statistically significant.
Results:
In this study, the prevalence of depressive symptoms among HIV-positive individuals was 39.1% with 95% confidence interval (33.7%–45.3%). Multivariable analysis showed that participants who had age group > 40 (adjusted odds ratio = 5.26, 95% confidence interval (2.24–12.35)), presence of perceived stigma and discrimination (adjusted odds ratio = 7.5, 95% confidence interval = (3.77–14.9)), poor medication adherence (adjusted odds ratio = 6.05, 95% confidence interval = (2.86–12.80)), and poor social support (adjusted odds ratio = 2.53, 95% confidence interval = (1.25–5.12)) were significantly associated with depression.
Conclusion:
The prevalence of depressive symptoms in this study was found to be significantly high. Age > 40 years old, the presence of perceived stigma and discrimination, poor medication adherence, and a lack of social support were found to be associated factors of depressive symptoms. It would be better for clinicians to give special emphasis to those patients who were stigmatized, who had compliance problems, and poor social support.
Introduction
Depression is the foremost psychiatric problem related to HIV disease. Various findings stated that people living with HIV had twice more risk for depression than those who were at risk of HIV but were not truly infected. 1 In the context of HIV, depression is a frequently unnoticed but possibly hazardous condition that can affect not only quality of life, relationship, employment, and adherence to medical care, but also possibly survival. 2
Various studies have revealed the global prevalence of depression among HIV-positive people across the world and in Africa. Studies report prevalence ranging between 12% and 60%. 3 According to a systematic review and meta-analysis study, the global prevalence rate of depression in HIV/AIDS patients was 31%, 4 and a systematic review and meta-analysis study conducted in Sub-Saharan Africa found that the pooled prevalence of depressive symptoms in untreated or mixed groups of PLHIV was 19%, and the pooled prevalence of depressive symptoms in PLHIV on anti-retroviral therapy (ART) was 12%. 5 Another meta-analysis study found that 15.3% of HIV-infected people had major depressive disorder in sub-Saharan Africa when assessed using a diagnostic interview. 6 A comprehensive review and meta-analysis study conducted in Ethiopia discovered that the total pooled estimated prevalence of depression in PLWHIV was 36.65%. 7
There are a number of associated factors with depression in PLHIV. These contributing factors were age, gender, marital status, low income, clinical stage, primary care giver type, maternal death, change in care giver type, and death in the family.7–10 Medication adherence, HIV related stigma, and a lack of social support were also identified as major risk factors for depression in this population.11–13
Depression damagingly influences the HIV disease prognosis. It reduces CD4 T-lymphocyte activity, increases viral load, and influences quality of life and drug adherence, which leads to a greater risk of mortality. 6 Depression has also been linked with great risk behaviors, including early sexual initiation, poor condom use, substance abuse, multiple sexual partners, and unplanned pregnancy.14–17 The combination of these problems resulted in treatment resistance, deteriorating medical outcomes, high risk of suicide, overutilization of medical resources, and increased illness and death.
Even though affective disorders, including depression, are vastly prevalent among PLWHA worldwide and in the nation, there are some studies which address the magnitude of depression in this population in Ethiopia, in which most of them were done a long time ago and reported with different and inconsistent findings with variability in measurements. As the quality of ART services and approaches to counseling are changing frequently, ART guidelines are updated accordingly. Assessing the magnitude of depressive symptoms and identifying associated factors will bring updated data on the area and could be used as input for intervention. This study attempts to address previous studies’ limitations by including important variables and employing standard measurements. The coexistence of these disorders is associated with treatment barriers such as treatment resistance, worsening medical outcomes, an increased risk of suicide, a greater likelihood of frequent use of medical resources, and increased morbidity and mortality. As a result, the study’s findings would contribute to bridging the gap in formulating necessary solutions by assessing the magnitude and associated factors of depression among HIV positive patients. While low- and middle-income countries face more than 90% of the burden of HIV/AIDS, there is no adequate knowledge about the link between HIV/AIDS and mental health in these countries, according to a World Health Organization report on HIV/AIDS and mental disease (WHO, 2008). The study’s findings may also influence the development of appropriate policies, plans, and intervention programs for the management of psychiatric illnesses in HIV/AIDS care settings. This, in turn, may improve the quality of life for HIV/AIDS patients who are also depressed.
Methods
Study area and period
The study was conducted in Debre Markos Comprehensive specialized hospital, East Gojjam, Amhara Region, which is located in the northwestern part of Ethiopia. Debre Markos Town is located in the East Gojjam Zone of Amhara Regional State, 265 km from Bahirdar and 300 km from the capital city of Ethiopia, Addis Ababa. Administratively, based on the 2007 Census conducted by the Central Statistical Agency of Ethiopia (CSA), Debre Markos Town has an estimated total population of 61,025.
Debre Markos Comprehensive Hospital is the only comprehensive hospital in East Gojjam and it serves for more than two million people. It provides care and treatment to around 3800 PLWHA from various places, of whom 3255 people are of reproductive age group and 545 are pediatric (< 15 age group). The hospital has a separate clinic that provides care and treatment for HIV/AIDS patients with daily visits ranging from 40 to 60. The total average monthly visit is 1200-1600 patients. An institutional-based cross-sectional study design was conducted from 25 April to 25 May 2019.
Source population and study population
Source population
All HIV positive individuals received treatment at the ART clinic of Debre Markos Comprehensive Specialized Hospital.
Study population
All HIV positive individuals who were attending ART follow up at Debre Markos Comprehensive Specialized Hospital and available during the time of data collection.
Inclusion and exclusion criteria
All HIV positive individuals aged 18 years old and above who were on ART treatment were included, but patients who were seriously ill and unable to give interview were excluded.
Sample size determination
Sample size is determined by using a single population proportion formula using a previous study conducted in Ethiopia revealed that the proportion of depression living with HIV would be 11.8%, 18 with an expected margin of error (d) of 4% just to maximize the sample size and improve the precision of the study given the cost and time, 95% confidence interval and non-response rate of 10%.
Then adding the non-response rate 10% = 25, 248 + 25 = 273
Where; n = required sample size, z a/2 = 1.96 and d = marginal error.
Sampling technique
For adult follow-up ART services, the hospital had two ART OPDs, OPD 5 and OPD 6. The systematic random sampling technique was used to draw a representative sample from a population by determining a sampling interval K, 3 and then the lottery method was used to randomly select a sample between 1 and k, 3 and every third participant was subsequently interviewed.
Measurements
PHQ-9 was used to measure the depression level of HIV/AIDS patients, which is a 9 items depression screening and diagnostic questionnaire for MDD based on DSM-V criteria. The PHQ 9 appears to be a reliable and valid instrument that is used to diagnose major depressive disorders among patients. 19 Participants rate depression according to the particular problem that had bothered them for the last two weeks. Scores ranged from 0-4 non-depression, 5-9 Mild depression, 10-14 Moderate depression,15-19 Moderately severe depression, and 20-27 Severe depression. For this study, depression is defined by a PHQ 9 score of ⩾ 5. PHQ-9 validation was conducted in attendees of primary care out-patient clinics in a predominantly rural area, and PHQ-9 had a sensitivity of 0.83 and specificity a of 0.75 for detection of major depressive disorder (MDD) at a cut-off value of five or more. 20 Social support was measured by the Osslo-3 items social support scale. The sum of support measures ranged from 3 to 14 and was operationalized into 3 broad categories of social support, as 3-8 poor social support, 9-11 moderate social support, 12-14 strong social support. 21 Drug adherence was measured by the 8 item Morisky medication adherence scale, and patients’ scores above 2 were considered as low adherence, 1 or 2 as medium adherence, and 0 was considered as high adherence. 22 CD4 count was classified based on CDC classification as 500,200–499 and 200 cells/µL. 23
Data collection
Both chart review and structured interview administered questionnaires were used to collect data by four trained clinical nurse data collectors using the Amharic version of the questionnaire, and they were supervised by two BSc psychiatry nurses. The questionnaire was developed in English and translated into the local language (Amharic) and translated back to English to maintain consistency prior to the actual data collection.
Statistical analysis
The coded data was checked, cleaned, and entered into Epi.data version 4.2 and then exported into SPSS version 24 for analysis. Frequencies, proportions, graphs, and cross tabs were used to present the descriptive results of the study. First, the PHQ-9 depression measurement scale was computed and recoded to get the prevalence. Binary logistic regression was performed to assess the association between binary outcomes with different explanatory variables. Bivariable analysis was first conducted for each potentially explanatory variable. Variables that satisfied p-value < 0.25 were selected for multivariable analysis. The strength of the association was interpreted using the odds ratio and 95% confidence interval. A p-value < 0.05 was considered statistically significant in the multivariable analysis of this study. The total value of the variance inflation factor in the final model was less than 10, thus there was no problem of multicollinearity and the model fitness was checked by using the Hosmer and Lemeshow test resulted in a p-value of 0.27.
Data quality assurance
Data quality control issues were addressed by conducting a pre-test among 5% of total samples obtained from patients attending at Debre Markos Health Centre, one of the health centers located in the town that provides care and treatment for patients with HIV/AIDS. Training was given to data collectors on the data collection tool and the ethics of confidentiality. Supervision was performed regularly during the data collection period. The collected data was checked on a daily basis for completeness and consistency. The questionnaires were translated to Amharic and back to English using backward forward translation.
Ethical consideration
Ethical clearance was obtained from the Ethical Review committee of Debre Markos University, College of Health Science with reference number of HSC/R/C/Ser/Co/204/11/12. The data collected for the purpose of this study did not include identification to ensure secrecy of participants and confidentiality was secured. The outline of the purpose of the study was explained, and written consent was obtained from participants.
Results
Socio-demographic characteristics of respondents
A total of 266 study participants were interviewed, giving a response rate of 97.4%. About 164 (61.7%) were female and 97 (36.5%) of the clients were in the age category of > 40 years old, followed by the age category of 31-40 (33.8%) years old. Around three-quarters of the participants were urban dwellers, with 62 (23.3%) of the participants being self-employed and 92 (34.6%) having a monthly income of 500–1000 Ethiopian Birr. More than half of the client’s 247 (92.9%) were Orthodox by religion, and most of the respondents were married 132 (49.6%) and regarding the education level of the respondents, 117 (44%) were unable to read and write, and 265 (99.6%) were Amhara in their ethnicity (Table 1).
Demographic and socio-economic characteristics of people living with HIV on ART program, in Debre Markos comprehensive specialized hospital, Ethiopia, 2019 (n = 266).

Others for occupation refer, merchant, students and unemployed participants.
Clinical and psychosocial characteristics of respondents
Out of the total respondents, the majority 204 (76.7%) were on WHO stage I and 109 (41%) were encountered stigma and discrimination. About 197 (74.1%) had good adherence to their medications and 169 (63.5%) had good social support. Coffee was consumed by 83 (63.8%) participants and 169 (63.5%) had good social support (Table 2).
Clinical, psychosocial and related characteristics of HIV positive clients attending ART follow up at Debre Markos comprehensive specialized hospital, Ethiopia 2019 (n = 266).

In the variable type of substance used: others refer to “shisha” and other illicit substances. Others in living condition: those with living with relatives
Prevalence of depressive symptoms
The prevalence of depressive symptoms was assessed using PHQ-9. Based on the cut of point ⩾ 5, the prevalence of depressive symptoms was found to be 104 (39.1%) with a 95% CI (33.7%–45.3%).
Factors associated with depressive symptoms among PLHA
Bivariable analysis indicated that socio demographic variables (age, residence, marital status, and occupation), clinical variables (CD4 count), and psychosocial factors (living condition, stigma and discrimination, adherence, social support, and ever use of substances) were scored with a p-value < 0.25. In the multivariate model analysis age group of > 40 years old, the presence of stigma and discrimination, poor drug adherence, and poor social support were statistically significant with depressive symptoms.
Patients whose age was > 40 were 5 times more likely to have depressive symptoms as compared to those whose age was 18-30 (AOR = 5.26, 95% CI = (2.24–12.35)). Those patients who had perceived stigma and discrimination were 7.5 times more likely to have depressive symptoms than those who did not have stigma and discrimination (AOR = 7.5, 95% CI = (3.77–14.9)).
Regarding drug adherence, patients who were non-adherent to ART (AOR = 6.05, 95% CI = (2.86–12.80)) had 6 times more depressive symptoms as compared to their adherent counterparts. Symptoms of depression were 2.5 times more likely to occur among those who have poor social support (AOR = 2.53, 95% CI = (1.25–5.12)) as compared to those who have good social support (Table 3).
Bivariate and multivariate analysis between socio demographic and clinical variables with depressive symptoms among people living with HIV on ART program in Debre Markos comprehensive specialized hospital, Ethiopia, 2019 (N = 266).

AOR: adjusted odds ratio; COR: crude odds ratio.
Others in living condition refer those with living with relatives. Others in occupation refer merchant, students and unemployed participants.
Indicates p-value < 0.05.
Discussion
The present study was conducted to address two research objectives. The first objective was to estimate the prevalence of depressive symptoms among HIV positive individuals in DMRH. The second objective was to identify the factors associated with depressive symptoms among PLHIA in DMRH.
The result of this study indicated that the overall prevalence of depressive symptoms was relatively high. Since the progress of HIV/AIDS has been interrelated with a greater risk of upcoming depressing experiences and countless long-term morbidities, these findings may affect the long-term health of patients attending in DMRH.
The prevalence of depression among the 266 participants of this study was found to be 39.1% with a 95% CI (33.7%–45.3%) measured through the PHQ-9 depression measurement scale. Symptoms of depression were significantly associated with factors such as participants’ age > 40 years old, the presence of perceived stigma and discrimination, poor medication adherence, and poor social support.
In this study, the prevalence of depressive symptoms among the participants was found to be 39.1% with a 95% CI (33.7%–45.3%) which is in line with studies conducted in Debre Birhan referral hospital (38.9%), 25 Zewditu hospital (44.4%), 26 Tigray region (41.2%) 27 and Alert hospital (41.2%). 28 But it is relatively low as compared to studies conducted in Harar (45.8%), 29 and 63.1% in Khartoum, Sudan. 30 In addition, this result is also higher than the studies done in Dilla (11.2%), 31 in South Africa (25.9%) 32 and Ghana (5.4%) 33 (these studies used different depression measurements and sample size). The reason for this discrepancy might be attributable to several factors, including the type of population being studied, the study periods, the depression screening instruments difference, and the sample size used. The difference might also due to social, cultural, and geographic differences and recalling bias during data collection and methodology. In inferring the results of this study, it is important to remind that the vast majority of participants were evaluated through self-reported inventories that measured depressive symptoms rather than gold-standard screening clinical interviews for most depressive disorder. In addition, even if each self-reported measure of depressive symptoms has limitations, there is an indication that the lack of anonymity in formal screening assessments may compromise precise assessment of sensitive personal information such as depressive symptoms.
Regarding to associated factors in this study, age > 40-year-old were five times more likely to have depressive symptoms than people between the ages 18 and 30. This might be due to physical health problems, functional disability, and chronic pain, which can make an older adult more susceptible to developing depression. 34 However, this result is not consistent with the study in Zewditu Memorial Hospital in which 18-24 years old were more depressed. 26 This variation could be due to increased fear of stigma, deteriorating health conditions, but this result is consistent with a study done at Debre Berhan Hospital. 25
This study also revealed that respondents having a history of perceived stigma and discrimination were 7.5 times more likely to have depressive symptoms than those with no history of perceived stigma and discrimination. This result is supported by a study done in Uganda 2 and Debre Birhan. 25 This reflects negative attitudes toward PLWHA in the community that exposed the patients to be depressed.
In addition, medication adherence was also significantly associated with symptoms of depression; participants with poor medication adherence were six times more likely to experience depressive symptoms compared to participants with good medication adherence. This might be due to HIV increases the risk of developing depression through a variety of mechanisms including: direct injury to subcortical areas of the brain; chronic stress; stigmatization; worsening social isolation; bereavement; debilitation; and intense demoralization. So, a long-term viral suppression requires consistent and high percentage adherence that reduce the risk of having depression. 35 This is consistent with a study done at Alert Hospital. 28
This study also revealed that participants with poor social support were 2.5 times more likely to have depressive symptoms compared to encounter groups. This is consistent with a study done in Uganda. 36 This might also be due to decreased social support within the context of HIV/AIDS, related to increased depression because of various factors such as educational disability, food insecurity, isolation, and debilitation. Low social support could result in poor adherence to medication, and as a result, poor adherence leads to immune suppression, which finally leads to depression.12,37
Limitation of the study
The interpretation of the findings of this study should consider the following potential limitations: First, the cross-sectional nature of this study may limit the causal and effect interpretation of the factors observed. Therefore, the data collected might not be as accurate as it might be due to recall bias from participants. Second, since the study was institutional-based, it might not generalize to the total population of people living with HIV in the region. This study also didn’t consider power analysis for sample size calculation.
Conclusion
The prevalence of depressive symptoms among adult patients with HIV/AIDS on ART was found to be relatively high, and it is still a public mental health problem in DMRH. Age group > 40 years old, presence of perceived stigma and discrimination, non adherence to ART, and lack of social support were found to be significantly associated with symptoms depression among adults with HIV/AIDS attending ART clinic. Therefore, based on the above findings, the investigators recommended the following points to health providers: to link those patients who are aged to experts for care and support services; and, to give health education on medication adherence extensively and to give concern to mental health along with medical illness. The Ministry of Health and other stakeholders should develop guidelines to screen and treat depression among HIV/AIDS patients and develop programs on counseling and close follow-up of adherence to ART. Further research on risk factors for depression should be conducted to strengthen and broaden these findings.
Supplemental Material
sj-docx-1-smoo-10.1177_20503121221100992 – Supplemental material for Depressive symptoms and associated factors among adults attending antiretroviral therapy clinic in Debre Markos comprehensive specialized hospital, Amhara, Ethiopia
Supplemental material, sj-docx-1-smoo-10.1177_20503121221100992 for Depressive symptoms and associated factors among adults attending antiretroviral therapy clinic in Debre Markos comprehensive specialized hospital, Amhara, Ethiopia by Haile Amha, Bethlehem Denekew and Sintayehu Asnakew in SAGE Open Medicine
Footnotes
Acknowledgements
The authors would like to give deepest gratefulness to the data collectors, supervisor and study participants for devoting their time to be part of the study. We also like to acknowledge Debremarkos referral hospital administrative office and ART follow-up patients for giving all information to us.
Availability of data and materials
All the data are available from the corresponding author up on a reasonable request.
Contributors
H.A. developed the proposal, supervised the data collection, analyzed the data, and wrote the draft manuscript. B.D., G.D., B.M., S.A., and M.G. revised the proposal, checked the data analyze, revise and approve the manuscript.
Data sharing statement
No additional data is available for this study; all the data are included in the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Ethical clearance was obtained from Ethical Review committee of Debre Markos University, college of Health Science with reference number of HSC/R/C/Ser/Co/204/11/12. Those people who have no willing to participate in the study were not forced to participate. Written consent was obtained from each study participants. The study participants were also provided with information about the objectives and expected outcomes of the study. Information obtained from individual participants was kept secure and confidential.
Informed consent
Written consent was obtained from participants and an outline of the purpose of the study explained with each client who agreed to participate voluntarily. Confidentiality was secured.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.