Abstract
Background
There is insufficient evidence to indicate using opioids in the management of chronic non-cancer pain (CNCP), yet ongoing prescribing is prevalent and remains a global public health matter. Inappropriate long-term prescribing of opioids is associated with side effects and adverse events. This article explores the significant barriers and enablers during opioid management indicated for CNCP within general practice, in the United Kingdom, and proposes recommendations to optimise practice.
Methods
A systematic literature review of the databases MEDLINE, EMBASE, CINAHL, Web of Science and Science Direct were searched. Titles, abstracts and full texts were screened against inclusion and exclusion criteria. Papers were evaluated using the Critical Appraisal Skills Programme qualitative appraisal tool.
Results
From 1027 citations, 6 papers were included (n practitioners = 168 and n patients = 52). Four key themes were identified: three barriers and one enabler. Barriers: general practice healthcare model constraints, relationships in primary care and attitudes towards CNCP management. Enabler: multidisciplinary team set up.
Conclusion
A change in culture from both service providers and service users is required to fully embrace the multidisciplinary team observed in general practice. Movement away from the traditional model of doctor led management needs to occur. Future policies need to prioritise reducing the long waiting times observed for specialist pain services. Non-pharmacological opportunities and services should also be developed to support patients.
Introduction
Chronic non-cancer pain (CNCP) is defined as pain lasting for more than 3 months that is unrelated to a cancer diagnosis. 1 The International Association for the Study of Pain describes pain as ‘an unpleasant sensory and emotional experience associated with actual or potential tissue damage’. 2 There is insufficient evidence to justify the use of opioids in the management of CNCP. Despite this, in the United Kingdom (UK), the prescribing of opioids for CNCP has progressively increased in the last 20 years. 3 Within the community setting in England, opioid prescribing for a minimum of 3 months has increased by 54% between 2015 and 2021. 4
Inappropriate long-term prescribing of opioids is associated with side effects including constipation, dizziness, sedation, nausea, dependence and addiction. 5 Moreover, although rare, significant immune and endocrine system disturbances, including osteoporosis, have been observed.6,7 Adverse events including falls, hospital admissions and opioid related death are also prevalent. 8 Opioids contribute to nearly half of drug-related deaths. In 2022, there were 2261 opioid related deaths within England and Wales, 1.9% higher from 2021. 9
Evidence supports the use of opioids in the management of acute pain, following a surgical intervention, cancer related pain and end of life pain. In England the bulk of repeat opioid prescribing occurs from primary care settings, contributing to high opioid prescribing rates. 10 English prescribing data between 2017 and 2018 showed that 5.6 million people, 13% of the population, had dispensed a prescription for an opioid medicine. 11
A significant financial investment supports the enhancement of the primary care structure. 12 Formation of Primary Care Networks (PCNs) in 2019 has seen a multidisciplinary team (MDT) approach at primary care level, increasing the presence of pharmacy professionals, occupational therapists and physiotherapists to name a few. PCN’s aim to increase access to healthcare, support capacity and meet the needs of the community. 13
This qualitative meta-synthesis aims to explore the current barriers and enablers encountered in the management of opioids for CNCP within the UK general practice setting. This review addresses the experiences of both clinicians and patients’ perspectives. Additionally, proposing recommendations to optimise opioids prescribed for CNCP.
Methods
This study was conducted in the form of a meta-synthesis qualitative systematic review. Reporting followed Preferred Reporting Items for Systematic review and Meta-Analysis (PRISMA) guidelines.
Search terms and synonyms.

A systematic search was conducted by one reviewer using the published literature databases MEDLINE, EMBASE, CINAHL, Web of Science and Science Direct between 1st December 2023 and 31st January 2024.
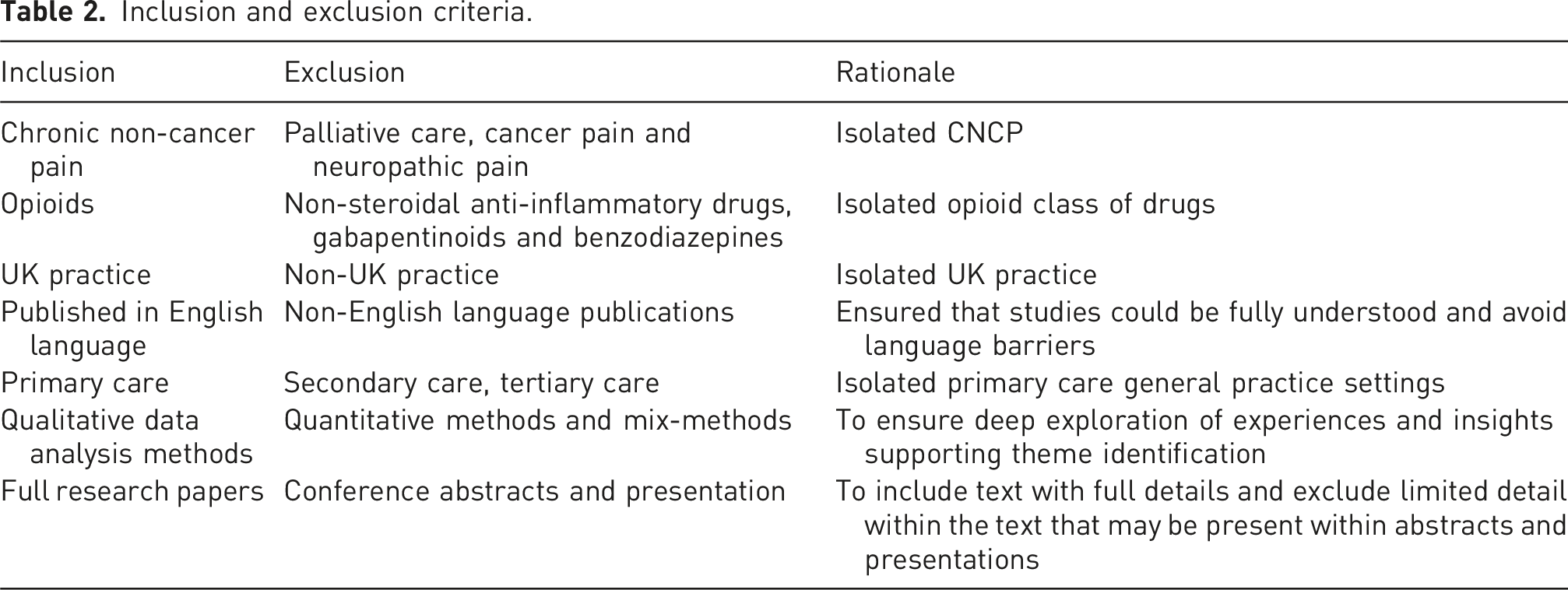
Inclusion and exclusion criteria.
The Critical Appraisal Skills Programme (CASP) qualitative appraisal tool was developed to support with appraising health-related research. CASP is endorsed by Cochrane and the World Health Organization and is used for health and social care qualitative synthesis.14,15 It uses a simple method of 10 questions to evaluate and critique on significance of results. 16 Each study was critically appraised using CASP.
Braun et al.’s 17 thematic analysis was employed from the start of synthesis and throughout the review. This analysis enabled the key topics to be identified and supported with ‘exploring, interpreting and reporting relevant patterns of meaning’. 17 Six phases were used to analyse the data including coding and theme generation. See Appendix 1.
Ethical approval and risk of bias
Ethical approval was not required. A sole researcher working in primary care carried out the review and unconscious notion of bias must be acknowledged. Reflexivity and the individuals’ preconceptions that impact on the decisions made during research influences subsequent credibility. Positively, an understanding of the general practice processes provides a valuable insider perspective. However, personal experience of supporting with opioid management can result in interpretivism. Therefore, as the sole researcher, it is important to aim for transparency. Rigour supports the management of any bias and enables auditability. This was maintained through adherence to strict inclusion and exclusion criteria as previously discussed in Table 2.
Results
The search retrieved 1027 papers after removing duplicates, and all papers had their titles and abstracts screened. Following screening of titles and full text, 6 papers were eligible to be included in analysis (Figure 1). PRISMA flow chart illustrating the results of search strategy.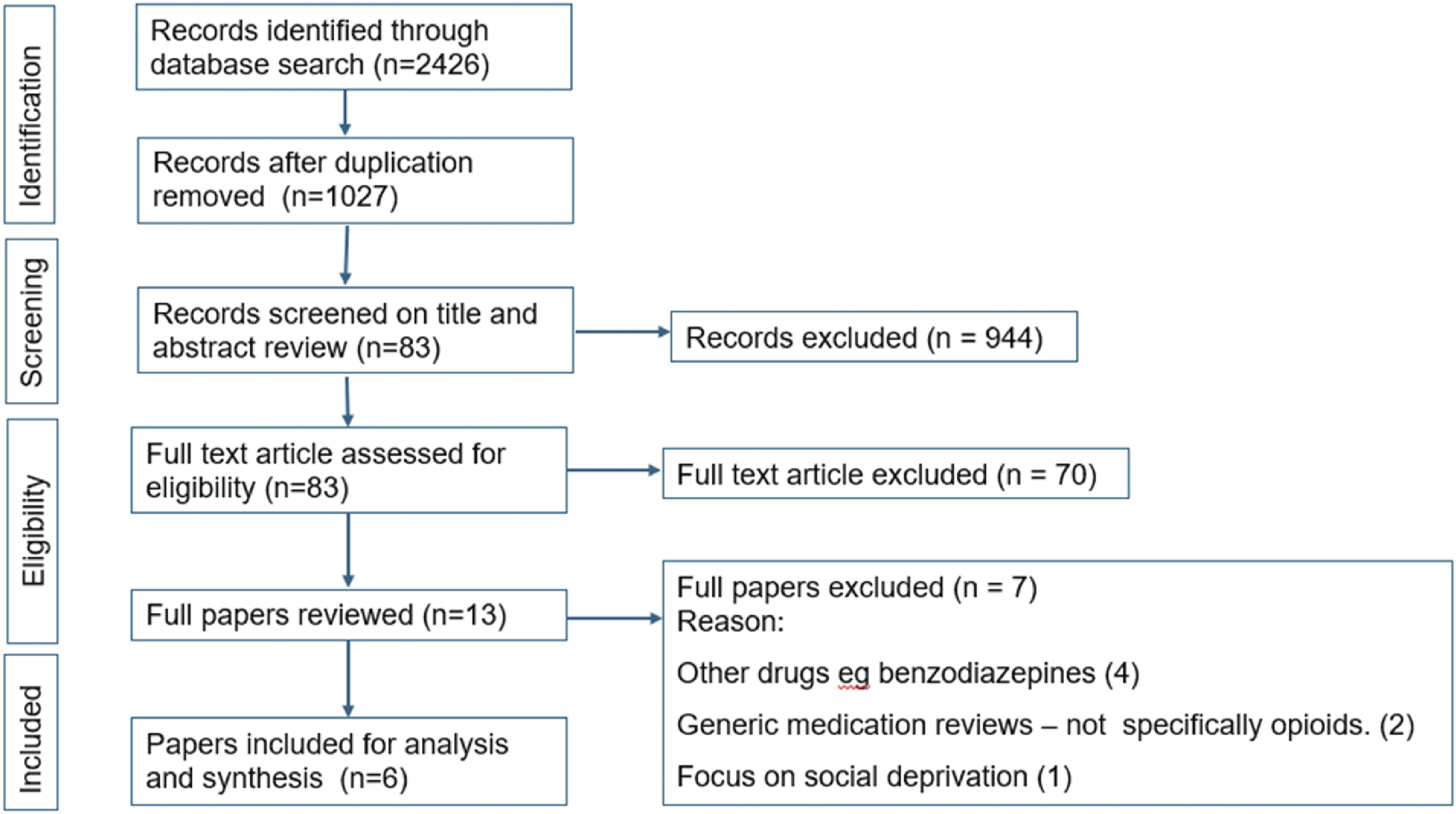
Study characteristics
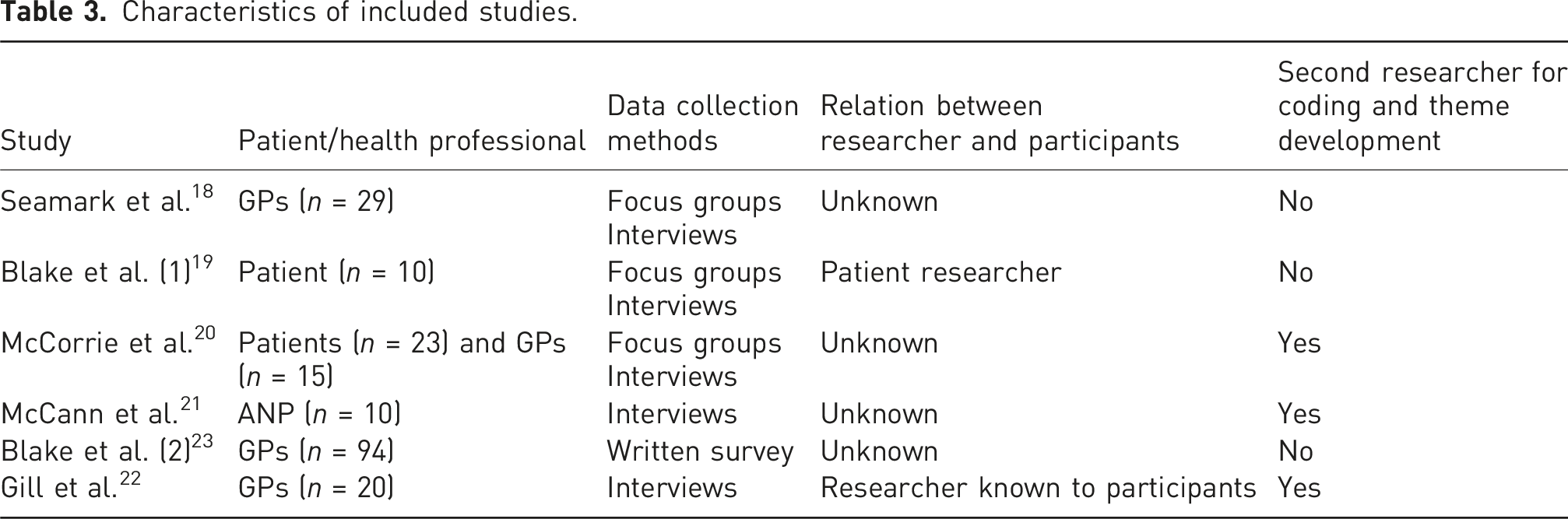
Characteristics of included studies.
Quality assessment
All studies demonstrated rigorous design, recruitment, data collection and analysis methods, therefore presenting moderate quality. Blake et al. (1) 19 and McCorrie et al. 20 both studied patient perspectives. Selection bias may be present as GPs supported with patient selection during invitation stage. Patients with valuable experiences may not have been invited to participate. Four studies18,20,21,23 do not clearly document the relationship between the researchers and the participants.
Gill et al. 22 utilised an interviewer known to the participants and Blake et al. (1) 19 utilised a patient researcher, which presents additional challenges including social desirability bias. However, both studies document a robust data analysis process. Gill et al. 22 utilised multiple researchers to support with analysis and refining themes.
Although a small study population of 10 participants, McCann et al. 21 add value as all participants were ANPs. This could be both a limitation and strength. The limitation presenting as a lack of exploration of the views of other allied health professionals (AHPs) and the strength as an insight into provision of AHP managing CNCP. McCorrie et al., 20 McCann et al. 21 and Gill et al. 22 utilised second researchers to support the reliability of coding and theme development, demonstrating robust methodologies (Table 3).
Synthesis
Themes and subthemes identified and corresponding papers.
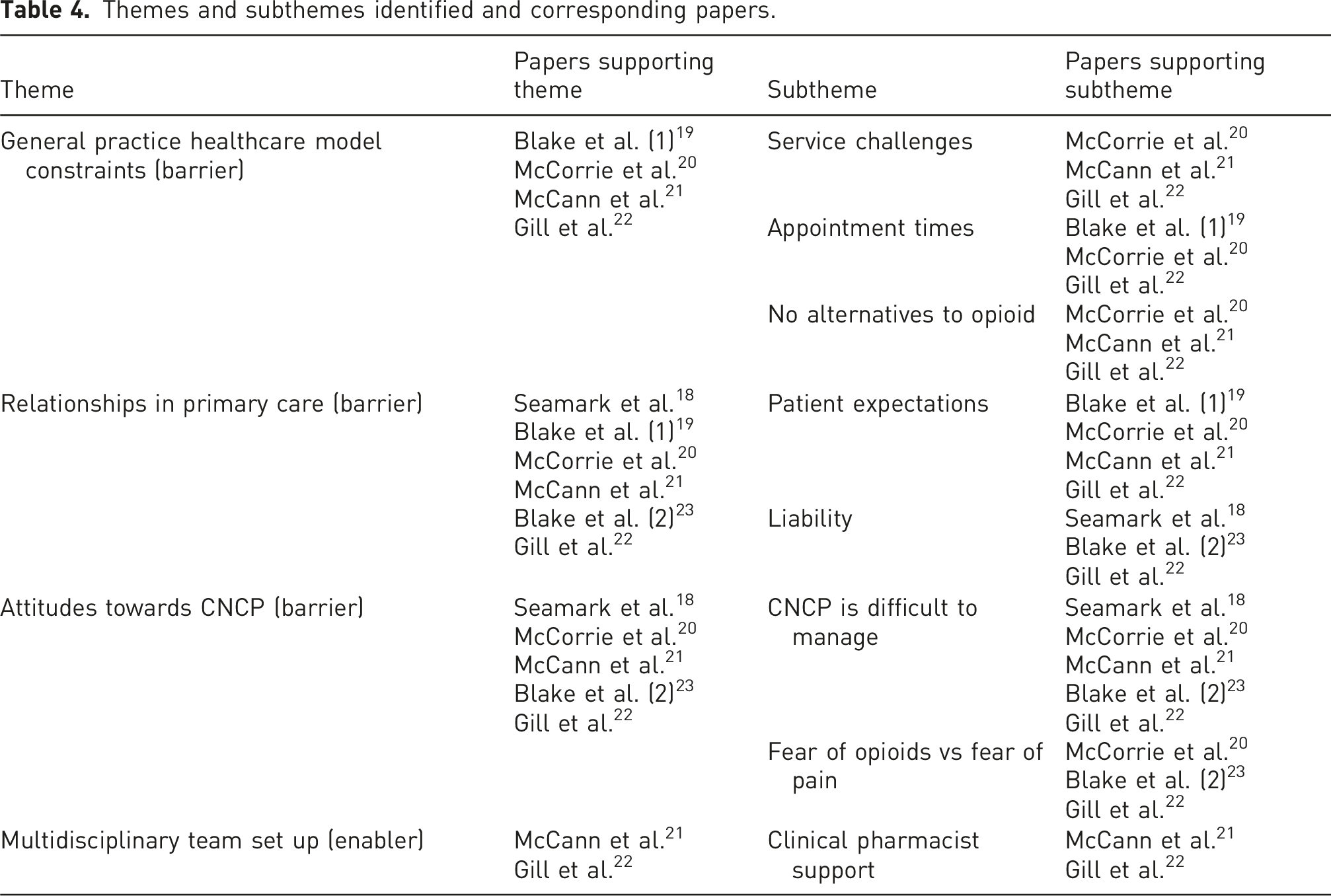
Theme 1: General practice healthcare model constraints (barrier)
Service challenges
Patients and clinicians expressed a lack of continuity of care. Multiple health professionals managing a single patient resulted in a lack of consistency and inability to fully understand a patient’s beliefs and behaviours.20–22 Gill et al. 22 stressed that inputs from different clinicians resulted in challenges for patient management plans to be followed correctly. On the other hand, intervention from a different clinician provides a new insight and opportunity to suggest alternative strategies for management. However, further research is required to support this.
McCorrie et al. 20 study was carried out in the north of England where prescribing rates of opioids are at higher levels than in other parts of the country. Increased socioeconomic deprivation has been shown to be associated with increased opioid prescribing. 24 Higher opioid prescribing levels exhibit higher demands and pressures on services; therefore, expressions are more informative and comprehensive. In contrast, Gill et al., 22 and McCann et al. 21 studies were carried out in other geographical areas representing different service pressures for CNCP management. Despite this variation, the same concerns regarding lack of continuity of care were observed.
High workloads and staff shortages also resulted in opioids being prescribed without a formal medication review. Long waiting times following referral to local chronic pain services contributed to opioid continuation, and ongoing prescribing becomes the normal behaviour.20–22
Appointment times
Patients expressed that GPs did not have the time to listen and address their concerns. 19 Expectedly, clinicians also highlighted that the lack of consultation time resulted in the inability to address all their patient’s needs.20,22 GPs expressed that time pressures contributed to repeat prescribing of opioids rather than making a shared management plan or exploring other ways to support with pain management.20,22 These three studies were carried out within different years over the past decade, demonstrating a continuing theme of concern regarding appointment time from both service providers and users.
No alternatives to opioids
A lack of alternatives to opioids contributed to ongoing and longer-term prescribing of opioid medications.20–22 Although clinicians may be motivated to support with inappropriate prescribing, findings suggest that clinicians found it was challenging with lack of either pharmacological or non-pharmacological alternatives to offer. Interestingly, all patients interviewed by McCorrie et al. 20 stated that they had experienced adverse side effects from opioids with minimal or no pain relief. There was still concern and apprehension expressed around dose reduction or stopping opioids and the lack of alternatives contributed to this. 20
Theme 2: Relationships in primary care (barrier)
Patient expectations
Clinicians found it difficult to engage patients in self-management, with unwillingness to try an opioid reduction resulting in pressure for the prescriber to continue.21,22 There was a lack of understanding of the problems with opioid prescribing and therefore management of patient expectations was challenging.
Studies acknowledged that building patient-clinician relationships takes time, skill and effort to achieve.21,22 Relationships are impacted by the number of encounters with the same clinician allowing for professional relations to form. This links back to the subtheme of service challenges identified in theme 1. Clinicians felt that the continuation of opioids maintained their patients trust, allowing for non-pharmacological measures to be employed later. 20 This was echoed by Gill et al. 22 where clinicians feared breakdown of relations may occur through discussing potential changes. Moreover, McCorrie et al. 20 expressed that establishing trust is challenging when experience and encounters have resulted in a fixed negative attitude towards a patient.
All three papers cover various geographical areas, including Northern Ireland, rural Wales, East Midlands and the northeast of England. Patient expectation on the limitations of opioid use in CNCP across the United Kingdom is lacking and requires patient education.
Liability
Clinicians expressed concerns about professional scrutiny following changes to inappropriate opioid medication where there was a lack of agreement or understanding from patients. 19 Fear of not meeting patient expectations may lead to formal complaints. 22 These studies were carried out 15 years apart, and clinician concern of liability is still present.
Seamark et al. 18 highlighted that clinicians inherit patients discharged from other sectors, which results in primary care clinicians taking over prescribing and therefore responsibility of potentially inappropriate doses. Subsequent changes of opioids can prove challenging as patients may be unwilling. 18
In addition to professional scrutiny, concerns on the nature of opioid medications and the potential for secondary gains. This includes the sale of prescribed opioid medicines in the community.18,22
Three papers; Seamark et al., 18 Blake et al. (2), 23 and Gill et al. 22 gathered data from different parts of the UK including Cornwall, Nottinghamshire and North Wales, together demonstrating a common theme of liability concerns.
Theme 3: Attitudes towards CNCP (barrier)
CNCP is difficult to manage
Some GPs expressed discomfort and lack confidence when prescribing opioids for CNCP in practice due to the subjectivity of the condition.19,20 The difficulty in managing CNCP occurs particularly when the condition is multi-factorial, and this can pose challenges in clinical judgement and decision-making. 18 Additionally, raising concerns and initiating a conversation on opioid deprescribing with patients is also a challenge. 18 There was evidence of clinicians understanding the clinical benefits of opioids in CNCP versus the side effects.18,20,22 However, the ability to apply this knowledge in practice with patients still proves to be challenging. These studies were carried out across different localities cross the UK and are inclusive of both doctors and ANP clinicians, thus representing the primary care settings.
Fear of opioids versus fear of pain
Explanation of the cause of CNCP could not always be provided which added to patient concerns, further highlighting the complexity of CNCP as a health condition.19,20 Patients were aware of and feared dependence towards opioids and aimed to balance pain relief with the adverse effects of opioids. 20 McCorrie et al. 20 is the only study that highlights patients’ awareness and understanding of opioid dependence and risks of long-term prescribing. This study was carried out in the north of the country where prescribing rates of opioids are more prevalent. Patients also expressed fear that decreasing their opioid dose would exacerbate their pain. 22 This links back to theme 1 subtheme; lack of alternatives that patients can be offered when discussing deprescribing.
Theme 4: Multidisciplinary team set up (enabler)
Clinical pharmacist support
Clinicians expressed positive experiences of working with a clinical pharmacist as part of the MDT to manage opioid prescribing.21,22 Gill et al. 22 and McCann et al. 21 acquire information and expressions from two professionals (GPs and ANPs) of the MDT observed in the real-world general practice setting. Both studies were carried out within the last 2 years and therefore reflect some of the current changes made to support a wider MDT in primary care.
Discussion
General practice in the UK is one of the first points of care. This meta-synthesis reviews the barriers and enablers of opioid management indicated for CNCP from the perspective of clinicians and patients.
The key enabler identified articulates that clinicians consider the MDT positive when supporting the management of opioids for CNCP. Clinical pharmacists are highlighted as adding value to the MDT by both doctors and ANPs, bringing expert knowledge of medicines to support with inappropriate prescribing and patient safety. At the time of writing there is no specific evidence evaluating the experiences of clinical pharmacists on managing opioid for CNCP in the UK and this requires further research. The PCN Direct Enhanced Service Contract 25/26 identifies that a variety of AHPs support transformation and service development. 25 The expansion of these roles within the PCN are reimbursed via the Additional Roles Reimbursement Scheme (ARRS).26,27
Unlike previous reviews, this analysis reinforces the current literature and combines experiences from service users (patients) and providers (doctors and ANPs) within general practice in the UK. Many barriers and enablers highlighted align with those identified internationally, for example Australia 28 and Canada, 29 supporting global understanding of opioid management.
Despite a rigorous search process some studies may have been missed. The data is limited to a small number of studies and populations, only six studies met the inclusion criteria. Title and abstract screening were carried out by a single reviewer and were not duplicated. Due to working in the general practice setting as a clinical pharmacist, there is an acknowledged potential bias in interpretation.
Recommendations for policy
The NHS Long-Term Plan outlines the redesign of patient care and addresses health inequalities within in a growing ageing population. 12 The plan outlines primary care pathways to relieve the pressure on secondary care services. In addition, financial incentives are in place for primary care and PCNs; including Impact and Investment Fund (IIF) and Quality Outcomes Framework (QOF). 25 In March 2023, NHS England published the ‘Optimising personalised care for adults prescribed medicines associated with dependence or withdrawal symptoms framework’, which addresses the complexity of these classes of medications and outlines a plan for system engagement. 30 Future policies need to focus on reducing the long waiting times observed for specialist pain services, which support the reduction of inappropriate ongoing opioid prescribing observed in general practice. Opportunities to support non-pharmacological management should be developed to provide alternative options when deprescribing opioids.
Recommendations for practice
Alignment of both policy and practice is required. This would ensure the best outcomes can be achieved and patient safety optimised. To overcome the barriers, education in multiple areas of the wider NHS network is required. To support with managing patient expectations, patients should be educated on the limitations of opioids indicated for CNCP. Clinicians are aware of the problems associated with inappropriate opioid prescribing. However, clinicians require education and training on soft skills (communication and shared decision-making) to support application of knowledge into consultations.
PCNs should optimise MDTs by utilising suitably trained AHP led clinics for CNCP. Using longer appointment times allocated to ARRS-funded professionals supports with medicines optimisation for CNCP. In addition, both clinicians and patients need to accept a change in culture within the general practice setting.
Recommendations for research
Current research focuses on doctor professionals and their experiences on opioids for CNCP. Following the proposed recommendations further research is required to identify potential barriers and enablers of additional AHPs managing opioids for CNCP within general practice. For example, at the time of writing there is no current literature on the barriers and enablers of CNCP management experienced by clinical pharmacist AHP’s. Research on the impact of roles, including clinical pharmacists, social prescribers and physiotherapists to name a few, would provide further evidence on medicines optimisation opportunities of opioids at practice level. Further reflection on patient experiences would also add value, including the consequences of opioid deprescribing on one’s mental health and well-being. Further research on patient understanding of opioids is needed, which may differ regionally.
Conclusion
Exploration of both the barriers and enablers towards opioid management in CNCP has enabled an understanding of the lived experience at practice level. A culture change from service providers and users is required to ensure skill mix is utilised optimally. A movement away from the traditional model of opioids being managed by a doctor needs to occur. Further utilisation of the MDT and AHPs within primary care ensures that patients are seen by the most appropriate practitioner for their needs and would support with safer opioid management.
Footnotes
Acknowledgements
Claire Poole – University of Northampton, University Drive, Northampton, NN1 5PH United Kingdom
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
