Abstract
Background:
Vitamin D (VD) deficiency has become a global public health problem, and published studies have demonstrated that patients with subacute thyroiditis (SAT) have worse VD nutritional status and that VD supplementation may alleviate thyroid-related diseases by fighting against infections and mediating autoimmunity.
Objectives:
This study explored the correlation between serum VD levels and the risk and extent of disease in patients with SAT.
Design:
A case-control study.
Methods:
We included patients with SAT diagnosed at the First People’s Hospital of Jining City between September 2021 and September 2023 and a healthy population during the same period. We collected clinical and laboratory data to determine differences in VD levels between the two populations and identify risk factors for the onset and extent of SAT.
Results:
The 25(OH)D level of SAT patients was significantly lower than that of the healthy population (
Conclusion:
VD levels are lower in patients with SAT than in healthy controls, and low VD levels increase SAT risk. Although VD levels are not related to SAT severity, adequate VD inhibits the conversion of FT4 to FT3, likely playing a protective role in SAT development.
Plain language summary
Introduction
Subacute thyroiditis (SAT) is the most common painful thyroid disease characterized by the destruction of thyroid follicles; infiltration of inflammatory cells such as neutrophils, lymphocytes, multinucleated giant cells, eosinophils, and plasma cells; and formation of granuloma. The pathogenesis of SAT has not yet been elucidated and is currently being considered related to immunity and infections: genetically susceptible individuals with certain types of human leukocyte antigen (HLA) 1 are susceptible to SAT following infection with upper respiratory tract viruses (occurring approximately 2–6 weeks prior). 2
Vitamin D (VD) is an essential fat-soluble vitamin, and serum 25(OH)D level is the best indicator for evaluating VD nutritional status. The classical physiological role of VD is to maintain calcium-phosphorus homeostasis, and in recent years, the extra-skeletal effects of VD and its analogues have continued to be discovered, such as with diabetes mellitus, cardiovascular disease, neoplasms, immune disorders, and infectious diseases. 3 Active VD calcitriol not only maintains cellular tight junctions to reduce the risk of infection but also encodes proteins required for the formation of gap junctions, tight junctions, and adherens junctions, which protects the integrity of cellular junctions from viral interference. 4 Inadequate levels of VD have been found to reduce immunity and increase the frequency and severity of viral infections, 5 while adequate VD levels have been found to also significantly reduce the risk of respiratory infections. 6
In recent years, an increasing number of studies have been conducted on the relationship between VD and thyroid-related diseases. However, there are relatively few studies on the relationship between VD and SAT diseases, and the results are inconsistent, with two studies reporting that serum 25(OH)D levels of SAT patients were lower than those of healthy populations,7,8 and the other study concluding that there was no difference in VD levels in SAT compared with those of the healthy populations. 9 Therefore, this study aimed to further understand the VD nutritional status of SAT patients and preliminary investigate the correlation between VD levels and SAT to provide a basis for the relationship between VD and SAT disease.
Subjects and methods
Subjects
The case group comprised patients with newly confirmed SAT selected from the outpatient or inpatient department of the Division of Endocrinology and Metabolism of the First People’s Hospital of Jining City from September 2021 to September 2023. The inclusion criteria were as follows: compliance with the diagnostic criteria for SAT in the Chinese Diagnostic Guidelines for Thyroid Diseases—Thyroiditis 10 ; all patients were informed of the nature of the study, following which written informed consent was obtained. The exclusion criteria were as follows: recent use of drugs interfering with thyroid function and VD level; use of non-steroidal anti-inflammatory drugs (NSAIDs), glucocorticoids, and immunosuppressive drugs; pregnant and lactating women; combination of chronic hepatic and renal insufficiency; parathyroid disease; adrenal disease; anorexia nervosa; post-gastrectomy; and nutrient metabolism and absorption disorders. As for sample size calculation, the proportion of VD deficiency in our population is approximately 70%, consistent with that in literature, 11 calculated according to the following formula:

Test efficacy was considered as 0.9, with an odds ratio of 3.0; based on calculation using PASS 15 software, 66 people were included from at least 66 cases of SAT; finally, 141 patients with SAT met the criteria for nadir exclusion. The control group was selected from the general medical checkup population from the same health checkup center, with “age, gender, and quarter of medical checkup” as the matching items, with a matching tolerance of 0.01; based on calculation using SPSS 25.0 software, propensity score matching was performed to match the SAT group with the control group in a 1:1 ratio, and 141 pairs were successfully matched. Laboratory tests of all participants were subject to quality control at the Department of Laboratory Medicine, Jining No. 1 People’s Hospital.
Research methods
General medical information including sex, age, medical history, height (cm), weight (kg), and body mass index (BMI; weight in kg/height in m2) was collected. In SAT patients, the presence of fever, the maximum temperature during fever, enlargement of the thyroid gland, and tenderness of the thyroid gland were recorded. Additionally, complete blood count, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), 25 (OH)D, free triiodothyronine (FT3), free thyroxine (FT4), thyroid-stimulating hormone (TSH), thyroperoxidase antibodies (TPOAb), 25(OH)D, thyroglobulin antibodies (TGAb), neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), and free thyroxine/free triiodothyronine (FT4/FT3) data were recorded in SAT patients. The severity of SAT was scored as follows 12 : fever—none, <38°C, and >38°C (0, 1, and 2 points, respectively); tenderness—none, mild, and severe (0, 1, and 2 points, respectively); goiter palpation—none and yes (0 and 1 point, respectively); and ESR—normal, 21–50 mm/h, and >50 mm/h (0, 1, and 2 points, respectively). A score of <3 and ⩾3 was defined as mild SAT and moderately severe SAT, respectively. After the SAT diagnosis, according to the treatment guidelines of the Chinese and American Thyroid Association,10,13 patients with mild SAT were advised general treatment (adequate rest and plenty of drinking water) or oral NSAIDs, and glucocorticoid hormone treatment was provided for other bodily symptoms such as persistent high fever, thyroid pain, enlarged thyroid gland with marked tenderness, or ineffective treatment with NSAIDs.
Statistical analysis
EpiData 3.1 software was used to establish the database, and SPSS (version 26.0; IBM Corporation, Armonk, NY, USA) was used to organize and analyze the study data. Measurement data were expressed as mean ± standard deviation, and the
Results
Comparison of general information and blood indices between the SAT and control groups
The 25(OH)D level, lymphocyte count, and BMI in the SAT group were significantly lower than those in the healthy control group (
Comparison of general information and serum indices between the SAT and control groups.

25(OH)D, 25-hydroxyvitamin D; BMI, body mass index; NLR, neutrophil-to-lymphocyte ratio; ns, not statistically significant; PLR, platelet-to-lymphocyte ratio; SAT, subacute thyroiditis.
Risk factor analysis for the occurrence of SAT
The indicators that were significant differences between groups were selected, and after covariate analysis, neutrophils, monocytes, NLR, and PLR with covariates were removed, and multifactorial logistic regression was performed with five factors, namely BMI, leukocytes, lymphocytes, platelets, and 25(OH)D, as independent variables and the occurrence or non-occurrence of SAT as the dependent variable. The results showed that low 25(OH)D (
Logistic regression analysis of risk factors for SAT development.

25(OH)D, 25-hydroxyvitamin D; BMI, body mass index; CI, confidence interval; OR, odds ratio; SAT, subacute thyroiditis.
Comparison of general information and blood indices between mild SAT and moderately severe SAT
Of the 141 SAT patients included, 43 had mild SAT and 98 had moderate-to-severe SAT. The average age of the mild SAT group was 48.51 ± 17.37 years, and 72.09% were female, and the average age of the moderate-to-severe SAT group was 47.91 ± 10.53 years, and 67.35% were female. There was no statistically significant difference between mild and moderate-to-severe SAT cases in terms of age and sex (
Comparison of general data and serum indices in patients with different severities of SAT.

25(OH)D, 25-hydroxyvitamin D; BMI, body mass index; CRP, C-reactive protein; ESR, erythrocyte sedimentation rate; FT3, free triiodothyronine; FT4, free thyroxine; NLR, neutrophil-to-lymphocyte ratio; ns, not statistically significant; PLR, platelet-to-lymphocyte ratio; SAT, subacute thyroiditis; TGAb, thyroglobulin antibodies; TPOAb, thyroperoxidase antibody; TSH, thyroid-stimulating hormone.
Risk factors for the severity of SAT
The indicators with significant differences among SAT patients with different severities of disease were selected, and after removing leukocytes, NLR, PLR, CRP, and TSH, which were covariate diagnostics, the remaining nine factors, namely goiter, fever, thyroid tenderness, BMI, neutrophils, platelets, ESR, FT4, and 25(OH)D, were considered as independent variables the severity of SAT as the dependent variable. The results showed that VD was not a risk factor for the severity of SAT, and fever, thyroid tenderness, elevated BMI, and elevated FT4 were independent risk factors for the severity of SAT (
Logistic regression analysis of risk factors for the severity of SAT.

25(OH)D, 25-hydroxyvitamin D; BMI, body mass index; CI, confidence interval; ESR, erythrocyte sedimentation rate; FT4, free thyroxine; OR, odds ratio; SAT, subacute thyroiditis.
Correlation analysis of 25(OH)D with inflammatory parameters and thyroid function
Spearman’s correlation analysis suggested that 25(OH)D levels did not correlate with leukocytes, neutrophils, lymphocytes, monocytes, ESR, CRP, NLR, PLR, FT3, FT4, TSH, TPOAb, and TGAb (
Correlation analysis of serum 25(OH)D levels with inflammatory parameters and thyroid function.

25(OH)D, 25-hydroxyvitamin D; CRP, C-reactive protein; ESR, erythrocyte sedimentation rate; FT3, free triiodothyronine; FT4, free thyroxine; NLR, neutrophil-to-lymphocyte ratio; PLR, platelet-to-lymphocyte ratio; TGAb, thyroglobulin antibodies; TPOAb, thyroperoxidase antibody; TSH, thyroid-stimulating hormone.

Scatterplot of serum 25(OH)D levels versus FT4/FT3.
Linear regression analysis of serum 25(OH)D with thyroid function and inflammatory parameters.
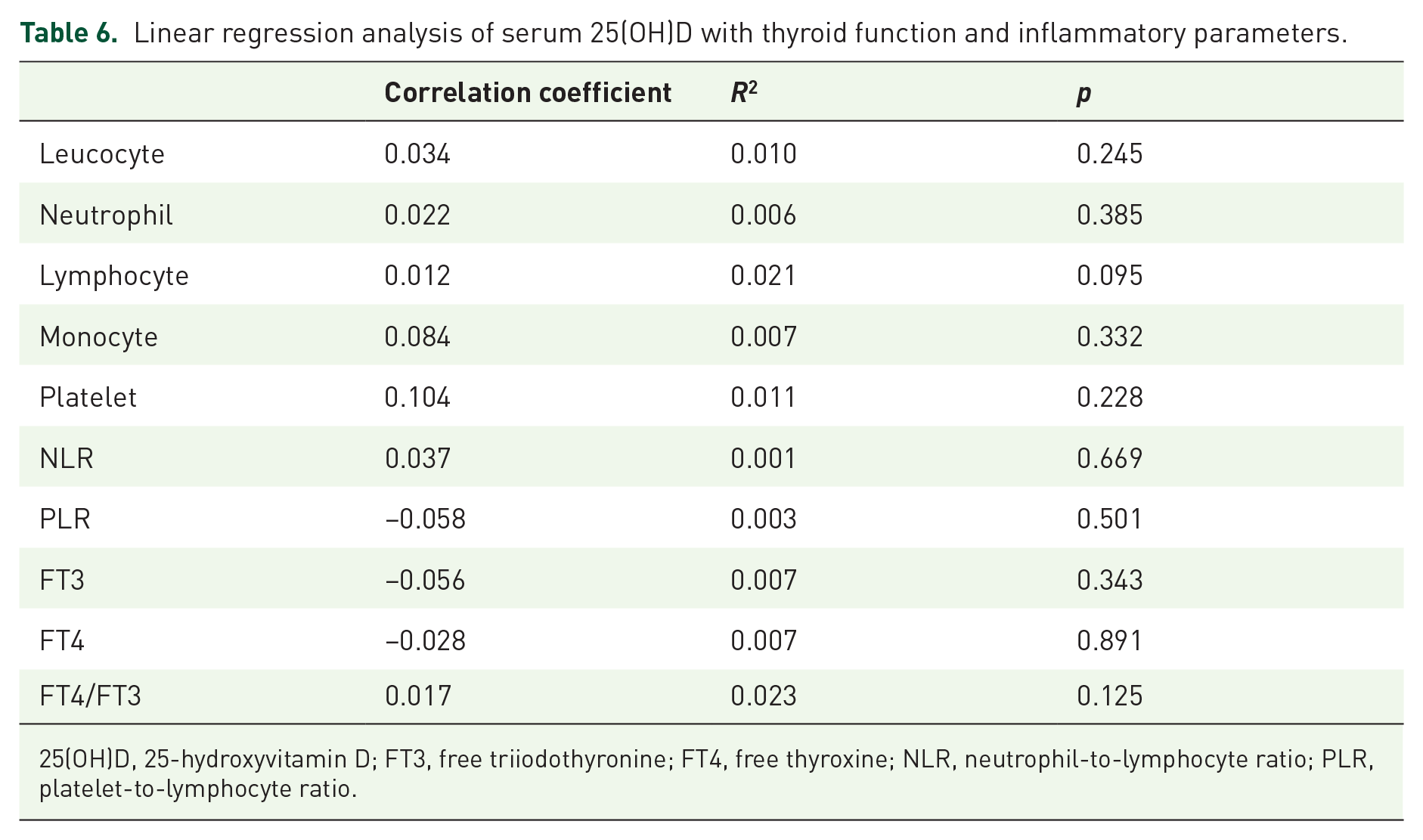
25(OH)D, 25-hydroxyvitamin D; FT3, free triiodothyronine; FT4, free thyroxine; NLR, neutrophil-to-lymphocyte ratio; PLR, platelet-to-lymphocyte ratio.
Discussion
VD plays a wide range of roles; in addition to its function of regulating calcium and phosphorus metabolism and maintaining bone health, it is also involved in tissue cell differentiation, proliferation, and immune regulation. 14 However, VD deficiency and insufficiency have now become one of the most common global public health problems. An increasing number of studies have shown that VD deficiency is closely related to the development of thyroid-related diseases. It has been found that patients with thyroid disorders such as Hashimoto’s thyroiditis, Graves’ disease, hypothyroidism, and thyroid tumors have significantly lower levels of VD than the healthy population,15–19 and increasing VD levels may reduce the risk of thyroid disorders. 20 There are few studies on the relationship between VD and SAT, and the conclusions are inconsistent. Therefore, this study aimed to assess VD levels in patients with SAT and conduct a preliminary investigation on the relationship between VD levels and the onset and extent of SAT.
SAT is a painful thyroid disorder that usually occurs after an upper respiratory viral infection. VD, a steroid hormone, is also an important immunomodulatory.21,22 VD deficiency disrupts the integrity of the tight junctions in the body’s cells, leading to viral invasion
4
thus increasing the prevalence of upper respiratory tract infections.
23
The occurrence of SAT may be associated with HLA-B*35
24
and recent studies have also observed that the presence of HLA-B*18:01, HLA-DRB1*01, HLAC*04:01, and HLA-A02:09 are associated with an increased risk of genetic susceptibility to SAT.
1
HLAs are a group of proteins encoded by histocompatibility complex genes, located on the distal part of the short arm of human chromosome 6, that recognize antigens presented to T lymphocytes to regulate adaptive immune responses.
25
VD receptor (VDR) response elements are present in the promoter region of some HLA alleles, and VD may play a role in the pathogenesis of SAT by binding to VDR to regulate
There are few studies on the relationship between SAT and VD with inconsistent conclusions. In a study by Korkmaz et al.
1
and Calapkulu et al.,
7
SAT patients were found to have significantly lower 25(OH)D levels than healthy controls (13.3 ± 5.1 vs 18.6 ± 9.3 ng/mL,
The clinical guidelines of the American Thyroid Association recommend prioritizing the use of NSAIDs in patients with mild SAT and glucocorticoids in those with moderate-to-severe SAT.
13
In this study, subgroup analyses were conducted with and without glucocorticoid application, and the results suggested that the proportions of fever, neck pain, goiter, and thyroid tenderness, as well as the leukocyte counts, neutrophil counts, platelet counts, NLR, PLR, ESR, CRP, and FT4 were significantly higher in moderate-to-severe SAT than in mild SAT (
Next, we explored the relationship between VD and the extent of SAT. There was no statistically significant difference in VD levels between patients with mild SAT and those with moderately severe SAT. Logistic regression analysis showed that VD levels were not a risk factor for the severity of SAT (
The present study further explored the correlation of VD with inflammatory parameters and indicators of thyroid function. Spearman’s correlation analysis showed that 25(OH)D levels were significantly and positively correlated with FT4/FT3 (
This study has some limitations. First, this study is a single-center case-control study, which may have biased the results to some extent given the restricted geographical area and study population. Second, this study did not follow up the patients with SAT, and it is not known if there is a relationship between the VD nutritional status and the recurrence of SAT. Third, this study did not involve the interventional therapy study of VD supplementation. Despite these limitations, to our knowledge, this is the first time the relationship between VD and the risk of SAT and the extent of disease has been explored, which provides new ideas for the next steps into in-depth research on the relationship between the two and the related mechanisms.
Conclusion
Our study found that patients with SAT had significantly lower VD levels than healthy controls and that reduced VD levels were an independent risk factor for the development of SAT. There was no statistically significant difference in VD levels between patients with mild SAT and those with moderately severe SAT. VD levels were not related to the degree of SAT disease, but 25(OH)D levels were positively correlated with FT4/FT3, and we hypothesized that adequate VD levels inhibited the conversion of FT4 to FT3, attenuated the symptoms related to hyperthyroidism in patients with SAT, and played a protective role in SAT progression. This preliminary study investigated the correlation between VD and SAT and provided a partial basis for future research on the relationship between the two, which still needs further verification by multicenter large-scale randomized controlled trials.
Supplemental Material
sj-doc-1-tae-10.1177_20420188251321600 – Supplemental material for Analysis of vitamin D nutritional status and disease risk factors in patients with subacute thyroiditis
Supplemental material, sj-doc-1-tae-10.1177_20420188251321600 for Analysis of vitamin D nutritional status and disease risk factors in patients with subacute thyroiditis by Rongrong Wang, Dehuan Kong and Xiaoqing Ma in Therapeutic Advances in Endocrinology and Metabolism
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
