Abstract
Umbilical endometriosis or Villar’s nodule is defined as the presence of endometrial tissue within the umbilicus and represent 0.5%–1% cases of endometriosis ectopia. It is classified as primary or secondary based on the surgical history. The important symptoms that characterize primary umbilical endometriosis were cyclical pain and a palpable mass that may be associated with bleeding. These features have temporal association with catamenia. Presented is a 30 year old woman with clinical features that suggested primary umbilical endometriosis in the past 5 years. It was confirmed by histology and coexisted with uterine fibroid. In the absence of previous surgery, primary umbilical endometriosis should be considered in the differential diagnosis in females of reproductive age with umbilical pain and nodule related to catamenia. Surgery is the treatment of choice and this should be individualized as some lesions can be managed by local excision with satisfactory outcome regarding the cessation of the presenting symptoms with good cosmetic outcome.
Introduction
Endometriosis is defined as the presence of functional endometrial tissue outside the uterine cavity. 1 The most common cutaneous site is the umbilicus. Clinically the umbilicus is a focus of attention, as a plethora of diseases that affected it presented as nodules. 2 Primary or spontaneous umbilical endometriosis is the presence of ectopic endometrial tissue in the umbilicus in the absence of prior surgery.2,3 Umbilical endometriosis also known as Villar’s nodule was described by Villar in 1886.4,5 It is rare with an incidence of 0.5%–1.0% of endometriosis ectopia.2,6 The pathogenesis of primary endometriosis is unknown. Three postulates had been proposed: the implantation (through retrograde menstruation), dissemination (through sanguineous or lymphatic spread) and coelomic metaplasia (differentiation of pluripotent peritoneal progenitor cells into endometrial tissue) theories.1,7 The symptoms of importance in the clinical diagnosis of primary umbilical endometriosis are cyclical pain and a palpable mass that may be associated with cyclical bleeding. These features have temporal association with the menstrual period. 2 Imaging modalities have not been conclusive in the diagnosis of umbilical endometriosis. Histology that showed endometrial glands and stroma were the hallmark of definitive diagnosis. 8 Surgery is the treatment of choice.2,9 Presented is a 30 year old woman with clinical features that suggested umbilical endometriosis confirmed by histology to increase the index of suspicion among clinicians who should disabuse the fears of patients as this disease condition is regarded in some cultural settings as an enigma. The location and macroscopic appearance of the lesion in the umbilicus were valuable indicators for local excision that preserved the umbilicus for cosmesis.
Case presentation
A 30-year-old trader, presented to the surgical outpatient department (SOPD) with a recurrent umbilical pain in the past 5 years, with the recent episode that lasted 2 weeks prior to presentation. Pain was cyclical, occurring monthly and lasted for 2 weeks. It was insidious in onset, sharp, intermittent, non-radiating and progressively worsened over the period of menstruation and associated with bloody discharge from the umbilicus. There was an associated umbilical swelling but no history of abdominal distension, masses nor gastrointestinal symptoms. There was no family history of similar condition. Menarche was at 15years; had a menstrual flow of 4-5 days in a 28-30 days cycle. She is single and Para 0. There was no history of the use of contraceptive. She was sexually active but abstained for about 2years now on account of this ailment. Delay in presentation was attributed to cultural concerns about this disease still regarded as an enigma.
On examination, she was in satisfactory general condition. The abdomen was full and symmetrical. The umbilicus was everted and measured 4 cm × 3 cm. There was a hyperpigmented dome shaped nodule that measured about 1.5 cm across the widest dimension at the left margin of the umbilicus, Figure 1. The swelling was tender and firm. A clinical diagnosis of umbilical nodule probably endometriosis was made. Clinical photograph of the umbilicus showing the umbilical nodule (red arrow).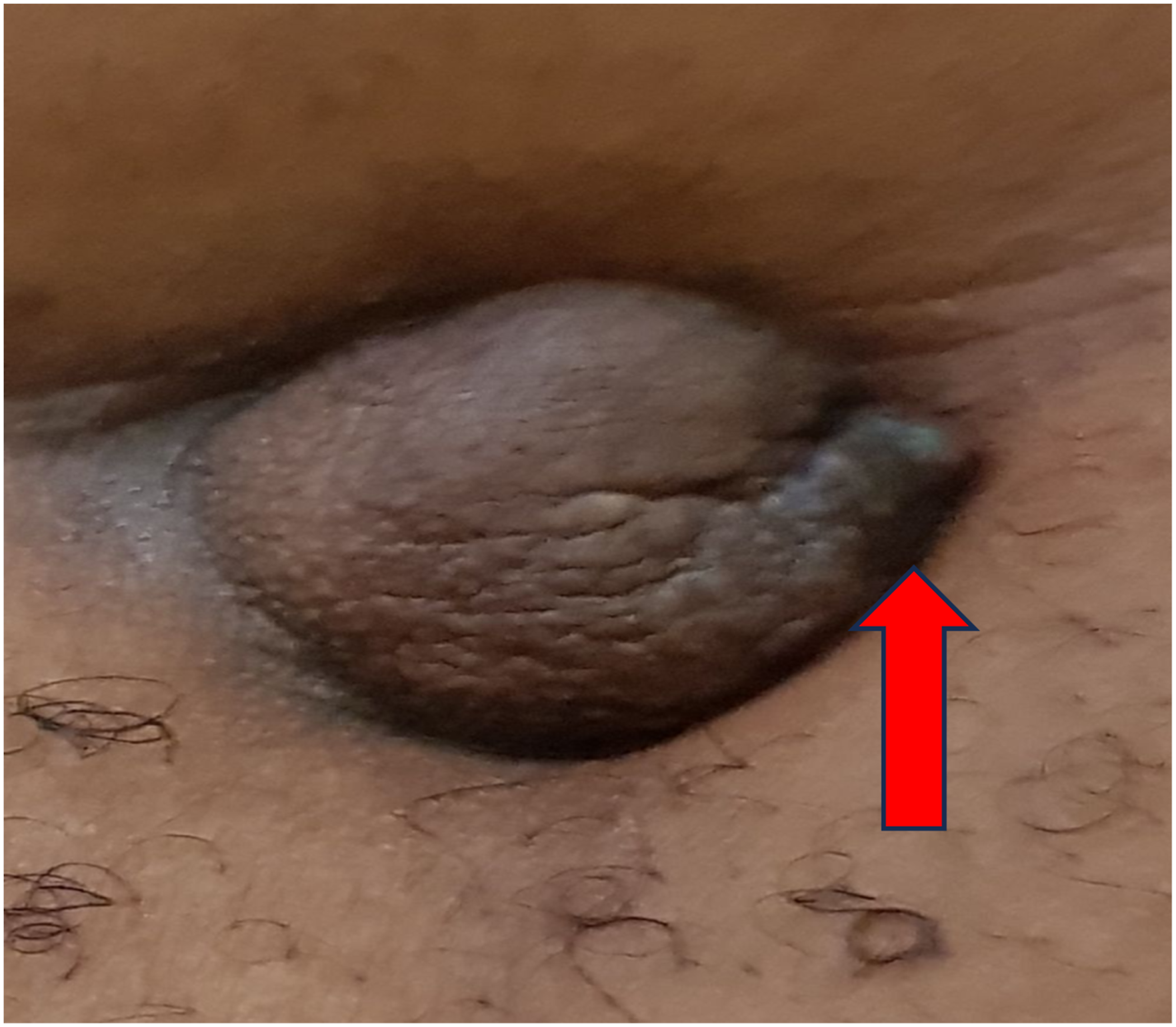
Blood test- Full blood count (FBC) and urinalysis were unremarkable. Abdominopelvic sonography showed a normal sized uterus with a preserved endometrial and myometrial echo complex. There was an oval-shaped hypoechoic solid mass that measured 6.82 × 5.04 cm in the left adnexium that suggested pedunculated subserous myoma, Figure 2. USS oval shaped hypoechoic solid mass (blue arrows) in the left adnexium- features suggestive of pedunculated subserous myoma.
She had local excision of the umbilical nodule, Figure 3(a) and (b). Postoperative period was uneventful and patient discharged to the outpatient department. The histology reported: macroscopy, a hyperpigmented dome shaped mass that measured 1.5 × 1,5 × 1.0 cm. Microscopy showed tissue lined by stratified squamous epithelium, endometrial glands surrounded by endometrial stroma in the sub epithelium consistent with umbilical nodule- endometriosis, Figure 4(a)–(d). The peripheral and deep resection margins were described as free of endometrial tissue. Patient was counselled on the risk of recurrence of the lesion and the need for follow up emphasized. She was referred to the gynaecologist for follow up care in view of the ultrasound scan (USS) finding that suggested uterine fibroid. Follow up in the surgical outpatient after 4 months of surgery, revealed that bleeding per umbilicus had ceased but had persistent umbilical pain for which she was placed on hormonal contraceptive (CombiFem) by the Gynaecolosist. The review of the patient in the SOPD 10 months post-surgery was satisfactory. 3a- Local excision specimen showing a hyperpigmented dome shaped nodule (red arrow). 3b- Local excision specimen showing part of the superficial (edge) and deep resection (blue arrow) margins. Umbilical nodule- endometriosis. H&E X 40. 4a- Tissue lined by stratified squamous epithelium showing acanthosis with melanin incontinence (blue arrow). 4b- Endometrial gland (red arrow) surrounded by endometrial stroma (blue arrow) in the sub epidermis, showing smooth muscle cells around the endometrial glands (brown arrow). 4c- Umbilical endometriosis, H&E X 100- Showing endometrial glands (blue arrow) lined by cuboidal epithelium, surrounded by endometrial stroma (red arrow). 4days, H&E X 40- Areas of old haemorrhage with hemosiderin laden macrophages and few congested blood vessels with inflammatory cells infiltrates (brown arrow).

Discussion
The occurrence of functional endometrial glands and tissue outside the endometrial cavity is endometriosis. 2 Cutaneous endometriosis is a rare disorder and the most common site for extra pelvic endometriosis. 10 The umbilical involvement though uncommon, is the commonest cutaneous site. 2 It was first described by Rokitansky in 1860 and defined as the presence of an extra uterine functional endometrial tissue formation in the skin. 10 It is a rare benign condition with an incidence of 0.5%–1.0% of extra pelvic endometriosis with a mean age of 33 years.1,10 In another report the mean age was 28 years. 5
Umbilical endometriosis is classified as primary or secondary based on the origin of the endometrial tissue. The primary or spontaneous develops spontaneously in the absence of prior abdominal surgery and it is also known as Villar’s nodule. In the primary variety, the endometrial tissue is found outside the uterine cavity and it is further classified as pelvic and extra pelvic. In the pelvic type it may be found in the ovaries, uterosacral ligaments and pouch of Douglas. Extra pelvic is found in various organs: skin- umbilicus, gastrointestinal tract, diaphragm, lungs, brain, genitals and urinary tract. 10 The secondary endometriosis also called scar endometriosis, occurs at the site of previous surgery due to iatrogenic implantation in scars from abdominal and pelvic surgery such as caesarian section, hysterectomy and laparoscopy.1,2,10
The umbilicus may act as a physiological scar with a predilection for endometrial tissue in the development of primary umbilical endometriosis. 4 The pathogenesis of umbilical endometriosis remains unclear, the possible theories proposed are: “Implantation theory”- implantation of endometrial tissue through retrograde menstruation, “Dissemination theory”- migration of endometrial cells to the umbilicus through the abdominal cavity, lymphatic system or through embryonic remnants in the umbilical fold such as the urachus and umbilical veins and “Coelomic metaplasia”- differentiation of pluripotential progenitor cells into endometrial tissue.1,7 The survival of the endometrial cells implant may depend on local or systemic factors. The inflammatory process initiated by microvascular endothelial injury might enhance adhesion of tissue implants through the production of adhesion molecules such as integrin and e-cadherin. 9 Genetic predisposition and immunological defects have also been suggested. 6 Coelomic metaplasia is reported by some as the most favored, 4 while others report the implantation as the most favored. 2 This is an area of further inquiry.
The most prevalent symptoms of endometriosis were umbilical nodule, pain, swelling which may include bleeding during catamenia.1,2,4 The nodule may be hyperpigmented and dome shapped,1,4 Figures 1 and 3(a). Pain may be due to tissue inflammation and distention from cyclical changes during menstruation. 2 In a study, umbilical swelling occurred in 90% of cases, while <50% had bleeding and 80% with pain. 2 However, asymptomatic variants should not be overlooked. The size of the lesions ranged from 0.5 to 4 cm6. Some cases have been described in postmenopausal women and a few cases that coexisted with uterine fibroid 5 consistent with our report. Case reports of umbilical endometriosis have been documented in pregnancy. 1 The presence of umbilical nodule has been generally regarded as a sign with grave prognosis. However, it has been demonstrated that most umbilical nodules are benign. 2 Clinical diagnosis can be made based on history and physical examination. The differential diagnosis of umbilical masses are diverse and may present a diagnostic difficulty. 11 They include umbilical hernia, keloid, pyogenic granuloma, melanoma and primary or metastatic carcinoma known as Sister Mary Joseph’s nodule. 2 Umbilical endometriosis though a rare entity, should be considered as a differential diagnosis in cases of umbilical disorders even in the absence of symptoms of pelvic endometriosis. 12
There is no pathognomonic finding consistent with umbilical endometriosis in any of the imaging modalities (USS, CT, MRI). However, they are useful in ruling out involvement of other organs or other pathologies as was our experience, Figure 2, including establishing the depth of the lesions that could aid in planning surgical therapy.1,2 Diagnosis was confirmed by histology that showed endometrial gland and stroma. It may also show deposits of hemosiderin and inflammatory changes, 2 Figure 4(a)–(d). Immunohistochemistry (IHC) with CD10 is positive in the endometrial stroma, this is very useful when the glands are not seen on histology. 2 This risk of malignant transformation of umbilical endometriosis to endometrial carcinoma has been described though rare. 9
Surgical treatment is the therapy of choice aimed at the prevention of recurrence and reduction in the risk of malignant transformation. 9 The choice of the surgical technique should be individualized based on the size and depth of the lesion. The options include a complete surgical resection which may involve fascial and peritoneal repair or a local excision of the endometrial nodule. 2 The later was the case in our patient, based on the location of the nodule at the periphery of the umbilicus, size, Figure 1 and depth of the lesion with a good cosmetic outcome. Surgical consensus regarding its treatment is lacking due to its rarity. The frequently preferred operation is total resection of the umbilicus. It carries a low risk of recurrence with complete excision. However, the challenge with this is the inferior cosmetic outcome. 2 Preoperative hormone treatment may be indicated in patients with large masses to reduce the clinical symptoms and size. 4 Commonly used hormones are oral contraceptives and Gonadotropin- releasing hormone agonists. 2 Postoperative hormonal therapy has been used particularly to reduce the risk of symptom recurrence. 13 This was indicated in our patient due persistent umbilical pain following excision. However, its actual benefit requires further studies. Despite the type of surgery, the patient should be advised on the risk of recurrence or malignant transformation and the need for follow up emphasized. In event of recurrence, histopathological evaluation should be requested always to ensure proper evaluation. 14
Conclusion
In conclusion, primary umbilical endometriosis should be considered in the differential diagnosis in females of reproductive age with umbilical pain and nodule related to catamenia in a patient without a history of previous surgery. It coexisted with uterine leiomyoma. Surgery is the treatment of choice and the choice of surgery should be individualized as some lesions can be adequately managed by local excision with the added advantage of a good cosmetic outcome often desired by females.
Footnotes
Acknowledgements
We acknowledge the patient and all the participating authors for their contribution to the paper.
Author contributions
All authors contributed to different aspect of the report.
Author’s note
The authors declare that this paper is not under consideration or published in some other journal.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
