Abstract
The coronavirus disease 2019 outbreak has been designated a public-health emergency in major cities around the globe. Major health-care institutions are scrambling to implement effective infection control measures to ensure the safety of patients and visitors while minimising disruptions to the provision of quality health care. We describe the measures taken by the nuclear medicine units in the major health-care institutions within Singapore to ensure optimal delivery of care to our paediatric patients and their caregivers.
Introduction
At the time of writing, much of the world is in the throes of the coronavirus disease 2019 (COVID-19) pandemic caused by a novel coronavirus, severe acute respiratory syndrome (SARS) coronavirus 2, which has significantly impacted health-care operations in major cities. Despite its low case fatality rate compared to other coronavirus epidemics in recent memory, SARS and Middle East respiratory syndrome, COVID-19 infection has proven to be more readily transmissible and has resulted in higher mortality and economic impact. 1 On 7 February 2020, the Ministry of Health Singapore stepped up their risk assessment from Disease Outbreak Response System Condition (DORSCON) Yellow to DORSCON Orange. 2 From 7 April 2020, ‘circuit breaker’ measures 3 were implemented to stem the rise of COVID-19 infections. As of 15 April 2020, Singapore has seen 3252 confirmed cases of COVID-19, with 99 cases in those aged ⩽20 years.
While much remains unknown about COVID-19, children and teens appear relatively spared.4,5 However, there are reports of asymptomatic carriage and convalescent viral shedding in the paediatric population,5,6 and it is postulated that they may play a significant role in disease transmission. Furthermore, it has been established that prolonged close and unprotected exposure plays a substantial role in viral transmission, in particular within family clusters. 7 These factors have obvious implications for paediatric medical practice and associated ancillary services. Children will continue to fall ill for other reasons, and they may sometimes require specialist hospital care, where they and their families may be put at risk of exposure to COVID-19, and likewise the medical team.
We describe some of the strategies adopted in the nuclear medicine units of the National University Hospital Department of Diagnostic Imaging, KK Women’s and Children’s Hospital (KKWCH) and Singapore General Hospital Department of Nuclear Medicine and Molecular Imaging (SGH DNMMI) to protect paediatric patients and their families.
These institutions form the entirety of secondary to quaternary paediatric care in the Singapore public health-care system, with KKWCH being a dedicated paediatric and obstetric-gynaecological hospital. In the context of nuclear medicine, common paediatric procedures performed include iodine-131 metaiodobenzylguanidine (MIBG) scans for neuroblastoma, hybrid positron emission tomography/computed tomography (PET/CT) for oncological, neurological and cardiac indications and renal scintigraphy for urological problems.
Unique challenges of the paediatric patient
Children pose a unique challenge to the nuclear medicine department. The paediatric patient necessitates the presence of at least one accompanying adult, which may pose a problem to the implementation of distancing or isolating measures. Furthermore, many paediatric nuclear medicine scans and procedures involve a significant waiting time between the administration of the radiopharmaceutical and the commencement of the scan (such as in renal scintigraphy and whole-body bone scintigraphy) or may require multiple visits on separate days (such as for MIBG scintigraphy). Adaptations in the form of screening for both patient and accompanying adult(s), as well as the provision of an adequate room and manpower for the isolation and assessment of at-risk individuals, are necessary.
Screening at points of entry
Physical access into both hospitals has been restricted to a few points of entry. Limitations on the number of accompanying adults have also been enforced.
Thermal scanners are employed to screen all visitors for fever. Administrative staff donning surgical face masks are also deployed to screen all visitors for symptoms of respiratory-tract infection, as well as high-risk travel and contact history. With the rise in local unlinked COVID-19 cases in Singapore, 8 any potential link to a known local cluster or location where COVID-19 transmission has been reported is also taken into consideration during screening. This list is also regularly redefined in the SGH COVID-19 surveillance list. High-risk visitors are either barred from entry or triaged to dedicated fever facilities for further review.
A secondary screening is performed on entry to the nuclear medicine department comprising the following three questions.
Have you travelled abroad in the past month or do you have any link to the clusters/cases at the location(s) listed in the SGH COVID-19 surveillance list?
Do you have any flu-like symptoms (e.g. fever, cough, sore throat or loss of smell)?
Are you currently or going to be monitored by the Ministry of Health for possible COVID-19 exposure?
Paediatric patients and their accompanying parent or guardian are dealt with accordingly based on their answers to the secondary screening questionnaire. High-risk patients are escorted by department staff to a designed isolation room where the nuclear medicine duty physician is called to assess the patient. There, a designated duty physician (after donning full personal protective equipment (PPE),7,8 including a N95 mask, visor, long-sleeve gown and gloves) is tasked with assessing the patient or accompanying adult before updating the designated COVID-19 consultant.
Figure 1 shows a concise illustration of our secondary screening workflow.

Concise illustration of secondary screening workflow.
Scheduling
In anticipation of potential COVID-19 surges with concomitant risks to other patients, elective procedures and scans have been rescheduled or postponed. If procedures or scans which are deemed essential have to be performed in patients known to have or who are at high risk of COVID-19 infection, they are scheduled at the end of the day to minimise contact with other patients. It is estimated that between 5 and 10 patients in the paediatric age group will still require nuclear medicine imaging at SGH.
Personal hygiene measures
Face masks are made available upon request to patients and their families. Hand sanitisers are placed at strategic locations throughout the hospitals en route to the clinics and nuclear medicine units.
Peri-procedure
Patients and accompanying adults are encouraged to sit further apart in the waiting areas. In KKWCH, two rooms have been designated as isolation rooms for use by COVID-19-suspect cases only. For PET/CT, patients and accompanying adults are held in separate uptake rooms (Figure 2).

Separate uptake rooms for paediatric patients and accompanying adult(s) for positron emission tomography/computed tomography examinations. A designed room for coronavirus disease 2019 suspect cases is marked clearly with a sign.
Across the institutions, all radiopharmaceutical injections are performed by a team of designated physicians in appropriate PPE using aseptic techniques.
Multi-day nuclear medicine scans such as MIBG scintigraphy have been designated to be performed at SGH DNMMI where physician, nursing and technologist teams have been segregated on a fortnightly rotation. Patients who require such scans will be attended to only by members of the team on the same rotation.
Equipment/room sterilisation
One gamma camera has been designated for confirmed or suspected COVID-19 cases. During the scan, the scanner bed is covered with disposable plastic sheets. 9 After completion of the scan and discharge of the patient and accompanying adults, the scanner bed and surroundings are sterilised with a terminal cleaning process (utilising agents such as the germicide detergent Mikro-Quat).
For patients undergoing PET/CT examinations, one isolated uptake room and toilet facility have been designated for confirmed or suspected COVID-19 cases. In addition, these patients will be scheduled as the first case in the morning or the last case in the afternoon to minimise disruption and delays suffered by other patients. Similarly, the PET/CT scanner bed is covered with disposable plastic sheets. After completion of the scan and discharge of the patient and accompanying adults, the scanner bed and surroundings as well as the uptake room and toilet facility undergo a terminal cleaning process.
Personnel management
Nuclear medicine staff, including physicians, technologists, nurses and health-care support staff, are critical to the daily operation of the department and hence the delivery of quality health care to patients. Hence, team segregation was instituted at an early stage, so that in the unlikely event of high-risk exposure, the affected personnel may be taken off the active roster without detriment to the delivery of health care. 10 These segregated teams work in alternate shifts of two or more weeks, alternating between direct patient and visitor contact areas (such as the main nuclear medicine department) and an isolated remote working environment (such as academia).
Staff who come down with respiratory symptoms are assessed individually, and a decision for admission into an isolated inpatient facility or discharge with five days of medical leave, respiratory sample for COVID-19 RNA polymerase chain reaction and self-quarantine will be made. All staff are also required to log their body temperatures in a national surveillance system twice a day.
One team of paediatric anesthesiologists from KKWCH is deployed to manage the paediatric cases on the SGH site. This team is kept segregated from the rest of the paediatric anesthesiologists who remain on clinical duty within KKWCH. Paediatric general anesthesiology services for nuclear medicine continue in the patients’ best interests.
Due to restrictions on cross-institution staff movement, paediatric multidisciplinary team meetings which were hosted by KKWCH are now conducted via password-secured video conferencing.
Figure 3 shows a summary of the key adaptations.
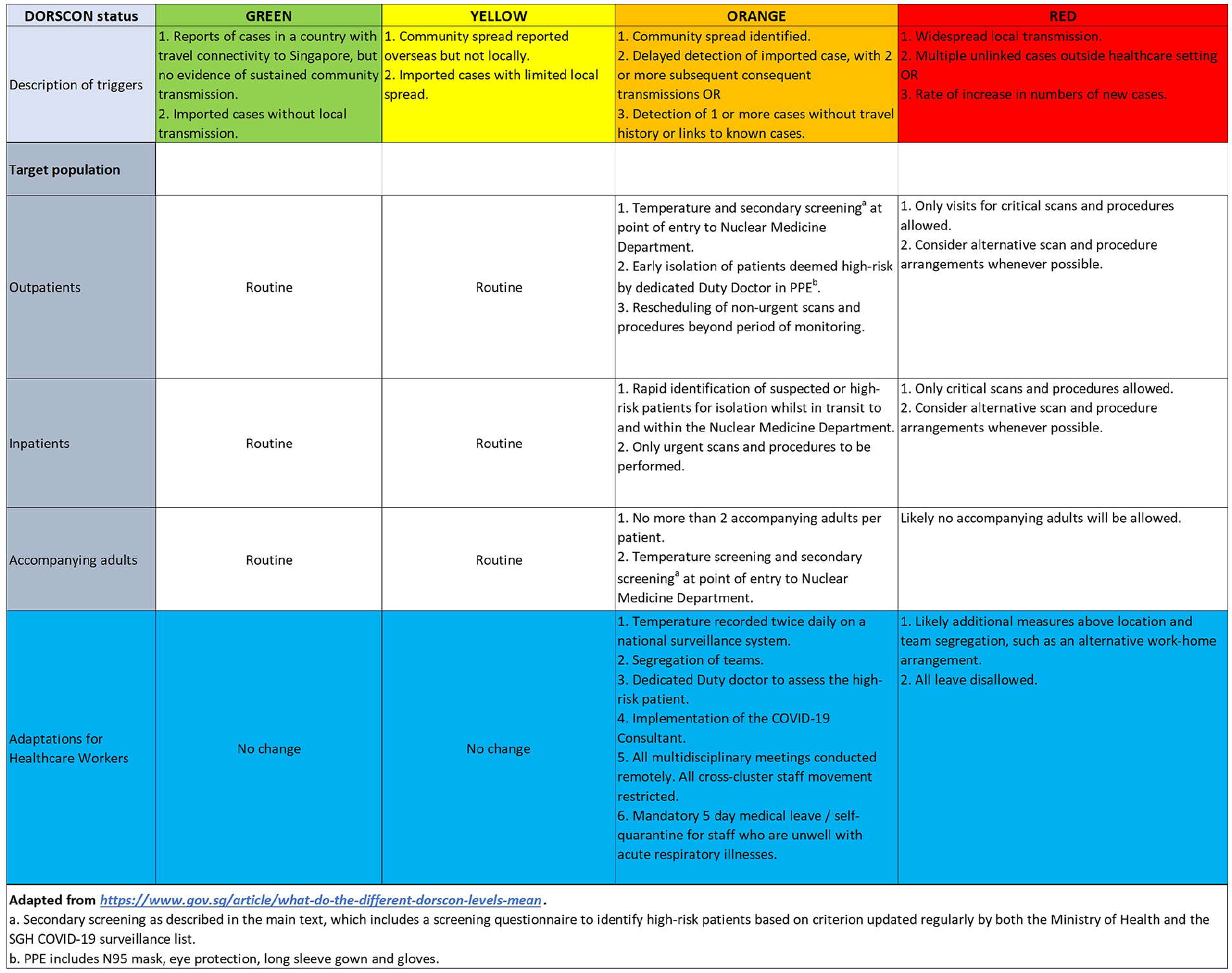
Summary of key adaptations as a response to the prevailing Disease Outbreak Response System Condition (DORSCON) status.
Conclusion
While the above practices are described in the context of nuclear medicine units, these are also broadly applicable to most paediatric ancillary services, which will be required for the continuation of paediatric care, despite the ongoing COVID-19 pandemic. We believe that with appropriate practices and measures, we can continue to protect our health-care workers, children and caregivers from contracting COVID-19 within a nuclear medicine unit in Singapore.
Footnotes
Acknowledgements
We thank Hao Cheng and Lim Yew Yee, lead technologists at National University Hospital Department of Diagnostic Imaging and KK Women’s and Children’s Hospital Department of Diagnostic and Interventional Radiology, for reviewing an early draft of the article and providing key information.
Authors’ contributions
L.C. conceptualised the article, designed the data collection instruments, collected data and revised and prepared the final manuscript for submission. P.W.M. carried out the initial analyses and drafted the initial manuscript. W.L. conceptualised the article and critically reviewed the manuscript for important intellectual information.
Availability of data and materials
Data sharing is not applicable to this article, as no data sets were generated or analysed during the current study.
Ethical approval
Not applicable because this article does not involve patient data.
Informed consent
Not applicable because patient data are not included in this article.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
