Abstract
Background:
Fibreoptic intubation via a supraglottic device (SAD) is ‘low skill fibreoptic intubation’ (LSFOI). ‘Standard’ second generation SADs (i-gelTM) have a gastric port. ‘Specialised’ second generation SADs (air-QTM) are designed to facilitate LSFOI and have wider ventilation ports. Our hypothesis was that performance of LSFOI differs between i-gelTM and air-QTM in a manikin with a simulated difficult airway.
Methods:
Our primary outcome was fibreoptic intubation success rate. Our secondary outcomes included SAD insertion and LSFOI times. A difficult airway was simulated by applying a hard cervical collar to a manikin. Anaesthetists performed LSFOI serially using both SADs in a random sequence. In the manikin study, 80 anaesthetists were recruited. To test the robustness of the conclusion from our manikin study, we repeated the study in 22 anaesthetised patients. Patients were fitted with the same cervical collar and randomly allocated to either devices. We used McNemar’s statistical test to analyse our primary outcome of successful intubations and paired nominal data. A Wilcoxon signed-ranks test was used to analyse nonparametric paired data and a Mann–Whitney U test was used for unpaired data analysis where appropriate. A p-value of <0.05 was considered statistically significant.
Results:
In the manikin study, the i-gelTM was superior to the air-QTM for successful tracheal intubation (98.8% vs 83.8%, respectively; p=0.002) and LSFOI times (34.0 s vs 36.0 s, respectively; p=0.012). In the patient study, LSFOI success rates were not significantly different between i-gelTM and air-QTM (100% vs 91.6%, respectively; p=0.545) but intubation times were shorter (52.5 s vs 60.0 s, respectively; p=0.036).
Conclusion:
In conclusion, we obtained LSFOI success rates for the i-gelTM or air-QTM of 98.8% and 83.8% respectively in a manikin; and 100% and 91.6% respectively in patients. It is in fact ‘low skill’ as many participants were successful despite no prior experience with LSFOI. The i-gelTM is superior for LSFOI compared with the air-QTM. This is despite being a ‘standard’ second generation SAD as compared to a ‘specialised’ second generation SAD (air-QTM).
Trial Registration:
The manikin and patient studies were conducted after being approved by the SingHealth Centralised Institutional Review Board (CRB reference number 2014/2039 and 2016/2069, respectively). The patient study was registered at ClinicalTrials.gov (ID: NCT02663843).
Introduction
Up to 93% of difficult intubations are unexpected 1 and may require advanced airway techniques to secure the airway. Fibreoptic intubation (FOI) involves the use of an intubating fibreoptic bronchoscope (FOB) to achieve correct placement of a tracheal tube through the glottis and into the trachea via the nasal or oral route. However, it is a complex psychomotor skill with a steep and long learning curve. To facilitate FOI, ‘low skill’ FOI (LSFOI) was developed. It involves placing a supraglottic airway device (SAD) into the oropharynx of an anaesthetised patient followed by FOI via the device. 2 The SAD acts as a conduit guiding the FOB towards the glottis. LSFOI is performed with the FOB preloaded with either a tracheal tube (‘direct’ method) or an Aintree intubating catheter (‘indirect’ method). 2 In the direct method, after FOB placement into the trachea via the SAD, the tracheal tube is railroaded over the bronchoscope and into the trachea. LSFOI features in many international difficult airway algorithms3–6 and has been used in both elective and emergency difficult airway cases.7,8
The first generation SADs, such as the classic laryngeal mask airway, are ‘simple airway devices’. ‘Standard’ second generation SADs have separate ventilation and gastric ports. Specifically designed ‘specialised’ second generation SADs have, in addition, wider (and some have shorter) ventilation ports to facilitate direct LSFOI. A shorter ventilation port allows a great depth of insertion of the tracheal tube tip beyond the SAD, therefore allowing proper cuff inflation to reduce the risk of a ventilation leak at the level of the vocal cords. 9 The i-gelTM (Intersurgical Ltd, Wokingham, Berkshire, UK) is a ‘standard’ second generation SAD but has a noninflatable cuff designed to reduce airway trauma. Its internal diameter and length of the shaft of a size 3 device is 11.2 mm and 189 mm, respectively. The air-QTM (ILA; Cook-gas®, St Louis, MO, USA) is a ‘specialised’ second generation SAD and has a conventional inflatable cuff. The internal diameter and length of the shaft of the size 2.5 (corresponding to the size 3 i-gelTM) are 11.4 mm and 150 mm, respectively. Both devices have been used successfully for LSFOI.7,8
We hypothesised that the success rates and performance of LSFOI differs between the i-gelTM and the air-QTM (a non-specialised vs a specialised SAD, respectively) in a manikin with a simulated difficult airway. Our primary outcome was LSFOI success rate. Our secondary outcomes were: SAD insertion and ventilation times; LSFOI times; fibreoptic view of the glottis; manipulation score of the FOB; resistance during railroading of the FOB; and intubation success in relation to the operator’s years of anaesthetic experience. Very few manikin studies have been followed up with a patient study.10,11 We therefore repeated the study using experienced operators in anaesthetised patients with a simulated difficult airway, randomised to either i-gelTM or air-QTM devices, to confirm the robustness of our initial results. Further secondary data in the patient study included: ease of face mask ventilation; complications (trauma to the lips, teeth of airway, SpO2<94%, wheeze or stridor, sore throat); and changes in physiological parameters (heartrate, blood pressure and pulse oximetry).
Methods
Manikin study
Eighty anesthetists of varying seniority were recruited, and informed consent obtained to participate in the study. Data were collected regarding participant’s experience: years of anaesthetic experience (<5 years or ⩾5 years); previous use of either SAD (i-gel™ or air-QTM); and previous performance of LSFOI in a manikin or patient. Each participant watched a video presentation detailing the technique of LSFOI before starting the study.
The manikin used was the Laerdal® Airway Management Trainer (Laerdal® Medical Ltd, Orpington, Kent, UK). A rigid cervical collar (Sierra Universal Collar™, Aspen Medical Products, Irvine, CA, USA) was applied to restrict mouth opening and neck movement to simulate a difficult airway. As part of the randomised crossover study, we compared the air-QTM size 2.5 and the i-gelTM size 3. A 4.4 mm intubating FOB (Olympus BF-MP 160F, Singapore Pte Ltd) was preloaded with a MallinckrodtTM (Covidien, Mansfield, MA, USA) 6.0 mm microlaryngeal tracheal tube for each test. All airway devices and the oropharynx of the manikin were lubricated before each attempt.
Each participant performed the two crossover LSFOIs sequentially without a rest period using the air-QTM and i-gelTM devices, the order of which was randomised by using an online research randomiser (https://www.randomizer.org/). No verbal cues or assistance were given. The primary outcome measure was the rate of successful LSFOIs (as evidenced by inflation of the manikin lungs). Failure was defined as an attempt ⩾3 minutes or accidental oesophageal intubation. The following secondary outcomes were also measured. SAD insertion times was the time from picking up the SAD to the start of delivering a single breath via the self-inflating bag. Intubation times was the time from picking up the FOB to the start of delivering a single breath via the self-inflating bag. Glottic view was the fibreoptic view of the glottis on exiting the bowl of the SAD: 1=vocal cords entirely visible; 2=vocal cords and/or arytenoids partially visible; 3=epiglottis only visible; and 4=no laryngeal structures visible. A manipulation score was based on the investigator’s observation of the amount of movement of the tip of the FOB during the LSFOI attempts: 1=minimal; 2=moderate; 3=extensive; 4=failed attempt; and any entry into the oesophagus by the FOB was also recorded. Resistance to railroading the tracheal tube through the SAD was scored as: 1=none; 2=minor; 3=marked; and 4=railroading not possible. We also recorded any oesophageal intubations.
Patient study
A study was conducted on 22 patients after written informed consent was obtained. Inclusion criteria were: aged 21 years or above; American Society of Anesthesiology (ASA) physical status I and II; and undergoing general anesthesia for elective surgery requiring tracheal intubation. Exclusion criteria were patients with: ASA physical status III and IV; a history of previous difficult endotracheal intubation; two or more predictors of difficult airway management (airway masses or previous airway operations, Mallampati III or IV 12 , thyromental distance <6.5 cm, interincisor distance <3 cm, head extension <30o, edentulous, large beard, obstructive sleep apnoea or snorer); indications for rapid sequence induction; and pregnant women. The patients were randomised into equal proportions for the two devices (10 for the i-gelTM and 12 for the air-QTM arm each) using www.randomizer.org. The operators were two authors (PW and GL) who had considerable experience with the i-gelTM (>50 insertions) but none with the air-QTM in patients (but practiced in manikins ⩾2 occasions before the study which revealed no issues during insertion or ventilation). Both were experienced in LSFOI. We used two experienced operators to standardise methodology and to minimise the risk to patients with a simulated difficult airway. They were not blinded to the SAD device due to their participation.
Before the induction of anaesthesia, patients demographics were documented and airway assessments were measured: age, sex, weight and height, Mallampati grade, interdental distance, thyromental distance, mandibular luxation score. 13 A rigid cervical collar (as used in the manikin study) was then applied, and the interdental distance was measured again. We applied standard monitoring and preoxygenated with 100% oxygen for 3 minutes. Intravenous induction was administered, with the choice and dose of anaesthetic agents at the discretion of the attending anaesthetist. After confirmation of adequate bag-mask ventilation, intravenous neuromuscular agent was administered (either atracurium 0.5 mg/kg or rocuronium 0.6 mg/kg). Bag-mask ventilation was continued for 3 minutes with 100% oxygen and sevoflurane (to obtain an end tidal concentration target of 1.5-2%). Complete neuromuscular blockade was established with train-of-four monitoring. The allocated SAD (at the discretion of the attending anaesthetist) was inserted, and, for the air-QTM, the cuff inflated (cuff pressure to 20 cmH2O). Successful insertion of, and ventilation using, the SAD was confirmed by the appearance of a normal capnograph tracing. LSFOI using the 4.2 mm fibreoptic bronchoscope (preloaded with a tracheal tube) was then performed. The tracheal tubes used were: 6.0 mm microlaryngoscopy tube or 6.5 mm standard tracheal tube for the air-QTM size 2.5 and i-gelTM size 3 (tracheal tube size was at the discretion of the attending anaesthetist); and 7.0 mm tracheal tube for the air-QTM size 3.5 and 4.5, and i-gelTM size 4. The tracheal tubes were previously well lubricated and checked for easy insertion into their respective SAD. Successful LSFOI was confirmed by the appearance of a normal capnograph tracing. If required, external laryngeal pressure, jaw thrust, or manipulation of the SAD were performed to facilitate LSFOI. After successful LSFOI, the SAD was carefully removed. Failure of LSFOI was defined as failure after two attempts, failure to intubate within 3 minutes, oesophageal intubation or the patient’s SpO2 decreasing to below 94%.
Data collected during LSFOI included: ease of face mask ventilation (Han’s classification: 1=ventilated by mask; 2=ventilated by mask with oral airway or other adjuvant; 3=difficult mask ventilation which is either inadequate, unstable or requiring two practitioners; and 4=unable to mask ventilate); 14 SAD insertion success (primary outcome, as indicated by the appearance of a normal capnograph trace) and number of attempts; SAD insertion time (time from picking up the SAD to the appearance of a normal capnograph trace); glottic view (as per the manikin study); LSFOI success and number of attempts (including oesophageal intubation); intubation times (time from picking up the FOB to the appearance of a normal capnograph trace); FOB manipulation score and resistance during railroading of the fibrescope (as per the manikin study); number of oesophageal entries by the FOB; and complications (trauma to the lips, teeth of airway, SpO2<94%, wheeze or stridor, sore throat). During the study, heartrate, blood pressure and pulse oximetry readings were measured every minute. Haemodynamic instability included bradycardia, tachycardia, hypotension and hypertension which were defined as >20% difference from baseline measurements.
Statistical analysis
We referred to previous similar manikin studies, 15 which evaluated LSFOI via the classic laryngeal mask airway. For our manikin crossover study comparing the i-gelTM with the air-QTM, we calculated that a minimum of 13 anaesthetists required to give values for α =0.05 and beta 0.2. As this was a manikin study, we used this opportunity to train anaesthetists on LSFOI and so recruited a total of 80 anaesthetists (approximately half our anaesthetic personnel). We used McNemar’s statistical test to analyse our primary outcome of successful intubations and paired nominal data. A Wilcoxon signed-ranks test was used to analyse nonparametric paired data and a Mann–Whitney U test was used for unpaired data analysis where appropriate. Statistical analysis was performed using SPSS version 20 software (SPSS Inc., Chicago, IL USA) and a p-value of <0.05 was considered statistically significant. To test the robustness of the conclusion from our manikin study, we explored the study in 22 anaesthetised patients.
For the statistical analysis, we combined the FOB manipulation ‘minimal’ and ‘moderate’ scores and compared them with the combined ‘extensive’ and ‘fail’ scores. Similarly, we combined the resistance during railroading of ‘none’ and ‘minor’ resistance gradings, and ‘marked’ with ‘not possible’ gradings. The timings of various components of LSFOI only included successful attempts.
The patients’ demographics and airway measurements are shown in Table 1 and results of LSFOI performance using both SADs in manikins and patients are tabulated in Table 2.
Baseline demographics and airway measurements of patients in each group: Air-QTM vs I-gelTM. Values are mean (SD), median [IQR].

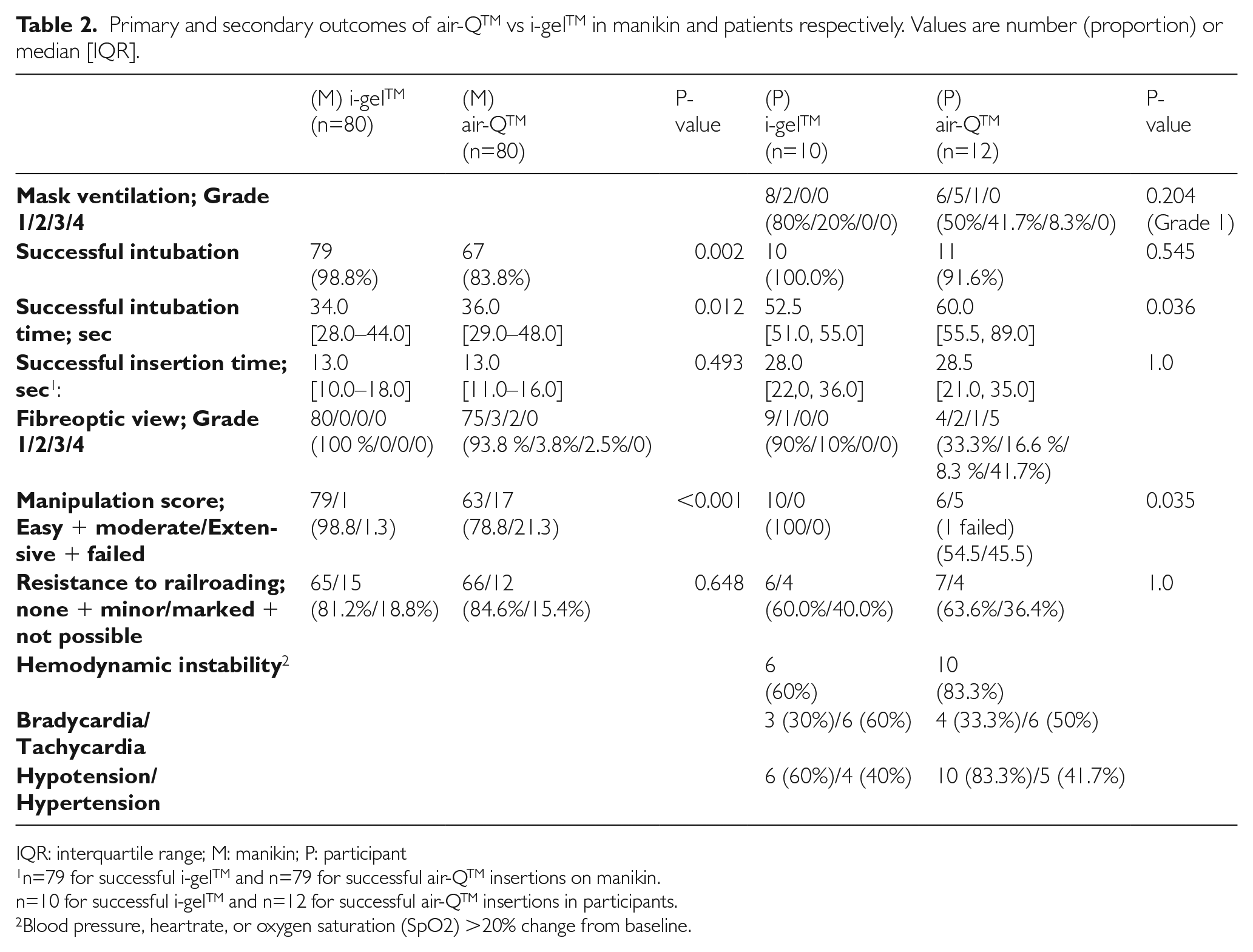
Primary and secondary outcomes of air-QTM vs i-gelTM in manikin and patients respectively. Values are number (proportion) or median [IQR].
IQR: interquartile range; M: manikin; P: participant
n=79 for successful i-gelTM and n=79 for successful air-QTM insertions on manikin.
n=10 for successful i-gelTM and n=12 for successful air-QTM insertions in participants.
Blood pressure, heartrate, or oxygen saturation (SpO2) >20% change from baseline.
Results
Manikin study
Eighty anaesthetists were recruited into the study. 39 participants (48.8%) had <5 years’ experience while 41 participants (51.2%) had ⩾5 years’ anesthetic experience. Thirty-four (42.5%) had previously inserted the i-gelTM while only three (3.8%) had done so with the air-QTM. Only 19 (23.8%) participants had previously performed LSFOI; 12 (15.0%) on a manikin only and seven (8.8%) on patients.
For the primary outcome of successful LSFOI, the i-gelTM was superior to the air-QTM (98.8% vs 83.8%, respectively; p=0.002). The results for the secondary outcomes are as follows. Successful SAD insertion rates and insertion times were similar for both SAD: 98.8% (one failure with both devices) and 13.0 s, respectively. The time for successful LSFOI was statistically significantly shorter with the i-gelTM than with the air-QTM (34.0 s vs 36.0 s, respectively; p=0.012). LSFOI with the i-gelTM gave superior results against the air-QTM: higher incidence of combined ‘easy’ and ‘moderate’ manipulation scores (98.8% vs 78.8%, respectively; p<0.001); less oesophageal entry by the FOB (1.3% vs 23.8%, respectively; p=<0.001); and fewer oesophageal intubations (1.3% vs 16.3%, respectively; p=0.007) were observed. There was a higher incidence of grade 1 glottic view obtained but this was not statistically significant (100% vs 93.8%, respectively; p=0.068). Resistance to railroading was similar for both devices (i-gelTM 81.2% vs air-QTM 84.6%, p=0.648). SAD insertion times and LSFOI times were not significantly associated with the operator’s anaesthetic experience (⩾5 years versus <5years).
Patient study
We recruited a total of 22 patients for the patient study: 12 for the air-QTM and 10 for the i-gelTM. The mean interdental distances before and after placing the cervical collar were: for the i-gelTM 4.2 mm and 3.7 mm, respectively; and for the air-QTM 4.5 mm and 3.9 mm, respectively. Successful LSFOI was high for both the i-gelTM and air-QTM (100% vs 91.6%, respectively; p=0.545). There was a higher incidence of grade 1 face mask ventilation with the i-gelTM compared with the air-QTM but this was not statistically significant (80% vs 50%, respectively). There was a 100% success rate for SAD insertion and also similar insertion times for both devices. Similar to the manikin study, LSFOI using the i-gelTM had superior results compared with the air-QTM: shorter time for successful LSFOI (52.5 s vs 60.0 s, respectively; p=0.036); higher incidence of glottic grade 1 views (90% vs 33.3%, respectively; p=0.011); and higher incidence of combined ‘easy’ and ‘moderate’ FOB manipulation scores (100% vs 54.5%, respectively; p=0.035). In addition, there was one LSFOI failure with the air-QTM but none with the i-gelTM. There was no statistical difference for the incidence of combined ‘none’ and ‘minor’ resistance during passage of the tracheal tube between the two devices (60.0% vs 63.6%, respectively; p=1.0). Haemodynamic instability during LSFOI occurred with both the i-gelTM and air-QTM: bradycardia in 30% of cases for both devices; tachycardia in 60% and 50%, respectively; hypotension in 60% and 83%, respectively; and hypertension in 40% for both.
Discussion
There are several conclusions from our study. First, we obtained LSFOI success rates for the i-gelTM or air-QTM of 98.8% and 83.8% respectively in a manikin; and 100% and 91.6% respectively in patients. Second, the i-gelTM is a superior device for various secondary outcomes of LSFOI. Third, in the manikin, LSFOI is in fact ‘low skill’ as evidenced by the high success rates in LSFOI despite only a small number of participants having previously performed LSFOI. Furthermore, the operator’s years of anaesthetic experience did not influence intubation timings. Fourth, outcomes of the manikin study were in concordance with the patient study, favouring the i-gelTM over air-QTM in LSFOI. This gives construct to our manikin study and overall result findings.
The i-gelTM (a ‘standard’ second generation SAD) performed better than the air-QTM (a ‘specialised’ second generation SAD designed for LSFOI by virtue of its wider shaft that allows for easier tracheal tube insertion). This indicates that other SAD design characteristics (discussed below) are important for LSFOI. In the manikin study, use of the i-gelTM was associated with higher LSFOI success rates, shorter successful LSFOI times, and superior manipulation scores, and more accurate passage of the FOB resulting in less entry into the oesophagus and less oesophageal intubation. In the patient study, the i-gelTM was associated with shorter successful LSFOI times, a higher incidence of grade 1 glottic views, and superior manipulation scores. Studies have shown that LSFOI with the i-gelTM has a high first attempt success rate (even in predicted difficult airway) of 93-96%.8,16 In contrast, success with LSFOI for the air-QTM was only 74%. 17 We therefore recommend the use of the i-gelTM for LSFOI over the air-QTM.
The i-gel TM is made of ‘medical grade thermoplastic elastomer designed to create a noninflatable, anatomical seal of the pharyngeal, laryngeal and peri-laryngeal structures’ (www.intersurgical.com). One cadaver study confirmed its design features befitting its function as a SAD: the gel-like mask’s ability to conform to the perilaryngeal anatomy and cervical oesophagus; improved the mucosal seal; and stable positioning against the base of the tongue. 18 The noninflatable cuff also reduces potential airway obstruction or an impaired view of the glottis. 19 In our study, the i-gelTM enabled a high incidence of fibreoptic grade 1 glottic views in manikin and patients (100% vs 90%, respectively). This is supported by other studies where a clear view of the glottis is seen in 71–91% of cases, with down-folding of the epiglottis occurring in 7% of cases.20,21 In one air-QTM study, glottic grades 1 and 2 views were seen in 88% and 12% of cases, respectively. 22 A clear view of the glottis is beneficial as less FOB manipulation is required and may lead to faster LSFOI times.15,23
Awake FOI is the gold standard technique for various types of difficult airways. 24 However, it is a complex psychomotor skill associated with a steep learning curve,25,26 which is compounded by a lack of training opportunities.27–29 In contrast, LSFOI is usually performed in anaesthetised patients. Our manikin study shows that it is in fact ‘low skill’ since LSFOI was performed with moderate to high success rates despite little or no previous experience with the i-gelTM, air-QTM or LSFOI. In addition, the operator’s years of anaesthetic experience also had no significant influence on intubation timings. The ‘low skill’ aspect is due to the SAD opening up the oropharyngeal cavity and providing a channel to guide the FOB towards the glottis (grade 1 view seen with the i-gelTM in 100% and 90% of cases in the manikin and patient studies, respectively). This obviates the need for inexperienced operators to recognise or manoeuvre around various anatomical structures of the airway to reach the glottis. One case series showed that, even in difficult airways, novices achieved successful LSFOI. 30
With 100% insertion success and similar times for both SADs, we consider it likely that the differences in glottic view during LSFOI is due to the anatomical fit of the SAD in the oropharynx rather than lack of familiarity with the air-QTM. Despite LSFOI with the air-QTM having higher incidences of grade 3 or 4 views than the i-gelTM (50% vs 0%, respectively), the difference in intubation time was only 7.5 s longer. This may be due to LSFOI being performed by experienced operators. Also, the glottic view recorded was defined by the view after the FOB exits the SAD bowl (e.g. an initial grade 3 view); however after minor manoeuvring and advancement of the FOB, a better view of the glottis may come into view (e.g. grade 1 view) and intubation completed without much delay.
Our study also shows that results and conclusions from the manikin study are in line with our patient study but should be cautiously interpreted. Manikins can be used to test and teach new airway devices and/or techniques, and they have many advantages over patients.31,32 However, there is a proviso that ‘manikin studies are all well and good, providing your patients are manikins’. 33 Manikins have larger oral, retropalatal and pharyngeal spaces, 34 and also they lack realism due to poor anatomical, functional and tissue fidelity.35,36 Therefore authors have questioned the validity of extrapolating manikin data to human subjects.32,34,37,38 Therefore, we followed up ours with a patient study. The latter confirmed the direction and sensitivity of the manikin study. However, the times for successful LSFOI were slower in patients than in the manikin, and this may be due to various reasons. First, there was a lower incidence of grade 1 glottic views in patients than in manikins. Second, resistance to railroading was higher in patients. The smaller dimensions of a patient may cause a more acute angle between the vertical standing shaft and the horizontal lying bowl of the SAD after insertion, making subsequent railroading more difficult. This may also lead to inadvertent withdrawal of the FOB out of the trachea, resulting in oesophageal intubation. 15 Third, the endpoint for times for successful insertion or intubation were different: in the manikin, it was visualisation of the lungs inflating whereas in patients it was the appearance of an adequate capnograph trace which includes a sampling lag time of 1–4 s. 39 In addition, LSFOI in the manikin was associated with FOB entries into the oesophagus and oesophageal intubations, more so with the air-QTM than with the i-gelTM. Neither events occurred in patients, and there are several possibilities. First, in patients, the tip of the bowl of SAD sits and blocks the upper oesophageal sphincter whereas the larger airway dimensions of manikins may preclude this. Second, in the manikin, we noticed that the air-QTM tended to be more posteriorly placed in the oropharynx resulting in a ‘wide angle’ view compared with the i-gelTM ‘telephoto’ view, thus exposing the oesophageal inlet. Third, only experienced operators performed LSFOI in the patient study.
Haemodynamic instability during LSFOI occurred with both devices in up to 30–83% of cases and may be partly due to the method of intravenous induction of anaesthesia being left at the discretion of the attending anaesthetist. However, all patients were easily stabilised.
Our study has several limitations. First, the manikin poorly replicates a patient’s anatomy or its physiological responses to airway management. However, we used the Laerdal manikin as it is one of the best performing low fidelity manikins. 36 Second, participants performed the crossover LSFOI sequentially without a rest period; performance of LSFOI with the second SAD may have benefited from prior practice with the first SAD. However, the sequence was randomised to minimise this effect. Third, we originally intended to recruit 12 patients for each SAD but were unable to do so within the original grant funding projections. Nevertheless, our primary intention was to explore the direction and sensitivity of our results from manikin study. It was also not possible for the investigator or the participants to be blinded due to the nature of the study. Next, participants may have more experience with insertion of, and LSFOI with, the i-gelTM rather than the newer air-QTM. This skewed data (greater familiarity with the i-gelTM) would bias results in favour of the i-gelTM. However, in the manikin study, most participants had never performed LSFOI and so may not be familiar with either SAD. In addition, in the patient study, where operators were senior consultants with considerable experience with LSFOI, successful SAD insertion rates and times were similar and yet glottic views obtained were poorer with the air-QTM. Passage of the FOB through the ventilation port (in order to view the glottis) is unlikely to be different between the SADs. This suggests that the poorer glottic view is due to less favourable anatomical seating of, rather than less familiarity with, the air-QTM. Finally, the scores for FOB manipulation and resistance to railroading were subjective leading to a possible source of bias. However, using a single investigator provided standardisation.
In conclusion, our study has demonstrated LSFOI success rates for the i-gelTM or air-QTM of 98.8% and 83.8% respectively in a manikin; and 100% and 91.6% respectively in patients. The manikin study included inexperienced operators, most of whom had no prior experience with LSFOI. The i-gelTM, despite being a ‘standard’ second generation SAD, was superior for LSFOI compared with the air-QTM, a ‘specialised’ second generation SAD. This indicates that specially designed SADs do not necessarily lead to better LSFOI performance. Both our manikin and patient studies showed similar results in favour of i-gelTM over air-QTM in LSFOI.
Footnotes
Acknowledgements
We thank Dr Tan Hiang Khoon, all reviewers, and members in the Division of Surgery for their help. The i-gelTM and air-QTM airway devices were kindly donated by TE Medicare Pte Ltd (Singapore) and Kenda (S) Pte Ltd (Singapore), respectively.
Authors’ contributions
SXLJ contributed to data collection, analysed the data and made significant contributions in writing the manuscript. HR and WGLT made substantial contributions to conception and design, interpreting the data, as well as editing the manuscript. GL and PW were both the senior anaesthetists involved in performing LSFOI in the patient study. PW was heavily involved in both the manikin and patient studies, and a major contributor in writing the manuscript. All authors read and approved the final manuscript.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Ethics approval
The manikin and patient studies were conducted after being approved by the SingHealth Centralised Institutional Review Board (CRB reference number 2014/2039 and 2016/2069, respectively). The patient study was registered at ClinicalTrials.gov (ID: NCT02663843).
Informed Consent
Written informed consent was obtained from all subjects before the study.
Trial Registration
The patient study was registered at ClinicalTrials.gov (ID: NCT02663843).
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Two of the authors (PW and WGLT) have received free SADs and loan of FOB from various companies for evaluation, research and airway workshop purposes, but they have no financial interests in any of the companies.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This initiative was funded by the SingHealth Duke-NUS Academic Medical Centre, facilitated by the Joint Office of Academic Medicine (JOAM). It was an initiative of the Surgery Academic Clinical Program (SURG ACP), hosted at the Singapore General Hospital (SGH).
