Abstract
Introduction:
The management of head and neck surgical patients is associated with increased morbidity and mortality, and so anticipating the difficult airway is important.
Methods:
We undertook a prospective survey on consecutive adult patients scheduled on the elective operating lists of four head and neck consultant surgeons. Data were collected over a 36 month period. Data included: patient characteristics; routine predictors of difficulty in airway management (bedside tests of the airway, a history of previous surgery or radiotherapy and the presence of airway symptoms); laryngoscopy grade; method of anaesthesia and airway management; and any airway complications arising during induction of anaesthesia and extubation.
Results:
The ‘study’ group consisted of 818 patients. The ‘direct laryngoscopy’ group contained 674 patients, that is, patients who had direct laryngoscopy and could therefore be classified as easy or difficult intubation. The prevalence of difficult intubation was 12.6%. Factors or tests that were statistically significantly associated with difficult intubation were: history of difficult airway; previous head or neck radiotherapy treatment; presence of airway symptoms; presence of moderate or severe limited neck movement; and short interdental distance. The sensitivity, specificity and positive predictive values were: history of difficult airway 16.5%, 98.6% and 63.6%; previous radiotherapy 12.9%, 96.6% and 35.5%; airway symptoms 42.9%, 69.6% and 15.9%; moderate/severe neck limitation 16.7%, 97.2% and 46.7%; Mallampati score 3 or 4, 38.8%, 83.8% and 25.8%; and interdental distance 9.4%, 98.8% and 53.3%, respectively. The Bonfils intubation fibrescope was the most commonly used indirect laryngoscopy device (63.9% of all such cases). Twenty-six patients (3.2%) had complications during their initial airway management after induction of anaesthesia. There was one case of ‘cannot intubate, cannot oxygenate’, which required an emergency tracheostomy.
Conclusion:
The prevalence of difficult intubation in head and neck surgical patients was higher than in the general population, but predictive tests for difficult intubation have poor to moderate value. In our study, rates of difficult face mask ventilation, failed intubation and complications during induction and extubation were low. However, serious morbidity, although rare, can still be encountered. Head and neck surgical patients can be managed safely in a tertiary centre where there is appropriate surgical and anaesthetic expertise in managing difficult airways.
Introduction
The American Society of Anesthesiologists defines a difficult airway as ‘the clinical situation in which a conventionally trained anesthesiologist experiences difficulty with facemask ventilation of the upper airway, difficulty with tracheal intubation, or both’. 1 The incidence of difficult intubation is higher in patients with ear, nose and throat (ENT) malignancies than in the general surgical population (15.75% vs. 2.5%). 2 The 4th National Audit Project in the UK (NAP4) reminded us that ‘head and neck’ (H&N) surgery is high risk and is associated with death and brain damage. 3 Difficult intubation is also associated with increased morbidity and higher rates of unplanned intensive care unit admissions and postoperative complications.3,4 The ability to predict such difficulties may therefore reduce these rates.
Objectives
We investigated the anaesthetic management of adult elective H&N surgical patients who presented to our teaching hospital, which is also a tertiary referral centre for H&N patients. Our aims were to:
Calculate the prevalence of difficult intubation (defined as a Cormack–Lehane laryngoscopy score of 3 or 4). 5
Determine the predictive value of routine anaesthetic airway assessment and other risk factors (airway symptoms, and previous H&N surgery or treatment with radiotherapy) for predicting difficult intubation.
Report on the anaesthetic management of H&N patients including failures of, and complications arising from, initial anaesthetic airway management and during extubation.
Methods
Data were collected prospectively over a 36-month period (from June 2010 to May 2013) on consecutive adult patients scheduled for elective H&N surgery at our institution, a large London teaching hospital and referral centre for H&N surgery. Surgery included benign and malignant disease, although occasional emergency airway cases were added to the operating lists. Surgery was performed by one of four H&N consultant surgeons with a specialist interest in cancer surgery, or by their registrars under supervision. Anaesthetic care was provided by one of four H&N anaesthetic consultants or by a specialist registrar under supervision (who had at least 4 years’ anaesthetic experience). Ethics approval was sought and the local research ethics committee advised that, as the project was a prospective survey, formal approval was not required. However, patients’ written consent was still obtained for collecting data.
Preoperative data were collected on patients’ physical characteristics, grade of anaesthetist and the findings on routine beside airway assessment. Predictive risk factors for difficult intubation were recorded under the following headings: airway symptoms (hoarse voice, stridor, dyspnoea or postural symptoms) and anatomical airway bedside tests (modified Mallampati score, 6 interdental distance (IDD), thyromental distance, mandibular luxation score 7 and neck movement.
The Mallampati score is an indirect measure of the oro-pharyngeal space (required for direct laryngoscopy), and is based on the ability to visualise various anatomical structures when a patient maximally opens his/her mouth: 6 grade 1 – soft palate, uvula, fauces and tonsillar pillars visible; grade 2 – soft palate, uvula and fauces visible; grade 3 – soft palate and base of uvula visible; grade 4 – only hard palate visible. Trismus was defined as IDD ⩽2.5 cm. Limitation of neck movement (mild, moderate or severe) was a subjective assessment made by the anaesthetist. Difficult face mask ventilation was one that required two hands or an oral airway. 8
Direct laryngoscopic view was graded according to the modified Cormack–Lehane scoring system: grade 1 – full view of vocal cords; grade 2a – partial view of vocal cords; grade 2b – only arytenoids and epiglottis visible; grade 3a – epiglottis visible and liftable; grade 3b – epiglottis adherent to pharynx and grade 4 – neither glottis or epiglottis visible.5,9,10 The best view obtained at direct laryngoscopy was recorded whether using a standard or long blade Macintosh laryngoscope, or whether cricoid pressure or external laryngeal manipulation was applied. If ‘check’ direct laryngoscopy was performed; for example, after awake fibreoptic intubation (FOI) or blind nasal intubation, then the best estimate of the Cormack–Lehane score was recorded. Difficult intubation was classified as a Cormack–Lehane score of 3a, 3b or 4. 10
Anaesthetic induction and airway management techniques, and any associated complications were recorded. Conduct of anaesthesia was operator specific. There were no restrictions or impositions placed on the intubating position, method of anaesthetic induction, muscle relaxant used and type of airway devices or adjuncts used. Tracheal intubation could be performed by direct laryngoscopy (using Macintosh or McCoy laryngoscopes) or indirect laryngoscopy (see Table 1 for list of techniques).
Study group (n=818) and direct laryngoscopy group (n=674): airway techniques performed and number of patients.

Airtraq (Prodol Meditec SA, Vizcaya, Spain), GlideScope (Saturn Biomedical Systems, Burnaby, BC, Canada) and the Venner AP Advance (APA; Venner Medical Pte. Ltd., Singapore).
The ‘study’ group.
The ‘intubation’ group.
Combined direct (Macintosh or McCoy) with indirect (Bonfils) laryngoscopy for tracheal intubation.
Statistical analysis
Statistical analyses were carried out using SPSS for Windows v20.0 (SPSS Inc., Chicago, IL, USA). The association between difficult intubation and bedside tests, previous treatments (radiotherapy or H&N surgery) or the presence of airway symptoms was determined using univariate analysis (predominantly chi-squared and Student’s t test) where appropriate. For each univariate analysis, records that did not contain either a record of the independent or the dependent variable, were excluded from the analysis.
Results
Data were collected from an initial group of 922 attendances. We obtained a ‘study’ group (n=818) after the following patients were excluded: refusal of consent for data collection, paediatric patients, repeat attendances (to avoid confounding the data) and those with no patient identification (therefore unable to verify if they were repeat attendances or not). These are shown in a study flowchart (see Figure 1). Six hundred and ninety-seven patients had a documented Cormack–Lehane score (either by direct or indirect laryngoscopy). The direct laryngoscopy group (n=674) were made up of patients who had direct laryngoscopy performed for one of three reasons (see below) (Table 1).

Study flowchart detailing patient attendances and the composition of ‘study’ and ‘direct laryngoscopy’ groups. Reasons for exclusion of various patient attendances are provided.
The patient characteristics of the study and direct laryngoscopy groups (mean (SD (range)) were as follows: age 55.9 (15.4) (18–95) and 56.0 (15.5 (19–95) years, respectively; and weight 76.5 (19.0) (35–150) and 76.9 (19.2) (35–150) kg, respectively. The numbers of male/female patients in each group were 465/349 and 381/289, respectively (deficit due to unrecorded data).
Prevalence of difficult intubation
Table 1 presents the Cormack–Lehane scores obtained from patients in the study group. The prevalence of difficult intubation was 12.6% in this group.
Predictive value of routine anaesthetic airway assessment and risk factors
Table 2 shows the number of patients with predictors of difficult intubation, and those who then presented with actual difficult intubation. Five out of nine tests were statistically significantly associated with difficult intubations: history of difficult airway; previous head or neck radiotherapy treatment; presenting with airway symptoms; presence of moderate or severe limited neck movement and short IDD. Table 3 presents the predictive values (sensitivity, specificity and positive and negative predictive values) of the airway predictors of difficult intubation.
Intubation group (n=674): predictors of difficult intubation and number of patients with difficult intubation on laryngoscopy (Cormack–Lehane score 3 or 4).

Percentages derived using denominator of total completed records for the predictor/test.
Percentages of difficult and easy intubation are derived using the denominator of those patients with a documented ‘positive’ test result.
Intubation group (n=674): predictors of difficult intubation and their predictive values.

PPV: positive predictive value; NPV: negative predictive value.
There was no significant difference in mean patient weight (kg) in patients difficult and easy to intubate (mean (SD)), that is, 73.52 (21.03) vs. 77.44 (18.98), respectively; t=−1.518, P=0.130 (data parametrically distributed – equal variances assumed).
Anaesthetic management, failures and complications
Table 1 shows the various techniques performed in the study and direct laryngoscopy groups: induction; type of airway used; adjuncts to facilitate tracheal intubation; and other means of securing the airway.
Direct laryngoscopy was performed in 674 patients in the direct laryngoscopy group for three reasons (Table 1). Firstly, to assist in conventional tracheal intubation, that is, Macintosh laryngoscope (n=455) and McCoy laryngoscope (n=6). Secondly, to assist during Bonfils FOI, that is, Macintosh laryngoscope (n=177) and McCoy laryngoscope (n=4). Thirdly, for checking direct laryngoscopy after the airway had previously been secured by indirect methods (n=32). This latter group included: flexible FOI (n=24); intubation via an intubating laryngeal mask airway (LMA) (n=5); ‘low skill’ FOI (n=2); and blind nasal intubation (n=1). This latter check provides valuable information to future anaesthetists about the ease or difficulty of tracheal intubation.
Indirect laryngoscopy techniques for tracheal intubation was used in 288 patients. There is an overlap in the number of patients who had direct and indirect laryngoscopy as these techniques were not mutually exclusive (Table 1). The main reason is that 184 patients had their trachea intubated using the Bonfils fibrescope (indirect laryngoscopy) while using a Macintosh or McCoy (direct laryngoscopes) to create the oro-pharyngeal air space required for Bonfils insertion. The other reason was providing a check of direct laryngoscopy.
Table 4 shows the complications in the study group patients (n=26, i.e. 3.2%) during initial airway management. However, not all difficult face mask ventilation cases were documented in this section of the audit form. There were nine cases of failed tracheal intubation on initial attempt (1.3% of the direct laryngoscopy group), which included eight attempts using the Bonfils fibrescope (four of which were performed by a trainee anaesthetist) and one awake FOI.
Complications during initial airway management.
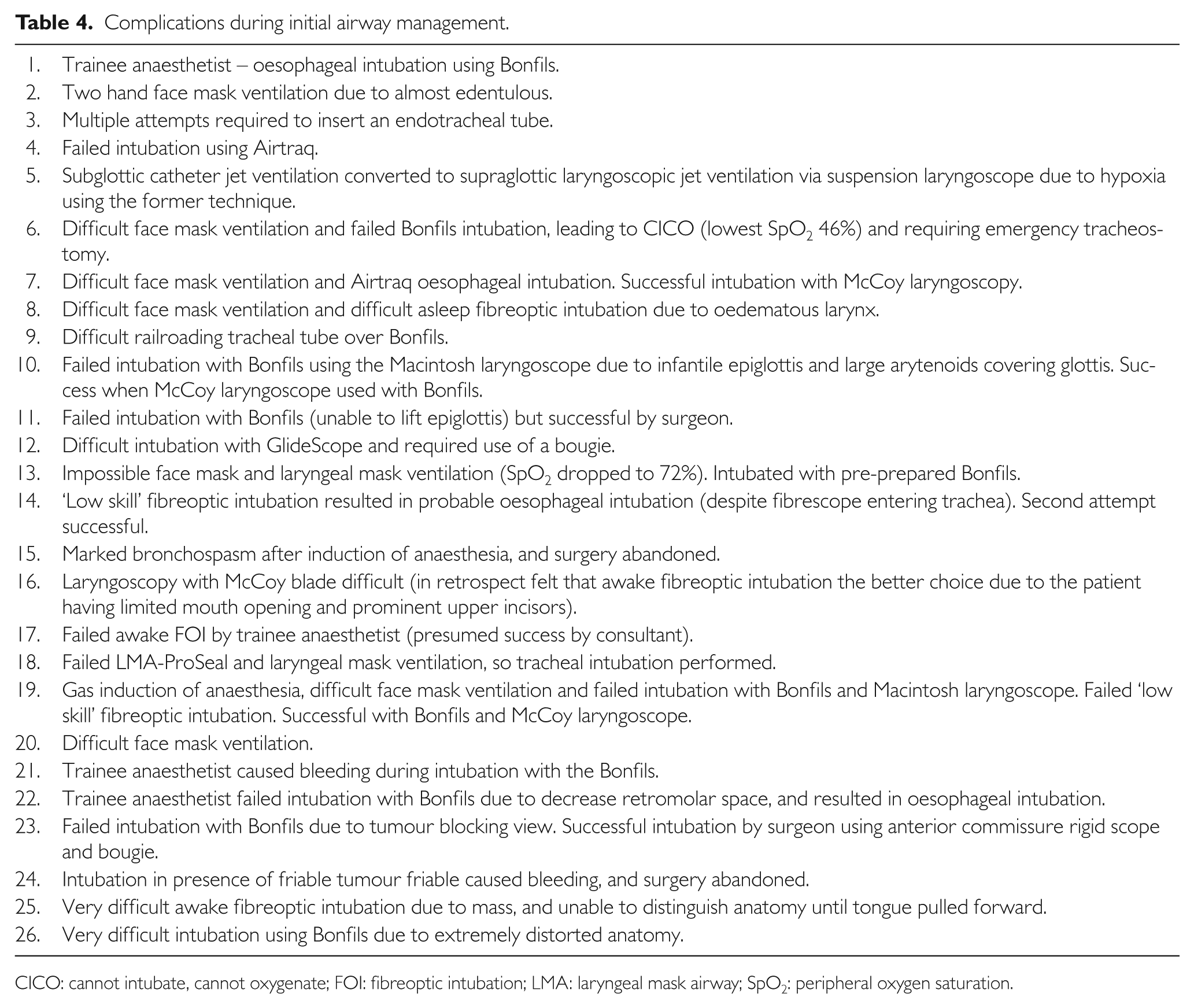
CICO: cannot intubate, cannot oxygenate; FOI: fibreoptic intubation; LMA: laryngeal mask airway; SpO2: peripheral oxygen saturation.
Nineteen patients had their airways secured using awake FOI from the study group (2.3%). From these, there were three complications (15.8%): oversedation with remifentanil causing apnoea and difficulty railroading the tracheal tube over the fibrescope (n=1, 5.3%), difficulty passing through the oral Bermann intubating airway (n=1, 5.3%) and failure by a trainee anaesthetist (n=1, 5.3%).
Face mask ventilation would only have been performed on anaesthetised patients, that is, 794 patients who had an intravenous induction of anaesthesia. All received intermediate acting muscle relaxants to facilitate tracheal intubation except for two who received suxamethonium. There were no data to determine if these two latter patients had a ‘rapid sequence induction’. Face mask ventilation was recorded as difficult and impossible in six (0.8%) and two (0.3%) patients, respectively. In the latter group, one patient with a history of failed intubation had also refused awake FOI. After induction of anaesthesia and failed face mask ventilation, the patient’s peripheral oxygen saturation (SpO2) dropped to 72% and the trachea was immediately intubated using the Bonfils fibrescope (Cormack–Lehane score was 3a). In the second case, attempts at tracheal intubation using the Bonfils fibrescope caused bleeding, resulting in a ‘cannot intubate, cannot oxygenate’ (CICO) scenario with the SpO2 dropping to 46%. The situation was rescued by an emergency tracheostomy.
There were 45 cases (5.5%) of postoperative complications in the study group (some had more than one): coughing (n=31, 3.8%); desaturation (SpO2 <94%) (
Discussion
H&N cases featured prominently in the NAP4 report. 3 Thirty-nine per cent of major airway complications involved H&N surgery and 70% of these were associated with obstructive lesions. Forty-three per cent of emergency surgical airways were performed in H&N patients. In addition, in almost one third of H&N airway complications, airway management was considered poor.
Airway assessment and prediction of difficult airways (face mask ventilation and laryngoscopy grade) for general and obstetric populations are well documented.11,12 This is in contrast with H&N, ENT or maxillofacial surgical populations, whose pathologies (e.g. laryngeal or tongue base tumours, oro-facial infection or trauma) or their subsequent treatment (surgery or radiotherapy to the head and neck) are associated with difficult airways.2,13,14 Predicting the latter is useful as it is associated with increased morbidity and mortality, 4 but it also allows appropriate management to be implemented.
Difficult intubation: predictors and risk factors
The rate of intubation in our H&N population was 91.3%: 90.6% using a tracheal tube and 0.7% via an intubating LMA. This high rate was due to the nature and site of surgery, often resulting in a ‘shared airway’. This contrasts with a 38% rate seen in all general anaesthetics administered in the UK. 3
The incidence of difficult intubation in various study populations ranges from 1.5% to 20.2%, with an overall incidence of 5.8%. 11 One study compared ENT with general surgical patients and found the incidences to be 3.5–15.7% (non-cancer and cancer patients, respectively) and 2.5%, respectively. 2 Our direct laryngoscopy group had a 12.6% incidence of difficult intubation.
Our predictors of difficult intubation in H&N patients yielded poor sensitivity (7–39%), poor PPV (Mallampati score 26%, mandibular luxation score 19% and IDD 53%) but high specificity (84–99%). Although IDD has low predictive value for predicting difficult intubation, it does have one benefit over other tests. It allows the clinician to determine whether the insertion of an oral airway or LMA (to facilitate ventilation) is possible. However, our study showed a low incidence of LMA use (2.5%) in H&N patients (compared with 56% LMA use in the general population). 3
To increase the predictive value of bedside airway tests, multifactorial models have been used to derive composite airway risk index scores or mathematical equations based on logistic regression analysis2,15–18 (although not all have demonstrated an increase in predictive power).11,19 The sensitivity, specificity and PPV have ranged from 5% to 93%, 76% to 99% and 9% to 38%, respectively. Similarly in our study, despite many showing statistical significance (Mallampati score, mandibular luxation, thyromental distance, IDD, history of previous H&N surgery), they all had poor sensitivities (7–39%). Due to the risk of false negatives, appropriate investigations (e.g. flexible nasendoscopy and radiological imaging) to complement bedside airway assessments are essential to manage H&N patients.
We found that having airway symptoms was associated with difficult intubation. Other studies have found that airway symptoms, 2 laryngeal dysfunction or the presence of a supraglottic tumour are associated with difficult intubation. 15 In our study, a total of 31 patients had previous radiotherapy treatment for cancer, of whom 11 (35.5%) were difficult to intubate, which was statistically significant. In a study of mixed ENT and maxillofacial (elective and emergency) surgical patients, 42.5% of patients with previous radiotherapy treatment had a difficult intubation. 14 Radiotherapy causes microvascular and lymphatic changes, tissue fibrosis and oedema, and decreased salivation, and is associated with an increased incidence of trismus (5–38%).20–27 It is therefore associated with and should be seen as a ‘red flag’ for difficult airways. 3 In our study, two patients with a history of radiotherapy had difficulties during their plan A (including the CICO case described above).
Induction of anaesthesia
A total of 97.4% of our patients had intravenous induction of anaesthesia and none had a gas induction (except one who had postoperative tongue swelling and so, as a re-attendee, was not used for statistical analysis). Gas induction is traditionally used in patients with severe airway obstruction. By preserving the patient’s own spontaneous ventilation, it has been considered to decrease the risk of complete airway obstruction following the induction of anaesthesia. 28 However, it has been associated with failed intubation, increased morbidity and the need to perform emergency ‘rescue’ surgical airways.3,29
Intubation techniques
In predicted difficult airway cases, the primary decision for this team is whether to secure the airway using an ‘awake’ technique or an ‘asleep’ technique (using intravenous or volatile induction agents, with or without muscle relaxants).1,28–30 We had 19 (2.3%) cases of awake FOI in the study group. In this group, there were three patients with complications (15.8%). Woodall et al. 31 reported complications that included epistaxis (10%), symptoms of lignocaine toxicity (36%), hypoxia (1.5%), rigors (1%) and lower respiratory tract infection (0.5%). However, flexible FOI may not be suitable in H&N patients as it may cause a ‘cork in a bottle’ obstruction in severely obstructed airways,28,29,32 and has been associated with failures and significant morbidity. 3 Our awake FOI failure rate was 5.3% (one case in 19) and this compares with 1.8–10% in other studies.31,33 Heidegger et al. 33 reported failures due to operator inexperience, being unable to visualise the glottis and associated complications. The latter group included: coughing (including one case leading to cyanosis); severe epistaxis (1.3%); airway passage too narrow and oesophageal intubation.
After the induction of anaesthesia, 1.5–8.5% of general surgical patients have difficult intubation but the failure rate is only 0.13–0.3%. 34 This is because Cormack–Lehane grade 3b and 4 views (very difficult laryngoscopy) are rare, and these require more advanced techniques, for example, indirect laryngoscopy (or, as a last resort, a surgical airway) to secure the airway and maintain ventilation. Our failed intubation rate of 1.3% is similar to other H&N studies (0–2%),2,14,15 and reflects the close working relationship between experienced H&N consultant anaesthetists and surgeons.
The most common method of indirect laryngoscopy was tracheal intubation using the Bonfils fibrescope (n=184, i.e. 22.5% of the study group). There are limited comparative data and evidence of benefit between standard direct laryngoscopy and indirect laryngoscopic techniques in ‘normal’ patients let alone in H&N patients. 35 However, our group of consultant anaesthetists have extensive experience in using the Bonfils fibrescope in difficult airway patients under anaesthesia, and there are increasing data to support its use in difficult airways.35–37 The Bonfils fibrescope has advantages over other forms of indirect laryngoscopy in patients with peri-glottic lesions due to its increased manoeuvrability around these lesions, and its rigid stylet component can push lesions aside and can also act as a guide for tracheal tube rail-roading and subsequent insertion through a distorted peri-glottis.32,38 As far as we are aware, this is the largest reported case series on the use of the Bonfils fibrescope in H&N patients. However, we had eight cases (four by trainees) of failed intubation using the Bonfils fibrescope (out of 184 uses, 4.3% failure rate) and the NAP4 reported one failure. 3
Predicting difficult or impossible face mask ventilation may therefore be life-saving as it may help decide whether to perform an ‘awake intubation’, obviating the need for (and potential failure of) face mask ventilation altogether. Difficult face mask ventilation is also associated with a four-fold and 12-fold increase in difficult and failed intubation, respectively. 39 There are many predictors of difficult face mask ventilation, which include: increased body mass index; history of snoring or sleep apnoea; presence of beard; lack of teeth; age over 55 years; Mallampati III or IV; limited mandibular protrusion; male gender and airway masses. 40 However, only the presence of a beard is easily modifiable. In one study, the most significant predictor for impossible face mask ventilation was neck radiation changes. 41 Our results for difficult and impossible face mask ventilation in H&N patients (0.8% and 0.3%, respectively) are similar to those in the general population (1.4% and 0.15%, respectively). 42 The CICO scenario is very rare in the general population (0.017%), 43 but may be as high as 0.1% in H&N patients. 14 As such, if a difficult airway is considered very high risk, a H&N surgeon must be fully prepared to perform a surgical airway immediately.
Our 5.5% postoperative complication rate is similar to the rate of Asai et al. 44 of 7.4% in general surgical patients, and it highlights that the extubation period is associated with significant adverse events. 3 Almost half of recovery airway complications occur in patients who have undergone oral or ENT surgery and have bleeding into the airway. 3
Limitations
The numbers quoted are based on recorded data available, and this may lead to an underestimation of various parameters due to unrecorded or missing data. In retrospect, the design of our data form could have been improved as some parameters only had tick boxes for the presence of positive findings; for example, difficult face mask ventilation. Therefore, ‘not difficult face mask ventilation’ could either have been a true easy face mask ventilation or a missed data entry, leading to an underestimation of true difficult face mask ventilation. We did not measure the patient’s height, and body mass index may be a more important factor in predicting difficult airways. 11 Limitation of neck movement was a subjective assessment made by the anaesthetist, and intra and inter-individual variation may occur. This study was performed with the observer undertaking both bedside tests and Cormack–Lehane scoring, introducing the potential for observer bias. There was no standardisation of induction and intubating techniques, but this reflected the actual clinical practice among a group of experienced H&N anaesthetists. In some cases, a tracheal tube was in situ before the Cormack–Lehane score was obtained (e.g. FOI or blind nasal intubation). This may underestimate the Cormack–Lehane score as the epiglottis is lifted up by the tracheal tube making visualisation easier. In our statistical analysis we have sought to split the predictors into simple ‘yes’ or ‘no’ values as opposed to their full numeric or categorical ranges. While this may seem a simplistic approach, in our day-to-day practice we feel that this more accurately represents our true evaluation of potential airway challenges.
Conclusions
The incidence of difficult and impossible face mask ventilation in our patient population is similar to that in the general population. The majority of patients had their airway managed under general anaesthesia by intravenous induction. Difficult intubation occurred in 12.6% of patients. Our predictors of difficult intubation yielded poor sensitivities. The rates of failed intubation and airway complications during induction and extubation were low. There was one case of CICO. This study shows that most H&N surgical patients can be managed safely by skilled and experienced H&N anaesthetists and surgeons. It also reminds us that management of high-risk cases may be associated with significant morbidity.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
