Abstract
We report a case of severe emphysema with bullae in a patient who underwent the new technique of bronchoscopic lung volume reduction to the right upper lobe. He was symptomatic with breathlessness and frequent exacerbations. He was not deemed suitable for a surgical lung volume reduction or bullectomy due to a very low forced expiratory volume in one second (FEV1). Endobronchial valves were not considered due to the incomplete fissures. The case was carefully screened, and was discussed in a multidisciplinary meeting prior to the final decision. This was the first case in Malaysia of bronchoscopic thermal vapour ablation (BTVA) for severe advanced emphysema. Multiple experts were involved prior, during and after the procedure. Despite having a poor lung reserve, he came through the procedure successfully with no immediate complications. His serial spirometry showed a 50% improvement at six months compared to baseline. This case highlights the important role of a multidisciplinary meeting, expert opinion and the careful selection of which patients should undergo BTVA. The procedure should be carried out at a centre of excellence in order to achieve a successful procedure.
Keywords
Introduction
Patients with advanced chronic obstructive pulmonary disease (COPD) typically present with breathlessness, acute exacerbations or both. They can have mild to severe dyspnoea as the disease progresses or when lung function declines. This results in a poor quality of life. The patient can have frequent exacerbations due to the low forced expiratory volume in one second (FEV1), and exacerbations also further decline the FEV1. An increase in breathing effort is caused by airflow limitation and air trapping. Lung emphysema and hyperinflation is due to the ongoing chronic inflammatory processes and bronchoconstriction. This is the pathophysiology of airway remodelling. Advanced COPD patients usually receive inhalers, vaccinations, active pulmonary rehabilitations or oxygen, and some are on domiciliary ventilatory support. However, it is notable that pharmacological agents do not work on the dynamic hyperinflation of the lungs. Hence, lung volume reduction surgery (LVRS) is an option for emphysematous patients in order to provide effective symptomatic relief. However, due to the underlying pathology, not everyone is deemed fit to undergo for surgery in view of poor lung function and co-morbidities. Currently, there are a number of modalities of lung reduction via the bronchoscopic technique. We report the case and outcome of an advanced severe emphysema patient who underwent a bronchoscopic lung volume reduction (BLVR).
Case description
Here, we describe the first case of bronchoscopic thermal vapour ablation (BTVA) performed in Malaysia in order to illustrate a successful procedure in a carefully selected patient – a 71-year-old gentleman with underlying hypertension and COPD on maximal triple inhalation therapies together with oral theophylline. He was referred from another tertiary centre for bronchoscopic management of advanced COPD. He was still having exertional dyspnoea on minimal exertion, despite being on these pharmacological agents. His Modified Medical Research Council Dyspnea Scale score was 3, with an annual history of multiple COPD exacerbations which were non-infective in origin. He was compliant with all of his medications and inhalers. His inhaler technique was correct, and he was using a soft mist inhaler (SMI; Spiolto Respimet®) daily, a pressured metered dose inhaler (pMI; beclomethasone) twice daily and salbutamol for rescue. His vaccination records for influenza and pneumococcal were up to date. All of his COPD exacerbations in the previous year were most likely due to multiple dynamic hyperinflations. His serum eosinophil count was on the border of 150×100 cells. There was no positive culture growth on either sputum or blood during multiple episodes of admissions.
His high-resolution computed tomography (HRCT) scan of the thorax (Figure 1) showed heterogeneous emphysema and hyperinflation of the lung fields, with mosaic attenuation suggestive of air trapping. Incomplete fissures were seen. The worst emphysema was at the right upper lobe.

(a)–(d) High-resolution computed tomography (HRCT) scan of the thorax of our patient, showing bilateral paraseptal and centrilobular heterogenous emphysema which is worst on the right upper lobe, with the presence of bullae and also mosaic attentuation suggestive of air trapping. The fissure was incomplete.
The case was discussed in a multidisciplinary team meeting with thoracic radiologists, cardiothoracic surgeons and interventional pulmonologists. He was deemed high risk for LVRS due to poor baseline lung-function tests. Endobronchial valve (EBV) therapy was not feasible due to the incomplete fissures. It was decided he should undergo BTVA, targeting the right upper lobe.
The case was carefully planned, and proper counselling was given to the patient and his caregivers. He had no exacerbation of his condition during his elective admission for the procedure. The BTVA was carried out under general anaesthesia using rigid bronchoscopy in the operation theatre (Figure 2). The procedure was done in a controlled environment, as the airway and ventilation were looked after by an experienced anaesthesiologist. As this was the first BTVA to be performed in Malaysia, we conducted the procedure together with BTVA experts from the People’s Republic of China.
There were no adverse events during and immediately after the bronchoscopic intervention. The patient was observed in the critical care unit for a day post extubation and subsequently was transferred to the general ward for a few days. He was prescribed a prophylactic intravenous (i.v.) antibiotic with i.v. cefuroxime for five days. The chest radiograph taken few hours post extubation showed significant improvement and lung volume reduction on the right upper lobe (Figure 3). He was discharged well with a given appointment for our post-procedure clinic follow-up.
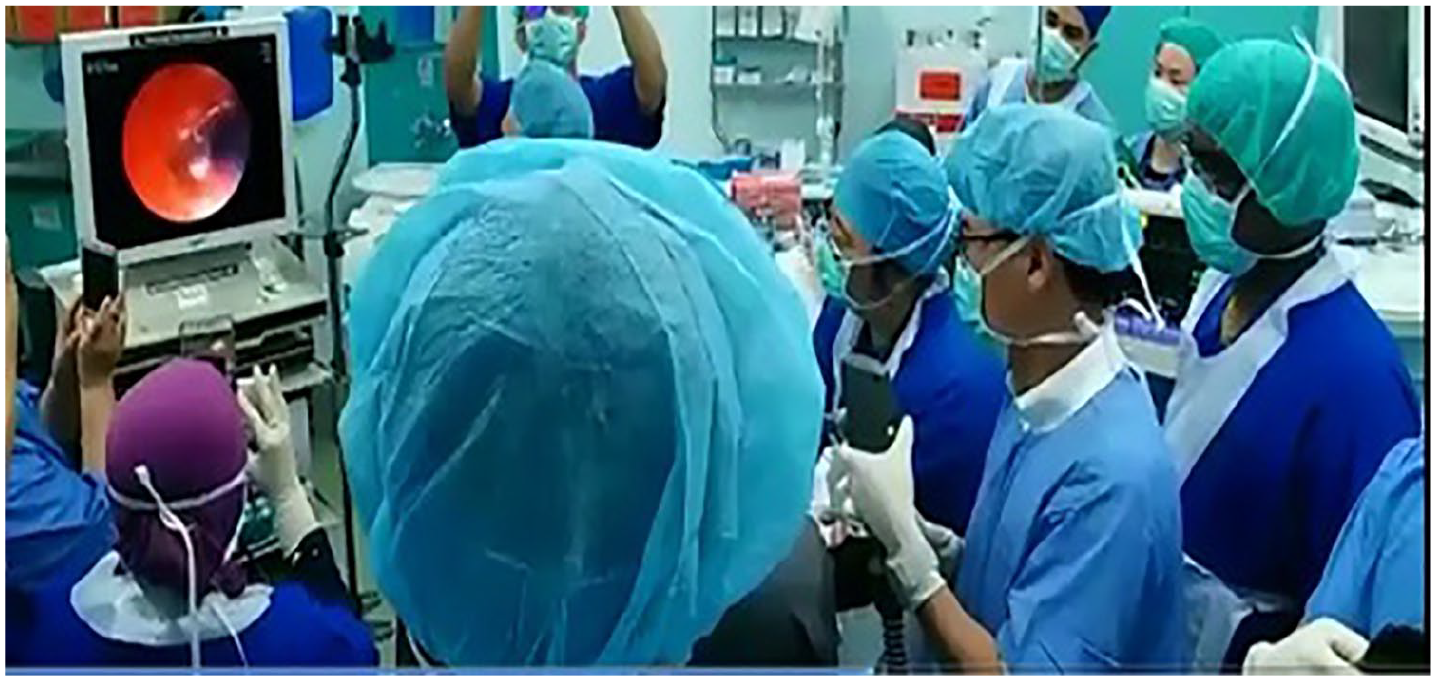
First Malaysian experience of bronchoscopic thermal vapour ablation (BTVA) under general anaesthesia and rigid bronchoscopy. The thermal vapour was delivered to the right upper lobe where the worse emphysema was seen on the HRCT of the thorax.

Chest radiographs before (a) and after (b) BTVA show a reduction in right upper-lobe volumes.
He was well during the follow-up with a reduced frequency of serious COPD exacerbations. He had had no hospital admissions due to breathlessness since the BTVA. His pulmonary physiology indices are shown in Table 1 pre and post BTVA. At six months, his FEV1 improved by almost 50% from baseline. This was also translated in terms of his exercise capacity, being able to walk from previously being wheelchair bound. The latter was a crude assessment because the patient had no baseline Six-Minute Walk Test (6MWT) due to severe breathlessness. He will have a 6MWT and repeat total lung capacity (TLC) and residual volume (RV) tests in due course. The 6MWT has not yet been done due to physical deconditioning, and he is still undergoing extensive pulmonary rehabilitation to improve muscle bulk and exercise tolerance. St George’s Respiratory Questionnaire (SGRQ) showed an improvement from 88 points before the procedure to 60 points at six months following the procedure.
Pre- and post- BTVA lung physiology indices.
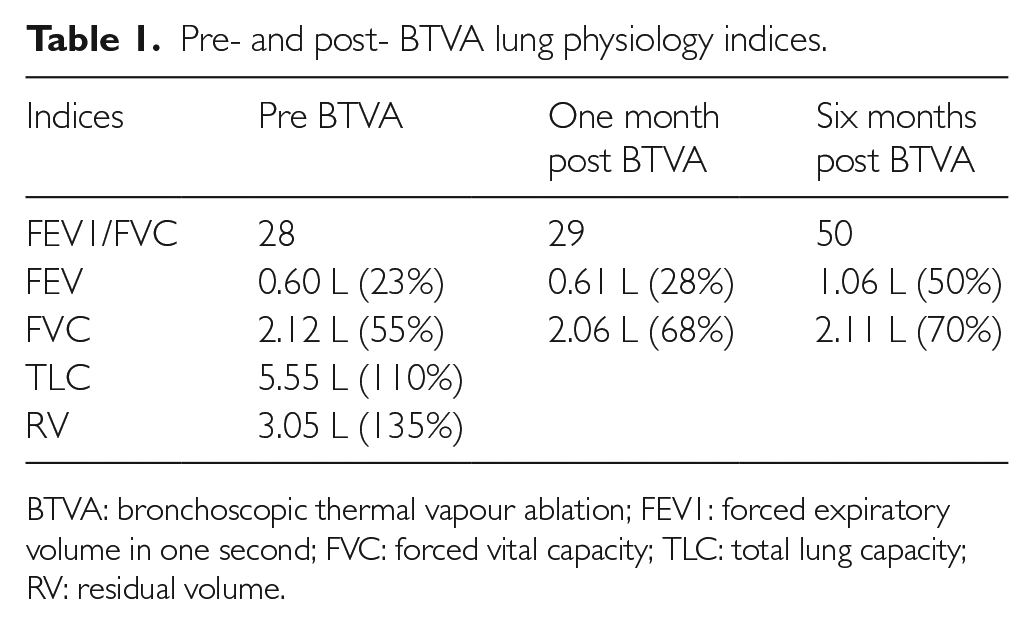
BTVA: bronchoscopic thermal vapour ablation; FEV1: forced expiratory volume in one second; FVC: forced vital capacity; TLC: total lung capacity; RV: residual volume.
Discussion
BLVR serves as an additional therapeutic option, and when applied to appropriately selected patients, it improves physical performance and lung functions. There are a few different BLVR options, including EBV (Zephyr®), coils, targeted lung denervation and airway bypass stent. 1
Currently in Malaysia, BLVR using valves had been adopted before the very first BVTA was carried out on this patient. This case illustrates that despite the modern advancing technique of BLVR, wise clinical judgement and the correct patient selection ultimately determine the success of the lung volume reduction procedure. This will reflect the patient’s improvement in terms of physiological lung function as well as exercise tolerance and capacity. 2
Objectively, these are measured using the full pulmonary function test compared to before and six months after the procedure, together with the 6MWT. The improvement in FEV1 as well as reductions in the TLC and RV are usually seen and define success. The aims of a successful procedure include few immediate procedural-related complications as well as long-term clinical improvement.
Generally, there can be multiple potentially serious and fatal complications, including pneumothorax and pneumonia, both of which may lead to respiratory failure and mechanical ventilation without early intervention. An exacerbation of COPD may also occur after BLVR. All of these complications may be avoided with careful selection of patients to undergo BLVR and a high index of suspicion for certain possible conditions if the patient deteriorates after or during the procedure. In BTVA, more common complication is severe pneumonia which may be associated with an enhanced local inflammatory response.
Theoretically, a more severe local inflammatory response corresponds to the lung volumes treated and also the effectiveness of the BTVA. 3 Therefore, it is a contraindication to do BTVA in a multiple infective exacerbated patient.
Lung volumes with emphysematous segments are reduced by the local inflammatory reaction from the instillation of heated water vapour. This results in fibrosis and scarring after approximately two to three months, and subsequently the patient can achieve the desired lung-volume reduction. 4
This technique has no implants left in situ compared to coils, valves or glue. Furthermore, the instillation of heated water vapour to targeted segments with emphysema can target the appropriate lung segments. 5 Hence, BTVA has the capacity to treat intra-lobar heterogeneous emphysema.
The criteria for pulmonary physiological tests must be fulfilled before subjecting patients with advanced emphysema to BLVR. The prerequisite are for FEV1 <45%, RV of at least >150%, preferably >200% and TLC >100% for the procedure to be a success. 5 However, in our patient, although the TLC was >100%, the RV was slightly lower than the approved criteria. Despite that, correlating the elevated RV and the HRCT, we concluded that this patient had a significant degree of air trapping which may benefit from BTVA.
To date, BTVA has been approved for the treatment of the upper lobes. There are ongoing trials for the middle or lower lobes using BTVA which may be approved in the future. There are fewer published BTVA studies compared with those using coils and EBVs. The positive outcome for this patient has led to a promising new technique that can be done in Malaysia. It is prudent to note that the treatment is expensive and can be burdening to the health-care system. Therefore, it should be done in a highly specialised centre to ensure successful outcomes. In conclusion, this is an illustration of a successful BTVA. Patients who have upper-lobe predominant emphysema and are not suitable for EBV therapy due to incomplete fissures may be offered this procedure in a centre of excellence with extensive expertise.
Footnotes
Acknowledgements
We thank Dr L.Y.F. who referred this case from a tertiary hospital.
Authors’ contributions
R.I., M.Z.N. and J.A. managed the patient. J.A. and N.M. prepared the manuscript. N.M. edited and approved the final draft.
Availability of data and materials
Data sharing is not applicable to this article, as no data sets were generated or analysed during the current study.
Ethical approval
Ethical approval was not sought for the present case report because it is not required as per university guideline. This study was completed in accordance with the Declaration of Helsinki.
Informed consent
Written informed consent was obtained from legally authorised representatives before the study.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
