Abstract
Background:
Videolaryngoscopes have become increasingly popular in recent years for use in both normal and difficult airways. Despite this trend, their benefit remains controversial. The McGrath® MAC videolaryngoscope (Aircraft Medical Ltd, Edinburgh, UK) is used for first line or rescue intubation, and for training in videolaryngoscopy intubation. We conducted a prospective observational study to assess the performance of the McGrath® MAC.
Methods:
We evaluated the use of the McGrath® MAC videolaryngoscope from January 2016 to April 2016. We recruited 500 adult patients undergoing elective surgery requiring endotracheal intubation. Data was collected via an online survey. The primary outcome was the success of intubation with the McGrath® MAC. Secondary outcomes included the ease of the McGrath® MAC insertion, best glottic view, ease of tracheal tube insertion, number of intubation attempts, evidence of airway trauma, quality of view, adjunct used, airway manoeuvres used, quality of image on monitor screen and overall impression of the device.
Results:
A total of 428 responses were analysed. The overall success rate was 97.9% (95% confidence interval 96.0–99.0%). The success rate for those with predictors of difficult airway was 95.5% (95% confidence interval 87.6–99.5%). Easy scope insertion was reported by 97.2% of anaesthetists and 89.7% reported easy tube insertion. Some of our cases (1.9%) were complicated by airway trauma involving superficial oropharyngeal or lip injury.
Conclusion:
The McGrath® MAC videolaryngoscope is a good choice for a videolaryngoscope, conferring advantages of a high intubation success rate, ease of laryngoscope insertion and ease of intubation. It is suitable for use in predicted difficult airways.
Introduction
The primary goal of airway management is to provide and maintain oxygenation. This may involve the use of pre-oxygenation, apnoeic high flow oxygen insufflation, face mask ventilation, supraglottic airway device ventilation, tracheal intubation and invasive ‘front of neck access’. Failure to provide oxygenation is associated with severe morbidity and mortality. 1
Tracheal intubation using direct laryngoscopy relies on alignment of the oral, pharyngeal and laryngeal axes. The most common direct laryngoscopy device is the Macintosh laryngoscope. In comparison, indirect laryngoscopy allows the operator to ‘see around the corner’ without relying on the same degree of the aforementioned alignment.
Modern videolaryngoscopy devices were introduced into clinical practice in the 1990s, and are now commonly available. They are used as first line or as airway rescue techniques and can be used for normal, predicted or known difficult airways. They are primarily used for oral tracheal intubation but may be used to guide nasal tracheal intubation. The video monitor provides a shared view which facilitates teaching and training in using the videolaryngoscopy device, and allows a ‘digital airway footprint’ to be made for clinical and medico-legal purposes. In spite of the rise in popularity of videolaryngoscopes, their benefit in airway management remains unclear. 2 The American Society of Anesthesiologists (ASA) difficult algorithm leaves the use of videolaryngoscopy devices at the discretion of the anaesthetist. 3 For the anticipated difficult airway, one should ‘consider the relative merits and feasibility [of videolaryngoscopy devices] as an initial approach to intubation’. 3 For the unanticipated difficult airway, numerous alternative difficult intubation approaches are described (including the use of videolaryngoscopy devices) but again there are no specific recommendations for videolaryngoscopy device use. 3 Likewise, the Difficult Airway Society guidelines for the unanticipated difficult airway state that ‘all anaesthetists should be trained to use, and have immediate access to, a videolaryngoscope’ but they do not specifically recommend when and where in their algorithm to use videolaryngoscopy devices. 4 The use of videolaryngoscopy therefore depends on ‘good clinical judgement’. 4 Some authors have recommended videolaryngoscope as first line device for normal and difficult airways. 5
We aimed to assess the performance of the McGrath® MAC videolaryngoscope (MMVL) and audit current practice by the anaesthetists (novices and specialists) in our department.
Methods
Study participants
This prospective observational study was conducted from January 2016 to April 2016, and involved all anaesthetists in a large tertiary hospital in Singapore. Participation by the individual anaesthetists was voluntary and included both specialists and novices. We identified all adult patients undergoing elective surgery requiring endotracheal intubation. The only exclusion criterion was age below 21 years; however, participation in the study was subject to the discretion of the consultant anaesthetist. Waiver of patient consent was obtained from the Centralized Institutional Review Board (CIRB Ref 2016/2547). We recruited 500 adult patients undergoing elective surgery requiring endotracheal intubation. Upon successful recruitment, the videolaryngoscope and disposable laryngoscope blade would then be issued to the anaesthetist for use. The size of the blade was chosen by the anaesthetist for individual patients. Patients were intubated based on the view seen on the videolaryngoscopic monitor.
Outcome
The primary outcome was the rate of successful intubation using the MMVL. Secondary outcomes included the ease of videolaryngoscope insertion, best glottic view, ease of tracheal tube insertion, number of intubation attempts, evidence of airway trauma (no definition was given and the method of filling the survey comment box was left to the discretion of the attending anaesthetist), quality of view, adjunct used, airway manoeuvres used, quality of image on monitor screen, and overall impression of the device.
Data collection
Data was collected via an online survey form. This included: the anaesthetist’s experience and previous use of the MMVL; patient’s characteristics (age, gender, ASA grade, weight and height, and features predictive of a difficult airway); anaesthetic technique (induction agent and muscle relaxant used); and evaluation of MMVL performance with regard to the primary and secondary outcomes of the study. With the exceptions of age, height and weight, options in the online form were given in multiple choice format. Free text was allowed for additional comments and descriptions.
The patients’ airways were examined by the attending anaesthetists. Predictors of difficult airway were described by the anaesthetists on the online survey. The best videolaryngoscope view of the glottis obtained was based on the Cormack–Lehane score: 1 – whole vocal cords seen; 2 – partial vocal cords or arytenoids only seen; 3 – epiglottis seen; and, 4 – no epiglottis seen. 6 The ease of videolaryngoscope insertion and ease of tracheal tube inserted was subjectively assessed to be either easy or difficult.
Statistical analysis
Statistical analysis was performed using IBM SPSS Statistics version 21. Nominal data is represented as n (%) together with the confidence interval in the tables. Fisher’s exact test was used.
Results
We achieved a response rate of 93.6% (468 responses out of 500 recruited patients). Patients were excluded from the study if they were subsequently found to be below 21 years of age or if the anaesthetist decided after recruitment not to use the MMVL. Missing data led to exclusion of that response from the final analysis. A total of 428 responses were finally analysed (Figure 1).

Study flowchart.
Baseline characteristics (Table 1)
The mean age was 54.1 years, and 48.6% were male. The majority of patients belonged to ASA II and III classification of physical status (52.1% and 29.2% respectively). The mean body mass index was 25.7 and 15.7% of the patients had predictors of a difficult airway. These predictors included: restricted mouth opening, receding chin, short thyromental distance, protruding upper teeth, Mallampati grades III and IV, history of difficult airway and various airway pathologies considered to make laryngoscopy difficult.
Baseline patient and anaesthetist characteristics.

Patients analysed = 406; 22 had missing data on height/weight.
Predictors included restricted mouth opening, receding chin, short thyromental distance, protruding upper teeth, Mallampati grades III and IV, history of difficult airway and various airway pathologies considered to make laryngoscopy difficult.
CI: confidence interval; ASA: American Society of Anesthesiologists physical status classification system; BMI: body mass index; MMVL: McGrath® MAC videolaryngoscope.
Intubation success rate (Table 2)
The overall success rate of tracheal intubation was 97.9% with nine cases of failed intubation. The success rate for those with predictors of a difficult airway was 95.5% (64/67). The number of patients with Cormack–Lehane grade 1, 2, 3, 4 using the MMVL were 297 (69.6%), 118 (27.6%), 11 (2.6%) and one (0.2%), respectively.
Intubation success rate, presented as number, percentage and 95% confidence interval.

Predictors included restricted mouth opening, receding chin, short thyromental distance, protruding upper teeth, Mallampati grades III and IV, history of difficult airway and various airway pathologies considered to make laryngoscopy difficult.
Videolaryngoscope screen blacked out, and direct laryngoscopy performed using the McGrath® MAC videolaryngoscope (patient successfully intubated).
CI: confidence interval; MMVL: McGrath® MAC videolaryngoscope; BMI: body mass index.
Ease of scope and endotracheal tube insertion (Table 3)
Easy scope insertion was reported by 97.2% of anaesthetists and 89.7% reported easy tube insertion. Eight cases (1.9%) were complicated by airway trauma: mild pharyngeal trauma (n=1), lip laceration (n=1), superficial abrasions but location not specified (n=1), bleeding from the nasopharynx (n=1), and trauma that was unspecified (n=4). All cases of airway trauma occurred with concomitant use of an intubating adjunct.
Secondary outcomes: ease of scope and tube insertion as well as airway trauma, presented as number, (percentage) and [95% confidence interval].

MMVL: McGrath® MAC videolaryngoscope; BMI: body mass index.
Predictors included restricted mouth opening, receding chin, short thyromental distance, protruding upper teeth, Mallampati grades III and IV, history of difficult airway and various airway pathologies considered to make laryngoscopy difficult.
Grade 4 view hence intubation not attempted with McGrath® MAC videolaryngoscope.
Use of airway adjuncts and manoeuvres (Table 4)
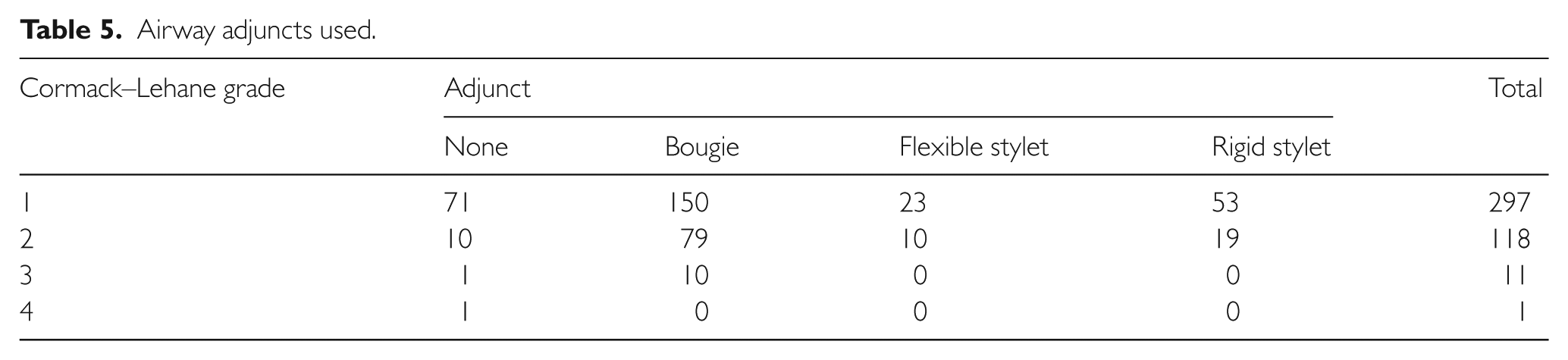
Intubating adjuncts that were used to facilitate intubation during videolaryngoscopy included the bougie, and rigid and flexible stylet. They were used 80.6% of the time. Airway manoeuvres including jaw thrust and external laryngeal pressure were used in 41.4% of patients. The Cormack–Lehane grade and the use of intubating adjuncts are given in Table 5.
Adjuncts and manoeuvres used, and quality of view and image.

Double counted for patients with more than one manoeuvre.
Troop mattress, forceps, combination with fibreoptic bronchoscope.
Image not obtained in one patient due to screen failure.
Due to fogging, secretions, blood.
Image not obtained in one patient due to screen failure; missing data in two patients.
Airway adjuncts used.
Quality of the image on the MMVL monitor and quality of view (Table 4)
The quality of the image on the MMVL monitor was considered as either ‘good’ or ‘satisfactory’ by 99.5% of anaesthetists; 94.4% rated the quality of view as ‘clear’.
Failed intubations (Table 6)
There were nine cases of failed intubation. Failures included those due to airway obstruction (n=2), failed laryngoscopy (n=3) and failed tube insertion (n=2). Most had predictors of difficult intubation such as prominent upper teeth, decreased neck movement and previous radiotherapy to the head and neck.
Reasons for failed intubation using the McGrath® videolaryngoscope.

‘Grade’ refers to laryngeal grade view as per Cormack–Lehane’s classification. 2
LMA: laryngeal mask airway; MMVL: McGrath® MAC videolaryngoscope; NPC: nasopharyngeal cancer.
Discussion
Though the Macintosh laryngoscope remains the default airway tool used in endotracheal intubation, videolaryngoscopes have become increasingly popular in recent years for use in both normal and difficult airways.
Our study showed positive results in both primary and secondary outcomes. The overall success rate was 97.9% in all patients and 95.5% in patients with predictors of difficult airways. This is comparable to other studies: 98–100% success rate in normal patients (MMVL); 7 100% in direct laryngoscopy simulated difficult airway patients (MMVL); 8 and in 95% of patients after failed direct intubation. 9 These high rates are because videolaryngoscopy facilitates tracheal intubation by improving the glottic view.
Videolaryngoscopy devices can be divided into two main types: blade (unchannelled) and channelled devices. The blade devices, in turn, may have a relatively gentle curve (similar to the Macintosh laryngoscope, e.g. MMVL) or have a hyper-acute curve to enhance its ability to ‘look around the corner’ (and so termed ‘difficult airway blades’), for example, C-MAC D-Blade (Karl Storz, Tuttlingen, Germany) or McGrath® X BladeTM (Aircraft Medical Ltd, Edinburgh, UK). The channelled devices have an integrated channel and so, unlike the blade devices, guide the tracheal tube to the glottis as visualized on its monitor, for example, AirtraqTM (Prodol Meditec S. A., Vizcaya, Spain). However, the integrated channel makes them more bulky to insert and less able to re-position once inside the oral cavity.
When using videolaryngoscopy devices, an easy view of the glottis does not equate to easy intubation and may still result in failed intubation.9,10 Although videolaryngoscopy devices do not require alignment of the oro-pharyngo-laryngeal axes, this may confer a disadvantage for the anaesthetist, who now has to attempt passing a (mildly curved) tracheal tube along an acutely angled pathway to the glottis. To overcome these difficulties, intubating adjuncts (bougie or stylet) and external laryngeal manipulation are required. Intubation adjuncts were used in the majority of our patients (80.6%). Most (97.2%, n=415) of our patients had Cormack–Lehane grade 1 or 2 views. Despite 91.8% of these cases being subsequently graded as easy tube insertions, intubating aids were used in 80.4% of cases. In contrast, 2.8% (n=12) had grade 3 or 4 views, of which only 16.7% were considered easy tube insertions. A ‘difficult’ view of the glottis is associated with difficult tube insertion or intubation for both direct and videolaryngoscopy.
Videolaryngoscopy is also associated with longer intubation times. Although we did not measure this outcome, other studies have shown that, when comparing the MMVL with the Macintosh laryngoscope, intubation time is 17 s longer in unselected patients by first year trainees 2 and 14 s longer in patients with simulated difficult airway. 8
Other videolaryngoscopy devices are still bulkier than the Macintosh laryngoscope and most require at least 2–2.5 cm inter-dental distance for oral insertion. With its relatively slim blade profile, the MMVL may be easier to use compared with the bulkier channelled counterparts. In our study, anaesthetists reported easy videolaryngoscopy device and tracheal tube insertion in 97.2% and 89.7% of cases, respectively.
In difficult airways, videolaryngoscopes may indeed confer a significant benefit. Direct laryngoscopy may be associated with up to a 25% first-attempt failure rate in patients with cervical spine immobilization. 11 This is significantly reduced to 10% with the use of alternative intubation devices. The McGrath was found to have a 98% intubation success rate on the first attempt, the highest among six videolaryngoscopes compared in a randomized controlled trial. 12
Difficult intubation occurs in about 5% of unselected patients, and is unanticipated in 58–91% of cases.13,14 For the management of the unanticipated difficult airway, plan A of the Difficult Airway Society guidelines includes the use of videolaryngoscopy devices. 4 The guidelines also state that ‘all anaesthetists should be trained to use, and have immediate access’ to videolaryngoscopy devices. We discuss our results in relation to available evidence in other studies using the MMVL. In our study, patients were selected at the discretion of the attending anaesthetist, and this may explain the high prevalence of patients with predictors of difficult airway (15.7%) as anaesthetists might be more keen to use a videolaryngoscope in such patients. Despite the high prevalence of predicted difficult airway, there was a high success rate of intubation. This may be partly explained by the fact that not all these patients with predictors end up being difficult to intubate as airway tests have low to moderate predictive value, with positive predictive values as low as 4.4%. 14 We also acknowledge that selection bias may have contributed to the high success rates found in our study.
We had a low rate of trauma (1.9%) although in half of these cases the nature of the trauma was unspecified. Risk factors for airway trauma are bulkier devices, looking at the monitor instead of the oral cavity during the initial stages of intubation, use of adjuncts, and the presence of a ‘blind spot’. The latter occurs when the tracheal tube is passed beyond the line-of-sight and ‘around the corner’, but before coming into view camera at the distal part of the laryngoscope blade. In our study, we observed that all incidences of airway trauma occurred in cases in which intubation adjuncts were used, but this failed to reach statistical significance (p=0.36). Reported cases of trauma using the McGrath videolaryngoscope include minor oro-pharyngeal injuries8,9,15 and palatal perforation. 16
Our results showed similarly high rates of successful intubation irrespective of anaesthetist seniority or prior number of MMVL uses. This may be due to help from the supervising consultant made easier by the shared view afforded by the MMVL monitor. It allows teaching and correction of laryngoscopic technique, and coordinated assistance with external laryngeal pressure to obtain the best glottic view. While the Macintosh laryngoscope requires 50 attempts to achieve proficiency in its use,17,18 from our study, the MMVL appears easy to learn even by anaesthetists with little or no experience with using the MMVL. There were high success rates in those who had 1–4, 5–20 and >20 prior MMVL uses (96.5%, 98.0% and 99.0%, respectively).
In our study, there was only one report of technical difficulty where there was a loss of screen image; the preserved tip light allowed successful intubation by using the MMVL as a direct laryngoscope.
In view of the high success rate and low risk, it is reasonable for anaesthetists to familiarize themselves with the use of the MMVL in patients with normal airways. Once comfortable with the use of the scope, a better success rate can then be achieved in difficult airways.
Though the MMVL is largely safe to use, it is important to recognize that its use is not completely without risk. In our study, all novice users were under the direct supervision of a consultant anaesthetist. Inexperienced users should still be wary of potential pitfalls in the use of the MMVL. As with any piece of airway equipment, appropriate care should be taken to avoid airway trauma and alternative airway plans should be immediately available in case of intubation failure.
Strengths and limitations
To our knowledge, this is the first study that has evaluated the McGrath® MAC in such a large sample of patients. It is also the first time a study has demonstrated a high success rate irrespective of seniority and prior experience.
However, several limitations exist. First, there is a potential for selection bias in our study. Participation in the study was voluntary on the part of the attending anaesthetists and the response rate was only 93.6%. There was no obligation to use the MMVL. This reflects true clinical practice when new devices are used, and also allows the anaesthetist to decide whether to use the MMVL either as a first line or as a rescue device. Some anaesthetists use the MMVL as a first line whether or not the airway is anticipated as difficult, but this reflects personal preference.
Second, as our study is based on a survey with subjective outcome measures, self-reporting and recall bias may have affected the intubation success rates. Third, error may also have occurred during the process of filling in the survey form, leading to exclusion of 11 patients from our data analysis. Lastly, the study was conducted in a single centre, and may not be readily applicable to all populations.
Conclusion
The MMVL is associated with a high intubation success rate, easy laryngoscope insertion and easy intubation when used for adult patients in an elective setting. It carries a low risk of airway trauma and is suitable for use in patients with both normal and predicted difficult airways, irrespective of anaesthetic seniority or prior experience. However, this survey was based on our departmental practice that all novices are directly supervised. Novices should be appropriately supervised when performing techniques for the first time until competent to do so without supervision.
Footnotes
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
