Abstract
Background
Internet adoption during the past decade has provided opportunities for innovation in advanced cardiac life support (ACLS) training. With pressure on budgets across health care systems, there is a need for more cost-effective solutions. Recently, traditional ACLS training has evolved from passive to active learning technologies. The objective of this study is to compare the cost, cost-savings and return on investment (ROI) of blended ACLS (B-ACLS) and face-to-face ACLS (F-ACLS) in Singapore.
Methods:
B-ACLS and F-ACLS courses are offered in two training institutes in Singapore. Direct and indirect costs of training were obtained from one of the training providers. ROI was computed using cost-savings over total cost if B-ACLS was used instead of F-ACLS.
Results:
The estimated annual cost to conduct B-ACLS and F-ACLS were S$43,467 and S$72,793, respectively. Discounted total cost of training over the life of the course (five years) was S$107,960 for B-ACLS and S$280,162 for F-ACLS. Annual productivity loss cost account for 52% and 23% of the costs among the F-ACLS and B-ACLS, respectively. B-ACLS yielded a 160% return on the money invested. There would be 61% savings over the life of the course if B-ACLS were to be used instead of F-ACLS.
Conclusion:
The B-ACLS course provides significant cost-savings to the provider and a positive ROI. B-ACLS should be more widely adopted as the preferred mode of ACLS training. As a start, physicians looking for reaccreditation of the ACLS training should be encouraged to take B-ACLS instead of F-ACLS.
Keywords
Introduction
Competency in advanced cardiac life support (ACLS) is a core component of many undergraduate1,2 and postgraduate medical curricula.3,4 Each year, more than 1.5 million medical professionals around the world attend advanced resuscitation courses. With pressure on budgets across health care systems,5–7 there is a constant search for a more cost-effective alternative for training.
The growing adoption of the internet has revolutionized the delivery of health care education. 8 Traditional ACLS (face-to-face (F)-ACLS) training has evolved from passive (classroom learning) to active learning technologies such as eLearning, blended learning and simulation. 9 F-ACLS is a 12-hour course offered by hospitals and private training providers to train physicians; 10 it consists both of didactic (face-to-face) and case-based discussion in an interactive learning environment. The course covers the following topics: advanced airway management, recognition of cardiac arrest rhythms and arrhythmias, management of medical emergencies—respiratory arrest, witnessed ventricular fibrillation, persistent ventricular tachycardia, pulseless electrical activity, asystole, bradycardia, acute coronary syndromes, and pharmacology of commonly utilized cardiovascular drugs and their administration. Upon successful completion of the theory and practical assessment, the participant is awarded an ACLS certificate, which is valid for two years.
Alternatives to the traditional model such as DVD11,12 or electronic learning (eLearning) and blended learning solutions 13 have proven to be effective alternatives for ACLS training.14–17 Blended ACLS (B-ACLS) 10 offered to physicians is conducted in three parts (Figure 1). Part 1 is offered online in which the participant learns through interactive lessons, video presentations and progressively staged quizzes. Participants have 24/7 access to the online lessons and materials, and are given up to 60 days to complete Part 1 online. They need to complete the Part 1 theory test before they can proceed to Parts 2 and 3 (five hours). In Part 2, participants have hands-on practice on the various clinical scenarios, such as cardiac arrest, bradycardia and shock under the guidance of ACLS instructors. Part 3 is the practical assessment.
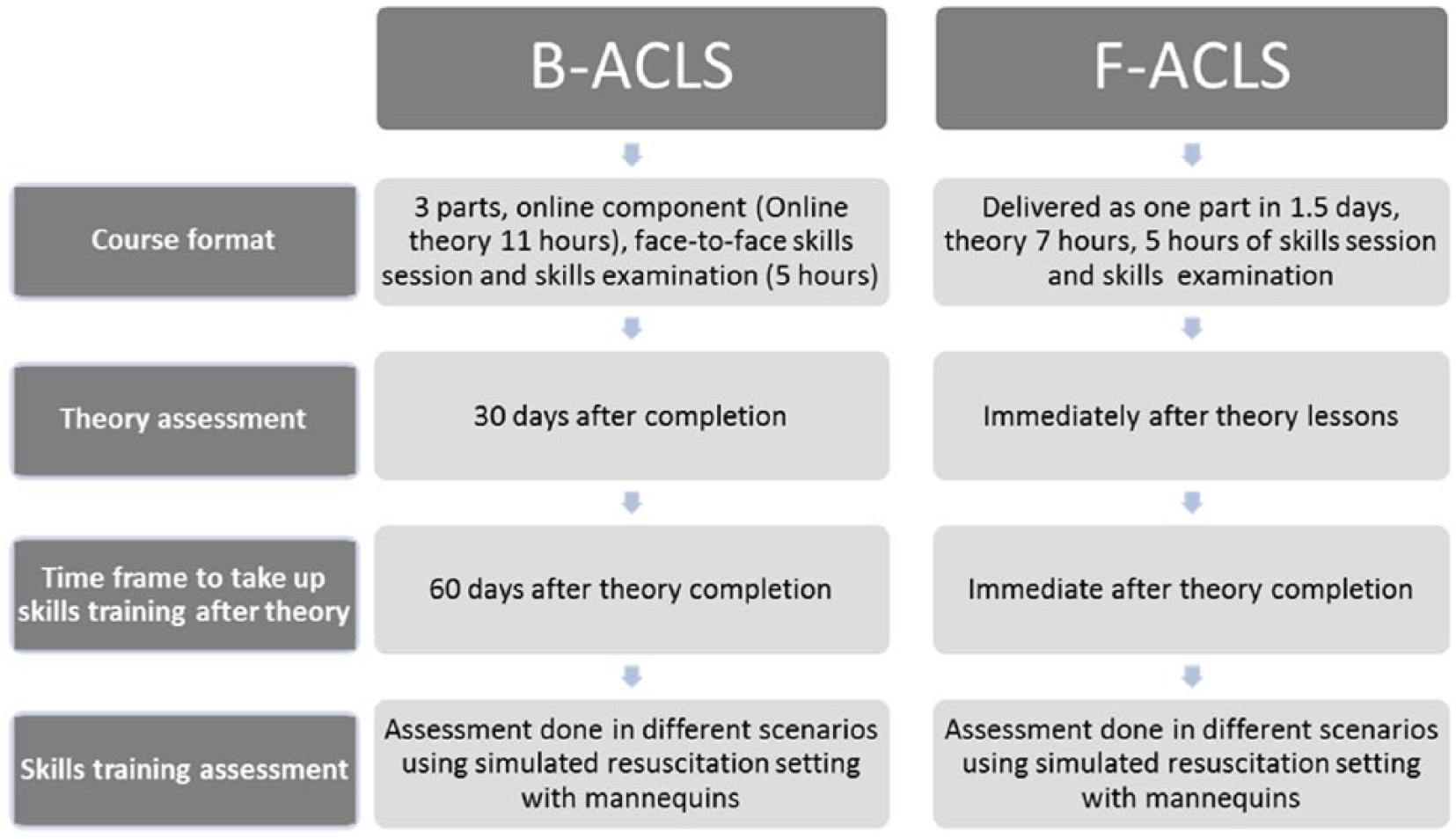
Course characteristics for B-ACLS and F-ACLS training.
Although studies18–20 have shown favorable results with B-ACLS training, there is a dearth of studies assessing its cost and return on investment (ROI). This study compared the cost, cost-savings, and ROI of B-ACLS and F-ACLS training for physicians in Singapore.
Methods
This study compares costs of B-ACLS, F-ACLS courses for physicians offered at Singapore First Aid Training Centre (SFATC) 10 and evaluates the ROI to the training provider by comparing costs over benefits (cost-savings if B-ACLS is used in place of the F-ACLS course) over a five-year time horizon. Cost data as of April 2016 were collected from the training provider and used for the ROI estimation.
Cost
F-ACLS is offered as a 1.5-day course with an average intake of three learners per class and is conducted 14 times a year while B-ACLS is offered as a 0.6-day course (five hours) with an average intake of five learners per class, conducted 15 times a year. Direct and indirect costs both of B-ACLS and F-ACLS were obtained from the training provider. Fixed costs included costs for facilities, hardware, software, maintenance and course development/production and revision costs (Table 1). Facility cost was calculated based on utilization percentage of the facility for B-ACLS (3.5%) and F-ACLS (7%) of the overall facility cost ($95,238).
Course and cost characteristics for B-ACLS and F-ACLS training.

All costs in United States dollars (1 SGD = $0.70 US). bIncludes purchase of hardware, software, simulator equipment and internal labor cost. cEquipment rental cost, dDiscount rate of 4% was used to compute cost of training over life of course (five years).
B-ACLS: blended advanced cardiac life support; F-ACLS: face-to-face advanced cardiac life support; ROI: return on investment.
Variable cost changes with the number of sessions per year include instructor costs, learners’ cost (productivity loss) and travel cost (Table 1). Productivity loss refers to the cost to the employer every time the learner is away on training; this was computed by multiplying total number of learners and their average hourly salary and hours spent both on travel and training. Average travel cost for B-ACLS and F-ACLS was $14 and $28, respectively. Five-year cost was computed by multiplying travel cost × number of learners per class × number of classes per year. All costs presented in this paper were calculated in Singapore dollars (SGD) and converted to United States dollars (USD) with time-discounting of 4% of the total cost over the life of the course. 21 As of January 1, 2016, SGD1.00 is equivalent to USD 0.70 and USD 1.00 is equivalent to SGD1.428. Detailed cost computation is presented in the supplementary file available at https://drive.google.com/open?id=1M27J_rJeOiIhLe8D98W82c3i8-Y-446T.
Benefits
The benefits considered for this analysis were the cost-savings between B-ACLS and F-ACLS. ROI is a comparison of net benefit (dollar benefits to the cost of the program). In this study, ROI was computed by dividing the cost-savings between B-ACLS and F-ACLS by the total cost of B-ACLS, expressed as a percentage and ratio. Calculations were performed using MS Excel, version 2010 (Appendix Figures A.1, A.2 and A.3).
Assumptions
The following assumptions were made in this study as the data were not collected.
The lifespan of the B-ACLS and F-ACLS courses were taken as five years. This assumption was made keeping in view the revision cycle of ACLS scientific updates, which is five years. 22 Hence, the current course could be used for the next five years without modifications to the course content.
Average annual compensation for trainees who are usually physicians (registrar level) was assumed to be SGD120,000 (equivalent to USD83,939). 23
The analysis was performed from the societal perspective and the outcome measures were:
total saving over the lifespan of the course;
average savings per month for B-ACLS;
ROI % and ratio; and
months to break even for B-ACLS.
Sensitivity analysis
Multiple univariate sensitivity analysis was performed on several input variables to test their impact on the outcomes (Table 2).
Impact of variables on ROI.
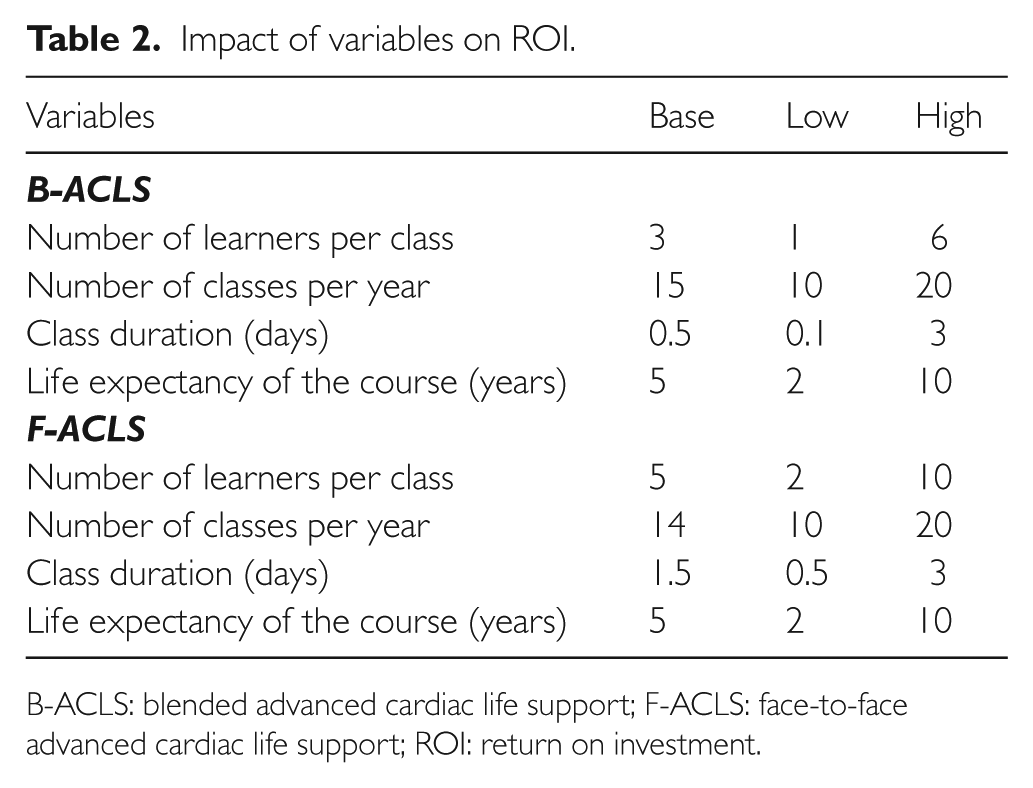
B-ACLS: blended advanced cardiac life support; F-ACLS: face-to-face advanced cardiac life support; ROI: return on investment.
Results
Table 1 shows the costs for conducting the F-ACLS and B-ACLS courses. Recurring development (revision and updating) costs accounted for 13% and 4% of the fixed cost for the B-ACLS course and F-ACLS course, respectively. Annual costs of productivity loss, travel costs and reading material costs was lower by 76%, 63% and 55% respectively in B-ACLS when compared to F-ACLS. Instructor costs were 70% lower for the B-ACLS group when compared to the F-ACLS group. The estimated annual cost was 1.7 times higher for F-ACLS when compared to B-ACLS. Similarly discounted total cost of training over the life of the course (five years) was 2.9 times higher for F-ACLS when compared to the B-ACLS course. Cost of productivity loss account for 53% and 21% of the costs among the F-ACLS and B-ACLS, respectively.
The cost-savings and ROI are presented in Table 1. B-ACLS training for physicians provides the best training value with an ROI of 160% over its lifespan. For every dollar invested in B-ACLS, the organization will save USD1.60 in training cost. In business language, one USD dollar invested brings 160% of returns in five years. This translates to 61% savings over the lifespan of the course if B-ACLS were to be used instead of F-ACLS.
Months to break even for B-ACLS training were estimated to be 38 (Table 2). When there are at least 15 sessions for B-ACLS per year with three learners in each session and 15 sessions for F-ACLS per year with five learners in each session, the cost advantage for B-ACLS increases steadily over F-ACLS with increasing numbers of sessions per year. Figure 2 shows the projected cost-differential between F-ACLS and B-ACLS for increasing sessions per year. Figure 3 shows the results of the sensitivity analyses performed using the most and least favorable conditions for all variables. The model was most sensitive to variations in life expectancy of the B-ACLS, followed by the class duration of B-ACLS course (Figure 3). The ROI for the sensitivity analysis ranged from 15% to 370% for the least favorable conditions, with an average of 179% favoring B-ACLS, and from 49% to 400% for the most favorable conditions, with an average of 197% favoring B-ACLS.

Five-year cost of B-ACLS and F-ACLS by number of sessions per year.

Tornado plot depicting change in return on investment due to change of one input at a time. Highlighted bar (class duration) refers to the best training value being F-ACLS. BACLS: blended advanced cardiac life support; FACLS: face-to-face advanced cardiac life support.
Discussion
Blended learning, a combination of traditional face-to-face learning and asynchronous or synchronous eLearning, is now widely used in life support training for physicians.24–27 The International Liaison Committee of Resuscitation evaluated the use of eLearning for basic life support training and passed recommendations to consider video- or computer-based learning as an alternative to instructor-delivered life support training.28,29 At this juncture our study was planned to determine the cost-savings and ROI of B-ACLS versus F-ACLS training for physicians in Singapore.
Studies worldwide have assessed the effectiveness of the blended ACLS/advanced life support (ALS) training for physicians and have showed that they achieved similar learning outcomes to face-to-face courses16,23–25 at reduced costs. 30 Ali et al. assessed the potential of eLearning (telemedicine technology) to teaching advanced trauma life support (ATLS) and found that knowledge and skills scores were similar for the eLearning and the standard ATLS course. 24 Furthermore, three randomized, controlled trials evaluated eLearning before 25 or after26,27 standard face-to-face ALS training. Two of these studies found no difference in knowledge or skills between the eLearning intervention and the standard intervention, whereas the third found small increases in knowledge domains in the e-ALS group. 26
Another open-label, randomized, controlled trial found that the blended approach to ALS training that included eLearning reduced the duration and costs of face-to-face training by one-half. The blended and conventional approaches had similar outcomes for knowledge- and skill-based domains. However, success rates in the CASTest were 6% lower in the e-ALS group than in the c-ALS group. 30 But not much is known about the cost-savings or ROI of this new technology to the provider.
The current study showed that B-ACLS training for physicians provides a 61% cost-savings over F-ACLS over five years to the provider and a 160% ROI, both in the base case and across a wide range of assumptions. The ROI (%) of 160 indicates that the course not only pays for itself, but it saves costs and time. So for every dollar invested in B-ACLS, the organization can save up to 1.60 SGD dollars in training cost in five years. Although there may be a substantial initial outlay for B-ACLS, the marginal cost of training approaches zero in the third year. The B-ACLS course offers a few advantages over the F-ACLS. It allows the trainer to use a combination of digital media and face-to-face instruction to improve efficiency of learning. It also offers adequate time for the trainer to update and enhance the learning content; trainers’ time spent in the classroom for the B-ACLS course is one-third the time spent for the F-ACLS course. Another advantage of B-ACLS is that it offers learners the ability to vary the learning pace to suit their learning style and work commitments.
Limitations
Our study has inherent limitations. First, we included only cost-savings attributable to the reduction in training days and the productivity loss cost of the learner. The study did not include the passing/failing rates of B-ACLS, the number of retests conducted and the number of doctors who subsequently drop out or move on to undergo F-ACLS training; changes in workflow such as increased workflow efficiency, trainer productivity, increase in productivity of the learner, and the effect of training in patient care were not factored into the analysis, as the supporting data were not available. Thus, we foresee that the savings may actually be higher. Further studies are necessary to accurately understand the full impact of the training on direct patient care. Finally, as our study was based on a single site, the findings may not be generalizable. ROI can be used both to justify a planned investment and to evaluate the extent to which the desired return was achieved. However, it cannot measure all aspects of educational success such as whether physicians liked the training, or the increased motivation and satisfaction or the extent to which learners’ personal objectives were achieved.
The blended mode of ACLS training for physicians provides significant cost-savings to the provider. These savings could be used to enhance the use of technology to further improve physicians’ learning experience. Further studies on this topic should assess the cost-effectiveness of the B-ACLS compared to the F-ACLS using objective assessment of the learners’ knowledge, practical skills and their retention. This would lend greater support for including blended teaching approaches in ACLS/ALS training worldwide.
Conclusion
This study provides crucial cost and ROI comparison of the two different ACLS training approaches in Singapore. B-ACLS had a high positive ROI when compared to F-ACLS. Although B-ACLS has a high capital cost, the annual cost of training is cheaper than F-ACLS. Its ROI will improve further if the development costs become proportionately less in the future. Implementation of B-ACLS in place of F-ACLS in hospitals and academic centers may potentially lead to greater cost and time savings.
Footnotes
Appendix 1
Appendix 2
Appendix 3
Acknowledgements
PPG gratefully acknowledges the funding received from the National Healthcare Group, Singapore, towards doctoral research at University of Adelaide.
The author contributions are as follows: PPG provided the conception and design of the study, acquisition of data, analysis and interpretation of data, drafted the article, revised it critically for important intellectual content, and gave final approval of the version to be submitted; CKO and EL assisted in data acquistion and drafted manuscript; CL and JC were responsible for the article’s critically important intellectual content; and KJ revised the article for critically important intellectual content.
We wish to confirm that there are no known conflicts of interest associated with this publication and there has been no significant financial support for this work that could have influenced its outcome. We confirm that the manuscript has been read and approved by all named authors and that there are no other individuals who satisfied the criteria for authorship but are not listed.
We further confirm that the order of authors listed in the manuscript has been approved by all of us. We confirm that we have given due consideration to the protection of intellectual property associated with this work and that there are no impediments to publication, including the timing of publication, with respect to intellectual property.
In so doing, we confirm that we have followed the regulations of our institutions concerning intellectual property. We further confirm that any aspect of the work covered in this manuscript that has involved either experimental animals or human patients has been conducted with the ethical approval of all relevant bodies and that such approvals are acknowledged within the manuscript.
We understand that the corresponding author is the sole contact for the editorial process (including editorial manager and direct communications with the office). He is responsible for communicating with the other authors about progress, submissions of revisions and final approval of proofs. The conflict of interest statement signed by all authors would be furnished shortly.
This study is part of a larger doctoral study. Ethics approval for the doctoral work was granted by the National Healthcare Group’s domain specific review board (2015/00549) and University of Adelaide Human Research Ethics Committee Office (HREC) (H-2015-237).
Declaration of conflicting interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
