Abstract
Background:
There is currently no review published on the prevalence and incidence of malnutrition in Singapore across various populations, or what interventions or policies are in place for preventing/treating malnutrition.
Objectives:
This review aims to determine the: (a) incidence and prevalence of malnutrition in the community, and in acute, intermediate and long-term care facilities; (b) interventions implemented for screening, assessing and treating/preventing malnutrition; (c) specific clinical populations investigated for malnutrition or nutritional therapy; and (d) implications of malnutrition and effectiveness of treating malnutrition or using nutritional therapy in Singapore.
Methods:
A structured search strategy was applied to available electronic databases (MEDLINE/PubMed, EMBASE, CINAHL, the Cochrane Library and Google Scholar) using selected search terms, with additional reports and grey literature identified using iterative searches.
Results:
Forty-two articles were found, with the majority of research performed in the community and acute care settings. Malnutrition screening and assessment is the most common nutritional research performed in Singapore. Approximately 14.7% to 65.0% of acute care and 2.8% to 31.5% of community populations are found to be malnourished. Limited interventional and economic-related studies are available.
Conclusion:
Malnutrition rates in Singapore appear to be similar to other developed countries. Future studies will need to focus on nutritional intervention, cost-effectiveness analyses and specific populations such as the underprivileged, chronically ill and those dependent on nutritional support.
Introduction
Malnutrition is associated with increased mortality and morbidity. Higher hospitalisation and general practitioner utilisation rates have been reported for malnourished populations as well, leading to increased healthcare and societal costs. 1 Internationally, the prevalence of protein–energy malnutrition ranges from 0.8% to 24.6%. 2 A consensus scheme for malnutrition diagnosis was recently reported, in which two criteria – one phenotypic (non-volitional weight loss, low body mass index (BMI) and reduced muscle mass) and one aetiological criterion (reduced food intake or assimilation and disease burden/inflammation) were required for diagnosis. 3
There is currently no review published on the prevalence and incidence of malnutrition in Singapore, or what interventions or policies are in place for preventing/treating malnutrition. Although costs and effects of malnutrition have been widely described in the literature worldwide, 1 the economic and clinical implications of malnutrition in the local Singapore population is unclear, which led to the conceptualisation and implementation of this scoping review.
This scoping review was conducted to map the research completed systematically and to identify any existing gaps in knowledge in Singapore’ clinical nutrition research field. It aims to determine the: (a) incidence and prevalence of malnutrition in community-dwelling residents and patients in acute, intermediate and long-term care (ILTC) facilities; (b) interventions implemented for screening, assessing and treating/preventing malnutrition; (c) specific clinical populations that are investigated for malnutrition or nutritional therapy; (d) effectiveness of treating malnutrition using nutritional therapy; and (e) implications (clinical and cost) of malnutrition in Singapore.
Methods
A structured search strategy was applied to MEDLINE/PubMed, EMBASE, CINAHL, the Cochrane Library and Google Scholar, using combinations of the following terms as shown in the Supplementary Appendix, and bibliographies of articles. Grey literature from iterative searches was also performed to provide a complete view of information.
There was no restriction on language and the control groups used in the studies. Inclusion criteria included: (a) Singaporean adult aged 18 years or over; (b) receiving care in the community, acute or ILTC settings; (c) receiving nutritional therapy (enteral nutrition (EN), parenteral nutrition (PN) or oral nutritional supplements (ONSs)) or screened/assessed for nutritional status; and (d) published studies in the past 20 years from 1 January 2000 to 31 December 2019.
Only data related to the adult population were used from studies that included mixed populations (paediatrics and adult). Randomised controlled trials, non-randomised interventional studies and observational studies that reported nutritional outcomes (such as nutritional status, anthropometric measurements and nutrition-related biochemistry) were included. Case reports, letters to editors, expert opinions, conference proceedings, clinical/interventional studies on healthy participants, validation studies of non-nutritional-related tools and studies without any relevant nutritional outcomes were excluded.
The protocol was drafted using the preferred reporting items for systematic reviews and meta-analysis (PRISMA) protocols, available on request from the corresponding author, and the review is written in accordance with the PRISMA extension for scoping reviews (ScR) checklist 4 (see Supplementary Appendix).
The title, abstract and keywords of the articles were screened for relevance by two assessors (AW and YX). Duplicates and studies that did not provide relevant information were excluded. Screened articles were retrieved for full-text reading and checked for relevance. Any discrepancies were resolved by consensus. If no agreement was reached, a third reviewer’s (JD) opinion was sought.
AW and YX extracted data with a piloted form and JD checked the data obtained. The extracted data were categorised into: (a) author and publication year; (b) population size and characteristics; (c) type of study and design; (d) the intervention examined; (e) study time frame/duration; (f) prevalence/incidence of malnutrition or risk of malnutrition; and (g) clinical, social or cost outcomes. After extraction, the data were analysed and summarised into a summary format based on the study populations.
Results
A flow diagram of the search results is shown in Figure 1. A total of 1873 records was retrieved from the database search, with 382 duplicates and 1440 articles excluded after title/abstract screening. Fifty-one articles were left for full-text screening, and nine were excluded secondary to reasons, as shown in Figure 1. A summary of the studies is presented in Tables 1 to 5.
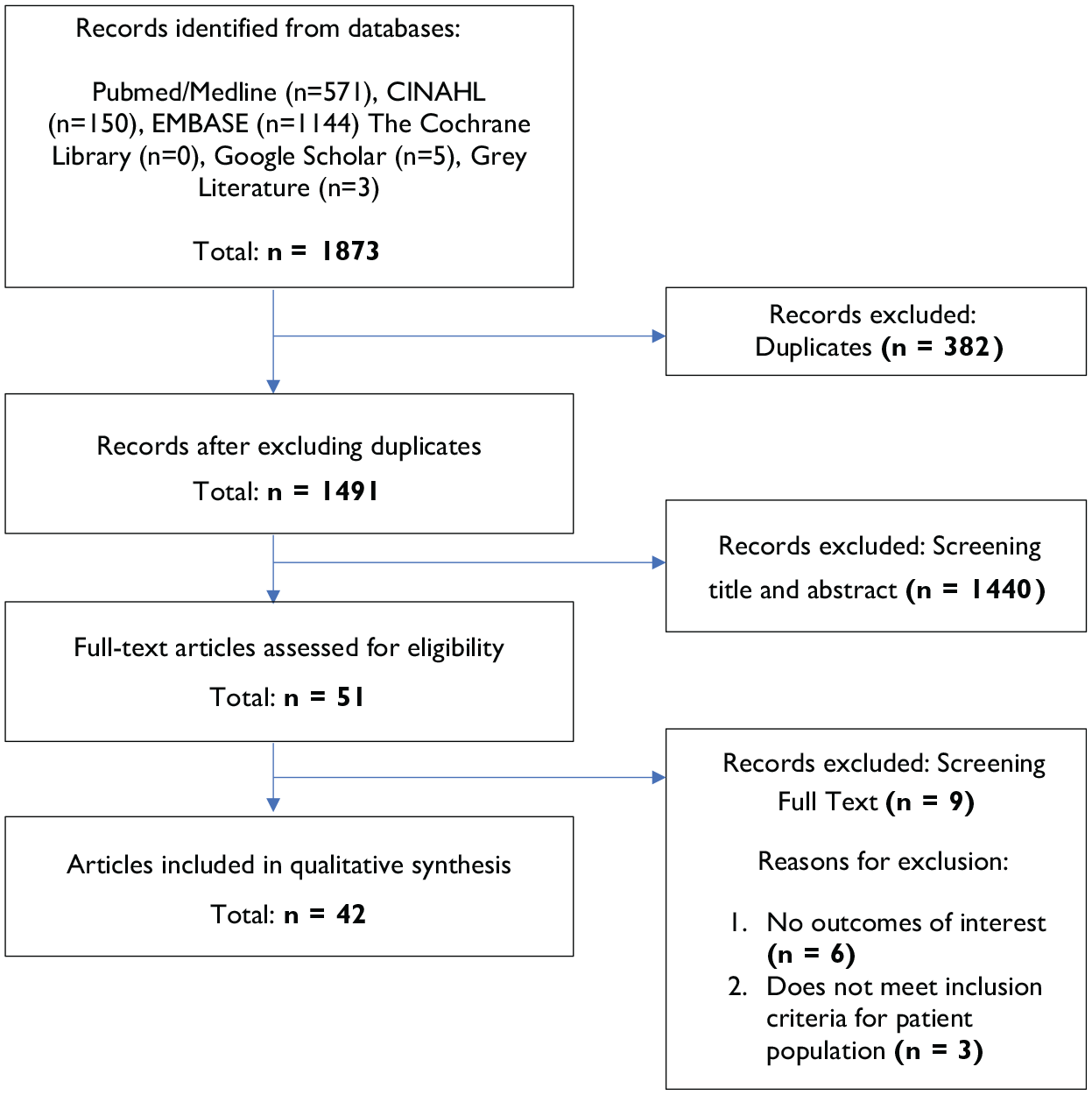
Flow diagram of search strategy.
Nutritional studies on populations residing in the community.

ADL: activities of daily living; ASMI: appendicular skeletal muscle index; BADL: basic activities of daily living; BMI: body mass index; CI: confidence interval; CRP: C-reactive protein; DRG: diagnosis-related group; EQ-5D VAS: EQ-5D visual analogue scale; GNRI: geriatric nutritional risk index; HR: hazard ratio; IADL: instrumental activities of daily living; LOS: length of stay; MNA: mini nutrition assessment; MNA-SF: mini nutrition assessment short form; NSI; nutrition screening initiative DETERMINE checklist; OR: odds ratio; QOL: quality of life; SGA: subjective global assessment; SF-12: 12-item short form survey.
Nutritional studies on patients in acute hospital settings.
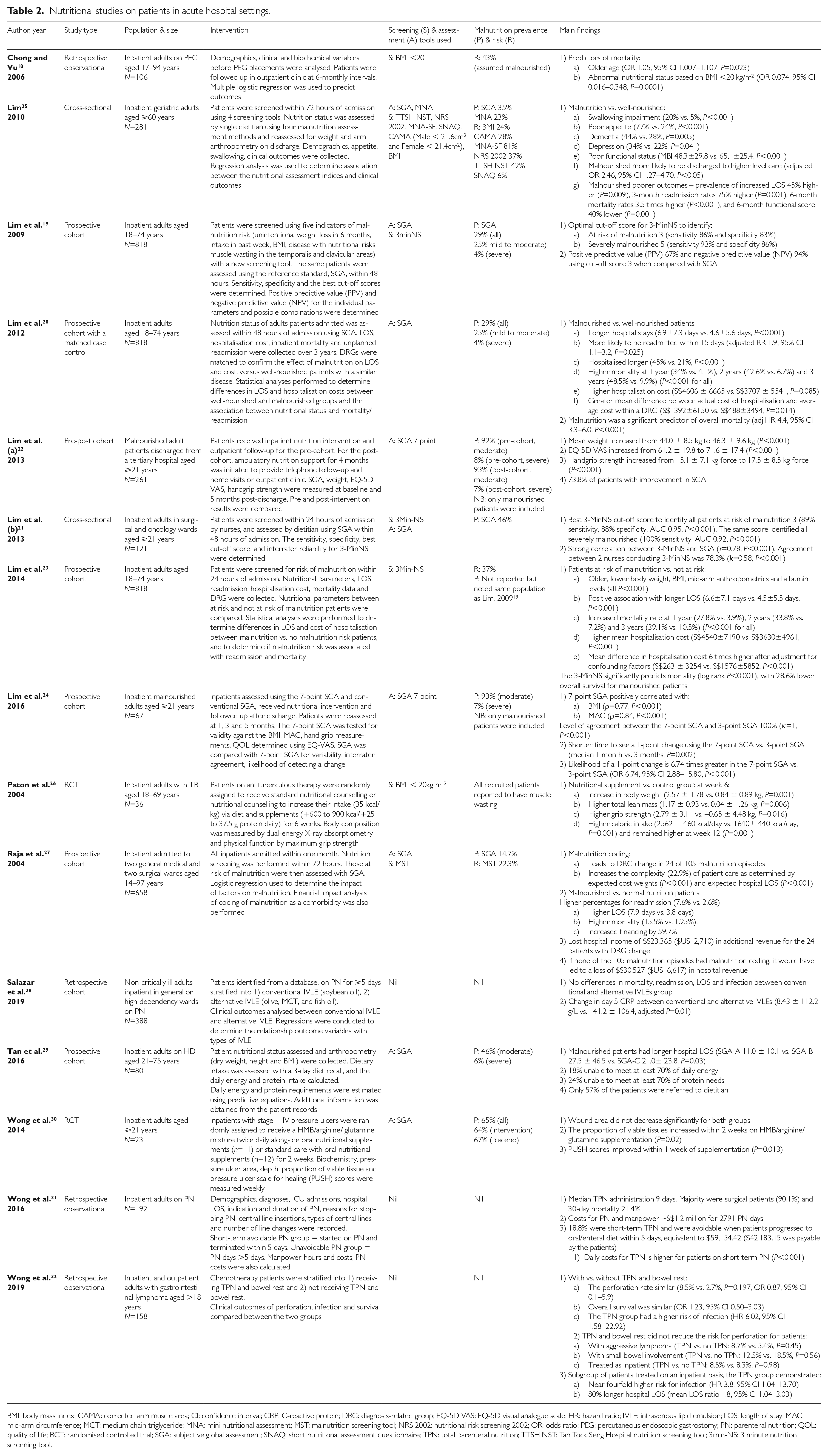
BMI: body mass index; CAMA: corrected arm muscle area; CI: confidence interval; CRP: C-reactive protein; DRG: diagnosis-related group; EQ-5D VAS: EQ-5D visual analogue scale; HR: hazard ratio; IVLE: intravenous lipid emulsion; LOS: length of stay; MAC: mid-arm circumference; MCT: medium chain triglyceride; MNA: mini nutritional assessment; MST: malnutrition screening tool; NRS 2002: nutritional risk screening 2002; OR: odds ratio; PEG: percutaneous endoscopic gastrostomy; PN: parenteral nutrition; QOL: quality of life; RCT: randomised controlled trial; SGA: subjective global assessment; SNAQ: short nutritional assessment questionnaire; TPN: total parenteral nutrition; TTSH NST: Tan Tock Seng Hospital nutrition screening tool; 3min-NS: 3 minute nutrition screening tool.
Nutritional studies on patients in critical care settings.
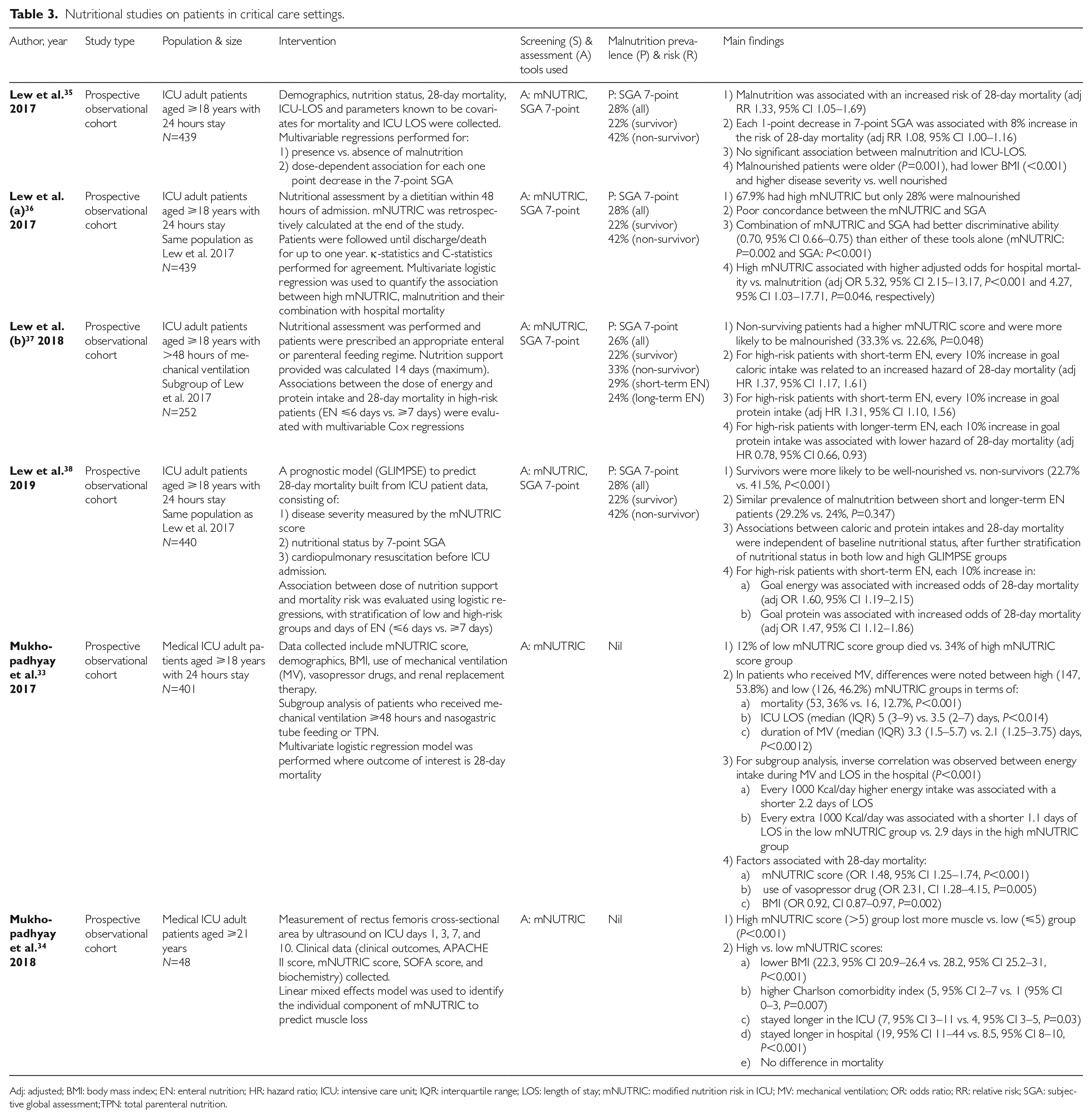
Adj: adjusted; BMI: body mass index; EN: enteral nutrition; HR: hazard ratio; ICU: intensive care unit; IQR: interquartile range; LOS: length of stay; mNUTRIC: modified nutrition risk in ICU; MV: mechanical ventilation; OR: odds ratio; RR: relative risk; SGA: subjective global assessment;TPN: total parenteral nutrition.
Nutritional studies on patients in long-term care settings.

BMI: body mass index; CI: confidence interval; HEN: home enteral nutrition; IQR: interquartile range; MNA: mini nutritional assessment; MNA-SF: mini nutritional assessment – short form; OR: odds ratio.
Nutritional studies on patients in outpatient settings.

ART: antiretroviral therapy; BMI: body mass index; CGA: comprehensive geriatric assessment; CI: confidence interval; DPI: daily protein intake; ECOG: Eastern Cooperative Oncology Group; GI: gastrointestinal; HIV: human immunodeficiency virus; HR: hazard ratio; MMSE: mini-mental state examination; NSI: nutrition screening initiative DETERMINE checklist; OR: odds ratio.
There were 13 studies performed in community populations5–17 (Table 1), 21 studies in acute care18–38 (Table 2), which includes six (
Twelve (
Nutritional screening and assessment
The majority of the studies used validated screening and assessment tools, which were described in other reviews,47–50 and thus will not be described in detail in this review.
In the community population (Table 1), the mini nutritional assessment short-form (MNA-SF)51, 52 (eight of 11 studies, 72.8%)6, 8, 9, 12–16 and the NSI determine your nutritional health checklist 53 (seven of 11 studies, 63.6%) were the tools of choice for screening.5–7, 13, 14, 16, 17 Some studies used multiple screening tools (five of 11 studies, 45.5%).6, 9, 13, 14, 16 One study 9 used the geriatric nutritional risk index 54 and ESPEN diagnostic criteria for malnutrition 55 for nutritional screening. The mini nutritional assessment (MNA) was found to be the tool of choice for nutritional assessment 56 (three of three studies, 100%).7, 10, 11
For inpatient acute care (Table 2), the locally designed 3-minute nutrition screening (3MinNS) is the most frequently reported tool (three of seven studies, 43%).19, 21, 23 One study 25 used four tools – Tan Tock Seng Hospital nutritional screening tool, nutrition risk screening 2002 (NRS 2002), 57 MNA-SF and short nutritional assessment questionnaire (SNAQ). 58 The malnutrition screening tool (MST) 59 was reported in one study, 27 while two studies used BMI as a surrogate for nutritional screening.18, 26 The preferred nutritional assessment tool was the subjective global assessment (SGA) 60 (seven of nine studies, 77.7%),19–21, 25, 27, 29, 30 7-point subjective global assessment (SGA 7-point) 61 (two of nine studies, 22.2%)22, 24 and MNA (one of nine studies). 25
All ICU studies reported using the modified nutrition risk in critically ill (mNUTRIC) score (Table 3).33–38 The mNUTRIC determines which ICU patients are more likely to benefit from nutrition support. 62 However, it does not contain any components of nutritional assessment, such as physical or dietary assessment. The recent ESPEN guidelines for critical care nutrition also disagree with its use as a nutritional screening tool in the ICU. 63 All studies35–38 used the SGA 7-point, which is an expansion of the traditional 3-point SGA. 61
In the outpatient settings (Table 5), BMI was used as a screening tool (two of five studies, 40%)43, 45 in the earlier years while the NSI (three of five studies, 40%) was used more recently.42, 44, 46 One study used a daily protein intake of less than 0.8 g/kg/day and albumin level as an indicator for malnutrition. 45 No assessment tools were used in the outpatient setting. Finally, in long-term care (Table 4), only one study used a validated nutritional assessment tool (MNA). 39 An older study used clinical impression as a surrogate of nutritional assessment. 41
Prevalence and incidence of malnutrition in Singapore
Malnutrition in acute care
National prevalence data in Singapore are limited. The majority of the studies in acute settings (non-critical care) found the prevalence to be 14.7–65.0% in various patient populations.19, 20, 25, 27, 29, 30 For specific inpatient populations, Lim
25
reported 35% of elderly patients to be malnourished, and Wong et al.
30
reported a 65% prevalence of malnutrition in patients (
In the ICU setting, Lew and colleagues35, 36 reported 28% of patients in a mixed-speciality ICU were malnourished using the SGA. Other ICU studies33, 34 reported 45.4% of the surgical ICU population with high mNUTRIC scores but not malnutrition risk or prevalence.
Malnutrition in step-down and long-term care
ILTC in Singapore is predominantly carried out in community hospitals and nursing homes. No studies reported on malnutrition prevalence rates in community hospitals. There are also minimal studies published examining the nutritional status of nursing home residents. In a paper published in 2003, 22% of residents appeared undernourished, but the nutritional assessment was performed based on clinical impression. 41 A newer study used MNA and reported a 39% malnutrition prevalence in a nursing home. 39
Malnutrition in community and outpatient settings
The Singapore Longitudinal Ageing Study 1 (SLAS-1) (
A higher malnutrition prevalence of 3.9% has been found in specific frailty subgroups of the SLAS study populations. 14 Another cross-sectional study of SLAS-1 and SLAS-2 showed that 14% of independent elderly with sarcopenia were at risk of malnutrition, compared to 4.7% of non-sarcopenic individuals. 10 The same authors also looked at those elderly adults with mild cognitive impairment and reported a 31.5% malnutrition prevalence rate. 11
In a study of socioeconomically disadvantaged Singaporeans who received public assistance, a malnutrition prevalence of 2.8% was reported using the MNA.
7
The study found recipients residing in nursing homes have a higher risk of malnutrition compared to community-dwelling adults (68.2% vs. 50.4%,
In the outpatient setting, none of the studies presented malnutrition prevalence data. Three studies performed nutritional screening using the NSI on a group of geriatric cancer patients attending an outpatient clinic and reported that 43.9% were at moderate risk and 29.9% at high risk of malnutrition.42, 44, 46 An older study reported that 30.5% of HIV outpatients have malnutrition 43 using a BMI of less than 17, which is not an appropriate indicator of nutritional status. 64
Clinical outcomes of malnutrition
Lim et al.
20
found malnutrition to be a significant predictor of overall mortality (adjusted hazard ratio 4.4, 95% confidence interval (CI) 3.3–6.0,
Patients with reduced nutritional status were also more likely to be discharged with higher-level care (adjusted odds ratio (OR) 2.46, 95% CI 1.27–4.70). 25 Malnourished patients were found to have poorer clinical outcomes compared to well-nourished patients in terms of a higher prevalence of hospital length of stay (LOS), 3-month readmission rates, 6-month mortality rate and lower modified Barthel index score. 25
In a specific dialysis patient population, Tan et al.
29
found that haemodialysis patients who were malnourished were more likely to have longer LOS (SGA-A 11.0 ± 10.1 vs. SGA-B 27.5 ± 46.5 vs. SGA-C 21.0 ± 23.8,
Frailty and sarcopenia in the elderly population
A considerable amount of research investigated frailty and sarcopenia in the elderly population. The SLAS-1 found that elderly at risk of malnutrition were more likely to have three or more comorbid medical conditions (OR 3.14, 95% CI 2.11–4.69), were hospitalised (OR 2.24, 95% CI 1.49–3.36), functionally dependent for activities of daily living (ADL) (OR 1.72, 95% CI 1.41–2.11) and to self-report poor or fair health (OR 2.29, 95% CI 1.91–2.74). 14
Elderly individuals at risk of malnutrition or malnourished were more than twice as likely to be pre-frail and more than four times likely to be frail.
15
The presence of cognitive impairment was also associated with increased odds (OR 4.19, 95% CI 2.83–6.20,
Malnutrition conferred significantly higher odds of sarcopenia in women (OR 5.71, 95% CI 1.13–28.84,
Older adults who were at risk of malnutrition or malnourished were also associated with increased odds of pre-frailty (OR 2.76, 95% CI 1.86–4.10) and frailty (OR 4.10, 95% CI 1.41–11.9). 15 Individuals who were pre-frail/frail were less likely to revert to a robust, healthy state when they were malnourished or at risk of malnutrition (OR 0.26, 95% CI 0.10–0.67). 15 At the end of the SLAS-1 and SLAS-2 studies, a nutritional improvement was associated with decreased 10-year mortality rates (hazard ratio (HR) 0.43, 95% CI 0.23–0.80). 16
Oral, enteral and parenteral nutrition support
Limited randomised controlled trials (RCTs) on nutritional intervention were available and were mostly performed on patients with specific diseases.26, 30 Paton et al.
26
assigned patients with tuberculosis to receive either standard nutritional counselling (control group) or nutritional counselling with ONSs for 6 weeks. The intervention group had a significantly greater increase in weight (2.57 ± 1.78 vs. 0.84 ± 0.89 kg,
Wong et al.
30
randomly assigned patients with stages II–IV pressure injuries to receive a β-hydroxy β-methylbutyrate (HMB), arginine and glutamine mixture twice daily in addition to ONSs for 2 weeks. Pressure ulcer scale for healing (PUSH) scores showed a significant improvement within one week of supplementation for the experimental group (
Lim et al.
22
performed a pre and post-intervention study on the effect of dietetic follow-up for malnourished patients previously admitted to hospitals. Patients who received inpatient nutritional intervention and outpatient dietetic follow-up/home visits achieved a higher quality of life (EQ5D VAS pre: 61.2 ± 19.8 vs. post: 71.6 ± 17.4,
A few studies reported on PN support. Salazar et al.
28
analysed a database of patients receiving either conventional soybean oil-based intravenous lipid emulsion (IVLE) or alternative IVLEs (olive, medium chain triglyceride and fish oil). The authors found no differences in mortality, infection or readmission rates and hospital LOS between the groups.
28
There was, however, a significant change in C-reactive protein at day 5 between conventional and alternative IVLEs (8.43 ± 112.2 g/L vs. –41.2 ± 106.4 g/L, adjusted
Wong et al.
32
investigated the effects of total parenteral nutrition (TPN) on perforation risk for gastrointestinal lymphoma. The authors compared patients on chemotherapy receiving TPN and bowel rest with those not receiving TPN and bowel rest. Perforation rates in both groups were similar (8.5% vs. 2.7%,
There were only two studies related to EN. Chong and Vu
18
followed outpatients for a change of percutaneous endoscopic gastrostomy (PEG) at 6-monthly intervals and found that abnormal nutritional status (OR 0.074, 95% CI 0.016–0.348,
Critical care nutrition
Mukhopadhyay et al.
33
explored the association of the mNUTRIC score with outcomes in medical ICU patients. Significant differences in mortality (36% vs. 12.7%,
In a series of studies on the ICU population,35–38 Lew and colleagues first reported that malnutrition led to an increased risk of 28-day mortality (adjusted RR 1.33, 95% CI 1.05–1.69).
35
A high mNUTRIC score was associated with higher odds of hospital mortality compared with malnutrition (adjusted OR 5.32, 95% CI 2.15–13.17,
Economic implications of nutritional therapy and malnutrition in Singapore
The earliest study exploring the economic implication of malnutrition was by Raja et al.
27
in 2004, on the impact of malnutrition on a diagnosis-related group and funding. They reported that if none of the 105 malnutrition episodes (of 684 episodes of care) had malnutrition coded as comorbidity, the hospital would have incurred a loss of S$30,527 in additional revenue.
27
A prospective matched case–control study subsequently found that hospital costs in malnourished patients were three times higher than well-nourished patients of the same diagnosis-related group (S$1392 ± S$6150 vs. S$488 ± S$3494,
In a retrospective analysis of inpatients receiving PN, Wong et al. 31 reported that the related costs for PN were approximately S$1.2 million for 2791 PN days. Thirty-six cases (18.8%) with a cost of $59,154.42 were considered to be unnecessary. A recent research survey performed in local nursing homes reported a median monthly EN cost per resident of S$799.47 (IQR 692.11, 940.30). 40 Nursing costs involved in enteral feeding were found to be the main contributor to overall costs (63%). 40
Discussion
This paper is the first scoping review targeted at local studies on nutrition-related research in inpatient, outpatient and community settings. The majority of the research included nutritional screening and assessment, and the tools used have progressed over the years. One of the reasons why nutrition screening/assessment is more widely researched could be due to the lack of funding for nutritional intervention studies in Singapore.
In the initial years, studies18, 41, 43, 45 tend to use non-validated screening/assessment tools such as BMI, weight and clinical observations as a nutritional screening/assessment tool. Subsequently, validated tools specific for individual populations such as MNA/MNA-SF and SGA/7-point SGA were adopted. This finding indicates the awareness of the importance of an accurate diagnosis of malnutrition and its impact on study results.
The majority of the studies that used MNA-SF to determine malnutrition status also did not follow-up with a further assessment using the full MNA.6–9, 12–16 The MNA-SF has been found to overestimate malnutrition in hospital settings, 65 although the criterion validity results look promising for the community population. 48
From this review, the prevalence of malnutrition in Singapore ranges from 14.7% to 65.0% in acute care,19, 20, 25, 27, 29, 30 28% in the ICU,35, 36 39% in long-term care 39 and 2.8–31.5% in community (elderly population) settings.6, 11, 14, 15 The local figures appear similar to other developed countries. 2 Other figures worth noting are the incidence rate of 15.7 per 1000 people-years and a point prevalence of 136.6 per 1000 residents on EN, 40 which provides us with a baseline number for comparison in future studies.
One of our concerns was the impact of food insecurity on malnutrition. A recent survey by the Lien Foundation showed that 19% of 236 participants reported severe food insecurity. 66 In this review, we found that malnutrition prevalence was higher in Singaporeans of lower socioeconomic status 7 than the general populations in the SLAS-1 and SLAS-2 studies. This finding indicates that food insecurity could be a significant contributor to malnutrition.6, 13 Future studies will need to assess the degree of malnutrition in individuals with food insecurity and ways to mitigate the issue.
More research is also required in the area of nutrition support. Only three observational studies on PN were identified within the past 20 years,28, 31, 32 and more interventional and economic evaluation studies are necessary to determine the clinical and cost-effectiveness of using PN in a local context. There was also a limited number of EN studies, particularly in acute care settings. While more studies were done on critical care nutrition,33–38 these studies were based on the same cohort. One of the observations made is the lack of cross-institution research. As Singapore is a small nation, pooling of data between institutions may be a viable option to achieve appropriate sample sizes for analysis.
There is a lack of direct nutritional support and cost-effectiveness studies. Only one study showed that hospital costs in malnourished patients were three times higher than in well-nourished patients of the same diagnosis-related group. 20 The benefits of the provision of nutritional support have been well documented in patients who are malnourished or at risk of malnutrition. 67 Similarly, in community and nursing homes, ONSs reduced hospitalisation and led to cost savings when used consistently for 3 months. 68 Only one study in this review reported the cost of EN in nursing homes. 40
Further local studies are necessary to determine the cost-effectiveness of EN in this population and to ascertain if current medical nutrition reimbursement in Singapore is adequate, as a recent systematic review reported a trend for cost savings and improvement in outcomes of patients on home EN. 69
Limitations
We did not perform risk of bias of the evidence as a scoping review does not aim to appraise the literature critically. However, we have incorporated the use of the PRISMA-ScR checklist to ensure that the data extracted are presented in a structured method. Multiple reviewers were also included to reduce the error and increase the reliability of this review.
As this is a scoping review, the papers identified are wide-ranging and may not be sufficiently focused. However, we have classified extensive literature within a few subtopics to provide a better understanding of the available nutritional research in Singapore. We have also included some studies that only used the controversial mNUTRIC scoring tool, which does not contain any components of nutritional assessment.33, 34 However, these studies were included as the mNUTRIC was initially designed with an intention of determining nutrition risk in the ICU population.
We were also only able to provide a range of figures for the prevalence of malnutrition, instead of a more accurate point prevalence due to the study designs and heterogeneity of the studies available. Despite the limitations, we are confident that this is the best representation of the malnutrition figures to date among the various populations in Singapore.
Conclusions
Nutritional research is gaining traction in Singapore, but the majority of the studies focus on nutritional screening and assessment, rather than on intervention. Malnutrition rates in Singapore appear to be similar to other developed countries, and more needs to be done to address the issue, considering malnutrition’s implications for health outcomes and the use of other resources. We suggest future studies to focus on nutritional intervention, cost-effectiveness/benefits analyses and specific populations such as the underprivileged, chronically ill and those dependent on nutritional support.
Supplemental Material
Appendix_Search_terms – Supplemental material for Adult malnutrition, nutritional interventions and outcomes in Singapore: a scoping review of local studies for the past 20 years
Supplemental material, Appendix_Search_terms for Adult malnutrition, nutritional interventions and outcomes in Singapore: a scoping review of local studies for the past 20 years by Alvin Wong, Yingxiao Huang, Przemyslaw M Sowa, Merrilyn D Banks and Judith D Bauer in Proceedings of Singapore Healthcare
Supplemental Material
PRISMA_ScR_Checklist_Malnutrition_Review – Supplemental material for Adult malnutrition, nutritional interventions and outcomes in Singapore: a scoping review of local studies for the past 20 years
Supplemental material, PRISMA_ScR_Checklist_Malnutrition_Review for Adult malnutrition, nutritional interventions and outcomes in Singapore: a scoping review of local studies for the past 20 years by Alvin Wong, Yingxiao Huang, Przemyslaw M Sowa, Merrilyn D Banks and Judith D Bauer in Proceedings of Singapore Healthcare
Footnotes
Authors’ contributions
A Wong and Y Huang contributed to the conception and design of the research; PM Sowa, MD Banks and JD Bauer contributed to the design of the research; A Wong and Y Huang contributed to the acquisition and analysis of the data; all authors contributed to the interpretation of the data; A Wong and Y Huang drafted the manuscript. All authors critically revised the manuscript and agree to be fully accountable for ensuring the integrity and accuracy of the work and read and approved the final manuscript.
Availability of data and materials
Not applicable.
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Not applicable.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Not applicable.
Supplementary material
Supplementary material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
