Abstract
Background:
This paper documents the history of the renal transplant programme at Singapore General Hospital. Renal transplantation in Singapore was born out of a necessity to offer a cheaper alternative to the expensive and scarce dialysis treatments in the 1970s. As a result, the first deceased kidney donor transplant was performed in 1970 at what Singapore General Hospital was then called ‘the Outram General Hospital’. However, deceased donation rates were dismal and prompted the start of a living kidney donor transplant programme in 1976 at Singapore General Hospital. Unfortunately, the prevalent population of patients with end-stage renal failure rapidly grew while kidney donation rates remain poor despite active efforts to raise awareness and even importing unwanted kidneys from other countries.
Discussion:
As a result, an opting-out legislation called the Human Organ Transplant Act was introduced in 1987 and increased the rate of deceased kidney donor transplantation in Singapore. Over the next two decades, access to kidney transplantation was further expanded with the introduction of living unrelated kidney donor transplantation and laparoscopic donor nephrectomy. In the past 10 years, there have been further advances in kidney transplantation with the introduction of newer immunosuppressive agents and technologies to perform incompatible kidney transplantation. The Human Organ Transplant Act has also been amended to allow the use of older deceased donors and permit paired kidney donor exchanges.
Conclusion:
Despite these many advances, kidney donation rates remain low and are even declining. This would certainly be the major challenge for the renal transplant programme in the next 50 years to come.
1970s: early days
Kidney transplantation in Singapore would not have been possible without a haemodialysis programme and the philanthropic support that the Singapore General Hospital (SGH) or what it was then called, Outram Road General Hospital, received in the 1960s.
In 1961, a generous donation of a Travenol (Kolff) twincoil dialysis machine from Dato Lee Kong Chian ushered dialysis into Singapore. 1 As a result, there was hope for patients with acute kidney failure as dialysis enabled 35% of those afflicted to recover from the illness. However, for those with irreversible end-stage renal failure (ESRF), there was no chronic haemodialysis programme and it was estimated that 100 Singaporeans died from ESRF every year then. Professor Khoo Oon Teik who was then head of Medical Unit 2 of SGH recognised the importance of developing a chronic haemodialysis programme so that patients on dialysis would be able to survive long enough to receive a kidney transplant. He initiated a donation drive to procure a chronic haemodialysis machine and eventually started a haemodialysis programme in 1968. By 1970, a 10-bedded dialysis unit was set up at SGH using the Drake Willock machine.
While the haemodialysis programme was developing, visits to overseas transplant centres were made in 1965 to develop the knowledge required for setting up a kidney transplant programme. In 1966, a proposal was made to the Ministry of Health to approve and support an organ transplant programme, and by 1967 Professor Khoo announced the plans for SGH to perform kidney transplantation. As a result, in the following year, a kidney transplant team was formed. In addition, an animal experimental surgery laboratory was set up using donations from Dato Dr Aw Cheng Chye and the China Medical Board. With this laboratory, the kidney transplant team led by Professor Chan Kong Thoe developed their surgical skills by performing one dog renal transplant per week. Simultaneously, protocols were developed at SGH for deceased donor kidney procurement, tissue typing and postoperative management. As there was no government funding available, the National Kidney Foundation (NKF) was set up in 1968 to develop dialysis and transplant-related funding and Professor Khoo Oon Teik became its first chairman.
By the end of 1969, SGH announced that it was ready to perform its first kidney transplant. However, there was little support from the University of Singapore and objections were voiced over whether this was a priority among many other primary healthcare needs at that time, such as hospital beds and better facilities for patients. A general practitioner even declared that ‘this move to transplant is both ill-timed and ill-considered. It entails a large sum of money spent on a handful of patients to achieve results which can at best be of short-term success’. 2 Nevertheless, the dream of performing a kidney transplantation persisted.
By the time a deceased donor was available, there were three candidates for transplantation but one had died while the other was too ill for transplantation. This left Ms Doreen Tan (Figure 1) who was a clerk at the British Royal Air Force and had been on haemodialysis since October 1969. As a result, she became Singapore’s first kidney transplant recipient on 8 July 1970 when she received a kidney from a 20-year-old national serviceman who died from a brain infection. This momentous transplant was financed by NKF and led by Professor Chan Kong Thoe, head of the surgical department at SGH back then. The transplant was complicated by delayed graft function but eventually Doreen was discharged in September of 1970.

Ms Doreen Tan, the first Singaporean to receive a kidney transplant in Singapore. (Image by Professor Chan Kong Thoe).
The significance of this event was that it was a quantum leap in the treatment of ESRF in Singapore and it was also the first deceased donor kidney transplant performed in South-East Asia. This kick-started the deceased donor kidney transplant programme, which eventually led to Singapore being the country with the highest deceased donor kidney transplant rate per million population rate in the South-East Asian region. 3 Another remarkable observation was also that Ms Doreen Tan continued to live for another 22 years before dying at the age of 52 years on 19 March 1992 from infection related to a hip replacement operation. This was truly a testimony to the skills and care of the healthcare team that was still practising medicine in what Singapore was then – a developing country, barely 5 years after achieving its sovereignty.
Kidney donation rates were very poor with only five more deceased donor kidney transplants performed, and the mortality rate of ESRF patients rose to 400 deaths per year in 1972. There were difficulties getting consent for kidney donations due to religious superstitions and fears that kidneys may be prematurely removed. 4 In 1972, the Medical Therapy Education and Research Act (MTERA) was introduced in 1972 to pave the way for individuals to pledge their kidneys for donation on their death.
With the passing of the MTERA, the NKF launched a campaign in 1973 to get more Singaporeans to pledge their kidneys by signing donor cards. However, deceased donor kidney transplant rates remained low, with only 20 deceased donor kidney transplants performed between 1970 and 1976. As a result, living kidney donation was subsequently legally permitted and resulted in the first living kidney donor transplant being performed in 1976. Between 1976 and 1983, living kidney donors became the predominant source of kidney transplantation at SGH, with 95 kidney transplants performed from parents and siblings.
1980s: desperate for donors
In 1981, the current SGH was opened by the then Prime Minister, Mr Lee Kuan Yew, and ushered in the second decade of kidney transplantation in Singapore. The renal unit in the old attic of the Outram General Hospital shifted to a sparkling new ward and dialysis centre on level 2 of the new SGH. Amid the excitement of a new hospital and progress in renal care, there was still not enough kidney donors to meet the growing demand of patients with ESRF. Between 1970 and 1982, there were only 30 deceased donor kidney transplants performed at a dismal rate of 2.5 transplants per year. To alleviate this shortage of deceased donors, unwanted kidneys from other countries were imported into Singapore for kidney transplantation under a trans-Pacific organ sharing programme. Between 1983 and 1987, a total of 33 kidneys (27 from the United States and 6 from Canada) were imported, all human leukocyte antigen (HLA) mismatched to their recipients and with very long cold ischaemia times of 50–73 hours. Although these imported kidneys helped to increase the annualised rate to 13.8 per year, the outcomes were very poor with one-year graft survival being only 27.3% compared to the 76.4% 1-year survival rate of local deceased kidney donor transplants. 5 As a result, the trans-Pacific organ sharing programme was abandoned.
Kidney donation rates remained very low and there were insufficient dialysis machines for all. As a result, patients who had the financial means turned to commercial kidney transplants from the black markets in India from 1979 and in China from 1986. Since then, 553 patients from SGH have received overseas commercial kidney transplants from these countries, but the outcomes are poor with infection rates as high as 47% (vs. 5.2% for kidney transplants performed locally) and lower 10-year allograft survival at 66.9% (vs. 77.9% for local kidney transplants). 6 Fortunately, commercial kidney transplantation from these countries has been largely eliminated by 2019 due to better local regulation and enforcement, but now patients go to Cambodia to receive kidney transplantation by a surgical team from China. Patients are referred by local syndicates in Singapore and donors are from Cambodia, Vietnam and even India.
In 1985, cyclosporine was introduced into Singapore and became the mainstay immunosuppression by the end of 1988, leading to dramatic improvements in outcomes. Prior to cyclosporine, the standard of kidney transplant immunosuppression was azathioprine and high doses of prednisolone. However, this regimen was associated with a low 10-year graft survival rate of 32.5% in which rejection was responsible for 81.2 % of graft losses. 7 With the introduction of cyclosporine, 10-year graft survival improved to 67.4%, and graft loss due to rejection fell to 42.3%. Similarly, 10-year patient survival also improved from 47.3% to 87.7% following the switch from azathioprine to cyclosporine-based regimen. This was because when azathioprine and prednisone was used, the doses of immunosuppression were very high, which contributed to the high rates of infective complications and deaths seen during those times, but the introduction of cyclosporine allowed lower doses of immunosuppression. 8
In spite of the advances in kidney transplantation in Singapore, deceased donation rates remained low. Between 1970 and 1986, only 69 deceased donor kidney transplants were performed over 16 years, which represented an annualised rate of 4.3 per year. Living kidney donors slightly buffered the burden of low transplant rates, as 146 living donor kidney transplants were performed between 1976 and 1986, representing a higher annualised rate of 13.3 per year. Nevertheless, there was an urgency to increase transplant rates in Singapore as haemodialysis was expensive and over 90% of patients on dialysis died after 5 years.
As a result, the government explored alternative ways to increase the deceased donation rates. Thus, in 1981, the then Minister of Health, Mr Goh Chok Tong, proposed considering an opting-out or presumed consent legislation to increase the number of organ donations from the deceased. Over the next 5 years, the idea of an opting-out legislation was debated and reviewed by many stakeholders. In the meantime, trained medical social workers called ‘kidney persuaders’ were sent to persuade families to donate the kidneys of their dead relatives in hospital in 1983, but this did not have a major impact on organ donation.
Eventually, in 1985, the health ministry announced its intention to introduce an opting-out legislation as efforts to increase organ pledgers were in vain. Over a period of 13 years, only 24,808 organ donor pledgers out of a target 800,000 organ pledgers were obtained at an astronomical cost of $4 million dollars spent on publicity campaigns. Furthermore, not a single kidney was procured from pledgers and all kidneys from deceased donors were obtained through obtaining consent from their next of kin. As a result, it was clear that the current framework of relying on MTERA to procure organs was not effective to improve transplantation rates. Between 1970 and 1987, only 85 local deceased donor kidney transplants were performed over a 17-year period, at an average rate of five deceased donor kidney transplants per year. Furthermore, there was also no significant drive to encourage more living kidney donations during this period as there were concerns about the health of living kidney donors after donation.
In 1986, Ms Sally Kong was appointed as the first transplant coordinator in Singapore. By 1987, the Human Organ Transplant Act (HOTA) was passed and came into effect in 1988. HOTA was an opting-out legislation, permitting the removal of only kidneys for the purpose of transplantation from Singaporean citizens between 21 and 60 years of age who had died from accidents and were otherwise known to be of sound mind. Muslims were excluded at that time as the Muslim community was not ready to accept donation and transplantation as routine care. 9 HOTA made Singapore the only Asian country in the world to have an opting-out legislation and increased deceased kidney donor transplants from 16 in 1987 to 23 in 1988.
1990s: birth of a modern programme
The annualised deceased donor kidney transplant rate increased to 31 per year between 1988 and 1990, with 58.5% of kidneys donated under HOTA. In that same year, SGH celebrated 20 years of kidney transplantation by holding a lunch gathering of patients, and released 346 balloons into the air which represented the number of kidney transplants performed at SGH. Another milestone achieved in 1990 was the introduction of government financial assistance in immunosuppression, which was previously fully borne by the patient. The 1990s also saw a policy drive to encourage patients to consider living related donor kidney transplantation if they had suitable related donors. This was because, despite HOTA, the deceased donation rates were still unable to meet the demand of a growing wait list of patients on dialysis. The decade also witnessed further moves to expand access to kidney transplantation to patients with ESRF. In order to expand further the potential living kidney donor pool, spouses were also allowed to be living kidney donors in 1991, and thence the first living spousal kidney donor transplant was performed on 4 March 1991 at SGH. Since then, spouses have become the dominant type of living kidney donors currently, accounting for over 80% of living kidney donor transplants being performed over the past 5 years at SGH. Prior to the 1990s, patients who received kidney transplants had either hypertension or chronic glomerulonephritis, but in the 1990s patients with systemic causes of ESRF also started getting transplanted such as systemic lupus erythematosus (1991) and diabetic kidney disease (1992). On 5 March 1994, SGH celebrated performing 500 kidney transplants at a gathering of more than 100 patients and healthcare providers. As a result of the increasing workload and complexity of evaluating donors and recipients while ensuring that post-transplant follow-up care was being provided, Ms Lu York Moi, a nurse, was employed to be the first dedicated post-transplant coordinator in 1998 and is now the longest serving transplant coordinator in the programme.
By the end of 1999, the renal transplant programme at SGH had performed 1000 kidney transplants (761 deceased donor and 239 living kidney donor transplants). Nationally, the introduction of the HOTA had significantly increased the annualised deceased kidney donor transplant rate to 44 per year during the period of 1988 to 1999, and reaffirmed the belief held by HOTA champions like Mr Thambirajah Tharmadurai (chief executive officer of NKF then) and others that an opting-out legislation was necessary to increase deceased donor kidney transplant rates in Singapore. 10
2000s: Foundations of an Academic Transplant Programme
The turn of the 21st century would see rapid advances in renal transplantation that would transform the renal transplant programme at SGH as a world class transplant centre. In 2002, hand-assisted laparoscopic donor nephrectomy was introduced and evolved to full laparoscopic donor nephrectomy by 2004. 11 This new surgical technique improved the acceptability of living kidney donation, as hospital stay was shortened to 3–4 days. New immunosuppressive drugs also started streaming in and formed the modern armamentarium which the renal transplant programme uses to prevent and treat rejection now (Table 1).
Timeline of Immunosuppressive Therapies at the Singapore General Hospital

With the advent of these newer immunosuppressive agents, extracorporeal therapies such as plasma exchange (2005) and the introduction of newer histocompatibility techniques such as flow cytometric crossmatch (2007) and solid phase assays to detect anti-HLA donor-specific antibodies (2008), the renal transplant programme embarked on performing HLA and ABO incompatible kidney transplantation to expand transplant options for patients. As a result, the first HLA incompatible kidney transplant was performed on 9 April 2008 while the first ABO incompatible kidney transplant was performed on 11 November 2009. With further development of critical care nephrology at SGH, newer antibody removal technologies such as double filtration plasmaphresis (2016), glycosorb immunoadsorption (2017) and regional citrate anticoagulation (2018) were introduced to improve the versatility and safety of extracorporeal therapies for incompatible kidney transplantation. For example, in 2018, patients with very high levels of both HLA and anti-ABO antibodies underwent desensitisation with a hybrid protocol using both immunoadsorption and plasmaphresis successfully to undergo living kidney donor transplantation. Such patients would have been considered ineligible for kidney transplantation barely a decade ago.
As experience grew with the use of modern immunosuppression and extracorporeal therapies, the renal transplant programme shared its expertise with others. In 2014, it helped ophthalmologists from the Singapore National Eye Centre to perform high immunological risk corneal transplants using a protocol with basiliximab and sirolimus, while in 2018 it assisted with immunoadsorption for Singapore’s first ABO incompatible liver transplantation at SGH.
Despite these advances in kidney transplantation, kidney donation rates have not significantly improved. After the introduction of HOTA in 1987, deceased donor kidney transplantation increased from an annualised rate of 4.7 per year (1970 to 1987) to 47 per year (1988 to 1999). However, during the first 5 years of the 21 century (2000–2004), the rate of deceased donor kidney transplants fell to 34 per year. At the same time, the number of patients requiring kidney transplants grew from 208 in 1988 to 673 in 2003. As a result, HOTA was reviewed and amended to allow deceased kidney donation from any cause of death in 2004. 12 At the same time, HOTA was also revised to include a regulatory framework for living kidney donation that mandated that all living donor kidney transplant candidates and their donors undergo review and approval from a transplant ethics committee. Following the amendments, the annualised rate of deceased donor transplants increased to 44 per year during the period of 2004–2009, but this was still not enough as 460 patients remained on the kidney transplant waiting list in 2009. As a result, further amendments to HOTA were made to include Muslims into HOTA (2008) and to lift the age cap of 60 years (2009) as an attempt to expand further the pool of potential deceased donors. With the lifting of the age cap, kidney transplantation from elderly deceased donors increased, with kidneys allocated as single or dual based on explant biopsy assessments. Indeed, the first dual kidney transplantation from an elderly donor in Singapore was successfully performed in 2009 at SGH. Since then, 24 dual kidney transplants have been performed with good 1-year 100% patient and 95.8% graft survival rates. Apart from elderly deceased donors, elderly living kidney donors were also increasingly accepted, and SGH performed a living kidney donor transplant from a 75-year-old mother in 2009. The use of elderly donors has become more acceptable, with the proportion of donors older than 60 years increasing from 2% in the 1970s to 7.4% in the period between 2000 and 2019. The amendment of HOTA in 2009 also permitted paired kidney donor exchange and led to the first paired kidney donor exchange in 2015 with a second one being performed in 2018.
With over 800 patients under its follow-up and facing challenging complications such as BK virus nephropathy and antibody-mediated rejection, the care of transplant patients has become more complex and demanded the need for healthcare professionals to be dedicated to transplantation. Notably, the team has grown, with staff having trained in world-renowned transplant centres from the United States, the United Kingdom, Canada and Spain. The number of transplant coordinators has also grown from two in the early 1990s to its current complement of nine. Transplant nursing also established its roots following the ring-fencing of kidney transplant beds in one ward in 2003, while the introduction of transplant advance practice nurses in 2016 augmented physician-directed care. Following the hepatitis C virus (HCV) outbreak in 2015, transplant infectious disease physicians became ‘embedded’ in the programme to provide guidance and advice on transplant infection control, diagnosis and therapies. With these investments in dedicated transplant personnel among other improvements in transplant care, the 3-year graft survival has improved from 87.6% (2000–2008) to 90% (2008–2016) whereas 3-year patient survival has improved from 94.4% (2000–2008) to 96% (2008–2016).
Infrastructure has also improved over the past 50 years. Previously, kidney transplant recipients were seen in the general nephrology clinics and had to travel to different areas to see other healthcare professionals such as the dietician and physiotherapist. There was a risk of exposure to contagious infections and it was difficult for kidney transplant recipients to socialise with one another. However, with the establishment of SingHealth Transplant in 2009 (now called the SingHealth–Duke NUS Transplant Centre) and philanthropic support from the Lee Foundation, the previous health screening centre in level 1 of block 7 at SGH was renovated to become a transplant centre in 2013. This is a one-stop facility for patients who could see their clinicians, pharmacists, dieticians and physiotherapists in one place while having more options for outpatient treatments. The centre also saw patients developing friendships with one another while they wait together for their appointments and led to the development of a Facebook-based patient community called ‘A New Sprout of Life’ in 2016. With greater patient socialisation and their desire to learn more about self-care, the kidney transplant programme in 2016 started an annual end of the year dinner symposium which is well attended by patients and families.
In 2005, a landmark collaboration between Duke University in the US and the National University of Singapore was established, leading to the formation of the Duke Medical School at the Outram campus. Under a SingHealth academic partnership of which SGH is a member, signature research programmes were established and herald a renaissance of academic excellence. The kidney transplant programme has benefited from this transformation by performing research not only with faculty from the Duke Medical School but also with its sister American transplant centre at the Duke University in Durham, North Carolina.
The 21st century has also seen major changes in the transplant coordinator profession. The turnover rate of transplant coordinators was previously high but improved following the separation of deceased donor coordination from pre-transplant and post-transplant recipient coordination in 2009. In 2019, transplant coordinators were also assimilated into the division of allied health to help retain talent and better structure career development.
Finally, despite half a century of improving organ donation legislation, expanding potential donor pools and introducing state of the art immunosuppressive regimens and technologies, there remains a shortage of kidney donors for an ever-increasing prevalent population of patients with ESRF in Singapore. Since the last amendment to HOTA in 2009, the annualised rate of deceased donor kidney transplant has not increased over the past 10 years in Singapore. In fact, it has dropped from 44 per year (2004–2009) to 32 per year (2010–2019). This has been compensated somewhat by an increase in living donor kidney transplants from an annualised rate of 33 per year (2004–2009) to 37 per year (2010–2019). Therefore, the policy of advocating living kidney donor transplantation in the 1990s continues to be relevant in this era of low deceased donation rates. This is especially true when living kidney donation in Singapore appears to be safe, while 41.6% of patients on the SGH wait list either die or become medically unsuitable for transplantation.13–15 As a result, there is a need to invest more efforts in encouraging living kidney donor transplantation.
The birth of the kidney transplant programme 50 years ago at SGH is a miracle. This is because a successful kidney transplant was performed just 5 years after Singapore achieved status as a sovereign developing nation. What is more amazing was that this medical milestone was reached while a young nation was still struggling with basic public healthcare needs. In contrast, many nations around the world currently have only begun to start transplantation programmes despite having the infrastructure and funding to do so earlier. Ever since then, the kidney transplant programme at SGH has progressed by leaps and bounds and is now a modern state of the art unit. It is also helping to develop other programs in the south-east asian region as a sister International Society of Nephrology regional training centre to the Southern Philippines Medical Centre since 2017. All this would not have been possible without the selfless contributions of medical leaders, NKF and charities over the years (Table 2).
Leaders and Supporters of the Renal Transplant Program at Singapore General Hospital
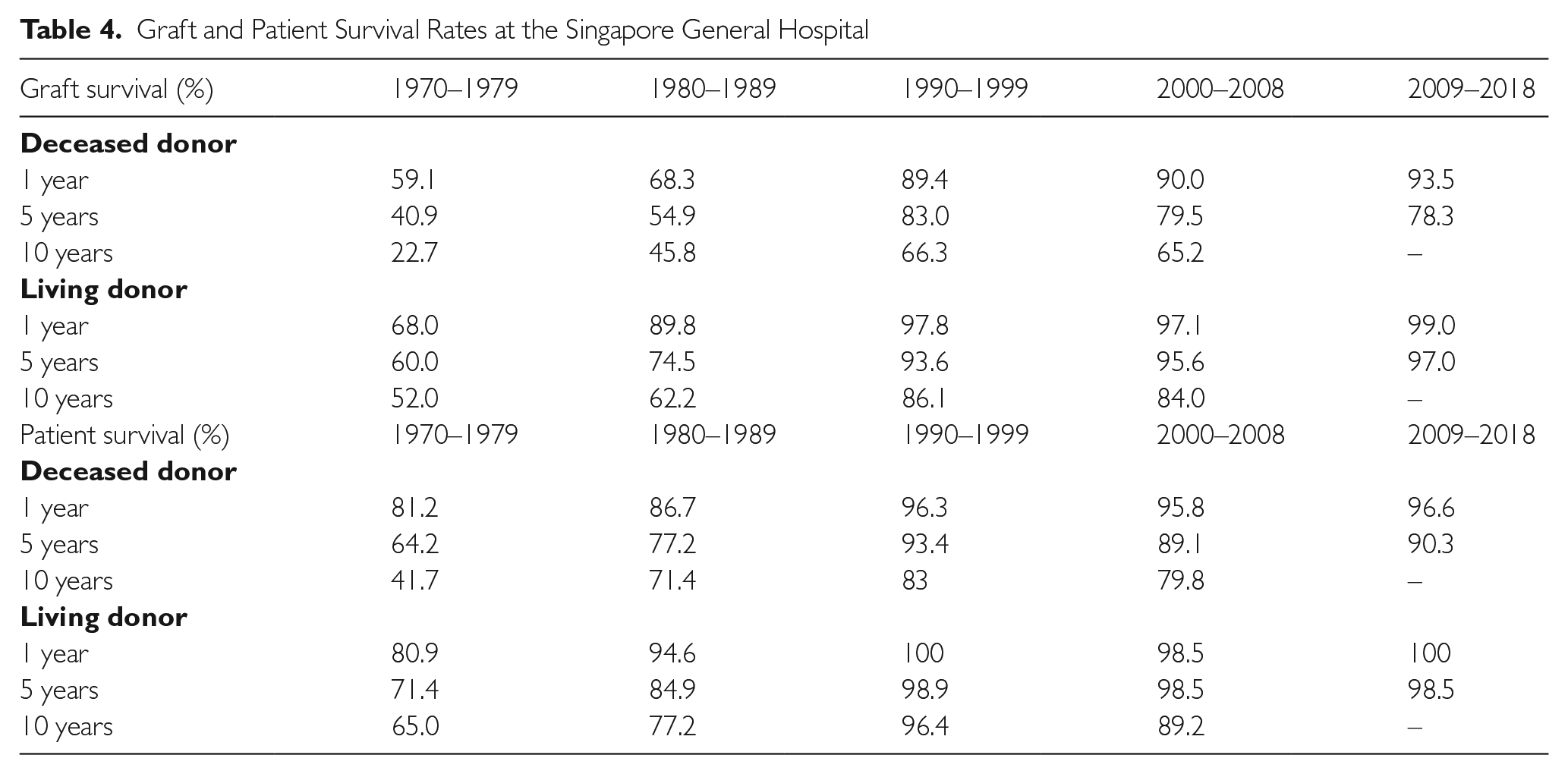
As of 31 December 2018, the renal transplant programme at SGH has performed 501 living kidney donor transplants and 1028 deceased kidney donor transplants (Table 3). The progress made in transplant medicine and surgery over half a century has witnessed significant improvements in short-term graft and patient survival rates (Table 4) while long-term survival rates are comparable to those seen in other countries (Table 5).
Type of kidney transplants and recipient age performed at Singapore General Hospital since 1970

Graft and Patient Survival Rates at the Singapore General Hospital
Graft and Patient Survival Rates at the Singapore General Hospital compared to other Nations

Australia and New Zealand data taken from the ANZDATA 41st Annual Report 2018 (https://www.anzdata.org.au/report/anzdata-41st-annual-report-2018-anzdata/).
United Kingdom data taken from the NHS Organ Donation and Transplantation Activity Report 2018/2019 (https://nhsbtdbe.blob.core.windows.net/umbraco-assets-corp/16537/organ-donation-and-transplantation-activity-report-2018-2019.pdf).
United States data taken from the USRDS Annual Report 2018 (https://www.usrds.org/2018/view/v2_06.aspx).
The future of the kidney transplant programme at SGH is promising as it builds a succession pipeline of future transplant healthcare professionals that will lead the programme into the future. The journey has witnessed historical cycles of growth, decline and tragedies, but with each cycle the experiences and lessons learnt have strengthened the foundations of the programme so that it will be better enabled to face future challenges. With the capabilities built up over the decades, the dream to be fulfilled over the next 50 years is for the kidney transplant programme to be recognised as a first class global centre where it will attract the best talents to train and work while being a key opinion leader in niche areas of clinical practice and research. Most of all, it will be a place where patients will truly feel that they have a second chance at life and the programme places them at the heart of all it does. This is what hope looks like.
Footnotes
Acknowledgements
The author(s) gratefully acknowledge the review of this article from Professor Woo Keng Thye, emeritus consultant from the Department of Renal Medicine. It also acknowledges assistance from the National Library of Singapore and the SGH library services in the retrieval of newspapers and publications that have contributed to the content of this article. The author finally acknowledges the photo contributions by Professor Chan Kong Thoe.
Authors’ contributions
The author(s) conceived the paper, collected literature to support the content of the manuscript and wrote the manuscript.
Availability of data and materials
Not applicable
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This did not involve any patient participation as it is a historical narrative of the transplant program. Data presented are data that are used in audits for governance and oversight.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Not applicable.
