Abstract
Background:
The long waiting time in our General Pediatric Clinic results in the delay in diagnosis and treatment leading to increase in morbidity and dissatisfaction rate among sick children who seek treatment at KK Women’s and Children’s Hospital, Singapore. The mean ± SD waiting time in our General Pediatric Clinic increased from 40 ± 4 days in 2008 and 45 ± 7 days in 2009 to 50 ± 5 days in 2010.
Objectives:
To reduce long waiting times in our General Pediatric Clinic by 20%.
Methods:
The Reducing Waiting Time Working Group was formed to tackle the waiting time problem in the General Pediatric Clinic. Extensive literature was searched and reviewed, brainstorming and discussions were carried out and strategies were developed. A series of implementations were carried out sequentially including clearing of the backlog of cases, development of general and fast track referral guidelines, triaging system and ‘5 Days SMS and 48 Hours Call’ system.
Results:
By clearing the backlog cases, waiting time was reduced from 57 days to 44 days. Through effective triaging system and ‘5 Days SMS and 48 Hours Call’ system, the mean ± SD waiting time was further reduced by 30% from 50 ± 5 days to 35 ± 7 days. By June 2012, the mean waiting time was 27 days.
Conclusions:
Waiting time is one of the important indicators of healthcare quality provided by any healthcare institution. Through these implementations, waiting time was successfully reduced by 30%. These methods may serve as viable options to improve waiting time in other healthcare settings.
Introduction
Long waiting time for medical care is a global challenge, especially in the public sectors. 1 The issue is unique in the field of pediatric care, which often involves many confounding factors, including caregiver availability, the level of parental anxiety and the urgency of the illness. The inability of the healthcare system to cope with the increasing demand has severe implications, for which many studies have shown that long waiting time leads to frustration for not only patients, but also the public and policymakers. 1 The demand for first outpatient visits is negatively affected by waiting time. 2 Long waiting times inevitably exhaust hospital resources, which include healthcare spending, manpower and time.1,3,4 Waiting time has a significant impact on patients’ overall experience and affects perceptions of quality, satisfaction and likeability. Patients who are not satisfied with the accessibility to healthcare are less likely to recommend physicians and attend a subsequent visit. 5 Moreover, patients’ needs may change significantly during the long waiting time, particularly among those with self-limiting diseases. Long waiting time also contributes to high default rate, resulting in disruption in clinic schedules and waste of clinic slots. In addition, delay in diagnosis as a result of long waiting time inadvertently leads to unfavorable clinical outcome. Therefore, waiting time has become increasingly important as an indicator of the quality of patient care, which is not only a tool of rationing and prioritizing healthcare in a resource-limited environment, but also increasingly is being recognized as an objective index for funding and quality improvement in many countries.1,3,4,6
From year 2000 to 2015, the population in Singapore swelled from 4.02m (year 2000) to 5.5m (year 2015). 7 Out of the 3.90m residents, 845,317 (21.6%) are children. 7 KK Women’s and Children’s Hospital (KKH), the largest children’s hospital in Southeast Asia, faces a similar burgeoning problem. In 2010, the General Pediatrics Outpatient Referral Clinic (GPC) in KKH received 9205 referrals from 18 (National Healthcare Group/SingHealth) polyclinics and KKH Children’s Emergency Department, making up 95% of the total GPC referrals.
Over the years, the mean waiting time in the GPC increased from 40 ± 4 days in 2008 to 45 ± 7 days in 2009, and 50 ± 5 days in 2010 (Figure 1). Delay in diagnosis and treatment caused by the long waiting time leads to a high dissatisfaction rate among sick children who seek treatment in KKH, and inadvertently a high default rate in the GPC of up to 60%. In order to improve the GPC waiting time and to effectively use the healthcare resources, the Reducing Waiting Time Working Group was formed in September 2010 to investigate the causes of the long waiting time and improve waiting time through stages of implementations.

Waiting time for subsidized pediatric medicine appointment at 95th percentile (days).
Methods
The Reducing Waiting Time Working Group Committee comprised eight general pediatricians and seven healthcare professionals dealing with outpatient appointments; these are two central appointment staff, two nurse managers, one information technologist, one representative from polyclinic clusters and one representative from Children’s Emergency.
Extensive literature search using PUBMED and CINAHL databases (1990–2013) was performed using keywords ‘healthcare’, ‘waiting time’, ‘waiting’, both separately and jointly. Articles that were not available in English or referred to waiting in disciplines other than healthcare were excluded. Thirty short-listed articles were retrieved and reviewed by the working group. Information was obtained through focus group meetings (include physicians, nurse managers, polyclinic representatives) and a computer-generated appointment tracking database system.
All the information and data were collected and reviewed by the working group. This was followed by multiple brainstorming and discussion sessions. Any disagreement was resolved by group consensus. A strategic and multi-stage implementation plan was finalized following the discussions.
Implementations
Clearing of backlog cases
In October 2010, there were 383 appointments with waiting time of ≥ 60 days. The first step was undertaken to create weekend clinics in order to clear these backlog appointments with waiting time ≥ 60 days. General pediatricians were recruited to evaluate these referrals at the extra hour clinics.
Development of the general and fast track referral guidelines
In January 2011, referral guidelines were formulated by general pediatricians and subspecialists in order to facilitate polyclinic doctors in deciding the urgency of the referrals. These guidelines were disseminated to the polyclinics in both clusters. Doctors from polyclinics were briefed about these guidelines, which were used to decide the types of cases that can be referred for a tertiary opinion and management. A timeline of three months was allocated for doctors from polyclinics to be familiarized with the guidelines before embarking on the triaging process.
Triaging system
This triaging process was first piloted on referrals from National Healthcare Group Polyclinics on 1 April 2011. This was followed by triaging of the referrals from SingHealth polyclinics cluster on 16 May 2011. Referral letters from polyclinics were faxed to the appointment desk a day before the triaging process was carried out. The clinic nurse in charge would collect the referral forms on the same evening and place them on the doctors’ desks. Five pediatricians from the working group triaged all outpatient referral letters from polyclinics on a daily basis. The triaging system was done with the aims of three Rs, which are: ‘Right Patient, Right Time and Right Subspecialty’. The referrals were prioritized based on the urgency of the medical conditions. After triaging, the appointment desk staff would reply to each polyclinic with regard to the appointment details. The turnover time of each referral reply was less than 24 h, except for Friday referrals. The effectiveness of the triage was based solely on medical information given by polyclinic doctors. Thus, feedback on the quality and appropriateness of the referrals was continuously carried out to the doctors in the polyclinic who referred the case. This improved the quality of the referral over time and reduced unnecessary referrals.
‘5 Days SMS and 48 Hours Call’
The ‘5 Days SMS and 48 Hours Call’ reminder system was started on 1 June 2011. This system was implemented in order to open up vacant slots for an appointment and to optimize our healthcare delivery resources. Our hospital central appointment staff sent-off a Short Message Service message (SMS) five days before the actual appointment, to remind patients’ caregivers of their appointment date and time. Patients would be contacted again 48 h before their appointment regardless of their responses, to confirm their attendance. If they were unable to come for the appointment, the slot would then be open to other patients. Patients who were not able to come would be allowed to reschedule their appointments.
After eight months’ analysis on the effectiveness in regard to the default rate, in March 2012 a modification to the above reminder system was implemented. The five-day reminder SMS asking caregivers to reply and confirm their appointments was used. Only the ‘non-responders to the SMS’ were to be contacted by phone 48 h prior to the appointments.
Results
After each intervention, an interim analysis was carried out to evaluate the effectiveness of each measure taken.
Clearing of backlog cases
Appointments with a waiting time exceeding 60 days were identified and prioritized for extra-hour clinics. A total of 28 extra clinics were opened on four consecutive Saturdays and a total of seven extra clinics were opened on weekdays in order to clear the backlog of 383 cases. By clearing the backlog of these cases in the GPC, the waiting time was reduced by 23% from 57 days to 44 days (Figure 2).
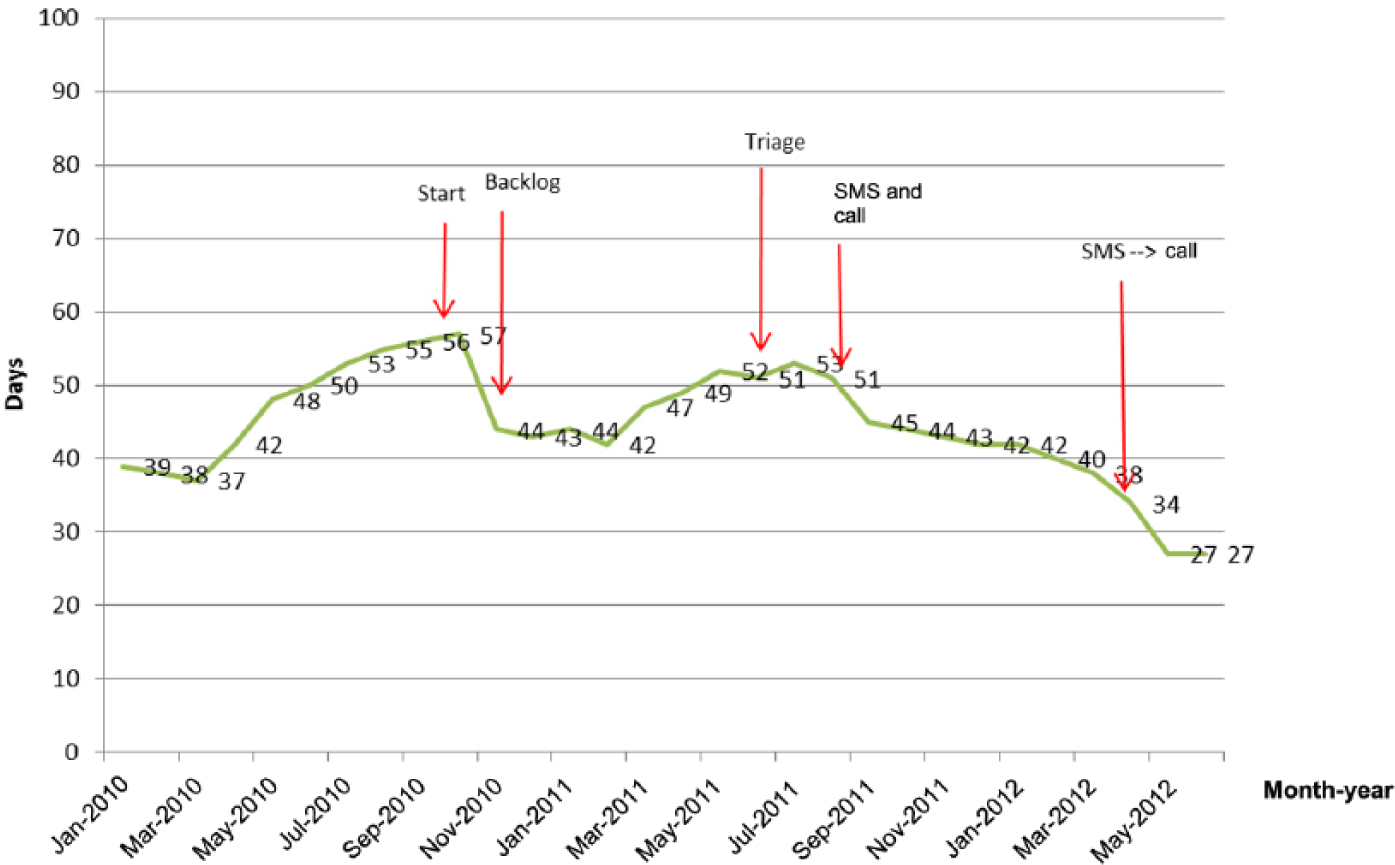
Waiting time for subsidized pediatric medicine (General Pediatric Clinic) appointment at 95th percentile (days).
Development of the general and fast track referral guidelines
As the referrals were not triaged before the development of the referral guidelines, the appropriateness and the quality of the referrals from polyclinics were not accessed adequately. Nevertheless, doctors from polyclinics provided positive feedback about the usefulness of these guidelines. Doctors who vetted the referrals uniformly felt that ‘unnecessary’ referrals were substantially reduced after the guidelines were introduced.
Triaging and the ‘5 Days SMS and 48 Hours Call’ system
Through effective triaging system and the ‘5 Days SMS and 48 Hours Call’ system, the mean waiting time was further reduced by 30% from 50 ± 5 days to 35 ± 7 days (Table 1). The default rate dropped from 53% to 42% (21% reduction) and 26% to 22% (15% reduction) for Children’s Emergency and polyclinic referrals, respectively. After an eight-month implementation of reminder SMS/call policies, the reminder calls were made only for the ‘non-responders to SMS’. There was no significant difference in default rate after the change of reminder policies. Regardless of the reminder system used, default rates remained high, which is possibly a unique problem for pediatric patients as the clinic attendance depends largely on parents’ schedules and availability.
The mean waiting time in General Pediatric Clinic.

Discussion
Waiting time for healthcare exists primarily because of the mismatch between the supply and demand in healthcare provision and these two factors become the main focus in many strategies targeting ways to reduce waiting times. 8 In the context of a general referral clinic in a children’s hospital, the ‘supply’ factors include hospital facility (clinic space), workforce capacity (doctors and allied health supports) and healthcare productivity (cost), while the ‘demand’ factors include patients’ preference and experience. 4 Historically, the main focus has been on increasing the former. Initiatives through increasing funding towards maximizing hospital capacity in terms of space and workforce were the dominant approach used to manage waiting time. A few developed countries, such as Australia, Canada, United Kingdom and New Zealand, have used the politically popular strategy of targeting funding towards increasing the supply, that is, hospital workforce and capacity, with varied degrees of success. 4
Existing capacity was reviewed and adapted more efficiently through streamlining workflow processes and innovating a better-designed system. This helped in optimizing the existing resources available in the hospital. Before the working group was set up, KKH had adopted similar approaches whereby more clinic spaces were created, more doctors and allied health support personnel were hired and more budget was allocated to improve the clinic environment. The scheduling and patient management process were reviewed and optimized through better time-slot arrangement for each appointment. Despite optimizing the supply factors, the committee adopted a different approach in striving for a balance between the supply and demand factors in order to achieve an acceptable target for the GPC waiting time. The committee decided that the demand factor should be mitigated first before dealing with the supply factor. We attempted to reduce our demand through clearing backlog cases and to improve the quality of our supply through reducing inappropriate referrals and prioritization strategy.
In the demand factors, clearing the existing group of patients with the longest waiting time of close to two months was a crucial and yet challenging step before any other intervention could be implemented. This intervention required manpower support (doctors and nurses) and facility backup (clinic space). It also involved patients’ convenience and willingness to attend. This process was completed in two months and successfully reduced the mean waiting time from 57 days to 44 days (Figure 2).
Waiting time may reflect inappropriate referrals. 9 For KKH as a tertiary hospital, the demand in the GPC largely depends on the types of cases being referred by polyclinics and Children’s Emergency. GPC clinics in KKH were often overburdened by the amount of cases referred that could have been treated at primary care level. This was one of the important demand factors that were targeted as a potential intervention. With the aim to reduce these ‘primary care’ cases, there were several steps undertaken which included training of polyclinic doctors and provision of referral guidelines to polyclinic doctors. The guidelines helped the polyclinic doctors in decision-making when the referral was made. This significantly reduced the amount of ‘unnecessary’ referrals to the GPC and improved the quality of referrals made.
Fast track systems have gained significant momentum in the healthcare system, especially in the setting of the emergency department.10–12 Grant et al. in Queensland reported a significant reduction in waiting time within accepted time standards from 59% to 39.1% when the rapid assessment team was operative. 12 These teams streamline the cases based on the urgency of cases. ‘Rationing’ or ‘prioritizing’ strategy was proven to be an effective strategy in reducing demand. 13 A similar strategic principle was adopted and applied in our intervention whereby cases were triaged based on the three-Rs principle – Right Patients, Right Time and Right Subspecialty. The adopted system aims to triage cases into a few categories, that is, urgent, semi-urgent and non-urgent cases. In general, urgent cases will be seen in the next 48 h, semi-urgent cases in two days to two weeks and non-urgent cases in 2–8 weeks. The ‘confirm-previous-day’ approach in adults cannot be applied to pediatric appointments as patients’ attendance depends largely on caregiver schedules and availability, sometimes involving more than one person.
As the term ‘urgent’ infers an impending crisis if left unattended, ‘priority’ was used to replace ‘urgent’ in some institutions. 14 Regardless of the term used, cases were triaged not only based on the urgency of the medical condition, but by taking psychosocial circumstances into great consideration as well. High-risk behaviors (i.e. self-harm, depression) and red flags (i.e. regression of milestones, increasing head circumference) were given significant weightage in the decision making for earlier appointment. Moving forward, a proper triage prioritization system that incorporates local context into such a model may be useful in standardizing the triaging process. Such a model is expected to help reduce variations amongst individuals who triage the referral cases in prioritizing each case. The two-tier ‘check and balance’ system, consisting of guidelines for referring polyclinic doctors and triaging system by pediatricians, did not result in unprecedented adverse outcome throughout the entire study period, that is, increase in emergency cases seen in Children’s Emergency or sick children being admitted due to late attendance or wrong triaging.
The ‘5 Days SMS and 48 Hours Call’ system was used to remind patients about their imminent appointments and to confirm their attendance. This system allows flexibility in arranging patient slots where vacant slots, created by patients not attending, can be taken by those who are keen to come. This indirectly reduces non-attendance. After eight months of implementation of the ‘5 Days SMS and 48 Hours Call’ reminder system, the committee decided to change the system whereby the reminder calls were made only for the ‘non-responders to SMS’. There was no significant difference in default rate after the change of reminder policies. Cost reduction from this policy change cannot be determined accurately due to variation of non-responders to SMS although no significant change in overall operational costs was observed.
There was a clear dose–response gradient where the risk for non-attendance increased with a longer waiting time. 15 Non-attendance rates can be as high as 42%, causing enormous volatility in clinic operations and waste of clinical resources. 16 Johnston et al. reported that for every one week increase in waiting time, there was an incremental rise in the risk of non-attendance by 3.9%. 9 Costs associated with non-attendance include appointment booking, cancellation and rescheduling translated into human capital, financial and time loss. By targeting this group of potential ‘defaulters’, the ‘5 Days SMS and 48 Hours Call’ system offers a ‘window of opportunity’, through which canceled appointment slots can be given to other patients. It will inevitably reduce the numbers of non-attendance and offer some feasibility for parents to change appointments when urgent matters arises.
Confounding events like opening or closing of new hospitals or clinics, changes in hospital’s service capacities or changes in patients’ demographics that could potentially affect the waiting time did not happen throughout the entire study period.
There are a few limitations in this study. First, there are no established guidelines to open ‘weekend clinics’ when the number of cases with excessively long waiting times reaches a certain threshold. Constant surveillance of waiting time is paramount in identifying the time point to reopen ‘weekend clinics’ before waiting time starts increasing. Second, the quality of referral letters was not monitored. The amount of information provided in the referral letter was important in prioritizing the urgency of the case. An internal audit of the referral letters is a potential intervention to improve the quality of referral letters and help in the decision-making process. Third, referral guidelines and triaging process did not involve referrals from Children’s Emergency. Moving forward, these interventions can be extended to those from Children’s Emergency although manpower for the triaging process is often a limiting factor.
This study is a stepping stone to developing the next initiatives to reduce the default rate. A high default rate is a complex issue particularly in pediatric clinics as attendance depends on availability of more than one individual. The estimated cost of non-attendance was close to 0.07% of the 2001 Hong Kong gross domestic product. 9 Non-attendance disrupts a healthcare system and poses financial loss to any country, including Singapore.
In conclusion, Singapore’s healthcare system is not spared from the challenges of how local healthcare managers can adapt to the changing needs of patients rather than expect patients to adapt to the inconveniences they face in the process of seeking medical advice. KKH, being the oldest and biggest children’s hospital in Singapore, has been the ‘brand of choice’ for local Singaporeans seeking medical treatment for their children. The challenge for healthcare managers in KKH is to meet patients and their parents’ expectations through the delivery of efficient healthcare service. To achieve this, waiting time plays an insurmountable role through shortest possible waiting time and cost-effective services in order to maintain positive perceptions of quality, satisfaction and likeability towards treatment they receive in KKH. Moving forward, sustainable and continuous improvement of realistic and short waiting time poses an on-going challenge to healthcare managers and waiting time will continue to serve as a useful index for policymakers to evaluate the quality of healthcare, not only in a single institution but at the national level as well.
Footnotes
Acknowledgements
The authors are grateful to Wang Hao for his assistance in editing the manuscript.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
