Abstract
Background:
Early mobilisation in the intensive care unit has been suggested to improve outcomes. However, safety and practical concerns have led to the slow uptake of early mobilisation.
Objectives:
We designed a study to evaluate the practicability and efficacy of an early mobilisation protocol in intensive care unit patients.
Methods:
We performed a prospective non-blinded observational cohort study based on a quality improvement project. We implemented a protocol for early mobilisation of suitable patients admitted to medical and surgical intensive care units of a tertiary care hospital. All other aspects of patient care were managed as usual. Patients were followed up to discharge. Data were collected from July to August 2016 pre-implementation and from November 2016 to February 2017 following protocol implementation. The primary outcome measure was the mobilisation rate, defined as the number of days mobilised divided by the number of days each patient met mobilisation criteria. Secondary outcome measures included adverse event rate, length of mechanical ventilation, intensive care unit and hospital stay, intensive care unit and inhospital mortality and discharge destination.
Results:
A total of 312 patients were analysed, of which 60% were men with a mean age of 63.4 years. Following early mobilisation implementation, the mobilisation rate increased from 39% to 65% (
Conclusion:
The implementation of an early mobilisation protocol in our intensive care unit was both safe and effective without requiring additional staffing. Efforts are ongoing to increase compliance with the protocol.
Introduction
Medical advances have increased the number of patients who survive critical illness. However, among survivors, significant impairments in neuromuscular function,1–3 physical functioning, 4 cognition, 5 mental health, 6 ability to return to work7,8 and quality of life persist for years post-intensive care unit (ICU) discharge. 9 Numerous individual studies have suggested that early mobilisation (EM) in the ICU is a safe and effective intervention which improves functional outcomes and reduces delirium in the ICU.10–14 However, the effect on ICU and hospital length of stay and ventilator-free days has not been conclusively demonstrated in meta-analyses;10,11,15–18 a recent Cochrane review found insufficient evidence to determine the effect of EM in critically ill patients. 19 However, the adoption of EM as the standard of care has been slow.16,20,21 An international survey of 801 ICUs revealed several barriers to ICU mobilisation including a lack of multidisciplinary rounds, setting of daily goals for patients, absence of a dedicated physiotherapist, suboptimal nurse–patient staffing ratio, inadequate knowledge and training as well as insufficient staffing and resources. 22
Efforts to introduce EM in our institution have been ongoing since 2014. Despite evidence demonstrating the feasibility and safety of EM, safety concerns remain significant among ICU care providers. In addition, perceived inadequate staffing ratios and poor perception of the potential benefits from EM present a constant challenge to its incorporation into our routine clinical practice. We hypothesised that implementing a protocol for EM in the ICU would improve mobilisation rates while remaining safe. Therefore, we designed a prospective observational cohort study based on a quality improvement project to evaluate systematically its practicability, safety and efficacy.
Methods
A protocol for early screening and initiation of EM was developed in conjunction with intensivists, critical care nursing and physiotherapy staff (Figure 1). Patients admitted to the medical ICU and surgical ICU of a large tertiary hospital were enrolled in a prospective non-blinded observational study and followed up to hospital discharge. Inclusion and exclusion criteria for the study were derived based on previous studies examining ICU mobilisation and reviewed by a panel of ICU consultants. The criteria are detailed in Figure 1.

Study protocol flowchart.
The medical and surgical ICUs in our hospital are located in separate wards with a capacity of eight and 10 beds, respectively. Nursing-to-patient ratios are 1:1 for patients deemed to be ‘high acuity’ and 1:2 for ‘low acuity’ patients, and nursing staff are allocated to patients on a per shift basis. Physiotherapy staffing for both ICUs is 1.5 full time equivalents during weekdays and 1 full time equivalent on weekends, split among three to five physiotherapists on a rotational basis. Prior to protocol implementation, the mobilisation exercises described below were already in practice but were not implemented in a systematic or rigorous manner.
Our study was conducted in three phases (Table 1). In phase 1, data were collected on baseline standard practice, in which patients were only referred for mobilisation on an ad-hoc basis at the direction of the attending consultant. Training conducted during phase 2 comprised a briefing to all ICU staff on the new protocol; in addition, nursing staff received didactic education on early ICU mobilisation as well as practical training on mobilisation of ICU patients by physiotherapists. A powered ceiling hoist system for transfer of patients was also installed in the ICUs and nursing and physiotherapy staff were trained in its proper usage. Finally, in phase 3, the screening protocol was implemented systematically, and all eligible patients were automatically referred for mobilisation. No additional manpower was given. All other aspects of patient care were managed as per the discretion of the attending intensivist.
Study timeline.

ICU: intensive care unit.
All patients admitted to the ICU were screened daily by nursing staff for suitability for EM based on set criteria (Figure 1). Mobilisation was defined as an activity involving the patient’s back leaving the bed for more than 5 minutes, in order both to differentiate between sitting up in bed and capture EM activity. Patient mobilisation was performed by physiotherapists and assisted by nurses. The type of activity was left to the discretion of the attending physiotherapists and was classified into five categories – sitting over the edge of the bed, sitting out of bed, sit to stand, stationary marching and ambulating. Passive mobilisation exercises such as passive range of motion exercises, tilt table and chest physiotherapy were also performed as indicated. However, for the purposes of the study, they were not considered to be a mobilisation activity as per our definition. Duration of mobilisation was based on patient tolerance, as there is currently no consensus regarding the optimal duration of mobilisation. 7
Patient demographics were collected prospectively including age, gender, need for mechanical ventilation, premorbid medical problems, functional status and diagnosis on ICU admission. The acute physiology and chronic health evaluation II (APACHE II) score was used as a surrogate measure for disease severity. The primary outcome measure studied was the mobilisation rate, defined as the number of days each patient underwent mobilisation, divided by the number of days each patient met the mobilisation criteria. This was first calculated for each patient, then the mean for each group was calculated. Secondary outcome measures included safety and efficacy aspects of the protocol, namely the incidence of adverse events during mobilisation including line dislodgement, haemodynamic instability, syncope, patient–ventilator dyssynchrony and agitation, ICU and hospital length of stay, duration of mechanical ventilation, ICU and inhospital mortality and discharge destination. Patients were followed up to hospital discharge by review of hospital electronic medical records. Missing data were treated by pairwise deletion. Post hoc subgroup analysis was performed comparing patients who required mechanical ventilation during their ICU stay versus non-ventilated patients.
Data were analysed using Stata 13 (Stata Statistical Software: Release 13; StataCorp LP, College Station, TX, USA). The independent
Results
From July 2016 to February 2017, a total of 312 patients were enrolled into the study. Baseline characteristics and admitting diagnoses of the patients are displayed in Tables 2 and 3, respectively. The median APACHE II score was 18 in the pre-implementation cohort and 21 in the post-implementation cohort; however, a large proportion (61.9%) of patients had missing APACHE II data; 65.6% in the pre-implementation cohort and 60.4% in the post-implementation cohort. The top three admitting diagnoses in descending order were respiratory failure, postoperative cases and sepsis. Both cohorts were similar except that there were more women (42.8% vs. 29.8%) and patients with pre-existing ‘other cardiovascular conditions’ including atrial fibrillation, cardiomyopathy and heart block (10% vs. 2%,
Study Demographics.

61.9% of APACHE data were missing.
ICU: intensive care unit; MICU: medical intensive care unit; SICU: surgical intensive care unit; ADL: activities of daily living; IQR: interquartile range; APACHE II: acute physiology and chronic health evaluation II.
# refers to
Diagnosis on ICU admission.

# refers to
The primary and secondary outcomes are displayed in Table 4. The mobilisation rate increased from 39.0% pre-implementation to 65.1% post-implementation. There was no significant difference in inhospital mortality, length of mechanical ventilation, ICU or hospital stay between groups. However, there was a significant increase in patients who were discharged home from hospital rather than to step-down care facilities or nursing homes. (49.0% pre-implementation vs. 75.9% post-implementation,
Outcome measures.

ICU: intensive care unit; CI: confidence interval; LOS: length of stay; IQR: interquartile range.
bold type refers to
Approximately one-third of patients admitted to the ICU did not meet the criteria for EM, the reasons for which are shown in Table 5; some patients had multiple reasons for ineligibility. Among patients who were eligible for mobilisation, 46.0% and 33.8% from the pre and post-implementation cohort, respectively, were not mobilised (Table 6). Lack of staffing (33%) and weekend (19%) accounted for over half of the reasons for not mobilising in the pre-implementation group. However, these reasons accounted for only 13% in the post-implementation group. Competing activities, such as transport for radiological investigations or invasive procedures and patient refusal, were the main reasons for not mobilising eligible patients in the post implementation cohort (Table 6).
Reasons for not meeting daily mobilisation criteria (n, [percentage]).
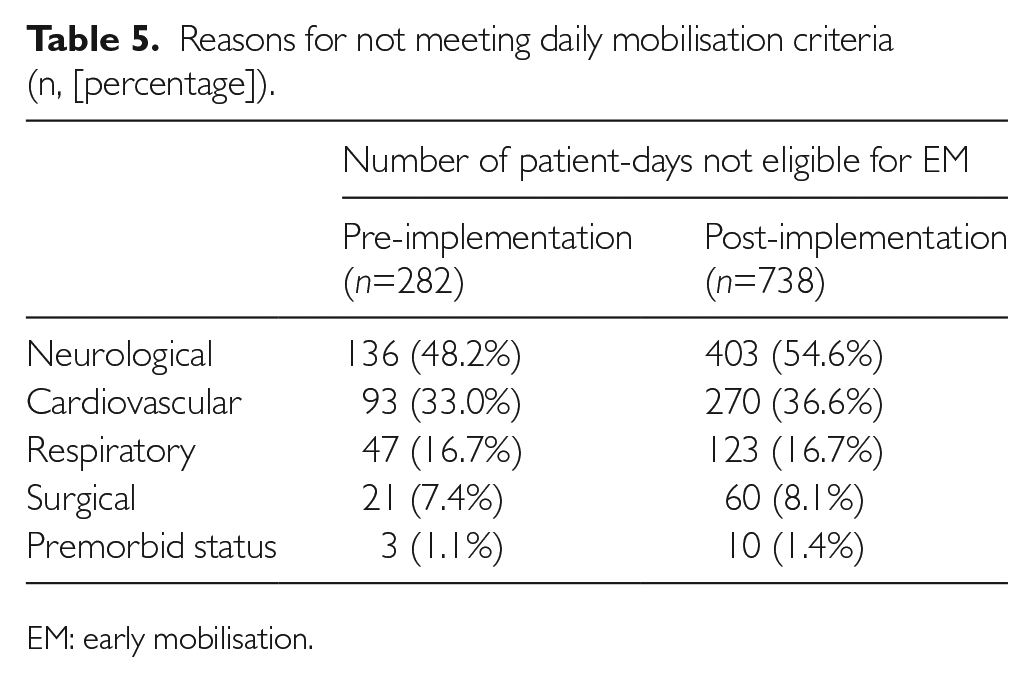
EM: early mobilisation.
Reasons for not mobilising despite meeting mobilisation criteria.

CRRT: continuous renal replacement therapy.
The rate of adverse events during mobilisation was 8.5% in the pre-implementation and 4.7% in the post-implementation group. A breakdown of the adverse events encountered in the study is shown in Table 7. No other adverse events studied were encountered; notably, there were no instances of falls, line or endotracheal tube dislodgement during mobilisation.
Adverse event rates per session.
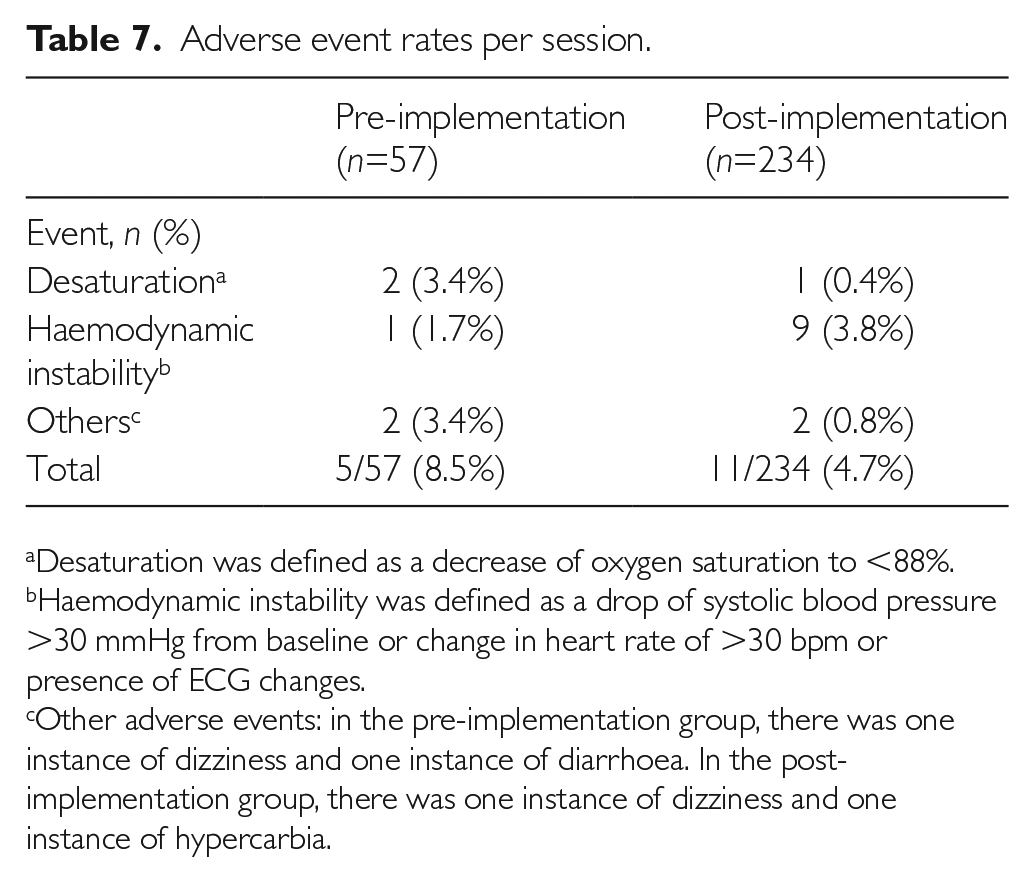
Desaturation was defined as a decrease of oxygen saturation to <88%.
Haemodynamic instability was defined as a drop of systolic blood pressure >30 mmHg from baseline or change in heart rate of >30 bpm or presence of ECG changes.
Other adverse events: in the pre-implementation group, there was one instance of dizziness and one instance of diarrhoea. In the post-implementation group, there was one instance of dizziness and one instance of hypercarbia.
Subgroup analysis of patients who required mechanical ventilation during their ICU stay versus non-ventilated patients was performed and is shown in Table 8. Notably, the relative risk of home discharge in ventilated patients post-implementation was over 1.5 times compared to the pre-implementation group.
Subgroup analysis of ventilated versus non-ventilated patients.

RR: relative risk; CI: confidence interval; ICU: intensive care unit; LOS: length of stay.
bold type result has 95% CI outside 1.
Discussion
Our study shows that the EM protocol was successful in improving mobilisation rates among suitable ICU patients from 39% pre-implementation to 65% post-implementation. This was due to an increase in the percentage of eligible patients being mobilised as well as an increase in the mean number of mobilisation sessions per patient. Although the post-implementation mobilisation rate remained relatively low, this is in part due to the inclusion of patients who were well enough to be transferred out of the ICU before receiving their first physiotherapy session although they were deemed suitable for EM at the point of assessment. These were included in the analysis because they represent a proportion of patients who may still benefit from EM even though they may no longer require intensive care support. It should therefore be emphasised that a robust step-down mobilisation practice to ensure patients continue mobilisation after discharge from the ICU is of equal, if not greater, importance. 23
Besides demonstrating an improved mobilisation rate with our protocol implementation, our study also highlights areas that may be addressed for further improvement. Competing activities, patient refusal and ongoing continuous renal replacement therapy account for over 70% of patients not mobilised despite meeting eligibility criteria. These are modifiable factors, potentially correctable with improved planning of activities for the patients and exploring means to address the concerns of patients who refuse treatment. There is an emerging body of evidence to support the feasibility of mobilising selected patients on continuous renal replacement therapy, a point that should be mooted to healthcare providers who share concerns of safety.24,25 Mobilising such patients nonetheless presents unique challenges in terms of staffing and logistics and represents another area for special attention.
There was a low rate of adverse events which decreased following protocol implementation. However, our adverse event rate is higher as compared to that previously reported in the literature (0.4–4%). Possible reasons include random chance due to a small sample size and a broader definition of adverse events. Of note, there were no major adverse events resulting in lasting patient harm. Overall, our findings are consistent with previous studies examining the safety of EM in ICU patients.7,10,13
We observed a significant increase in the proportion of patients who were able to be discharged home following protocol implementation. There was no significant difference in length of stay, mortality and duration of mechanical ventilation, although our study was not adequately powered to detect differences in these secondary outcomes. Subgroup analysis of ventilated versus non-ventilated patients showed a larger treatment effect of the EM protocol in the ventilated group in terms of discharge to home. Having a higher severity of illness and longer duration of ICU stay, ventilated patients may stand to benefit more from EM. However, the generalisability and validity of these results are limited by small sample sizes in the non-ventilated group and the post hoc nature of the analysis and are therefore at best hypothesis generating.
The strengths of our study included the prospective and practical study design. Our wide inclusion criteria captured virtually all patients admitted to the medical and surgical ICUs during the study period. As a result, our study cohort is highly representative of daily ICU practice. In contrast to previous studies which specified the addition of dedicated staff to facilitate EM, we were able to implement our protocol with existing staffing numbers.10,17 This improves the sustainability of our intervention. We also allowed the attending physiotherapist to prescribe the most appropriate activity for the patient without requiring specific input from the attending intensivist, as opposed to a protocolised stepwise approach as in previous studies. The results of our study suggest that this approach is safe.
There were some limitations in our study. Firstly, it was non-randomised, instead comparing a non-matched pre and post-implementation group. Although the temporal gap between cohorts was only a few months, differences in outcomes due to secular trends in patient management that were unrelated to mobilisation practice cannot be excluded. The Hawthorne effect, that is the effect of being observed, may have introduced bias to the results, although the magnitude of its effect would be likely to have been similar in both the pre and post-implementation cohorts. APACHE II score data were used as a matter of convenience as scoring had already been implemented in our hospital for the calculation of standardised mortality rates. However, poor compliance with scoring meant data were not available for the majority of patients studied, making comparisons of illness severity between the pre and post-implementation groups unreliable, and may have been a potential confounding factor for the outcomes studied. Functional scores were also not recorded before and after the intervention studied, as follow-up after ICU discharge was done by review of hospital discharge records. Finally, our study involved a single centre with its own unique set-up and logistics, which may limit the generalisability of our results. Implementation of our protocol in other institutions will probably require adaptation to suit local needs and challenges.
Finally, our results were collected immediately following the implementation of the EM protocol, which involved a period of intensive training and education. It is hoped that these practices will be integrated into the standard protocol in our unit in a sustainable fashion. Regular education sessions on the EM protocol are ongoing, especially for staff new to our units. A repeat audit in one year is planned which will certainly be most informative.
Conclusion
The implementation of an EM screening and referral protocol in the ICUs in our institution was both safe and effective in increasing the mobilisation rate, with a low rate of adverse events. Our study reported an increase in the proportion of patients discharged home, which bears further study. However, barriers to effective mobilisation still exist, including administrative, logistical and personnel factors, and a lack of patient cooperation. These problems may be addressed by a systematic multidisciplinary approach involving intensivists, physiotherapists and nursing staff, as well as changing both staff and patient mindsets regarding mobilisation in the ICU through education.
Footnotes
Acknowledgements
The author(s) would like to thank the surgical and medical intensive care unit nursing staff Lau Yoke Yen, Xu Xu Hong, Deborah Heymamarini D/O Thiruselven, Win Win Moe, Chan Si Anwen, Malek Bin Amat and Abhishek Subodh Mhaisalkar for their contribution to the work, as well as Loo Chian Min (senior consultant, Head of Department of Respiratory and Critical Care Medicine) and Soh Chai Rick (senior consultant and director, Surgical Intensive Care Unit; Hyperbaric and Diving Medicine Centre) for their support and assistance. This material has been presented in poster format at the 39th International Symposium on Intensive Care and Emergency Medicine from 18 to 22 March 2019 in Brussels, Belgium.
Authors’ contributions
HVK, LXW and OHK researched the literature. HVK, KCHL, YHL, OHK and VP were involved in conception of the study, planning and protocol development. HVK and LXW obtained ethical approval for the study. OHK, VP and YHL were involved in patient recruitment and data collection. LXW, KBRL and LXY performed the data analysis. LXW wrote the first draft of the manuscript, and all authors reviewed and edited the manuscript and approved the final version.
Availability of data and materials
The datasets generated and analysed during the current study are available from LXW.
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval by the hospital’s institutional review board was obtained prior to study commencement.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Informed consent was not sought for the present study as waiver of informed consent was approved by the Singhealth CIRB based on ethical consideration.
