Abstract
Takotsubo cardiomyopathy usually occurs as a result of catecholamine release causing myocardial ‘stunning’ during physical or emotional stress. Typically coronary angiogram shows normal or minor coronary artery disease and echocardiogram shows apical ballooning with basal wall hyperkinesia. The prognosis is excellent with good cardiac functional recovery within days to weeks. We report the first case of takotsubo cardiomyopathy in a patient with acute-on-chronic liver failure.
Introduction
‘Broken heart’ or takotsubo cardiomyopathy is also known as stress-induced cardiomyopathy. It was first described by Dr Dote from Japan in 1991 following a case reviews of five patients presenting with typical chest pain accompanied by electrocardiogram (ECG) changes typical of acute coronary syndrome but with paradoxically normal coronary angiograms or minor coronary artery disease (<50% luminal stenosis). Typical echocardiogram findings are apical left ventricle hypokinesia (apical ballooning) with basal wall hyperkinesia. 1 Despite dramatic presentation, most patients recover fully with rapidly improving left ventricular function within days to weeks. Positive (happy heart syndrome) and negative (broken heart syndrome) stressors can both induce takotsubo cardiomyopathy. The proposed mechanism is not entirely clear but it is postulated that myocardial dysfunction is due to catecholamine release causing reversible myocardial ‘stunning’ during physical or emotional stress. 2 We report a case of takotsubo cardiomyopathy in a patient with acute-on-chronic liver failure (ACLF) with underlying hepatitis B liver cirrhosis.
Case report
A 66-year-old woman presented to our center with approximately two weeks history of lethargy and jaundice. She was known to have Child’s A hepatitis B liver cirrhosis but defaulted her nucleoside analogue over the last few months. Her other medical history included diabetes mellitus, hypertension, and hyperlipidemia. She was diagnosed with hepatitis B flare resulting in ACLF as defined by acute deterioration of pre-existing chronic liver disease, usually related to a precipitating event (hepatitis B flare in this context) and associated with increased mortality at three months due to multi organ failure. Her condition was complicated by hepatorenal syndrome, hepatic encephalopathy, and coagulopathy. On admission, her creatinine was 188 µmol/L (previously normal), bilirubin 255 µmol/L (peaked at 480 µmol/L), ALT 1160 U/L, AST 1660 U/L, and international normalized ratio (INR) 2.7 (peaked at 5.10). HBV DNA titer was 7.44 log (147,934,797 copies/mL). She was started on renal adjusted tenofovir for her hepatitis B infection. Her hepatic encephalopathy responded well to lactulose and she remained hemodynamically stable. Evaluation for liver transplant was initiated. However, subsequently on day 6 she developed chest pain and ECG (Figure 1) showed ST elevation in inferolateral leads V3–V6, II, and III and AVF suggestive of acute myocardial infarction.

ECG showing inferolateral ST elevation (a) that resolved within 1 week (b).
The cardiologist was activated immediately for possible percutaneous coronary intervention (PCI). Her initial troponin-T level was 275 ng/L and rose to 1480 ng/L 12 hours later. Her coronary angiogram revealed minor coronary artery disease (Figure 2). Transthoracic echocardiogram showed left ventricular ejection fraction of 40%, apical ballooning with normal basal wall contraction.
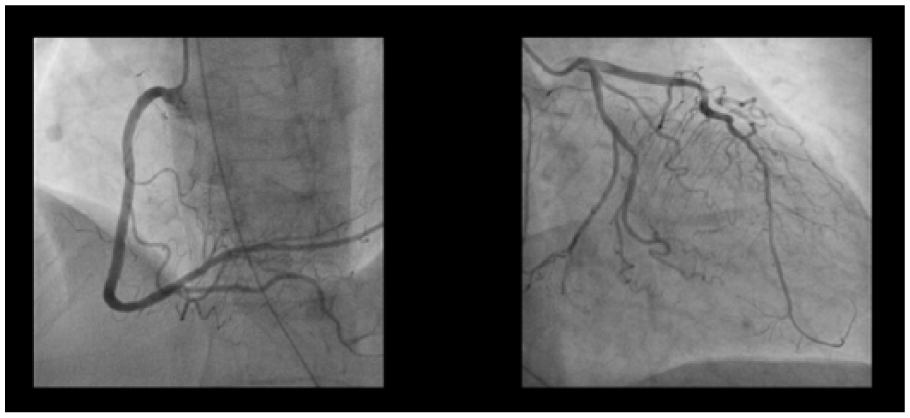
Coronary angiogram showing minor coronary artery disease in the patient.
A diagnosis of takotsubo cardiomyopathy was made based on her coronary angiogram and echocardiographic findings. A week later, repeat ECG showed resolution of ST segment and a repeat transthoracic echocardiogram also showed marked improvement in regional wall abnormalities. Unfortunately she passed away from severe ACLF (after 24 days of hospitalization) while awaiting deceased liver graft.
Discussion
ACLF has been gradually being recognized as an entity characterized by hepatic decompensation from an underlying chronic liver disease associated with organ failure that conveys high short-term mortality. 3 Mortality rate within 28 days has been reported in up to 50–80% of cases. Troponin-I elevation in acute liver failure (ALF) is observed in up to 60% of patient and its clinical significance has been disputed recently.4,5 The troponin-I elevation observed maybe related to metabolic stress rather than true myocardial injury. 6 Though studies of troponin-I elevation and its clinical relevance had been done in ALF setting, none have been reported in the context of ACLF. Intuitively, similar stress response can be expected in ACLF. Here, we report the first case of takotsubo cardiomyopathy in the context of ACLF. The prognosis of an acute coronary event differs greatly from that of takotsubo cardiomyopathy and has important implications for further management in such critically ill patients. Although our patient recovered from her takotsubo cardiomyopathy sufficiently to be listed for liver transplant consideration, she unfortunately subsequently succumbed to ACLF while awaiting liver transplantation.
In summary, catecholamine release mediated stress response can be expected in ACLF. It is likely that such stress response may further complicate clinical outlook in this group of patient. Nevertheless, thorough cardiovascular investigations should be performed in patients with liver failure suspected of having acute coronary event.
Footnotes
Acknowledgements
We thank HK Tan, PC Cheow, and RS Tan for contributing to the care of patients.
Declaration of Conflicting Interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Informed consent
From patient’s family.
