Abstract
With the rising application of chest CT scans, the detection rate of pulmonary nodules (PN) has witnessed a remarkable increase. Traditional Chinese Medicine (TCM) offers a unique method for the treatment and management of PN, with a strong focus on regulation of the body's overall balance and stopping disease progression. This systematic review aimed to identify evidence-based TCM formulae from both clinical research and authorized Chinese invention patents for the management of PN. Built on 69 original PN treatment formulae, the study unveiled the most commonly used TCM types and herbs in these formulae. These are tonic herbs, heat-clearing herbs, phlegm-resolving, cough-relieving and asthma-relieving herbs, as well as blood-activating and stasis-removing herbs. The frequently used herbs include Glycyrrhizae Radix et Rhizoma, Astragali Radix, Pinelliae Rhizoma, Fritillariae thunbergii Bulbus, Citri teticulatae Pericarpium, Platycodonis Radix, Ostreae Concha, and Poria cocos. To sum up and assess the therapeutic effects of TCM on PN, the study employed three indicators: nodule size changes (clinical efficacy), the Traditional Chinese Medicine Syndrome Score Scale (TCMSSS), and the malignancy risk assessment (Mayo Model Score, MMS). Compared to the control group with no pharmacological intervention, the treatment group delivered superior results across all three indicators. The clinical efficacy saw a P-value < 2.2 × 10−16 and confidence intervals of [0.2873004, 0.3595156], TCMSSS showed a p-value < 2.2 × 10−16 and confidence intervals of [0.5692573, 0.6422647], and MMS presented Z = -2.929 and a P-value of 0.0034. The overall clinical response rate of the treatment group was 40.43%, and the overall TCMSSS response rate was 76.95%. Additionally, after a comprehensive assessment, Bai Zhengping's Qingfei Sanjie Formula exhibited the most favorable overall therapeutic outcome in the treating of PN.
Keywords
Introduction
Pulmonary Nodules
With the growing use of low-dose chest CT in routine physical checkups, an increasing number of pulmonary nodules (lung nodules, PN) are being detected. PN is a type of interstitial lung disease marked by non-caseating necrotic epithelioid granulomas. Imaging typically shows focal, round, solid, or subsolid shadows, with higher density than surrounding lung parenchyma. These nodules are ≦3 cm in diameter, with no atelectasis, hilar lymphadenopathy, or pleural effusion. 1 The formation of PN is associated with various factors, including, but not limited to, age, smoking history, occupational exposure, family history, and environmental influences. 2 Globally, the CT detection rate of PN is around 30%, but varies by country.3–6 Chen et al reviewed 32 studies and included 24 in their meta - analysis. 7 The results showed a 27% overall prevalence of PN. While the incidence in males was slightly higher than in females, the difference wasn't statistically significant. PN is commonly detected in people aged ≧50 worldwide, with significant geographical differences in detection rates. Additionally, incidence increases considerably with age. Older adults are more susceptible to PN likely due to the combined effects of various factors, like age - related physiological changes, long - term environmental exposure, and pre - existing medical conditions.
The classification of PN is based primarily on four factors: quantity, size, density, and morphology. In terms of quantity, a single lesion is termed isolated, while two or more are considered multiple. Regarding size, nodules are categorized as mini (≤5 mm in maximum diameter), small (5-10 mm), medium (10-20 mm), and large (20-30 mm). Generally, the larger the nodule, the higher the likelihood of malignancy. When it comes to density, PN can be categorized into three types: solid nodules, partially solid nodules, and pure ground-glass nodules. Among these, partially solid nodules have the highest probability of malignancy, followed by ground-glass nodules and then solid nodules. PN can also be classified into several shapes, such as circular, lobulated, serrated, cavitary, and calcified. Lobulated and serrated nodules are frequently linked to malignancies. PN can be classified as either benign or malignant. At least 95% of all detected PN are benign. 8 Benign nodules may originate from infections, inflammation, or granulomatous diseases like pneumonia, tuberculosis, and fungal infections. In stark contrast, malignant nodules can be early signs of lung cancer. Most small PN are asymptomatic. However, as nodules grow, symptoms such as coughing, chest pain, breathing difficulties, fatigue, weight loss, anxiety, and insomnia may emerge. For benign nodules < 8 mm, initial management usually centres on observation and follow - up rather than immediate medical intervention. Malignant nodules or those exceeding 8 mm may demand more aggressive diagnostic and treatment strategies. 9 These strategies cover medical microbiological examination, biopsy, nuclear medicine evaluation, pharmacological intervention, surgical resection, stereotactic radiotherapy, ablation therapy, and other relevant procedures. In modern medicine, deciding on routine drug intervention for PN requires comprehensively evaluating the nodule's size, density, growth rate, etiology, and the patient's overall clinical condition. For PN caused by Mycobacterium tuberculosis, anti - tuberculosis drugs like isoniazid 10 and rifampicin 11 are usually prescribed. When PN results from bacterial infections, doctors often recommend antibiotics like ofloxacin and moxifloxacin.12–13 For PN linked to fungal infections, antifungal agents such as itraconazole 14 and fluconazole 15 are used. In cases of pulmonary sarcoidosis due to immune system dysfunction, physicians may prescribe immunosuppressants like methotrexate 16 and glucocorticoids such as dexamethasone 17 to control immune responses. If a patient has a severe cough, inhaled corticosteroids, particularly budesonide, 18 can help relieve symptoms and address airway hyper - responsiveness in sarcoidosis. If PN is diagnosed as malignant or is at high risk of malignancy, doctors may suggest anti - tumor therapies, including chemotherapy and targeted therapy, to reduce or eliminate the tumor.
Traditional Chinese Medicine
Originating in the Neolithic Age over 5000 years ago, Traditional Chinese Medicine (TCM), also known as Chinese Traditional Medicine, is an ancient medical system. TCM, with its holistic “unity of man and nature” view and dynamic dialectical thinking, systematically regulates the interplay between health and disease. TCM primarily aims to restore the body's natural balance and harmony. This goal is achieved through various therapeutic approaches such as herbal therapy, acupuncture, tuina massage, lifestyle modifications, and dietary interventions. TCM emphasizes the harmonious balance of Yin and Yang, the Five Elements, and Qi and blood. It also underscores the interconnections and coordinated functions among the Zang - Fu organs.19–20 In TCM theory, Yin and Yang are core concepts representing nature's and the body's opposing yet interdependent forces. The Five Elements—Metal, Wood, Water, Fire, and Earth—explain the complex relationships and changes in nature and the human body. Qi, blood, and body fluids are vital for sustaining human activities, with their smooth circulation and distribution crucial for health. TCM classifies internal organs into five Zang organs (heart, liver, spleen, lung, kidney) and six Fu organs (gallbladder, stomach, large intestine, small intestine, bladder, triple burner), all connected to body parts via the meridian system.
The TCM theoretical system has evolved over a long period. In early times, Chinese ancestors observed in daily life that certain plants and animals could treat specific diseases, starting the initial accumulation of TCM knowledge. “Huangdi Neijing” systematically explored human physiology, pathology, diseases, and treatment principles, forming a theoretical framework for TCM. Zhang Zhongjing's “Treatise on Cold Damage and Miscellaneous Diseases” established a comprehensive dialectical treatment system. Huangfu Mi's “Acupuncture Jiayi Jing” deeply explored the theories of viscera and meridians, laying the foundation for acupuncture and moxibustion principles. Li Shizhen's “Compendium of Materia Medica” was the world's first scientific classification of medicinal plants and animals, greatly advancing TCM theory and practice. As Western medicine emerged, scholars started exploring the integration of Chinese and Western medicine. The modern TCM industry has grown rapidly, with TCM now practiced in many countries and regions, becoming a key bridge for exchanging traditional Chinese and global medicines.
How TCM Treats Patients?
In TCM, the diagnostic process integrates four methods—observation, auscultation, inquiry, and palpation—into syndrome differentiation and treatment. Observation covers the patient's complexion, tongue coating, tongue texture, posture, movements, and mental state to assess qi, blood, yin, yang, and the illness's severity and nature. Auscultation involves listening to the patient's voice, breathing, cough, and hiccups to detect visceral function changes, while also evaluating body odor, breath, and excrement. Inquiry delves into the patient's medical history, including chief complaints, current issues, past medical history, personal and family history, as well as diet, sleep, bowel habits, and emotional changes. Palpation includes pulse diagnosis to identify pulse fluctuations, delays, and deficiencies, indicating the disease's location and nature, and assessing skin, hand, and foot temperature, along with abdominal softness and tenderness. From the information gathered via these four methods, a comprehensive analysis is conducted to determine the disease's etiology, location, and nature. Establishing the patient's syndrome type is fundamental to TCM treatment. Based on syndrome differentiation, treatment principles are set, treatment plans formulated, and appropriate therapies like herbal medicine, acupuncture, moxibustion, massage, and dietary therapy selected. Modern TCM combines these traditional diagnostic techniques with contemporary Western medical examinations, such as biochemical analyses and imaging studies, to achieve a more thorough understanding of the patient's condition.
TCM and PN
In ancient Chinese medical text, although the term “Lung Nodules” or “Lung Mass” were not explicitly mentioned, such conditions could be categorized under disorders such as “lung accumulation”, “cough”, “asthmatic disease”, or other syndrome patterns based on their clinical manifestations and characteristics. The term can be traced back to the Warring States period (475-221 BC) in China, when it appeared in the medical text “Nanjing: 54 Difficulties” written by the medical expert Bian Que. Patients with lung accumulation commonly exhibit symptoms like labored breathing, coughing, breathlessness, respiratory distress, discomfort and fullness in the hypochondriac area, and radiating pain in the back region. Ancient Chinese medical practitioners gradually deepened their understanding of the disease, suggesting it was usually caused by external pathogenic factors, internal organ dysfunction, emotional issues, and improper diet. These factors can result in stagnation of the lung qi, phlegm accumulation, and nodule formation. In the treatment of PN, ancient physicians advocated for a syndrome differentiation - based approach, with oral TCM administration being the most preferred method. In the Qing Dynasty medical text “Za Bing Yuan Liu Xi Zhu” by Shen Jin'ao, further clarification is provided on the pathological changes of lung accumulation. It explains that when pathogenic factors accumulate in the chest and block the airways, the smooth flow of energy is hindered. Regardless of whether it is phlegm, food, or blood, these substances can conflict with the body's healthy energy. If pathogenic forces dominate and healthy energy cannot overcome them, a mass will form. Ancient Chinese medical literature also records formulae for the treatment of lung accumulation. Ancient Chinese medical literature also documents formulae for the treatment of lung accumulation. “Tai Ping Sheng Hui Fang”, compiled by Wang Huaiyin et al, during the Northern Song Dynasty records several formulae for treating lung accumulation, such as Bing Lang Powder, Zi Wan Powder, and Zhi Shi Powder. In the Ming Dynasty, Wang Kentang's medical text “Zhengzhi Zhunsheng: Zabing” also notes the use of Da Qi Qi Decoction, which includes mulberry bark, pinellia, and apricot kernel, alongside Xi Ben Pill for treating lung accumulation. In modern times, with the revolutionary advancements in medical diagnostic techniques, TCM practitioners typically treat patients by integrating imaging and medical examinations with the clinical manifestations of conditions such as lung accumulation, cough, asthma, and other related symptoms. 21 For PN requiring follow-up observation, TCM may offer a low-risk and non-invasive alternative intervention. 22 In cases where PN requires surgical resection or chemoradiotherapy, TCM may serve as an adjuvant before and after Western medical treatments. It can reduce toxicity, enhance efficacy, improve patients’ quality of life, and potentially extend life expectancy. 23 Many people in China use TCM to treat diseases like PN, 24 because it has the potential to shrink nodules or even make them disappear. 25 The Expert Group in China, drawing on relevant literature and clinical experience, has classified the syndrome of PN into the following categories: qi stagnation and lung injury syndrome, cold phlegm obstructing lung syndrome, phlegm-heat accumulation in the lung syndrome, phlegm stasis and toxin accumulation syndrome, lung yin deficiency syndrome, and lung-spleen qi deficiency syndrome. 26 TCM practitioners prescribe effective formulas based on their assessment of the patient's symptoms and overall health status. The aim of the review study was to identify evidence-based TCM formulae derived from both clinical research and authorized Chinese invention patents for the management of PN.
Results
Some Selected Herbal Formulae and Their Composition
Many TCM treatment for PN are available in China. This study presents several original TCM formulae derived from 53 clinical research papers (T1-T53),27–79 and 16 authorized Chinese invention patents (P1[CN113908229B], 80 P2[CN114042124B], 81 P3[CN115381915B], 82 P4[CN115990224B], 83 P5[CN116036174B], 84 P6[CN116407600B], 85 P7[CN116270921B], 86 P8[CN116350695B], 87 P9[CN116570699B], 88 P10[CN116531465B], 89 P11[CN116898942B], 90 P12[CN116920066B], 91 P13[CN117482193B], 92 P14[CN118542906B] 93 P15[CN115252748B] 94 P16[CN118924865B] 95 ) for the treatment of PN. These formulae function as foundational treatments for PN or its specific subtypes, and can be tailored to individual patient symptoms.
The fundamental formulae and their compositions are shown in Figure 1. These 69 formulae are made up of 242 Chinese herbal medicines, which consist of 213 plant-based medicines, 23 animal-based medicines, 3 fungal-based medicines, and 3 mineral-based medicines. Unprocessed herbs accounted for 78.9% of 242 Chinese herbal medicines. Among these, P3 contained the highest number of Chinese herbal medicines, whereas P4, P5, and P9 contained fewer. Table 1 provides a comparison of the Chinese and Latin names, biological classifications, genera, sampling locations, and processing statuses of these Chinese herbal medicines. Table 2 presents the pharmacological classifications of Chinese herbal medicines appearing in these formulae at a frequency of four or more. The original and processed forms of each Chinese herbal medicine are combined into a single category. It contains 68 Chinese herbal medicine. Among them, Glycyrrhizae Radix et Rhizoma, Astragali Radix, and Pinelliae Rhizoma are the three most frequently used herbs. The pharmacological classification of these herbs in TCM mainly includes tonic herbs, heat-clearing herbs, phlegm-resolving, cough-relieving, and asthma-relieving herbs (PRCRARH), as well as blood-activating and stasis-removing herbs (BASRH).

Information on 242 TCMs Contained in 69 Formulae.

High-Frequency TCMs for the Treatment of PN.

Tonic Herbs
Tonic herbs are used to address qi, blood, yin, and yang deficiencies in the human body. These herbs can improve organ function, enhance physical fitness, boost disease resistance, and provide targeted supplementation and treatment for various deficiency syndromes. Tonic herbs have diverse pharmacological roles, including enhancing immune function, improving adaptability, stimulating the adrenal cortex, regulating metabolic processes, acting as cardiac stimulants, promoting hematopoiesis, enhancing overall physical performance, combating fatigue, treating deficiency syndromes, and strengthening the body's resistance to pathogenic factors. In TCM, qi tonics, such as Astragali Radix, 96 primarily address qi deficiency syndrome, characterized by symptoms such as fatigue, shortness of breath, reluctance to speak, and weak voice. In contrast, modern medicine typically attributes these clinical manifestations to anemia, nutritional deficiencies, or chronic fatigue syndrome. Yin tonics, such as Polygonati Rhizoma, 97 are used in TCM to treat yin deficiency syndrome, whose symptoms manifest as emaciation, dry mouth and throat, dizziness, and tinnitus. Modern medicine frequently attributes these symptoms to endocrine dysfunction, dehydration, electrolyte imbalance, chronic inflammation, and various other systemic disorders. The role of blood tonics, such as Angelicae sinensis Radix, 98 in TCM primarily involves the treatment of blood-deficiency syndromes. This syndrome manifests with pallor of the complexion, lips, and nail beds, accompanied by dizziness, blurred vision, insomnia, poor memory, and palpitations. By contrast, modern medicine often attribute these symptoms to hypovolemia and regional ischemia. The first condition can result from poor diet, excessive fatigue, or chronic illness. The second condition may be caused by hypoxia, localized edema, vascular stenosis, or blood disorders. In TCM, yang tonics, such as Epimedii Folium, 99 replenish the body's Yang energy and address conditions associated with Yang deficiency. Modern pharmacological research has confirmed that these herbs can improve sexual function, alleviate symptoms such as impotence and premature ejaculation, stimulate blood circulation in reproductive organs, and enhance sexual desire and capacity. Qi tonics were most commonly found in these 69 formulae, whereas yang tonics were relatively rare.
Heat-Clearing Herbs
In TCM pharmacology, heat-clearing herbs demonstrate broad therapeutic utility, primarily targeting pathogenic heat through multifaceted mechanisms. These include dissipating excess heat, detoxifying the body, cooling the blood, soothing the throat, promoting liver health, enhancing vision, strengthening the body, and dispelling pathogenic factors. Modern pharmacology has elucidated the diverse therapeutic actions of heat-clearing herbs, which include antimicrobial activity, antipyretic effects, anti-inflammatory actions, anti-tumor effects, immune regulation, sedative effects, cardiovascular benefits, and diuretic properties. Among the 69 types of Chinese herbal medicines mentioned above, heat-clearing herbs primarily include heat-clearing and toxin-removing herbs such as Hedyotis diffusae Herba, 100 as well as heat-clearing and blood-cooling herbs, such as Scrophulariae Radix. 101 In addition, there are specific herbs that fall under other subcategories of heat-clearing herbs. These include heat-clearing and dampness-drying herbs, such as Scutellariae Radix, 102 and heat-clearing and fire-purging herbs, such as Prunellae Spica. 103 The concept of “heat-clearing” in modern medicine encompasses various aspects, including anti-infective and anti-inflammatory effects, antipyretic properties, immune regulation, antitumor activity, cardiovascular effects, and diuretic functions. The concept of “toxin-removing” in modern medicine encompasses several aspects, including infection control, anti-inflammatory effects, immune regulation, endotoxin neutralization, antioxidant activity, metabolic detoxification, and toxicity-induced injury repair. The concept of “blood-cooling” in modern medicine encompasses multiple aspects, including reducing capillary permeability, stopping bleeding, regulating internal heat balance, affecting the blood system, and protecting the cardiovascular system. The concept of “dampness-drying” in modern medicine encompasses the regulation of digestive system function, alleviation of gastrointestinal symptoms, modulation of gut microbiota, improvement of metabolism, and anti-inflammatory effects, among other factors. The concept of “fire-purging” in modern medicine encompasses several aspects, including fever reduction, temperature regulation, anti-inflammatory effects, sedation, and blood pressure management. There is another category of heat-clearing herbs known as clearing deficiency-heat herbs, such as Artemisiae annuae Herba. 104 These herbs can be used to address persistent low-grade fevers and night sweats associated with chronic consumptive diseases, hot flashes, and night sweats resulting from decreased estrogen levels, as well as fever and palpitations due to autonomic dysfunction. Such herbs are seldom incorporated in the aforementioned anti-PN formulae.
PRCRARH
Based on their pharmacological actions, PRCRARH can be classified into three major categories: herbs that dissolve cold phlegm with warmth (HDCPW) (eg, Pinelliae Rhizoma), 105 herbs that clear and dissolve hot phlegm (HCDHP) (eg, Fritillariae thunbergii Bulbus), 106 and cough-suppressing and panting-calming herbs (CSPCH) (eg, Armeniacae Semen Amarum). 107 HDCPW is primarily used to treat symptoms, such as wheezing, excessive sputum production, white sputum, and thin sputum. HCDHP is mainly used for symptoms including excessive sputum, coughing, wheezing, and thick yellow sputum. CSPCH is primarily used to alleviate cough and asthma for various reasons. The three categories of herbs demonstrated varying degrees of effectiveness in resolving phlegm, suppressing cough, and calming asthma. HDCPW and HCDHP are particularly effective in resolving phlegm, whereas CSPCH is especially proficient in alleviating cough and asthma symptoms. The mechanism for resolving phlegm involves enhancing the secretion of bronchial glands, reducing mucus viscosity, and promoting the expulsion of sputum through coughing. The mechanisms for alleviating cough include inhibiting the medullary cough center, relieving bronchial smooth muscle spasms, targeting components of the cough reflex arc, reducing sensitivity to stimuli through anti-inflammatory actions, increasing respiratory tract secretions, and reducing mucus viscosity. The mechanisms for alleviating asthma include inhibiting the release and expression of pro-inflammatory mediators, reducing airway inflammation, relaxing bronchial smooth muscles to dilate the bronchi, alleviating airway constriction, improving pulmonary ventilation, promoting sputum expulsion, and exerting immunomodulatory effects. these mechanisms attenuate airway hyperresponsiveness. The pharmacological domains of PRCRARH include expectorant properties, cough suppression, asthma relief, antibacterial and antiviral effects, anti-tumor activity, anti-inflammatory benefits, diuretic effects, enhancement of blood circulation, and regulation of immune responses.
BASRH
Based on their therapeutic properties and clinical applications, BASRH can be categorized into the following groups: blood-activating and pain-relieving herbs (BAPRH) (eg, Chuanxiong Rhizoma), 108 blood-activating and menstruation-regulating herbs (BAMRH) (eg, Salviae miltiorrhizae Radix et Rhizoma), 109 blood-activating and mass-eliminating herbs (BAMEH) (eg, Curcumae Rhizoma), 110 and blood-activating and trauma-treating herbs (BATTH) (eg, Eupolyphaga sinensis Walker). 111 BASRH refers to specific herbs that can alleviate the symptoms associated with blood stasis by enhancing circulation and dispersing stagnant blood. The pharmacological domain of BASRH primarily includes antiplatelet aggregation, anticoagulation, enhancement of blood circulation, anti-inflammatory effects, antioxidant properties, promotion of tissue repair, modulation of the immune response, and improvement of capillary permeability. In TCM, BAPRH primarily alleviate various pain symptoms by promoting circulation of blood and qi, unblocking meridians, and dissipating blood stasis. Most BAPRH can improve blood rheology by reducing blood viscosity, decreasing platelet aggregation, preventing thrombosis and the formation of atherosclerotic plaques, and dilating the coronary arteries. The active ingredients of these drugs may provide analgesic effects by regulating targets and signaling pathways that inhibit pain-related neurotransmitters. In TCM, BAMRH is used to harmonize qi and blood and to unblock meridians, thereby alleviating symptoms associated with menstruation. Most BAMRH therapies enhance blood circulation, regulate endocrine function, relieve muscle spasms, reduce inflammation, and promote microcirculation. Collectively, these effects contribute to the normalization of the menstrual cycle and alleviation of menstrual discomfort. In TCM, BAMEH refers to herbs that promote blood circulation, eliminate blood stasis, and disperse concretions. These herbs demonstrate strong antiplatelet aggregation and anticoagulant properties, and are primarily used to treat various symptoms and conditions associated with blood stasis, including pain, tumors, and inflammation. In TCM, BATTH refers to a group of herbs used to alleviate symptoms such as pain, swelling, and functional disorders resulting from falls, injuries, blood stasis, and other related conditions. The primary effects of these herbs include promoting blood circulation and reducing stasis, decreasing swelling, relieving pain, facilitating wound healing, and restoring bodily functions.
Other Types of Herbs
In addition to the four primary categories of TCM used for the treatment of PN, various other types of Chinese herbal medicines are also utilized in therapy. These include qi-regulating herbs (eg, Citri reticulatae Pericarpium), 112 diaphoretic herbs (eg, Bupleuri Radix), 113 diuretic and dampness-excreting herbs (DDEH) (eg, Poria cocos), 114 liver-calming and wind-extinguishing herbs (LCWEH) (eg, Bombyx batryticatus), 115 and detoxifying, insecticidal, and anti-itch herbs (DIAIH) (eg, Gleditsiae Spina). 116 Qi-regulating herbs are well-known for their ability to improve gastrointestinal function, promote digestion, stimulate bile flow, relax bronchial smooth muscle, regulate uterine function, and exert specific effects on the cardiovascular system. These effects establish a pharmacological basis for the use of qi-regulating medications in the treatment of related symptoms and diseases. Diaphoretic herbs function through multiple mechanisms, including inducing sweating, reducing fever, alleviating pain, combating pathogens, exerting anti-inflammatory effects, and regulating the immune system. These actions establish the pharmacological basis for the treatment of related symptoms and diseases. DDEH are commonly used to relieve symptoms such as edema, oliguria, poor appetite, and restlessness. The properties of LCWEH have various regulatory effects on the nervous system. These effects include sedation, anticonvulsant properties, antiepileptic activity, and blood pressure-lowering effects, which collectively establish a pharmacological foundation for the treatment of associated symptoms and conditions. DIAIH are primarily manifested as diverse pharmacological effects, including antibacterial, anti-inflammatory, antiparasiticidal, and immunomodulatory effects. These effects provide a scientific foundation for the treatment of the associated symptoms and diseases.
Assessment of the Therapeutic Effects of Formulae
Assessment Items and Methods
Evaluation of the therapeutic effects of TCM on PN primarily focuses on three key aspects: clinical efficacy, TCM Syndrome Score Scale (TCMSSS), and malignancy risk assessment. The clinical efficacy of PN is classified into four levels: cured (disappearance of PN), markedly effective (reduction in the maximum diameter of PN by ≥50%), effective (reduction in the maximum diameter of PN by 25% to < 50%), and ineffective (reduction in the maximum diameter of PN by < 25% or increase in the diameter of PN). The TCMSSS serves as a reference standard for evaluating the therapeutic effects on PN in the context of TCM syndromes in China. This standard is included in Zheng's “Guidelines for Clinical Research on New TCM Drugs”.
117
The TCMSSS evaluates the therapeutic effects on TCM syndromes in patients both before and after treatment using a scoring system. The reference indicators included primary symptoms, such as cough and chest tightness; secondary symptoms, such as fatigue and weakness; tongue appearance; and pulse characteristics, with scoring items, scoring criteria, and point values determined by the researchers based on clinical practice. The therapeutic efficacy evaluated by TCMSSS is also classified into four levels: cured (a reduction of ≥90% in symptom scores), markedly effective (a reduction of ≥70% in symptom scores), effective (a reduction of ≥30% in symptom scores), and ineffective (a reduction of less than 30% in symptom scores). The Mayo model is a predictive tool designed to evaluate the likelihood of malignancy in PN.
118
It was used in this study. It estimates the risk of cancer in PN by analyzing both the clinical characteristics and imaging characteristics of the patients. Specifically, the model considered six independent factors: age, smoking history, history of extrathoracic cancer, size of the PN, presence of spiculation at the margin of the PN, and location of the PN in the upper lobe of the lung. Additionally, a case-control study was conducted over a period of three months, or 12 weeks. The case group received a basic formula with specific herbs added or omitted according to the individual symptoms of each patient throughout the study period, whereas the control group did not receive any medication or other physical treatments (some were given guidance on healthy lifestyle or psychological counseling; regular follow-ups are required). After three months, a chest CT scan was performed, and the therapeutic effects were evaluated using the three aforementioned criteria. The scope of clinical trial data collection was limited to the 69 data sources aforementioned. This study incorporated clinical data that met the criteria for three key aspects, as well as additional inclusion criteria. Clinical trial criteria that were inconsistent with the aforementioned criteria were excluded. In terms of clinical efficacy and TCMSSS, chi-square tests and P-value calculations were performed using R programming language, while the rest of the data were referenced from the original text. To assess malignancy using the Mayo model, the value of t-statistic or Z-statistic and P, as well as summarized data, were calculated using the R programming language, while the rest of the data were referenced from the original text. When the sample size is less than or equal to 30, a t-test is appropriate. However, when the sample size exceeds 30 and the population standard deviation is known, a Z-test is typically used. If the mean values of Mayo Model Score (MMS) before and after treatment are denoted as 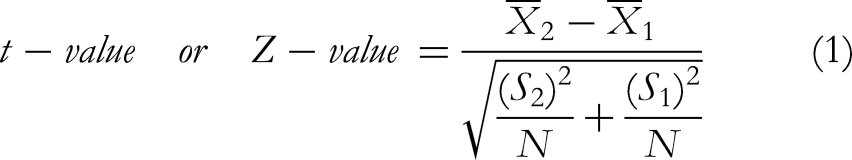
For the t-test, degrees of freedom was calculated as df = 2n−1. The two-sided P-values for t-value or Z-value can be computed using 2×pt(−∣t-value∣,df) or 2×pnorm(−∣Z-value∣). Because the MMS can be expressed using either the mean and standard deviation or the median and quartiles, and the former is more commonly used, the t-test or Z-test must be converted from the latter format to the former. Here is the translation of the estimation formula from the sample size (N), median (M), quartiles (P25, P75) to the mean (
Estimation of the mean:
1) For small sample sizes (N ≤ 25)
2) For small sample sizes (N > 25)
Estimation of the S:
1) For small sample sizes (N ≤ 15)
2) For small sample sizes (15 < N ≤ 70)
3) For small sample sizes (N > 70)
In summary, this study uses multiple group sample sizes (Ni), means (
Estimation method for overall mean: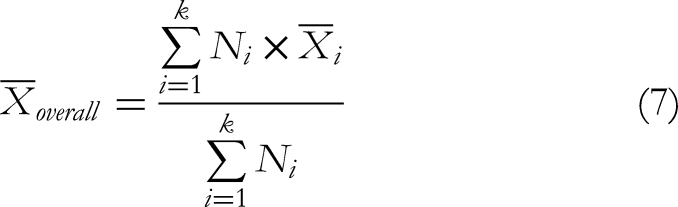
Estimation method for overall standard deviation: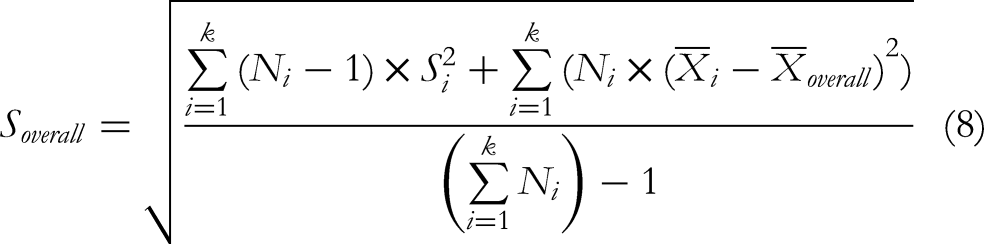
In the final MMS analysis, the overall means and standard deviations of multiple data groups before and after treatment were calculated. Next, a Z-test was performed, and the formula for calculating the Z-value is as follows:
After calculating the Z-value for a two-tailed test, this study used the pnorm() function in R software to obtain the corresponding P-value. Analytical results regarding clinical efficacy, TCMSSS, and MMS are presented in Tables 3, 4, and 5, respectively.
Comparison of Clinical Efficacy, Measured by Changes in maximum Nodule Diameter of Different Formulae for PN After Three Months of Treatment.

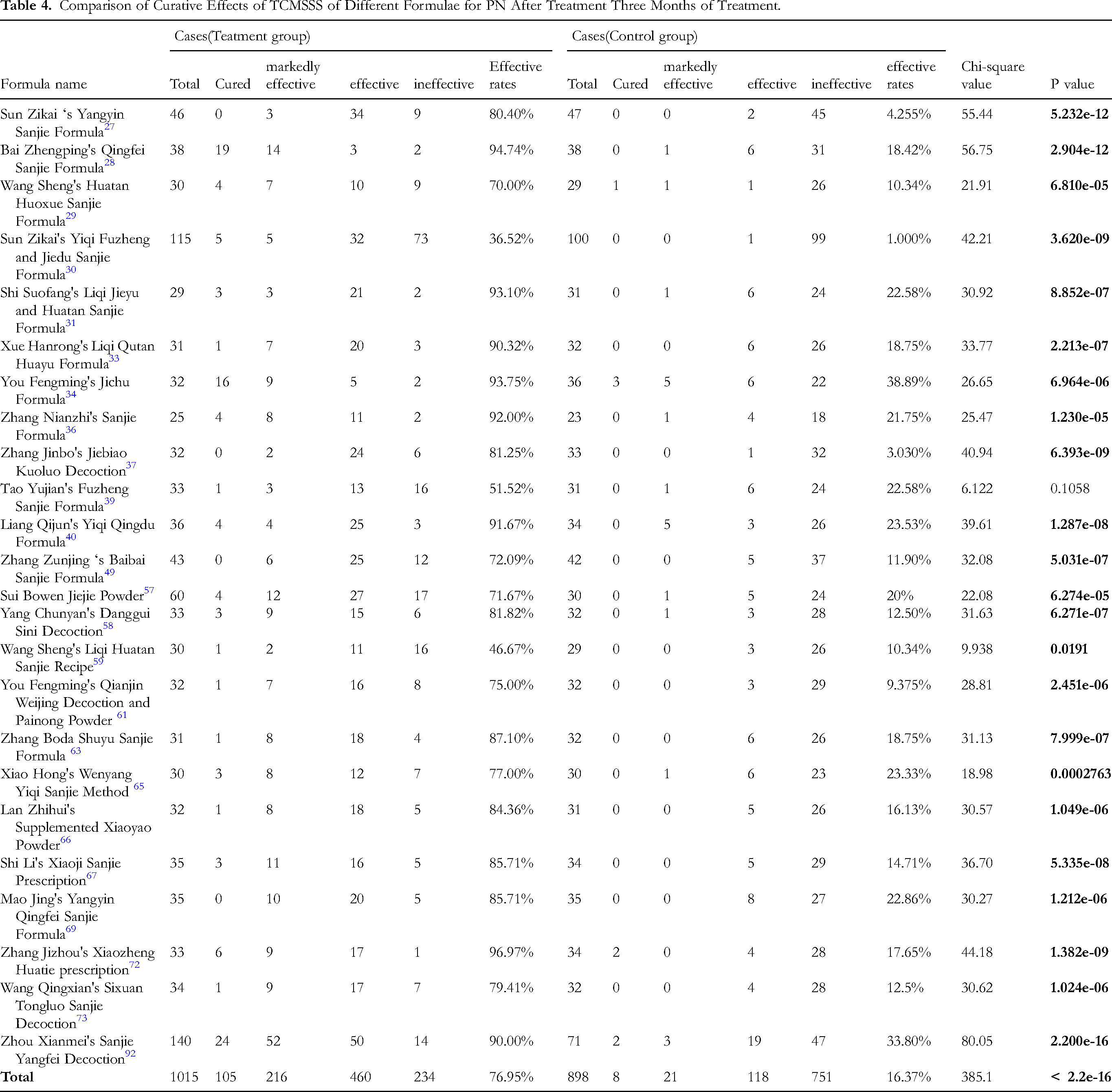
Comparison of Curative Effects of TCMSSS of Different Formulae for PN After Treatment Three Months of Treatment.
Assessment Clinical Efficacy
As shown in Table 3, the treatment group consisted of 1014 individuals, whereas the control group consisted of 902 individuals. In the treatment group, the cure rate was 9.961%, marked improvement rate was 8.580%, effective rate was 21.89%, and overall response rate was 40.43%. In the control group, the cure rate for PN was 0.8869%, with a marked improvement rate of 0.8869%, an effective rate of 6.319%, and an overall response rate of 8.093%. The two sets of data were compared using the chi-squared test, which yielded a P-value < 2.2 × 10−16. This result indicated a statistically significant difference, demonstrating that the treatment group was more effective than the control group in terms of clinical efficacy. In this study, the prop.test function in R (prop.test(c(410, 73), c(1014, 902), alternative = “two.sided”)) was used to calculate the confidence interval (CI) for the difference in the proportions of effective cases between the treatment and control groups. The results were as follows: chi-squared statistic = 263.11, df = 1, P-value < 2.2× 10–16, 95% CI: (0.2873004, 0.3595156). The above data indicate that the difference in proportions between the two groups was statistically significant, with the treatment group showing a significantly higher proportion of effectiveness than the control group, with the difference in proportions ranging from 28.73% to 35.95%. Then, we analyzed the heterogeneity of the Odds Ratio (OR, ad/bc) using the metabin function from the R package meta. The data included the number of effective cases in the treatment group (a), the number of ineffective cases in the treatment group (b), the number of effective cases in the control group (c), and the number of ineffective cases in the control group (d) for each formula. The results are as follows: The pooled OR was 8.31 (Common effect model, 95% CI: 6.2992-2910.9585), indicating a significant association between the treatment and the clinical outcome. Heterogeneity Measures: The H statistic was 1.16 (95% CI: 1.00-1.49), indicating minimal heterogeneity across studies. The I² statistic was 25.2% (95% CI: 0.0%–54.7%), suggesting that approximately 25.2% of the total variation in the OR is attributable to heterogeneity rather than chance. The Q statistic was 30.73, with degrees of freedom (df) = 23 and a P-value of 0.1295. The P-value of Q test was greater than 0.05, indicating no significant heterogeneity among the studies. Overall, the results suggest that there is no significant heterogeneity among the studies, which is consistent with the I² statistic. This indicates that the treatment effect was relatively consistent across studies. Figure 2 presents a forest plot depicting the heterogeneity analysis of the OR for clinical efficacy. Additionally, Wang Qingxian's Sixuan Tongluo Sanjie Decoction, 73 Bai Zhengping's Qingfei Sanjie Formula, 28 and Xiao Hong's Wenyang Yiqi Sanjie Method 65 ranked in the top three among the 24 formulae, with effectiveness rates of 82.35%, 78.95%, and 73.33%, respectively.

Assessment TCMSSS
As shown in Table 4, the treatment group consisted of 1015 individuals, whereas the control group comprised 898 individuals. In the treatment group, the cure rate was 10.34%, marked improvement rate was 21.28%, effective rate was 45.32%, and overall improvement rate was 76.95%. In the control group, the cure rate for PN was 0.8909% with a marked effectiveness rate of 2.339%, an effective rate of 13.14%, and an overall effectiveness rate of 16.37%. The two sets of data were compared using the chi-squared test, which yielded a P-value of less than 2.2 × 10–16. This result indicated a statistically significant difference, demonstrating that the treatment group had significantly better efficacy than the control group in terms of TCMSSS. Using the same calculation method (prop.test(c(781, 147), c(1015, 898), alternative = “two.sided”)), this study obtained relevant data for the CIs of the TCMSSS in both the treatment and control groups. The results were as follows: chi-squared statistic = 697.54, df = 1, P-value < 2.2× 10–16, 95% CI: (0.5692573,0.6422647). The above data indicate that the difference in proportions between the two groups was statistically significant, with the treatment group showing a significantly higher proportion of effectiveness than the control group, with the difference in proportions ranging from 56.93% to 64.22%. We then analyzed the heterogeneity of the OR. The results are as follows: The pooled OR was 23.55 (Common effect model, 95% CI: 17.9845-9830.8412), indicating a significant association between the treatment and the outcome. Heterogeneity Measures: The H statistic was 1.19 (95% CI: 1.00-1.52), indicating low levels of heterogeneity across studies. The I² statistic was 28.9% (95% CI: 0.0%–56.9%), suggesting that approximately 28.9% of the variability in the ORs can be attributed to heterogeneity rather than random chance. The Q statistic was 32.34, with 23 degrees of freedom and a P-value of 0.0933. The P-value of Q-test was greater than 0.05, indicating no significant heterogeneity among the studies. Overall, the results suggest that there is no significant heterogeneity among the studies, which is consistent with the I² statistic. This indicates that the treatment effect was relatively consistent across the studies. Figure 3 presents a forest plot depicting the heterogeneity analysis of OR for TCMSSS. Additionally, Zhang Jizhou's Xiaozheng Huatie prescription, 72 Bai Zhengping's Qingfei Sanjie Formula, 28 and You Fengming's Jichu Formula 34 ranked in the top three among the 24 formulae, with effectiveness rates of 96.97%, 94.74%, and 93.75%, respectively.

Assessment MMS
As shown in Table 5, the treatment group consisted of 563 individuals, whereas the control group comprised 501 individuals. In the treatment group, the overall mean and standard deviation (SD) of MMS before treatment were 0.0529 ± 0.0496, whereas the overall mean and SD of MMS after treatment were 0.0445 ± 0.0466. The two sets of data were compared using the Z-test, which yielded a P-value of 0.0034, indicating a statistically significant reduction in nodule malignancy. In the control group, the overall mean and SD of MMS before treatment are 0.0500 ± 0.0550, while the overall mean and SD of MMS after treatment were 0.0489 ± 0.0539. The two sets of data were compared using the Z-test, which yielded a p-value 0.749. This result indicated that there was no statistically significant difference, suggesting no change in nodule malignancy. In this part, R language was used to separately evaluate the CIs for the changes in the mean and SD in the treatment and control groups after the treatment course. The evaluation of the CI for the mean change involved first calculating the mean change, then the standard error, followed by the t-value (at the 95% confidence level with degrees of freedom n−1), and finally determining the upper and lower bounds of the CI. For the SD change, the CI was first calculated for the variance, with degrees of freedom set to n−1, followed by calculating the critical values of the chi-squared distribution using the qchisq function, determining the CI for the variance, and subsequently obtaining the CI for the SD by taking the square root. Finally, we calculated the CI for the change in SD. Based on the above data processing steps, this study obtained a 95% CI for the mean change in the treatment group (−0.0140338, −0.002766201), indicating that the mean MMS decreased by 1.403% to 0.2766% after treatment. The 95% CI for the SD change in the treatment group (−0.00698724, 0.0009872401) indicating that the SD of the MMS changed from 0.6987% to 0.09872% after treatment. In addition, this study obtained a 95% CI for the mean change in the control group (−0.007859535, 0.005659535), indicating that the mean MMS changed from −0.7860% to 0.5660% after treatment. The 95% CI for the SD change in the treatment group (−0.00588449, 0.00368449) indicated that the SD of MMS changed from −0.5884 to 0.3684% after treatment. In this study, we evaluated the heterogeneity of the mean (M) and SD values of MMS using the OR, and the means and variances before and after treatment were multiplied by 1000 for the analysis. The analysis produced the following results: IM² = 0.0% [0.0%; 55.0%], HM = 1.00 [1.00; 1.49], and QM = 5.47 (df = 13, p-value = 0.9634); ISD² = 0.0% [0.0%; 55.0%], HSD = 1.00 [1.00; 1.49], and QSD = 2.49 (df = 13, p-value = 0.9992). These results indicated no heterogeneity among the studies, suggesting a high level of consistency in the findings for both the mean and SD values of MMS. Forest plots of the heterogeneity analysis for the mean and SD using the OR are shown in Figures 4A and 4B, respectively. Additionally, Bai Zhengping's Qingfei Sanjie Formula, 28 Zhou Xianmei's Sanjie Yangfei Decoction, 92 and Niu Caiqin Jiawei-Loubei Erchen Decoction, 53 demonstrated greater efficacy in reducing nodule malignancy compared to the other 11 formulae.

A Comparative Analysis of the MMS Using various Formulae for PN Before and After Three Months of Treatment.

Discussion
An Exploration Based on Network Pharmacology of Potential Mechanisms of Bai Zhengping's Qingfei Sanjie Formula for the Treatment of PN
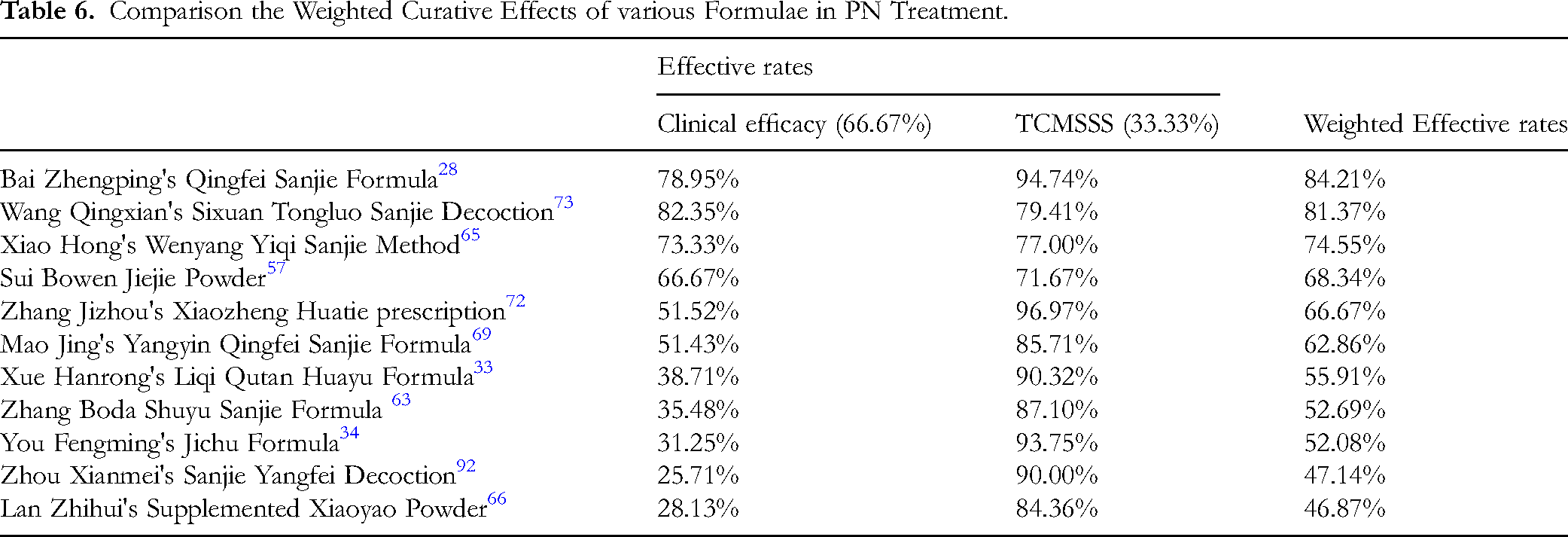
In this study, the therapeutic effects of various formulae on PN were assessed, with clinical efficacy weighted at two-thirds and TCMSSS weighted at one-third. Detailed data are presented in Table 6, where Bai Zhengping's Qingfei Sanjie formula (BZQSF) ranked highest The BZQSF formula exhibited notable efficacy, achieving a clinical efficacy rate of 78.95%, a TCMSSS of 94.74%, and a significant reduction in the MMS (from 0.046 to 0.026, P-value = 1.396e-106). Importantly, 42.11% of the nodules completely disappeared following treatment, with the average nodule diameter decreasing by 55.97% after treatment. Therefore, further investigation into its underlying mechanisms is warranted. The basic formula of BZQSF consists of the following 20 herbs: Ai Di Cha (Ardisiae japonicae Herba), Bie Jia (Trionycis Carapax), Gan Cao (Glycyrrhizae Radix et Rhizoma), Gua Lou Pi (Trichosanthis Pericarpium), Huang Qi (Astragali Radix), Huang Qin (Scutellariae Radix), Jin Yin Hua (Lonicerae japonicae Flos), Ju Geng (Platycodonis Radix), Lu Gen (Phragmitis Rhizoma), Ma Bo (Lasiosphaera Seu Calvati), Mi Pi Pa Ye (Honey-fried Eriobotryae Folium), Qian Hu (Peucedani Radix), Sang Bai Pi (Mori Cortex), Shan Ci Gu (Cremastrae Pseudobulbus), Tu Fu Ling (Smilacis Glabrae Rhizoma), Xia Ku Cao (Prunellae Spica), Xing Ren (Armeniacae Semen), Ye Gan (Belamcandae Rhizoma), Yu Jin (Curcumae Radix), and Zhe Bei Mu (Fritillariae Thunbergii Bulbus). Among the 20 mentioned herbs, Huang Qi, Gan Cao, and Bie Jia were classified as tonic herbs. Huang Qin, Lu Gen, Xia Ku Cao, Jin Yin Hua, Ye Gan, Ma Bo, Shan Ci Gu, and Tu Fu Ling are categorized as heat-clearing herbs. Ai Di Cha, Xing Ren, Mi Pi Pa Ye, Sang Bai Pi, Jie Geng, Qian Hu, Gua Lou Pi, and Zhe Bei Mu were grouped as PRCRARH. Yu Jin was identified as BASRH.
Comparison the Weighted Curative Effects of various Formulae in PN Treatment.
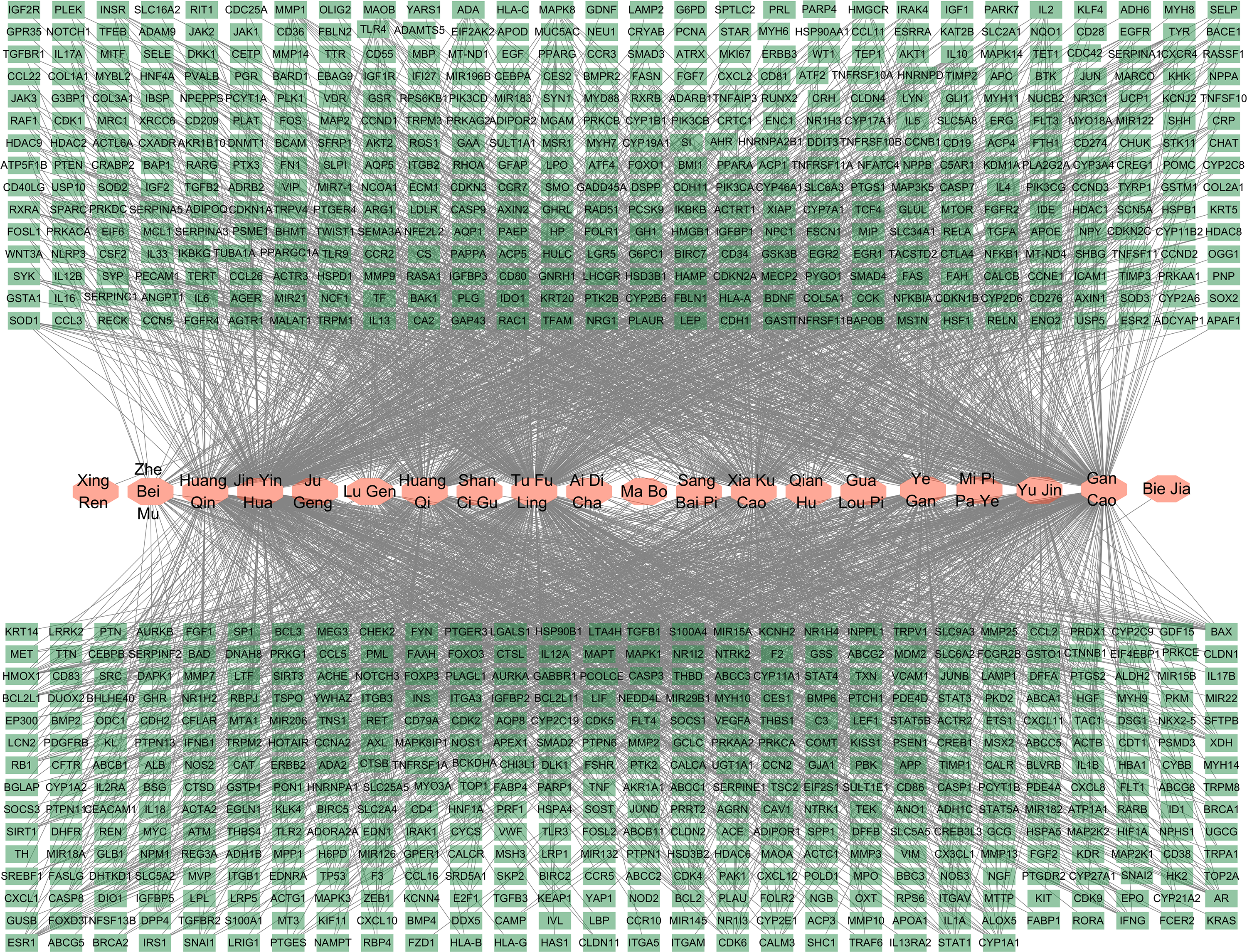
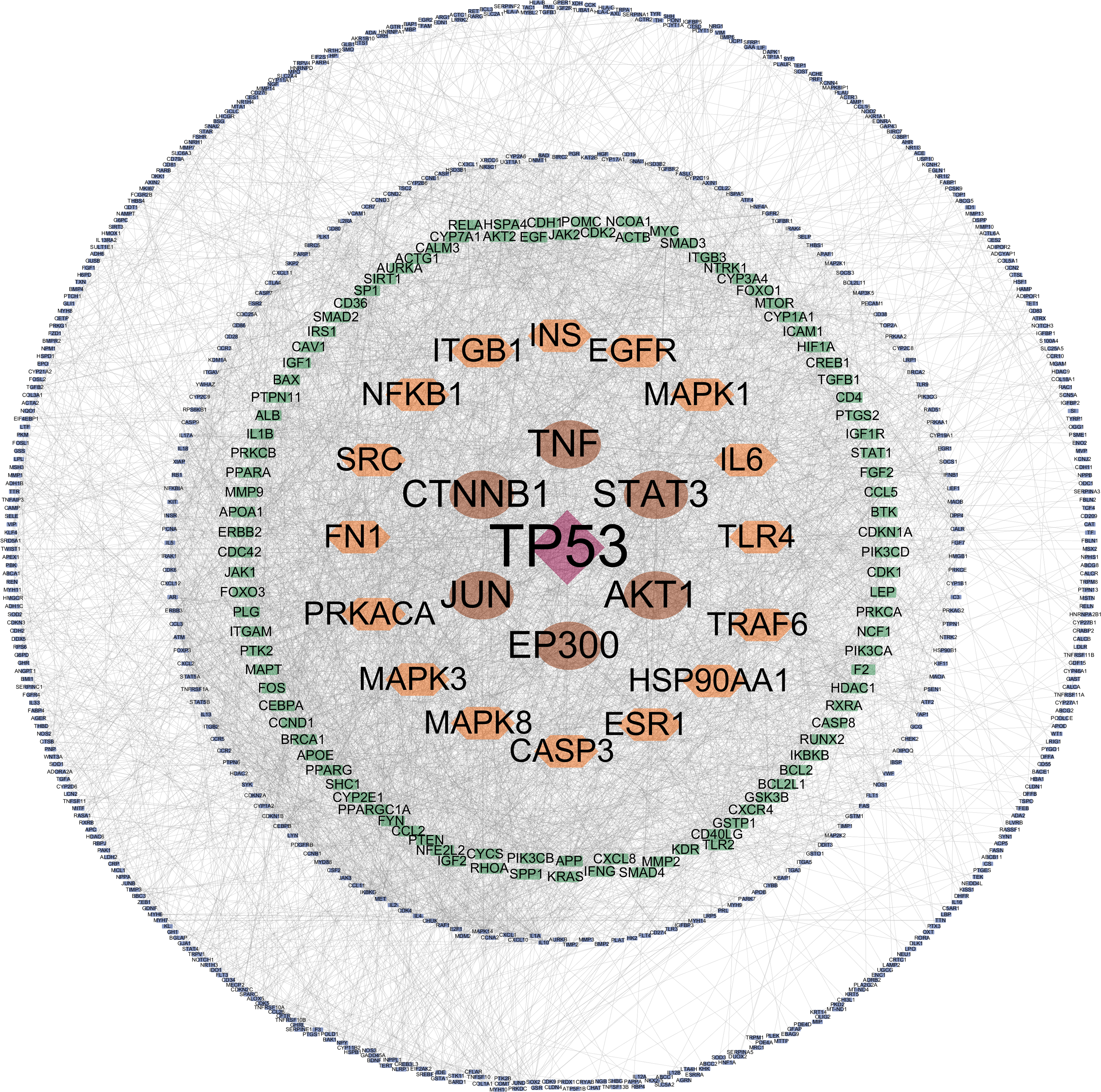
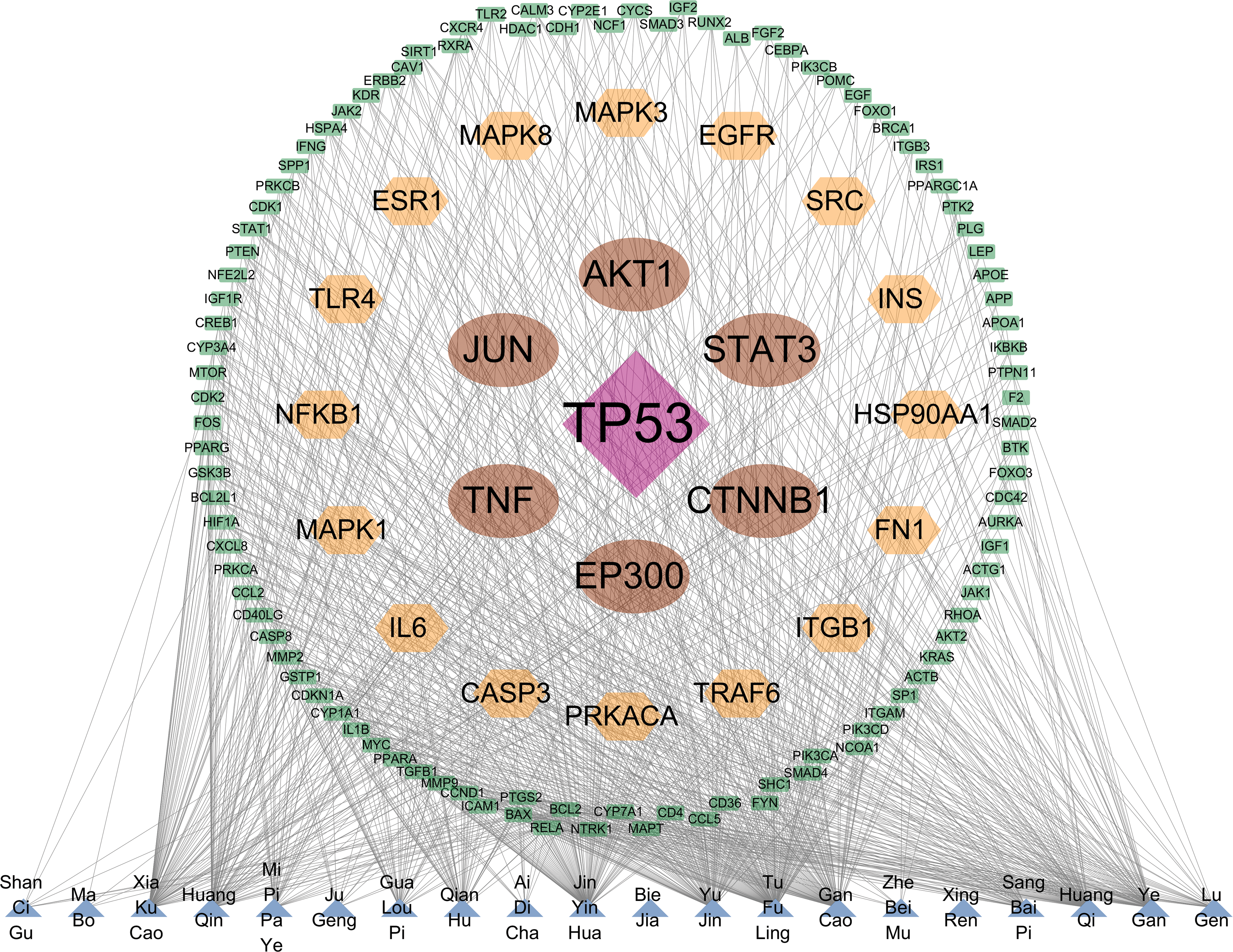
This study initially obtained the predicted targets of the aforementioned 20 Chinese herbs using the HERB and HIT databases. After merging these targets, 1411 drug targets were identified. Subsequently, disease targets for PN were retrieved from the GeneCards database using both “pulmonary nodules” and “lung nodules” as search terms. Following this merging process, 4699 disease targets were identified. Through Venn diagram analysis, we identified 835 overlapping targets representing potential therapeutic candidates (Figure 5). Subsequently, we constructed a comprehensive drug-target interaction network using Cytoscape software to visualize the relationships between these 835 potential therapeutic targets and their corresponding herbal compounds (Figure 6). For deeper network analysis, these 835 targets were imported into the STRING platform (with a stringent confidence score threshold of > 0.900) to establish a protein-protein interaction (PPI) network, which was subsequently refined by excluding unconnected nodes (Figure 7). The resulting PPI data were analyzed in Cytoscape using the CytoNCA plugin to calculate network topology parameters, including Degree and Betweenness centrality. Target prioritization was conducted through an iterative screening process in Excel, and nodes scoring above the average for both parameters were classified as higher-level targets, resulting in five stratified importance levels. The final optimized protein-protein interaction (PPI) network was constructed using Cytoscape to visually represent both the interaction relationships and the hierarchy of target importance (Figure 8). Based on the previously derived target grading data and the associations between targets and drugs, this study used Cytoscape to construct a network map illustrating the relationships between the 20 drugs and targets of grades 1 to 4 (Figure 9). Next, we performed systematic functional enrichment analysis of the 835 potential therapeutic targets using Metascape and conducted parallel Gene Ontology (GO) and Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway analyses. GO annotation covered three fundamental domains: biological processes (BP), cellular components (CC), and molecular functions (MF). For each analytical category, we extracted data from the top 20 most statistically significant terms (ranked by P-values) for subsequent visualization. Analytical metrics, including adjusted p-values, gene counts, and enrichment scores, were processed using the Bioinformatics platform to generate comprehensive bubble chart representations (Figure 10). Finally, this study utilized the downloaded enrichment analysis data to analyze the mapping relationships between the targets of grades 1–3 and the top 10 pathways with the lowest P-values. The results were imported into the Bioinformatics platform and visualized in the form as a chord diagram (Figure 11). Through network pharmacology analysis, this study identified the top core potential targets of the formula for treating PN as TP53, AKT1, STAT3, TNF, EP300, CTNNB1, and JUN. Furthermore, the key pathways involved in the therapeutic mechanism of this formula included the “hsa05200 Pathways in cancer” (P-value = 1e-100), the “hsa05417 Lipid metabolism and atherosclerosis” (P-value = 1e-100), and the “hsa04151 PI3K-Akt signaling pathway” (P-value = 1e-100).


Protein-Protein Interactions Network of Predicted Therapeutic Targets in Bai Zhengping's Qingfei Sanjie Formula. the Interaction Data Were Obtained from the STRING Database.


Chord Diagram Showing Associations Between Level 1-3 Core Target Proteins and the top 10 Significant Pathways (p-Value Ranked) in Bai Zhengping's Qingfei Sanjie Formula. the Full Names of the Corresponding Pathways can be Referred to in Figure 10.Pathway codes are displayed due to space constraints, with full names provided in Figure 10.
Discrepancy Between Imaging Improvements and TCM Symptom Relief
Based on the research findings, we observed a significant discrepancy between imaging improvement and TCM symptom relief in PN treatment. The overall average effective rate for nodule shrinkage was 40.43%, whereas the improvement rate for TCMSSS reached 76.95%. The discrepancy between imaging improvement (reduction in lesion size) and TCM symptom relief in the treatment of TCM PN may be attributed to multiple factors of mechanistic differences and evaluation limitations. From a mechanism perspective, Chinese herbal medicine may primarily stabilize lesions rather than induce rapid shrinkage by modulating the microenvironment (eg, inhibiting angiogenesis or regulating immune function), whereas antitussive and expectorant agents may improve respiratory symptoms independently of tumor biology. Regarding evaluation systems, current CT measurements lack sufficient sensitivity to detect subtle density changes, and traditional TCM symptom scoring lacks standardization, leading to discrepancies between objective imaging and subjective symptom assessments. Additionally, the inherent heterogeneity of nodules (eg, differing responses of inflammatory pseudotumors and malignant nodules to TCM) and individual metabolic characteristics (eg, CYP450 enzyme polymorphisms affecting drug metabolism) may contribute to variations in therapeutic efficacy.
Comparative Analysis of Clinical Differences Between TCM and Western Medicine in the Treatment of PN
The therapeutic mechanisms of TCM and Western medicine for PN differ significantly. TCM usesemploys a holistic approach, targeting multiple pathways to restore the body's yin-yang balance and organ function. In contrast, Western medicine focuses on specific etiological and pathophysiological mechanisms, utilizing targeted drugs with more direct but singular actions. In terms of efficacy, TCM demonstrates advantages in improving overall symptoms, enhancing quality of life, and reducing nodule recurrence. However, it may be less effective than Western medicine in rapidly shrinking or eliminating nodules. On the other hand, Western medicine can rapidly treat nodules with clear etiologies, such as bacterial infections or tuberculosis. However its effectiveness may be limited for complex or idiopathic nodules, and long-term use may be associated with certain adverse effects. In terms of suitability, TCM may be more appropriate for patients with weaker constitutions who cannot tolerate the adverse effects of Western drugs or those with complex conditions that respond poorly to monotherapy with Western medicine. For cases requiring rapid intervention and with well-defined etiologies, Western medicine remains the preferred treatment option.
Limitations of TCM in the Treatment of PN
Research on TCM formulae for PN has identified several limitations in their application. These limitations are evident in several aspects. First, standardization and quantification of TCM treatments for PN are challenging, which may hinder the assessment and comparison of their therapeutic effects. For instance, variations in the composition, dosage, and preparation methods of TCM formulas among individuals, making it difficult to uniformly evaluate treatment outcomes. Second, the interactions between TCM and modern medications are not fully understood, which may raising safety concerns. In clinical practice, the combined use of TCM and Western medicine should be approached with caution to avoid potential adverse reactions. Third, most TCM formulae are target specific TCM syndromes and lack universal applicability. However, there is a lack of standardized TCM diagnostic and treatment protocols for PN. The absence of standardized TCM syndrome criteria for the diagnosis and treatment of PN means that most approaches are derived from clinical practice and the experience of experts. Assessing treatment outcomes for PN is complex. Finally, evaluating the efficacy of TCM treatments should consider various imaging indicators, such as nodule size, shape, and density, as well as improvements in patients’ symptoms. Currently, there is a lack of standardized criteria for efficacy assessment.
This study outlines key strategies to address the limitations of TCM in PN treatment. To enhance standardization and quantification, the study recommends collecting commonly used TCM prescriptions for PN from different regions and schools, analyzing their composition, dosage, and preparation methods, and developing a standardized TCM prescription manual with clear processing guidelines for each herb. To improve the safety and enhance understanding of interactions in integrated TCM-Western medicine therapy, the study emphasizes the need to strengthening basic and clinical research to clarify drug interaction mechanisms and to develop evidence - based guidelines for combined treatment. Regarding efficacy evaluation, the study proposes forming a multidisciplinary expert team incomprising TCM practitioners, Western radiologists, and clinical pharmacologists to establish standardized efficacy assessment criteria for TCM treatment of PN. This includes assigning weighted values to different evaluation indicators based on their clinical significance for patient prognosis and therapeutic outcomes, and conducting long - term follow - up studies to optimize the timing of efficacy assessments.
Prospects for Future Research
Future research on PN treatment using TCM should focus on several key areas. First, more high-quality clinical trials are needed to evaluate the efficacy and safety of TCM in treating PN, particularly across different nodule types and sizes. Second, it is essential to further investigate the mechanisms of action of TCM in the treatment of PN. Third, based on existing research findings, efforts should be made to develop relatively standardized TCM treatment guidelines to enhance treatment consistency and reproducibility. Fourth, TCM should be integrated with other treatment modalities such as surgery, radiotherapy, and chemotherapy to improve overall therapeutic outcomes in PN. Finally, in the context of genomics and personalized medicine, further research should explore the potential of personalized TCM treatments. Targeted TCM treatment protocols can be developed based on the genetic characteristics and gene expression profiles of patients to improve therapeutic outcomes.
Conclusion
The overall advantages of TCM in the treatment of PN are summarized in several key points. TCM targets the pathological processes associated with PN through multiple components and therapeutic targets. It regulates organ function, promotes the circulation of qi and blood, and enhances disease resistance. It employs personalized treatment plans and syndrome differentiation, thereby enhancing the precision and effectiveness of the treatmenttherapy. TCM generally has fewer adverse effects, allowing for better patient tolerance during long-term use. The clinical efficacy of TCM has been demonstrated in several key areas. TCM can lead to shrinkage or even disappearance of PN in some patients. It has been shown to significantly relieve symptoms such as cough, chest tightness, and shortness of breath, thereby enhancing patients’ quality of life. It may also help reduce the malignancy potential of PN in certain individuals. However, limitations and challenges remain in the use of TCM for PN treatment. According to the data obtained in this study, the primary clinical efficacy of TCM in treating PN—specifically its ability to effectively reduce the size of these nodules—is limited. Moreover, there is a lack of high-quality clinical studies on TCM for PN treatment. In addition, there is a significant shortage of large-scale, multicenter, and randomized controlled trials to validate its efficacy and safety. In summary, the use of TCM in PN treatment warrants further investigation. It not only complements existing Western medical therapies but also offers potentially more personalized therapeutic options.
Methods
The study selected CNKI (https://www.cnki.net/), a comprehensive Chinese academic literature database, as the data source for literature analysis. The CNKI database can be used to search for both Chinese journals and doctoral and Master's theses. It also allows for the retrieval of English journal articles. However, some high-quality Chinese journal articles are duplicated in both the Chinese and English literature databases of CNKI. In accordance with the key concepts of this study, the search terms “Pulmonary nodules” and “Traditional Chinese Medicine” were strategically selected and used to conduct comprehensive literature searches within CNKI. Specifically, the initial search was conducted using the term “pulmonary nodule”, followed by a second search using the term “Traditional Chinese Medicine”. In the first round of searches, 7646 Chinese journal articles, 2424 doctoral and master's theses, and 17,136 journal articles in English literature database were identified. In the second round of searches, the number of articles was significantly reduced, and a total of 536 papers were retrieved. This included 329 Chinese journal articles, 200 doctoral and master's theses, and only nine journal articles in English literature database—seven of which were English-language articles and two were duplicate Chinese articles. A manual screening process was conducted in the third round of searches. This involved a careful review of abstracts to ensure that the studies focused specifically on clinical research involving TCM for PN. As a result, 470 studies that did not meet these criteria were excluded. The full texts of the remaining 66 papers were thoroughly examined. This process led to the exclusion of three papers due to content duplication, eight papers that involved non–Chinese medicine treatments, such as acupuncture or the use of more than one TCM therapeutic modality, and two papers that utilized multiple formulae for treatment. Ultimately, 53 studies were included in the final analysis. The literature screening process is shown in Figure 12. Given the strong originality of TCM invention patents, this study also searched for Chinese invention patents related to PN treatment using CNKI, identifying a total of 16 patents. This study used Cytoscape 3.9.1, a network visualization software, to create an association graph between formulae and the TCM herbs they contain. This study organized the information of TCM in the aforementioned formulae, mainly including their genera, medicinal parts, and whether they were processed through the China Medical Materials Information Platform (https://www.dayi.org.cn/). Finally, based on the therapeutic efficacy data from the aforementioned papers and patents, this study used the R software to evaluate the therapeutic effects of TCM on PN using a case-control method, including changes in nodule size, TCMSSS, and nodule malignancy. Due to the limited data on the therapeutic efficacy of TCM in treating PN, and variations in research methods, this study retained only the most commonly used method and consolidates the data accordingly. For example, 10 items were listed in the evaluation of nodule size, 10 in the TCM symptom scores, and 6 in the changes in nodule malignancy. For analyzing changes in nodule size and TCMSSS, this study used the chi-squared test. For changes in nodule malignancy, the statistical method employed in this study was a t-test or Z-test.
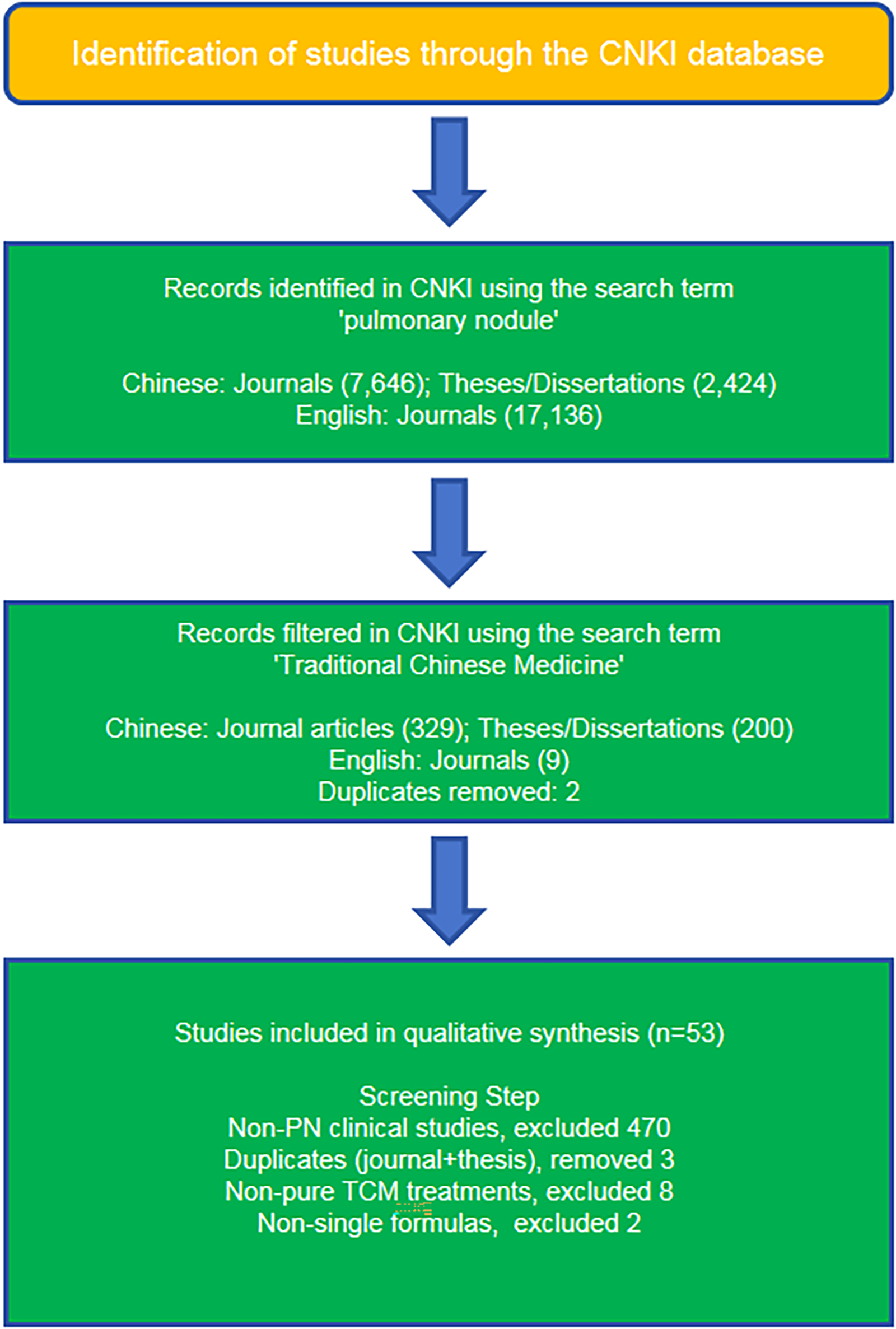
Literature Screening Flowchart for 53 Core Publications on Data Mining of TCM Formulas Used in Pulmonary Nodule Treatment.
Network pharmacology is an emerging interdisciplinary field that maps complex networks linking drugs, targets, and diseases, using database and software tools. By leveraging systems biology and advanced network analysis techniques, it elucidates the mechanisms of drug action, identifies potential therapeutic targets, and predicts drug synergies. This study aimed to employ network pharmacology to explore the potential mechanisms of the most effective TCM formula for treating PN. The databases used for herbal target prediction in this study were HERB (https://herb.ac.cn/) and HIT (http://hit2.badd-cao.net/). The GeneCards database was used for disease target prediction (https://www.genecards.org/). The Venn diagram were generated using Venny 2.1 (http://www.liuxiaoyuyuan.cn/). PPI analysis was performed using the STRING database (https://cn.string-db.org/). Gene enrichment analysis was conducted using Metascape (https://metascape.org/). Bubble plots for enrichment analysis and chord plots for pathway–target relationships were generated using the Bioinformatics platform (https://www.bioinformatics.com.cn/). Network analysis and visualization were performed using Cytoscape 3.9.1. Data processing was performed using Excel 2007.
Footnotes
Author Note
All data generated or analyzed during this study are included in this published article and its supplementary information files. The type of this article is a review. This study did not involve human, animal, or cellular experiments. The data comes from papers, patents, and databases, and does not address issues related to patient ethics. Therefore, this study did not require approval from an the ethics committee.
Ethical Considerations
The type of this article is a review. This study did not involve human, animal, or cellular experiments. The data comes from papers, patents, and databases, and does not address issues related to patient ethics. Therefore, this study did not require approval from an the ethics committee.
Funding
This research was supported by the doctoral research start-up fund project of Xianyang Polytechnic Institute of People's Republic of China, “Application of information and automation technology in biological medicine” (2021BK07).
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability
All data will be made available by the authors upon reasonable request.
