Abstract
20(S)-protopanaxadiol (PPD) is an active natural product which is transformed from protopanaxadiol-type ginsenosides. The present study was conducted to evaluate the effects of PPD on myocardial ischemia/reperfusion (I/R) injury in a rat model. PPD (20mg/kg) or positive-control drug Diltiazem (10mg/kg) was administered daily for 7 days before left anterior descending I/R operation. After 2-hour reperfusion, changes of cardiac morphology, structure, and function were evaluated by HE staining and echocardiography. Myocardial infarct size was assessed using nitroblue tetrazolium staining. The activities of cardiac enzymes in serum were also evaluated. Cardiomyocyte apoptosis was detected using the terminal dUTP nick end labelling (TUNEL) assay. The extent of oxidative stress was evaluated according to the activities of superoxide dismutase (SOD) and glutathione per oxidase (GPx) and the levels of malondialdehyde (MDA). Western blot and immunohistochemistry were used to determine the expression of apoptosis associated proteins, including Bcl-2, Bax, cleaved Caspase-3, cleaved Caspase-9, and cytochrome C. According to the results, PPD reduced I/R‑induced increases in myocardial infarct size and improved cardiac function. Furthermore, PPD decreased cardiomyocyte apoptosis on TUNEL staining, which was verified by increased Bcl-2, and decreased expression of Bax, cytochrome C, cleaved Caspase-9, and cleaved Caspase-3 in I/R rat myocardium. Additionally, PPD reduced MDA levels and increased the anti-oxidative capacity by upregulating the activities of SOD and GPx. Taken together, the results suggest that PPD serves a protective role against oxidative stress and cardiomyocyte apoptosis during myocardial ischemia/reperfusion injury.
Keywords
Acute myocardial infarction (AMI) is currently the leading cause of mortality and morbidity worldwide, which results from the acute occlusion of one of the major coronary arteries. In this scenario, the recommended treatment strategy to limit the size of the myocardial infarct is the timely restoration of coronary blood flow, by either intravenous thrombolysis or primary percutaneous coronary artery angioplasty. Despite these current reperfusion strategies applied in a timely manner, the mortality of treated patients still reaches 10%. 1,2 The poor prognosis of AMI is usually attributable to the ischemia-reperfusion injury (I/R), thus necessitating the development of novel cardioprotective strategies, which can be used as adjunctive therapy to the current reperfusion strategies.
There are several theories mechanisms have been proposed to contribute to IR injury: oxidative stress, iron mobilization, and Ca2+-overload. 3 The level of myocardial tissue oxygenation increases following restoration of blood flow, which is initiated with a burst of reactive oxygen species (ROS) generation. Excessive ROS lead to deregulation of cellular ion homeostasis, and apoptosis with consequent inflammatory responses. 4,5 Therefore, manipulating oxidative stress induced secondary injury might be a promising strategy to prevent I/R injury.
20(S)-protopanaxadiol (PPD, chemical constitution showed in Figure 1) is an active natural product which is transformed from protopanaxadiol saponins (eg., Rb1, Rb2, Rb3, Rc, and Rd). PPD has been widely reported to possess pleiotropic anticancer activities in various cancers. Our previous studies revealed the protective effects of protopanaxadiol saponins against cerebral ischemic injury and AMI in rats, the mechanisms were associated with the inhibition of oxidative stress and apoptosis. 6,7 Furthermore, the cardioprotective effects of Rb1, Rb2 and Rb3 were proved by our studies. 8 -10 But as the active metabolite of these ginsenosides, the effects on myocardial ischemia-reperfusion injury of PPD are still unclear.

The chemical structure of PPD. Downloaded from PubChem (pubchem.ncbi.nlm.nih.gov), CID 11213350.
Diltiazem (DLZ) is an oral and parenteral non-dihydropyridine calcium channel blocker, which is widely used in the therapy of angina pectoris and arrhythmias. Previous studies have reported that DLZ demonstrated cardioprotective effects and contributed to further mechanisms related to reducing oxygen stress damage, reduce myocardial cell injury, apoptosis induced by ischemia reperfusion and myocardial infarct size. 11 -13 Therefore, DLZ was selected as a positive control in the present study.
The objective of this study was to identify the cardioprotective effects of PPD on myocardial ischemia-reperfusion injury in rats, particularly its effect on reducing oxidative stress and apoptosis.
Materials and Methods
Reagents
PPD, white powder, provided by Hainan Asia Pharmaceutical Co., Ltd. (Haikou, China), purity >95%, was suspended in 0.5% sodium carboxymethyl cellulose solution for use. DLZ was purchased from Tianjin Tanabe Seiyaku Co., Ltd, grinded and suspended in 0.5% sodium carboxymethyl cellulose solution for use. All other chemicals were analytical reagents.
Animals and Myocardial I/R Model
Male Wistar rats (200, 250 g) were obtained from the Liaoning Changsheng Biotechnology co., Ltd. The rats were maintained with standard feeding conditions including adequate food and water ad libitum, a 12 hours light/dark, 20 to 25˚C and 50% to 65% humidity.
All of 60 rats were randomly divided into 4 groups (n = 15 each group) and treated as follows: (1) the Sham surgery group, treated with same volume of vehicle; (2) the I/R model group, treated with same volume of vehicle; (3) the PPD group, treated with PPD dose of 20 mg/kg; (4) the positive-control group, treated with DLZ at dose of 10 mg/kg. The drug or vehicle treatment was administered once a day for 7 consecutive days. 30 minutes after the final treatment, the rats were anesthetized for surgery. Following skin incision, the hearts were exposed through a left thoracic incision in the fourth intercostal space. A 6‐0 silk suture with a slipknot was placed around the left anterior descending coronary artery. The slipknot was loosened after 30-minute occlusion, which was followed by 2 hours of reperfusion. The same surgical procedures without ligation were performed on rats in sham group.
Echocardiography
After 2 hours reperfusion, transthoracic echocardiography was performed for assessment of cardiac function using a standard setting with a 10S scan head (GE Vivid-I, GE Healthcare, USA). Animals were anesthetized with Pentabarbital Sodium (30 mg/kg, intraperitoneally) and placed supinely on a heating pad to maintained body temperature. Two dimensional and M-mode echocardiographic measurements were conducted. Then M-mode images were acquired at a sweep speed of 100 mm/s and stored digitally. Following this, left ventricular fractional shortening (FS) and left ventricular ejection fraction (EF) were calculated automatically by the equipment.
Measurement of Infarct Size
To measure myocardial infarct size, the hearts were cut into 5 hoursorizontal slices and incubated at 37 ˚C for 10 minutes in a 5% solution of buffered nitroblue tetrazolium staining (NBT). In the presence of intact dehydrogenase enzyme systems, the normal myocardium stained dark blue by NBT, but the necrotic zone unstained because of the dehydrogenase lack. 14 The slices were photographed and analyzed by Image Pro-Pus 6.0 (Media Cybernetics, USA). The infarct rate was calculated as infarcted myocardium size divided by total myocardium slices size, and expressed as a percentage.
Assessment of Serum Cardiac Enzymes
Blood samples were collected from the abdominal aorta, and then centrifuged at 2,000 × g for 10 minutes at 4 °C.The serum obtained was assayed for the activity of cardiac enzymes [creatine kinase-MB (CKMB) isoenzyme, aspartate transaminase (AST) and lactate dehydrogenase (LDH)]. The activity levels of CKMB, AST and LDH were detected using the assay kit (Nanjing Jiancheng Bioengineering Institute, Nanjing, China) and follow the protocol provided by the manufactures.
Histopathological Staining and Examination
Heart tissue samples were obtained and fixed in 4% buffered paraformaldehyde solution, and then embedded in paraffin to section. 3-μm-thick paraffin wax sections were mounted on slides, which were dried for 30 minutes in an oven (60 °C), dewaxed in xylene and hydrated with gradient alcohol. Hydrated sections were stained with hematoxylin and eosin (HE) for histopathological examination. TdT-mediated dUTP Nick-End Labeling (TUNEL) staining was performed according to the protocol provided by the In Situ Cell Death Detection Kit, POD (Roche Ltd., Basel, Switzerland). The stained sections were examined and photographed by light microscopy (Nikon Eclipse 80i; Nikon Corporation, Tokyo, Japan). The Image Pro-plus 6.0 Software was used to analyze the photomicrographs of the TUNEL, and the apoptosis rate of cardiomyocytes was presented as the percentage of total cells counted. 4',6-diamidino-2-phenylindole (DAPI) staining was chosen for counting total cells.
Biochemical Assays
To assess the extent of oxidative stress, the activity of superoxide dismutase (SOD) and glutathione peroxidase (GPx), the content of malondialdehyde (MDA) in heart tissue were measured. Heart tissue samples were homogenized in PBS, and centrifuged at 12,000 g for 5 minutes. The supernatant was assayed using SOD Activity Assay Kit (Beyotime, Shanghai, China) and Total GPx Assay Kit (Beyotime, Shanghai, China). Heart tissue samples were homogenized in RIPA lysis buffer and centrifuged at 12,000 g for 10 minutes for MDA content assay using Lipid Peroxidation MDA Assay Kit (Beyotime, Shanghai, China).
Immunohistochemistry
After conventional dewaxing and hydrated, Immunohistochemistry staining was performed with an immunohistochemistry kit (ZSGB-BIO, Beijing, China) according to the manufacturers protocol. The slides incubated in Cytochrome C antibody (1:200, CST, MA, USA) for 12 hours at 4 °C. After DAB and hematoxylin staining, the slides were dehydrated, cleared with xylene, mounted with permanent mounting medium, then photographed by light microscopy. Finally, the pictures were analyzed by Image Pro-plus 6.0 software.
Western Blot Analysis
The protein of the left ventricles was separated by sodium dodecyl sulfate-polyacrylamide gel electrophoresis and then transferred to the polyvinylidene difluoride membranes using an electrophoretic transfer system. The membranes were blocked for 1 hours with 5% nonfat dry milk at 37 °C and incubated overnight at 4 °C with primary antibody. The primary antibodies were as follows: anti-Bax (1:1000, Abcam, Cambridge, UK), anti-Bcl-2 (1:1000, Abcam, Cambridge, UK), anti-cleaved Caspase-3 (c-Cas3, 1:1000, Abcam, Cambridge, UK), anti-cleaved Caspase-9 (c-Cas9, 1:1000, Abcam, Cambridge, UK) and GAPDH (1:2000, ZSGB-BIO, Beijing, China). The membranes were washed 3 times in TBST, and then incubated 1 hours with goat anti-rabbit secondary antibody (1:2000) at 37℃. The blots were visualized using an enhanced chemiluminescence (ECL) reagent (Tanon, Shanghai, China) and scanned with multiple exposure times to achieve an optimal signal in the Gel Image Analyzing System (Tanon-4200, Shanghai, China). The density of the immunoblot bands was analyzed by the Image J Software.
Statistical Analysis
All data were expressed as mean ± SEM. SPSS 22.0 Statistical Software was used for the analysis, and the statistical significance of the data was determined using one-way analysis of variance (ANOVA) followed by Dunnett’s test. < 0.05 was considered as statistically significant.
Results
PPD Improves the Cardiac Function in I/R Rats
After 2 hours reperfusion, echocardiography showed that LVIDs and LVIDd were significantly increased in I/R group compared with sham group (P < 0.01). Meanwhile, EF% and FS% were significantly decreased in I/R group (P < 0.01). Pretreatment with PPD or DLZ significantly recovered LVIDs, LVIDd, EF and FS, indicating that PPD improved cardiac function in I/R rats (Figure 2).
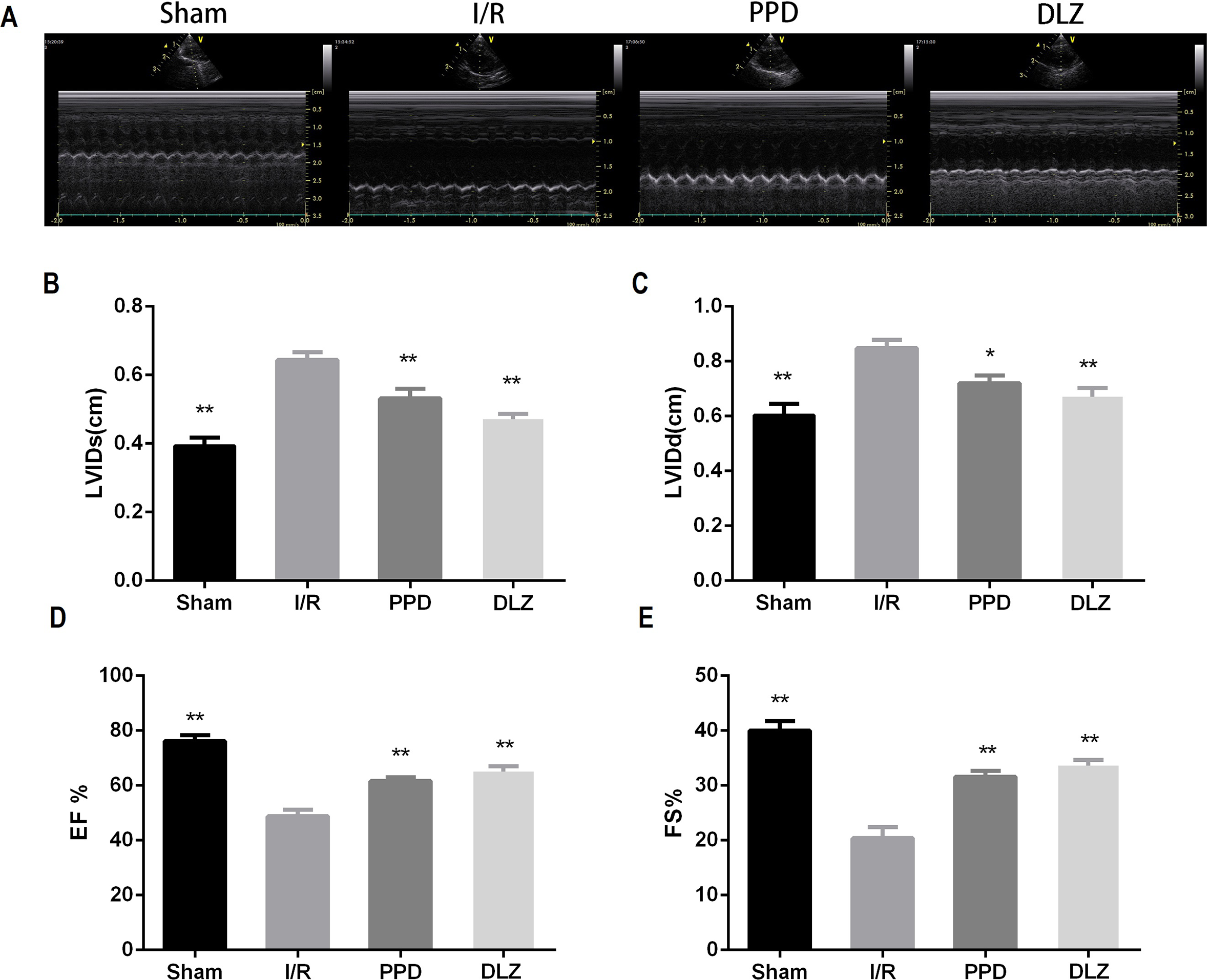
Changes in cardiac function of rats. A, Representative echocardiographic M-mode records; B-E,LVIDs (B), LVIDd (C), EF% (D) and FS% (E) of rats following reperfusion. Data are expressed as mean ±SEM, n = 6. **P < 0.01 and *P < 0.05 vs. I/R group.
PPD Reduces Infarct Size in I/R Rat Heart
The infarct size was observed by NBT staining (Figure 3). Compared with Sham group, there were obvious lesions found in I/R rat hearts. Statistical analysis revealed that myocardial infarct size in PPD and DLZ group were significantly reduced compared with I/R group (P < 0.05).
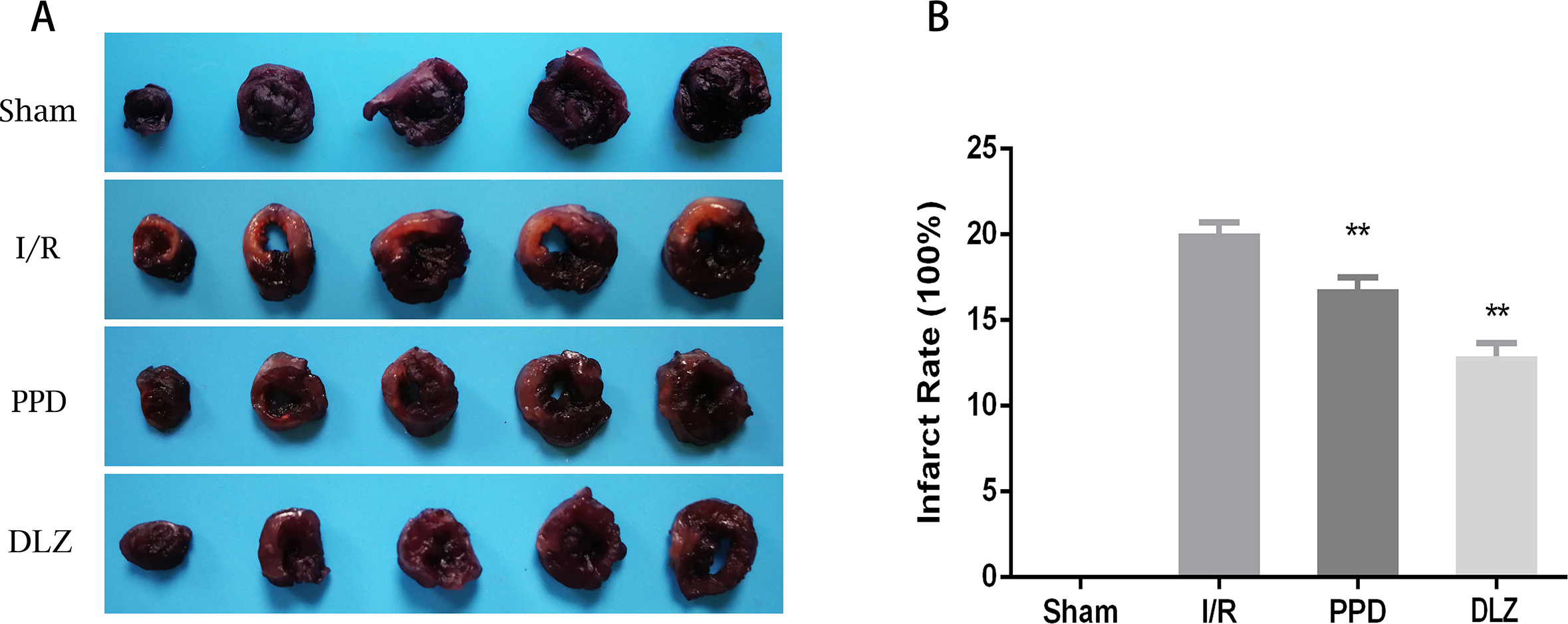
Myocardial infarct size of rats. A, NBT staining graph; B, Statistics of infarction area results. Dataare expressed as mean ± SEM, n = 4. **P<0.01 and *P<0.05 vs. I/R group.
PPD Facilitates the I/R Induced Increase in LDH, AST and CKMB in Rat Serum
Serum LDH, AST and CKMB levels were detected to evaluate myocardial injury induced by I/R. Compared with the sham group, LDH, AST, and CKMB activities in I/R model group were significantly increased (P < 0.01), Whereas the activities of LDH, AST, and CKMB were significantly decreased in PPD and DLZ group compared with the I/R model group (P < 0.05) (Figure 4).
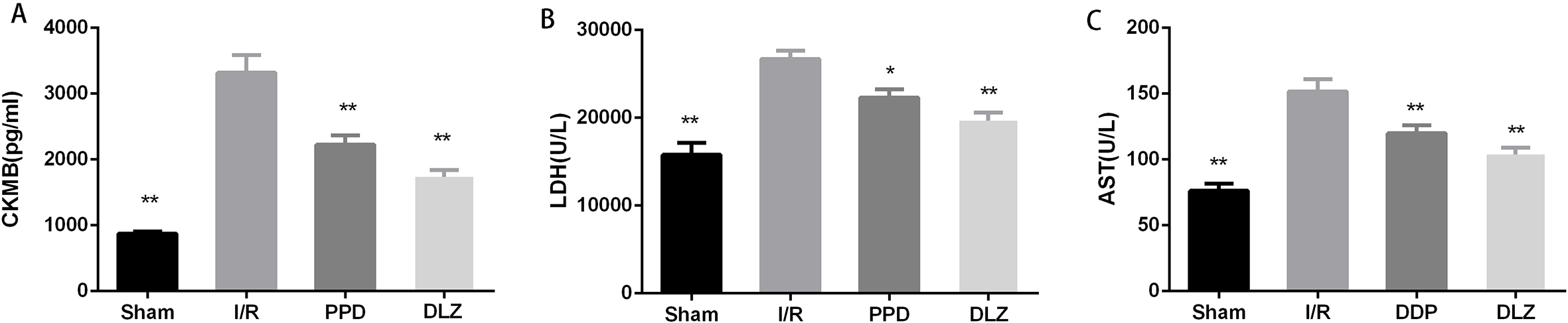
Changes in myocardial enzymes in serum of rats. (A) CKMB levels; (B) LDH levels; (C) AST levels. Data are expressed as mean ± SEM, n = 6. **P<0.01 and *P<0.05 vs. I/R group.
PPD Ameliorates Histopathological Injury of I/R Rat Heart
The myocardium histopathological alteration was observed by HE staining. As shown in Figure 5, Sham group exhibited normal architecture of myocardium, an orderly arrangement of myocardial fibers and no inflammatory cell infiltration. Meanwhile significant cardiomyocytes membrane damage such as extensive edema and inflammatory cell infiltration were observed in the I/R model group. In the PPD and DLZ group, these changes were markedly attenuated compared with in the model group. However, the myocardial cells still exhibited some swelling and a small amount of inflammatory cell infiltration was observed in the PPD group.

Representative HE staining histology photomicrographs of the myocardium following reperfusion (at magnification 200 ×).
PPD Decreases Cardiomyocyte Apoptosis in I/R Rats
Cardiomyocyte apoptosis plays a role in myocardial I/R injury. TUNEL assay was employed to ascertain the apoptosis of cardiomyocyte. Figure 6 showed that I/R injury significantly increased cardiomyocyte apoptosis compared with the sham group (P < 0.01). Pretreatment with PPD or DLZ markedly reduced myocardial apoptosis (P < 0.01).

Levels of apoptosis of rat cardiomyocytes. (A) Representative fluorescence photomicrographs (TUNEL, DAPI and the merge of them) of the myocardium following reperfusion (at magnification 200 ×); (B) relative cell death rates. Data are expressed as mean ± SEM, n = 5. **P<0.01 and *P<0.05 vs. I/R group.
PPD Alleviates Oxidative Stress in I/R Rats
To investigate whether PPD influence oxidative stress induced by I/R, we examined the SOD, GPx, and MDA level in rat heart homogenates. I/R increased MDA content and decreased the activities of SOD and GPx in heart tissues, indicating that oxidative stress occurred following I/R injury. PPD or DLZ treatment reduced MDA content, and increased the anti-oxidative capacity by upregulating the activities of SOD and GPx (Figure 7).

The levels of oxidative stress markers. (A) SOD activities; (B) GPx activities; (C) MDA levels. Data are expressed as mean ± SEM, n = 6. **P<0.01 and *P<0.05 vs. I/R group.
PPD Influences the Expression of Apoptotic Proteins
We also examined the expression of apoptosis-related proteins the rat heart by Western blotting and Immunohistochemistry analysis. As shown in Figure 8 the Bcl-2 was significantly lower, and the expression of Bax, c-Cas3 and c-Cas9 were higher in I/R group compared with sham group (P < 0.01). By contrast, treatment with PPD or DLZ markedly increased Bcl-2 and decrease the expression of Bax, c-Cas3, and c-Cas9 compared with I/R group (P < 0.01). Cytochrome C is a component of the electron transport chain in mitochondria. Once the integrity of mitochondria is impaired, the cytochrome C would be released to cytoplasm, resulting in apoptosis. Immunohistochemistry analysis showed that the expression of cytochrome C was significantly increased in I/R group compared with Sham group (P < 0.01), PPD or DLZ treatment significantly decreased cytochrome C protein expression (P < 0.01) (Figure 9), indicating that PPD confers a favorable role in maintaining the integrity of mitochondria.

The expression of apoptotic proteins via western blot. (A) Representative fluorescence photographs of western blot; (B-E) relative levels of protein expression of Bax (B), Bcl-2 (C), c-Cas3 (D), and c-Cas9 (E). Data are expressed as mean ± SEM, n = 4. **P<0.01 and *P<0.05 vs. I/R group.

The expression of cytochrome C via immunohistochemistry. (A) Representative immunohistochemistry staining histology photomicrographs of the myocardium following reperfusion (at magnification 200 ×); (B) relative levels (presented as IOD/Area) of protein expression of cytochrome (C). Data are expressed as mean ± SEM, n = 5. **P<0.01 and *P<0.05 vs. I/R group.
Discussion
Ischemia leads to many pathophysiology conditions, such as myocardial infarction, peripheral vascular dysfunction, stroke, and hypovolemic shock. Although restoration of blood flow is essential for ischemic organ to prevent irreversible damage, rapid changes in the intracellular environment following blood reperfusion cause serious cytotoxicity, which may exceed tissue injury that produced by the ischemia alone. 15
Myocardial ischemia/reperfusion elicits cardiomyocyte apoptosis, induces left ventricular remodeling, which in turn leads to irreversible functional and structural damage to the myocardium.
Ginsenosides, the major active components in ginseng, were classified into 2 types: protopanaxadiol and protopanaxatriol. Our previous studies has showed that protopanaxadiol-type ginsenosides exert significant cardioprotective effects. 6,9,10 In this study, PPD as the active metabolite of protopanaxadiol-type ginsenosides significantly attenuated I/R-induced myocardial infarction and improved left ventricular function with decreased LVIDs, LVIDd, and increased EF%, FS%. Elevation of cardiac enzyme, including AST, LDH, and CKMB, indicated the presence of myocardial injury. 16 This study observed simultaneous increases in serum AST, CKMB, and LDH following I/R, however, these increases were attenuated by PPD pre-treatment. It demonstrated that PPD could maintain membrane integrity thereby restricting the leakage of these enzymes. In addition, histological examination showed PPD prevent I/R-induced enhanced inflammatory cell infiltration and cardiac cell death, that further confirmed the protective effect of PPD on myocardium.
Previous studies have indicated that apoptosis serves an important role in the pathogenesis of heart dysfunctions induced by myocardial I/R injury. 15,17 Apoptosis is an evolutionarily conserved cell death pathway that is responsible for the programmed culling of cells during normal eukaryotic development and maintenance of organismal homeostasis. There were reports identified elements of apoptosis in myocytes as a response to reperfusion but not ischemia, 18,19 which indicated apoptosis may be a specific feature of reperfusion injury in cardiac myocytes, leading to late cell death. 20 In current study, TUNEL assay indicated that the level of apoptosis in PPD group was significantly lower than I/R group, indicated that PPD played a role in myocardial protection by resisting the apoptosis of cardiomyocytes in I/R rats.
Oxidative stress, defined as disturbances in the pro-/antioxidant balance, remains a major contributor to myocardial injury after ischemia followed by reperfusion. The restoration of blood flow initiated with a burst of ROS generation. ROS are typically scavenged by antioxidant enzymes, including SOD and GPx, which serve important roles in the prevention of lipid peroxidation. These markers could reflect the extent of oxidative stress. In present study, I/R increased MDA content and decreased the activities of SOD and GPx, that excessive oxidative stress was significantly prevented by PPD. Accumulating data suggest that ROS play an important role in the release of cytochrome C and other pro-apoptotic proteins, which can trigger caspase activation and apoptosis. Mitochondria releases cytochrome C which then binds to Apaf-1, recruits Caspase-9, leads to Caspase-3 activation. 21,22 Bcl-2 and Bax, members of the Bcl-2 family, are crucial regulatory factors in apoptosis. Bcl-2 can bind selectively to the active conformation of Bax to block it from inserting into the mitochondrial outer membrane, and prevent the release of cytochrome C, indirectly regulate the activation of caspases in related apoptotic pathways. 23 -26 The protein expression of cytochrome C, c-Cas3, c-Cas9, Bax, and Bcl-2 were detected using Immunohistochemistry or western blotting. According to the results, cytochrome C, c-Cas3, and c-Cas9 were overexpressed in the I/R myocardium; in turn, these proteins were decreased in the PPD pretreated I/R group. By contrast, the Bcl-2/Bax ratio was decreased in the I/R group compared with in the sham group, and subsequently increased by PPD pretreatment compared with the I/R group. The data indicated that PPD could reduce the products of oxidative stress, regulate Bcl-2 family, reduce the release of cytochrome C, thus inhibit the activation of caspase cascade.
Conclusions
The present study provided evidence that pretreat with PPD could alleviate apoptosis in myocardial ischemia/reperfusion injury by upregulating Bcl-2/Bax ratio, then reducing the release of cytochrome C and activation of Caspase-9 and Caspase-3. Another mechanism of the protective effects of PPD might be associated with the suppression of oxidative stress and mitochondrial damage as it could upregulate the activities of SOD and GPx. Taken together, PPD may be a potent drug for prevention of myocardial ischemia/reperfusion injury.
Footnotes
Acknowledgments
This study was supported by the Science and Technology Development Projects of Jilin Province (Grant 20170101002JC).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
