Abstract

Type 1 diabetes (T1D) is an autoimmune chronic disease characterized by absolute insulin deficiency, which causes abnormal blood glucose regulation. Currently, there are 1.25 million Americans diagnosed with T1D with approximately 64 000 new cases of T1D being diagnosed every year.1,2 There is no cure for T1D and patients with T1D rely on daily insulin administration. So, self-management of T1D is crucial to prevent or delay major complications. However, only a very small proportion of T1D patients have met the target range set by the American Diabetes Association. 3 Recent years have witnessed an explosion of artificial intelligence (AI)-enabled and data-empowered innovations in treating T1D patients. For instance, closed-loop systems (ie, “artificial pancreas”) and insulin pumps are reported to effectively improve T1D management as well as patient outcomes. To summarize the latest research in AI-enabled T1D treatment, we conducted a literature review with PubMed and Google Scholar to retrieve publications in peer-reviewed healthcare journals from January 2019 to May 2020 (see Table 1).
Literature on Artificial Intelligence and T1D Management (January 2019-May 2020).
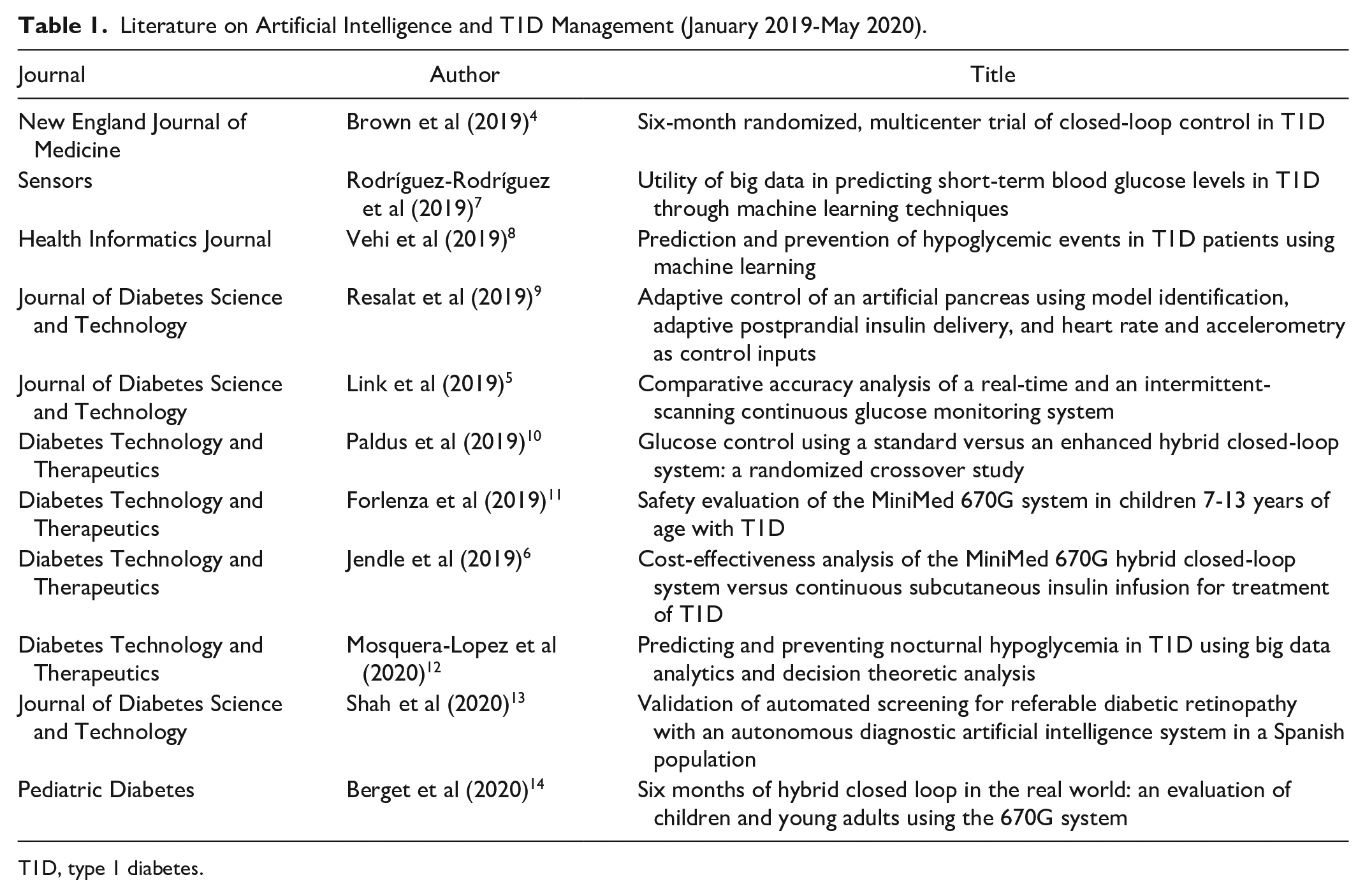
T1D, type 1 diabetes.
Overall, continuous improvements in safety, effectiveness, efficiency, and patient satisfaction using closed-loop systems to control blood glucose level in a broader T1D population (especially pediatric patients) were reported. The newest evidence was derived from various types of studies ranging from well-designed multicenter randomized clinical trial with six-month follow-up on closed-loop system to comparative study between real-time and intermittent-scanning continuous glucose monitoring (CGM) and to cost-effectiveness study on a hybrid closed-loop system compared with a continuous subcutaneous insulin infusion system.4-6 Notably, machine learning techniques applied in CGMs were reported to lead to significant reductions in postprandial hypoglycemia, decreased rates of closed-loop exits and alerts, improved glycemic control without detectable changes in psychosocial outcomes, and accurate prediction and prevention of nocturnal hypoglycemia. Also, the autonomous diagnostic AI system demonstrated superior sensitivity and specificity for diagnosing referable diabetic retinopathy and macular edema. Additionally, higher glycated hemoglobin level and workload required to use hybrid closed loop were suggested to be the significant factors associated with discontinuation. In a nutshell, there have been remark-able progress in AI-enabled technology in treating T1D reported in literature since 2019.
Yet, practical challenges and opportunities exist. Whether the observed benefits will sustain for prolonged use in real-world settings and how AI technologies will protect patient data privacy and security are crucial questions to address. During the past few years, personalized data, machine learning (in particular, deep learning and convolutional neural network techniques), and real-time adaptive algorithms combined with wearable devices have improved prevention and early detection, clinical decision support, deterioration risk prediction, and patient self-management of T1D. Future research endeavors and technological innovations should meet patients’ needs such as mitigating user’s workload and further enhancing outcomes, optimizing data protection, and realizing patient-centered care. Unquestionably, AI, Big Data, interdisciplinary research, and global collaboration will play an increasingly important role in achieving precision medicine for T1D patients.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
