Abstract
Oxidative stress induces nerve damage in type 2 diabetes mellitus and leads to diabetic polyneuropathy (DPN) and can affect the DNA and antioxidant status. Statins have pleiotropic, protective effects on the peripheral nerves of patients with diabetes. The aim of this study was to determine the effects of ezetimibe/simvastatin and rosuvastatin on DNA damage in patients with DPN. This randomized, double-blind, placebo-controlled, clinical trial comprised outpatients from Guadalajara, Mexico. The inclusion criteria were either gender, age 35–80 years, type 2 diabetes, glycated hemoglobin ≤10%, diabetic polyneuropathy stage 1/2, and signed informed consent. Patients who were taking antioxidant therapy or statins, had hypersensitivity to drugs, experienced organ failure, were pregnant or breastfeeding, or had other types of neuropathy were excluded. We assigned patients to placebo, ezetimibe/simvastatin 10/20 mg, or rosuvastatin 20 mg, and the primary outcomes were 8-hydroxy-2′-deoxyguanosine (8-OHdG) for DNA damage, 8-oxoguanine-DNA-N-glycosilase (hOGG1) for DNA repair, and superoxide dismutase (SOD). Seventy-four patients were recruited. Nine patients were included as negative controls. There were no differences in 8-OHdG between the healthy subjects (4.68 [3.53–6.38] ng/mL) and the DPN patients (4.51 [1.22–9.84] ng/mL), whereas the hOGG1 level was 0.39 (0.37–0.42) ng/mL in the healthy subjects and 0.41 (0.38–0.54) ng/mL in patients with DPN at baseline (p = 0.01). SOD decreased significantly in patients with DPN (5.35 [0.01–17.90] U/mL) compared with the healthy subjects (9.81 [8.66–12.61] U/mL) at baseline (p < 0.001). No significant changes in DNA biomarkers were observed in any group between baseline and final levels. We noted a rise in hOGG1 in patients with DPN, without modifications after treatment. There was a slight, albeit insignificant, increase in SOD in patients who were on statins.
Keywords
Introduction
Diabetes mellitus (DM) is a heterogeneous, chronic, and progressive disease that is caused by insulin resistance and pancreatic β-cell dysfunction leading to extracellular hyperglycemia. 1 Hyperglycemia promotes the characteristic macro- and microvascular complications of DM by increasing oxidative stress through reactive oxygen species (ROS) formation, 2,3 which in turn induces DNA damage, 4,5 including damage to the oxidized base, nonbase locations, and rupture of cross-links and DNA chains. 5 Further, fatty acid signaling pathways and oxidative stress defense against proinflammatory cytokines become dysregulated, as do DNA repair mechanisms. 6
Position 8 of guanine in DNA is susceptible to ROS-induced injury, causing oxidative DNA damage, reflected by the increase in 8-OHdG, a sensitive and specific mutagenic biomarker that effects DNA damage. 7 DNA repair through base excision is achieved through hOGG1 to reduce the noxious effects of 8-OHdG. 8 ROS can also impair cellular defense and compromise the antioxidant status, thus promoting oxidative stress-induced injury. 9
Diabetic polyneuropathy (DPN) is the most frequent microvessel complication in type 2 DM patients, developing in nearly 110 million people worldwide. 10 Its prevalence increases approximately 10% one year after DM is diagnosed and can be found in 50%, 25 years after the diagnosis of type 2 DM. 11 Several groups have described the mechanisms of peripheral nerve dysfunction, secondary to oxidative stress-induced damage in DM. 12
Statins (3-hydroxy-3-methylglutaryl coenzyme A inhibitors) are potent serum cholesterol reducers that have pleiotropic, protective effects on peripheral nerves in patients with DM. 13,14 Epidemiological studies have reported that dyslipidemia is a risk factor for DPN. 15 Simvastatin has antioxidant activity against hydroxyl radicals. 16 By adding ezetimibe to simvastatin, greater cardiovascular protection is achieved, secondary to a reduction in low-density lipoprotein cholesterol. 17 Rosuvastatin upregulates antioxidant defense in vitro and reduces the production of ROS-dependent nicotinamide adenine dinucleotide phosphate; 18 thus, it diminishes oxidative stress in patients with dyslipidemia. 19
We aimed to determine the effects of ezetimibe + simvastatin and rosuvastatin on oxidative stress-induced DNA damage and superoxide dismutase (SOD) in patients with DPN.
Materials and methods
In this randomized, double-blinded, placebo-controlled, clinical trial, patients took one daily dose of placebo (calcined magnesia), ezetimibe + simvastatin 10/20 mg, or rosuvastatin 20 mg at night for 16 weeks. We also included nine clinically healthy individuals to establish normal values of the biomarkers. Randomization was performed through computer-based assignment of codes. A pharmacist packed the medication in vials, containing 30 units each, similar in appearance, size, and form. We oversaw delivery of the vials every 4 weeks, which had been tagged with the assigned codes. Each patient received a diary to record the time and date that the pills were administered, to ensure adherence. Every month, the diary was revised, and a pill count was performed to guarantee adherence and medication safety. Laboratory safety profiles (creatine phosphokinase and liver and kidney function) were analyzed each month, and those who had significant adverse reactions were eliminated from the study.
The subjects were outpatients who had been recruited from the primary care clinics of Guadalajara and its surrounding areas. The inclusion criteria were either gender, age 35–80 years, type 2 DM that had been diagnosed per the American Diabetes Association criteria, 20 glycated hemoglobin (HbA1c) ≤10%, DPN as confirmed by Dyck, 21 and signed informed consent. The exclusion criteria were patients who had been taking any antioxidant therapy or statins for the past 3 months, hypersensitivity to the test substances, liver/kidney failure, pregnancy/breastfeeding, and other types of neuropathy. We rejected patients if they were nonadherent to the pharmacological treatment (less than 80% of pill intake) or when a statin was necessary, acute complications of DM, or evidence of severe impairment that prevented continuation with the treatment.
The sample size was calculated, based on the comparative effects of simvastatin and atorvastatin on oxidative stress markers and antioxidant status. 22 The type I error was 0.05, and the type II error was 0.20; the mean SOD in the control group was 106.87 versus 75.63 in the experimental group. The standard deviation (SD) was 14 µmol/L, with two treatment groups, an allocation rate of 1:1, and two tailed. As a result, there were 19 patients in each group.
After blood samples had been collected in two tubes (one with 0.1% ethylenediaminetetraacetic acid and the other dry), we separated the plasma and serum by centrifugation at 2000 r/min for 10 min at room temperature; then, the samples were stored at −80°C until use. The Synergy HT (BIOTEK, Winooski, Vermont, USA) microplate reader was used to perform all optical density readings.
8-Hydroxy-2′-deoxyguanosine
We used the enzyme-linked immunosorbent assay kit (8-hydroxy-2-deoxyguanosine; No. ab10124 Abcam®, Cambridge, UK) according to the manufacturer’ instructions. First, the plasma sample, enzyme immunoassay (EIA) buffer, standards, and 8-OHdG-AChE tracer were added to all the wells except for the blank. Then, we added the 8-OHdG monoclonal antibody and incubated the plate for 18 h at 4°C. The plate was washed with buffer for the recommended times, and 200 µL Ellman’s reactive was added to each well. The optical density was read at 405 nm, and levels of 8-OHdG were reported in nanograms per milliliter.
8-Oxoguanine-DNA-N-glycosylase-1
The repair of oxidative damage to DNA was measured using a commercial kit (Human-8-oxoguanine-DNA-glycosylase; MBS702793 MyBiosource®, San Diego, California, USA) according to the manufacturer’s instructions. The reagents and samples were prepared for the indicated dilutions. We added 100 µL of plasma and standards to the wells and incubated the plate at 37°C. The biotinylated antibody was aggregated and then incubated. We performed the corresponding washes and added the horseradish peroxidase–avidin, substrate, and stop solution at the appropriate times. The optical density was read at 450 nm, and the levels were reported in nanograms per milliliter.
Superoxide dismutase
We measured
Statistical analysis
We reported categorical variables as frequencies and percentages and analyzed them by χ 2 or Fisher’s exact tests as needed. We performed Kolmogorov–Smirnov and Shapiro–Wilk tests to determine the distribution of the main variables and concluded that they did not follow a normal distribution; thus, we expressed continuous variables as median (min − max). We used Wilcoxon test for intragroup comparisons and Kruskal–Wallis test for between-group comparisons, followed by Mann–Whitney U test as the post hoc analysis. We performed an intention-to-treat analysis. Results were significant at a two-sided p-value of <0.05, with the 95% confidence interval.
Ethical considerations
The Helsinki statements in the 64th General Assembly in Fortaleza, Brazil, in October 2013 were followed, in agreement with national and international laws. The protocol was revised and approved by the local research and ethics committee of the University of Guadalajara, under registry CEI/044/2014 and international clinical trial number NCT02129231 (clinicaltrials.gov).
Results
Demographics
A total of 107 patients were evaluated—18 were taking statins, 5 did not sign the informed consent form, 8 had another type of neuropathy, and 2 had end-stage renal disease. The remaining 74 subjects were randomly allocated to one of the three groups (Figure 1). The mean age was 54.55 ± 10.65 years, and none of the patients was aged under 30 years. The female:male ratio was 1.5:1. Gender, age, weight, height, body mass index, and duration of diabetes were similar between all treatment groups (Table 1).
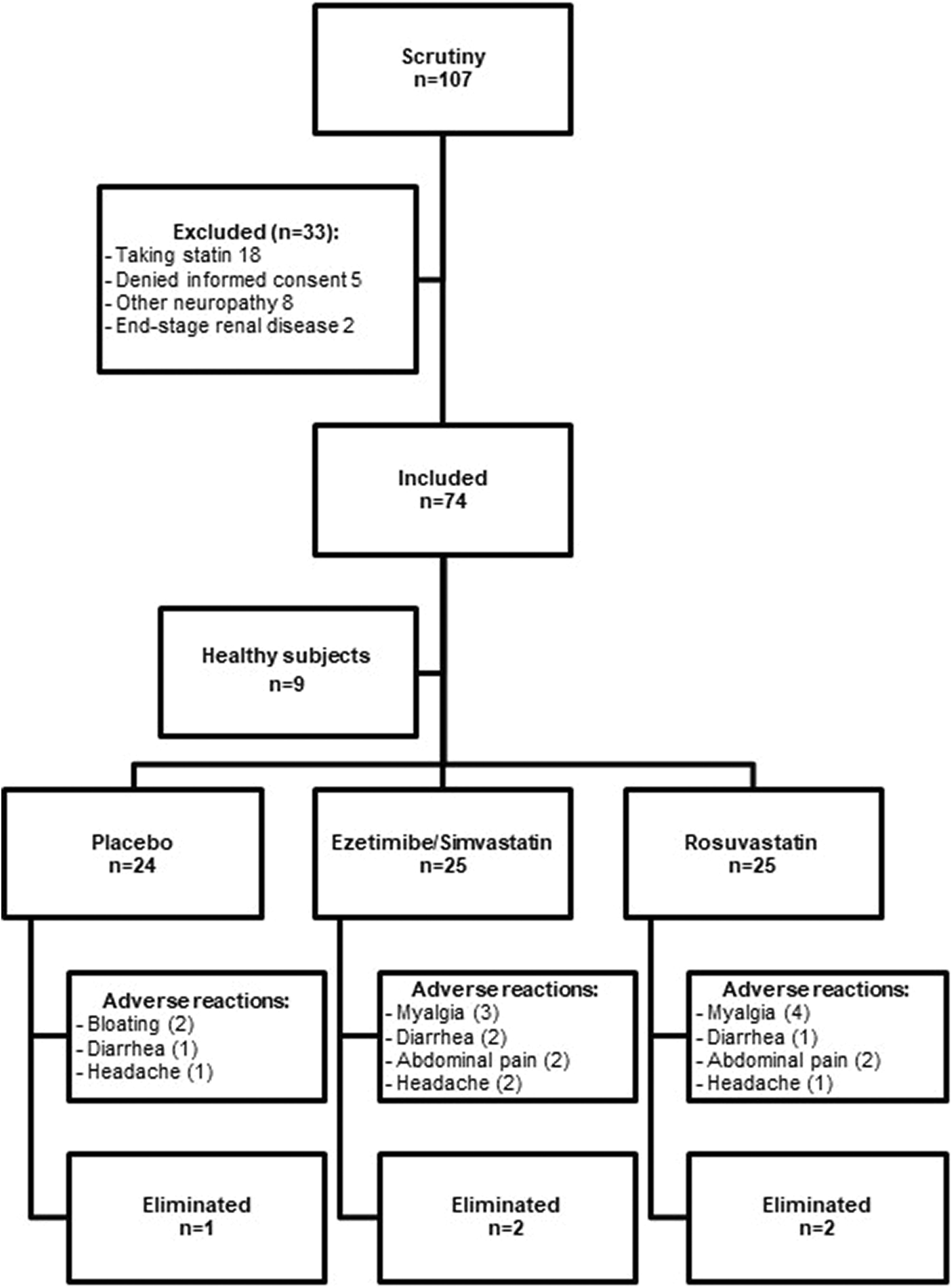
Flow chart diagram of patients.
Baseline demographic and clinical characteristics of healthy subjects and patients in each treatment group.a
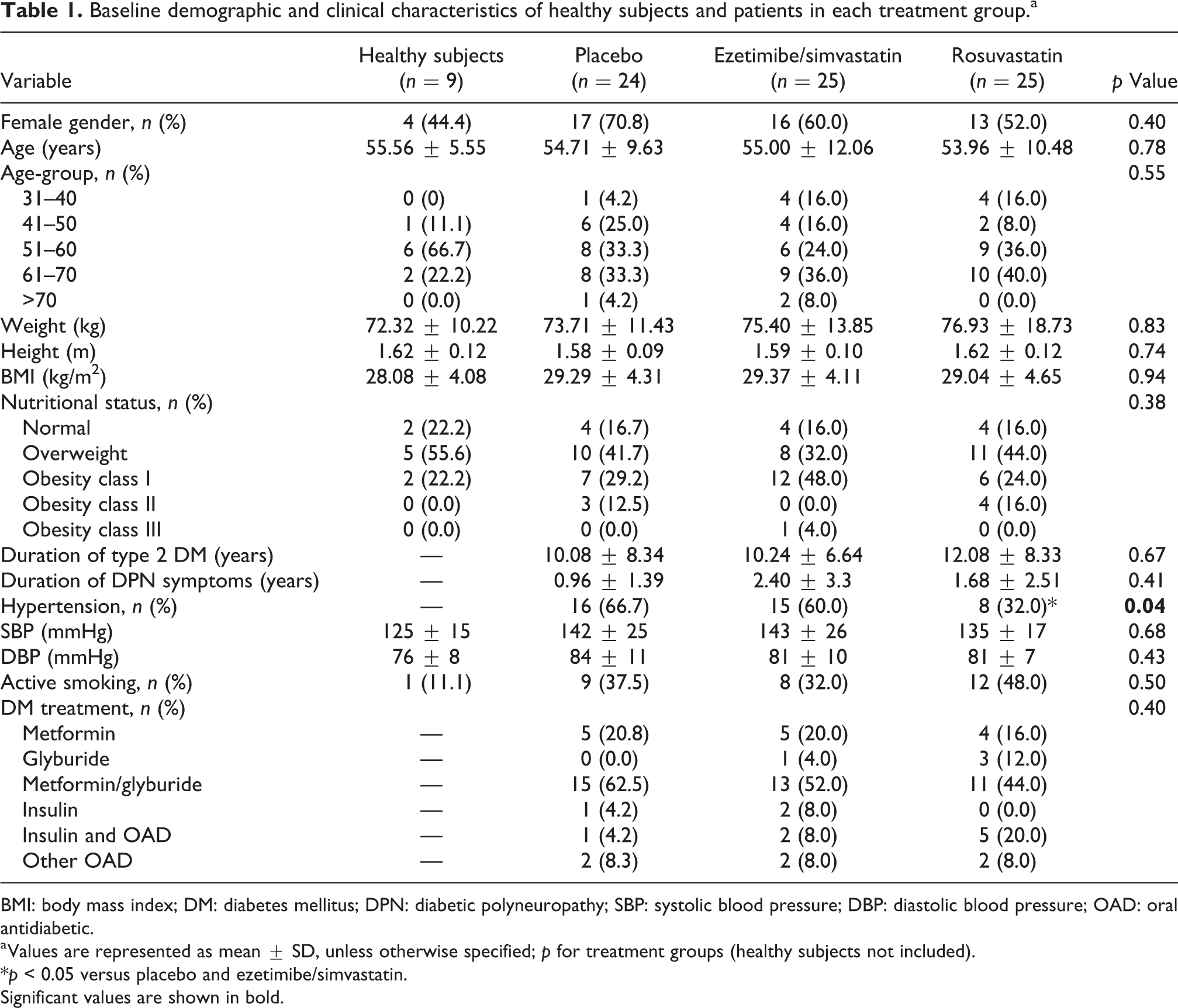
BMI: body mass index; DM: diabetes mellitus; DPN: diabetic polyneuropathy; SBP: systolic blood pressure; DBP: diastolic blood pressure; OAD: oral antidiabetic.
a Values are represented as mean ± SD, unless otherwise specified; p for treatment groups (healthy subjects not included).
*p < 0.05 versus placebo and ezetimibe/simvastatin.
Significant values are shown in bold.
Metabolic parameters
The baseline plasma glucose level in the placebo group was 186.40 ± 70.94 mg/dL versus 146.49 ± 49.75 mg/dL in the ezetimibe/simvastatin group and 188.59 ± 64.80 mg/dL in the rosuvastatin group (p = 0.07). Hyperglycemia was persistent, despite medical treatment, and did not differ between groups (p = 0.44).
The HbA1c level in the placebo group was 8.83 ± 1.76%, compared with 7.92 ± 1.51% in the ezetimibe/simvastatin group and 8.86 ± 1.99% in the rosuvastatin group (p = 0.16), and did not differ significantly at the end of the trial (p = 0.12).
Baseline total cholesterol levels were 211.43 ± 56.24 mg/dL for the placebo group, 210.71 ± 50.77 mg/dL for the ezetimibe/simvastatin group, and 216.81 ± 39.45 mg/dL for the rosuvastatin group (p = 0.80). The levels after the intervention were 202.35 ± 38.53 mg/dL, 130.35 ± 48.11 mg/dL, and 141.12 ± 41.89 mg/dL, respectively (p < 0.001).
The baseline triglyceride levels for the placebo, ezetimibe/simvastatin, and rosuvastatin groups were 240.13 ± 131.48 mg/dL, 239.22 ± 249.19 mg/dL, and 217.08 ± 121.32 mg/dL, respectively (p = 0.55); the final levels were 242.39 ± 142.56 mg/dL, 162.26 ± 105.97 mg/dL, and 167.75 ± 114.40 mg/dL (p = 0.03).
Laboratory safety parameters underwent minimal changes and did not affect creatine phosphokinase or liver or kidney function during the treatment period (data not shown).
The median and range for plasma 8-OHdG in healthy subjects was 4.68 (3.53–6.38) ng/mL versus 4.51 (1.22–9.84) ng/mL for patients with DPN (p = 0.79). The baseline levels for the placebo, ezetimibe/simvastatin, and rosuvastatin groups were 5.00 ng/mL (1.99–9.84), 3.99 ng/mL (1.22–9.84), and 4.06 (3.41–7.57) ng/mL, respectively (p = 0.57). After treatment, these levels were 4.50 ng/mL (1.83–19.63), 4.17 ng/mL (2.34–7.23), and 4.22 ng/mL (2.20–9.84) (p = 0.89).
The normal value of hOGG1 in the healthy subjects was 0.39 ng/mL (0.37–0.42) and 0.41 ng/mL (0.38–0.54) for patients with DPN (p = 0.01). The baseline levels were 0.41 ng/mL (0.38–0.54), 0.41 ng/mL (0.38–0.47), and 0.40 ng/mL (0.39–0.53) for the placebo, ezetimibe/simvastatin, and rosuvastatin groups (p = 0.65), compared with 0.41 ng/mL (0.38–0.45), 0.41 ng/mL (0.38–0.49), and 0.41 ng/mL (0.38–0.51) (p = 0.92), respectively, after the intervention.
SOD levels in healthy subjects were 9.81 U/mL (8.66–12.61) versus 5.35 U/mL (0.01–17.90) in DPN patients (p < 0.001). The baseline SOD levels were 5.73 U/mL (2.56–17.90) for the placebo group, 4.61 U/mL (1.99–7.97) for the ezetimibe/simvastatin group, and 5.72 U/mL (0.01–9.41) for the rosuvastatin group (p = 0.56). The final levels were 7.64 U/mL (0.12–17.69), 4.34 U/mL (1.51–18.09), and 5.23 U/mL (0.01–25.81) (p = 0.19) (Table 2).
Baseline and final levels of 8-OHdG, hOGG1, and SOD in patients with DPN.a
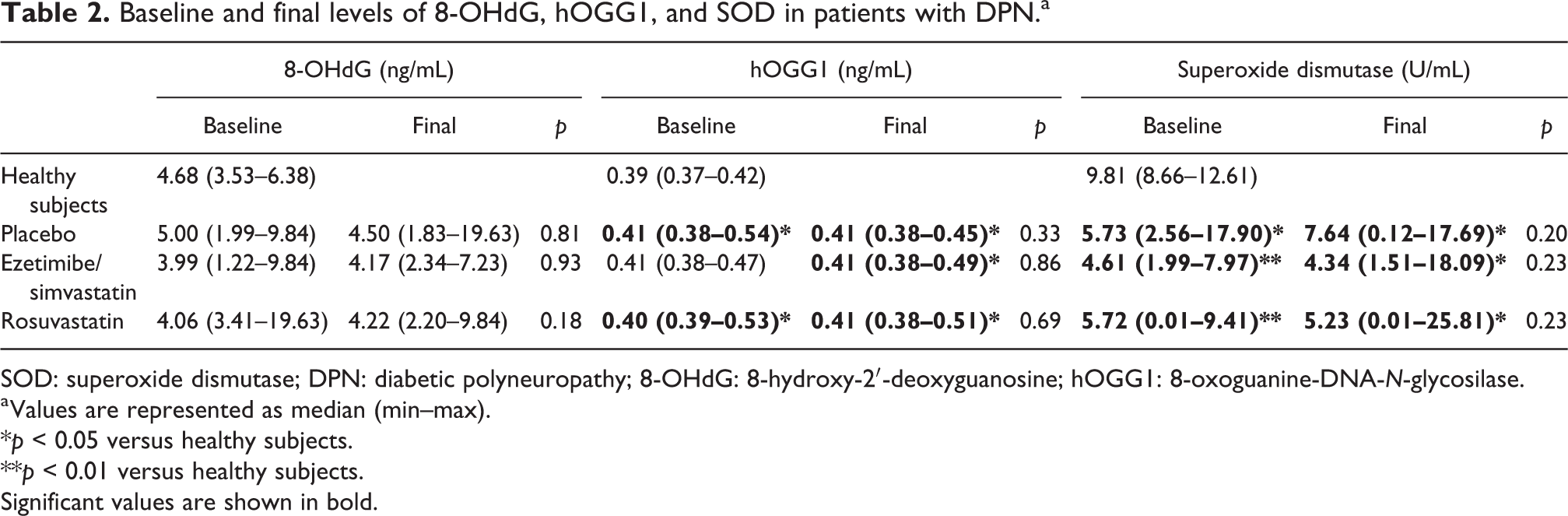
SOD: superoxide dismutase; DPN: diabetic polyneuropathy; 8-OHdG: 8-hydroxy-2′-deoxyguanosine; hOGG1: 8-oxoguanine-DNA-N-glycosilase.
a Values are represented as median (min–max).
*p < 0.05 versus healthy subjects.
**p < 0.01 versus healthy subjects.
Significant values are shown in bold.
Discussion
The baseline clinical and metabolic characteristics of patients with type 2 DM and DPN were similar between all groups. With regard to dyslipidemia, as expected, there was a significant reduction in the lipid profiles of patients who were treated with either statin, but rosuvastatin was more efficient in improving the triglyceride levels. Although our aim was not to examine metabolic parameters, glycemia status and lipid profile are variables that can alter antioxidant/oxidative homeostasis.
Studies have shown a reduction in the urinary levels of 8-OH2dG in patients with insulin-dependent and non–insulin-dependent DM; 23,24 further, higher levels of this biomarker have been implicated in the severity of microvascular complications in DM, suggesting a direct effect of 8-OH2dG in DPN. 25 Tonolo et al. reported a significant decrease in urinary 8-OHdG in patients with type 2 DM, microalbuminuria, and hypertension after 4-year treatment with simvastatin. 26 Abe et al. observed a decline in urinary 8-OHdG after 6 months of treatment with rosuvastatin in patients with diabetic nephropathy. 23
However, we failed to note any difference in the plasma levels of 8-OHdG in patients with DPN versus the healthy subjects or any change after 16 weeks of treatment with statins. These findings suggest that the baseline plasma 8-OHdG is similar in those with and without diabetes, at least in our study groups. Moon et al. reported similar results in patients with atherosclerotic cerebrovascular disease, wherein 99 patients with acute or chronic stroke received rosuvastatin 20 mg/day for 1 month. They evaluated the antioxidant effects of rosuvastatin on malondialdehyde (MDA), oxidized LDL (oxLDL), protein carbonyl content (PCO), and 8-OHdG (oxidative damage in lipids, proteins, and DNA) but did not observe any significant reduction in 8-OHdG or PCO, whereas MDA and oxLDL declined significantly. 24
Few studies have examined the response to the concentration of hOGG1 following the use of antioxidants. An observational study in patients with acute myocardial infarction reported that there were no differences in the concentrations of hOGG1 between patients who were receiving statin therapy or not. 26 In our study, the concentrations of hOOG1 were significantly elevated in the three groups of DPN versus the healthy controls. This finding suggests this repair enzyme is upregulated in response to oxidative damage and that concentrations within the normal ranges of 8-OHdG can be offset by the rise in hOOG1.
SOD is the first-line of defense against ROS. 27 In experimental and clinical research, a decrease in the activity of antioxidant enzymes, SOD, catalase, and glutathione peroxidase favors the development of microvascular complications in DM. 28,29 The baseline activity of SOD was reduced in patients with DPN compared with the healthy subjects before treatment initiation, consistent with other clinical investigations. 30 However, statins did not improve SOD activity significantly in our study. In streptozotocin-induced diabetic rats, a significant increase in SOD and catalase was reported with simvastatin treatment, 31 but we could not reproduce these results in patients with type 2 DM and DPN.
The baseline level of hOOG1 was increased in our study, likely due to counteracting mechanisms of DNA oxidative stress-induced damage; however, we would need more data on signaling pathways to make a definitive conclusion. Ezetimibe/simvastatin and rosuvastatin might provide antioxidant benefits by reducing dyslipidemia; however, statins did not reduce 8-OHdG or hOOG1 plasma levels. There was a slight increase in SOD in patients who were on statins, but this change was not significant, perhaps because the study was too short to induce relevant changes in uncontrolled patients with a long duration of diabetes.
Footnotes
Acknowledgments
We thank the laboratory staff of Hospital Civil of Guadalajara “Dr Juan I. Menchaca” for their aid in performing the metabolic parameters.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
