Abstract
Background:
Although botulinum neurotoxin (BoNT) injections may alleviate involuntary muscle contractions in hemifacial spasm substantially, it is less clear whether the motor effect would translate into improvements of health-related quality of life (HR-QoL).
Methods:
In this open-label clinical observational study, we characterized outcomes on HR-QoL in terms of the EuroQol (EQ-5D-5L) from BoNT in a prospective cohort of patients with hemifacial spasm (n = 73). Additionally, we characterized appendicular motor and nonmotor signs on motor symptom improvement, depressive symptoms, pain and sleep quality. Patients were assessed at the end of a regular 3-month period from last injection (timepoint1) and 4 weeks after the reinjection of BoNT (timepoint2).
Results:
Patients showed improved HR-QoL on the EQ-VAS (visual analogue scale) at timepoint2 compared with timepoint1. Moreover, we identified, that impairments in HR-QoL at timepoint1 correlated with life satisfaction and depressive symptoms, respectively. However, these associated variables did not predict the therapeutic effect. Instead, EQ-VAS at timepoint1 accounted for 34.5% of the variance of EQ-VAS improvement expressed as the difference between timepoint2 and timepoint1.
Conclusion:
Our study supports HR-QoL improvements in hemifacial spasm and the value of generic HR-QoL measures to estimate therapeutic outcome. However, the findings should be considered descriptive, and future high quality trials are needed for confirmatory purposes in order to refine treatment referral in hemifacial spasm with respect to QoL.
Introduction
Hemifacial spasm is characterized by involuntary muscle contractions. Although botulinum neurotoxin (BoNT) injections may alleviate the involuntary muscle contractions of hemifacial spasm substantially, it is less clear whether the therapeutic motor effect would translate into improvements of health-related quality of life (HR-QoL). 1 Previous studies provided sparse and heterogeneous findings to this end.2–5 This consideration is even more important as movement disorders characterized by involuntary muscle contractions reduce HR-QoL, not only through motor impairment. In addition, ancillary nonmotor domains like anxiety, depressive symptoms or pain regularly modulate HR-QoL, and may thereby deeply affect activities of daily living. Depiction of this multimodal interplay is critical, as HR-QoL outcomes emerge as a mainstay for therapy referral across movement disorders therapy. However, the data are sparse and there is a lack of high quality trials to confirm the effect of BoNT on HR-QoL in hemifacial spasm. HR-QoL outcomes may also be important in the future to support therapeutic decisions towards different therapies like BoNT or microvascular compression; however, comparative studies are still missing.
To get a closer insight on the effect of BoNT on HR-QoL in patients with hemifacial spasm, this observational clinical study was performed. We evaluated HR-QoL at the end of a regular 3-month reinjection interval (timepoint1), and after a 4-week follow up (timepoint2) together with an assessment of associated motor and nonmotor variables in patients regularly treated with BoNT.
Methods
Patients and study design
In total, we enrolled 75 patients with hemifacial spams receiving BoNT injections. We excluded two patients with hemifacial spasm secondary to underlying neurological conditions (i.e. one patient with spastic hemiparesis and one patient with multiple sclerosis). These two data sets were excluded since we assumed that HR-QoL would be critically dependent on motor manifestations in addition to hemifacial spasm, and therefore, these data might have confounded the outcome analysis. Patient characteristics are given as Table 1. A total of 72 of the 73 patients were having repeated BoNT injections and 1 patient received a first-time injection. We performed this open-label observational clinical study in a similar way to a current study on BoNT injections in different forms of dystonia (Weiss et al.; manuscript under review). Taken together, we assessed the self-reporting scores 3 months from the last BoNT injection (n = 72) or prior to first-time injection (n = 1) (timepoint1) during the patient’s visit in the outpatient clinic. The patients provided the self-reporting scales again 4 weeks after injection (timepoint2), at the time when we expected optimal BoNT efficacy. The assessments at timepoint2 were filled out by the patients at home and were returned by post. Therefore, given that the study focused on self-perceived outcome variables, no clinical severity ratings or clinical side effect assessment was considered in this study. We used the EuroQol (EQ)-5D-5L and EQ-VAS (visual analogue scale) to assess HR-QoL. These scores reflect the patient’s HR-QoL at the time of completion, 6 but do not recall the health status of the preceding days or weeks. Patients were recruited at the following neurological centres and practices in Germany: Centre for Neurology, Department for Neurodegenerative Diseases, Tübingen University, the Centre for Neurology Stuttgart Bürgerhospital, Centre of Neurology Sindelfingen, Neurology Practice ‘Dr Appy & Molt’ Stuttgart, and Neurology Practice ‘am Seelberg’ Stuttgart.
Patient characteristics.

BoNT, botulinum neurotoxin.
BoNT treatment was performed by neurologists with at least 5 years of experience in BoNT treatment. Patients received best individual treatment with injections plans that were generally established over repeated injection cycles (except for one first-time recipient). Further inclusion criteria were age > 18 years, written informed consent (given by the patient or, if applicable, by the legal representative). We excluded patients with intake of oral anticoagulants (e.g. phenprocoumon) or aminoglycoside antibiotics. The local ethics committee of Tübingen University and of the Landesärztekammer Baden-Württemberg, Germany approved the study, and patients participated after written informed consent was obtained. All patients were treated with BoNT A preparations (Dysport®, Botox®, and Xeomin®; Table 1).
Assessments
We analyzed outcomes on HR-QoL of the EuroQol (EQ) self-rating scale as the primary measure. The first part, EQ-5D-5L, comprises five questions on subjectively perceived mobility, self-care, usual activities, pain/discomfort, and anxiety/depression. Patients report as a self-rating on a five-point scale whether they have no problems (1), slight problems (2), moderate problems (3), severe problems (4), or extreme problems (5). The second part, EQ-VAS, is a vertical 20 cm visual analogue scale from 0–100 with steps of one in order to assess the self-rated momentary health state (0 indicating worst possible state, 100 indicating best possible state).
Further, we recorded the questionnaire on life satisfaction validated in the German language [i.e. ‘Fragen zur Lebenszufriedenheit’ (FLZ)] including the modules on: ‘general life satisfaction’ (FLZ-A), ‘satisfaction with health’ (FLZ-G), and satisfaction with movement disorder (FLZ-BS). Please note, that the acronyms are inspired by the original German version of the score. Further, we recorded Beck’s depression inventory (BDI), subjective ratings of self-perceived severity in both dystonia and head tremor, ranging from 1–10 respectively, average and maximal pain during the last 7 days assessed as visual analogue scale, Clinical Global Impression Scale, and Pittsburgh sleep quality index (PSQI). We obtained all scores in the German language. No sample size estimation was performed beforehand, as all statistical analyses were performed with exploratory intent.
Statistical analyses
We conducted nonparametric spearman correlation analysis in order to identify variables associated with impairments in HR-QoL at timepoint1.
Nonparametric Wilcoxon tests were applied for pairwise comparisons between timepoint1 and timepoint2. All tests were assessed using a two-sided alpha level of p < 0.05 (SPSS, Version 23, IBM, Ehningen, Germany). We corrected for false positives using the false discovery rate. 7 Finally, we used linear regression analysis to assess whether the variables from timepoint1 would yield predictive value for HR-QoL improvements. The statistical significance threshold was set to p < 0.05.
Results
HR-Qol of life was impaired at timepoint1 both according to EQ-5D-5L and EQ-VAS. We found that impairments in EQ-5D-5L correlated with ‘general life satisfaction’ scores of both movement disorders domain (FLZ-BS) and health domain (FLZ-G). Moreover, EQ-5D-5L correlated with depressive symptoms according to the BDI, and both mean and maximum pain intensity (Table 2). Similarly, impairments in EQ-VAS correlated with life satisfaction [general domain (FLZ-A), movement disorders domain (FLZ-BS), and health domain (FLZ-G)]. There were no correlations with either pain or sleep quality. Together, life satisfaction aspects and depressive symptoms were associated tightly with HR-QoL along EQ rating instruments, as expected.
Determinants of impairments in HR-QoL in facial hemispasm.

Correlation of quality of life according to EQ-5D-5L (1) and EQ-VAS (2) with associated variables. Spearman correlations were conducted. To correct for multiplicity, we adjusted the alpha level according to the false discovery rate. Significant correlations are indicated by asterisks.*
BDI, Beck’s depression inventory; EQ-VAS, EuroQol-visual analogue scale; FLZ-A, general life satisfaction; FLZ-BS, satisfaction with movement disorder; FLZ-G, satisfaction with health; HR-QoL, health-related quality of life; PSQI, Pittsburgh sleep quality index.
EQ-5D-5L indicated impairment of HR-QoL at timepoint1 (1.9 ± 2.7). EQ-5D-5L slightly decreased at timepoint2 (1.7 ± 2.8), however this did not reach significance (p = 0.241). However, there was a significant improvement measured with the EQ-5D-5L visual analogue scale when comparing timepoint1 (72.8 ± 17.6) with timepoint2 (77.7 ± 14.6; p = 0.008). Similarly, there was an improvement in ‘general life satisfaction’ (FLZ-A) (p = 0.011) and in depressive symptoms according to the BDI at timepoint2 (p = 0.005) (Table 3).
Outcome variables in facial hemispasm.
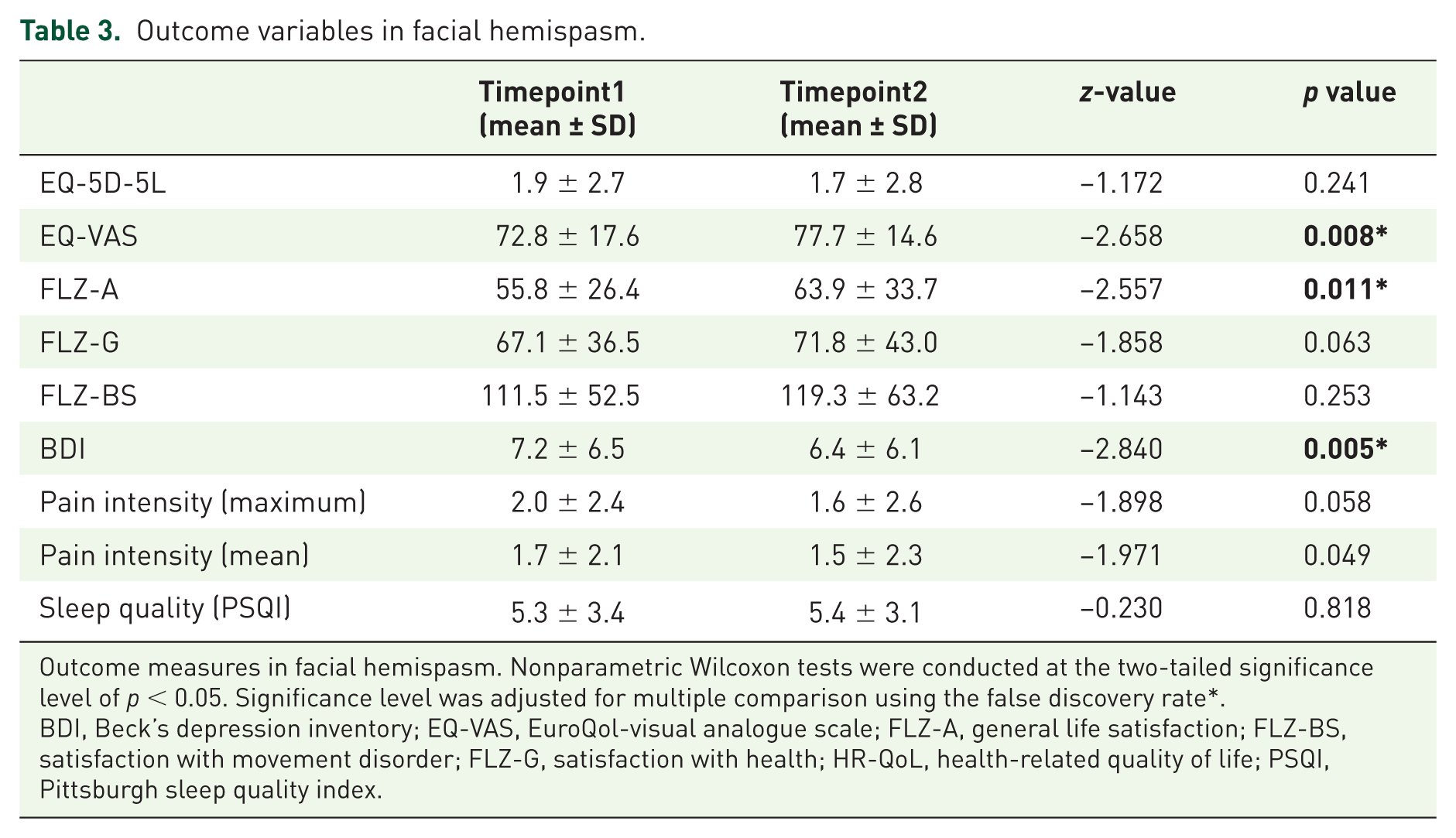
Outcome measures in facial hemispasm. Nonparametric Wilcoxon tests were conducted at the two-tailed significance level of p < 0.05. Significance level was adjusted for multiple comparison using the false discovery rate*.
BDI, Beck’s depression inventory; EQ-VAS, EuroQol-visual analogue scale; FLZ-A, general life satisfaction; FLZ-BS, satisfaction with movement disorder; FLZ-G, satisfaction with health; HR-QoL, health-related quality of life; PSQI, Pittsburgh sleep quality index.
Finally, we tested whether life satisfaction or depressive symptoms at timepoint1 would predict improvement of EQ-VAS expressed as the difference of the EQ-VAS scores at timepoint2 and timepoint1. There was no predictive value of any ‘life satisfaction’ domain (FLZ-A, FLZ-G, FLZ-BS), or BDI on EQ-VAS improvement. However, the EQ-VAS score at timepoint1 predicted EQ-VAS improvement (R2 = 0.345; p < 0.001).
Discussion
In this observational open-label clinical study, we identified that impairment in HR-QoL at timepoint1 (at the end of a treatment period and before reinjection) associated with impairment in life satisfaction and with depressive symptoms. Moreover, we provide evidence that BoNT improves HR-QoL according to the EQ-VAS. HR-QoL at timepoint1 was a suitable predictor of HR-QoL improvement through BoNT injection.
The effect of BoNT on HR-QoL was evident from the EQ-VAS scale, however, the improvement on EQ-5D-5L did not reach significance. On the one hand, the EQ-VAS may be sensitive to more fine-grained changes, since the score is scaled in narrow intervals from 0–100 in steps of one and allows the patient to give a rather global nonspecified impression of HR-QoL. On the other hand, we did not estimate the sample size of this study beforehand as we did not intend to conduct a proof-of-efficacy study here. Therefore, we will not draw any confirmatory conclusions from this study, and larger sample sizes might lead to a significant effect on EQ-5D-5L as well. Instead, we aimed to describe BoNT effects in this open-label study. These findings might support construction of future high quality trials including estimates of effect size and sample size as may be approached from this data pool. Such a high quality trial on HR-QoL still constitutes an unmet need in hemifacial spasm, even more, as only very few open-label studies with heterogeneous findings are available at present. In this aspect, one open-label uncontrolled study (n = 106) showed improvement of SF36 subdomains (except ‘social support’) 6–8 weeks after BoNT injection as compared with the preinjection period. 4 Interestingly, this improvement did not correlate with the formal severity improvement of hemifacial spasm. However, a prospective, double-blind randomized study (n = 36) found no difference in any SF36 subscale when comparing HR-QoL before and 16 weeks after BoNT injections. 5 Using such generic HR-QoL rating instruments like EQ or SF36 is warranted, given that patients with hemifacial spasm show impairment on such scales when compared with healthy patients. 8 Nonetheless, such scales may miss some specific disease-related aspects, and therefore the so-called HFS-30 questionnaire was introduced. In such a study, formal motor improvement of hemifacial spasm severity to BoNT correlated with the HFS-30 subdomains ‘stigma’, ‘emotional wellbeing’, and ‘social support’ whereas other subdomains lacked association (n = 80). 2 Interestingly, a further study (n = 106) identified greater knowledge about the disease condition as a predictor of therapeutic improvement of hemifacial spasm from BoNT injections. 3
As another important aspect, we found that HR-QoL impairment at timepoint1 correlated with several life satisfaction domains as well as with depressive symptoms. This is not surprising given that generic HR-QoL generally associates with several ancillary motor and nonmotor domains in addition to the severity of the core motor symptom. This was similar for example in patients with cervical dystonia. 9 Together, when considering BoNT therapy, it is important to notice that such ancillary variables may closely associate with HR-QoL and this fact may explain why some patients end up with unsatisfactory HR-QoL outcomes despite of a formal relief of involuntary muscle spasms. In addition, this study demonstrates that ancillary signs such as depressive symptoms may by themselves not be sufficient to predict therapeutic effects. In other words, although depressive symptoms strongly correlated with impaired HR-QoL at timepoint1, they did not predict the improvement of EQ-VAS from BoNT, nor did any other independent variable at timepoint1. Therefore, more complex interplay and multimodal influence may likely determine the degree of HR-QoL improvements. Only the EQ-VAS score at timepoint1 itself had weak predictive value for HR-QoL improvement accounting for 34.5% of the variability observed on the EQ-VAS improvement (p < 0.001) between timepoint2 and timepoint1.
Together, a complex interplay of HR-QoL, life satisfaction, motor and nonmotor variables will provide steps towards HR-QoL improvement and more accurate stratification and prediction models may arise from larger, prospective, and well-controlled data sets. To this end, a robust baseline assessment of untreated patients (prior to first BoNT injection) and follow up after first-time injection would give closer insight. Moreover, such a study would incorporate patients with unsatisfactory response to BoNT. We expect that poor responders were not well represented in this cohort, since they would presumably discontinue injections prematurely. Stratifying HR-QoL outcomes in hemifacial spasm may also be relevant when counseling patients for different therapy options that may include, apart from BoNT, microvascular decompression or alternative pharmacological treatment.
Together, we identified in this open-label uncontrolled study that BoNT improved HR-QoL according to the EQ-VAS in a ‘real-world’ setting. We consider these findings not confirmatory but hypothesis generating, and encouraging for future high quality trials on BoNT on HR-QoL. Apart from ‘proofing’ therapeutic efficacy on generic HR-QoL, such a study might also be of substantial value to refining treatment stratification procedures to distinct therapeutic alternatives. This is important, as HR-QoL stratifications are not well applicable, hitherto due to the very limited data sets available. However, they are important given that HR-QoL emerges as a key outcome variable in large fields of movement disorders nowadays.
Footnotes
Acknowledgements
We would like to thank Merz Pharmaceuticals (Frankfurt and Main, Germany) for financial support on this study.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study received financial support from Merz Pharmaceuticals.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
